Abstract
Objectives
This study quantified the total time required by staff to complete intrahospital transfers (IHTs) and identified key activities and facility attributes affecting efficiency.
Background
IHTs, which involve moving patients between rooms or units, place significant demands on healthcare staff and facility resources. While previous studies have explored the impact of IHTs on patient safety and clinical efficiency, few have assessed the specific tasks and time demands on all staff members involved.
Methods
Fifty IHTs (39 between-unit, 11 within-unit) were observed at a 718-bed level-1 trauma hospital. Transfer tasks were categorized into 13 activity types. These included managing equipment, belongings, and supplies (EBS), handoff communication, and patient transport.
Results
IHTs required a mean of 77 min of staff time, 53 min (75%) of which was nursing time. EBS management accounted for the largest share of transfer time, followed by handoff communication. Transfers with an increase in acuity level required more staff and additional total time. Elevator use was associated with a significant increase in nursing time. Issues that added to transfer time included miscommunication about room readiness and the need to acquire or transport specialized equipment.
Conclusions
Streamlining EBS processes, optimizing staffing for acuity-related transfers, and improving elevator availability could reduce IHT times and alleviate workload on nurses. Enhanced coordination during shift changes, better communication about room readiness, and support for non-clinical tasks offer further opportunities to improve efficiency. These findings underscore the role of facility design and operations management in enhancing hospital efficiency, reducing nursing burden, and improving patient care.
Keywords
Introduction
Intrahospital transfers (IHTs), which involve transporting patients from one room to another within a hospital (Blay et al., 2017), are frequent occurrences that have been extensively studied due to their substantial impact on patient safety and hospital operations. Hendrich and Lee (2005) identify three key reasons for patient relocation inside the hospital: the technological capacity of the unit, the clinical expertise of the caregiver, and the nursing hours allocated per patient per day. A study by Bristol et al. (2020) has determined that patients undergo an average of 2.4 room transfers during their hospitalization, and approximately 96% of individuals undergo at least one transfer during their hospitalization. Additionally, a 2004 study revealed that nursing units were transferring or discharging 40% to 70% of their patients daily, placing a substantial burden on nurses to manage this high turnover and the associated care transitions (Hendrich et al., 2004).
IHTs can cause complications for both patients and healthcare facilities. These transfers are linked to respiratory (Waydhas et al., 1995) and cardiovascular (Taylor et al., 1970) complications. Additionally, IHTs can result in higher medication errors (Tully et al., 2019), increased patient falls (Kok et al., 2021), and increased infection rates (Boncea et al., 2021), all of which negatively affect the quality of care and operational efficiency.
Transfers significantly affect nurses’ perceived workload, as measured by end-of-shift surveys (Ivziku et al., 2022). Blay et al. (2017) demonstrated that nurses spend a considerable amount of time on transfers. However, few studies have considered the time demands placed on other hospital staff, such as nurse assistants, technicians, and administrative personnel, during IHTs. These time pressures not only affect those directly involved in the transfer, but also the remaining unit staff, who must manage while the transferring team is occupied. This challenge is especially critical in understaffed units or when intensive care unit (ICU) nurses must leave their specialized environment to assist with transfers. Additionally, Hendrich and Lee (2005) examined the cost implications of IHTs, focusing on overall process efficiency. Building on their work, modern studies could explore how technological advancements, such as real-time communication tools and automated bed management systems, have further improved transfer efficiency and cost-effectiveness.
In addition to negatively affecting patient outcomes and consuming staff time, IHTs increase demand for facility resources. Facility designers can plan for these demands, minimize their occurrence, and mitigate their effects on patients. For example, when a patient is transferred to another room, two rooms become unavailable until the origin room is cleaned. With an average of 2.4 transfers per patient (Bristol et al., 2020), facility planners must consider the effect of these additional rooms being unavailable on a large scale. Furthermore, when an IHT involves a change in acuity or clinical specialty, patients receive care that may be insufficient or unnecessarily costly while waiting for the transfer to the appropriate resource. Facility designs might prevent the need for some IHTs by providing more specialized resources (Magazine et al., 2021) or acuity-adaptable environments (Hendrich et al., 2004). Accurate cost estimates due to preventable IHTs could help designers and executives make informed decisions about the costs and benefits of these resources.
Facility design may also contribute to the efficiency and safety of IHTs. Ulrich and Zhu (2007) have highlighted the architectural implications of IHTs, noting that there are key design considerations that can affect IHT outcomes. For instance, longer transport durations are linked to higher complication rates, underscoring the need for hospital layouts that minimize transfer times, especially in high-acuity areas such as ICUs and operating rooms. Additionally, inadequate space and congestion can delay transfers, making it important to design sufficiently large rooms and corridors (Matz et al., 2019). Elevator use can also affect transfer times, especially in high-rise layouts, if elevator service does not meet demand during high traffic times. More research is needed to quantify patient and facility attributes that could be influenced by facility designs to reduce IHT times. The primary objectives of the present study were to quantify the overall time required by all relevant staff to accomplish an IHT, as well as to identify common tasks and their associated time demands. A secondary objective was to identify attributes of the patient and transport route that affect the time to complete an IHT.
Longer transport durations are linked to higher complication rates, underscoring the need for hospital layouts that minimize transfer times, especially in high-acuity areas such as ICUs and operating rooms.
Methods
The study was conducted at a 718-bed, Level 1 trauma center spanning approximately 2.4 million square feet across three towers. The facility has a total of 21 elevators, six of which are designated exclusively for patient transport, equipment movement, and staff use. Among these, one is a larger trauma elevator that requires a key for access.
Fifty complete IHTs (39 between unit, 11 within unit) were observed by at least one of the same two observers. At a 718-bed level-1 trauma hospital. Five additional observations were excluded from the analysis due to discontinuity or change in the destination during the IHT.
Before formal data collection, seven IHTs were observed as pilots to categorize subtasks and establish consistent measurement methods. These preliminary observations were considered together with the classification by Blay (2017) to identify the 13 categories in which each activity would be classified (Table 1). Most of these tasks were easy to categorize, and the start and end times were straightforward to define, except for gathering items that must be moved with the patient. Gathering items included disconnecting or connecting equipment, organizing patient belongings, and gathering supplies. Because of the fluidity and rapid transition of tasks when gathering items, the management of equipment, belongings, and supplies (EBS) was combined into a single task called EBS. Figure 1 provides an overview of the transfer process, organized around three main phases: origin room, patient movement, and destination room. It illustrates the range of activities that may occur at each stage of the transfer.
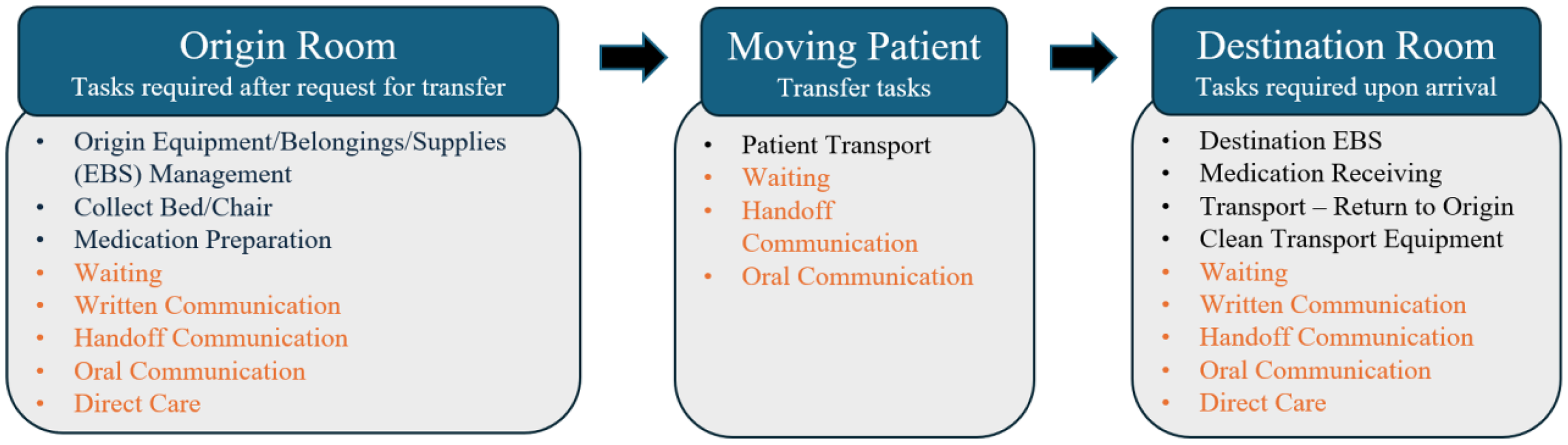
Overview of the Patient Transfer Process, Organized Around Three Main Phases: Origin Room, Patient Movement, and Destination Room. The Sequence of Tasks Does Not Follow a Fixed Order, and Tasks Highlighted in Orange May Occur at Multiple Stages. The Figure Represents the Breadth of Observed Activities, Though Not All Tasks Occurred in Every Transfer.
The Identified Subtasks in IHTs and Their Definitions.
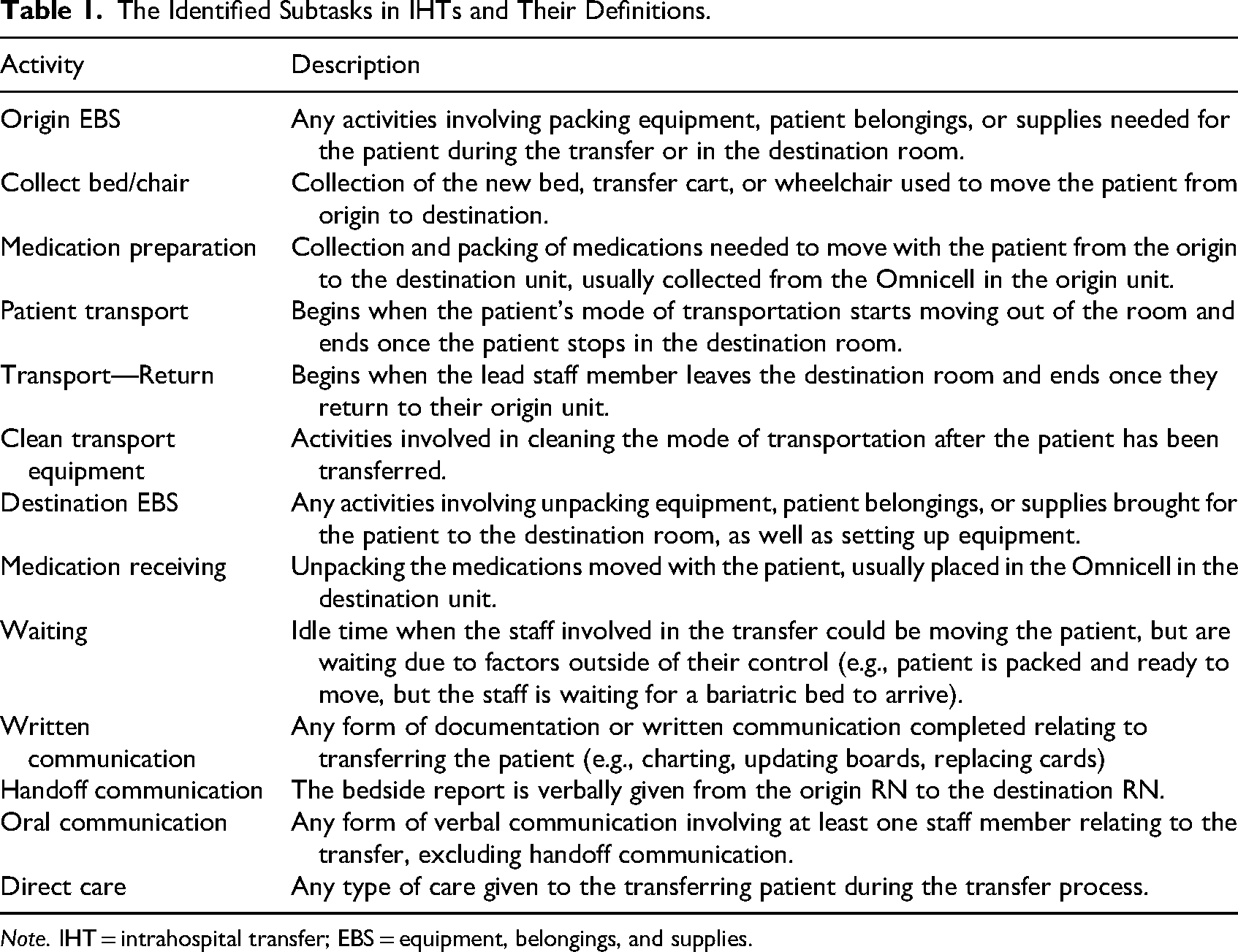

Note. IHT = intrahospital transfer; EBS = equipment, belongings, and supplies.
For the hospital in this study, a transfer is typically initiated when a provider (e.g., a physician) requests a change in care in the electronic health record (EHR). This change in care may involve an upgrade or downgrade in acuity, or a change to a unit with a different specialty. A within-unit transfer, often requested by a nurse, may also occur for a variety of reasons that include moving a patient to a room with a ceiling lift, to a room near the nurse station, or to vacate a room requiring maintenance. After the request is made in the EHR, the Central Transfer and Communications Center (CTaC) assigns a new room that meets the needs of the patient. This room may be clean and ready, unoccupied and unclean, or even occupied by a different patient who will soon be discharged. The status of the destination room is displayed on a monitor at the nurse station of the origin unit. After the assigned room is designated as clean by an Environmental Services (EVS) staff member, the nurses in the origin unit can begin the transfer process. Staff in the origin unit gather medical equipment, patient belongings, supplies, and medications. In many cases, the bed from the origin room will travel and remain with the patient in the destination room, and the clean bed in the destination room will be returned to the origin room. However, as is common in many facilities, ICU beds in this hospital remain in the ICU and are not used in lower acuity units. This means when transferring from the ICU to a lower acuity unit, staff must first retrieve the clean bed from the destination room to transport the patient, or use a wheelchair or cart. Unlike the beds, which are stored in the central supply, wheelchairs and transfer carts are stored on the units. When the patient has reached the destination room, staff reconnect the medical equipment, unpack patient belongings, and perform the handoff communication.
Before each IHT, observers from the research team monitored the status board of the bed assignment system to confirm the destination bed was still being cleaned and that transfer tasks had not begun. Staff were shadowed for all observable elements of the transfer process from the origin to the destination unit. In addition to documenting the time that staff were involved in the transfer, the following contextual data about the transfer were also collected:
− Origin room and unit: The room number and unit type the patient is leaving. − Destination room and unit: The room number and unit type to which the patient is moving. − Origin nurse workload (1–10): A self-assessment, queried after the IHT, of nurse workload for the shift preceding the transfer on a scale of 1 to 10, with 10 being the most chaotic day. − Number of patient belongings (above average/average/below average): A subjective question posed to the origin-nurse to reflect how many personal belongings each patient had during the transfer. − Patient attributes: Specific characteristics of the patient noted in the bed assignment system that may affect their transfer time (e.g., isolation precautions, bariatric, monitoring by a sitter, etc.).
When the transfer began, the observers recorded the time and staff involved for each transfer-related activity. Activities not related to the transfer were not recorded or counted toward the transfer. The transfer was deemed complete, and observation ended when the origin-nurse returned to their unit after moving the patient.
Data Analysis
Staff time was defined as the sum of the time contributed to transfer-related tasks by all staff members (e.g., nurses, techs, unit secretaries, etc.) across all activities. Because nursing resources can be particularly in demand, nurse time was separated and then calculated as the sum of time spent specifically by nurses. The independent variables considered for this study, and recorded in the data sheet per observation, are included in Table 2.
The Independent Variables Considered in the Step-Wise Regression Analysis for Staff Time and Nurse Time.
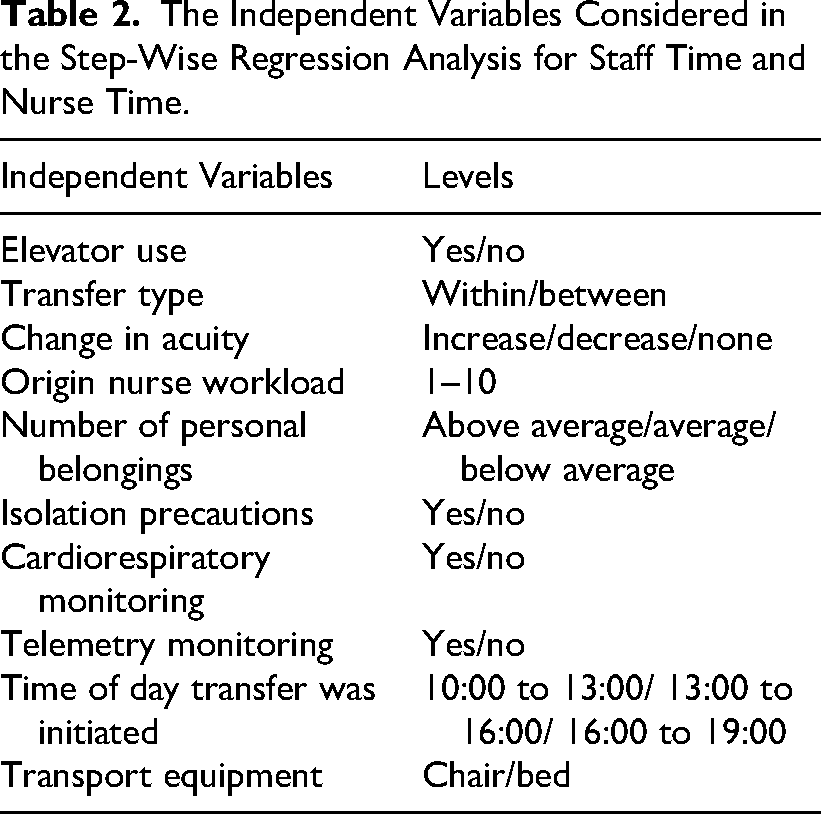

JMP (v16.0.0, SAS, NC, USA) was used for statistical analysis. A backward stepwise regression approach was used to identify the most influential variables affecting staff time and nursing time, with a stopping rule based on p-value thresholds (probability to enter = 0.25, probability to leave = 0.1). Following this preliminary selection, the identified variables were subjected to a standard least squares regression analysis in JMP to determine which ones had significant main effects on staff time and nursing time. In addition to the predefined times and independent variables, we also identified pain points and nonstandard workflows.
Results
Table 3 presents the times spent on various transfer-related activities by staff members and registered nurses (RNs), along with the percentage of total time allocated to each activity. The mean total time spent by all staff members for each transfer was 77 min. For most IHTs, this total staff time tended to exceed the elapsed time of the observation, reflecting the involvement of multiple team members of varied roles. Mean nurse time was 53 min, or 75% of the total staff time required for the transfer. The subtask requiring the most time was managing patient belongings, supplies, and equipment, followed by handoff communication.
Time Spent by all Staff Members and RNs Across the Transfer-Related Activities.
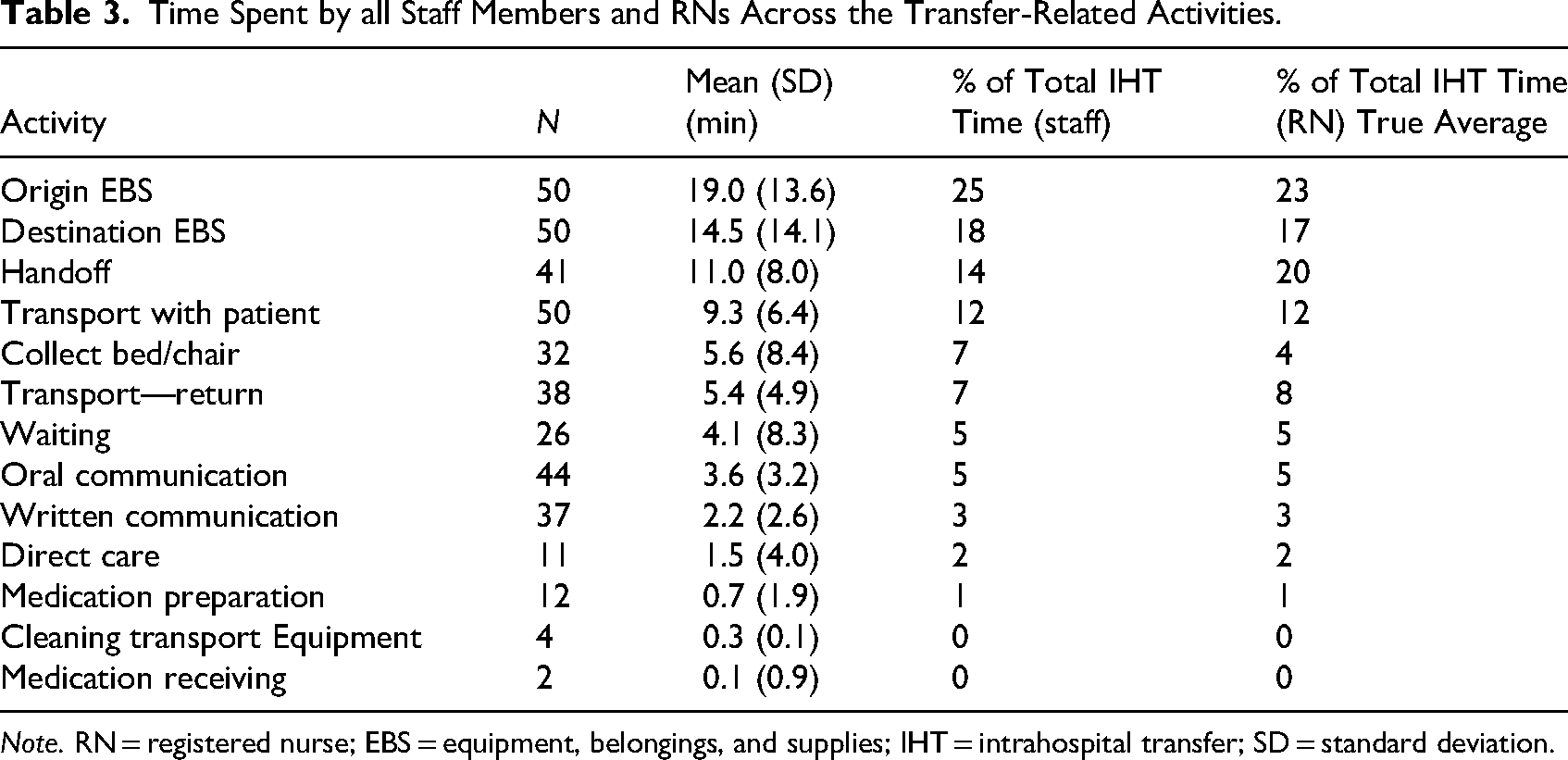
Note. RN = registered nurse; EBS = equipment, belongings, and supplies; IHT = intrahospital transfer; SD = standard deviation.
The result of the regression analysis for staff time and nurse time (see Tables 4 and 5, respectively) indicated that a change in level of acuity significantly affected staff time (p = 0.03) and nurse time (p < .0001) (see Figure 2). The post-hoc Tukey-HSD test further revealed a significant increase in staff time (p = 0.03, mean difference = 48.12 min) and nurse time (p < .0001, mean difference = 74.16 min) from the no change in acuity level to increase in acuity level conditions (i.e., moving from progressive care unit [PCU] to ICU).
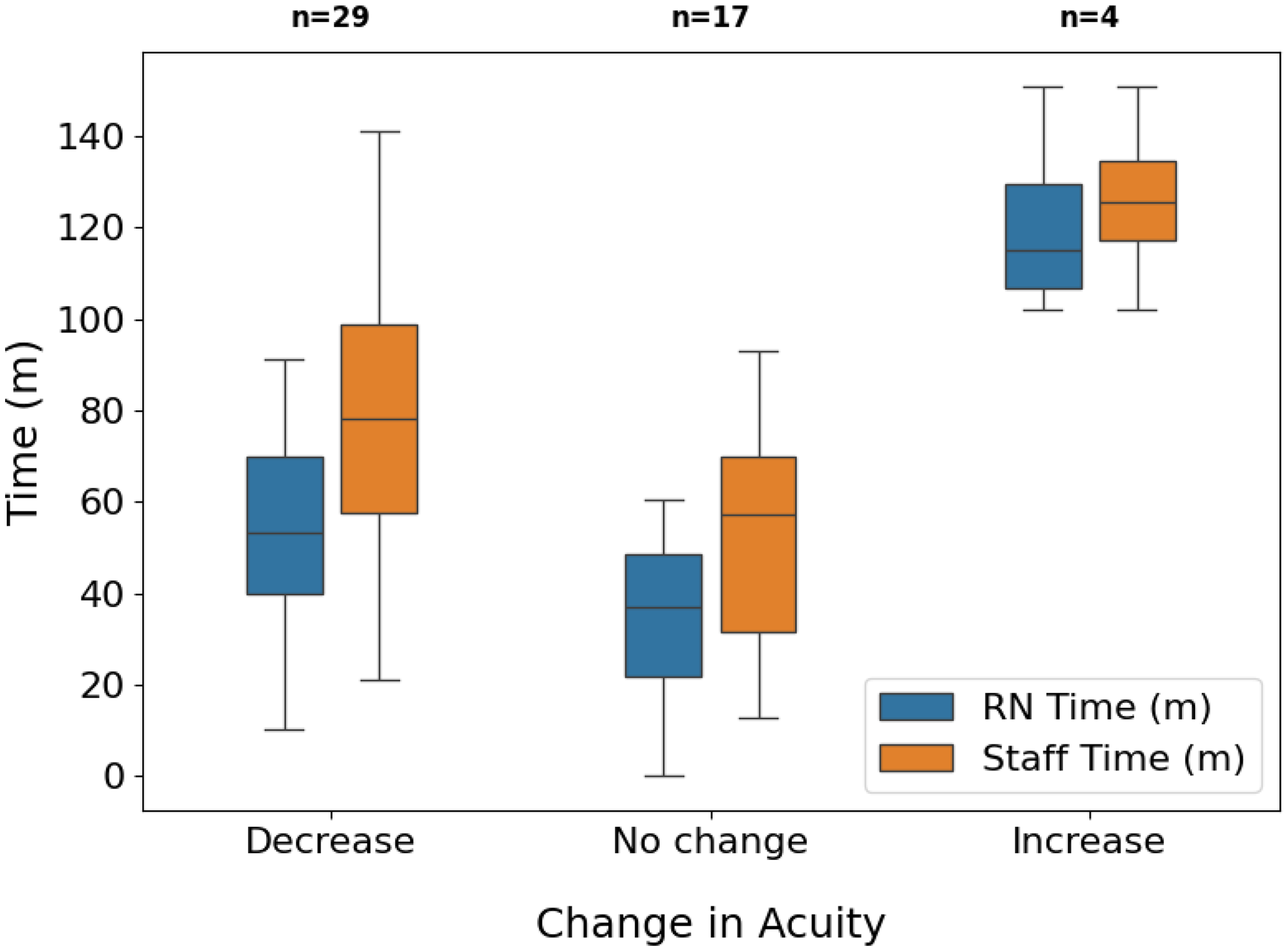
Time (min) Versus Change in Acuity for Staff Time and RN Time (The Box Plot Visualizes the Distribution of Time Spent, With Whiskers Showing the Minimum and Maximum Values, Box Ends Representing the IQR, and the Central Line Indicating the Median).
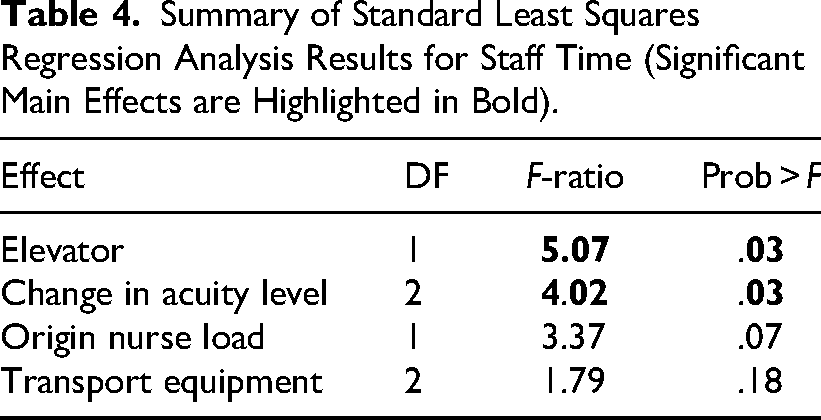
Summary of Standard Least Squares Regression Analysis Results for Staff Time (Significant Main Effects are Highlighted in Bold).
Summary of Standard Least Squares Regression Analysis Results for Nursing Time (Significant Main Effects are Highlighted in Bold).

Additionally, the regression analysis indicated that the use of an elevator was associated with significantly more staff time and nursing time. Mean times without and with elevator use were 50 and 89 min for all staff (p = 0.03), and 27 and 65 min for nurses (p = 0.0006), respectively (see Figure 3). This means that a transfer requiring a change in floors (which would typically include elevator wait times and the need to exchange beds) would take significantly more staff time to complete compared to a transfer between units on the same floor or a room exchange within the same unit.
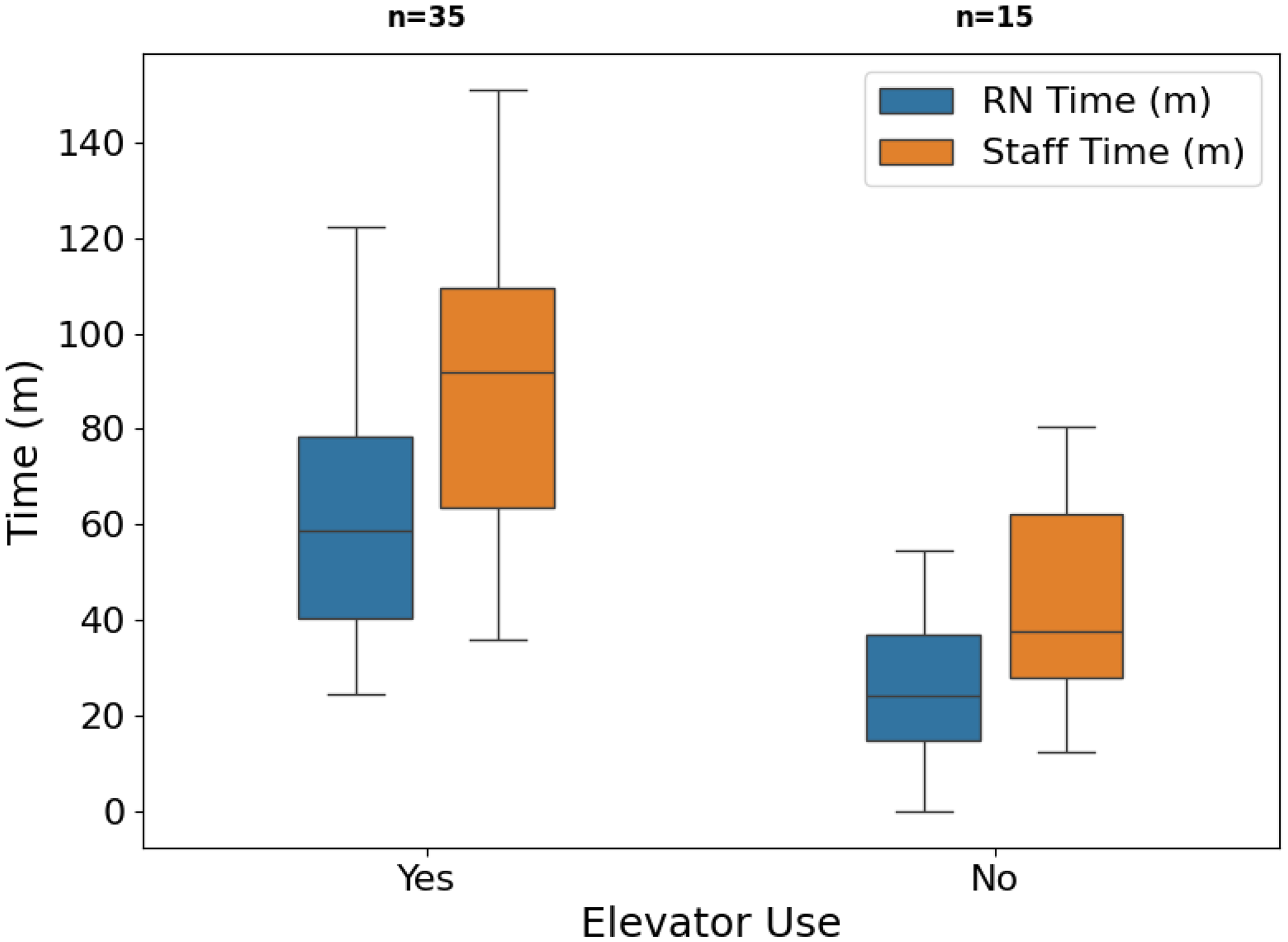
Time (min) Versus Elevator Use for Staff Time and RN Time (The Box Plot Visualizes the Distribution of Time Spent, With Whiskers Showing the Minimum and Maximum Values, Box Ends Representing the IQR, and the Central Line Indicating the Median).
Discussion
This study aimed to quantify the impact of IHTs on hospital operations by quantifying time requirements, identifying key subtasks, and investigating the factors that significantly impact staff time during transfers. The results indicate that greater staff time was required for transfers involving an upgrade in acuity, likely due to the need for more clinical staff to accompany the patient in case of sudden deterioration during the transfer. Additionally, hospital policy mandates that specially trained staff members be present for all upgrades. This added coordination ensures a safe transfer but naturally increases total staff time. Moreover, the need to handle more medical equipment and communicate more information at handoff could have further contributed to the increased time demands of an upgrade in acuity.
Greater staff time was required for transfers involving an upgrade in acuity, likely due to the need for more clinical staff to accompany the patient in case of sudden deterioration during the transfer.
The significant increase in staff time and nurse time due to elevator use highlights the impact of vertical transportation on hospital efficiency. A study comparing stairs and elevator use in hospitals found that elevator use added an average of 15 min to staff travel time per workday, primarily due to waiting for elevators (Shah et al., 2011). Additionally, elevator wait times can vary significantly depending on the time of day and week. For instance, one study found that on weekday mornings, elevator travel times across six hospital floors can range from 1.1 to 6.9 min in early hours of the day (Shah et al., 2011), introducing unpredictability to staff schedules and causing delays in patient care.
There are several possible reasons why travel times reported by previous studies were <38 min of increased nursing time associated with elevator use in the current study. The vertical layout of the facility and the limited number of elevators exclusively dedicated to patient transport may have contributed to long elevator wait times. Furthermore, because multiple staff were often involved in IHTs, the contribution of elevator delays was multiplied across the number of staff involved. Finally, elevator use tended to occur most often in conjunction with a change in acuity. Although both elevator use and change in acuity were significant in the regression model, it is challenging to interpret the relative contributions of each factor. In many cases, an increase in acuity would require wait times due to elevator use, but also more staff and more work requirements.
The vertical layout of the facility and the limited number of elevators exclusively dedicated to patient transport may have contributed to long elevator wait times. Furthermore, because multiple staff were often involved in IHTs, the contribution of elevator delays was multiplied across the number of staff involved.
The effect of elevator use on staff time requirements emphasizes the need for hospitals to explore solutions such as proper capacity planning (Ng & Lin, 2016) to reduce wait times, improve staff productivity, and enhance overall hospital operations. Additionally, the choice between a high-rise building, which relies heavily on elevators for vertical transport, and a low-rise, horizontally designed structure, which minimizes elevator use, can greatly affect operational efficiency and patient care (Ulrich & Zhu, 2007). However, a horizontal layout (e.g., exclusively one floor) that reduces reliance on elevators can increase the distance required for transfers between units, highlighting a tradeoff between elevator usage and walking distances.
Effective hospital design and staffing strategies are critical for enhancing operational efficiency. Hendrich et al. (2004) demonstrated this by transitioning a large coronary ICU from traditional two-bed rooms and a transfer-dependent care model to acuity-adaptable single-bed rooms with an optimized staffing approach. This redesign resulted in a 90% reduction in patient transports and fewer nursing hours required per patient bed. Additionally, a proximity-based redesign of the Heart Hospital at Tampere University Hospital reduced patient transfer distances by 33% (Karvonen et al., 2022), illustrating how optimized unit placement can enhance transfer efficiency and streamline workflows. In our study, transfers between ICU and PCU units made up 30 out of 50 total transfers, highlighting the opportunity in considering unit proximity. For example, two transfers originating from the same ICU unit revealed how differences in layout can significantly affect efficiency. Both transfers are depicted in Figure 4: the first transfer, shown in orange, occurred on the same floor, resulting in a shorter and more direct route (a total of 65 paces between the room of origin and destination). In contrast, the second transfer, illustrated in blue, involved moving the patient to a PCU on a different floor (a total of 351 paces between the room of origin and destination). This required the use of an elevator, which increased both the transfer distance and delays due to elevator wait times. Consequently, the patient transport time increased significantly, from 3 min for the same-floor transfer to 18 min for the transfer to a different floor. Interestingly, when researchers asked nurses why they did not use the dedicated-staff-only elevators around the corner from the public elevators, one nurse replied, “everyone knows those staff elevators are as slow as Christmas.”
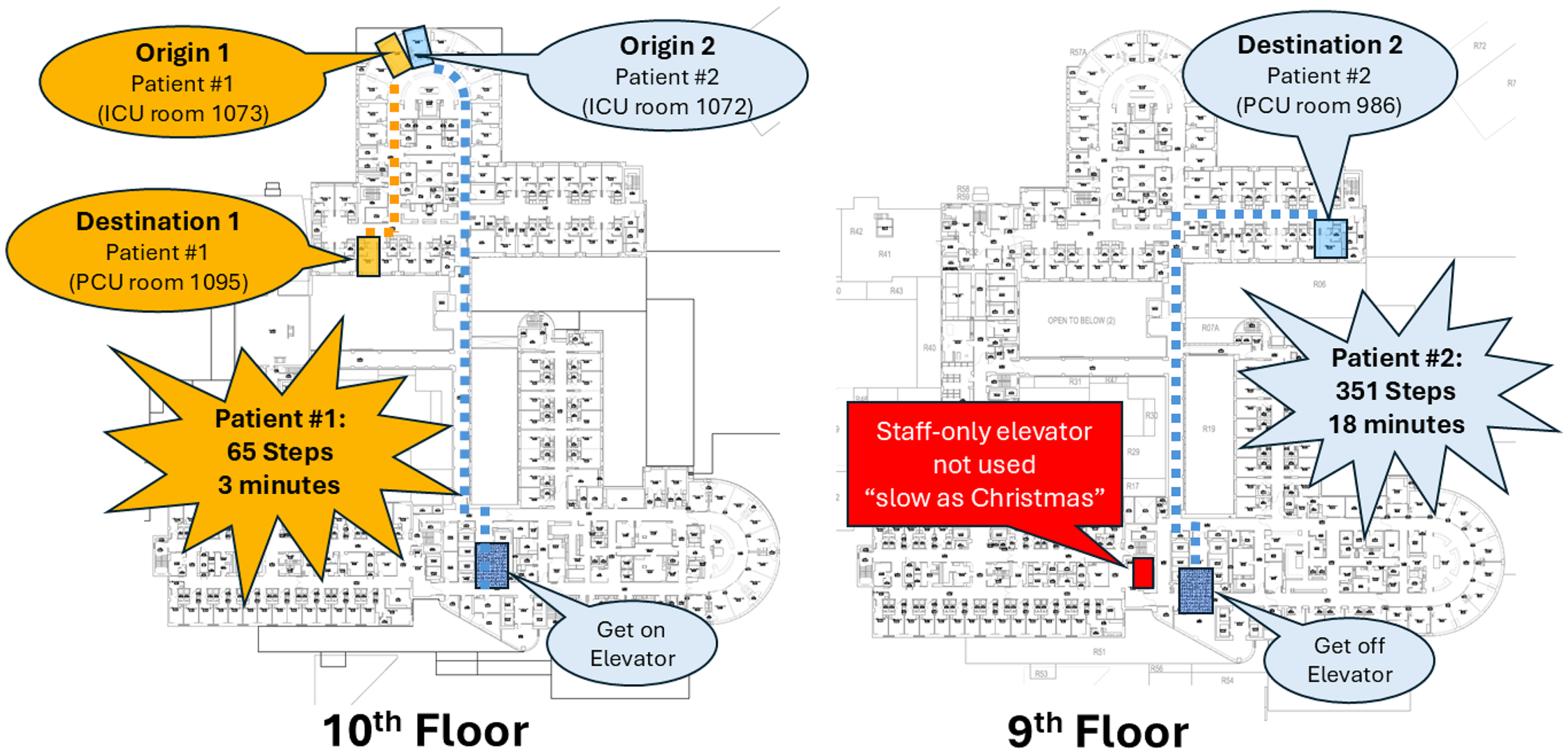
Comparison of Two ICU-to-PCU Transfers Originating From the Same ICU Observed in Our Study. In Transfer 1 (Orange), the Transfer Occurred on the Same Floor, Resulting in a Shorter Transfer Distance. In Transfer 2 (Blue), the Patient Was Moved to a PCU on a Different Floor, Which Increased Both the Transfer Distance and Patient Transport Time Due to Elevator Usage and Associated Delays.
In addition to measurements of staff time, many pain points and nonstandard workflows were observed that provide an opportunity for improving the IHT process. When transfers were scheduled during shift changes, outgoing nurses struggled to find the destination nurse for handoff communications, increasing the time of the transfer and the risk that critical patient information was not communicated. Because specialized ICU beds were not allowed to remain in other units to which patients were transferred, ICU staff spent more time off the floor returning ICU beds to their units or searching for a clean bed if the destination room did not have one present. The transport of bariatric beds was particularly time-consuming, and their nonstandard size complicated maneuverability through certain doorways and elevators. When transferring isolation patients, a cart containing personal protective equipment needed to be transported separately, and staff donned and doffed personal protective equipment, often requiring more staff and time. Lastly, in four instances, a soiled room was incorrectly communicated as clean and available, further increasing staff time to complete a transfer.
The transport of bariatric beds was particularly time-consuming, and their nonstandard size complicated maneuverability through certain doorways and elevators.
Limitations
There are several potential activities contributing to IHTs that may not have been fully captured in this study. Certain tasks, such as medication receiving (n = 2) and cleaning transport equipment (n = 4), were observed infrequently, limiting our understanding of their overall impact. Furthermore, activities known to occur, such as retrieving charts, updating medical records, cleaning medical equipment, or redirecting virtual sitters, were difficult to consistently document. The staffing estimates in this study also do not include the time required for EVS personnel to clean the room. It is also possible that other unobserved activities carried out by CTaC, pharmacy, or other personnel contributed to the transfer process. The current study was also limited to the transfer devices and environments specific to this facility. Transport time may be reduced when using transport equipment not considered in this study, such as beds with a powered drive. Transport time may be increased by navigating ramps, uneven surfaces, or congested hallways. Taken together, these limitations suggest the staff times documented in this study could be underestimated. There may be unidentified or unmeasured factors not included in the observations that influence the efficiency and complexity of patient transfers, underscoring the need for further comprehensive observation and analysis.
Future Work
Future work could focus on conducting studies with more patient transfers across multiple facilities to enhance the robustness and generalizability of findings. These studies could also include hospitals with diverse architectural layouts and elevator configurations to better understand how these factors influence operational efficiency and patient care. Additionally, variations in elevator designs, such as dedicated staff-only elevators versus shared patient and visitor elevators, could be analyzed to assess their impact on transfer times and workflow efficiency. Such assessments of elevator design should consider acuity level and the number of staff involved. Moreover, future research could include activities related to patient transfers for specialties such as EVS, pharmacies, and CTaC, offering a more holistic perspective on transfer-related workflows across the hospital environment.
Conclusion
This study quantified the significant staffing demands of IHTs and the time dedicated to transfer-related activities. On average, the total time spent by staff on each transfer was 77 min, with nurses contributing 75% of this time. Of the transfer-related activities, managing patient belongings, supplies, and equipment took the most time, followed by handoff communication. Transfers involving an increase in acuity level required more time due to the additional staff needed. The use of elevators also contributed substantially to delays. Challenges were observed that included delays during shift changes, issues with specialized equipment, and miscommunication of room readiness. These findings highlight opportunities for refining hospital design and enhancing scheduling to improve overall hospital efficiency and patient care.
Implications for Practice
Nurses contributed 75% of the total time spent on transfers, suggesting opportunities to reduce their workload that could include delegating non-clinical tasks or introducing dedicated support staff for transfer-related activities.
Managing patient belongings, supplies, and equipment took the most time during transfers, suggesting a need for streamlined processes to reduce this burden.
Elevator use during transfers significantly increased total staff time from 50 to 89 min and nursing time from 27 to 65 min, likely because they were associated with higher-acuity transfers and wait times experienced by multiple staff.
Transfers involving an increase in acuity level took more staff time due to the additional staff required, emphasizing the importance of planning for these scenarios.
Delays caused by elevator usage, shift changes, and miscommunication of room readiness highlight opportunities to improve coordination and scheduling.
Footnotes
Acknowledgments
The authors gratefully acknowledge Harsh Sanghavi for assistance with planning and data collection, as well as Laurie Fuchs and Constance Aaron for their help in planning data collection and interpretation of results.
Ethical Approval and Informed Consent Statements
The study was approved by the Carilion Clinic Institutional Review Board (IRB) under protocol number IRB-24-2206.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was partially supported by Baxter Healthcare Corporation.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data are not publicly available.
