Abstract
Keywords
Introduction
In 2020, NAFLD was officially renamed metabolism-associated fatty liver disease (MAFLD) and its definitive diagnosis was clearly stated to be a pathology characterized through hepatic lipid accumulation with metabolic disorders.1,2The pathogenesis of MAFLD is closely related to “multiple strikes,” involving multiple processes such as insulin resistance (IR), lipotoxicity, oxidative stress and endoplasmic reticulum stress. 3 A recent study found that the global prevalence of MAFLD is 39%, 4 a cross-sectional study of 139,170 subjects in China according to newly defined diagnostic criteria through Chen et al 5 found the prevalence of MAFLD to be 26.1%. MAFLD strongly associated with advanced age, obesity and other factors. 6 With the urbanization of human society, MAFLD also tends to be younger and could induce other chronic metabolic diseases, 7 MAFLD seriously jeopardizes human health and brings a huge burden to society and families. However, there is no specific drug for MAFLD, and lifestyle intervention is the first line of treatment, taking into account prophylaxis and therapy for metabolic cardiovascular conditions and hepatic inflammatory injury.
Huanglian Jiedu Decoction (HLJDD), recorded in “Zhouhou Beiji Fang,” is a representative formular of clearing heat and detoxifying. The formula is composed of Huanglian (Coptis chinensis Franch), Huangqin (Scutellaria baicalensis Georgi), Huangbo (Phellodendron amurense Rupr), and Zhizi (Gardenia jasminoides Ellis). Recent pharmacological investigations found that HLJDD has a series of functions such as anti-inflammatory, antioxidant, anti-tumor and immune regulation. 8 However, current studies have only demonstrated that HLJDD could improve disorders of glucose and lipid metabolism, but its mechanism has not been clarified. This research project focuses on the preliminary investigation of the target and molecular mechanism of HLJDD for treating MAFLD through network pharmacology combined with molecular docking technology, validated through animal pharmacodynamic studies and cellular experiments.
Methods
Targets of Action and Main Active Components for Huanglian Jiedu Decoction
The chemical compositions of the four Chinese herbs of HLJDD were searched in TCMSP2.3 Pharmacological Analysis Platform for Traditional Chinese Medicine Systems (https://old.tcmsp-e.com/tcmsp.php), TCMSP allowed for retrieving additional targets for active components obtained within previous step, and the screening was completed through mapping the targets to standard gene names within UniProt (https://www.uniprot.org) mapped targets to standard gene names.
Targets for Huanglian Jiedu Decoction for the Treatment of MAFLD
Using “metabolism-related fatty liver disease,” “NAFLD,” and “MAFLD” as keywords, we searched the GeneCards5.0 database for potential targets for MAFLD. After searching the GeneCards5.0 database for the potential targets of MAFLD, combining the targets within disease database, deleting the duplicates to the MAFLD targets, and the intersection of MAFLD target genes and HLJDD principal component targets was screened, key targets for HLJDD for treating this condition were finally obtained.
Network Construction of Target Interactions
Construction of a Target Network Concerning Principal Components in Huanglian Jiedu Decoction
Principal components for HLJDD and their action targeted networks were developed through Cytoscape 3.7.2 package. Throughout the network, the nodes are the target proteins of the drug during disease intervention, and the edges represent the interactions across drug components and these target proteins. Topological parameters of the interaction network were calculated using the “Analyze Network” function in Cytoscape, and the important active ingredients of HLJDD for treating MAFLD were identified according to the degree of connectivity of the nodes, and increased node value raised active ingredient importance.
Protein Interaction Networks and Important Targets
The targets of HLJDD for treating MAFLD were imported into STRING11.0 platform, and the species type was set as “Homo sapiens,” the confidence level was set as “0.9,” and all other parameters are filtered through default settings. Finally, the target protein interaction information files obtained after screening were inserted within Cytoscape to construct PPI networks.
KEGG Pathway Annotation and Enrichment Analyses
The drug–disease intersection targets were imported within DAVID 6.8 (https://david.ncifcrf.gov), with species selected as “Homo sapiens,” which was then subjected to KEGG pathway annotation and enrichment analysis, and the results were visualized.
Molecular Docking
3D frameworks for AMPK and mToR proteins were downloaded from the PDB database, and the proteins were dehydrated and hydrogenated through AutoDock Tools 1.5.6 package. Active ingredients of AMPK and mToR were obtained from TCMSP database depending upon composition of HLJDD (International Compound Identifier, the InChIKey of each compound is unique), and were searched through PubChem. InChIKey to obtain the SDF format of the 3D structure of the active ingredient of the drug, and the format conversion of mol2 was performed using OpenBabel2.4.1. The processed proteins and active ingredients were molecularly docked through AutoDock Vina, and the binding capacity below 0, indicating that the ligand and receptor could spontaneously bind, and these results were analyzed and visualized using Pymol 2.4.0.
Animal Pharmacodynamic Study
Laboratory Animals and Drugs
Sixty male SD rats of SPF grade are all weighing (180 ± 20) g. These rats were procured through Changsha Tianqin Biotechnology Co, License No. SCXK (Xiang) 2019-0013; HLJDD was purchased from Jiangyin Tianjiang Pharmaceutical Co. Ltd of Sinopharm Group, Su 20160102; high-fat diet was purchased from Suzhou Shuangshi Experimental Animal Stall Food Technology Co., Ltd, License No. Su Feeding License (2017) 05005(high-fat diet was made up of 20% lard, 4% sugar, 2% powdered milk, 1% cholesterol, and 73% normal diet). The study protocol was approved by the Ethics Committee of Hainan Medical University, approval number: HYLL-2021-009.
Preparation of Pharmaceutical Solution
The human clinical dose (Drug1) was converted into the equivalent dose for rats (Drug2) according to the body surface area, the formula:
Establishment of Rat Model
Sixty male SD rats were fed adaptively for one week and divided into normal group (N group, n = 10) and model group (MAFLD group, n = 50) according to random number table method. The rats in group N were fed with ordinary diet, the rats in the MAFLD group were fed high-fat diet and all rats were given free water. To detect whether the model of MAFLD was built successfully, we detected the pathological change of a rat’s liver after 4 weeks of modeling by HE and oil red O staining. HE staining results showed that there is an abnormal arrangement of hepatocytes, small vacuoles in some cells, and a large number of vacuole-like structures around liver cells in the model group compared with the control group. In addition, Oil red O staining results showed a large amount of oil red O precipitation with a large number of lipid droplets in the liver of the model group compared with the control group. The above results indicate that the animal model of MAFLD has been established successfully (see Appendix Figure 1 for details). Rats in MAFLD group were randomly divided into model group (M, n = 10), HLJDD low-dose group (HL-L, n = 10), HLJDD medium-dose group (HL-M, n = 10), HLJDD high-dose group (HL-H, n = 10), and silybin group (SF, n = 10). The feeding of all groups remained unchanged. HL-L group, HL-M group, HL-H group, and SF group were administered the corresponding drug solution (10 mL/kg/d) by gavage for 6 weeks, N and M groups were administered the same volume of normal saline.
Specimen Collection and Processing
After modeling was completed, rats were deeply anesthetized with 1% sodium pentobarbital given at 4 ml/kg, and abdominal aortic blood and liver tissue were taken. The rat serum was allowed to stand for 30 minutes and then centrifuged (3000 rpm; 10 minutes) and the supernatant was poured into EP tubes. The treated serum and part of the liver were stored in an ultra-low temperature refrigerator at −80 °C for subsequent experiments. Part of the liver was soaked in 4% paraformaldehyde and stored at room temperature.
Liver HE Staining
After the fresh tissue was treated with 4% paraformaldehyde overnight, it was cleaned with PBS buffer, paraffin embedded, sliced, and then stained through HE.
Liver Oil Red O Staining
Fresh tissue was washed in 4% paraformaldehyde overnight with PBS buffer, and liver tissue was directly glued to the sample table coated with OCT glue and placed within frozen microtome for direct freezing. The frozen sample table with tissue was clamped on the microtome clamp, and the section was performed with a thickness of about 5 to 10 µm.
Verification Through Cell Experiment
Palmitic acid (PA)-induced MAFLD model was established using human hepatocellular carcinoma cell line (HepG2), and intervention of drug-containing serum of HLJDD and drug-containing serum of silybin was given. The specific group are as follows: Normal group (N), Model group (M), HLJDD treatment group (HL), silybin treatment group (SF), and AMPK inhibitor (drug-containing serum of HLJDD + Compound C) group (HL + CC), for details, see Table 1. Lipid droplet changes of HepG2 cells were detected through oil red O staining; the levels of TG and FFA in HepG2 cells were detected; the expressions of AMPK, mToR, and Beclin-1 were detected through Western blot.
(1) Common Culture medium Preparation System. (2) Cell Grouping and Intervention.

Statistical Analysis
Data were analyzed using GraphPad Prism 8.0, and the results were expressed as mean ± standard deviation (±sd). One-way analysis of variance compared inter-group data, P < .05 indicates statistical difference, P < .01 indicates a statistically significant difference, P < .001 indicates a statistically significant difference.
Results
After screening, 102 substances were obtained through analyzing the active ingredients of each group of HLJDD, including 14 substances of Huanglian, 37 substances of Huangbo, 36 substances of Huangqin, and 15 substances of Zhizi, and after removing duplicate entries, we obtained 70 of the active ingredients in HLJDD (Table 2), 229 targets (Table 3); and 1090 targets of MAFLD; Using Venny2.1.0 to map the common targets for HLJDD and MAFLD (Figure 1), 85 common targets of HLJDD-MAFLD were obtained (Table 4).

Huanglian Jiedu decoction-MAFLD target Wayne's plot.
Main Constituents of Huanglian Jiedu Decoction.

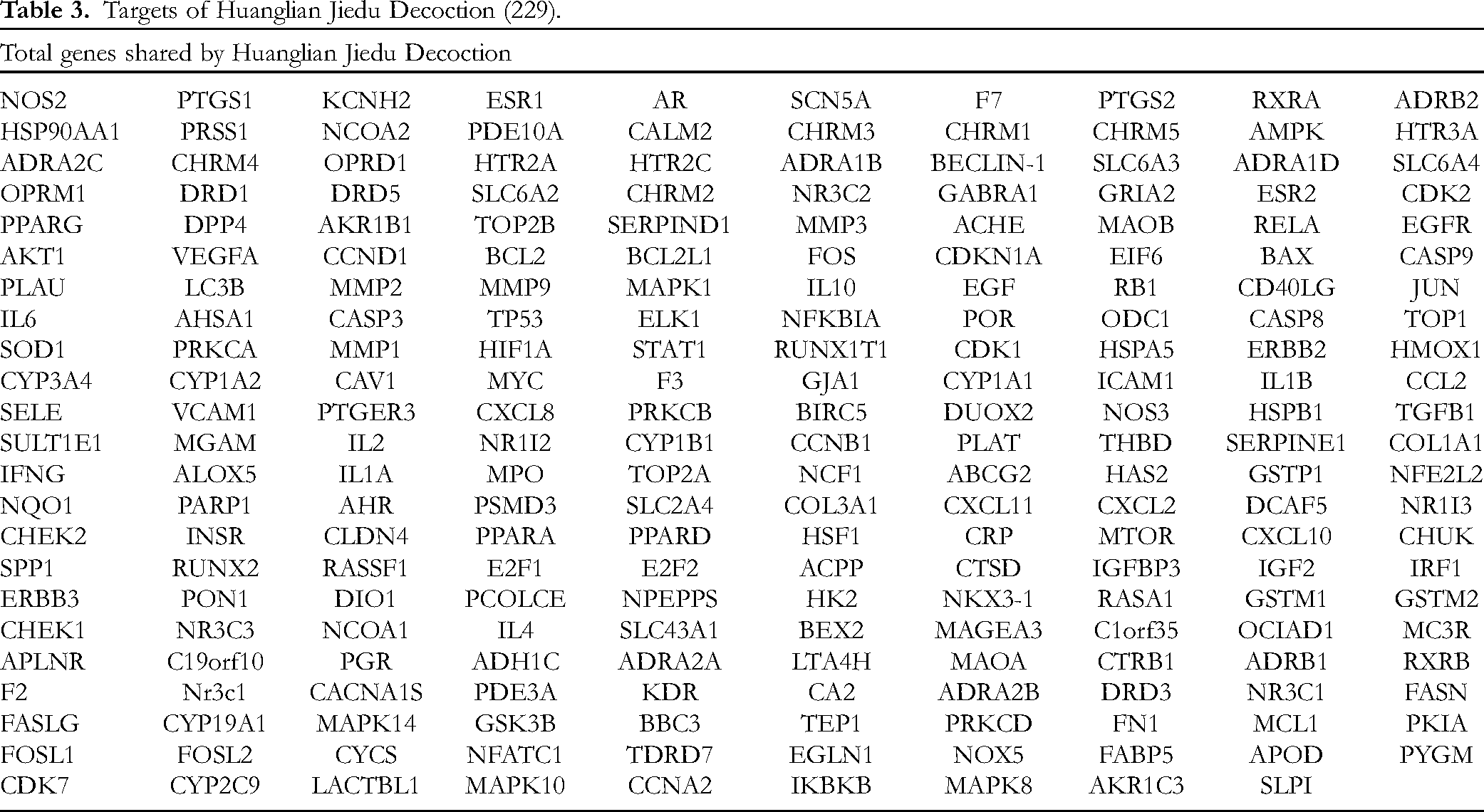
Targets of Huanglian Jiedu Decoction (229).
Targets of Huanglian Jiedu Decoction for the Treatment of MAFLD (85).
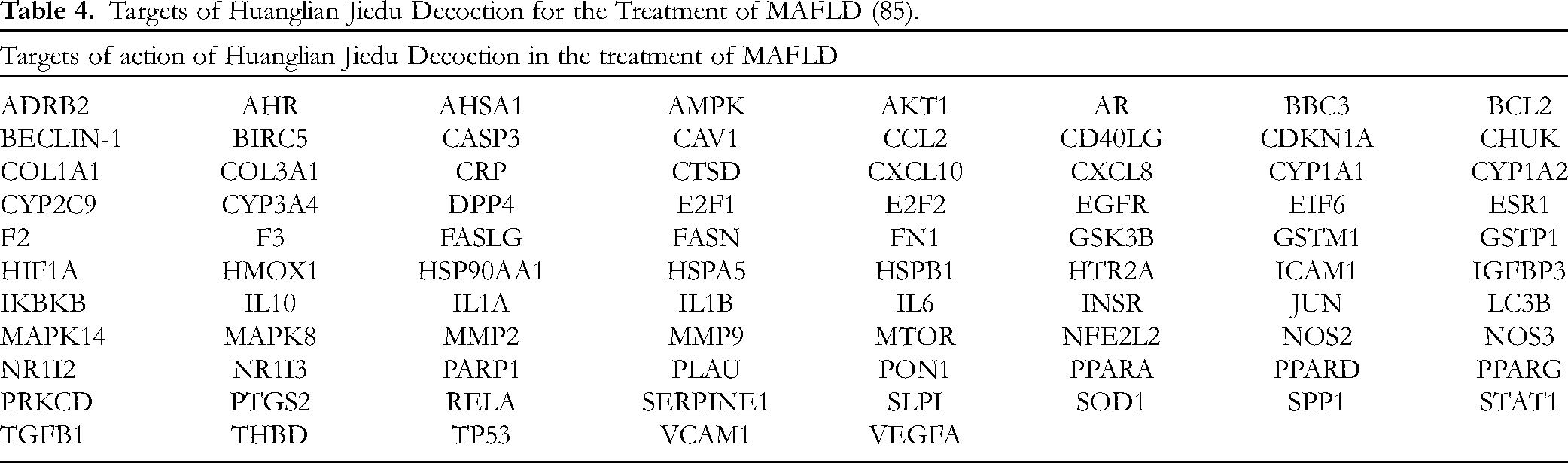

CytoScape network analysis showed that quercetin (MOL000098) had a Degree of Connectedness (Degree) of 145, BetweennessCentrality of 0.5784, and ClosenessCentrality of 0.5547, which predicted that quercetin was the main component, followed through kaempferol (MOL000422) with a connectivity of 57, a BetweennessCentrality of 0.0892, and a ClosenessCentrality of 0.3953, and baicalein (MOL000173) with a connectivity of 44, a BetweennessCentrality of 0.0689, and a ClosenessCentrality of 0.3798, which suggests that quercetin, kaempferol, and baicalein may be principal active ingredients HLJDD in treating MAFLD (Figure 2).

Component-MAFLD target-pathway network diagram of Huanglian Jiedu decoction.
Triangles indicate herbs, ovals indicate active ingredients, rectangles indicate potential therapeutic targets:
HL: Coptidis Rhizoma (huanglian) HQ: Scutellaria Radix (huangqin) HB: Phellodendri Chinensis Cortex (huangbo) ZZ: Gardenia (zhizi) A: (HL + HB), B: (HL + HQ), D1: (HQ + ZZ), C1: (HL + HB + HQ), C2: (HL + HB + ZZ), C3: (HB + HQ + ZZ)
In order to better predict mode of function for HLJDD, 85 target proteins jointly contained in HLJDD and MAFLD were inputed into STRING platform, and PPI network of HLJDD was mapped as shown in Figure 3(a), which contained 85 nodes and 1535 edges, and the targets with the top 25 degree values were shown in Figure 3(b).

(a). Huanglian Jiedu Decoction-MAFLD target network. (b) Top 25 targets for PPI network median value ranking.
KEGG pathway enrichment analysis within DAVID6.8 database, a total of 133 pathways were screened at P < .05, and after deleting some pathways not related to this disease and sorting them according to the P value from smallest to largest, the top 20 were truncated to do the enrichment analysis of the bubble diagram. The results are shown in Figure 4, these targets mainly focused on NAFLD, MAPK/PI3K-AKt/AMPK signaling pathways, animal autophagy, insulin signaling pathway, etc. Based on P-value magnitude, enriched therapeutic target quantities, together with correlation with MAFLD, the AMPK signaling pathway was considered to be the key pathway for HLJDD to treat MAFLD.

KEGG pathway enrichment analysis of Huanglian Jiedu decoction for MAFLD treatment.
The molecular docking dataset outcomes illustrated free binding energy for quercetin to AMPK was −6.4 kcal/mol and that of quercetin to mToR was −7.7 kcal/mol; the free binding energy of baicalein to AMPK was −6.9 kcal/mol and that of baicalein to mToR was −7.7 kcal/mol; the free binding energies of kaempferol and AMPK were −6.5 kcal/mol, and that of kaempferol and mToR were −7.9 kcal/mol. It is generally accepted that the stability of the bound conformation is negatively correlated with binding energy, whereby reduced binding energy increased likelihood that such protein will bind to the compound. Molecular docking simulation shows that quercetin, kaempferol, and hansenin successfully established docking with AMPK and mToR, confirming the reliability of the predicted results (Figure 5).

Molecular docking diagram. (a) Quercetin with AMPK, green for quercetin. (b) Quercetin with mToR, green for quercetin. (c) Baicalein with AMPK, green for baicalein. (d). Baicalein with mToR, blue for baicalein. (e) Kaempferol with AMPK, green for kaempferol. (e) Kaempferol with AMPK, green for kaempferol. (f) Kaempferol with mToR, orange for kaempferol.
Effect of HLJDD on Lipid Level and Liver Function in MAFLD Rats
Compared with group N, the contents of ALT, AST, TC, TG, GLU, HDL, and LDL in serum of group M rats were significantly increased, after drug intervention, the levels of ALT, AST, TC, TG, GLU, HDL, and LDL were significantly decreased in Silybin group and each dose group of HLJDD (Figure 6).

Effect of HLJDD on lipid level and liver function in MAFLD rats(χ±s, n = 8). Note: compared with group N: #P < .05, ##P < .01, ###P < .001, ####P < .0001; compared with group M: **P < .01, ***P < .001, ****P < .0001; ns: no statistical significance.
HLJDD Alleviated Hepatic Lipopathology and Steatosis in MAFLD Rats
Compared with the normal group, the liver of rats in the model group turned yellow significantly with granular-like degeneration, and the liver of rats in Silybin group and each dose group of HLJDD was improved in different degree, as shown in Figure 7. HE staining of liver showed that hepatocytes within normal group were of normal size and morphology, with large and round nuclei located within center, and the inter-cell boundaries were clear and tightly arranged; while a large number of white round vacuoles of different sizes appeared within cytoplasm of hepatocytes within model group, and the boundaries were clear, the nuclei of the cells were pushed to the other side through the white vacuoles, and the cells became smaller and the boundaries of the inter-cells were blurred, and a small number of inflammatory cells infiltrated, presenting a mixed fatty cytopathy; significant improvement within in Silybin group and each dose group of HLJDD in comparison with model group. See Figure 8.

Liver pictures of rats in each group.

HE staining of liver in each group (400×).
Dataset outcomes for oil red O staining highlighted nuclei of hepatocytes within normal group were blue, and no red lipid droplets were seen within cells; a large number of red lipid droplets of different sizes were seen within hepatocytes of rats within model group. Compared with model group, the content of lipid droplets in hepatocytes of SF group, HL-L group, HL-M group, and HL-H group was significantly decreased. See Figure 9.

Oil red O staining of rat liver in each group (400×).
Cell Experiment
As shown in Figure 10, the intracellular levels of TG and FFA in group M were significantly higher than those in group N (P < .05). HLJDD-containing serum and silybin-containing serum could reduce PA-induced increase of TG and FFA levels (P < .05), and HLJDD therapeutic effect was significantly attenuated after the application of AMPK inhibitor, suggesting that HLJDD and Silybin could both improve the intracellular lipid level in HepG2 cells and the therapeutic effect of HLJDD is closely related to AMPK.

Levels of TG and FFA in HepG2 cells (n = 3). Note: Compared with group N: #P < .05, ##P < .01; compared with group M: *P < .05; ns: no statistical significance.
Western blot results showed that HLJDD could up-regulate the protein expression of AMPK and Beclin-1, down-regulate the protein expression of mToR, as shown in Figure 11.

Expression of AMPK and mToR-related proteins in HepG2 cells of each group.
Through observing the oil-red O staining results in Figure 12, it was found that there was no red lipid droplet development within group N, while a considerable population of red lipid droplets formed within group M cells. After the intervention of HLJDD and Silybin drug-containing serum, the color of intercellular lipid droplets became lighter and the number of lipid droplets was considerably reduced compared with that of group M. However, HLJDD therapeutic effect was considerably weakened after the application of inhibitors, indicating that HLJDD and Silybin could improve lipid accumulation in HepG2 cells and the therapeutic effect of HLJDD is closely related to AMPK.

Lipid droplet changes in HepG2 cells (400×).
Discussion
Chinese Medicine Theory of “Lipid-Heat-Toxicity”
Traditional Chinese medicine points out that the addiction to fat, sweet and thick flavors, resulting within accumulation of cream and fat within liver, is a characteristic of the disease development of MAFLD. Therefore, MAFLD lipid metabolism disorders, oxidative stress and inflammatory imbalance, and other pathological processes could be attributed to the fat and sweet and thick flavors lead to the obstruction of lipid turbidity, and over time, it turns into heat and toxicity, damaging the liver, resulting in “lipid-heat-toxicity” interlinked. HLJDD is a reflective formula in clearing heat and removing toxins, with the efficacy of diarrhea and removing toxins, and it is mainly used for treating the evidence of tangible heat and toxins and San Jiao heat. Based upon traditional Chinese medicine theories, HLJDD conforms to treating MAFLD.
Autophagy Signaling Pathway AMPK-mToR and MAFLD
Autophagy is a metabolic process dependent on the lysosomal pathway, having pivotal parts within removing damaged or aged substances, structural remodeling, cell growth and development, maintenance of protein metabolic homeostasis, and stability of the intracellular environment. 11 The lipophagy theory, which has emerged in recent years, refers to a procedure whereby cells selectively identify and degrade lipid droplets of cholesteryl esters and triglycerides through the activation of autophagy-linked molecules, developing cholesterol, free fatty acids and glycerol, in order to circumvent the over-aggregation of lipids within the cells. 12 In fact, lipophagy is a specific form of autophagy. Overall, autophagy remains controlled through differing autophagy-related genes (ATGs), and approximately 40 autophagy-linked genes were identified. Such genes remain highly conserved within yeast and mammals, and are essential molecules implicated within different stages of autophagy. Including Akt, MAPK, P53, AMPK, mTOR, Beclin-1, LC3B, and others play a regulatory role in cellular autophagy.
Adenylate-activated protein kinase (AMPK), known as the “master switch of cellular energy metabolism,” is a major regulator for lipid and glucose metabolism, being one of the central regulators of cellular and body metabolism, which could effectively regulate cellular autophagy and inhibit the mToR, having pivotal parts in controlling cellular energy homeostasis. Mammalian target of rapamycin (mToR) complex is an evolutionarily conserved serine/threonine protein kinase complex, which is closely linked to the PI3K/AKT-related kinase family, and together with a variety of other kinase families, it constitutes a broad signaling pathway in cells. 13 mToR plays a negative regulatory role in autophagy through regulating the biosynthesis of autophagy-related proteins and lysosomes. 14 As a classical pathway related to cellular autophagy, AMPK/mToR is closely related to MAFLD, and MAFLD and various metabolic diseases caused through long-term overnutrition are associated with mToR over-activation. It has been reported that regulating the AMPK/mToR pathway could effectively reduce fatty liver degeneration. 15 AMPK/mToR pathway may be an important target for autophagy-based prevention and treatment of MAFLD. 16 The mToR signaling pathway serves as a signaling pathway that controls cell growth, metabolism, and autophagy. More and more experiments have demonstrated that the mToR signaling pathway is involved in adipogenesis.17,18 The mToR complex contains two forms, mToRC1 and mToRC2. mToRC1 is mainly involved for controlling cellular development, survival, stress together with energy metabolism. 19 Extremely sensitive to the specific inhibitor rapamycin, mToR complexes contain kinases that regulate lipid metabolism within their C-terminal region. 20 It has been shown that mToRC1 is able to activate lipolysis and autophagy, thereby affecting adipogenesis. 21 Also, mToR downstream proteins are able to regulate the activity of multiple adipose transcription factors, 22 the role of the mToR complex in regulating adipogenesis and lipid metabolism was established, whereas the activation of AMPK phosphorylation level could affect adenosine triphosphatase synthesis and metabolism to maintain the homeostatic balance of cellular energy, 23 targets and inhibits the activation of its downstream gene mToR molecule to activate cellular autophagy response, 24 lipid homeostatic balance was maintained.
Huanglian Jiedu Decoction and its Components
HLJDD and its components have some modulatory effects on the targets of action such as AMPK and mToR. Chen et al 25 found that berberine (the active ingredient of HLJDD) potentially lowers apoptosis in high glucose-stimulated rat retinal Müller cells through enhancing autophagy and AMPK/mToR signaling; Wang et al 26 found that berberine could induce autophagy within glioblastoma through affecting AMPK/mToR/ULK1 pathway; Sun et al 27 found that quercetin (the active ingredient of HLJDD) regulated glucose and lipid metabolism through GPRC6A/AMPK/mToR signaling pathway and attenuated osteoporosis within testisectomized mice; Cao et al 28 confirmed that quercetin shields oral mucosal keratinocytes against lipopolysaccharide-driven inflammatory toxicity through inhibiting AKT/AMPK/mToR pathway; Yuan et al 29 found that kaempferol (the active ingredient of HLJDD) orchestrated AMPK/mToR signaling pathway contributes prophylaxis influence against cerebral ischemia/reperfusion injury within rats through driving autophagy; Varshney et al 30 demonstrated that kaempferol modulates the cytoprotective influence by autophagy on palmitic acid-induced pancreatic β-cell necrosis via the AMPK/mToR signaling pathway. Chen et al 31 demonstrated that baicalein (the active ingredient of HLJDD) induces rat mitochondrial autophagy via miR-30b and SIRT1/AMPK/mToR pathways to prevent Parkinson's disease.
Zhuoxi et al 32 demonstrated that HLJDD has a certain intervention effect on atherosclerotic aortic plaque formation in ApoE-/- mice, and its mechanism may be related to the increase within levels of AMPK and PPARα involved in autophagy and apoptosis; Man 33 found that HLJDD could regulate the hepatic AMPK-ACC signaling pathway, promote the oxidation of fatty acids, regulate lipid metabolism, meanwhile, it could increase the expression and activity of AMPK in aortic tissues and protect endothelial function; Xiaohu 34 demonstrated that berberine (main-active ingredient in HLJDD) could ameliorate disorders of glucose and lipid metabolism in T2DM rats, with mechanistics potentially linked to regulation of the expression for LKB1-AMPK-TORC2 signaling pathway proteins within skeletal muscles and adipose tissues. Li 35 demonstrated experimentally that HLJDD could improve atherosclerosis through blocking PI3K-Akt-mToR pathway and increasing autophagy; Yu et al 36 found that HLJDD containing serum inhibited AKT/mToR/p70S6K signaling pathway together with overexpression of inflammatory factors IFN-γ and IL-18 in foam cells and promoted the autophagy and inhibition of inflammatory response in foam cells, this may be one of the mechanisms to prevent and control atherosclerosis; Liwang et al 37 confirmed that HLJDD may reduce CLP-induced liver injury in septic mice through inducing autophagy and inhibiting apoptosis; Li et al 38 found that HLJDD could effectively improve the damage of aortic tissues in SHR, while mechanism/s being possibly linked to thwarting AKT/mToR and Beclin-1 autophagy.
The above indicated that: AMPK-mToR signaling pathway is a classical pathway related to cellular autophagy and closely related to MAFLD; HLJDD is a representative formula for clearing heat and removing toxins, with anti-inflammatory and lipid-lowering effects, which is suitable for the theory of the pathogenesis of MAFLD “lipid-heat-toxicity”; HLJDD and its components are able to modulate AMPK-mToR signaling pathway. The results of molecular docking, animal experiments and cellular experiments also proved our hypothesis. Based on the above points, we believe that HLJDD could regulate the autophagy pathway AMPK-mToR signaling pathway, so as to achieve the effect of treating MAFLD.
Conclusion
This research project focuses on screening principal components of HLJDD and their targets from the perspective of network pharmacology to study mechanistics for HLJDD for treating MAFLD, providing a reliable theoretical basis for this study through combining the theory of “lipid-heat-toxicity” in traditional Chinese medicine, as well as carried out molecular docking and relevant experimental validation.
However, HLJDD has the characteristics of multi-components and multi-targets. The limitation of this study is that only the mechanism of HLJDD on MAFLD was verified, but the corresponding relationship between the components of HLJDD and its targets was not verified by in vivo and in vitro MAFLD models. In the future, we will use MAFLD animal and cell models to verify whether the components of HLJDD, such as berberine and quercetin, inhibit hepatic lipid deposition in MAFLD through lipophagy signaling. Although the results of this study are consistent with the advantages of multi-target, multi-pathway treatment of diseases in traditional Chinese medicine, there are many Chinese medicines and a variety of active ingredients in the prescription, so it is difficult to fully elucidate its therapeutic principle. However, this is precisely the advantage of traditional Chinese medicine, traditional Chinese medicine is never limited to the treatment of a single disease, but has a holistic view of syndrome differentiation and treatment, we should strengthen their research and application.
In conclusion, HLJDD could treat MAFLD through regulating the autophagy signaling pathway AMPK-mToR.
Supplemental Material
sj-docx-1-npx-10.1177_1934578X241235604 - Supplemental material for Mechanism for Huanglian Jiedu Decoction-Based Therapy for MAFLD Analyzed Through Network Pharmacology and Experimental Verification
Supplemental material, sj-docx-1-npx-10.1177_1934578X241235604 for Mechanism for Huanglian Jiedu Decoction-Based Therapy for MAFLD Analyzed Through Network Pharmacology and Experimental Verification by Jixian Zheng, Anni Zheng, Sufei Song, Mengyu Lin and Tao Liu, Qiuling Xu in Natural Product Communications
Footnotes
Data Availability
The data used to support the findings of this study are available from the corresponding author upon request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
This study was approved by the Ethics Committee of Hainan Medical University, approval number: HYLL-2021-009.
Funding
This study was supported through the Youth Qi Huang scholar project of state administration of traditional Chinese medicine, National Natural Science Foundation of China, Natural Science Foundation of Hainan Province (grant numbers 81760795, 821RC579).
Statement of Human and Animal Rights
All of the experimental procedures involving animals were conducted in accordance with the Animal Care Guidelines of Hainan Medical University, China and approved by the Ethics Committee of Hainan Medical University, approval number: HYLL-2021-009.
Statement of Informed Consent
There are no human subjects in this article and informed consent is not applicable.
Supplemental Material
Supplemental material for this article is available online.
Appendix
The incoming blood components of HLJDD-containing serum.

| Name | Formula | RT [minutes] | mzCloud best match | |
|---|---|---|---|---|
| 1 | 2-Hydroxymyristic acid | C14 H28 O3 | 18.337 | 85.5 |
| 2 | (+/-)9,10-Dihydroxy-12Z-octadecenoic acid | C18 H34 O4 | 18.333 | 85.1 |
| 3 | 4-Methylumbelliferone | C10 H8 O3 | 10.507 | 80.9 |
| 4 | Propachlor ESA | C11 H15 N O4 S | 14.725 | 78.3 |
| 5 | 2,4,6-Trihydroxy-2-(4-hydroxybenzyl)-1-benzofuran-3(2H)-one | C15 H12 O6 | 16.853 | 64.8 |
| 6 | Geniposide | C17 H24 O10 | 10.509 | 64.3 |
| 7 | Andrographolide | C20 H30 O5 | 19.358 | 64.1 |
| 8 | 1-Benzyl-8-(4-chloro-3-methylphenoxy)-3,7-dimethyl-3,7-dihydro-1H-purine-2,6-dione | C21 H19 Cl N4 O3 | 10.515 | 58.7 |
| 9 | Piceatannol | C14 H12 O4 | 13.821 | 45.9 |
| 10 | trans-Clovamide | C18 H17 N O7 | 14.059 | 45.1 |
| 11 | (+)-Syringaresinol | C22 H26 O8 | 10.684 | 39.4 |
| 12 | Phenylacetylglycine | C10 H11 N O3 | 10.074 | 32.4 |
| 13 | N-Isovalerylglycine | C7 H13 N O3 | 8.406 | 31.3 |
| 14 | 5-(4-Methylpiperazino)-4-nitrothiophene-2-sulfonamide | C9 H14 N4 O4 S2 | 12.922 | 30.5 |
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
