Abstract
Objective
To compare the severity of cartilage degeneration after meniscal tears between juvenile and adult rabbits.
Design
This study included 20 juvenile rabbits (2 weeks after birth) and 20 adult rabbits (6 months after birth). Meniscal tears were prepared in the anterior horn of medial menisci of right knees. Rabbits were sacrificed at 1, 3, 6, and 12 weeks postoperatively. Cartilage degenerations in the medial femoral condyle and medial tibial plateau were evaluated macroscopically and histologically. The semiquantitative assessment of cartilage degeneration was graded by macroscopic Outerbridge scoring system and histological Osteoarthritis Research Society International (OARSI) scoring system.
Results
In juvenile rabbits, the morphologically intact cartilage and normal extracellular matrix architecture were observed at the first week postoperatively. Mild uneven cartilage surface and toluidine blue depletion in the medial femoral condyle were observed on histological assessment at 3 weeks postoperatively. The worsened cartilage deterioration demonstrating chondral fibrillation, prominent cell death, and glycosaminoglycan (GAG) release was observed at 6 and 12 weeks postoperatively. In adult rabbits, only mild cartilage degeneration was observed in the medial femoral condyle at 12 weeks postoperatively. The outcomes of Outerbridge and OARSI scores were consistent with the aforementioned findings in juvenile and adult rabbits.
Conclusions
Our study validated that earlier and more severe cartilage degenerations were observed in juvenile rabbits after meniscal tears compared with adult rabbits. Moreover, the post-tear cartilage degeneration demonstrated regional specificity corresponded to the tear position. However, caution is warranted when extrapolating results of animal models to humans.
Introduction
Meniscus is irreplaceable for knee joint physiological function due to its unique composition and structure. The critical functions of menisci include load-bearing, load transmission, and shock absorption. 1 Meniscal lesion was one of the most common orthopedic injuries in the United States. Approximately 850,000 surgeries on the menisci annually have been reported, which constitutes 10% to 20% of all orthopedic surgeries.2,3 The overall incidence of meniscal injury is 5.1 per 100,000 athlete exposures in high school athletes, with incidence of 3 of 100,000 during practice sessions and higher incidence of 12 of 100,000 during games and competition. 4 Therefore, meniscal injury occurs across a wide range of age groups ranging from children, young adults, elderly individuals, as well as the general population, and athletes.
There is ample evidence including animal and clinical studies suggesting that meniscal injuries are associated with the development of cartilage degeneration or even knee osteoarthritis (OA).5-8 Enormous animal studies have utilized medial meniscal transection (MMT) or destabilization of medial meniscus (DMM) to prepare OA animal model, which provided direct evidence that meniscal injuries cause joint degeneration or even OA often called post-traumatic osteoarthritis (PTOA).9-12 In clinic, a previous study evaluated baseline and follow-up MRIs of the knees in 43 patients (minimum time interval of 1 year, mean 1.8 years, range 52-285 weeks). They reported a higher incidence of cartilage loss in patients with meniscal injuries compared with those with intact meniscus. 13 Another previous study performed by Hunter et al. 14 assessed the baseline and follow-up MRIs of patients with OA and concluded that meniscal position and degeneration constituted a substantial proportion of the variances contributing to joint space narrowing. Overall, those studies highlighted that each abnormal change of meniscus had a substantial effect on cartilage loss.
To our knowledge, there is lacking study comparing the severity of cartilage degeneration after meniscal tears between juvenile and adult. In the present study, we prepared meniscal tears in the anterior horn of medial meniscus in juvenile and adult lapine model. The cartilage degeneration of knee joint was evaluated macroscopically and histologically in different time courses.
Method
Study Design
This study was approved by the Institutional Laboratory Animal Ethics Committee, and all experimental procedures were performed in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals. The present study included 20 juvenile female New Zealand white rabbits (2 weeks after birth) and 20 adult female rabbits (6 months after birth). A longitudinal vertical tear was created in the anterior horn of medial meniscus of the right knee, and the tear remained untreated. The intact menisci of the left knees served as the control. The designed sample size for each group was 5. The rabbits were sacrificed at 1, 3, 6, and 12 weeks postoperatively. Then, the knee joints were harvested and the cartilage of medial femoral condyle (MFC) and medial tibial plateau (MTP) was evaluated macroscopically and histologically.
Meniscal Tear Preparation
The rabbits were administered an intramuscular injection of xylazine hydrochloride (2 mg/kg). Then the rabbits were placed in a supine position. Following standard skin preparation and disinfection, the patella was dislocated laterally after creating a medial parapatellar incision. The anterior horn of the medial meniscus was pulled forward with forceps to enable sufficient exposure of the anterior horn. Then, a longitudinal vertical tear was created with corneal scissors. The meniscal tear with a length of 1 mm and a rim width of 1 mm was made in juvenile animals ( Fig. 1a ). The tear in the meniscal avascular area measuring 2.5 mm in length with a rim width of 1.5 mm was created in adult animals ( Fig. 1b ). All tears remained untreated. The patellar tendon and skin incision were then closed with a continuous suture pattern. The animals were injected with penicillin sodium once a day for 1 week to prevent infection and were permitted to move freely in a comfortable environment.
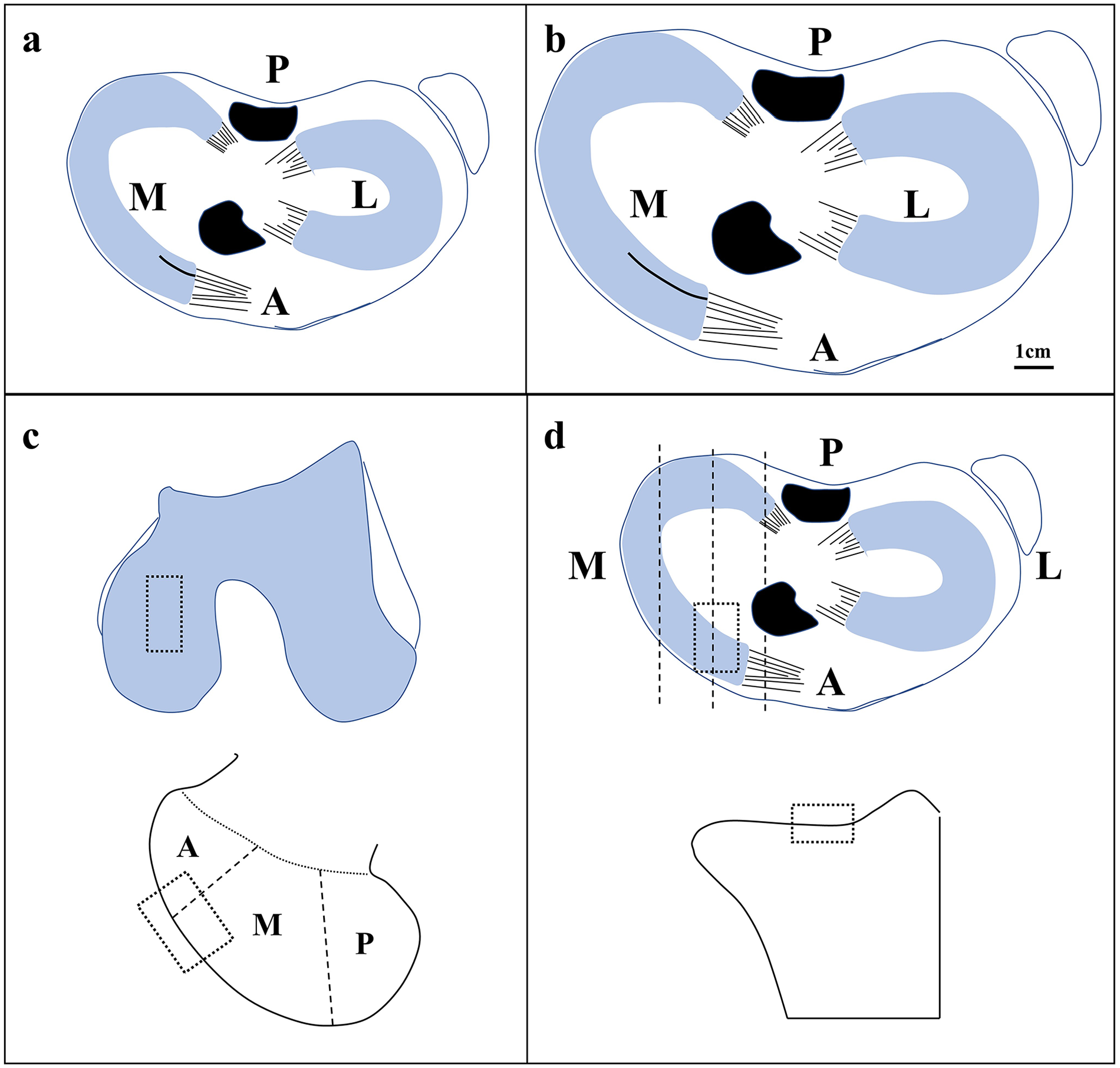
The diagram showing the preparation of medial meniscal tear and cartilage evaluation area. (
Sample Collection and Processing
Both left and right knees were harvested at 1, 3, 6, and 12 weeks postoperatively. After removing extra soft tissues, the femoral condyle and tibial plateau were harvested. Then, photographs of femoral condyle and tibial plateau were collected for subsequent macroscopic evaluation according to the Outerbridge classification. 15 After fixation in 4% paraformaldehyde for 5 days, the samples were decalcified by hydrochloric acid for 7 days. Then, the decalcified bone was embedded with paraffin after dehydration in graded ethanol. Subsequently, 3-µm-thick paraffin slices across the sagittal plane of the MFC and MTP were prepared by a microtome (Leica) for histological evaluation. The prepared slices were stained with hematoxylin-eosin (HE) and toluidine blue. The stained slices of HE and toluidine blue were captured by a digital slide scanner (NanoZoomer, Hamamatsu) and the subsequent histological evaluation of cartilage degeneration in MFC ( Fig. 1c ) and MTP ( Fig. 1d ) was completed according to OA cartilage histopathology assessment (Osteoarthritis Research Society International [OARSI] system).16,17
Statistical Analysis
All data are demonstrated with mean values with standard deviation (SD). The 2-way ANOVA along with Bonferroni multiple comparison test was applied for analysis. All statistical analyses were completed with the GraphPad Prism software, version 8.0.1 (GraphPad Software, USA). A P value < .05 is considered statistically significant.
Results
As observed in juvenile group, macroscopic assessment demonstrated a smooth surface of the MFC and MTP at the first week postoperatively after meniscal tears. Histological assessment showed similar outcomes demonstrating morphologically intact cartilage and normal extracellular matrix architecture. Otherwise, a mild uneven cartilage surface and toluidine blue depletion were observed on histological assessment at 3 weeks postoperatively. Moreover, the worsened cartilage deterioration was observed macroscopically and histologically at 6 and 12 weeks postoperatively. From the perspective of macroscopic evaluation, an uneven surface and abrasions in the MFC were detected. From the perspective of histological evaluation, the HE-stained samples of MFC demonstrated superficial chondral fibrillation, chondral erosions, and prominent cell death. The depletion of glycosaminoglycan (GAG) deposition in the MFC was reflected by toluidine blue staining. However, the findings aforementioned in MFC were not demonstrated in the MTP (
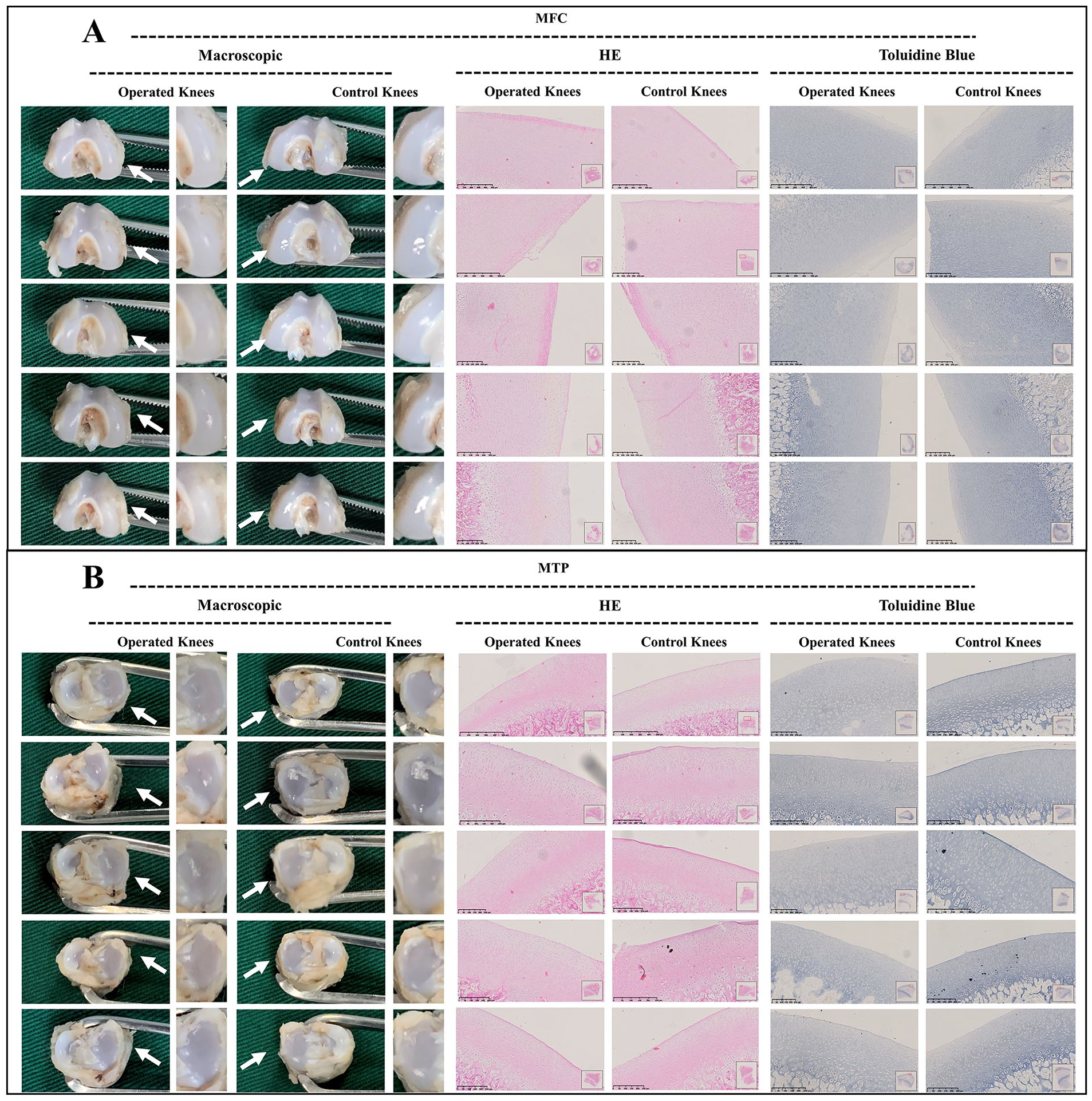
Macroscopic and histological analysis of cartilage degeneration in juvenile group at 1 week postoperatively. (
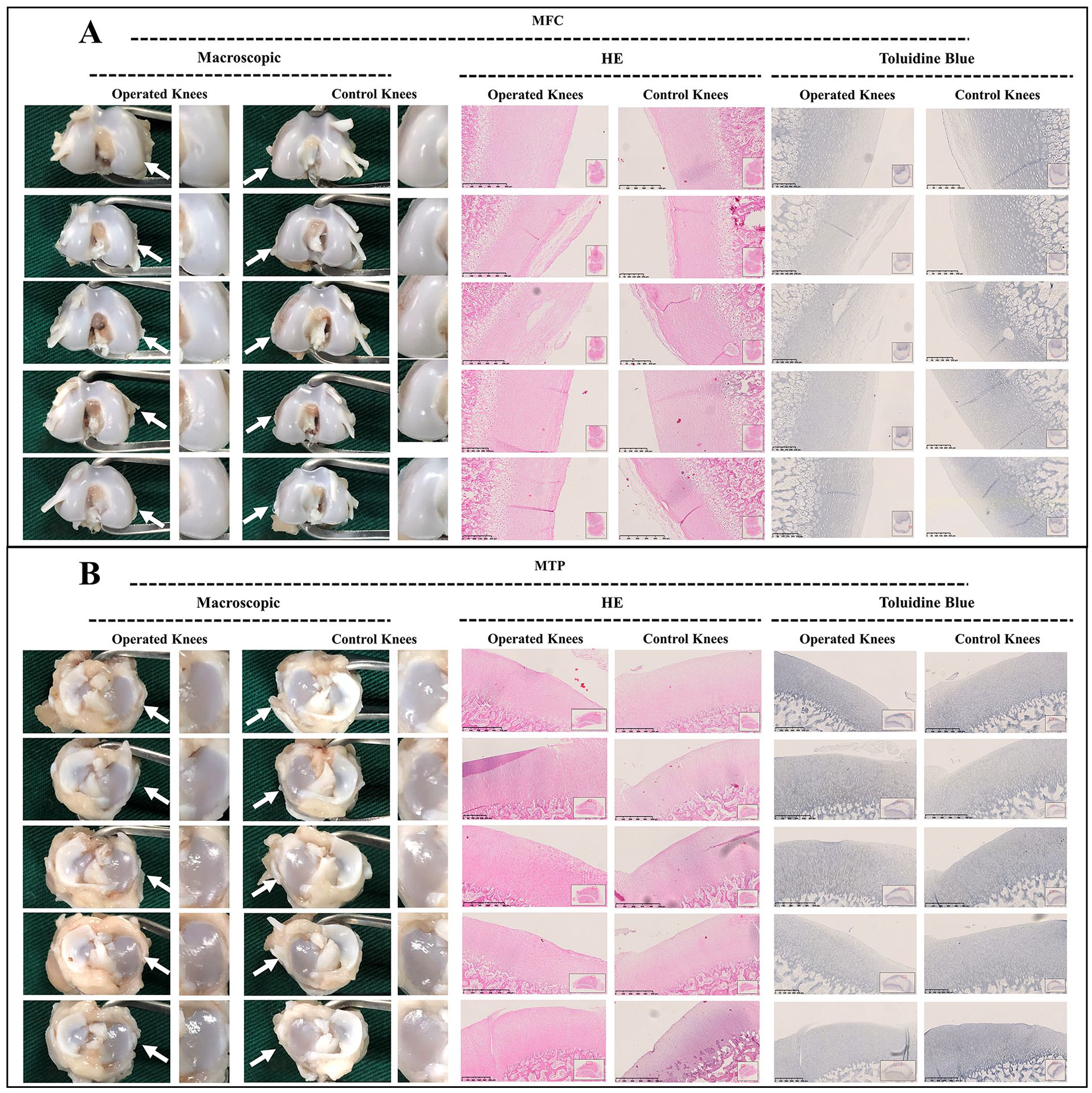
Macroscopic and histological analysis of cartilage degeneration in juvenile group at 3 weeks postoperatively. (
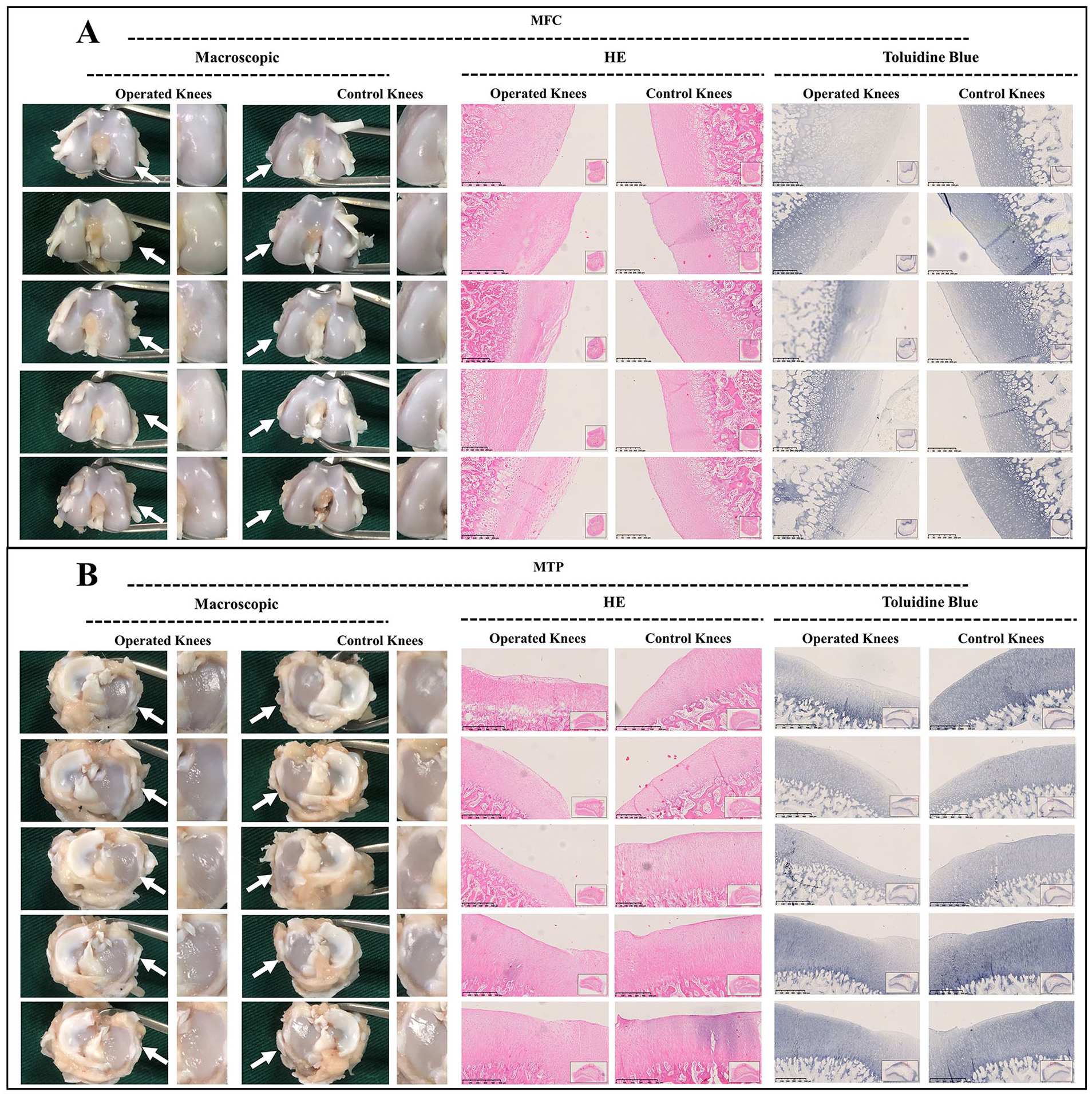
Macroscopic and histological analysis of cartilage degeneration in juvenile group at 6 weeks postoperatively. (
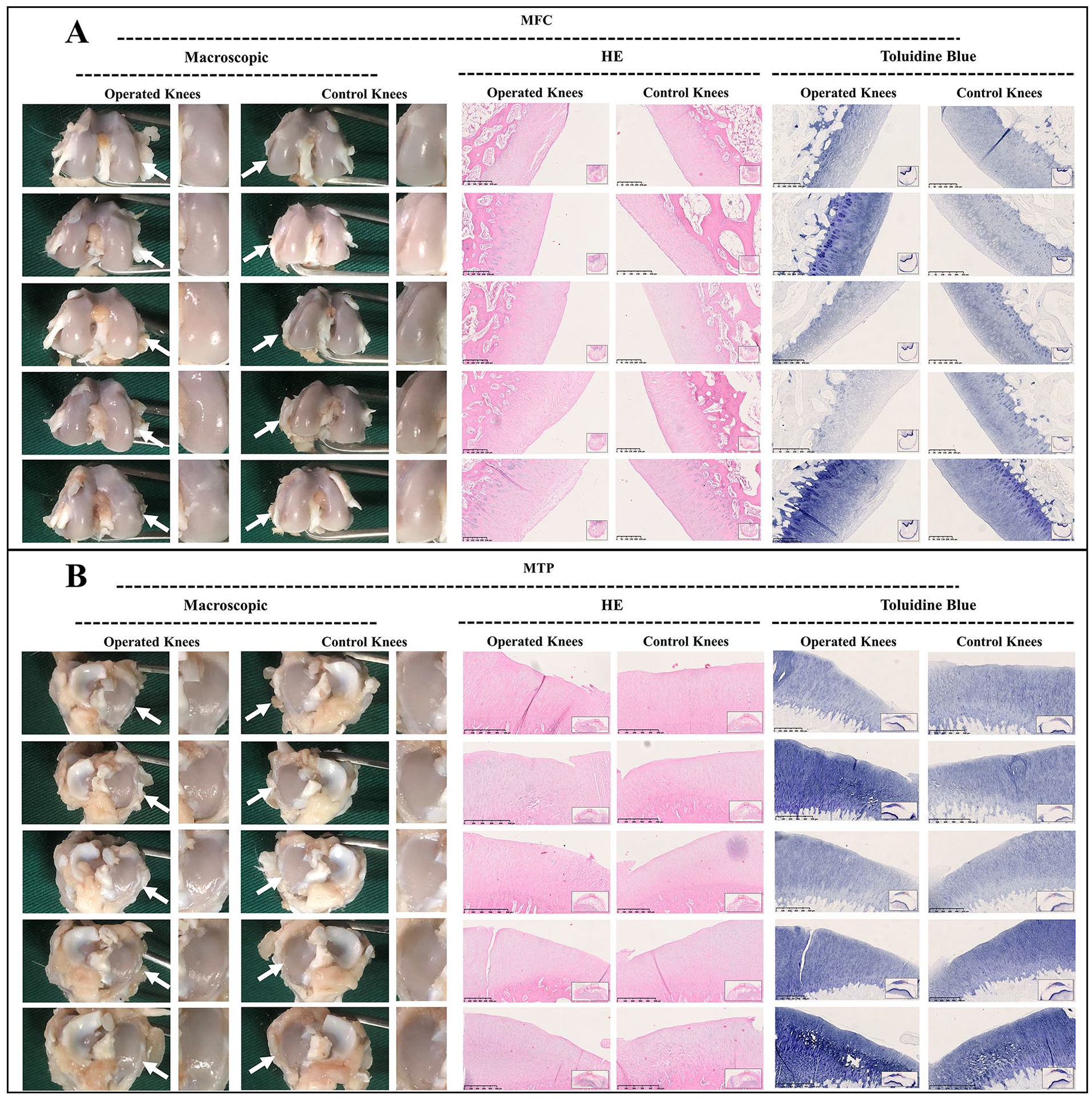
Macroscopic and histological analysis of cartilage degeneration in juvenile group at 12 weeks postoperatively. (
As demonstrated in adult group, macroscopic assessment of the MFC and MTP demonstrated a smooth surface without chondral erosions at 1, 3, and 6 weeks postoperatively, and the findings of histological evaluation were consistent with those of macroscopic findings. Only mild cartilage degenerations were observed in the MFC at 12 weeks postoperatively. Identically, the histological evaluation demonstrated a mild uneven surface and depletion of toluidine blue staining. Nevertheless, no clearly visible cartilage erosions or degenerations were observed in the MTP from the perspective of macroscopic or histological evaluation, even at 12 weeks postoperatively (
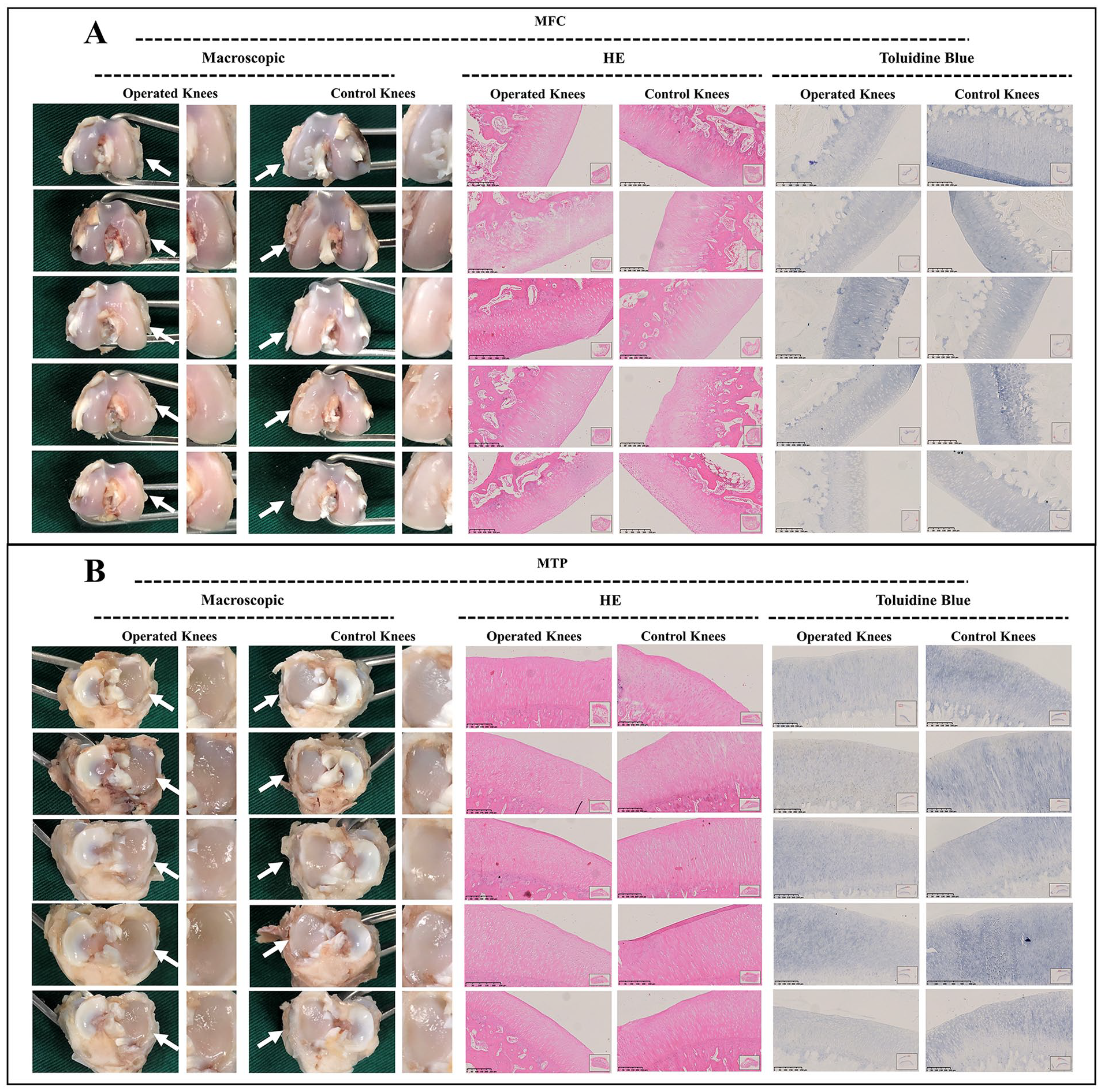
Macroscopic and histological analysis of cartilage degeneration in adult group at 1 week postoperatively. (
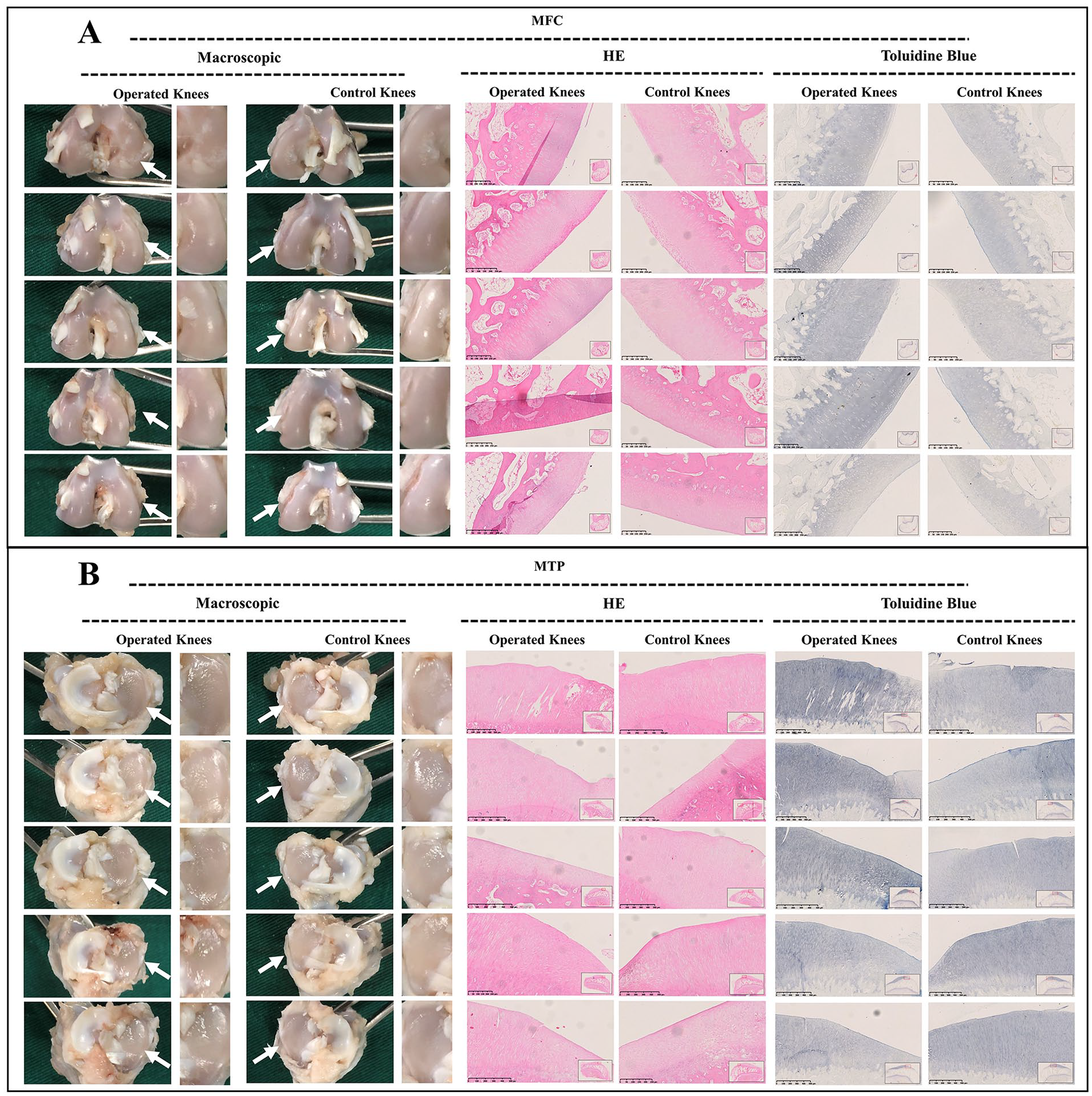
Macroscopic and histological analysis of cartilage degeneration in adult group at 3 weeks postoperatively. (
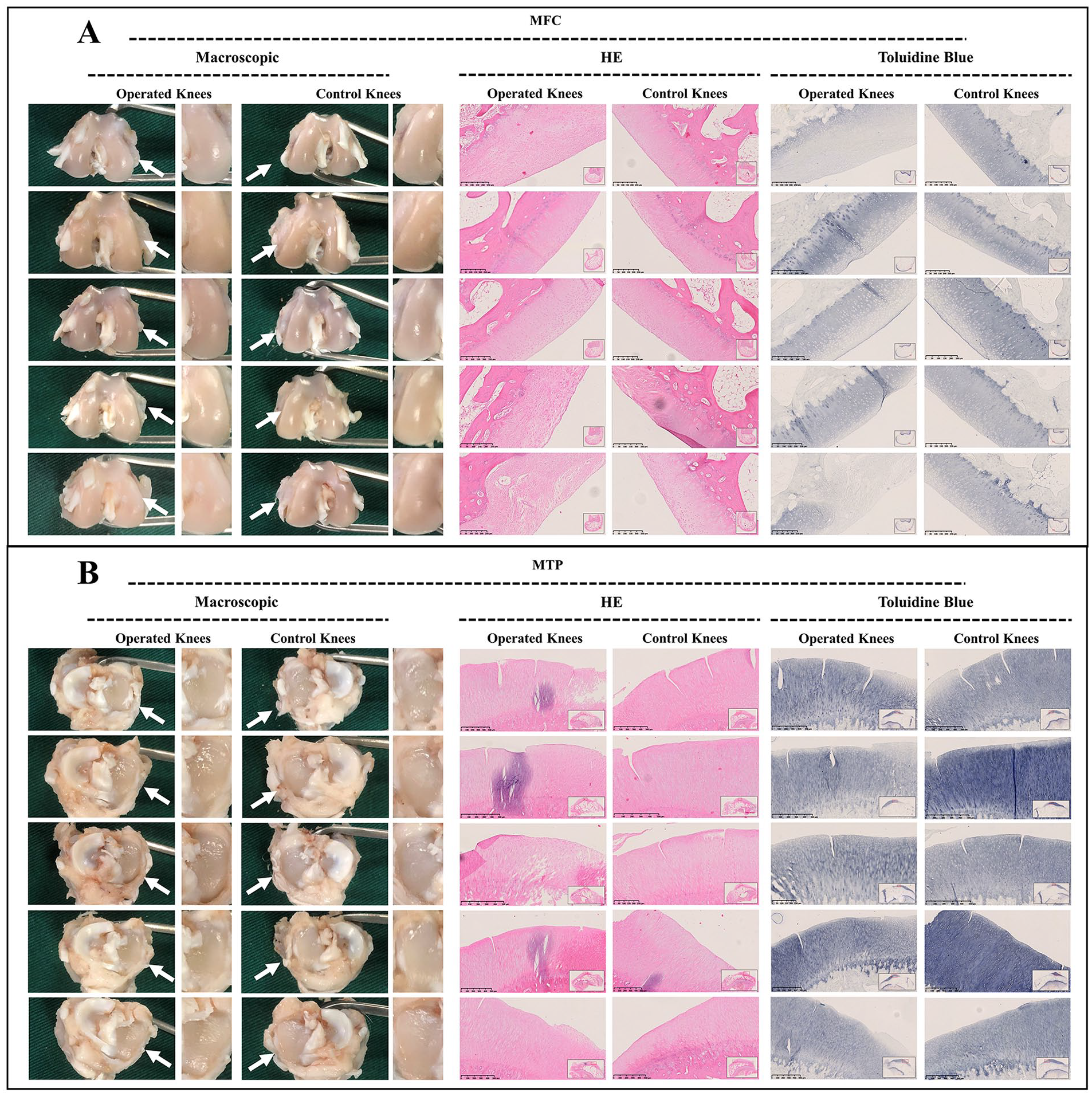
Macroscopic and histological analysis of cartilage degeneration in adult group at 6 weeks postoperatively. (
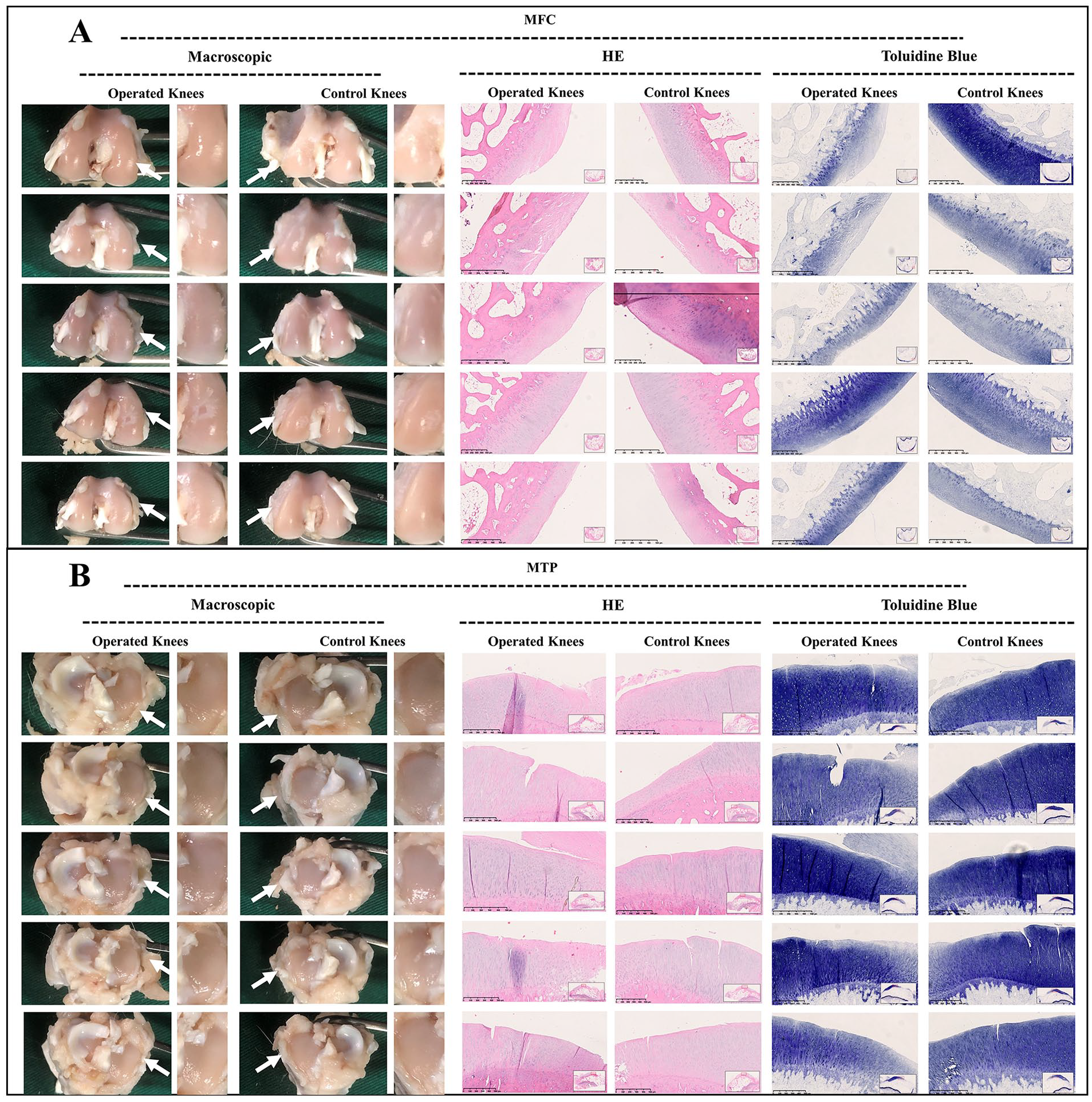
Macroscopic and histological analysis of cartilage degeneration in adult group at 12 weeks postoperatively. (
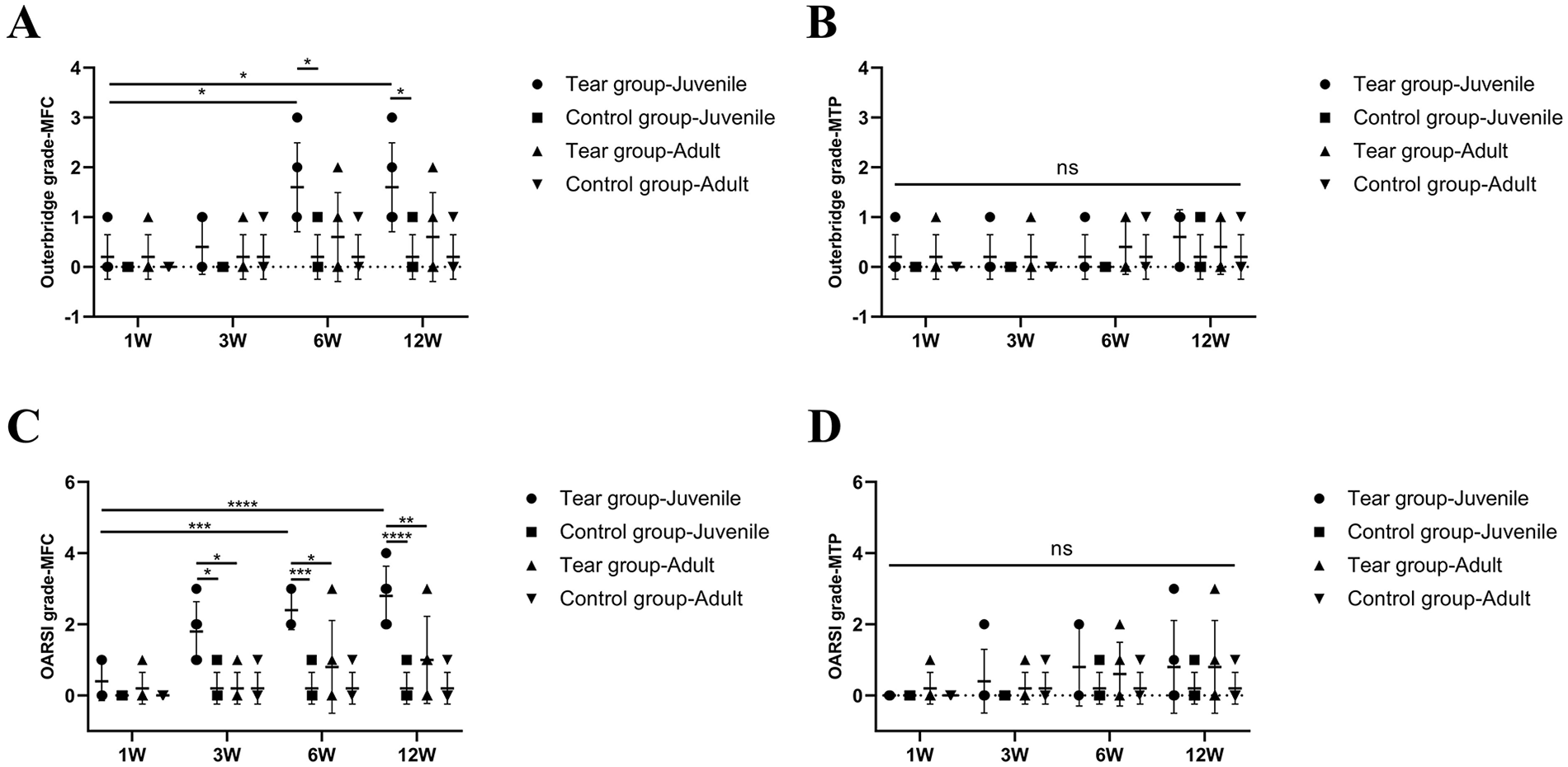
Outerbridge scoring and histological OARSI scoring for cartilage degeneration. (A) Outerbridge scoring of MFC. (B) Outerbridge scoring of MTP. (C) OARSI scoring of MFC. (D) OARSI scoring of MTP. Scores are expressed as mean values with SD. n = 5. MFC = medial femoral condyle; MTP = medial tibial plateau; ns = no significant difference; OARSI = Osteoarthritis Research Society International. *P < 0.05, **P < 0.01, ***P < 0.0005, ****P < 0.0001.
Discussion
In this study, earlier and more severe knee joint cartilage degeneration occurs after meniscal tears in juvenile rabbits compared with adult rabbits. The uneven cartilage surface and GAG degradation were observed in juvenile MFC cartilage at 3 weeks postoperatively. The worsened cartilage deterioration with superficial cartilage fibrillation, cartilage erosions, and prominent cell death was observed at 6 and 12 weeks postoperatively. However, no signs of cartilage degeneration were observed in adult lapine joint cartilage at 1, 3, and 6 weeks postoperatively. Only mild degeneration was presented in MFC at 12 weeks postoperatively.
The subsequent cartilage degeneration after meniscal injuries has been demonstrated by many previous studies including animal and clinical studies.9-12 In our study, we also observed cartilage degeneration in MFC after medial meniscal tears, especially in juvenile rabbits. Moreover, previous study has elucidated that the deleterious effect of meniscal tears on cartilage loss was not spatially uniform across the joint. 18 Chang et al. 18 assessed the relationship between a tear within a specific meniscal segment and subsequent cartilage loss in subregions that the torn segment overlies. They concluded the medial meniscal body tear was correlated with cartilage loss in external femoral subregions as well as central and anterior tibial subregions. Interestingly, we observed cartilage degeneration mainly in the anterior region of MFC and MTP after meniscal tears in the anterior horn of medial meniscus.
The alterations in joint biomechanics caused by meniscal tears have been reported to play a role in the initiation and progression of cartilage degeneration. 19 Moreover, many previous studies have validated that abnormal excessive mechanical load would lead to cartilage matrix degradation20,21 and chondrocyte apoptosis. 22 Recent researches have also assessed the biological impact of meniscal lesions on synovial fluid and articular cartilage. A previous study demonstrated elevated activity of matrix metalloproteinase (MMP) and level of prostaglandin E2 (PGE2) in the synovial fluid of patients diagnosed with meniscal tears. 23 They found total activity of MMP and PGE2 were increased 25-fold and 290-fold, respectively, in meniscal tear patients as compared with the controls. These biological factors are proinflammatory and may initiate the degeneration of cartilage. This may further predispose cartilage to mechanical damage after meniscal injuries.
Our findings indicated that earlier and more severe cartilage degeneration was observed in juvenile rabbits compared with adult rabbits after meniscal lesions. Previous studies have demonstrated that juvenile cartilage was more susceptible to injurious loads compared with adult cartilage.24,25 Levin et al. 24 demonstrated that chondrocytes in immature cartilage were more vulnerable to load-induced injury compared with cells in mature cartilage. They speculated that the less organized pericellular matrix, less deposition and organization of collagens, and the greater thickness of cartilage superficial zone may account for the increased susceptibility of immature cartilage to abnormal loading. A review concluded increased level of cell death, GAG loss, and reduction in biosynthetic activity were observed in immature cartilage tissue that responded to mechanical-caused injury compared with mature cartilage. 25 The aforementioned studies were consistent with our findings. Interestingly, we also found cartilage degeneration in the femoral condyle was more severe compared with that of tibial condyle. The paradoxical motion between femoral condyle and meniscus during joint motion may potentially account for greater cartilage degeneration. Thus, based on the findings of our study, meniscal tears necessitate urgent restoration of mechanical stability to prevent subsequent cartilage degeneration, especially for juvenile.
Following are the limitations of this study: (1) We only evaluated cartilage degeneration after meniscal tears. The evaluations for other tissues, such as synovium and subchondral bone, within the knee joint were absent in the present study. (2) This study included only a 12-week observation period, without any further investigations on cartilage changes that might occur beyond 12 weeks. (3) We only prepared longitudinal vertical tears in the anterior horn of medial meniscus; however, other tear types in other meniscal segments were not included.
Conclusion
Our study validated that earlier and more severe cartilage degenerations were observed in juvenile rabbits after meniscal tears compared with adult rabbits. Moreover, the post-tear cartilage degeneration demonstrated regional specificity corresponded to the tear position. However, caution is warranted when extrapolating results of animal models to humans.
Footnotes
Acknowledgments and Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by National Natural Science Foundation of China (Nos. 82172420, 81972101, 81871770) and Beijing Municipal Science & Technology Commission (No. Z171100001017085).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
