Abstract
Polysaccharide, one of the main components in Schisandra chinensis, has been discovered to have an antidiabetic effect. In this study, we further observed the effect of the secondary component of Schisandra polysaccharide, acidic polysaccharide, on diabetes induced by streptozotocin (STZ) in mice and H2O2-induced MIN6 cell injury model and investigated the underlying mechanisms at the same time. The results showed that S. chinensis acidic polysaccharide (SCAP) could increase the content of fasting blood insulin and the activity of superoxide dismutase, lower the level of fasting blood glucose and malondialdehyde, and improve the pathological changes in the pancreatic islet in STZ-induced diabetic mice. SCAP decreased the percent of apoptotic cells and increased Cleaved Caspase-3 activity in H2O2-incubated cells. Furthermore, SCAP treatment inhibited the upregulation of phospho C-Jun N-terminal kinase (JNK), BAX, and Cleaved Caspase-3 protein expressions, and increased the expression of Bcl-2. These results indicate that SCAP has a therapeutic effect on STZ-induced diabetic mouse, and this protective effect may be mediated through preventing the apoptosis of β-cells via inhibiting the expression of JNK and related apoptotic proteins.
China has witnessed one of the most dramatic rises in diabetes prevalence anywhere in the world. An estimated 110 million people have diabetes in China and the prevalence is approximately 11%. 1 Although type 1 diabetes mellitus (T1DM) accounts for less than 5% diabetes cases, it is still seriously harmful to patients. T1DM is a chronic autoimmune disease mediated by autoreactive T-cells. 2 Histological studies of T1DM have found that the infiltration of a large number of T lymphocytes in islet and its surrounding, the progressive destruction and loss of islet cells, and thus the decreased number and functional failure of pancreatic β-cells result in the absolute insufficiency of insulin secretion. 3 Studies have demonstrated that apoptosis is the main way for the destruction of diabetic pancreatic β-cells. Glucose and lipid metabolism disorder, oxidative stress, and inflammatory reaction can cause the apoptosis of pancreatic β-cells. 4 Therefore, inhibition of the apoptosis of islet cells and protection of the number and function of islets are considered key to prevent and cure diabetes.
Schisandra chinensis (S. chinensis) is the dry and mature fruit of Magnoliaceae plant, Schisandra chinensis (Turcz.) Baill. As a genuine medicinal material from Changbai Mountain in China and a famous tonic traditional Chinese medicine, it was recorded first in Shennong Bencao Jing as the top grade, with functions of relieving the thirst due to insufficiency of body fluid and the diabetes due to internal heat. Polysaccharide is one of the main active components of Schisandra, accounting for about 10%, with a significant therapeutic effect and high safety, showing a great development value. It was reported that Schisandra polysaccharide reduced the blood glucose of diabetic mice by scavenging oxygen free radicals and antilipid peroxidation. 5 Our previous studies found that Schisandra polysaccharide could significantly alleviate the symptoms of diabetes such as weight loss, polydipsia, polyuria, and hyperglycemia in diabetic mice. However, the specific antidiabetic mechanism of Schisandra polysaccharide is still unclear, and there is no report on whether it exerts its effect by protecting the islet cells and preventing the pancreatic β-cells from apoptosis at home and abroad. In this study, a mouse diabetes model was established by the continuous intraperitoneal injection of low-dose streptozotocin (STZ) and an MIN6 islet cell damage model was induced by H2O2 to observe the protective effect of S. chinensis acidic polysaccharide (SCAP) against the damage of islet cells and explore the role of C-Jun N-terminal kinase (JNK) signaling pathway in the antidiabetic activity of SCAP, in order to reveal the molecular mechanism through which SCAP can protect pancreatic β-cells from apoptosis.
The water-soluble crude polysaccharide component was isolated from the dried fruits of S. chinensis by water extraction and alcohol precipitation method first, with a yield of 8.55%. Then, Schisandra polysaccharide was separated by diethyl aminoethyl (DEAE)-sepharose fast flow column chromatography. S. chinensis neutral polysaccharide (SCNP) could be obtained by the elution with distilled water and the SCAP could be prepared by the elution with 0.5 M NaCl solution, with a yield of 4.02% and 2.31%, respectively. Due to the poor activity of SCNP, SCAP was used for the subsequent experiments in this study. The analysis of physicochemical properties and monosaccharide composition are showed in Table 1.
Chemical Composition of SCAP.
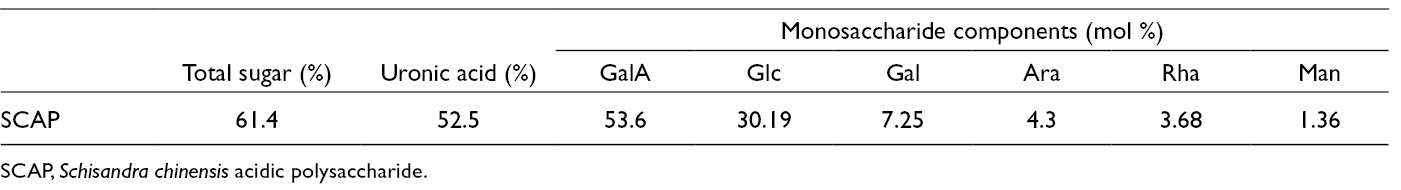
SCAP, Schisandra chinensis acidic polysaccharide.
Streptozotocin, an alkylating agent containing nitroso-group, can damage islet cells by oxidative stress and alkylation, 6 and is an ideal reagent for inducing animal diabetic models. In this study, mice were intraperitoneally injected with STZ (40 mg·kg−1) for 5 days to establish the diabetic model. The results showed that fasting blood glucose (FBG) levels were significantly increased (Figure 1a) and fasting blood insulin levels were decreased in MOD group (Figure 1b). The pathological results showed that the number of islets was reduced, the volume was smaller, and the number of β-cells in islets was significantly reduced in pancreatic tissues of mice in MOD group (Figure 1c), suggesting that STZ-induced diabetic model was successfully established in mice. Compared with MOD group, SCAP treatment significantly decreased the FBG levels, increased the insulin levels (Figure 1a and b), and improved the pathological change in islet cells (Figure 1c). These results indicate that SCAP has a certain therapeutic effect on mice diabetes induced by STZ.

Effects of SCAP on serum FBG, FINS levels and the pathomorphology of pancreatic tissue in mice.
As shown in Figure 2, serum malondialdehyde (MDA) levels increased significantly, while superoxide dismutase (SOD) activities decreased in diabetic mice (P < 0.01). Schisandra chinensis acidic polysaccharide treatment attenuated significantly MDA levels and increased SOD activities (Figure 2a and b), indicating that antidiabetic effect of SCAP might be related to enhancing its antioxidant capacity. Furthermore, both in vitro and in vivo studies have shown that STZ can increase the expression of Caspase-8, Caspase-9, and Cleaved Caspase-3 proteins, and increase the ratio of BAX/Bcl-2 in islet cells to induce the apoptosis of pancreatic β-cells. 7 Our results also showed that after the continuous injection of STZ (40 mg·kg−1) for 5 days, the expression of Cleaved Caspase-3 was upregulated, and the ratio of BAX/Bcl-2 increased in mice, while the SCAP treatment could downregulate the expression of Cleaved Caspase-3 and decrease the ratio of BAX/Bcl-2, showing a certain antiapoptotic effect (Figure 3a).

Effects of SCAP on serum MDA and SOD levels. (a) MDA level in serum; (b) SOD activity in serum.
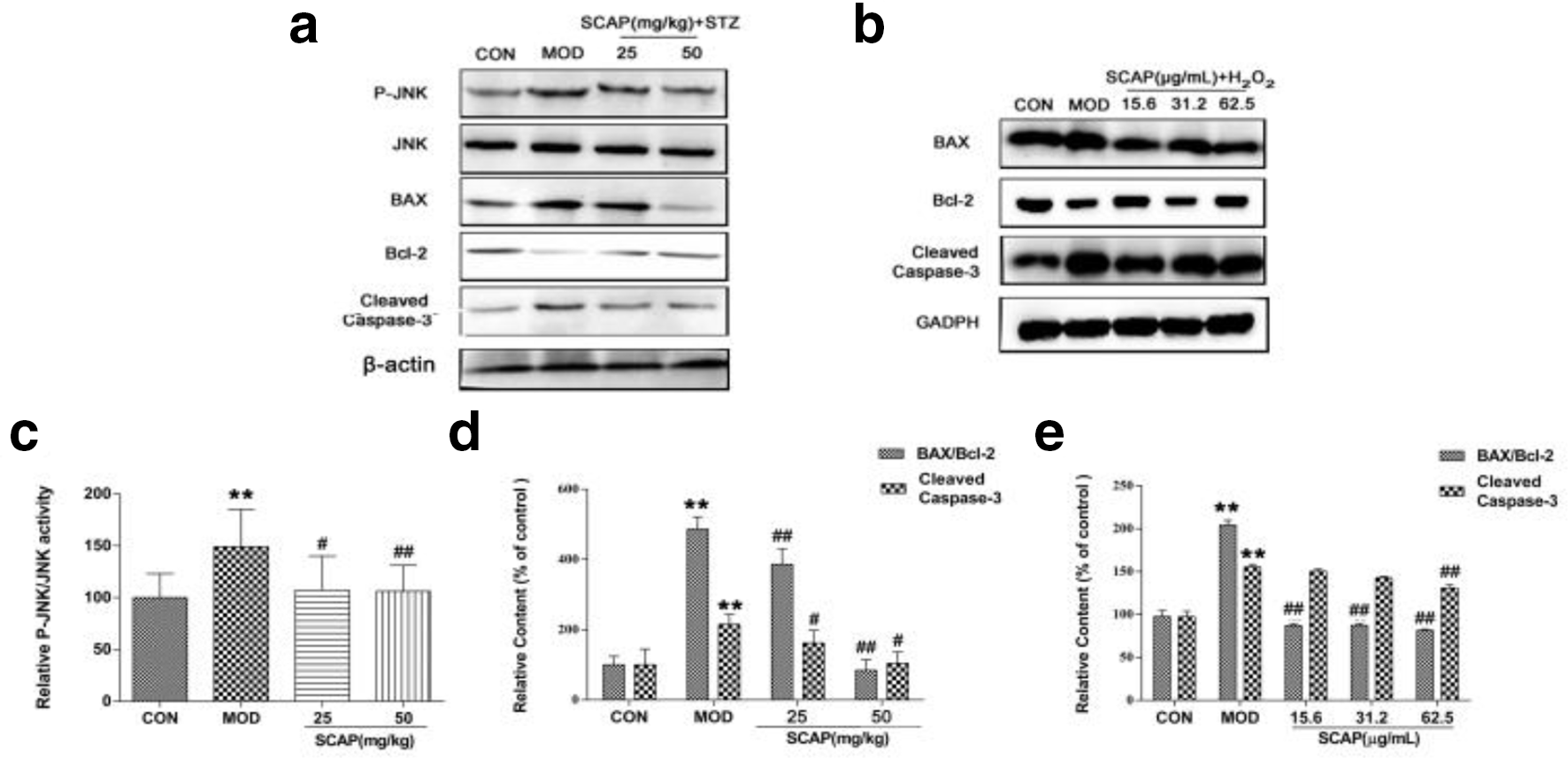
Effects of SCAP on protein expression of P-JNK, JNK, BAX, Bcl-2, and Cleaved Caspase-3. (a) Protein expression of P-JNK, JNK, BAX, Bcl-2, Cleaved Caspase-3, and β-actin in pancreatic islet tissues. (b) The protein expression of BAX, Bcl-2, Cleaved Caspase-3, and GAPDH in MIN6 cells. (c) The P-JNK protein levels are expressed relative to JNK. (d) The Cleaved Caspase-3 protein levels are expressed relative to β-actin and the apoptotic cell protein levels are expressed relative to BAX/Bcl-2 in diabetic mice. (e) The Cleaved Caspase-3 protein levels are expressed relative to GAPDH and the apoptotic cell protein levels are expressed relative to BAX/Bcl-2 in MIN6 cells.
To explore the protective effect of SCAP on pancreatic β-cells, we established an injury model of MIN6 cells (with many characteristics of normal pancreatic β-cells) induced by H2O2. H2O2, a reactive oxygen species (ROS), can directly oxidize lipids and proteins on the cell membrane, and freely penetrate the cell membrane to cause the lipid peroxidation, leading to an oxidative stress, which may damage the mitochondrial function of the islet cells to induce the apoptosis of pancreatic β-cells. 8 MIN6 cells were incubated ±0.7 mmol·L−1 H2O2 or incubated with
SCAP (15.6, 31.2, and 62.5 μg·mL−1) and 0.7 mmol·L−1 H2O2. The apoptosis of MIN6 cells was determined by flow cytometry analysis as described in Materials and methods. As shown in Figure 4, SCAP treatment significantly decreased the average percent of apoptotic cells in H2O2-incubated cells (Figure 4a and b). Caspase-3 is the most critical protease in the apoptotic cascade reaction. The activity of Caspase-3 in injured MIN6 β-cells induced by H2O2 was significantly increased compared to that in the control (CON) group, while SCAP treatment attenuated the increased Caspase-3 activity (Figure 4c). Moreover, SCAP treatment reduced the protein expression of Caspase-3, and the ratio of BAX/Bcl-2 in the cells (Figure 3b), suggesting that SCAP can inhibit the apoptosis of islet cells.

SCAP attenuates H2O2-induced apoptosis in MIN6 cells. (a) MIN6 cells were stained with Annexin V-fluorescein isothiocyanate and propidium iodide; (b) Percentages of Annexin V positive cells (early and late apoptosis) ; (c) Caspase-3 activities in MIN6 cells. Caspase-3 activity is expressed relative to control.
To further explore the mechanism through which SCAP could inhibit the apoptosis of islet cells, we examined the expression of JNK and P-JNK proteins in mouse islets. C-Jun N-terminal kinase, a member of mitogen-activated protein kinase, is involved in the regulation of the proliferation, differentiation, and apoptosis of cells. 9 An important mechanism involved in the apoptosis of β-cells in diabetes is that ROS mediates the inhibition of antiapoptotic protein expression in Bcl-2 family and the promotion of proapoptotic protein expression by activating JNK, leading to changes in the cell membrane permeability and then the release of cytochrome c, which further causes the Caspase cascade reaction to resulting in the apoptosis. 10,11 Therefore, the regulation of JNK signal activity and the inhibition of the excessive apoptosis and necrosis of pancreatic β-cells can help to protect the damage of diabetic islet cells. The results of this study showed that with the increase of SCAP concentrations, the expression level of P-JNK protein decreased (Figure 3a and c), suggesting that SCAP could inhibit the apoptosis of pancreatic β-cells by regulating the activity of JNK signaling pathway.
To sum up, SCAP shows a significant preventive and therapeutic effect on the mouse diabetes induced by STZ, and can inhibit the apoptosis of the pancreatic β-cells by regulating the activity of JNK signal pathway to lower the ratio of BAX/Bcl-2 and downregulating the expression of Cleaved Caspase-3, thereby increasing the secretion of insulin to reduce the blood sugar, which may provide theoretical basis for the further application of S. chinensis in the prevention and treatment of diabetes.
Experimental
Reagents
Streptozotocin was purchased from Sigma-Aldrich (St Louis, MO, USA). Kits for measuring levels of glucose and MDA, SOD, and Caspase-3 activities were purchased from Nanjing Jiancheng Bioengineering Institute (Nanjing, China). Insulin radioimmunoassay kit was obtained from Shang Hai Lengton Bioscience Co. Ltd (Shanghai, China). MIN6 cells were obtained from American Type Culture Collection (ATCC, USA). Dulbecco’s modified Eagle medium (DMEM) and other culture reagents were obtained from Gibco Life Technologies (Gibco, GrandIsland, NY, USA). Polyclonal antibodies of P-JNK, JNK, BAX, Bcl-2, Cleaved Caspase-3, GAPDH, and â-actin were purchased from ABclonal Biotechnology (Wuhan, China).
Extraction, Isolation, and Purification of SCAP
Schisandra chinensis acidic polysaccharide was prepared in the Center of Life Science, Northeast Normal University. Briefly, Schisandra was steeped in 10 times volume of distilled water overnight, then extracted 2 times by boiling it in 100°C hot water, and the extract was concentrated. The concentrated extract was precipitated overnight with 75% ethanol, then centrifuged (4500 rpm, 15 minutes) and the precipitation was collected. The precipitation was washed with 95% ethanol and absolute ethyl alcohol in turn, and dried routinely to obtain a powder-like Schisandra polysaccharide. A 0.5% polysaccharide solution was prepared and was loaded on a balanced DEAE-cellulose ion-exchange chromatographic column (20 mL, Cl-type), and eluted with distilled water to remove the neutral polysaccharide. Then 0-1.0 M NaCl solution was used for the linear gradient elution at a flow rate of 1 mL·min−1 to obtain the eluent, and the eluent was concentrated and dried routinely to obtain the SCAP.
Characterization of SCAP
Using d-glucose as the reference substance, the total sugar content was determined with phenol-sulfuric acid method. Using galacturonic acid as the reference, the uronic acid content was measured with meta-hydroxydiphenyl method. Coomassie brilliant blue was used to determine the protein content.
Analysis of Monosaccharide Composition
Each monosaccharide composition of SCAP was analyzed by PMP derivatization and high-performance liquid chromatography (HPLC). Details are as follows: 2 mg SCAP was dissolved in 1 mL anhydrous methanol solution containing 1 mol·L−1 hydrochloric acid; the sample solution was inflated with nitrogen and the tube was sealed, then the solution was hydrolyzed at 80°C for 16 hours and added with 1 mL of 2 mmol·L−1 trifluoroacetic acid after it was blown dry with an air pump, and hydrolyzed at 120°C for 1 hour, added with a small amount of ethanol, then dried in water bath at 60°C, which was repeated 3-5 times for the complete removal of trifluoroacetic acid. The dry sample obtained after the complete acid hydrolysis was added with 0.5 mL of PMP reagent and 0.5 mL of 0.3 mol·L−1 NaOH solution, respectively, and then 0.1 mL of the sample was placed into a microcentrifuge tube after it was fully dissolved and the tube was placed in water bath at 70°C for 30 minutes. After the sample solution was centrifuged at 10 000 rpm for 5 minutes, 500 µL of 0.3 mol·L−1 hydrochloric acid solution and 500 µL distilled water were added into it, which was vortex-mixed for 2 minutes and then extracted 3 times by adding 1 mL chloroform. After blending, the remaining PMP reagent was extracted, and the trichloromethane layer was removed to retain the water layer. The water phase was filtered with a 0.22 µm microporous membrane and the filtrate was analyzed by HPLC. The chromatographic conditions were as follows: chromatographic column: DIKMA Inertsil ODS-3 (4.6 × 150 mm); mobile phase: 0.1 mmol·L−1 phosphate buffer solution (PBS) (pH = 7.0)-acetonitrile (82:18); flow rate: 1.0 mL·min−1; sample size: 20 µL; detection wavelength: 245 nm.
Animals
Male ICR mice, weighing 19-21 g, were provided by Changchun Yisi Laboratory Animal Technology Co. Ltd. (Changchun, China) (license number: SCXK (JL) 2016-0003, SPF). The mice were raised in separate cages at 18-22°C (relative humidity 40%-60%), under normal lighting conditions, and with ad libitum access to water. All procedures were approved by the Ethics Committee for Use of Experimental Animals at Beihua University (Jilin, China).
Establishment of DM Model in Mice
Ten of 70 ICR mice were randomly selected as normal CON group, and then the remaining 60 mice were intraperitoneally injected with STZ (40 mg·kg−1·day−1), continuously for 5 days for establishing DM model. Mice in the normal CON group were given the equal volume of citrate buffer. One week after the injection, the level of FBG in serum of mice was measured, in which the mice whose FBG levels were higher than 7.0 mmol·L−1 were considered those with diabetes induced by STZ.
Animal Grouping and Treatment
Diabetic mice were divided into model group (MOD), low-dose SCAP group (25 mg·kg−1), and high-dose SCAP group (50 mg·kg−1), 10 in each group. Mice in the CON group and MOD group were intragastrically given the equal volume of saline, and those in SCAP-treated groups were administered 25 and 50 mg·kg−1 of SCAP in the same way, once daily successively for 4 weeks. After the last administration, all mice were forbidden food but not water for 12 hours, and anesthetized with ether, then 0.8-1.0 mL of blood was collected from each mouse by removing eyeballs. The serum was separated by centrifugation (3500 rpm, 10 minutes) and stored at −80°C. The pancreatic islet tissue was carefully isolated for the histopathological examination and Western blotting experiments.
Detection of Biochemical Indexes in Serum
Fasting blood glucose was estimated by a commercially available glucose kit based on the glucose oxidase method. Insulin was measured by radioimmunoassay method. Malondialdehyde level and SOD activity were determined by enzymatic method according to the kit instructions.
Histomorphological Analysis of Pancreatic Islet
The pancreatic tissue samples were fixed in 10% neutral formalin solution, and then the fixed samples were washed, eluted with alcohol gradient elution, paraffin-embedded, and cut into slices. The slices were dewaxed with xylene, eluted with alcohol gradient elution, stained with hematoxylin-eosin, eluted with alcohol gradient elution again, clarified with xylene and mounted by adding neutral balata. Pathological changes in the morphology of cells were observed under a light microscope.
Cell Culture and Administration
MIN6 cells were cultured in DMEM supplemented with 10% fetal bovine serum (Gibco), 100 IU·mL−1 penicillin, 0.1 µg·mL−1 streptomycin, and 144 µ·L−1 β-mercaptoethanol (Sigma). The cells were incubated in humidified atmosphere of 5% CO2 at 7°C and used for experiments from the logarithmic phase of growth, and seeded into 96-well plates (1 × 104 cells per well, 100 µL). The final concentration of H2O2 was 0.7 mmol·L−1 for inducing the cell injury, and cells in SCAP-treated groups were treated with 15.6, 31.2, 62.5 µg·mL−1 SCAP, respectively. All cells were cultured for 48 hours.
Determination of Cell Viability
The cell viability was determined by MTT assay method. Briefly, MTT (5 mg·mL−1, 20 µL/well) was added into the cell-seeded 96-well plates and the cells were incubated at 37°C for 4 hours. Then the solutions were removed and dimethyl sulfoxide (100 µL/well) was added into the wells. The absorbance was measured at 490 nm using a 96-well plate reader. The cell viability was calculated as follows: cell viability (100%) = absorbance of SCAP-treated group/absorbance of CON group × 100%.
Apoptosis Determination
The cell apoptosis was assessed by Caspase-3 activity and Annexin V-fluorescein isothiocyanate (FITC)/propidium iodide (PI) staining. Caspase-3 activity was measured using a Caspase-3 colorimetric assay kit (Nanjing Jiancheng Bioengineering Institute) according to the manufacturer's instructions. Briefly, MIN6 cells in the logarithmic growth phase were seeded into 6-well plates at 1 × 105 cells/well, and incubated with the corresponding agents for 48 hours. The cells were washed with cold PBS, resuspended in lysis buffer, and left on ice for 30 minutes. The lysate was centrifuged at 12 000 rpm at 4°C for 15 minutes. The production of p-nitroaniline was measured at 405 nm using a microplate reader. Caspase-3 activity was normalized to the total extracted protein concentration. After the treatment of SCAP in 6-well plates, the cell apoptosis was analyzed using Annexin V-FITC/PI (KeyGEN BioTECH), according to the manufacturer’s instructions. Briefly, the cells were harvested, washed twice with cold PBS, and then incubated with 5 µL of Annexin V-FITC for 15 minutes and 10 µL of PI for 5 minutes in dark place at room temperature, respectively. The cellular fluorescence was measured with a flow cytometer (FACS Calibur™, BD Biosciences, CA, USA).
Western Blotting Analysis
The protein samples were collected and the protein concentrations were measured using Bradford assay (Bio-rad protein assay kit). For Western blot detection of P-JNK, JNK, BAX, Bcl-2, Cleaved Caspase-3, β-actin, and GAPDH homogenization protein expression, the protein samples (30 µg) were denatured by boiling for 5 minutes and separated on 10% sodium dodecyl sulfate-polyacrylamide gel electrophoresis, and then transferred at 4°C to polyvinylidenediflouride membranes (Millipore, USA). The membranes were blocked in 5% nonfat milk for 2 hours at room temperature and then incubated with rabbit polyclonal antibodies for P-JNK, JNK, Bcl-2, BAX, Cleaved Caspase-3, β-actin, and GAPDH (diluted 1:1 000) with gentle agitation overnight at 4°C. The membranes were washed and then incubated with the second antibodies (1:2 000 goat anti-rabbit IgG horseradish peroxidase conjugate, ABclonal Biotechnology) at room temperature for 1 hour. The proteins were then visualized with enhanced chemiluminescene solution and the images were taken using chemiluminescent imaging system (Protein simple, FluorChem, CA, USA). The relative expression of proteins was expressed by the target protein band/GAPDH or β-actin band.
Statistical Analysis
Data are presented as mean ± standard deviation derived from at least three separate experiments. A comparison of the results was performed with one-way nalysis of variance using the GraphPad Prism program (GraphPad Software, Inc., San Diego, USA). P <0.05 was considered statistically significant.
Footnotes
Acknowledgments
We thank all our colleagues working at the Jilin Schisandra Development and Industrialization Engineering Research Center, Beihua University.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The research was supported by Jilin Pharmaceutical Industry Promotion Plan (20170309006YY), Jilin Natural Science Foundation Project (20160101176JC), and Science and Technology Project of the Education Department of Jilin Province (JJKH20180375KJ).
