Abstract
Objectives
Considering the lack of cure for MNCD, this article focuses on non-pharmacological interventions such as outdoor activities, their characteristics and their effects on behaviors, symptoms, quality of life, autonomy and cognitive functioning.
Background
People living with major neurocognitive disorders (MNCD) may experience reactive behaviors, symptoms, decreased autonomy, quality of life and cognitive functioning. There is currently no treatment that can reverse or halt the cognitive decline resulting from MNCD.
Methods
A scoping review was conducted using the method of Arksey and O'Malley (2005) and following PRISMA guidelines. AgeLine, APA PsycInfo, CINAHL Plus with Full Text and MEDLINE were used to conduct the literature search.
Results
Most outdoor activities identified in this study were: activities carried out in a garden (n=5); activities involving active participation (n=14); activities offering the possibility of being carried out in a group or individually (n=6); activities lasting less than an hour (n=7); and activities taking place in the participants' place of residence (n=13). Most of studies showed that outdoor activities were associated with positive impacts on overall mood (n=12). Several studies reported reduced agitation (n=7), improved cognitive functioning (n=5) and increased well-being (n=5) in participants undertaking various outdoor activities.
Conclusions
Outdoor activities and the associated freedom to make decisions led to a range of benefits in the five categories that were studied. These benefits apply whether the activities are carried out in a group or individually, whether they are active or inactive, and whether they take place close to home. Future research would be relevant to specify the characteristics of the activities to be performed according to the desired benefits.
Introduction
The ageing of the Canadian population is accompanied by an increase in the prevalence of major neurocognitive disorders (MNCD) also called dementia (Alzheimer Society of Canada, 2024a; Alzheimer Society of Canada, 2024c). In fact, in 2020, 8.4% of Canadians over 65 were living with an MNCD. It is estimated that by 2050, this proportion could rise to 13.2%. By 2030, nearly 1 million Canadians will be living with dementia, and more than 1.7 million by 2050. Alzheimer's disease is the most prevalent MNCD that also includes vascular neurocognitive disorders, frontotemporal degeneration, Lewy body, and other forms of MNCDs (Sheppard & Coleman, 2020). Decreased cognitive functioning and autonomy resulting in difficulties remaining at home are among the major impacts that can result from MNCD. In fact, memory, thinking, language, and problem-solving difficulties, most often resulting from MNCD, affect a person's ability to carry on with daily activities (Alzheimer Society of Canada, 2024c). Furthermore, MNCD can lead to different consequences such as a change in behaviors (e.g., agitation, wandering) and appearances of symptoms (e.g., mood swings, varying levels of wakefulness). Moreover, people living with MNCD are often unable to meet their needs independently or communicate them clearly to others, which can adversely affect their quality of life (Bourbonnais et al., 2021). Thus, it appears essential to find ways to intervene more effectively with this clientele in order to meet the needs of the growing number of people living with an MNCD.
Despite the lack of a cure for MNCDs (Alzheimer Society of Canada, 2024b), there are alternative means of slowing the progression of the disease and reducing its impact. Among these, environmental design (e.g., camouflaging doors or doorknobs) shows positive impacts on behavioral and psychological symptoms of dementia (BPSD) (Bonin et al., 2020). Cognitive stimulation is also among the non-pharmacological treatments with benefits for cognitive functioning and quality of life in people with MNCD (Alvares Pereira et al., 2022).
Across a range of health conditions, outdoor activity shows positive effects on affect, cognition, well-being, and symptoms of anxiety and depression (Lackey et al., 2021). In addition, a scoping review of the effects of nature-based rehabilitation found that it improved motor and sensory-motor function, quality of life, and cognitive function in people with brain injury (stroke, CBT, and neurotoxic accident) (Vibholm et al., 2020). To our knowledge, no study has documented the benefits of outdoor activities and their impact-related characteristics specifically for people living with MNCD. In order to contribute to the improvement of behaviors, symptoms, quality of life, and autonomy of people living with MNCD, it appears important to explore the possible impacts of outdoor activities specifically for people living with MNCD as well as the characteristics of these activities. Thus, this scoping review will identify and describe the characteristics of outdoor activities and their effects on the behaviors, symptoms, quality of life, autonomy, and cognitive functioning of people living with MNCD.
Methodology
This scoping review followed the methodology proposed by Arksey and O’Malley (2005), which consists of five stages: identification of the research question, identification of relevant studies, selection of studies, extraction and classification of data, and finally, synthesis of data and communication of results. PRISMA guidelines were also followed (Figure 1). The aim of this methodology is to examine the extent and nature of research related to the question posed, to synthesize and disseminate research findings, and to identify gaps in the literature.
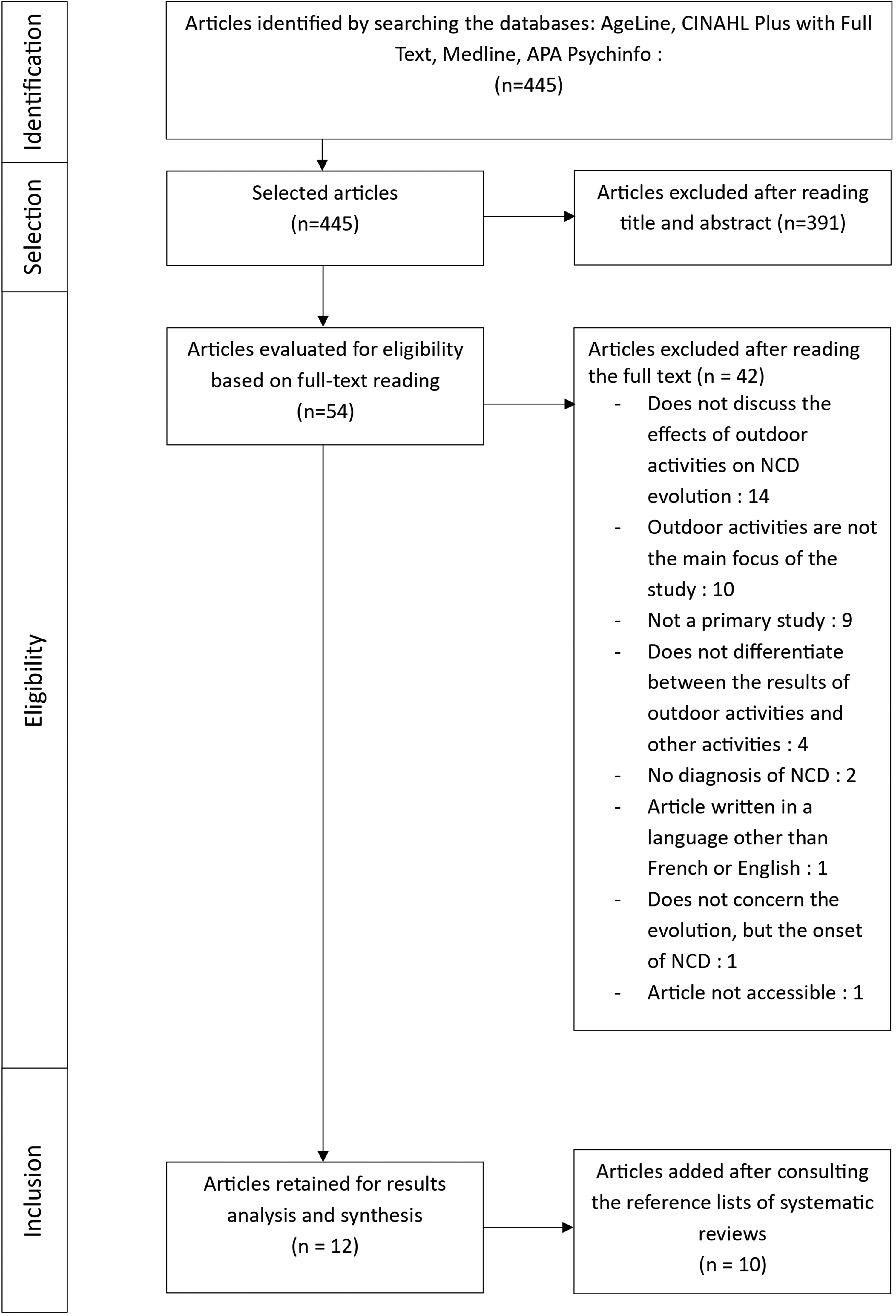
Flowchart.
Identifying the Research Question
The research question selected for this study is as follows: What are the characteristics of outdoor activities and their effects on the behaviors, symptoms, quality of life, autonomy, and cognitive functioning of people living with MNCD?
Identifying Relevant Studies
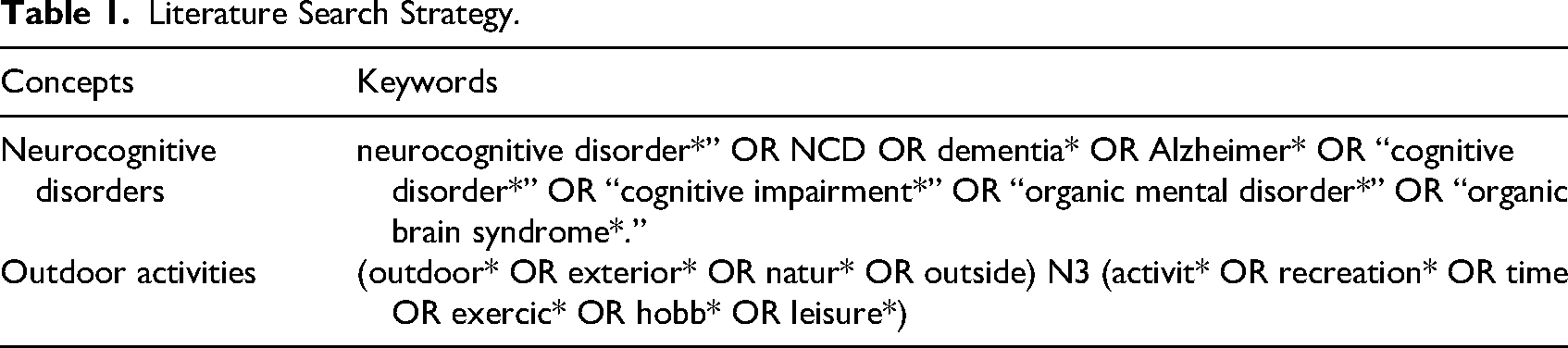
The literature search was carried out on January 31, 2024, and updated on October 24, 2024. The search strategy was based on a concept plan whose keywords were determined by the entire research team (Table 1). This strategy was validated and improved by an expert librarian in the healthcare field. Four databases were consulted: AgeLine, APA PsycInfo, CINAHL Plus with Full Text and MEDLINE. Selected keywords were searched in document titles and abstracts.
Literature Search Strategy.
Selection of Studies
Search results were exported to Zotero, a bibliographic reference management software, where duplicates were removed. To be selected, publications had to meet the following inclusion criteria: (1) The study population had an MNCD. Studies in which caregivers or family members reported effects on people living with MNCD were included. (2) Selected studies had to include one or more outdoor activities in which individuals participated actively (e.g., going for a walk) or inactively (e.g., sitting in a garden). These activities had to take place outside of a building. Articles dealing with activities taking place outside the home but taking place in an indoor environment (e.g., grocery shopping, visiting a fitness center) were not considered. In addition, articles mentioning activities that are typically performed outdoors but were carried out indoors (e.g., gardening indoors) were not retained for this study. (3) Only empirical studies were included (primary studies). (4) The publication had to report qualitative and/or quantitative results related to the research question. (5) The publication date was between 2009 and 2024. In addition, publications were excluded if they met the following exclusion criteria: (1) Studies in which participants had cognitive deficits without a diagnosis of MNCD. (2) There were no results linking outdoor activities to MNCD or its manifestations. (3) Outcomes associated with outdoor activities were not dissociable from those associated with indoor activities. (4) The article was written in a language other than English or French.
To select the articles relevant to the research, we first formed two dyads within the research team. The articles were divided equally and randomly between the dyads, with each reviewer individually analyzing the title and abstract according to inclusion and exclusion criteria. The dyads then pooled their findings to identify any differences in the articles selected. A discussion between the members of the dyad resolved any differences. If a disagreement persisted after the discussion, all members of the research team were consulted at a meeting to validate the selection of articles, and a joint decision was taken. After this consultation, if ambiguity persisted, the articles were included for full-text reading. The second step in the article selection process was to read the full texts to assess whether they should be retained. New dyads were formed among the members of the research team, and the articles selected for full reading were distributed equally and randomly among them. The same method as in the first stage, starting with an individual analysis, was applied to the inclusion of articles and to the resolution of ambiguities. Ambiguities were resolved at a validation meeting involving all members of the research team. Subsequently, articles included in the reference list of four systematic reviews and a scoping review meeting the inclusion criteria were considered. At the end of this process, 22 articles were included in the scoping review.
Data Extraction and Classification
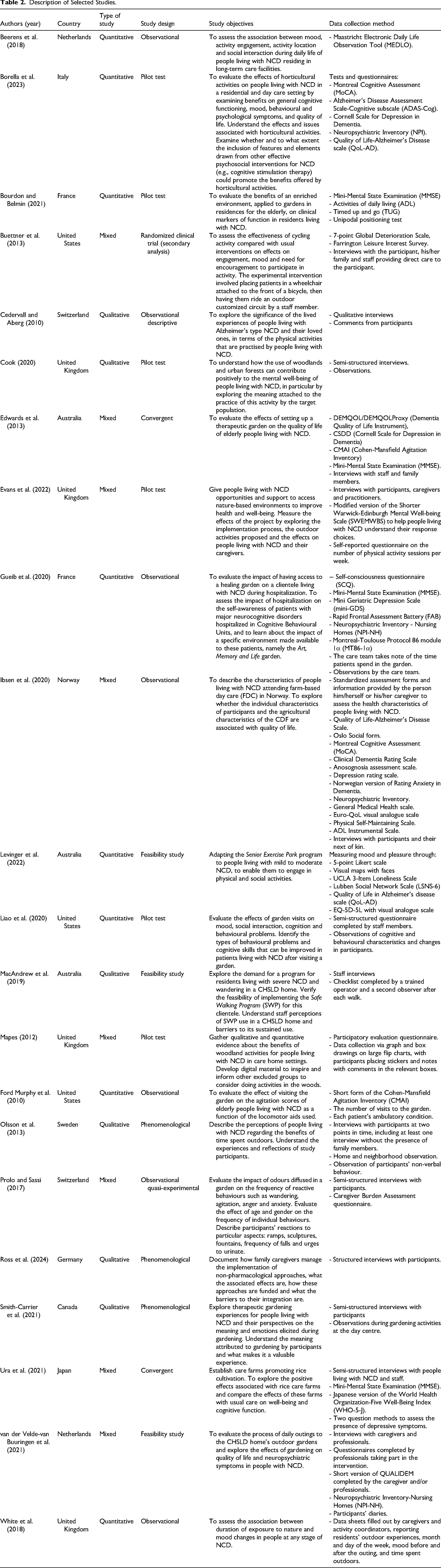
The extraction of data relevant to answering the research question was carried out following a complete reading of the articles. This identified the authors, date of publication, country, type of study, specifications, objectives, and data collection method (Table 2). The extraction also highlighted the characteristics of the outdoor activities (type of activity, context, frequency, duration, and location of activity), the characteristics of the study population, the effects observed on the autonomy, symptoms, behaviors, quality of life, and cognitive functioning of people living with MNCD, and finally, the limitations and recommendations of the studies (Table 3). These characteristics were chosen because they were the main variables investigated by the selected studies. The results reported in the reviewed studies concern both decision-making autonomy and functional autonomy. With regard to symptoms, the results of the studies reviewed included: mood, affect, level of arousal, feelings of loneliness, depression, happiness, levels of distress, energy levels, emotional changes, disinhibition, apathy, dysphoria, euphoria, hallucinations, delusions, and so on. On the other hand, behavioral findings in the studies reviewed included: agitation, social interactions and isolation, aggressive behaviors, communication (patient-patient, and patient-caregiver), resistance to care, wandering, repetition (words/questions/activities), expressions of suspicion, etc. For quality of life, results included perception of well-being and satisfaction with social relationships. Finally, results dealing with memory, visuospatial skills, executive functions, attention, concentration, working memory, language skills, temporal and spatial orientation, learning, reminiscence, problem solving, anosognosia, judgment, introspection, and body representation were extracted in relation to cognitive functioning. Data extraction was carried out individually. Two data extraction validation meetings were held at the beginning and end of the process, to ensure standardization.
Description of Selected Studies.
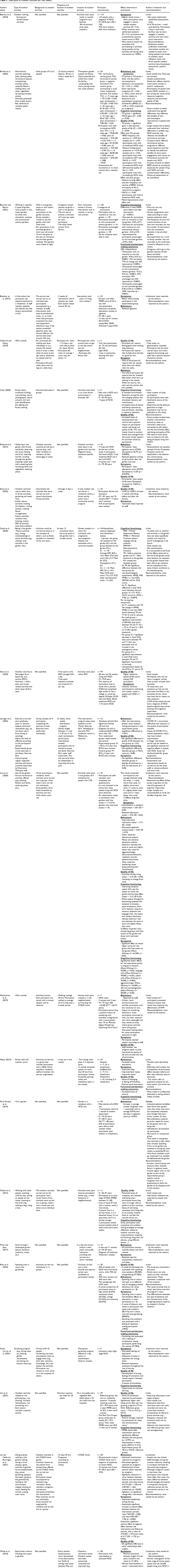
Description of Outdoor Activities and Their Effects.
Data Synthesis and Communication of Results
In order to highlight the effects of outdoor activities on MNCD, the data collected were categorized according to behaviors, symptoms, quality of life, autonomy, and cognitive functioning. The characteristics of outdoor activities relevant to the analysis were also categorized: type of activity, context, frequency, duration, and location (Table 3).
Results
After removing duplicates, 445 publications were identified. Following analysis of titles and abstracts, 54 articles were read in full to check whether they met the selection criteria. Of these, 12 articles were selected. Following the consultation of systematic reviews and a scoping review, 10 additional articles from the reference list of these publications were added. In all, 22 publications meeting the inclusion criteria were selected (Figure 1).
Descriptive data are presented in Table 2. Studies were conducted in Australia (n = 1), Canada (n = 1), France (n = 2), Germany (n = 1), Italy (n = 1), Japan (n = 1), the Netherlands (n = 2), Norway (n = 1), Sweden (n = 1), Switzerland (n = 2), the UK (n = 4), and the USA (n = 3). Eight studies used a quantitative design, six a qualitative design, and eight a mixed design. Quantitative designs included: observational studies (n = 4), pilot trials (n = 3), and feasibility studies (n = 1). Qualitative designs included: phenomenological studies (n = 3), a descriptive observational study (n = 1), a feasibility study (n = 1), and a pilot trial (n = 1). Finally, the mixed designs included: observational studies (n = 2), pilot trials (n = 2), convergent studies (n = 2), feasibility study (n = 1), and randomized clinical trial (secondary analysis) (n = 1).
For each of the studies identified, a description of the different characteristics of outdoor activities, i.e., type, context, frequency, duration and location, as well as a presentation of their effects on participants’ quality of life, symptoms, behaviors, cognitive functioning, and autonomy, is presented in Table 3.
Characteristics of Outdoor Activities
Type of Outdoor Activities
The studies identified in this scoping review present a wide variety of outdoor activities. Those identified in the greatest number were activities that took place in a garden, such as going for a walk, getting together with family, and birdwatching (Bourdon & Belmin, 2021; Edwards et al., 2013; Ford Murphy et al., 2010; Gueib et al., 2020; Prolo & Sassi, 2017; Ross et al., 2024). In some studies, the activities performed were highly diversified, as participants could choose for themselves which ones they wished to perform (Cook, 2020; Edwards et al., 2013; Gueib et al., 2020; Ibsen et al., 2020; Olsson et al., 2013). For example, some people could listen to music or just sit outside, while others preferred to feed the animals (van der Velde-van Buuringen et al., 2021). In two studies reviewed, only walking was performed as an outdoor activity (Cedervall & Aberg, 2010; MacAndrew et al., 2019). One study included both walking and picnicking (Mapes, 2012). In three studies, participants took part in plant-related activities such as gardening and horticulture (Borella et al., 2023; Liao et al., 2020; Smith-Carrier et al., 2021). One study offered participants a variety of forest-related activities, such as tree-planting, walks, preparing meals in the forest, as well as making natural works of art (Cook, 2020). One study included only a cycling activity where the person sat on a front seat and was propelled by another person (Buettner et al., 2013). Rice-growing activities were carried out by participants in one of the studies (Ura et al., 2021). In another study, the outdoor activity was physical exercise in the form of a circuit (Levinger et al., 2022). Some of the activities performed by participants were associated with farming and animals (Beerens et al., 2018; Ibsen et al., 2020). One study included both indoor and outdoor activities, with the latter ranging from flower arranging to museum visits (Evans et al., 2022). More than the majority of studies reviewed included outdoor activities where participants were active (Beerens et al., 2018; Borella et al., 2023; Bourdon & Belmin, 2021; Cedervall & Aberg, 2010; Cook, 2020; Evans et al., 2022; Ibsen et al., 2020; Levinger et al., 2022; Liao et al., 2020; MacAndrew et al., 2019; Mapes, 2012; Prolo & Sassi, 2017; Ross et al., 2024; Smith-Carrier et al., 2021; Ura et al., 2021) such as walking or gardening. In some studies, both active and inactive outdoor activities could be performed (Edwards et al., 2013; Gueib et al., 2020; Ford Murphy et al., 2020; Olsson et al., 2013; van der Velde-van Buuringen et al., 2021; White et al., 2018). Only one study included an outdoor activity where participants were inactive as they were on a seat on the front of a bicycle and were driven by another person (Buettner et al., 2013).
Context of Outdoor Activities
Several studies (n = 4) included group activities (Borella et al., 2023; Cook, 2020; Evans et al., 2022; Mapes, 2012). Other studies (n = 5), meanwhile, presented activities performed individually or in the presence of a caregiver (Bourdon & Belmin, 2021; Buettner et al., 2013; Cedervall & Aberg, 2010; Gueib et al., 2020; MacAndrew et al., 2019). In addition, a few studies (n = 7) included both activities performed alone and in groups (Edwards et al., 2013; Levinger et al., 2022; Liao et al., 2020; Olsson et al., 2013; Ross et al., 2024; Smith-Carrier et al., 2021; van der Velde-van Buuringen et al., 2021). Finally, six studies reported no information on this subject (Beerens et al., 2018; Ford Murphy et al., 2010; Ibsen et al., 2020; Prolo & Sassi, 2017; Ura et al., 2021; White et al., 2018).
Frequency and Duration of Outdoor Activities
With regard to the frequency and duration of outdoor activities, these two aspects show a fair degree of variability between studies. In terms of frequency, the activities identified in some of the studies (n = 7) took place several times a week (Borella et al., 2023; Bourdon & Belmin, 2021; Buettner et al., 2013; Cedervall & Aberg, 2010; Evans et al., 2022; Levinger et al., 2022; MacAndrew et al., 2019). In one of the included studies, participants took part in outdoor activities with variable frequency, i.e., according to personal preference (van der Velde-van Buuringen et al., 2021). One study reported the effects of a one-off outdoor activity taking place on a single day (Mapes, 2012). In terms of duration, most studies (n = 7) included activities lasting less than an hour (Borella et al., 2023; Bourdon & Belmin, 2021; Buettner et al., 2013; Cedervall & Aberg, 2010; MacAndrew et al., 2019; Ura et al., 2021; van der Velde-van Buuringen et al., 2021), while the activities reported in two studies were spread over a period of more than an hour (Ibsen et al., 2020; Levinger et al., 2022). Furthermore, outdoor activities in one of the studies ranged in duration from 10 to 200 min, with the majority (76.6%) taking place between May and September (White et al., 2018). The activities reported in one study did not specify the frequency (Gueib et al., 2020), but reported a total duration of hours for the study period. Indeed, the total activity period was reported as 12 h, spread over 2 weeks. On the other hand, five studies reported on activity programs taking place over a period of 2 weeks (Buettner et al., 2013), 3 weeks (MacAndrew et al., 2019), 6 weeks (Borella et al., 2023), 12 weeks (Levinger et al., 2022), and 25 weeks (Ura et al., 2021) respectively. Some studies did not report information about the frequency, period or duration of activities performed (Beerens et al., 2018; Cook, 2020; Edwards et al., 2013; Ford Murphy et al., 2010; Liao et al., 2020; Olsson et al., 2013; Prolo & Sassi, 2017; Ross et al., 2024; Smith-Carrier et al., 2021).
Location of Outdoor Activities
The majority of outdoor activities took place directly in the participants’ places of residence, whether in a nursing home (Beerens et al., 2018; Borella et al., 2023; Buettner et al., 2013; MacAndrew et al., 2019; van der Velde-van Buuringen et al., 2021), a specific unit for people living with MNCD (Edwards et al., 2013; Ford Murphy et al., 2010; Gueib et al., 2020; Liao et al., 2020), a seniors’ residence (Bourdon & Belmin, 2021; Ross et al., 2024; White et al., 2018) or their home neighborhood (Cedervall & Aberg, 2010; Olsson et al., 2013; Ross et al., 2024). Other activities took place on the premises of a day center (Prolo & Sassi, 2017; Smith-Carrier et al., 2021) or a green care farm (Ibsen et al., 2020). A few studies specified that outdoor activities took place in nature, for example in green spaces and forests (Cook, 2020; Mapes, 2012) or in a rice paddy and vegetable fields (Ura et al., 2021). Only one of the studies mentioned that the activities took place in a park (Levinger et al., 2022). For one of the studies, outdoor activities were carried out in several different locations, i.e., in a nursing home, in a forest, on a green care farm and in a community space (Evans et al., 2022).
Effects of Outdoor Activities
Effects on Quality of Life and Well-Being
With regard to the effects on participants’ quality of life, several studies indicated an increase in well-being following outdoor activities (Cedervall & Aberg, 2010; Cook, 2020; Evans et al., 2022; Ibsen et al., 2020; Ross et al., 2024; Ura et al., 2021). What's more, the results of some studies specifically identified an improvement in participants’ quality of life (Borella et al., 2023; Edwards et al., 2013; MacAndrew et al., 2019). As for social relationships, other studies (n = 3) showed a positive impact of outdoor activities, notably through the creation of a sense of belonging (Mapes, 2012), positive social encounters (Mapes, 2012; Smith-Carrier et al., 2021) as well as a feeling of connection (Smith-Carrier et al., 2021; Ura et al., 2021). However, in one study, quality-of-life ratings did not increase in the experimental group compared with the control group, which performed usual indoor activities (Levinger et al., 2022). In another study, a lack of significant difference was also reported, although this was related to social relationships (van der Velde-van Buuringen et al., 2021). On the other hand, one study found a decrease in perceived well-being among participants who realized they were no longer able to carry out their usual outdoor activities (Olsson et al., 2013).
Symptom-Related Effects
With regard to symptoms, the majority of studies included in the scoping review (n = 12) showed favorable effects on mood (Beerens et al., 2018; Buettner et al., 2013; Cedervall & Aberg, 2010; Evans et al., 2022; Ibsen et al., 2020; Liao et al., 2020; MacAndrew et al., 2019; Mapes, 2012; Smith-Carrier et al., 2021; van der Velde-van Buuringen et al., 2021; White et al., 2018). In one of the studies reporting this effect, nuances were added in relation to the amount of time spent outdoors. Indeed, marked improvements in mood were linked to a duration of time spent outdoors of at least 20 min. The most significant benefits occurred at 80 to 90 min, and there were no additional benefits beyond this. When the duration exceeded 100 min, the benefits diminished rapidly (White et al., 2018). In the study by Liao et al. (2020), a greater improvement in mood was observed in participants with free access to the garden than in those with restricted access. A reduction in negative emotions experienced by participants, including depressive symptoms and distress, was also reported in several studies (n = 5) (Borella et al., 2023; Edwards et al., 2013; Liao et al., 2020; Ross et al., 2024; Smith-Carrier et al., 2021; van der Velde-van Buuringen et al., 2021). In addition, the results of one study indicated a better level of wakefulness in association with outdoor activities (van der Velde-van Buuringen et al., 2021). Improved sleep was also reported among participants in two studies (Mapes, 2012; Ura et al., 2021). One study showed an increase in food intake among participants (Mapes, 2012). In the study by Prolo and Sassi (2017), a reduction in antipsychotics and sleep medication was observed. In addition, perceptions of relaxation and pleasure were reported by participants who spent time outdoors (Ross et al., 2024). In relation to depression levels, one study reported no significant difference between participants in the experimental group, performing an exercise circuit in a park, and participants in the control group, taking part in usual activities (Levinger et al., 2022).
Behavioral Effects
With regard to behaviors, an overall positive effect on behaviors was observed in one study (needs citation). Indeed, a reduction in the quantity and severity of BPSD was found in participants in the experimental group engaged in horticultural activities (Borella et al., 2023). More specifically, in several studies (n = 7) agitation decreased in participants following the introduction of outdoor activities (Buettner et al., 2013; Cedervall & Aberg, 2010; Edwards et al., 2013; Ford Murphy et al., 2010; Liao et al., 2020; MacAndrew et al., 2019; van der Velde-van Buuringen et al., 2021). Fourteen of the 15 participants in another study reported feeling calmer and more relaxed after attending the garden over a 90-day period (Prolo & Sassi, 2017). In addition, improved verbal communication was observed among participants in three studies (MacAndrew et al., 2019; Mapes, 2012; Ura et al., 2021). Furthermore, in two studies, staff reported a decrease in resistance to care (MacAndrew et al., 2019) and reactive behaviors (Edwards et al., 2013) among participants. In another study, spending time in nature was perceived as an effective way to manage participants’ reactive behaviors (Ross et al., 2024). In addition, a decrease in wandering, especially at night, was observed, as well as an increase in walking intentions for meaningful activities (MacAndrew et al., 2019). One study reported a significant decrease in social isolation following diversified outdoor activities taking place in a garden (van der Velde-van Buuringen et al., 2021). However, in the study by Levinger et al. (2022), social isolation was higher among participants in the experimental group performing an individual exercise circuit in an outdoor park. No hypothesis was put forward by the authors to explain these results. On the other hand, there was a lack of overall effect in one of the studies, as a reduction in the quantity and severity of BPSD was observed in both participants in the experimental group and those in the control group attending or not attending the garden (Gueib et al., 2020).
Effects on Cognitive Functioning
Some studies highlighted the positive effects of outdoor activities on cognitive functioning during horticultural activities (Borella et al., 2023) or visits to conventional sensory or enriched gardens (Bourdon & Belmin, 2021). More specifically, in terms of memory, an improvement was reported following outdoor activities (Cook, 2020; Mapes, 2012). One study showed that outdoor activities enabled participants to use problem-solving strategies (e.g., stopping and taking a moment to think, using cues or a cell phone) (Olsson et al., 2013). In Smith-Carrier's (2021) study, participants reported that outdoor activities enabled them to learn new things. Finally, an improvement in long-term memory, language skills, and spatial skills was observed for participants who had free access to the gardens compared with those who had restricted access (Liao et al., 2020). On the other hand, several studies reported a lack of change following the realization of outdoor activities. Indeed, there was no change in cognitive abilities when participating in an exercise circuit (Levinger et al., 2022), a rice-growing program (Ura et al., 2021), or an activity involving access to a garden (Gueib et al., 2020).
Effects on Decision-Making and Functional Autonomy
Finally, two studies found positive effects in relation to autonomy. On the one hand, with regard to decision-making autonomy following outdoor activities, participants reported a sense of control (Mapes, 2012) and competence (Ross et al., 2024). With regard to functional autonomy, all (100%) participants who were encouraged to visit the enriched gardens, which are gardens with stimulation modules, showed an increase in functional independence compared to 24% of participants who visited conventional sensory gardens (37% worsened; 39% unchanged) and only 10% of participants who were not encouraged to visit the gardens (13% worsened; 77% unchanged) (Bourdon & Belmin, 2021). Enriched gardens were co-designed by seniors’ residence staff and an architecture team (e.g., washable canvas for paintbrushes, mirrors and colored pyramid prisms, pyramidal constructions of tactile, olfactory, and visual effects, bars for exercises, slopes and obstacles crossing, outdoor musical instruments).
Summary of the Results
Analysis of the results of the studies included in this scoping review shows positive effects of most outdoor activities on behaviors, symptoms, quality of life, autonomy, and cognitive functioning in older people with MNCD, but failed to identify common characteristics of outdoor activities associated with these positive effects. Regardless of the type, context, duration, frequency, or location of the outdoor activities performed, all the studies reviewed reported a positive effect on at least one of the MNDC consequences studied.
Discussion
This scoping review identified and described the characteristics of outdoor activities and their effects on the behaviors, symptoms, quality of life, autonomy, and cognitive functioning of people with MNCD. The most frequent characteristics of the outdoor activities identified that showed positive effects were: 1) activities carried out in a garden; 2) active activities; 3) activities offering the choice of being carried out in a group or individually; 4) activities lasting less than an hour; and 5) activities taking place in the participants’ place of residence. Positive effects of outdoor activities on mood were reported in the majority of studies. Several studies also reported improved cognitive functioning, increased well-being, and reduced agitation. This scoping review also found that different types, contexts, frequencies, duration, or locations of activities are associated with beneficial effects on at least one of the consequences of MNCD, i.e., behaviors, symptoms, quality of life, autonomy, or cognitive functioning.
Firstly, both active and inactive activities show benefits in terms of the five main consequences of MNCD named above. However, more studies used active activities which, as in the general population, constitute physical activity which is largely recognized to bring positive effects on health, well-being (Cedervall et al., 2015) and mood (Junge et al., 2020). Even just walking, a generally free and accessible physical activity, leads to an improvement in mood and a reduction in BPSD (Abraha et al., 2017; Brett et al., 2016; Souto-Barreto et al., 2015).
Secondly, the results show that whether the activity was carried out in a group or individually, it brought benefits in terms of behaviors, symptoms, quality of life, autonomy, and cognitive functioning in people living with MNCD. On the one hand, group outdoor activities frequently imply social interactions that have shown positive effects on cognitive functioning, specifically memory (Haslam et al., 2010). Moreover, participation in a group social activity has been shown to improve well-being, reduce stress, and increase decision-making autonomy (Weinstein et al., 2023). Because in this scoping review individual outdoor activities were related to positive effects, it could be hypothesized that some people benefit more from individual outdoor activities and others benefit more from group outdoor activities. Thus, it is essential to support them in adapting or changing activities that meet their needs and interests and encourage their preserved abilities. In clinical and long terms care settings, supervised group activities are more frequently offered than supervised individual activities due to shortage of staff in the healthcare system (Flaherty & Bartels, 2019). In the context of aging of the population (Altman et al., 2016), when offering outdoor group activities, it appears important to remain vigilant for manifestations of discomfort in the group for some people, in which case, activities with individual supervision could be offered.
Thirdly, the location in which the outdoor activities take places does not seem to influence positive or negative effects on behaviors, symptoms, quality of life, autonomy, and cognitive functioning in people living with MNCD. However, the literature brings up that nearby streets are the most commonly used location for recreational activities among older adults (Giles-Corti & Donovan, 2002; Huston et al., 2003) due to the opportunities they offer (Liu et al., 2020). Older adults prefer to carry out activities close to where they live, because it saves them time and money, brings them closer to their friends and is more convenient (Hu, 2022). Furthermore, among older adults, proximity to friends for informal social activities is associated with a sense of satisfaction with life (Huxhold et al., 2014) and more positive affect. Thus, outdoor activities could be performed according to the preferences or convenience and still provide benefits. Finally, the greater the frequency with which older adults engage in activities with friends, the more positive feelings they experience.
The benefits on behaviors, symptoms, quality of life, autonomy, and cognitive functioning shown in this scoping review regardless of the individual/group basis, the location and the timing of outdoor activities implies that some characteristics suit some people more and other characteristics suit other people more. Moreover, there are positive effects irrespective to the decisional freedom offered (e.g., location, frequency, individual or group basis). However, because decision latitude in choosing activities improves functional status, psychological health, perceived health, and life satisfaction in people living with MNCD (Karademas et al., 2011; Vallerand et al., 1989; Weinstein & Ryan, 2011), efforts could be made to offer minimally a few options in the type, timing, location, or duration of outdoor activities. In fact, in clinical settings, for example in hospitals and long-term care settings, choices are rarely offered regarding the type of activity, when and where it is performed, and these are primarily determined by the organization to optimize institutional efficiency and convenience (Burack et al., 2012; Das, 2017). Moreover, for people living with MNCD, decision latitude in choosing activities improves functional status, psychological health, and perceived health (Karademas et al., 2011; Weinstein & Ryan, 2011). Finally, for people living in retirement homes, the ability to make choices is associated with a higher level of satisfaction with life (Vallerand et al., 1989).
This study highlights the benefits of outdoor activities on the autonomy, behaviors, symptoms, quality of life, and cognitive functioning of people living with MNCD. However, there is little information on the characteristics of activities that have the greatest effect on participants according to their personal characteristics (level of autonomy, behaviors, symptoms, quality of life, cognitive functioning). An important point is, because of cognitive deficits and often also physical limitations, outdoor activities should be adapted to the capabilities of the person with MNCD and sometimes benefit from the supervision of staff or a caregiver. In order to target the optimal intervention to be offered to people living with MNCD, which would enable a response to their needs in a personalized way, it would be interesting to better understand how the characteristics of the activities have an impact on the different spheres listed above. It would be interesting for qualitative research to explore the benefits of specific outdoor activities for a population with MNCD and with certain specific personal characteristics, while varying the following activity characteristics: type of activity, context (e.g., group vs. individual, presence of companions, structured vs. free activities), frequency, duration, location, and participants’ decision-making freedom. Such research would be useful in targeting the characteristics of activities to be integrated into programs for people living with MNCD, in order to obtain maximum benefits, according to their personal characteristics.
Strengths and Limitations
Methodological rigor is one of the strengths of this scoping review. Firstly, the method used is based on the steps proposed by Arksey and O’Malley (2005). Secondly, the co-validation of study selection ensures the consistency of the process. The strengths of this study also include the inclusion of qualitative, quantitative, and mixed method studies. This combination enriches understanding of the effects of outdoor activities with people living with MNCD on behaviors, symptoms, quality of life, autonomy, and cognitive functioning.
A limitation of this scoping review is the identification of studies relevant to the research question. Despite consultation with the librarian, the choice of the concept of outdoor activity in the search strategy, as well as the associated keywords, may have omitted some studies. The concept of outdoor activity is very broad and includes a wide range of activities, such as outdoor sports. In the case of activities generally practiced outdoors (e.g., hiking, gardening), they are not always specified in the title, summary, or keywords that the activity takes place outdoors. It is therefore possible that certain articles, which would have been relevant to the study, were not identified. Finally, we have not discussed the stages of different health conditions accompanied by MNCD, as well as the associated symptoms across those different illnesses.
Conclusion
This scoping review examined the benefits of outdoor activities for behaviors, autonomy, symptoms, cognitive functioning, and quality of life in people living with MNCD. Given the degenerative nature of MNCD and the current lack of curative treatments, exploring non-pharmacological interventions such as outdoor activities represents a promising avenue for maintaining and improving the condition of people living with MNCD. However, given the limited number of studies on interventions involving outdoor activities, further studies are needed to better target the specific characteristics of these activities in relation to the benefits sought. Further studies are also needed to clarify the benefits of different activity features on quality of life, behaviors, symptoms, autonomy, or cognitive functioning. Such research is essential if we are to improve the management of patients living with MNCD.
Implications for Practice
Collaborating with caregivers of people living with a MNCD is a key element to implement the practice of outdoor activities. Activities, whether active or passive, can produce one or more benefits in terms of behaviors, symptoms, quality of life, autonomy, or cognitive functioning. Everyone can benefit:
The activity bank offers options both for people whose physical condition enables them to be active and for those whose physical condition does not allow them to be. The activities can also be modulated according to the stage of MNCD.
Footnotes
Acknowledgements
The authors would like to express their sincere thanks to Florence Nadeau, librarian, at the Faculty of Medicine and Health Sciences, Université de Sherbrooke, for her help with the literature search, and to Roseline Bergeron for the translation of the article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are available on demand by contacting C. Viscogliosi.
