Abstract
Primary care clinicians (PCCs) manage 90% of patients with diabetes, 30% of whom require insulin with a substantial number poorly controlled because of the challenges that PCCs face (time constraints and lack of experience). The author has developed Federal Drug Administration cleared and Conformite Europeenne mark registered comprehensive computerized insulin dose adjustment algorithms (CIDAAs) to enable PCCs to significantly lower HbA1c levels in insulin-requiring patients. Reports sent to PCCs contain scatter plots of glucose readings, their organization into pre- and postprandial and before bedtime values, their analyses, and recommendations for insulin dose adjustments (if indicated) that the PCC can accept or modify. The glucose readings are provided to the CIDAAs for analysis at either in-person visits or remotely. The new doses accepted by PCCs serve as the basis for the subsequent report. Published studies evaluating this comprehensive CIDAA involved 104 poorly controlled patients taking insulin for greater than or equal to six months who were independently managed by PCCs. Over four to six months, initial HbA1c levels of 9.7% fell by 1.7%. Combining these results with 138 other better controlled patients in real-world situations, initial measured and estimated HbA1c levels of 8.3% fell by 0.7% in 6.4 months enabling PCCs to significantly improve glycemic control. Other advantages of PCCs utilizing these comprehensive CIDAAs are saving time for PCCs so that they can address non-diabetes issues and/or see other patients and ongoing PCC education in adjusting insulin doses by matching glucose patterns and dose-change recommendations with subsequent glycemic responses.
Keywords
Introduction
Insulin secretion is approximately 50% of normal when type 2 diabetes is diagnosed 1 and subsequently progressively decreases in most patients in spite of ongoing treatment with non-insulin drugs. 2 This pattern of insulin secretion leads to early effective treatment with non-insulin drugs but eventual need for insulin therapy in about 30% of people with diabetes (which includes the 5% of patients with type 1 diabetes). 3 Ninety percent of individuals with diabetes are cared for by primary care clinicians (PCCs) 4 who are challenged using insulin. 5 Strikingly, the average HbA1c level has not changed in over 30 years in patients receiving insulin with ~15% maintaining a value >10.0% 6 in spite of the development of many analogue insulins more closely mimicking the pattern of endogenous insulin secretion since the mid 1990s. This clearly indicates that improvement in glycemic control in these patients lies outside of changes in the pharmacokinetics/pharmacodynamics of insulin preparations.
In general, there are three types of CIDAAs; bolus dose calculators, those for adjusting only basal insulin doses and comprehensive computerized insulin dose adjustment algorithms (CIDAAs) for more intensive insulin regimens. This article will describe the effect of PCCs using a comprehensive CIDAA and compare it to the other three types.
Methods
The author has developed CIDAAs for adjusting insulin doses that are based on the following three fundamental principles:
Depending on when injected, each component of the insulin regimen has a maximal effect on a specific period of the 24-hour cycle, for example, overnight, morning, afternoon, and evening.
The glucose pattern in that period determines whether the dose of that component of the insulin regimen requires adjusting or not.
There needs to be enough glucose readings in a period to reflect a patient’s current lifestyle for a decision to be made about that component of the insulin regimen that maximally affects that period.
These CIDAAs (called Insulin Insights) have been cleared by the Federal Drug Administration (FDA) and are Conformite Europeenne (CE) mark registered. The algorithmic program can interact with more than 60 glucose meters and with continuous glucose monitoring (CGM) devices. Insulin Insights can handle more than 25 different types of insulin preparations and can analyze 11 different insulin regimens, for example, (1) basal insulin alone, (2) bedtime NPH insulin alone, (3) basal/bolus (with 1, 2, or 3 bolus injections), (4) self-mixed/split human insulins, (5) self-mixed/split analogue insulins, (6) premixed human insulins, (7) premixed analogue insulins, (8) premixed basal/rapid-acting insulins, (9) U-500 regular insulin, and the unusual delayed responses to (10) NPH and (11) U-500 regular insulins.
Registering a patient to use Insulin Insights is simple and straightforward. After the initial registration of the patient into the system requiring year of birth, height, weight, sex, insulin regimen, approximate time range for each meal and bedtime, and pre- and postprandial targets selected by the clinician, there is no further administrative interactions. The generated report includes a scatter plot of all glucose readings, the glucose values organized into before and after each meal and before bedtime, an analysis of the glucose patterns, and recommendations for insulin dose adjustments (if necessary) that the clinician can accept or modify (Supplementary Figure 1). If the insulin algorithmic program is contained in an electronic health record or an office computer, the report is generated within one minute of downloading the glucose meter. When the program is placed on a secure, Health Insurance Portability and Accountability Act (HIPAA)-approved cloud source and receives remotely measured glucose readings, reports can be generated and sent to the PCC at frequencies determined by them or by the medical care system in which they work. Once the clinician designates the new doses, these serve as the basis for the subsequent report.
The hallmark of CIDAAs is that analysis of glucose readings and initial recommendations to clinicians for insulin dose adjustments occur automatically which were the inclusion criteria for studies. Appropriate published studies for comparison with Insulin Insights were identified by searching PubMed using the term “computerized insulin dose adjustment algorithms,” the author’s extensive personal bibliography and the reviews identified by both. Papers describing non-computerized algorithms were excluded.
There has been a recent emphasis on using real-world situations to externally validate the findings of randomized studies.7,8 Under these circumstances, the sources of the data are limited to the instruments available for the study, for example, insurance and pharmacy databases, and electronic health records. In terms of evaluating the effect of these CIDAAs in real-world studies, strictly scheduled measurements of HbA1c levels did not occur. Information was limited to what was provided in the reports, that is, average glucoses and their estimated HbA1c (eHbA1c) levels 9 between the final and initial reports.
Results
Effect of Insulin Insights on Remote Glucose Monitored Patients
Adult patients in a Federally Qualified Health Center receiving insulin for greater than or equal to six months with HbA1c levels ≥8.0% whose diabetes care was being independently managed by a nurse practitioner (NP) were eligible for the first study. 10 Glucose readings were sent to a secure, HIPAA cloud containing the Insulin Insights program. Reports were sent to the NP every two to three weeks. Twenty-eight patients were enrolled, 11 taking basal insulin alone, 14 on a basal/bolus insulin regimen, and 3 on a self-mixed split NPH/regular insulin regimen. After the initial education session, all further interactions with the patients occurred telephonically. The results are shown in Figure 1. The total daily doses of insulin increased by 24%. No patient experienced severe hypoglycemia or visited an emergency department for hypoglycemia.
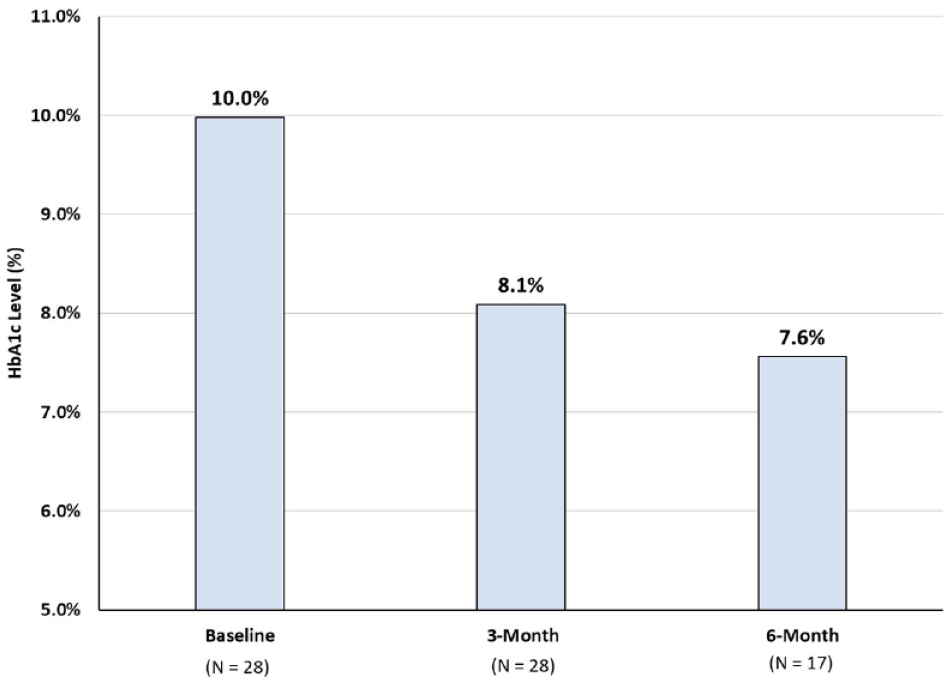
HbA1c responses to remote glucose monitoring utilizing Insulin Insights. Originally published in Davidson and Davidson 10 and reproduced here with permission.
The second study 11 was a randomized three-arm one involving insulin-requiring patients enrolled in a Medicare Advantage Plan receiving insulin for at least six months and a HbA1c level of ≥8.0%. Patients in two of the arms (groups A and B) were also registered in a remote patient monitoring (RPM) program in which glucose concentrations of <70 and >200 mg/dL triggered calls from a diabetes educator to discuss lifestyle changes to avoid subsequent episodes. Patients in one of the RPM arms group A were also followed by PCCs (two physicians and a physician assistant) utilizing Insulin Insights. Again, after the initial education session, all subsequent interactions between group A patients and the PCCs utilizing Insulin Insights occurred telephonically. Patients in groups B and C received usual diabetes care by their personal PCC.
The clinical outcomes and insulin regimens at the end of the study are shown in Table 1. Baseline HbA1c levels were no different among the three groups, but the decrease in HbA1c levels after six months was twice as great in group A (−1.5%) compared with groups B and C (−0.7%) which were identical. There were significant decreases in the high alerts in group A compared with group B, but no differences in the low alerts reflecting the safety of Insulin Insights. No patients in groups A and B visited an emergency department for hypoglycemia, whereas six patients in group C did. The insulin regimens at the end of the six-month study were comparable among the three groups.
Clinical Outcomes and Insulin Regimens.

N, number of patients; ED, emergency department.
Groups A, B, and C, P = .20; †Group A vs B, P = .001; Group A vs C, P = .001; Group B vs C, P = .37; ‡Group A vs B, P = .02; §Group A vs B, P = .002;||Group A vs B, P = .14.
Effect of Insulin Insights on Patients Using CGM
Two PCCs utilized Insulin Insights to independently manage patients receiving insulin. 12 A PharmD, who was routinely referred patients with HbA1c levels >9.0%, independently managed 23 insulin-requiring patients using a Free Style Libre 2 Pro CGM. An NP working in the endocrinology section of a large medical care system independently managed 13 insulin-requiring patients using a G6 Dexcom receiver. Both CGM devices had to be brought to in-person visits for downloading. The primary outcomes were differences in the average glucoses and their calculated eHbA1c levels 9 between the final and initial reports. Because the frequency of glucose reading would accurately reflect the patient’s overall glucose patterns, the eHbA1c level would also very likely accurately reflect a measured one.
Insulin Insights issued 159 reports over a mean of 113 days so that on average there were 4.4 reports per patient (159 reports/36 patients) who were seen at approximately monthly intervals (113 days/4.4 reports). The clinical changes over the average of the nearly four months of the study are shown in Table 2. There was a 1.2% decrease in eHbA1c levels. Insulin doses increased by 42% signifying that these patients were markedly under-insulinized. Hypoglycemic glucose values of <70 mg/dL were <2.0% and not significantly different between the initial and final reports reflecting the safety of the algorithms underlying Insulin Insights. Intensification of the insulin regimen occurred in three patients.
Clinical Changes in Patients Using Continuous Glucose Monitoring.

P < .001 by a paired t test (since average glucoses are converted to eHbA1c levels, they are not independent parameters and their P values are the same).
Total Published Experience With Insulin Insights
In addition to the 68 poorly controlled patients in whom HbA1c levels were measured on schedule,10,11 PCCs used Insulin Insights under real-world situations in 138 better controlled patients with fingerstick glucose readings 13 and 36 patients using CGM. 12 Using average glucoses to estimate HbA1c levels in these 242 patients, the eHbA1c levels fell 0.7% from 8.3% to 7.6% over 6.4 months in these mostly low socioeconomic status, minority patients.
Effect of CIDAAs Recommendations Sent Directly to Patients
To address the problem of few endocrinologists and large distances between PCCs and their insulin-requiring patients in rural areas of Australia, a small six-month study was conducted in which patients were randomized into Insulin Insights and a Usual Care group. 14 In the CIDAA group, patients measured glucose readings by meters that allowed values to be sent to a central Australian server with subsequent transfer to Insulin Insights. Reports with insulin dose adjustment recommendations were sent weekly for two months to the endocrinologist serving the rural area. Patients were messaged to ensure that the prescribed insulin doses were being taken. If so, the endocrinologist reviewed the recommendations and accepted or modified them which were then sent directly to the patient (without personal contact by the endocrinologist). After two months, patients returned to their usual care.
A repeated-measures analysis of variance determined that trajectories of curves depicting HbA1c levels were significantly different (P = .005) and showed a significant difference in HbA1c levels between Insulin Insights and Usual Care groups at three months but not at baseline or six months (Table 3). Paired t tests between baseline and three and six months revealed a significant difference in the Insulin Insights group at three and six months (P values <.01), but no difference in the Usual Care group (P values >.35). Note that recommendations for insulin dose adjustments were sent to the patients for only the first two months of the six-month study. This indicates that ongoing analyses of glucose readings by CIDAAs with subsequent recommendations for insulin dose adjustments made available to patients were necessary to sustain or continue improvement in glycemic control. Although HbA1c levels remained significantly decreased from baseline four months after the patients stopped receiving recommendations for insulin dose changes in the Insulin Insights group, cessation and return to usual care led to regression back toward poor glycemic control.
Effect of Insulin Dose Recommendations Sent Directly to Patients on HbA1c Levels.

% ± SD; aWilcoxon rank-sum test; CIDAA, computerized insulin dose adjustment algorithms.
Discussion
These comprehensive CIDAAs, Insulin Insights, are effective to facilitate PCCs quickly improving glycemic control in patients taking insulin under a variety of circumstances, for example, whether being seen in person or remotely and with glucose readings obtained by fingersticks, CGM, or possibly sent directly to patients. Continuous glucose monitoring removes the patient challenge of painful and inconvenient fingersticks leading to too few glucose readings. For PCCs, it requires increased amounts of time to analyze the patterns of multiple glucose values as well as newly acquired experience to translate them into insulin dose adjustments, especially when the insulin regimen is intensive, that is, requiring two different insulin preparations injected two or more times per day. Unfortunately, very few PCCs utilize CGM because of these challenges, 15 both of which are met by Insulin Insights.
An important advantage of Insulin Insights involves hypoglycemia. Fear of hypoglycemia by clinicians is a prominent reason for therapeutic inertia, especially regarding starting and intensifying insulin regimens. 16 In insulin-requiring patients, hypoglycemic episodes measured by fingerstick10,17 and CGM 18 glucoses are very common, occurring in more than 80% and 90% of patients, respectively. Continuous glucose monitoring documented 18 6.7 and 2.1 episodes per week in patients with type 1 and type 2 diabetes, respectively. Most episodes are due to patient behavior factors rather than excessive insulin. Insulin Insights weights hypoglycemia appropriately, not overemphasizing it in making its recommendations. Note that hypoglycemia was not increased in the three studies in which these comprehensive CIDAAs enabled PCCs to effectively improve diabetes control.10-12 An example of overemphasizing hypoglycemia occurred in a small project evaluating Insulin Insights in an endocrinology clinic in Southern California Kaiser Permanente. Twenty-eight patients were followed for 5.2 months engendering 139 reports. Hypoglycemic values were 7% and 6% in the initial and final reports, respectively. Although recommended dose increases averaged 9 units per report, the mean total insulin dose of 112 units in the initial report fell to 98 units in the final one. No change in the percent of hypoglycemic glucose readings supports lifestyle factors rather than excessive insulin. The initial eHbA1c level of 7.2% rose to 7.6% before the endocrinologist terminated the project.
Although RPM programs are often used by insulin-requiring patients, it should be pointed out that few of them are effective in improving glycemic control. In most RPM programs, high and low glucose readings are sent to health educators who contact patients to provide lifestyle counseling to prevent subsequent episodes. Two randomized studies comparing this type of RPM program to usual care found that although these RPM programs did lower hypoglycemia risk, they did not improve glycemic control.11,19 That requires ongoing insulin dose adjustments by knowledgeable clinicians.20-22
Computerized insulin dose adjustment algorithms are used to calculate bolus insulin doses which require preprandial glucose testing and carbohydrate (CHO) counting. In addition to obvious challenges of patient testing before each meal, CHO counting has its own challenges. It requires intensive education over months after which patient and dietitian estimates of meal CHO content still differed by 20%. 23 Recent studies have shown that both fat24-27 and protein25,26,28,29 contents of the meal importantly affect the post-prandial rise of glucose invalidating relying only on the CHO content. In patients using a bolus calculator, the HbA1c level was a clinically insignificant 0.1% less compared with standard care. 30
Computerized insulin dose adjustment algorithms have also been used in six randomized controlled trials in 856 patients to adjust basal insulin doses. 31 In spite of the fact that 54% of the patients were insulin-naïve (whose responses would expected to be more robust than in those already taking basal insulin), HbA1c levels fell only 0.25% more by automated titration compared with controls. This decrease is only half of what the FDA considers a clinically significant response. Perhaps this disappointing result occurred because of the inability of these basal only CIDAAs to recommend changes in therapy to control daytime glucoses.
A number of studies have shown that clinicians using comprehensive CIDAAs significantly (P <.05) lowered HbA1c levels (Table 4). However, to the author’s knowledge, only Insulin Insights is currently available for direct treatment of insulin-requiring patients with comprehensive CIDAAs although one of the co-founders of Hygieia still supports patients remaining on d-Nav. Importantly, using Insulin Insights does not remove patients’ diabetes care from their PCCs but effectively facilitates their insulin management.
Effect of Comprehensive Computerized Insulin Dose Adjustment Algorithms on Glycemic Control.

Estimated HbA1c calculated from average glucoses. 9
NP, not provided; SMBG, self-monitored blood glucose that patient had to enter into program.
A potential limitation is missing some papers describing CIDAAs. If so, they were also missed in the reviews.30,31,37
In conclusion, Insulin Insights can interact with more than 60 glucose meters and CGM devices, handle all FDA-approved insulin preparations, and analyze glucose patterns and recommend dose adjustments within minutes to PCCs whose patients use any one of 11 different insulin regimens. These easily scalable comprehensive CIDAAs enable PCCs to significantly lower HbA1c levels, save time10,11 to address non-diabetes issues, and/or see additional patients and learn how to better adjust insulin doses by matching the glucose patterns and recommendations of Insulin Insights with the subsequent glycemic responses of their patients. In the longer term, the use of Insulin Insights by PCCs should improve glycemic control in patients taking insulin, result in less microvascular complications, and thus lower medical care costs related to diabetes.
Supplemental Material
sj-png-1-dst-10.1177_19322968241306127 – Supplemental material for The Effective Use by Primary Care Clinicians of a Comprehensive Computerized Insulin Dose Adjustment Algorithm
Supplemental material, sj-png-1-dst-10.1177_19322968241306127 for The Effective Use by Primary Care Clinicians of a Comprehensive Computerized Insulin Dose Adjustment Algorithm by Mayer B. Davidson in Journal of Diabetes Science and Technology
Footnotes
Abbreviations
CE, Conformite Europeenne; CGM, continuous glucose monitoring; CHO, carbohydrate; CIDAA, computerized insulin dose adjustment algorithms; eHbA1c, estimated HbA1c; FDA, Federal Drug Administration; HIPAA, Health Insurance Portability and Accountability Act; NP, nurse practitioner; PCC, primary care clinician; RPM, remote patient monitoring.
Declaration of Conflicting Interests
The author declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The author is the Chief Medical Officer of Mellitus Health, Inc. The author takes sole responsibility for the contents of this review.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
