Abstract
Purpose
To evaluate autologous matrix-induced chondrogenesis (AMIC) for isolated focal retropatellar cartilage lesions and the influence of patellofemoral (PF) anatomy on clinical outcomes at a minimum of 2-year follow-up.
Methods
Twenty-nine consecutive patients (31 knees) who underwent retropatellar AMIC with a mean age of 27.9 ± 11.0 years were evaluated at a follow-up averaging 4.1 ± 1.9 years (range, 2-8 years). Patient factors, lesion morphology, and patient-reported outcome measures, including Knee Injury and Osteoarthritis Outcome Score (KOOS), Tegner, Kujula score, and visual analogue scale (VAS) score were collected. PF anatomy was assessed on pre- and postoperative imaging, and subsequently correlated to outcome scores and failure to determine risk factors for poor outcome.
Results
At final follow-up, the AMIC graft failed in 4 cases (12.9%) at a mean follow-up of 21 ± 14.1 months. Patients with failed grafts had a significantly smaller patellar and Laurins’s PF angle than patients whose graft did not fail (
Conclusion
AMIC for retropatellar cartilage lesions in combination with concomitant corrective surgery for patellar instability results in low failure rate with satisfactory clinical outcome and patient satisfaction of almost 80% at mid-term follow-up. As most failures occurred in patients without concurrent tibial tubercle osteotomy and both a smaller patellar and Laurins’s PF angle were associated with less favorable outcome, this study supports the growing evidence for the need of unloading retropatellar cartilage repair, when indicated.
Level of Evidence
Case series; level of evidence, 4.
Keywords
Introduction
Articular cartilage lesions of the knee are commonly found on magnetic resonance imaging (MRI) and reported in up to 2/3 of all knee arthroscopies.1,2 One-third of the lesions are located in the patellofemoral (PF) joint and are associated with pain, disability and can eventually progress to osteoarthritis.3,4 The pathomechanism of PF cartilage lesions is multifactorial, including direct trauma, PF dislocation, instability, and maltracking.5,6
Treating retropatellar chondral defects is particularly challenging due to the complex biomechanical circumstances with high loading stress on its surface. 7 Associated patho-anatomical morphologies are known causes for cartilage lesions and thus have to be addressed during treatment.5,8,9 Consequently, determining lesion etiology is crucial to define and initiate an individual treatment plan.
Various options exist for the treatment of focal cartilage lesions of the knee. 10 Primary treatment consists of nonoperative management with nonsteroidal anti-inflammatory medications, intra-articular corticosteroid injections, hyaluronic acid viscosupplementation, and physiotherapeutic strengthening and stretching of the thigh muscles.7,11 If symptoms persist, surgical therapy may be considered. Hence, various surgical techniques are available, but the optimal treatment remains controversial.12-19
A treatment option for contained retropatellar full-thickness cartilage lesions is autologous matrix-induced chondrogenesis (AMIC). The technique combines bone marrow stimulation of microfracturing and the augmentation of a collagen type I/III bilayer membrane to contain the subchondral bleeding and provide a matrix for repair tissue maturation. It has been shown effective for the treatment of cartilage lesions in the knee joint.20-22 However, results of AMIC for retropatellar cartilage lesions are only reported in small case series or are embedded in studies investigating AMIC for tibio- and patellofemoral lesions missing thorough subanalysis.23-27 Furthermore, evidence of factors influencing the outcome after retropatellar AMIC is lacking, especially the effect of recently determined risk factors for PF cartilage lesions, including trochlear dysplasia, patella alta, and excessive lateral tilt remains unknown. 9
The purpose of this study was therefore to report the clinical outcome of AMIC for isolated focal retropatellar cartilage lesions and to evaluate the influence of PF anatomy. It was hypothesized that AMIC would generally result in favorable mid-term clinical outcomes, yet individual PF anatomy significantly affects patient outcome.
Materials and Methods
Ethical approval (No. 2020-01052) was granted by the local research ethics committee and all included patients gave their written consent.
Patients
A total of 36 consecutive patients (38 knees) underwent retropatellar cartilage repair with AMIC for isolated focal full-thickness chondral lesions (Outerbridge type III and IV) of the patella at our institution between August 2013 and June 2018. 28 The treatment with AMIC was indicated in patients with (1) symptomatic contained retropatellar cartilage lesion with fissuring to the level of subchondral bone and (2) failed conservative management which was initiated for a minimum of 3 to 6 months ( Fig. 1 ). Exclusion criteria comprised advanced osteoarthritis, inflammatory joint diseases, and infection. To minimize confounding, 2 patients with concomitant high tibial and distal femur osteotomies were excluded from the study. A total of 5 patients (5 knees, 14%) were not available for follow-up; Three refused to participate and 2 could not be traced. According to telephone or chart review, none of the 5 patients had undergone revision surgery. Thus, this study included 29 patients (31 knees) that received retropatellar AMIC with a minimum follow-up of 2 years.
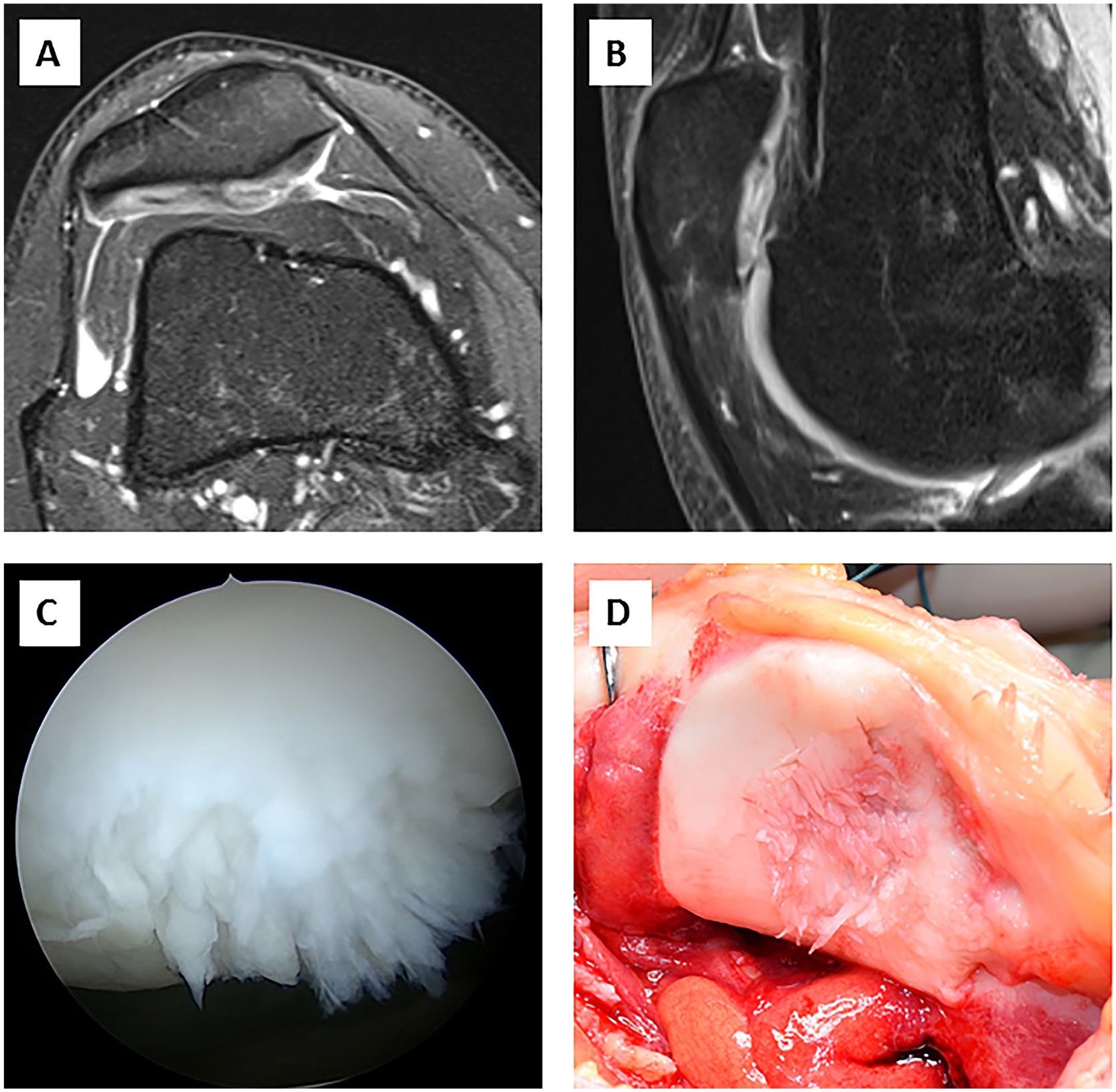
(
Clinical and Radiographic Assessment
Clinical notes and operative reports were reviewed to determine patient’s age at the time of surgery, sex, body mass index (BMI), smoking status, previous surgery, concomitant surgical procedures, defect size, location, lesion location type according to Fulkerson, 29 etiology, complications, and reoperations.
Patients were contacted and asked for any complications or reoperations since the initial procedure. Clinical outcomes were evaluated using patient-reported outcome measures (PROMs), including Tegner activity score, 30 Knee Injury and Osteoarthritis Outcome Score (KOOS) with its subscales, 31 Kujula score, 32 and visual analogue scale (VAS) pain score. 33 Patients rated their overall postoperative outcome as “excellent,” “good,” “fair,” or “unsatisfactory.”
Radiographic analysis on preoperative MRI, radiograph, and orthoradiogram in all patients consisted of assessment of tibial tubercle trochlear groove (TTTG) distance, 34 Caton-Deschamps index (CDI), 35 Laurins’s PF angle, 36 trochlear sulcus angle, 37 Merchants’s congruence angle, 38 sulcus depth, 39 patellar angle, 40 PF index, 41 patella morphology according to Wiberg, 42 and degree of trochlea dysplasia according to Dejour.43,44 Postoperative radiographic analysis was based on standard radiograph of the knee in all patients and MRI if available.
All images were analyzed by two independent observers (M.W. ad C.S). In the event of disagreement, a third observer (J.A.) assessed the images to achieve consensus.
Surgical Technique and Postoperative Care
All patients’ cartilage lesions were accessed via arthrotomy through an open approach.
First, the retropatellar cartilage defect was identified and carefully debrided creating a defect with vertical walls. Necrotic/cystic bone was excised until vital bone tissue was visible. Then, microfracturing of the bone was achieved by drilling with an awl or K-wire (Ø 1.2 mm, DePuy Synthes, Oberdorf, Switzerland). In case of a large bony defect, the joint surface of the patella was reconstructed with autologous cancellous bone from the ipsilateral tibia or femur. Thereafter the bilayer type I/III collagen matrix (Chondro-Gide, Geistlich Pharma AG, Wolhusen, Switzerland) was cut to fit the defect and placed on the lesion. After complete coverage of the defect, surgical fibrin glue was applied to secure the membrane to the adjacent cartilage (Tissucol Duo S, Baxter International Inc., Deerfield, IL) ( Fig. 2 ). To ensure stable membrane fixation, the joint was brought through full range of motion. Concomitant corrective surgery for patellar instability was performed as indicated. Arthrotomy was closed using running absorbable sutures followed by standard wound closure.
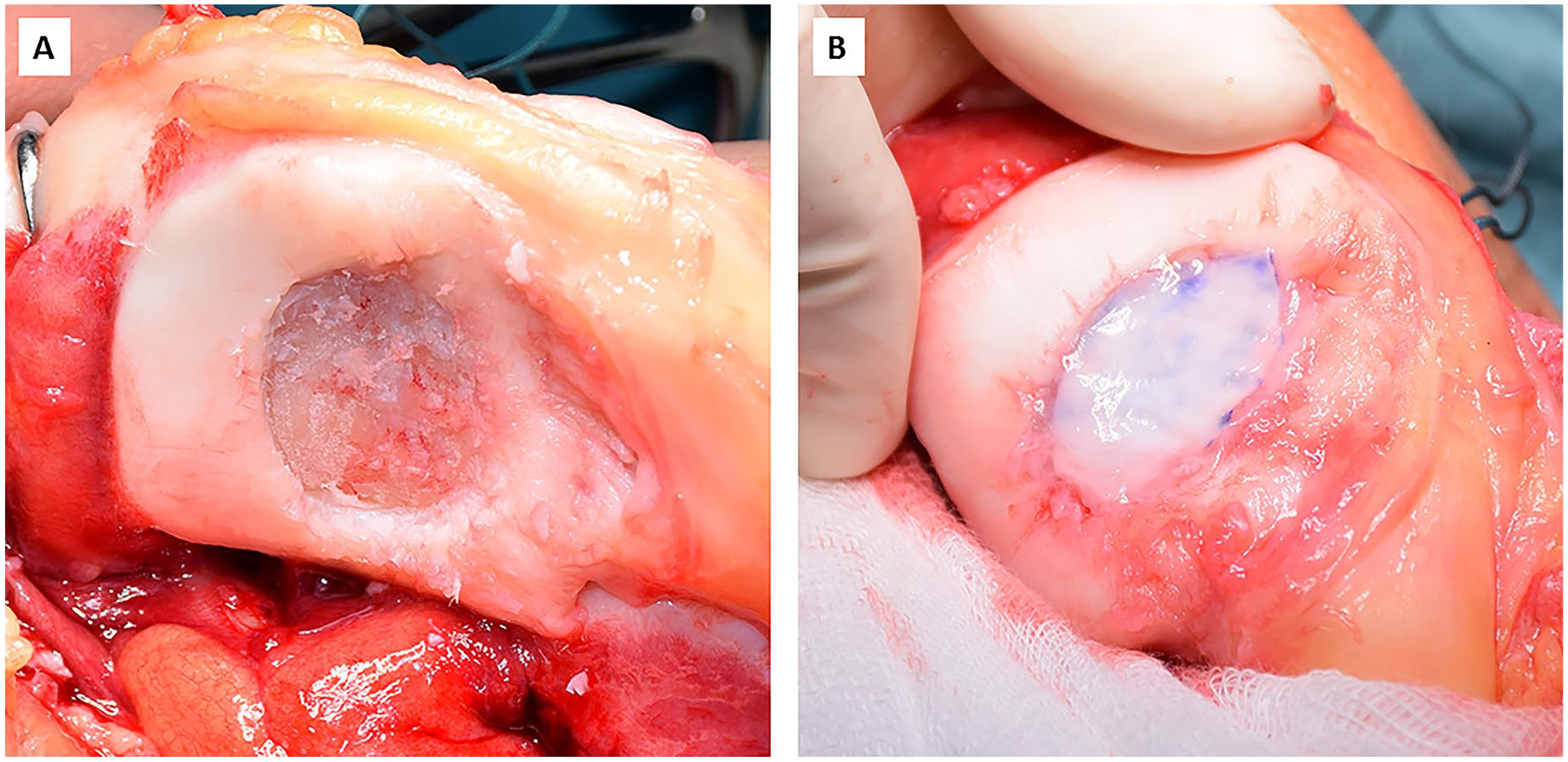
(
Postoperative Rehabilitation
After surgery, patients were immobilized in a knee brace for the immediate postoperative period. After 2 days, protected partial weightbearing was allowed with the knee in a dynamic brace for the first 6 weeks. Stepwise increase of active and passive range of motion was emphasized during that time to avoid arthrofibrosis. After 6 weeks, the brace was removed and full weightbearing was allowed. Return to sport was permitted by 6 to 9 months postoperatively, depending on the sport (running vs. cutting sports).
Definition of Failure
Patients who presented with persistent pain and therefore underwent revision procedures such as autologous chondrocyte implantation, osteochondral grafting, microfracture, arthroplasty, or failure of more than 25% of the graft, were considered a failure. This definition was previously utilized for autologous chondrocyte implantation grafts and served to provide standardization and improve comparability.6,45-47
Statistical Analysis
Sociodemographic and clinical characteristics of patients were determined using descriptive statistics. All data were assessed for normality utilizing the Shapiro-Wilk test. Subsequently, continuous variables were analyzed with the independent
Results
The reviewed cohort included 31 knees of 29 patients with a mean age at the time of surgery of 27.9 ± 11.0 years and a BMI averaging 25.4 ± 5.5 kg/m2. Of these, 29 knees (93.5%) underwent concomitant corrective surgery for patellar instability ( Table 1 ). The mean postoperative clinical follow-up was 4.1 ± 1.9 years. While 9 knees (29%) had prior knee surgery, of which 7 (22.6%) had cartilage surgery (4 debridement, 2 mosaicplasty, and 1 chondral flake refixation), the remaining 21 knees (67.7%) received primary retropatellar AMIC. A history of patellar dislocation was present in 20 knees (64.5%) with recurrent dislocations in 16 knees (51.6%). Traumatic injury without patellar dislocation was reported in 4 knees (12.9%) ( Table 2 ).
Demographics and Treatment of the Patient Cohort.
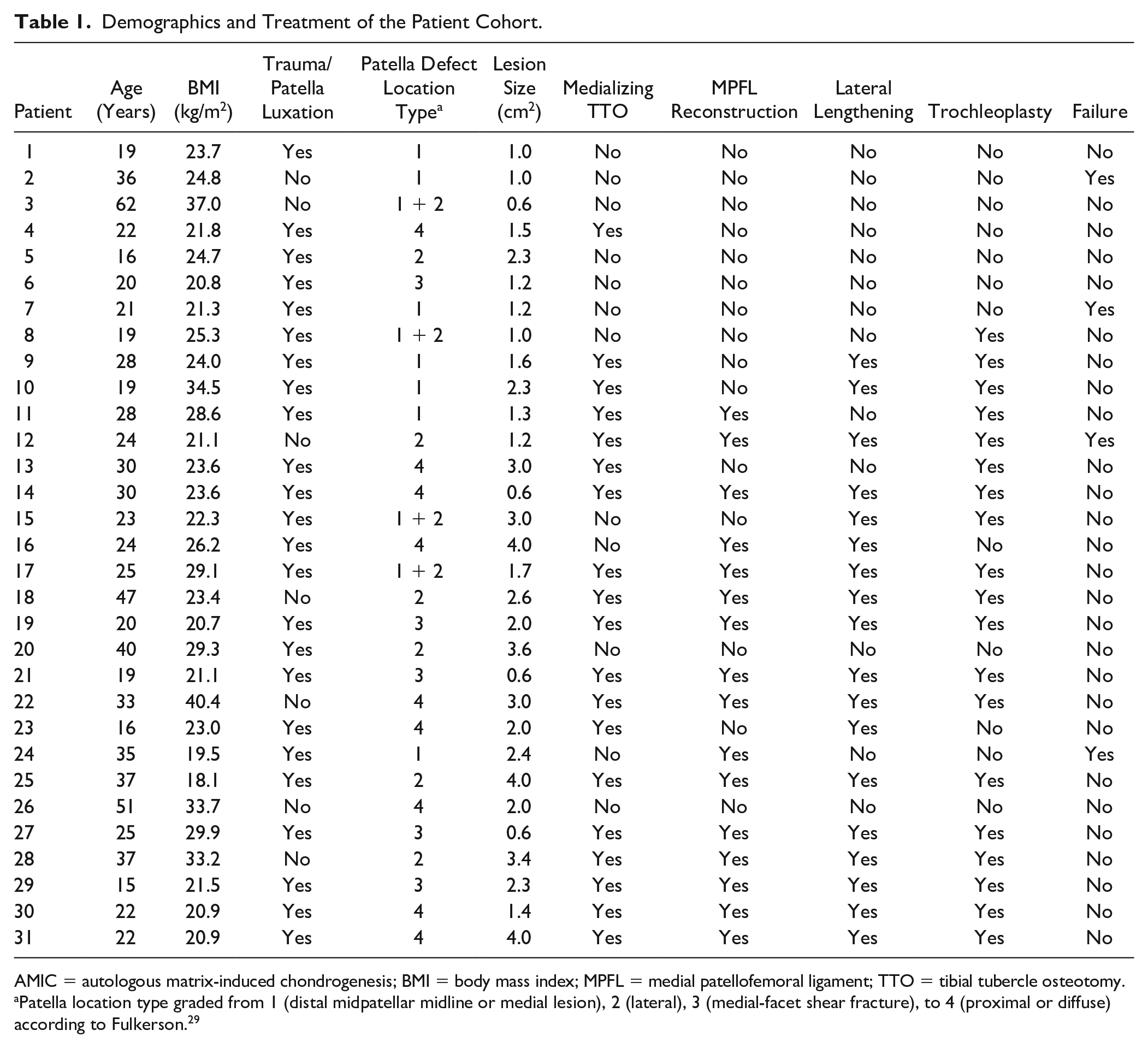
AMIC = autologous matrix-induced chondrogenesis; BMI = body mass index; MPFL = medial patellofemoral ligament; TTO = tibial tubercle osteotomy.
Patella location type graded from 1 (distal midpatellar midline or medial lesion), 2 (lateral), 3 (medial-facet shear fracture), to 4 (proximal or diffuse) according to Fulkerson. 29
Patient and Lesion Characteristics.
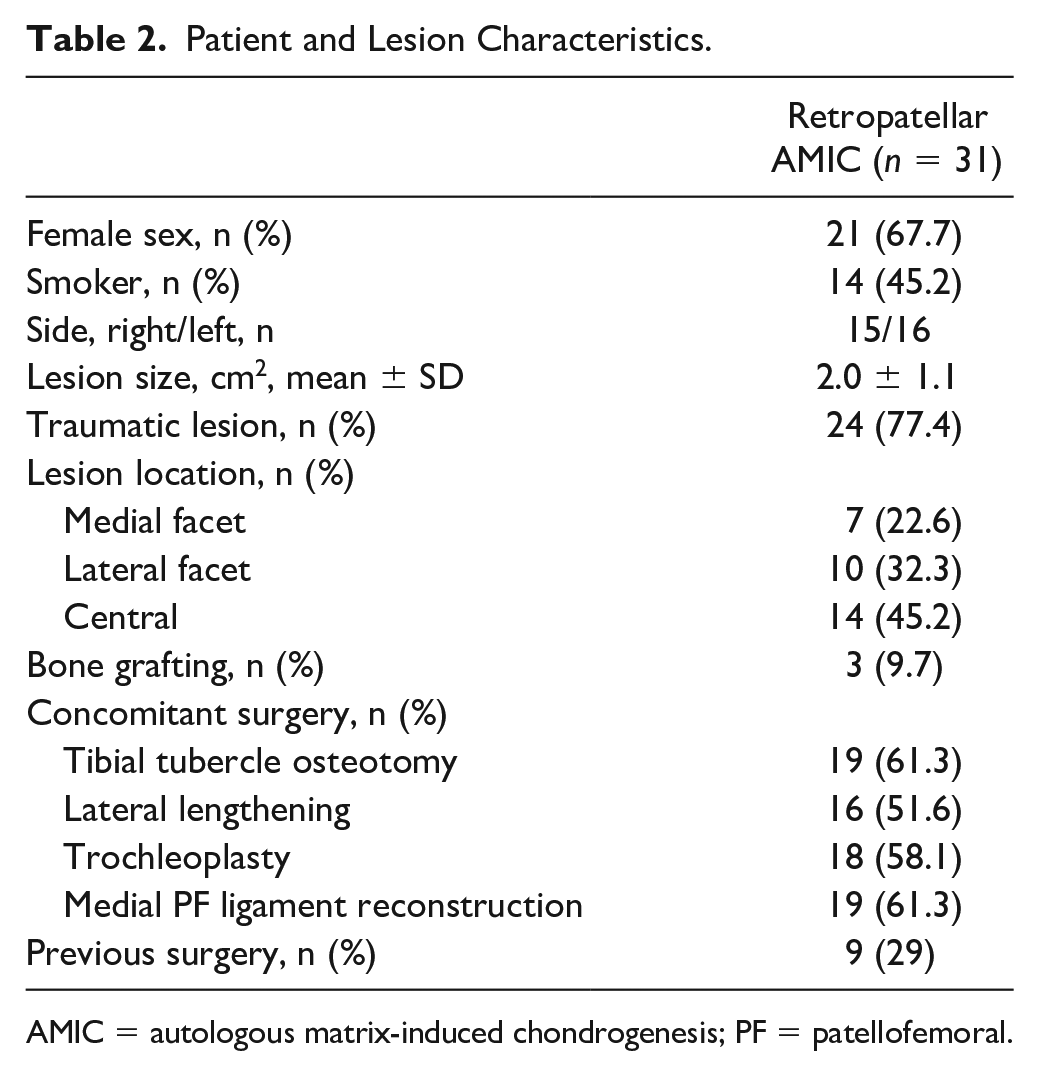
AMIC = autologous matrix-induced chondrogenesis; PF = patellofemoral.
Agreement for trochlear (Dejour) and patellar dysplasia (Wiberg) assessed with Cohen’s kappa were substantial (κ = 0.71) and excellent (κ = 0.94), respectively. ICCs assessed for all other postoperative PF parameters but TTTG (ICC = 0.82) resulted in excellent agreement (ICC > 0.9) between the readers (all,
Complications and Reoperations
In the study period, the AMIC graft failed in 4 patients (12.9%) at a mean follow-up of 21 ± 14.1 months. Of these, 3 patients (75%) presented with an initial patellar lesion type I and 1 patient with a lesion type II (25%). None of the lesion type I patients underwent concomitant TTO. A total of 11 knees (35.5%) underwent reoperations, of which 8 (25.8%) had screw removal after tibial tubercle osteotomy (TTO), 1 patient (3.2%) had revision with microfracturing because of a partial AMIC-membrane dissection and proximalization TTO, 1 patient (3.2%) was revised to PF arthroplasty (PFA) because of symptomatic PF osteoarthritis, and 1 patient (3.2%) had medial patellofemoral ligament (MPFL) reconstruction due to persistent PF instability. One patient (3.2%) presented with persistent anterior knee pain (VAS = 80) and postoperative MRI showed failure of the entire AMIC graft, yet revision surgery was refused.
Clinical Outcome
At the final follow-up, patients who underwent retropatellar AMIC that did not fail (
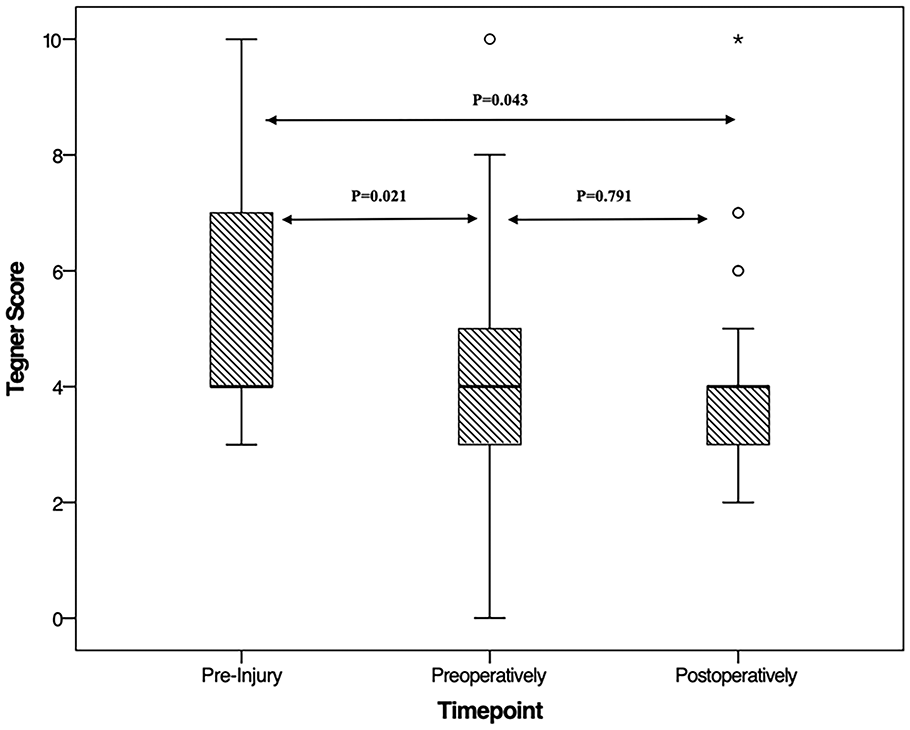
Comparison of Tegner scores between preinjury, preoperatively, and postoperatively.
When correlating postoperative clinical scores and patient-/lesion-specific characteristics, female sex was negatively associated with KOOS QOL (
Patients with failed grafts within the study period had a significantly smaller patellar and Laurins’s PF angle than patients whose graft did not fail (
Comparison of Patient-/Lesion-Specific Characteristics and Postoperative PF Parameters between Failures and Nonfailures.
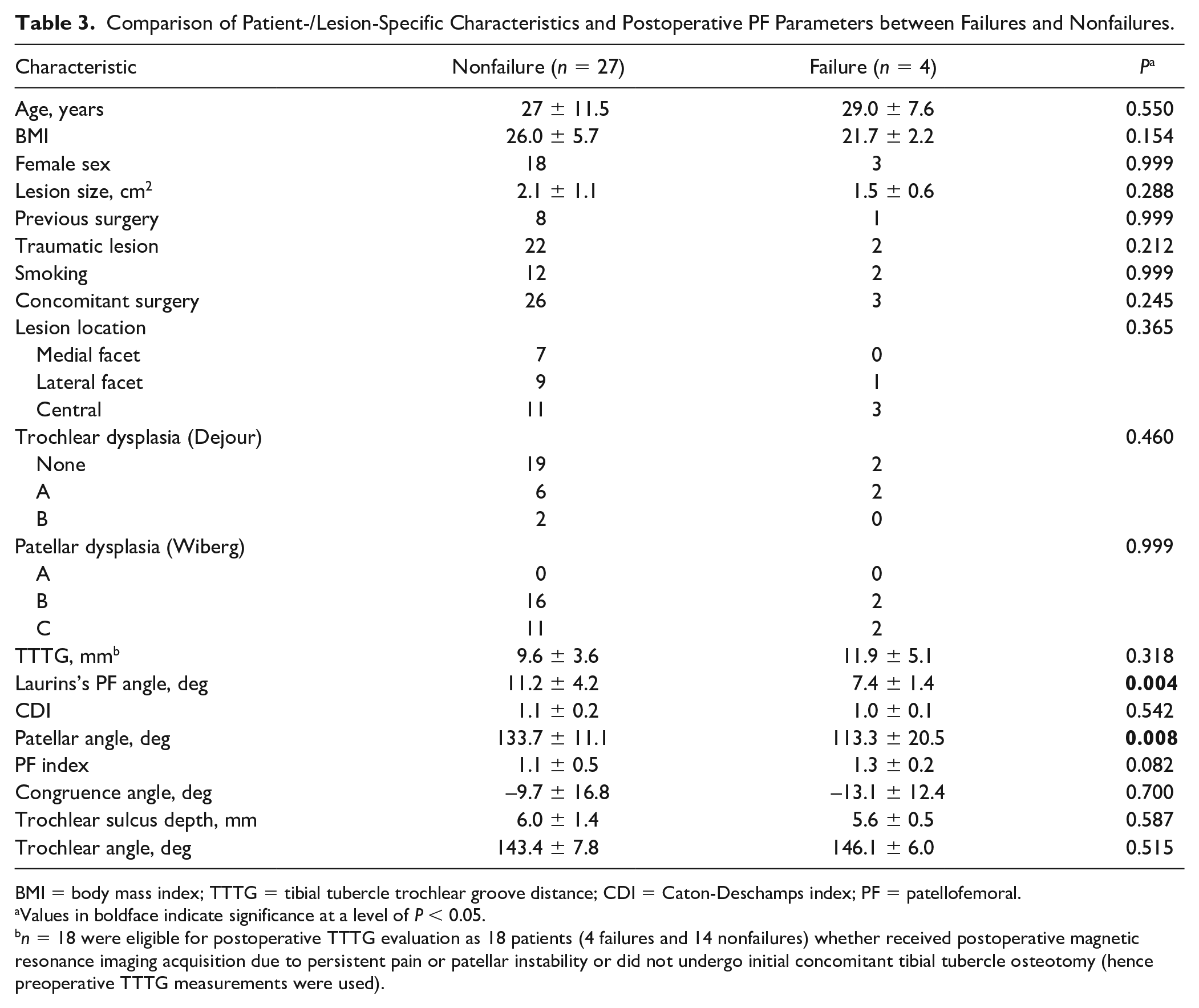
BMI = body mass index; TTTG = tibial tubercle trochlear groove distance; CDI = Caton-Deschamps index; PF = patellofemoral.
Values in boldface indicate significance at a level of
At final follow-up, 19 patients (61.3%) complained about anterior knee pain with a mean VAS of 21.7 ± 26.5 points during daily life and 45.7 ± 28.4 points during sports. Generally, 25.8% of patients reported that they were very satisfied with the result of the surgery, 51.6% were satisfied, 9.7% were rather unsatisfied and 12.9% were very unsatisfied at final follow-up. Of all determined patient- and lesion-specific factors, the patellar angle was the only parameter that was significantly associated with the patient’s satisfaction level (
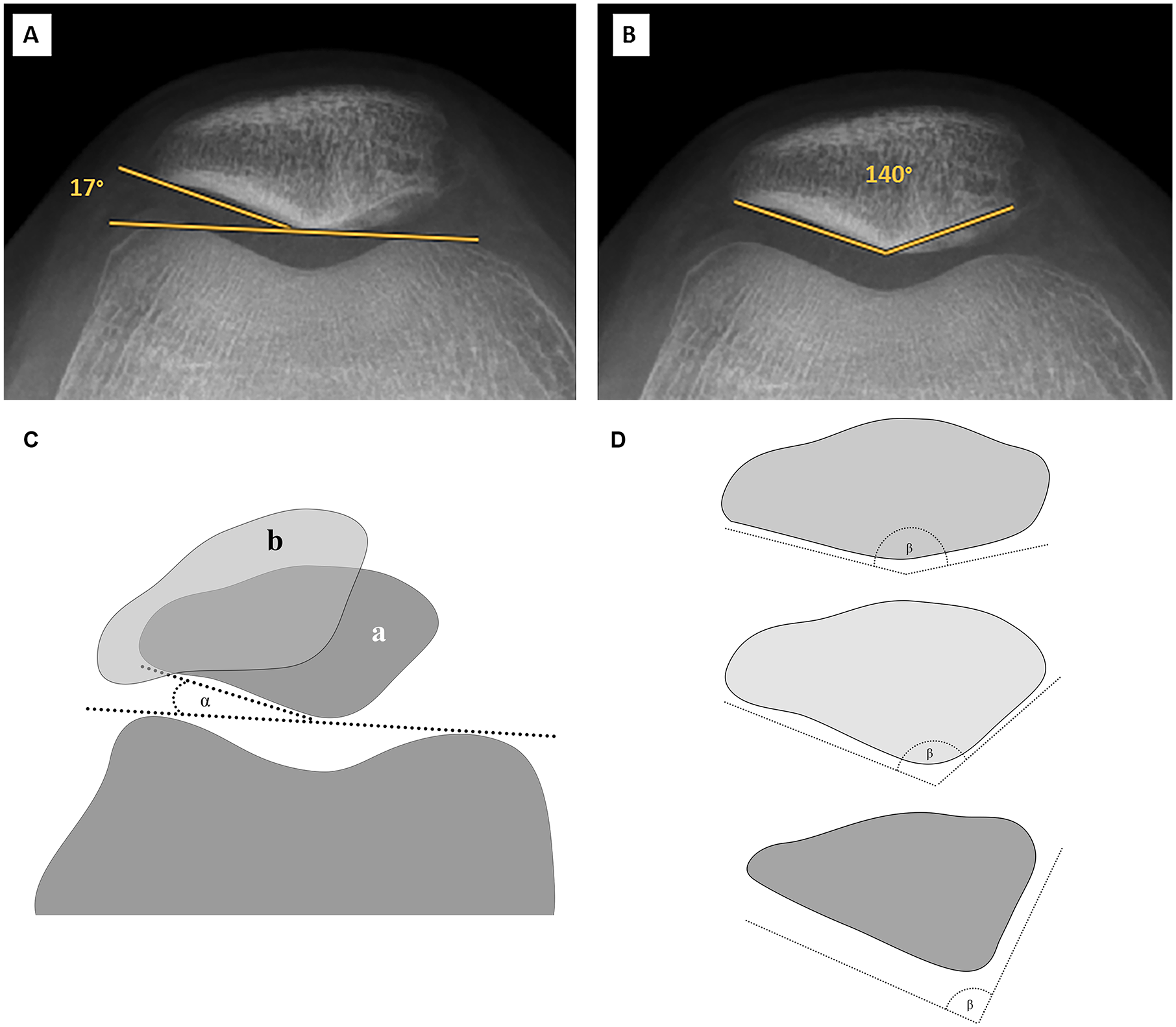
(
Discussion
The key findings of this study are that retropatellar AMIC with concomitant corrective surgery for patellar instability resulted in satisfactory clinical outcome with a low failure rate (12.9%) at a mean follow-up of 4.1 ± 1.9 years. Both, a smaller patellar and Laurins’s PF angle were the only PF parameters that were significantly associated with failure of retropatellar AMIC. Generally, 77.4% of patients reported a satisfactory result after retropatellar AMIC, yet only 35.4% returned to the previous level of sport.
In 2003, Behrens
D’Hollander
In a subanalysis of retropatellar AMIC in 20 patients, Kusano
In another small case series, Sadlik
A more recent study by Tradadi
Kaiser
Certain anatomical factors such as dysplasia and patellar maltracking can lead to premature cartilage degeneration. In a study by Ambra
In the current study, only a smaller Laurins’s PF and patella angle were significantly associated with retropatellar cartilage repair failure, suggesting an appropriate correction of PF morphology. However, as a smaller Laurins’s PF angle is an indirect indicator of increased patellar tilt, this finding underlines the results reported by Ambra
To assess return to sporting level after retropatellar AMIC, preinjury to postoperative Tegner activity scores were reported. Despite generally good patient satisfaction, the level of sport activity decreased significantly. Similar to a previous report of AMIC for osteochondral lesions of the talus, especially high preinjury sporting level activity patients tend to not return to their previous level. 60
The following limitations have to be acknowledged. First, preoperative KOOS were unavailable and only 67.7% of preoperative Kujala scores were available as the study was retrospective in its design. Tegner preinjury and presurgery scores collected retrospectively at the postoperative follow-up assessment, potentially introducing recall bias. However, selection bias was minimized by reviewing all patients with retropatellar AMIC since the introduction of this technique at our institution and achieving a follow-up rate of 86%. Second, postoperative MRI was not available in all patients, which would have enabled this study to assess repair tissue quality and postoperative patellar tilt. Moreover, due to the limited clinical value of postoperative MRI or arthro computed tomography in cartilage repair, 61 this study did not assess or report postoperative MR imaging outcome. Contrarily, postoperative MRI would have been useful in evaluating postoperative patellar tilt, thus assessing the effect of concomitant corrective surgery. As MRI was not available in all patients, this study utilized the Laurins’s PF angle, which is an accepted indirect measurement for patellar tilt. 41 Third, the high rate of concomitant procedures makes it difficult to evaluate the isolated clinical effect of retropatellar AMIC. Yet, this cohort represents the real-world scenario of patients that receive retropatellar cartilage repair, who often present with complex PF anatomical pathologies and therefore require extensive surgical intervention. Considering the high failure rate in type I lesions without concomitant TTO and the negative overall effect of a small patellar and Laurins’s PF angle, this study supports the growing evidence for the need of unloading retropatellar cartilage repair, when indicated.
By assessing postoperative anatomical parameters and analyzing their influence on the outcome of retropatellar AMIC, the current study is an important contribution to the knowledge about the outcome of AMIC for isolated focal cartilage lesions of the patella.
Conclusion
AMIC for retropatellar cartilage lesions in combination with concomitant corrective surgery for patellar instability results in low failure rate with satisfactory clinical outcome and patient satisfaction of almost 80% at mid-term follow-up. As most failures occurred in patients without concurrent TTO and both a smaller patellar and Laurins’ PF angle were associated with less favorable outcome, this study supports the growing evidence for the need of unloading retropatellar cartilage repair, when indicated.
Supplemental Material
sj-pdf-1-car-10.1177_19476035211021908 – Supplemental material for Autologous Matrix-Induced Chondrogenesis (AMIC) for Isolated Retropatellar Cartilage Lesions: Outcome after a Follow-Up of Minimum 2 Years
Supplemental material, sj-pdf-1-car-10.1177_19476035211021908 for Autologous Matrix-Induced Chondrogenesis (AMIC) for Isolated Retropatellar Cartilage Lesions: Outcome after a Follow-Up of Minimum 2 Years by Manuel Waltenspül, Cyrill Suter, Jakob Ackermann, Nathalie Kühne and Sandro F. Fucentese in CARTILAGE
Footnotes
Authors’ Note
Investigation performed at the Balgrist University Hospital, Switzerland.
Acknowledgments and Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval (No. 2020-01052) was granted by the local research ethics committee.
Informed Consent
All included patients gave their written informed consent.
Trial Registration
Not applicable.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
