Abstract
Objective:
Autologous matrix-induced chondrogenesis (AMIC) is a 1-step cartilage restoration technique that combines microfracture with the use of an exogenous scaffold. This matrix covers and mechanically stabilizes the clot. There have been an increasing number of studies performed related to the AMIC technique and an update of its use and results is warranted.
Design and methods:
Using the PubMed database, a literature search was performed using the terms “AMIC” or “Autologous Matrix Induced Chondrogenesis.” A total of 19 basic science and clinical articles were identified.
Results:
Ten studies that were published on the use of AMIC for knee chondral defects were identified and the results of 219 patients were analyzed. The improvements in Knee Injury and Osteoarthritis Outcome Score, International Knee Documentation Committee Subjective, Lysholm and Tegner scores at 2 years were comparable to the published results from autologous chondrocyte implantation (ACI) and matrix ACI techniques for cartilage repair.
Conclusions:
Our systematic review of the current state of the AMIC technique suggests that it is a promising 1-stage cartilage repair technique. The short-term clinical outcomes and magnetic resonance imaging results are comparable to other cell-based methods. Further studies with AMIC in randomized studies versus other repair techniques such as ACI are needed in the future.
Introduction
Marrow stimulating techniques have been used to treat cartilage defects since 1959 when Pridie
1
introduced subchondral drilling. Steadman
The limitation for marrow stimulation techniques is that the bone marrow stem cells and growth factors are released into the joint rather than being contained at the site of the defect. It is also suggested that the newly formed clot is not mechanically stable to withstand tangential forces. 5
Some authors have modified the traditional marrow stimulating techniques to enhance its efficacy; by combining it with an intraarticular injection of platelet-rich plasma (PRP) or
Autologous matrix-induced chondrogenesis (AMIC) is a novel technique of cartilage restoration. It is a one-step procedure that combines microfracture with the fixation of a biological scaffold, such as a porcine collagen matrix. This matrix covers the blood clot, permitting the ingrowing of MSCs to differentiate into the chondrogenic lineage. The matrix acts as a temporary structure to allow the cells to be seeded and establish a 3-dimensional structure.
Over the past few years, there has been an increasing number of reports of AMIC-like techniques used for cartilage resurfacing in the knee and ankle joint.10,11 There has also been a variation in the surgical techniques, the type of matrix used, and the addition of supplementary growth factors and exogenous cell transplant. Thus, it is necessary to discuss the differences in these variants in AMIC techniques.
Our aim is to review the basic science rationale, the various techniques and results of AMIC for knee cartilage repair. We also hope that this can be a basis for standardization during reporting of surgical techniques and comparing outcomes of AMIC in future.
Methods
Using the PubMed database a literature search was performed using the terms “AMIC” or “Autologous Matrix Induced Chondrogenesis.” A total of 11 publications published in English were identified with this initial search.10,12-20 Following this, the summary and references of each publication were reviewed to identify other relevant studies. Another 8 studies were identified and included in this review.21-28
In total, we identified 4 technical notes explaining AMIC surgical techniques,10,12,15,19 10 outcome reports of the AMIC technique for chondral defects in the knee5,13,14,17,18,23,24,26-28 and 5 basic science studies on the AMIC technique16,29-31,34 The full text of these publications were reviewed and summarized by the primary author for this review.
Basic Science Rationale
Gille
Tallheden
Knee surgeons have made use of different scaffolds for the AMIC technique in cartilage repair. The ideal scaffold should mimic biology, architecture, and structural properties of the native tissue, facilitating cell infiltration, attachment, proliferation, and differentiation. It should first support tissue formation and then gradually be replaced by the regenerating tissue with no harmful breakdown products released.
There are different types of scaffolds available: natural protein–based or carbohydrate-based scaffolds, and synthetic scaffolds. The 3 scaffolds that have been reported in the literature for AMIC are ChondroGide (Geistlich Biomaterials, Wolhausen, Switzerland), Hyalofast (Fidia Advanced Biopolymers, Padua, Italy), and Chondrotissue (BioTissue, Zurich, Switzerland). There are other commercially available collagen and alginate scaffolds that have been used for cartilage repairs that are reported in the literature.32,33
ChondroGide (Geistlich Biomaterials, Switzerland)
The porcine-derived type I/III collagen membrane ChondroGide is the commonest type of matrix used. This is a protein-based natural bilayer collagen matrix that exists as a porous cell adhesive and a smooth cell occlusive layer.
The cell adhesive layer ensures that the MSCs are attached to the collagen fibers for the proliferation of stem cells and the differentiation into chondrocytes. The second cell occlusive nonporous layer of ChondroGide makes sure that the super clot remains in the defect.
Gille
Breinan
Gigante
Chondrotissue (BioTissue, Switzerland)
Chondrotissue is an absorbable polyglycolic acid (PGA) textile treated with hyaluronan. 31 In AMIC, the Chondrotissue scaffold acts as a sponge which holds the clot and MSCs within the defect. 31
This hypothesis was reinforced by the work of Erggelet
Hyalofast (Fidia Advanced Biopolymers, Italy)
Hyalofast is made from semisynthetic derivative of hyaluronic acid. Hyaluronic acid has been shown to induce MSCs from the bone marrow to differentiate along the chondrogenic lineage.9,35
Hyalofast is nonwoven, porous, 3-dimensional structure consisting of 10- to 15-µm thick fibers. The interstices of variable sizes allow cell contact, cluster formation, and extracellular matrix deposition.
36
It also helps entrap the MSCs. It is resorbed following the breakdown pathway of endogenous hyaluronic acid. Buda
Surgical Technique
The original AMIC technique was described by Benthien and Behrens10,12 and performed via an arthrotomy. The surgery begins with an arthroscopy to verify the size and location of the defect. Their indications for AMIC are symptomatic full thickness chondral or osteochondral lesions that do not exceed 1.5 cm2. For osteochondral lesions, they recommend harvesting the cancellous bone from the proximal tibia and impacted into the defect before the scaffold is attached on the defect.
After an assessment of the defect, the chondral lesion is debrided till a stable shoulder surrounds the cartilage defect (Figure 1). Microfracture was performed in the original technique using microfracture awls. 12 Other authors describe subchondral drilling using 1.1 mm K-wires where multiple holes are drilled at 5-mm intervals 37 (Figure 2).
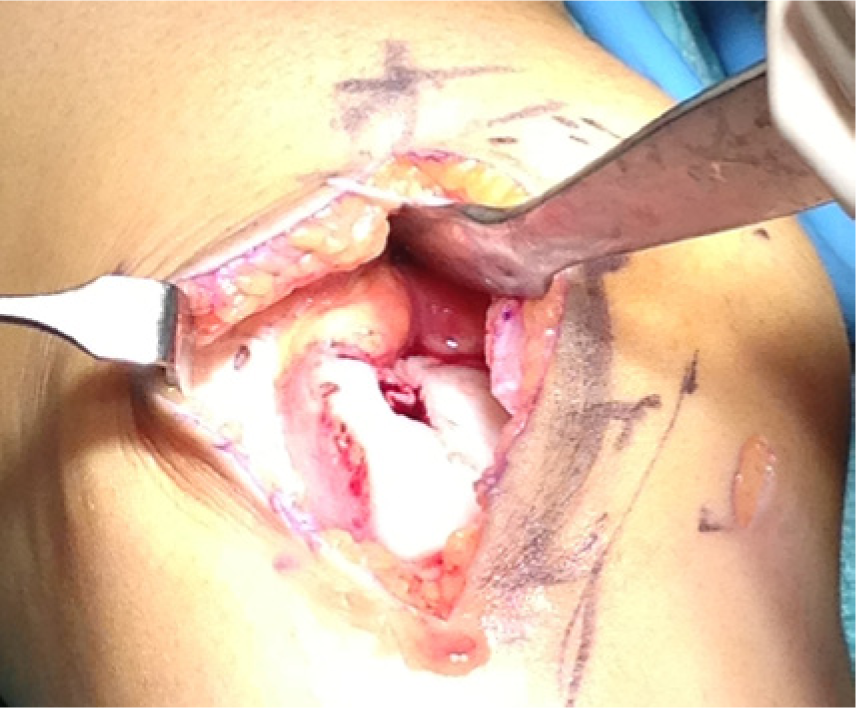
Preparation of the defect with stable shoulders around the defect.
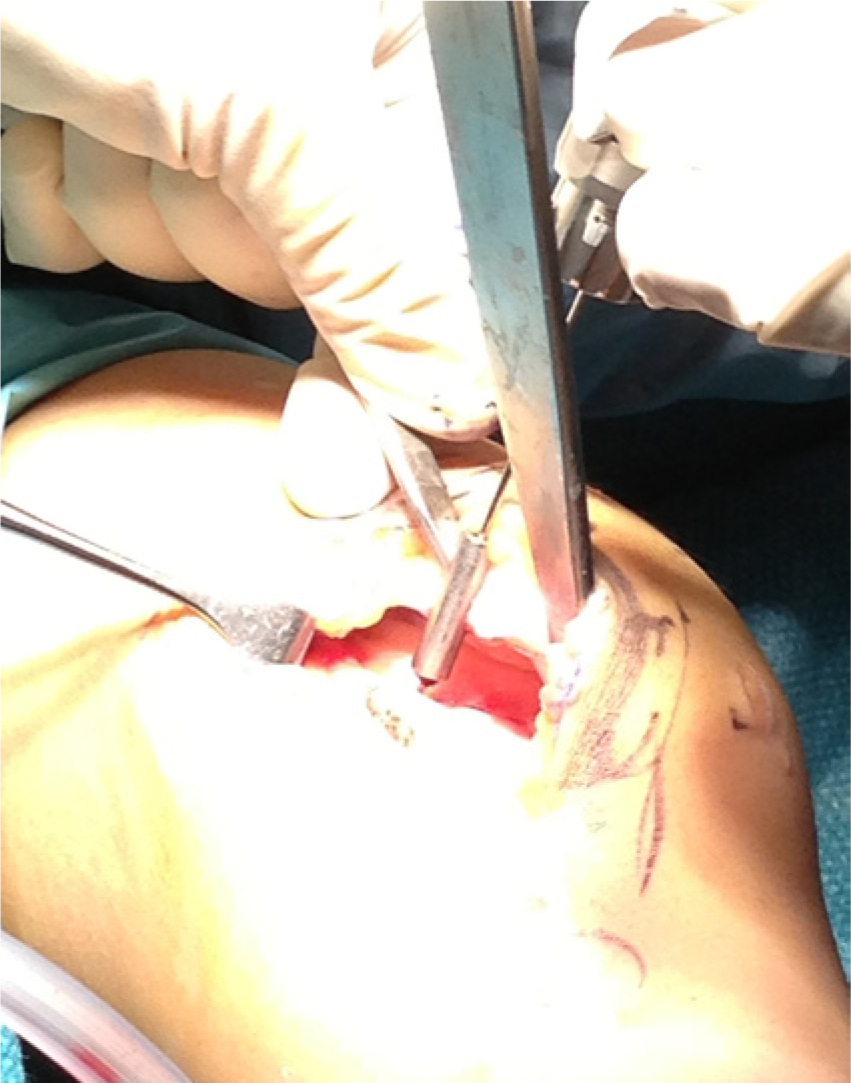
Subchondral drilling with K-wires.
The matrix is trimmed to the size of the defect. Most authors use a size that is slightly smaller than the actual lesion and others make multiple patches to cover the defect. If multiple patches are used, the patches are overlapped over each other. The ChondroGide matrix is moistened with physiological saline, and the Chondrotissue matrix is immersed in autologous serum10,19 (Figure 3).
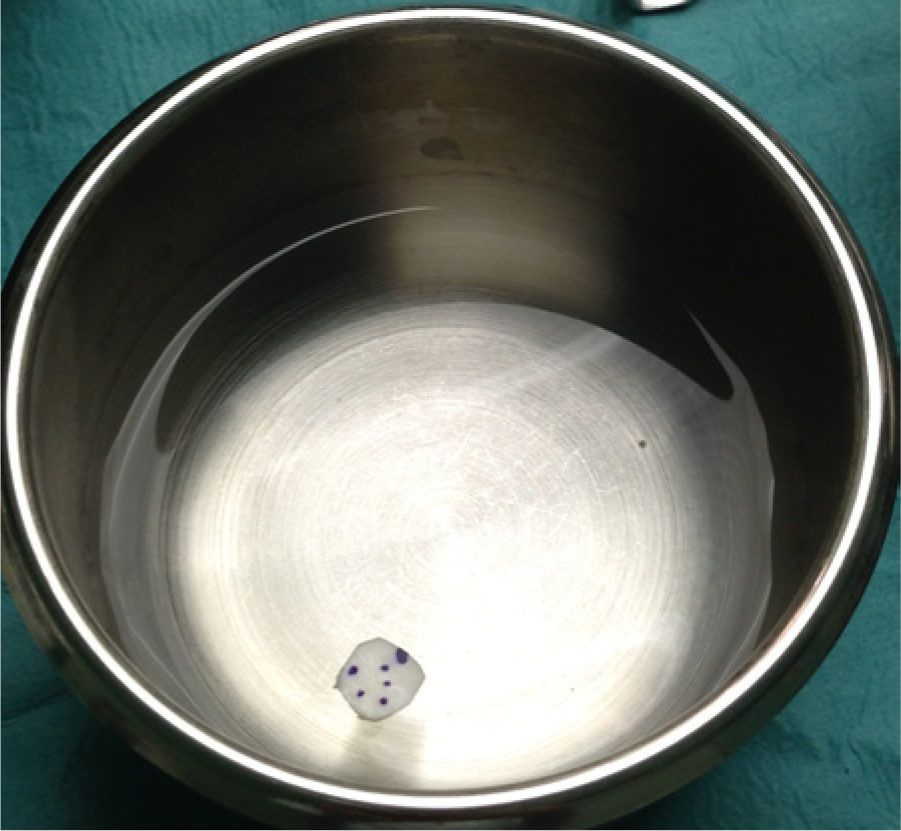
Preparing the ChondroGide matrix prior to implantation. Note the dots placed on the surface to indicate the nonporous side (ie, the side not on bone).
The bilayer ChondroGide matrix is placed in the defect with the porous surface of the membrane (rough) is facing the bone surface. Fibrin glue (Tissucol, Baxter, Warsaw, Poland) is applied over the membrane-covered areas and left for 5 minutes to set10,12 (Figures 4 and 5). The knee is then brought through a series of flexion and extension movements to check the stability of matrix in the defect before wound closure.
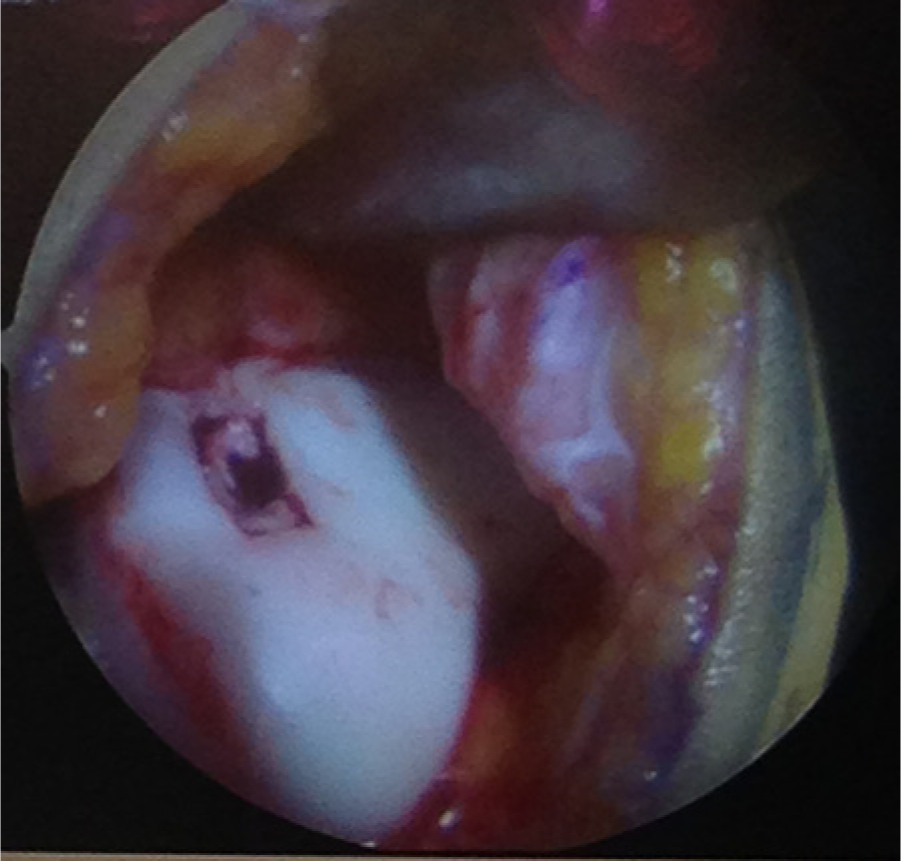
Defect covered with the ChondroGide matrix.
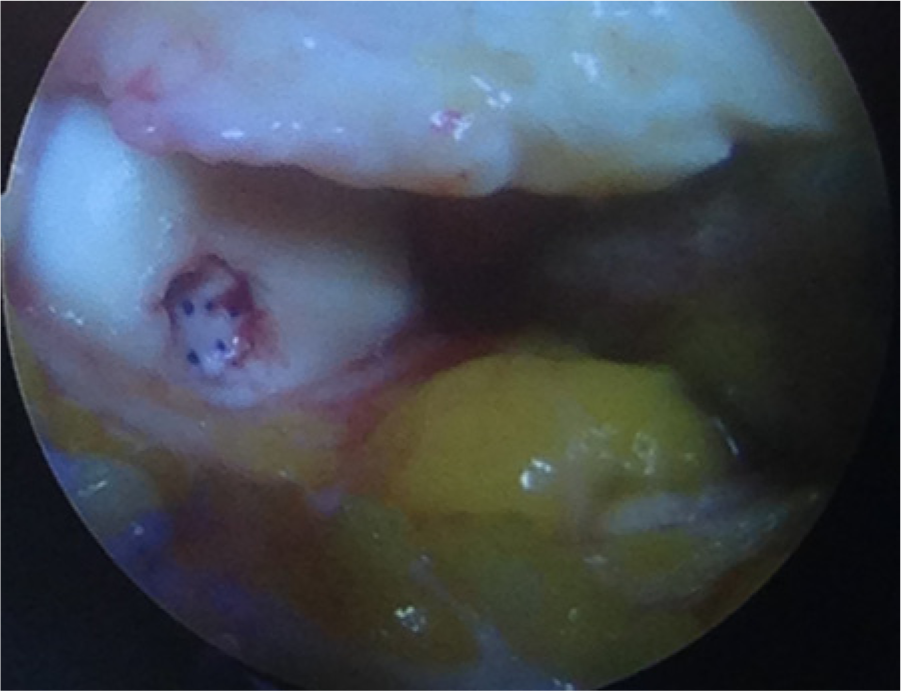
Femoral condyle defect with a ChondroGide matrix.
Some authors have reported the use of sutures to prevent matrix from being dislodged. 14 However, Hunziker and Stähli 38 in their studies have suggested that suturing of the articular cartilage can induce local damage, with histology changes seen that are similar to the early osteoarthritis.
The mechanical stability of some scaffolds, such as Chondrotissue allows ease of handling and secure fixation with resorbable pins.
30
Zantop
For the authors who use Hyalofast for AMIC, their technique is often supplemented with bone marrow–derived MSCs and PRP.27,28 They harvest 60 mL of bone marrow aspirate from the posterior iliac crest and this is processed with a cell separator to obtain 6 mL of bone marrow–derived MSCs. Together with PRP centrifuged from the patients’ blood, these MSCs and growth factors are delivered onto the Hyalofast matrix and inserted into the defect.
Piontek
In the postoperative phase, some authors recommend knee immobilization for a period of time.
17
In addition, other authors limit the knee to non-weightbearing for between 2 and 6 weeks13,14,17,24,26-28 and Kusano
Clinical Results
Ten studies that were published on the use of AMIC for knee chondral defects and the results of 219 patients are summarized in Table 1.5,13,14,17,18,23,24,26-28 The first 6 reviewed studies made use of ChondroGide as the matrix.5,13,17,18,23,26
Summary of Clinical Studies on AMIC for knee chondral defects.
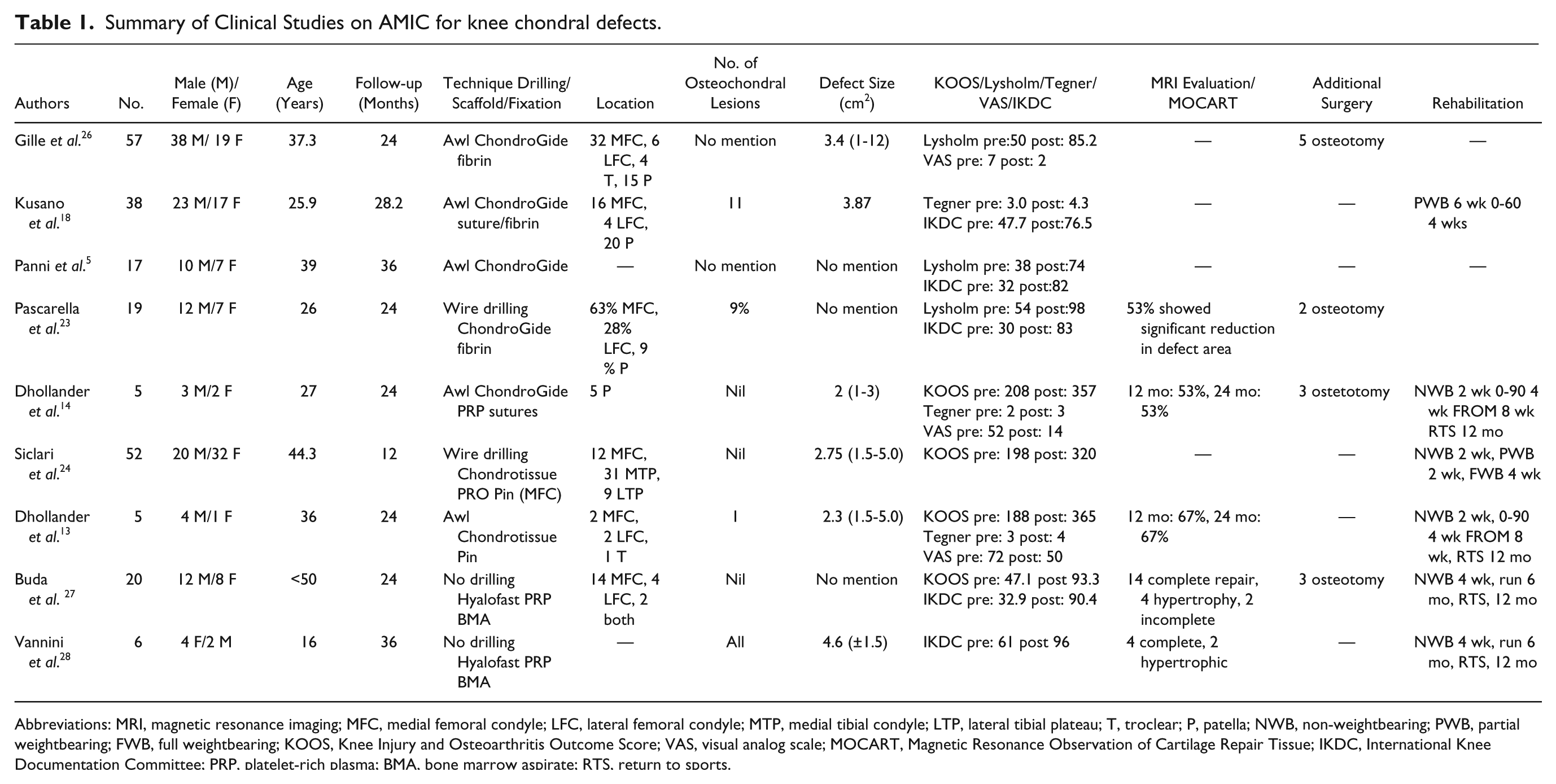
Abbreviations: MRI, magnetic resonance imaging; MFC, medial femoral condyle; LFC, lateral femoral condyle; MTP, medial tibial condyle; LTP, lateral tibial plateau; T, troclear; P, patella; NWB, non-weightbearing; PWB, partial weightbearing; FWB, full weightbearing; KOOS, Knee Injury and Osteoarthritis Outcome Score; VAS, visual analog scale; MOCART, Magnetic Resonance Observation of Cartilage Repair Tissue; IKDC, International Knee Documentation Committee; PRP, platelet-rich plasma; BMA, bone marrow aspirate; RTS, return to sports.
In 2010, Gille
Gille
Kusano
Panni
Pascarella
Siclari
Dhollander
Using the Hyalofast matrix, Buda
Discussion
Knutsen
The initial results of ACI by Peterson
These encouraging outcome results and the concept of a single-stage cartilage resurfacing technique are attractive for many sports surgeons. However, there are many factors from a basic science standpoint that are not completely understood in AMIC.
The cartilage repair from AMIC is postulated to be from MSC chondrogenesis. De Girolamo
In ACI, the chondrocyte density required for treatment is 106 cells per cm2. 46 The cell density required for chondrogenesis from MSC is thought to be higher than ACI.30,40, 46 These studies highlight the benefit of using a matrix to concentrate the MSCs within the defect in the AMIC technique.
Using a rabbit model comparing microfracture awls versus subchondral drilling, Chen
The ideal scaffold for cartilage resurfacing is still a matter of debate. When we look at the outcome studies of these 3 matrices: ChondroGuide, Chondrotissue, and Hyalofast, they all have comparable clinical results as well as follow-up MRI. However, the ChondroGide matrix is more well studied and has the most published literature when compared with the other 2 matrices.
From the basic science perspective, various authors suggest that hyaluronic acid–enriched microenvironment seems to induce chondrogenesis.49,50 Wu
However, Welsch
There has been a trend toward the use of PRP and MSC to supplement the AMIC technique. This has led to some confusion as these were called AMIC plus techniques. PRP has shown to stimulate cartilage repair after microfracture in a sheep model. 51
In their rabbit animal model, Qi
From our review, we find that there is a need to standardize reporting of the AMIC technique. This will enable future comparison to determine the efficacy of these techniques and determine if various technical variations can potentially affect outcomes. The technical factors that should be reported are
arthroscopic or open surgery
method of subchondral drilling or microfracture
type of matrix or scaffold used
matrix is seeded with PRP or bone marrow stem cells
fixation of the matrix or scaffold
postoperative rehabilitation program
In addition, we suggest that the outcome measures should be standardized. The commonest outcome instruments are the KOOS, Lysholm, Tegner, and IKDC scoring. We suggest that these 4 instruments should be used in all studies at a minimum at 1 year and 2 years to allow comparison.
Most studies use the MRI protocol for cartilage assessment such as the modified MOCART score by by Marlovits
The key limitation for AMIC is its use in larger defects. Minas
Conclusion
Our review of the current state of the AMIC technique suggests that this is a promising cartilage resurfacing technique. The outcome scores and MRI results are comparable to other cell-based cartilage methods. It should be pointed out that we still lack understanding on the ideal conditions for chondrogenesis.
Footnotes
Acknowledgment and Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
This study was approved by our institutional review board.
