Abstract
Introduction
Injuries to articular cartilage have a poor spontaneous repair potential and no gold standard treatment exist. Particulated cartilage, both auto- and allograft, is a promising new treatment method that circumvents the high cost of scaffold- and cell-based treatments.
Materials and Methods
A comprehensive database search on particulated cartilage was performed.
Results
Fourteen animal studies have found particulated cartilage to be an effective treatment for cartilage injuries. Many studies suggest that juvenile cartilage has increased regenerative potential compared to adult cartilage. Sixteen clinical studies on 4 different treatment methods have been published. (1) CAIS, particulated autologous cartilage in a scaffold, (2) Denovo NT, juvenile human allograft cartilage embedded in fibrin glue, (3) autologous cartilage chips—with and without concomitant bone grafting, and (4) augmented autologous cartilage chips.
Conclusion
Implantation of allogeneic and autologous particulated cartilage provides a low cost and effective treatment alternative to microfracture and autologous chondrocyte implantation. The methods are promising, but large randomized controlled studies are needed.
Keywords
Introduction
The use of particulated articular cartilage (minced cartilage or cartilage chips) is emerging as a treatment modality in articular cartilage repair to overcome the current challenges in cost and long-term outcome for marrow stimulation and cell-based cartilage repair. 1 The surge of these collective methods has been motivated by both encouraging clinical and experimental results, but also the need for a cheaper and potentially more cost-effective treatment for articular cartilage lesions.
Microfracture-based treatments are widely accepted as an effective gold standard for small and intermediate sized cartilage defects as they provide a predictable clinical improvement in the majority of patients. 2 However, the repair tissue is not hyaline cartilage, but rather a mixture of fibrous tissue and fibrocartilage, and the early good outcome tends to deteriorate in long-term follow-up.3,4 For larger cartilage defects the most promising method in short- and long-term follow-up studies has been autologous chondrocyte implantation (ACI) treatments. Most reports on clinical outcomes following ACI-based treatments are on small or intermediate sized defects, 5 but despite relatively good results, the high cost of commercial cell culture and 2-step surgery have severely limited their use. Recently, the high cost of up to €20-30,000 per chondrocyte culture has resulted in public health care providers in many countries completely abandoning their use. 6 Instead, stand-alone scaffolds and plugs has provided an alternative that is financially more acceptable and with short-term outcomes comparable to microfracture. However, concerns regarding their regenerative potential and repair tissue morphology and consequently the long-term outcomes have been raised.7-9
The clinical use of particulated cartilage for cartilage defects was first described in 1983 by Albrect
In 2007, a new cartilage chip-based product, the Denovo NT was introduced. Denovo NT utilizes the increased chondrogenic potential of juvenile articular cartilage by implanting juvenile articular cartilage fragments in chondral defects. The use of allogenic juvenile cartilage makes Denovo NT an off-the-shelf product. A large number of patients have been treated and the clinical results are promising. 13
This recently motivated the group behind the present review to follow-up on the encouraging findings from previous studies. This application allowed the use of techniques and technology readily available in any conventional surgical setting by simply cutting autologous cartilage biopsies into 0.25 to 0.5 mm3 chips using a scalpel in the operating theatre and embedding these in fibrin glue before placing them in the debrided defect.
The increasing number of publications describing the use of particulated cartilage for the repair of cartilage defects in the knee motivated the present literature review. Hence, the scope is to review the current experimental and clinical literature on the use of particulated autologous and allogenous cartilage for articular cartilage repair.
Materials and Methods
Article Identification and Selection
Literature search was performed using the Cochrane Database of Systematic Reviews, the Cochrane Central Register of Controlled Trials, PubMed, Scopus, and MEDLINE (1980 to 2019).
The queries were performed in January 2020. The literature search strategy included the following: Search ((CAIS [All Fields] OR “cartilage autograft implantation system” [All Fields]) OR (ADTT [All Fields] OR “autologous dual tissue transplantation”[All Fields]) OR (PJAC [All Fields] OR “particulated juvenile articular cartilage”[All Fields]) OR (CAFRIMA [All Fields] OR “cartilage autologous fragment implantation matrix augmented”[All Fields]) AND (“allografts”[MeSH Terms] OR “allografts”[All Fields] OR “allograft”[All Fields]) OR (“autografts”[MeSH Terms] OR “autografts”[All Fields] OR “autograft”[All Fields])) AND (“chondral”[All Fields] OR “osteochondral”[All Fields] AND “cartilage”[All Fields]) OR “articular cartilage”[All Fields]).
Inclusion criteria were as follows: clinical and experimental outcomes of particulated cartilage for the treatment of chondral and osteochondral defects in articular joints in human and large animal studies, English language, minimum follow-up of 6 months for all patients in the cohort, and minimum study size of 5 patients.
We excluded cadaveric studies, biomechanical reports, editorial articles, case reports, literature reviews, surgical technique descriptions, instructional courses, studies comparing different techniques in which isolated particulated cartilage subgroups were not reported independently.
Two independent reviewers (MLO and NLB) performed a review of the abstracts from all identified articles. Full-text articles were obtained for review if necessary, to allow for further assessment of inclusion and exclusion criteria. Additionally, all references from the included studies were reviewed and reconciled to verify that no relevant articles were missing from the review.
Results
Selected In Vitro Studies
In 2000, Qiu
There is substantial evidence suggesting that juvenile cartilage has increased chondrogenic potential. As cartilage ages, an increased calcification of the tissue is seen.
16
In addition, there is a decrease in proteoglycan synthesis and a decreased response to growth factor stimulation with increased age.17,18 Namba
Bonasia
Animal Studies
A comprehensive literature search returned 14
Experimental Studies on Particulated Cartilage. a
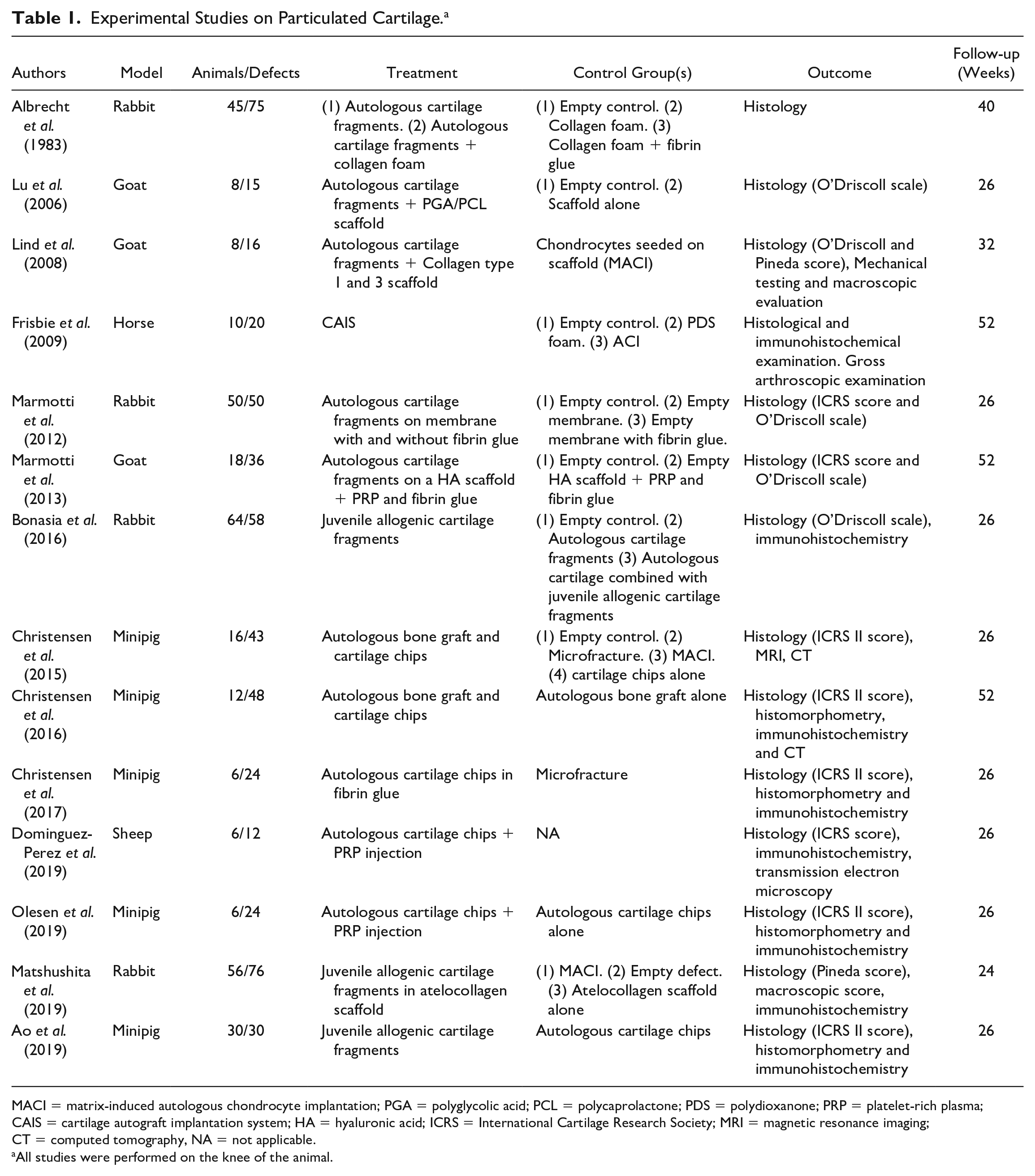
MACI = matrix-induced autologous chondrocyte implantation; PGA = polyglycolic acid; PCL = polycaprolactone; PDS = polydioxanone; PRP = platelet-rich plasma; CAIS = cartilage autograft implantation system; HA = hyaluronic acid; ICRS = International Cartilage Research Society; MRI = magnetic resonance imaging; CT = computed tomography, NA = not applicable.
All studies were performed on the knee of the animal.
In 1983, Albrecht
In 2006, the next landmark study in particulated cartilage was published by Lu
In 2008, Lind
In 2009, Frisbie
In 2012, Marmotti
In 2013, the same research group 27 conducted a similar study in osteochondral defects in goats with three groups investigated: (1) cartilage fragments loaded onto a hyaluronic acid scaffold in combination with platelet-rich fibrin matrix and fibrin glue; (2) hyaluronic acid scaffold, platelet-rich fibrin matrix, and fibrin glue alone; or (3) untreated. Group 1 showed superior outcome both mechanically and histologically with features of hyaline-like cartilage and presence of type II collagen after 12 months.
In 2016, Bonasia
Christensen
In 2019, Dominguez-Perez
In 2019, Olesen
In 2019, Matsushita
In 2019, Ao
Clinical Studies
The literature search returned 16 clinical studies ( Table 2 ) describing 4 different techniques for clinical use:
The CAIS is a minced autologous cartilage embedded in a synthetic scaffold
DeNovo NT Natural Tissue Graft—particulated juvenile articular cartilage
Autologous cartilage chips—with and without concomitant bone grafting
Augmented autologous cartilage chips
Clinical Studies on Particulated Cartilage.
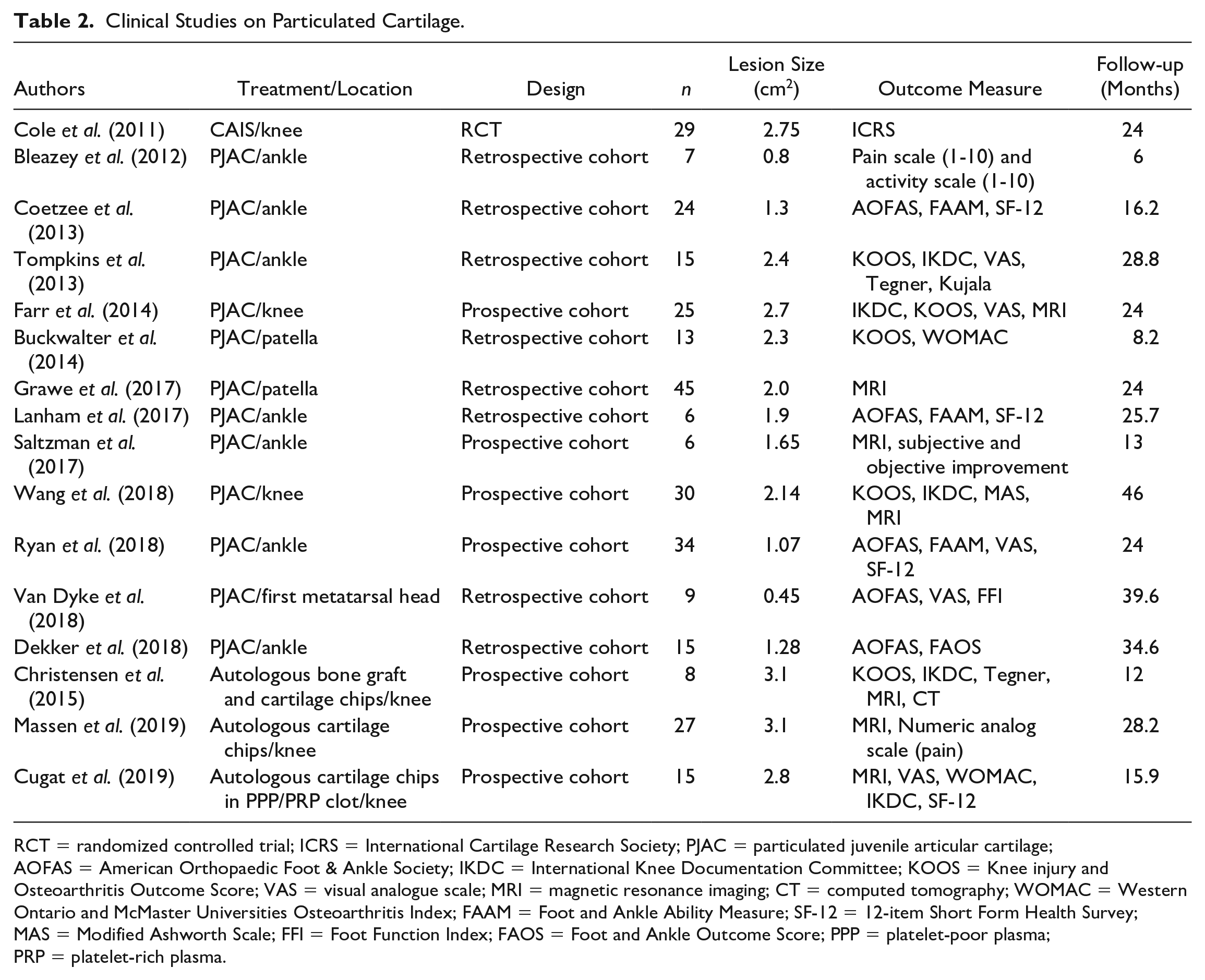
RCT = randomized controlled trial; ICRS = International Cartilage Research Society; PJAC = particulated juvenile articular cartilage; AOFAS = American Orthopaedic Foot & Ankle Society; IKDC = International Knee Documentation Committee; KOOS = Knee injury and Osteoarthritis Outcome Score; VAS = visual analogue scale; MRI = magnetic resonance imaging; CT = computed tomography; WOMAC = Western Ontario and McMaster Universities Osteoarthritis Index; FAAM = Foot and Ankle Ability Measure; SF-12 = 12-item Short Form Health Survey; MAS = Modified Ashworth Scale; FFI = Foot Function Index; FAOS = Foot and Ankle Outcome Score; PPP = platelet-poor plasma; PRP = platelet-rich plasma.
The Cartilage Autograft Implantation System
In the CAIS technique, hyaline cartilage is arthroscopically harvested from a low load-bearing area of the knee. The cartilage biopsy is minced into 1- to 2-mm fragments using a specifically designed device. The device disperses the minced cartilage onto a biodegradable scaffold. The CAIS scaffold is a polymer foam consisting of 35% PCL and 65% PGA, reinforced with a PDS mesh. The cartilage fragments are secured to the scaffold using fibrin glue. Through a mini-arthrotomy, the defect is prepared by creating a clean bone bed with stable cartilage shoulders. The CAIS scaffold, cut to size and loaded with cartilage, is implanted and fixed with biodegradable staples. 25
The study to evaluate the safety of CAIS and to test whether CAIS improves quality of life by using standardized outcomes assessment tools is the only published CAIS study to date and represents the only randomized controlled trial on cartilage fragments. Twenty-nine patients were randomized to treatment with either microfracture or CAIS. SF-36, International Knee Documentation Committee (IKDC), and Knee injury and Osteoarthritis Outcome Score (KOOS) were reported at 6, 12, and 24 months. MRI was performed at baseline, and 6, 12, and 24 months postoperatively. Patient reported outcome measures showed an overall improvement in both groups. The IKDC and KOOS scores showed that improvements were maintained at 24 months. MRI revealed that defects treated with microfracture had higher rate of intralesional osteophyte formation. No differences were found in terms of fill of the graft bed, tissue integration, or presence of subchondral bone cysts. 12 A 300-patient randomized controlled trial comparing CAIS with microfracture was started in 2013. Unfortunately, the company behind the trial withdrew the study sponsorship and the trial was terminated. CAIS is not available for patients at this time.
DeNovo NT Natural Tissue Graft
The commercial allogeneic application of implantation of particulated juvenile cartilage is termed
In 2011, Farr
In 2013, Tompkins
In 2014, Buckwalter
In 2017, Grawe
In 2018, Wang
A number of case series for the application of PJAC in talar osteochondral lesions have been published. In a 2012 study by Bleazey
In 2017, Lanham
In 2018, Dekker
Van Dyke
In 2018, Ryan
Autologous Cartilage Chips
An alternative to the PJAC treatment is ADTT. In ADTT, an osteochondral defect is prepared with a trephine. A bone biopsy is taken from the tibial tuberosity and implanted in the bony part of the defect. A cartilage biopsy is taken from the intercondylar notch, and the cartilage is fragmented using a No. 23 scalpel. The cartilage fragments are implanted into the defect and embedded in fibrin glue.
At this point, 1 short-term clinical study on ADTT has been published. In the 2015 study by Christensen
In 2019, Massen
Augmented Autologous Cartilage Chips
In 2019, Cugat
Discussion
The efficacy of particulated cartilage for treatment of chondral and osteochondral defects have been demonstrated experimentally and clinically. While the initial study dates back to 1983, most studies have been published within the recent 8 years highlighting an increased interest in the technique. The increased interest has likely been motivated by the high cost of cell culturing in and the lack of a gold standard treatment for cartilage lesions.
The repair mechanism involved in cartilage regeneration when using cartilage chips is thought to be by chondrocyte outgrowth from the cartilage fragments, as demonstrated by Lu
Only 2 studies, both experimental, have compared juvenile with autologous (adult) cartilage chips. Bonasia
A similar pattern is seen in a clinical setting. While no clinical studies have compared juvenile cartilage with autologous cartilage, the results are quite comparable. 1 In Figure 1 , the KOOS scores from clinical studies on either juvenile cartilage chips or autologous (adult) cartilage chips have been compared. The limited amount of data does not allow for a statistical comparison, but it becomes apparent that the patient reported outcome is very similar, both preoperative, at 1 year and at 2 years. While juvenile cartilage chips hold a theoretical advantage over adult cartilage chips, further studies are needed to see if the theoretical benefit translates to a clinical setting.
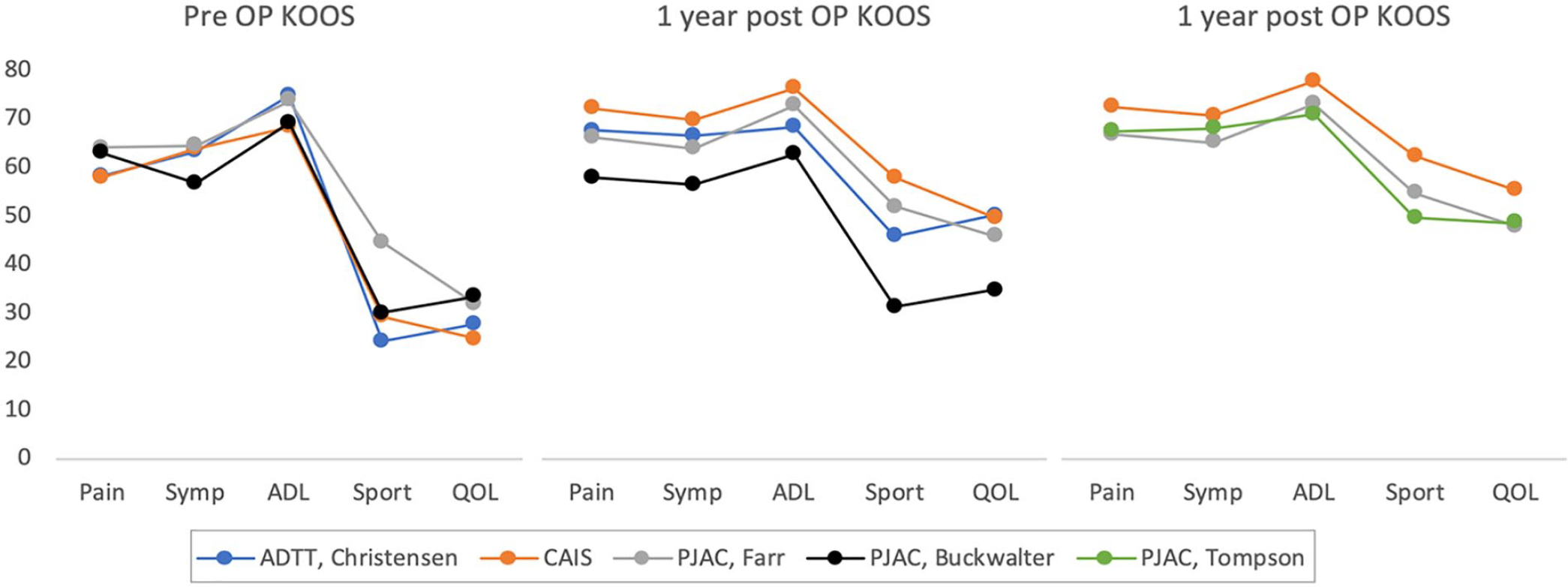
The preoperative, 1-year, and 2-year KOOS scores from 2 studies on autologous cartilage chips (ADTT, Christensen
In general, the results of treatment with particulated cartilage have been encouraging, however poor results and failures have been reported when the treatment is applied to the talus. In the study by Saltzman
An arthroscopic technique for implantation of particulated cartilage has been described. After preparation of the defect, the joint is emptied of fluid. The surgeon can perform the procedure in an empty joint, or by using CO2 arthroscopy. The particulated cartilage is retrogradely loaded into an arthroscopic cannula and delivered to the defect using a trocar. The fibrin glue is injected into the defect filled with particulated cartilage. The arthroscopic technique has been used in talar defects, 56 and application in knee and hip cartilage defects is a possible future augmentation of the treatment.
This is a comprehensive literature review, that covers the subject of particulated cartilage in experimental and clinical studies. Despite the good experimental evidence for the concept of cartilage chip-based treatment, then there is still a lack of high-quality clinical trials to support clinical efficacy and long-term outcome.
Conclusion
Treatment with particulated cartilage, allogeneic or autologous, provides a low cost and effective treatment alternative to microfracture and ACI. Good clinical outcomes are best documented for knee lesion whereas high failure rates have been seen for talar lesions. The perspective of implanting the particulated chips arthroscopically and using particulated cartilage as an adjuvant treatment to other cartilage treatments only broadens the appeal.
Footnotes
Acknowledgments and Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
