Abstract

Keywords
Gut dysbiosis observed in diabetes has been shown to result in elevated levels of lipopolysaccharide (LPS) through the impaired epithelial barrier and increased intestinal permeability. 1 This phenomenon, known as metabolic endotoxemia, is believed to contribute to the development and persistence of low-grade inflammation in people with type 1 diabetes (T1D). 2 Presepsin is expressed on the surface of monocyte/macrophage and is involved in the recognition of pathogen ligands, including LPS. Previous studies have shown that presepsin is a reliable biomarker for the detection of bacterial infections and sepsis. 3 Based on the hypothesis that increased circulating LPS concentrations should be accompanied by a respective upregulation of presepsin levels, we recently showed that presepsin can serve as a surrogate marker of glycemic control in infection-free individuals with diabetes. 4 Given that glycemic variability and poor glycemic control are key drivers of inflammation, we assumed that presepsin values could also correlate with continuous glucose monitoring (CGM) metrics in individuals with T1D.
For this pilot study, we recruited 20 subjects with T1D (mean age 35.5 years) treated with insulin pumps (n = 6) or multiple daily injections (n = 14) who were free of acute or chronic infections and other inflammatory disorders, such as autoimmune diseases or malignancies. Twelve patients used CGM. Based on their glycated hemoglobin (HbA1c) values, the participants were classified into well-controlled (HbA1c < 7%) and uncontrolled (≥7%) groups. Presepsin was determined in serum using an ELISA kit (Wuhan HealthCare Biotechnology Co., Wuhan, Hubei, China). From the last 14-day CGM recordings, the following metrics were extracted: time in range (TIR), time above range (TAR), time below range (TBR), glucose management indicator (GMI), coefficient of variation, and average glucose values. The target glucose range was set between 70 (minimum value) and 180 (maximum value) mg/dl for all patients. The Spearman rank correlation coefficient was used to express the correlations between presepsin values and CGM metrics. All study participants gave their informed written consent before enrollment in the study, and the study protocol was approved by the Scientific Council of the Hippokration General Hospital of Thessaloniki (approval number 47699/23-10-2023).
There were no significant differences in presepsin levels between the well-controlled and poor-controlled groups (2.22 [4.20] vs 2.48 [4.04] ng/ml, P = .43). As shown in Figure 1, presepsin levels presented a positive correlation with GMI (r = .575) and a negative correlation with TIR (r = −.525), which in both cases marginally missed statistical significance (P = .06 and P = .07, respectively). In addition, we calculated the Glycemia Risk Index (GRI), a composite metric for the quality of glycemia from CGM tracings, 5 and found a positive correlation with presepsin values (r = .423, P = .05).
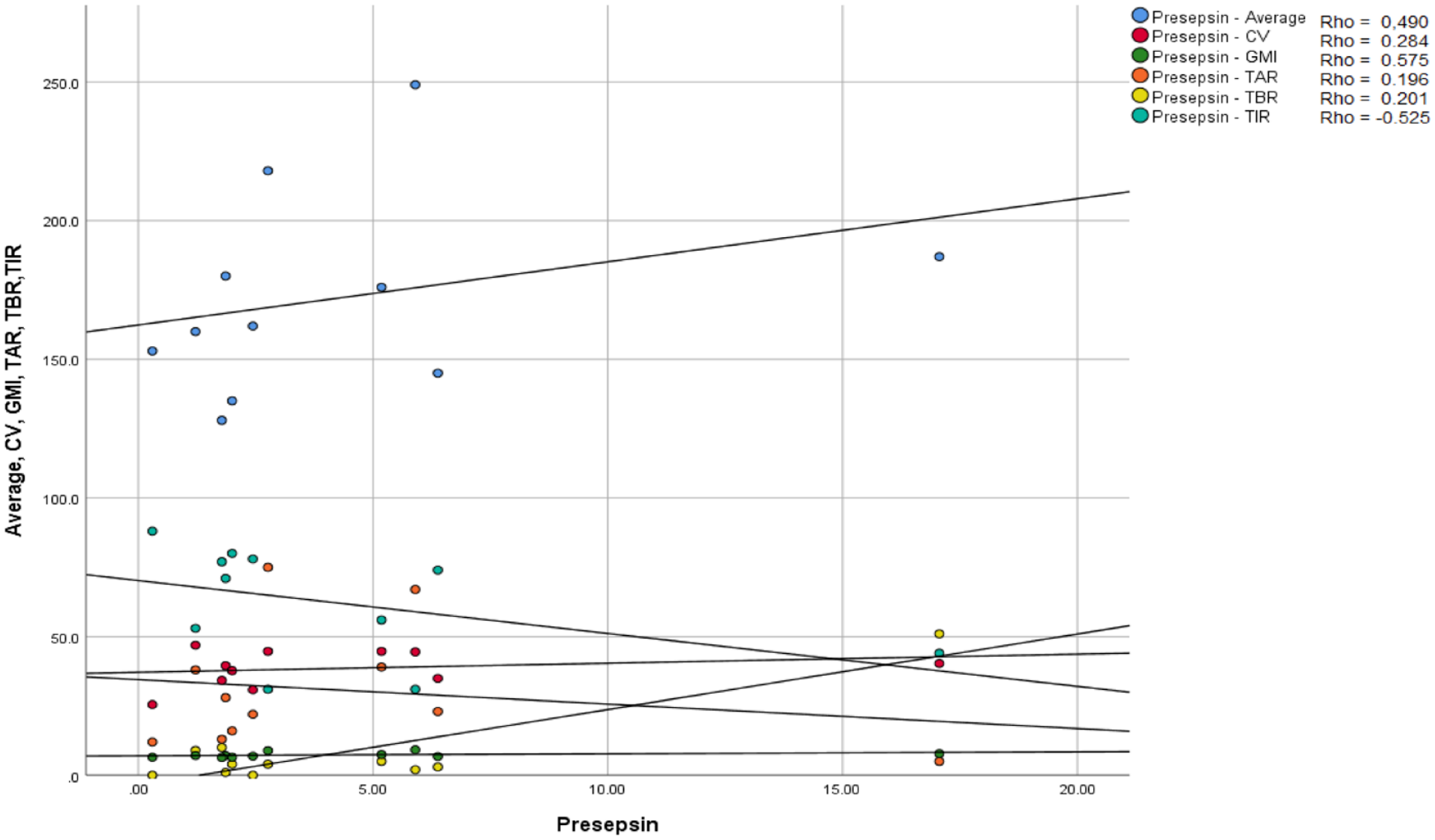
Correlation between presepsin values and CGM metrics.
To our knowledge, this is the first study in the literature investigating the relationship between presepsin levels and CGM data in people with T1D. We observed a trend toward an association between glycemic control expressed by CGM metrics and circulating presepsin concentrations. These data support the notion that intestinal dysbiosis is related to inadequate metabolic control in T1D, either as a cause or as a consequence. They also confirm in a T1D sample our previous observations regarding the possible value of presepsin in reflecting metabolic control in people with diabetes in the absence of infection. Interestingly, presepsin appears to be affected not only by hyperglycemia but also by low glucose levels, considering that GRI is based on weighted combinations of TBR (the hypoglycemia component) and TAR (the hyperglycemia component). It is possible that a larger number of participants would have improved the potential of the study to establish significant correlations. Furthermore, the pilot character renders the findings hypothesis-generating, warranting additional confirmation in larger samples.
Footnotes
Abbreviations
CGM, continuous glucose monitoring; GMI, glucose management indicator; GRI, glycemia risk index; HbA1c, glycated hemoglobin; LPS, lipopolysaccharide; T1D, type 1 diabetes; TAR, time above range; TBR, time below range; TIR, time in range.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
