Abstract
This review presents the current understanding of the etiology, pathogenesis, and how to diagnose and treat osteochondritis dissecans (OCD) at the elbow joint followed by an analysis of particular characteristics and outcomes of the treatment. OCD is seen in patients with open growth plates (juvenile OCD [JOCD] and in adults [AOCD] with closed growth plates [adult OCD). The etiology at smaller joints remains as unclear as for the knee. Mechanical factors (throwing activities [capitulum] seem to play an important role. Clinical symptoms are unspecific. Thus, imaging techniques are most important for the diagnosis. In low-grade and stable lesions, treatment involves rest and different degrees of immobilization until healing. When surgery is necessary, the procedure depends on the OCD stage and on the state of the cartilage. With intact cartilage, retrograde procedures are favorable while with damaged cartilage, several techniques are used. Techniques such as drilling and microfracturing produce a reparative cartilage while other techniques reconstruct the defect with osteochondral grafts or cell-based procedures such as chondrocyte implantation. There is a tendency toward better results when reconstructive procedures for both the bone and cartilage are used. In addition, comorbidities at the joint have to be treated. Severe grades of osteoarthritis are rare.
Keywords
Introduction
In a recent article on osteochondritis dissecans (OCD), 1 the etiology, pathogenesis, histology, and diagnostics have been thoroughly discussed with a special focus on the knee. A retrospective study 2 showed that the knee joint (61.7%) is the most often involved joint followed by the ankle joint (25%) and the elbow joint (2%-12%). The shoulder (0.6%) and the foot (0.3%) are rarely involved.2,3
In this article, we will focus on OCD in the elbow joint. The most common type of lesion is the capitellar osteochondritis dissecans (OCD), and it is a condition that can be a significant problem in adolescents especially in athletes. The aim of this article is to provide a review of the current literature and present how to best make the diagnosis and the possible available treatment of elbow osteochondritis dissecans with published outcomes.
Etiology and Epidemiology
At the elbow joint, a possible mechanical traumatic or repetitive microtraumatic etiology is proved by the fact that those OCD lesions are usually located at the capitulum humeri, either centrally or laterally and occur in almost all patients predominantly in the dominant arm. Patients are mostly males who indulge in an activity that involves throwing and/or manual work or gymnastics (in females).4-21 Only a few cases are located at the trochlea humeri and are most often seen in combination with a cubitus varus or are rarely located at the radial head probably accompanied with radial head instability.7,16,21
-26 However, Klekamp
Regarding the load transmission, the radio-capitellar joint provides axial stability to the elbow with the capitellum transmitting approximately 60% of compressive forces across the joint.20,21,23,29
There are several biomechanical studies on the elbow joint with data contributing toward a biomechanical etiology of OCD lesions in elbow joints. A study in cadaveric elbows testing biomechanical properties of the radio-capitellar articular surface 30 showed that the medial portions of the radial head are the softest of all tested radio-capitellar segments. The central radial head is significantly stiffer than the lateral capitellum and at the capitellum there is a trend of decreased stiffness from medial to lateral. No significant difference between the stiffness of the radial head sites and the medial capitellum were found. It was supposed that the disparity of the stiffness might be an etiological factor in the development of a capitellar OCD. Another biomechanical study using fresh-frozen cadaveric upper limbs exhibited that valgus torque increases the contact pressure in the radio-capitellar joint. 31 Capitellar osteochondral defects increase elbow valgus laxity and contact pressure without increasing ulnar collateral ligament strain. When valgus torque is applied, contact pressure in the radio-capitellar joint is greater with a lateral than with a central defect. 31 Measurements of the bone density in different parts of the elbow joint assessed by computed tomography osteo-absorptiometry showed that the actual stress across the elbow is concentrated in the posterior part of the trochlea in humans.
Baseball pitching may produce excessive or repetitive stress against not only this part but also the anterior part of the capitellum. The majority of OCD lesions affecting the elbow are found in the anterior part of the capitellum in throwing athletes. 17 The results may support an important role of mechanical conditions in the cause of elbow OCD. 17 Clinically, bone bruises seen at the capitellum may be the precursor of an OCD lesion, for example, at the elbow. 32
Injuries of the ulnar collateral ligament (UCL) seem to play an important etiological factor in the development of elbow OCD.
33
In a radiographic examination
34
using magnetic resonance imaging (MRI) and normal radiographs (anterior-posterior and lateral view) adolescent patients suffering from capitellar OCD lesion (
Regarding radial instability, there are only 2 reports on radial head subluxation or radial head dislocation accompanied with OCD lesions at the capitellum 35 or with a very rare OCD lesion at the radial head. 25 In contrast to these aforementioned biomechanically orientated studies in recent publication no greater analyses on other etiological factors such as genetics, blood supply to the elbow joint, for example, the capitellum for initiation of an OCD in the elbow joint are available.
Regarding the epidemiology of OCD lesions in the elbow joint different statements are made: It is of interest to note that the incidence of such lesions is reported to be high among young baseball players4,11 and the male to female ratio is reported to be 42:4 5 and 35:3 37 . Weiss et al. 2 studied the general incidence of OCD lesions in 317 patients with 334 involved joints. The majority of lesions (61.7%) were seen in the knee, followed by the ankle (25.4%) and the elbow (12%). The percentage of all lesions progressing to surgery was 35.3%; surgical progression for knee, ankle, and elbow joints was 33.5%, 31.8%, and 55.0%, respectively. Patients aged 12 to 19 years had a 7.4 times greater risk of progression to surgery for knee OCD lesions than 6- to 11-year-olds. 2
Diagnostics
Conventional X-rays and MRI are the most important imaging tools also in OCD lesions of the elbow (Fig. 1).1,16,23,24,36,37 There are divergent data regarding the predictive value whether a lesion is a stable one or is unstable, which is important for the decision whether the treatment should be conservatively or surgical. Iwasaki
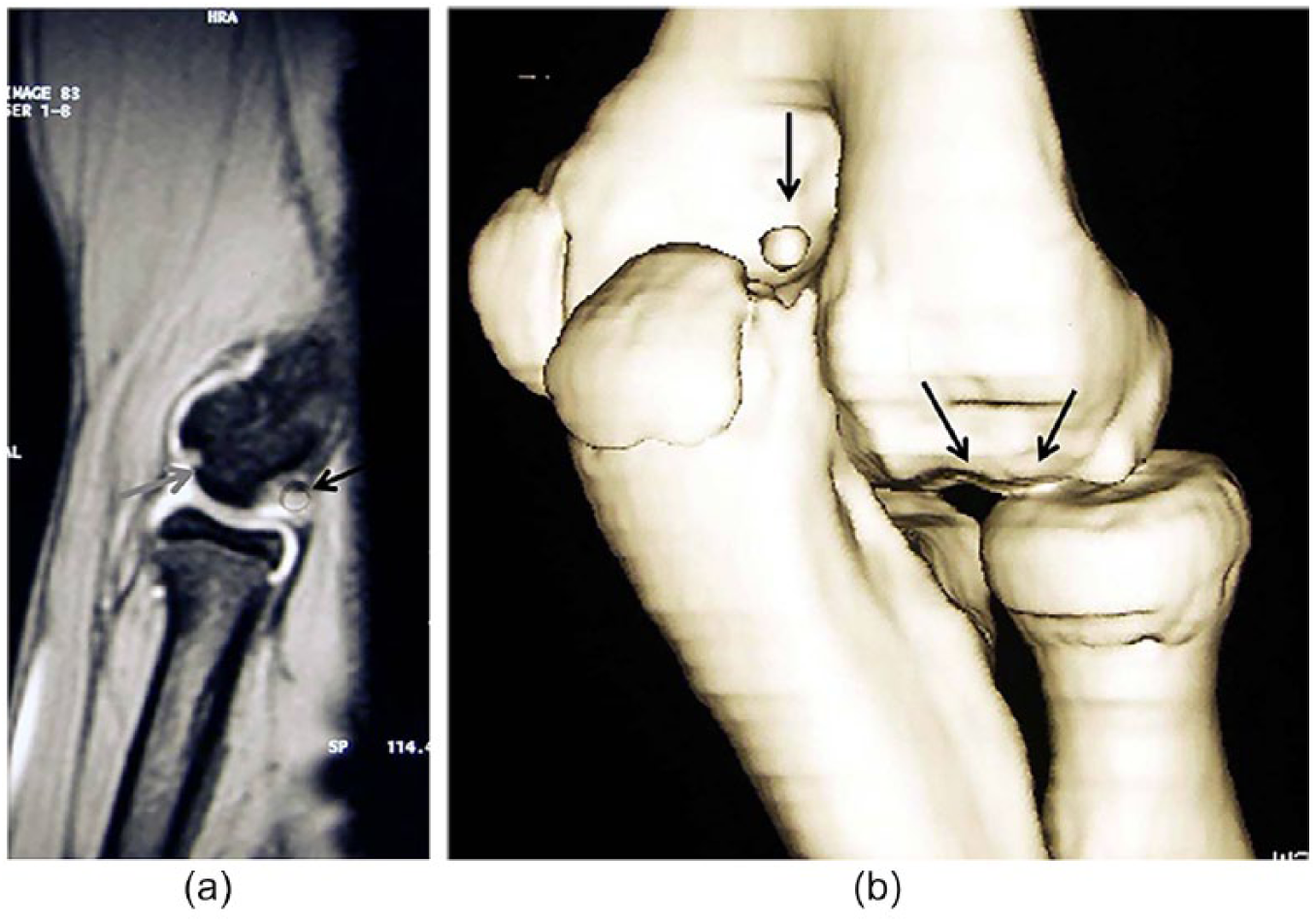
(
Regarding staging or classification of OCD lesions in the elbow joint, several systems have been used ( Table 1 ) . However, there are 3 systems particularly for staging elbow lesion1,36,48,101,102 that are most often used.
Staging systems used for classification/staging of capitellar OCD-lesions.
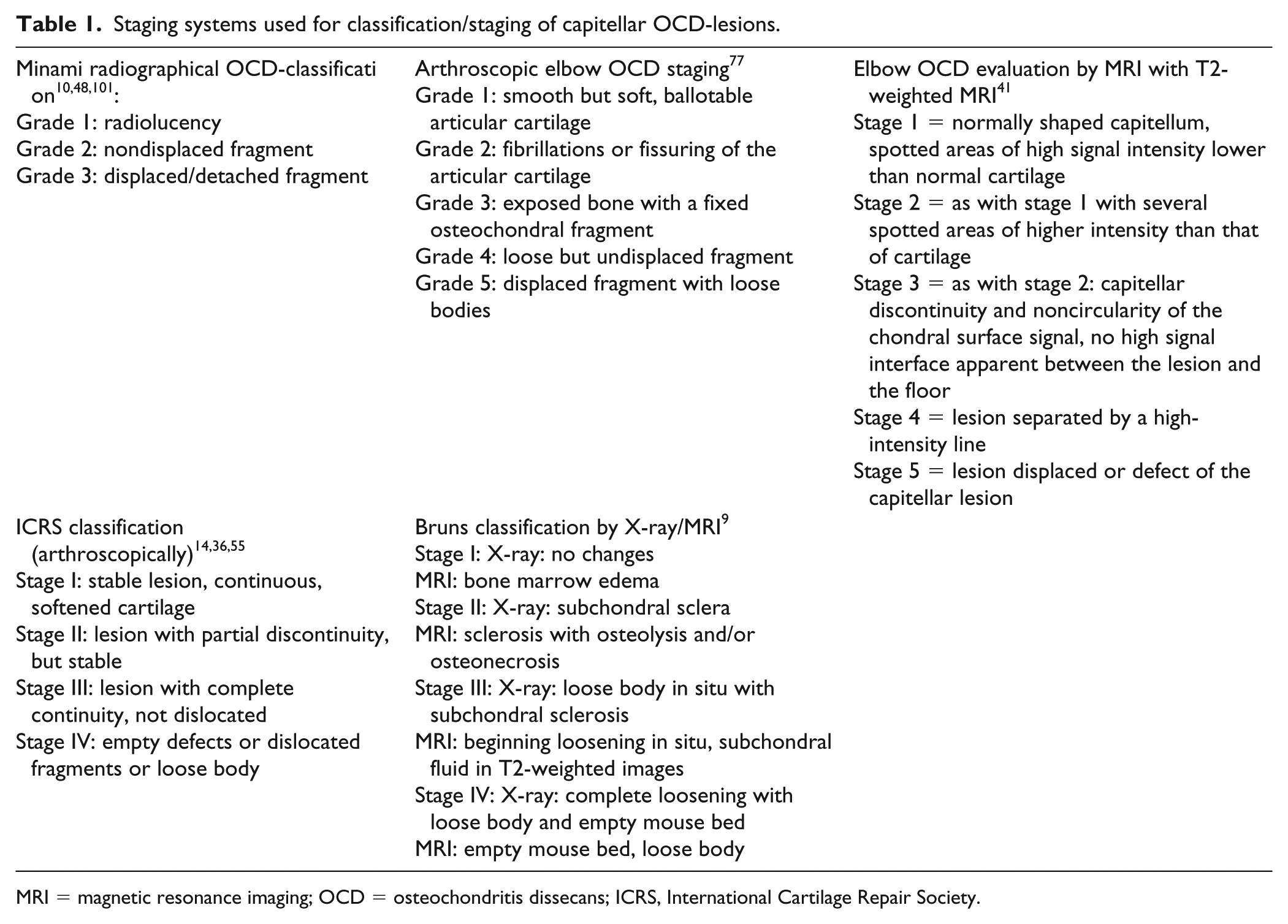
MRI = magnetic resonance imaging; OCD = osteochondritis dissecans; ICRS, International Cartilage Repair Society.
Treatment Options and Results
The general scientific problem as in other OCD lesions such as the knee joint is that no controlled prospective studies exist describing standardized procedures which take into account the stages of the lesions, the stages of the physes or standardized therapeutically regimes.43 -45 Furthermore, the different outcome scoring systems not being consistent makes scientific comparison even more difficult. It has been suggested 46 that only half of all lesions will be symptomatic and that only half of these will need surgical therapy after unsuccessful conservative treatment. In addition, there are no studies existing comparing prospectively different protocols in order to give reliable data for OCD lesion treatments at the elbow joint.
Conservative Treatment
In the past, most of the authors have recommended conservative treatment for stable initial lesions only, particularly in those patients with open physes.6,15,45,47 This treatment should include restriction from sports activities or other physical activities stressing the elbow joint and rest.15,16,23,47
-49 In initial stages with open physes, about 95% of the lesions may heal without surgery,
47
whereas conservative treatment is successful in only 50% of patients who have closed capitellar physes. Mitsunaga
Surgical Treatment
A retrospective analysis exhibited that the elbow is the third often existing OCD lesion besides the knee and ankle joint needing surgery in 31.8% of the patients. 2 There seems to be consensus that advanced lesions, for example, unstable lesions, those with loose bodies or lesions with a fragmented cartilaginous layers or fragmented loose bodies need surgical intervention.20,23,37,53,54 As for other lesions, for example, in the knee joint, 1 several surgical procedures have been advocated even for the elbow joint. Surgical treatment includes different procedures such as:
Arthroscopic removal of loose bodies
Abrasion chondroplasty
Retrograde drilling
Microfracture/nano-drilling
In situ fixation
Autologous chondrocyte implantation (ACI)
Osteochondral autograft transplantation (mosaicplasty and osteochondral transplantation (OAT)
Costal osteochondral transplantation (COT)
The appropriate surgical intervention depends on many factors including lesion size, amount of lateral extension, and the presence of a stable cartilage cap as well as on the patients’ claim.15,16,21,60,62 The scientific problem is that reliable studies comparing different procedures prospectively do not exist. Almost all reports are retrospective level-4 studies.4,15,20,29,37,41,43,60 -68 Furthermore, there are no exact definitions of the different surgical procedures such as debridement and/or chondroplasty versus microfracturing or mosaicplasty versus OAT.4,15,20,29,37,41,43,60 -68 Even when authors had sampled a reasonable number of patients treated differently a comparison has not been done.29,69 Apart from this dilemma, simple surgical procedures can be divided in those with a
minimally invasive character procedures such as drilling either in a retrograde or anterograde manor to perforate the subchondral sclerosis surrounding the lesions, only indicated in stable lesions after a previous unsuccessful conservative therapy. 43
procedures with a rather “palliative” character, for example, simple removal of the loose bodies.15,29,48,69
When the cartilage layer is damaged and it is not possible to refixate the loose body, removal is the simplest procedure, but the lesions remain untreated and are accompanied with worst results.7,70 Thus, removal of loose bodies should at least be combined with bone marrow stimulation procedures such as drilling or microfracturing probably combined with the use of scaffolds in order to improve ingrowth of hyaline-like cartilage known as autologous matrix-induced chondrogenesis (AMIC).
71
Simple excision combined with superficial cartilage shaving does not produce good results, so far comparison is possible to the better results as seen with drilling or curettage.6,9 In addition, a long delay until surgery does not provide satisfactory results.6,9 All these procedures are not capable to restore the osteochondral unit completely because they produce hyaline like repair cartilage with a disorganized collagen fiber orientation being far away from the natural collagen structure known as Benninghoff arcades.15,67,72
-74 Thus, they should be defined as palliative procedure due to the low quality of the regenerated tissue. Nevertheless, there are somehow acceptable short- and medium-term results. The clinical advantage is that these procedures can be done arthroscopically. Bradley and Petrie
46
recommended that the choice of surgical technique should depend on the size of the lesion and integrity of the subchondral bone. They stated that microfracturing alone resurfaces the cartilaginous defects but do not reconstitute the subchondral bone. Even ACI produces only hyaline-like cartilage and there is uncertainty whether the subchondral bone can heal and the osteochondral unit can be reconstructed, even when ACI is combined with cancellous bone transplantation.75,76 In a systematic review on arthroscopic surgery of elbow OCD lesions, de Graaff
In athletes with OCD of the elbow, there was a trend toward better results after OATS or COT and the authors concluded that simple removal should be avoided.
43
However, some authors did recommend simple fragment resection7,70 only for capitellar lesions with a diameter smaller than half of the diameter of radial head. Several authors have combined resection with drilling, curettage, and trimming10,11,16,17,21,22,77,78 and acceptable short-term results have been reported.21,44 Even though Bexkens
In contrast, Mihara
Bone-Peg Grafting and Refixation
While Maruyama
Reconstruction
Only reconstructive techniques such as mosaicplasty14,65,82,83 or OATS67,74,84 are capable of repairing the lesions more or less completely. In principle, and theoretically, only OATS—the osteochondral grafts—are capable of reconstructing the osteochondral unit. With this technique, one may implant the plugs in an overlapping manner,67,74,84 in a mosaic pattern,73,88 or as a single plug
85
and a variant of the technique had been published already in 1964 by Wagner.
1
The cartilage layer of these plugs has the inborn normal architecture of collagen type-II fibrils.72,86,87 Mosaicplasty is a technical variant of the osteochondral transplantation procedure. In contrasts to OAT, in mosaicplasty, plugs are implanted not in an overlapping manner but as a mosaic with remaining clefts between the single plugs.
73
Thus, defects are filled with cartilage covering only 60% to 70% of the defect area.
73
The remaining gaps between the single plugs will be filled up spontaneously with fibrous tissue in growing from the subchondral bone only after transplantation.67,73,74,84 This might have an influence on the quality of the reconstruction and thus on the grafts stability and on the resulting clinical outcome.67,73,74,84 This particular technique had been introduced and studied by Hangody
Regarding the fit of osteochondral transplants harvested from the knee joint and transplanted into the capitellum there are at least 2 interesting articles.89,90 Mapping of the cartilage depths at the recipient site at the capitellum and the donor site (knee joint) by means of MRI in both sites exhibited that best match for capitellar reconstruction is with the posterior aspect of the medial condyle and the distal-most aspect of the anterior-lateral femoral condyle. 89 A topographic analysis on the congruence of the capitellum and distal femur using computed tomography scans showed that there is a less than 0.1-mm difference in the topographic articular surface match among the 4 commonly used donor sites of the distal femur and the capitellum. The findings suggest that all 4 donor sites provide close articular matching for the capitellum articular surface, with the lateral trochlea articular surface providing the best match. 90
The COT procedure is using osteochondral plugs harvested from ribs.55,61,79 In comparison with osteochondral articular grafts, these transplants have a completely different structure of the cartilage and lacks the typical osteochondral transition. 91 Nevertheless, based on their convincing mid-term results of between 25 and 45 months postoperatively, several authors recommend that reconstructive techniques, such as mosaicplasty,14,65,82,83 OAT,13,20,56,58,67,74,84,92 or COT grafting harvested from ribs55,61,79 could be used since they are more successful than nonreconstructive procedures, at least for larger lesions (>50% of the capitellar size) or those involving the lateral capitellar margin.11,27,55,56,79 For all reconstructive techniques it seems to be of importance that the lateral capitellar rim is reconstructed to achieve optimal results.92 -94
Osteochondral Autograft Transplantation
Transplanting osteochondral grafts in an overlapping manner is suggested to result in a more stable reconstruction.
73
To our knowledge, Shimada
A survey of the literature on the significance of lesion location of capitellar OCD lesions showed, regardless of the location, that after OAT in 87% of lateral lesions and 91% of central lesions excellent or good results were found.
93
In addition, there was a trend toward better results after a more aggressive reconstructive surgery of lateral lesions particularly for those including the lateral capitellar rim. Furthermore, the authors found that the failure rate of nonreconstructive procedures was significant for lateral lesions and that one study reported a failure rate of 44% for bone peg grafting.
93
Matsuura
Kirsch
There are at least 6 more reports on the OAT procedure used for treatment of OCD lesions in the elbow joint.20,67,74,84,85 All these studies confirmed the good to excellent results in almost all patients with an excellent and almost complete integration of the grafts with a minimum of osteoarthritic changes. Another report included at least a rather large number of patients treated with OATS but did not compare the results of 19 patients to other techniques that have been included in the report. In addition, it is unclear whether they performed a mosaicplasty or OAT procedure.
20
Most recently, Bae
Costal Osteochondral Graft Transplantation
There are only 3 reports on the use of COT.55,61,79 Mihara
Mosaicplasty
Iwasaki
Allograft Transplantation
Mirzayan and Jim 63 are the first and still the only group found to report on the use of allografts to repair advanced capitellar OCD lesions. All 9 basketball players who had been treated with fresh femoral allografts returned to throwing and were still active in their sport or played at least 2 years of baseball before leaving the sport unrelated to the elbow problems. 63
Autologous Chondrocyte Implantation
As for allografts also for ACI very little is known on its use in the treatment of OCD lesions in the elbow joint. Only 2 articles have been found related to cell transplants for elbow OCD. Sato
Additional and Preventive Procedures
It is important to treat additional comorbidities that might be responsible for the initiation of the OCD lesions and to avoid recurrences. But little is known about these potentially causative conditions. Kiyoshige
Long-Term Results
Little is known about long-term results on the different elbow OCD treatment conditions. No studies exist comparing different therapeutic regimens in a long-term follow-up. Takahara
Similar results after arthroscopic debridement or removal had been published by Brownlow
Conclusion
The natural history of OCD of the elbow is not well-known. But it is obvious that mechanical stress at the elbow, for example, the capitellum, is supposed to be the most important etiological factor because of the fact that almost all of the patients are involved in sports activities that are stressing the elbow joint.
Conservative treatment seems to be successful only in initial early lesions without damage or loosening of the cartilage layer in young patients with still open physes. Thus, in many patients, conservative therapies seem reasonable if the growth plates are still open.
The best therapy for elbow OCD patients may be early diagnosis and prevention by avoidance of the heavy joint disturbing activities. Nevertheless, there is a large group still suffering from different symptoms after such a nonsurgical therapy. Although there are a numerous articles reporting on different surgical procedures mentioned above, there is no reliable prospective study comparing these surgical treatment options in a prospective and randomized manner. However, it seems clear based on existing reports that it is not an advisable procedure to simply remove loose bodies and debride the ground base of the lesion. Furthermore, bone-marrow stimulating procedures are not capable of restoring the damaged osteochondral area, but they still are those techniques that are performed most often but with suboptimal results.18,37
Instead a clear trend toward better results is seen after refixation of fragments as well as after any reconstructive procedure, for example, OAT, mosaicplasty, or COT.20,43 Especially for a return to sport, the use of osteochondral autografts seems recommended.
99
The reports on OAT experiences with a long-term follow-up are in our opinion convincing.67,84 The arthroscopic techniques may be tempting to use but still there is a need of more evidence to determine the superiority of the open versus arthroscopic techniques in treating elbow OCD. Thus, the question should not be whether it can be done arthroscopically or is to be done open with arthrotomy; instead the question should be which technique is the best one to reconstruct the capitulum with long-term durability.
7
Westermann
Based on the findings of this review, refixation of fragment could give symptom relief in capitellar OCDs but only the osteochondral autografting techniques restore the very important osteochondral unit with the transition between cartilage and subchondral area. We believe that guidelines can contribute to the choice of treatment in OCD of the elbow but should be based on methodologic well-designed research. In the treatment of capitellar OCD most techniques cannot restore the hyaline cartilage; the exception is the osteochondral autografting technique.
Footnotes
Author’s note
Mathias Werner is now affiliated with Vivantes Klinikum Friedrichshain, Dept of Osteopathology, Berlin, Germany.
Acknowledgments and Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
