Abstract
Managing data from continuous glucose monitoring (CGM) systems presents challenges to health care provider teams that rely on the electronic health record (EHR) during patient visits. A method of integrating CGM data with the EHR that relies on the Dexcom API was developed by Northwestern Medicine and Dexcom to address these challenges. Here, we describe the data management steps and user interface of the integrated system. Providers can access patients’ historical and latest daily CGM data in the form of modal day plots and stacked columns showing time in various glucose concentration ranges. The integration facilitates the acquisition, storage, analysis, and display of CGM data within an EHR system and may be appropriate for deployment in other health care facilities.
Introduction
Continuous glucose monitoring (CGM) systems are a centerpiece of modern diabetes management. Continuous glucose monitoring–generated data are used to assess glycemic status, guide insulin delivery systems, and prompt timely therapeutic interventions. Retrospective analysis of CGM data can assist clinicians to make appropriate therapy modifications to achieve glucose targets and prevent diabetes-related complications. 1 Continuous glucose monitoring use has been expanding to different areas of health care, including primary care 2 and telemedicine.3,4 However, despite the benefits of CGM and its expanded uses, CGM data are not easily accessible to clinicians primarily because they are not widely integrated with electronic health records (EHRs).
Growing adoption of CGM, combined with an undersupply of endocrinologists, suggests that primary care teams will increasingly need to familiarize themselves with and analyze CGM data during routine care. For clinicians and patients, accessing CGM data in outpatient settings involves multiple processes to retrieve data from several manufacturer-specific portals. Clinical staff bear the additional burden of manually importing data into the patient’s EHR. There are also institutional and financial barriers such as contracting needs, software costs, and liability considerations. 2 Such barriers hinder the expansion of CGM technology use in outpatient settings. A survey of 21 pediatric and adult diabetes clinics reported using seven different web-based portals to access patient data yet only one clinic reported CGM-EHR integration. 3
With a large majority of office-based clinicians using an EHR system, 5 there is an urgent need to integrate CGM data directly into clinician workflows. Making CGM data available in the EHR may vastly improve diabetes care in outpatient settings by allowing clinicians to access and interpret data more efficiently and provide their patients with more relevant education. 6 We integrated CGM (G6, Dexcom, Inc., San Diego, California) data with the Epic (Epic Systems, Verona, Wisconsin) EHR using the Dexcom API (developer.dexcom.com).
Methods
The Northwestern Medicine CGM Remote Physiologic Monitoring (CGM-RPM) Project aimed to simplify access to CGM data within Epic. The Dexcom API utilizes the OAuth 2.0 standard, allowing individuals to securely authorize sharing of their CGM data with third-party applications. This solution eliminates the need for third-party EHR integration companies, simplifies the clinician workflow by not requiring repeated orders within their EHR system, and provides greater flexibility in interpretation and display.
A team from the health center’s Information Services department developed the integration solution, including building the patient-facing enrollment platform and the data management workflow from the Dexcom API to Epic. The development team embedded a custom web application called My Home Devices into the MyNM portal, a branded version of Epic MyChart (MyChart, Epic Systems), which allows patients to integrate device data from external vendors. Once patients completed authentication and authorization steps, Dexcom provided an API token to allow data retrieval through the Dexcom API. The development team created custom web services to manage each patient’s API token using Epic Interconnect, an API gateway that allows custom applications to retrieve and store EHR data. Every morning at 4:00
In preparation for launch of the integration, provider education was conducted with live demonstrations of the workflow. Clinicians were also provided with step-by-step workflow tip sheets. Patient education was provided through flyers available in the clinic and automated MyNM messages with enrollment instructions.
Results
After a clinician places a one-time order for CGM data integration in Epic, patients receive a message in MyNM that explains how to link their EHR and Dexcom CGM account through the My Home Devices application. Clicking the “Link Account” button redirects patients to a Dexcom login page to enter their credentials, authorizing MyNM to access their data. After completing the login process, CGM data are integrated with the patient’s EHR, whereupon clinicians can interact with the data in Epic. The initial setup tasks for clinicians and patients to link Dexcom data to the EHR are outlined in the process map depicted in Figure 1a. Similarly, Figure 1b shows how uploaded data are requested every day through the Dexcom API. The integration solution produces custom data visualizations in the EHR that allows clinicians to view single-point data or data trends across a date range. Figure 2 shows the CGM dashboard as displayed to Northwestern Medicine providers. Hovering the cursor over the graph lines reveals the underlying numerical values.
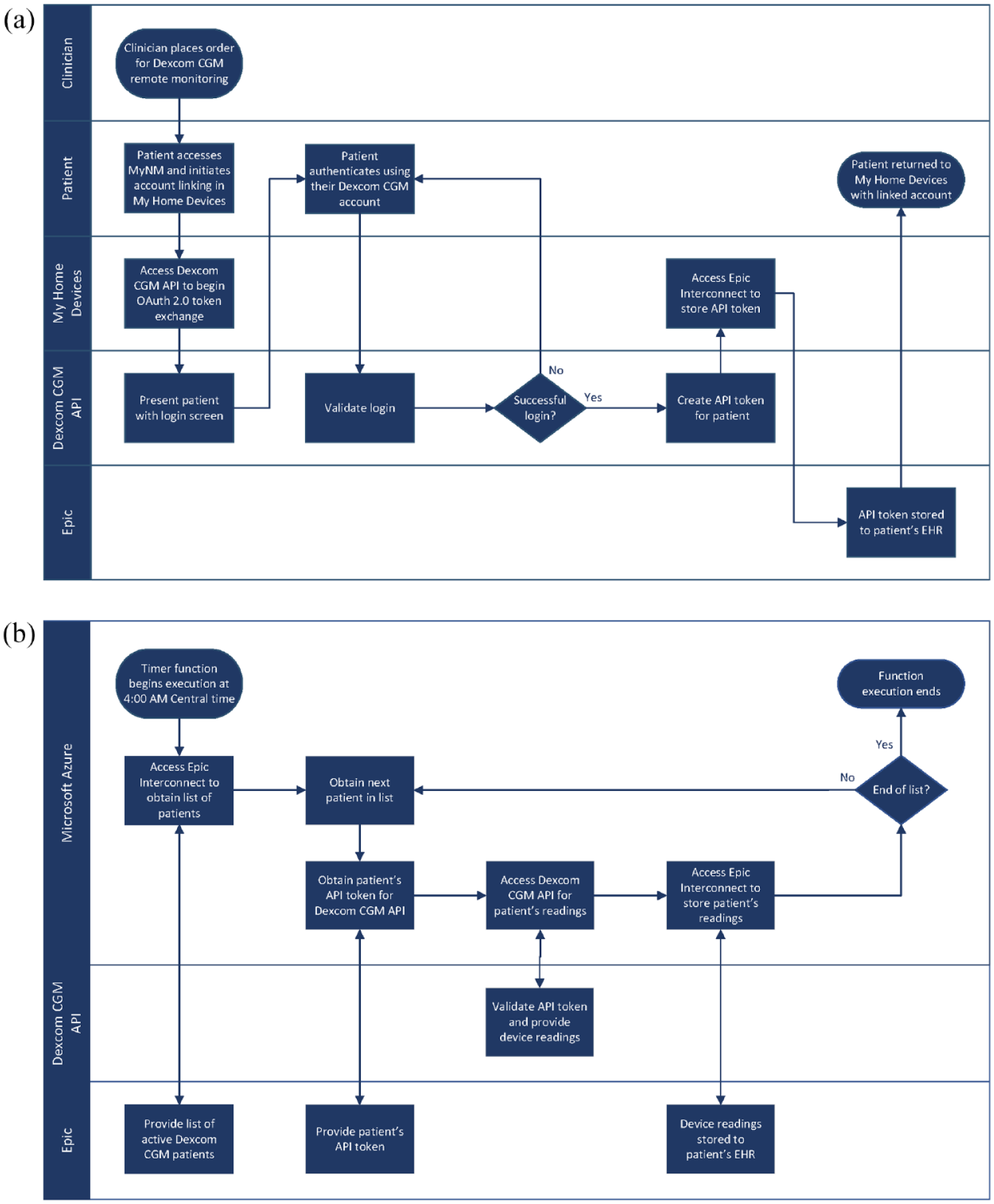
(a) Setup tasks for clinicians and patients to initiate CGM-EHR integration. (b) The daily token-based retrieval of CGM data via the Dexcom API.
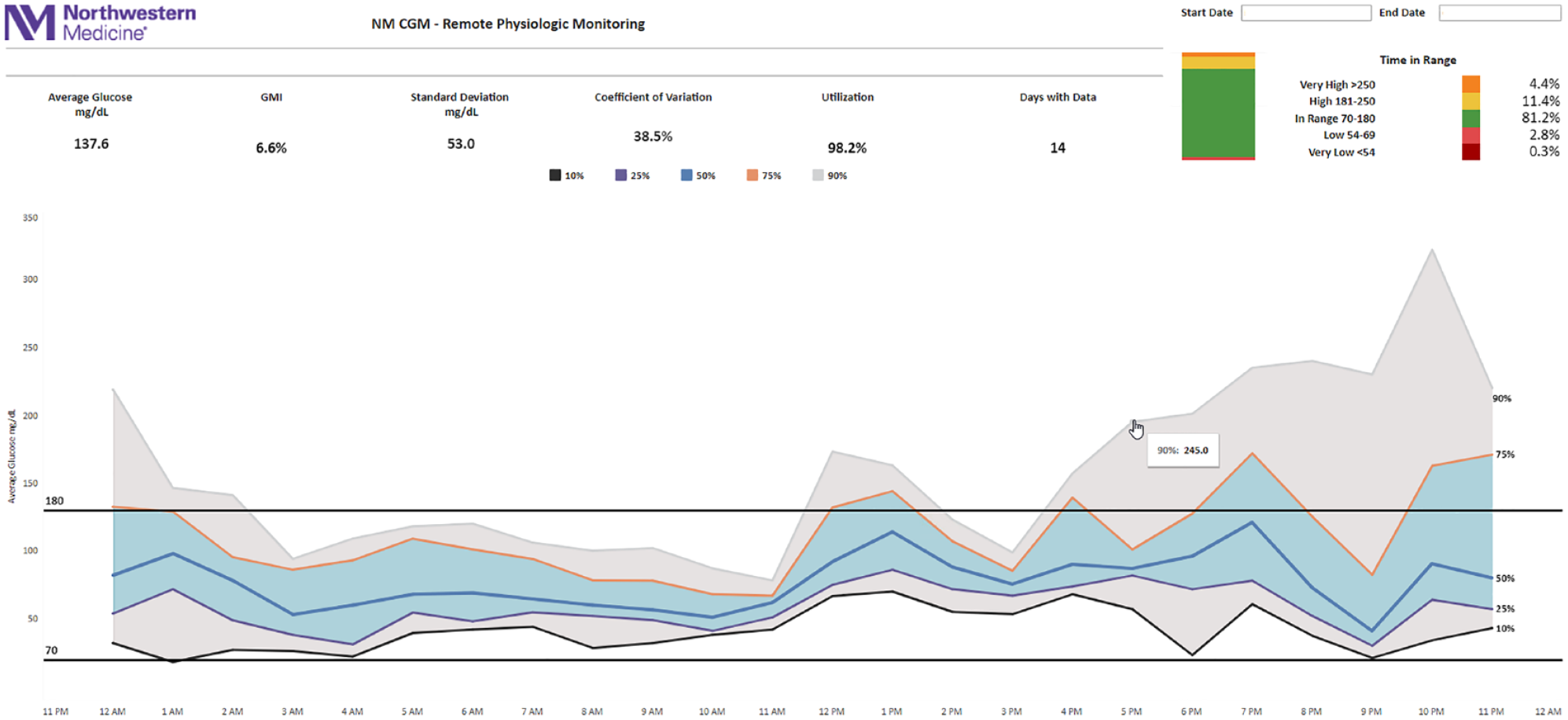
A dashboard providing CGM data during a modal day and as a stacked column showing time in various glucose concentration ranges.
Discussion
Continuous glucose monitoring technology has become standard of care for people with diabetes and is supported by major professional societies.8-10 Continuous glucose monitoring use is an integral tool in clinical practice to reduce therapeutic inertia and optimize diabetes care, whether in the endocrinology setting or primary care. 1 Nevertheless, accessing data can be time-consuming and requires the use of multiple software programs. 2 The integration solution with Epic using the Dexcom API that we report offers a method for clinicians to easily interact with CGM data without additional manual entry and order requests in the EHR. Early solutions that integrated CGM data used third-party smartphone applications 11 and physician computer request modules to send data directly to the EHR server. 12 However, these solutions raise concerns about data accessibility. A previous solution using Dexcom data could only provide one-time snapshot reports which had to be requested at each patient appointment. 12 The solution also required a separate EHR order to obtain patient consent to allow data sharing before clinicians could submit a CGM data request. The current solution utilizes a no-cost, public API that does not require a high-commitment partnership with the manufacturer or a cumbersome patient consent process, making this solution more replicable in other institutions. Another integration solution with a different CGM manufacturer used a physician computer request system mediated by a third-party API. 13 The integration described here builds on this work by eliminating the need for repetitive EHR orders and contracting with a third-party API company.
The Integration of Continuous Glucose Monitoring Data into the Electronic Health Record (iCoDE) Project 2 is a consortium that developed consensus recommendations outlining best practices for CGM-EHR integration. The solution we describe utilizes the iCoDE consensus recommendations, including a data pull strategy, a CGM account linkage strategy that simultaneously establishes patient identity and acquires consent, and data readily displayed in a dedicated space in the EHR. The solution builds on iCoDE recommendations by providing a platform through the EHR to view interactive data visualizations and a pathway for patients to self-authenticate their identity and allow data sharing using their Dexcom account credentials.
Additional benefits of CGM-EHR integration include more consistent EHR documentation, 14 possible capacity for remote patient monitoring, and time savings. One example of time savings is seen in a glucose monitoring dashboard that switched from an early version requiring accessing a separate CGM data portal to direct data integration. 15 This update reduced the estimated time spent reviewing data per patient by 37% and increased the estimated clinic patient capacity by 58%. 15 Although the current implementation did not measure appointment or staff time savings, we anticipate that it may serve this goal by eliminating the need to manually access software portals during patient appointments.
Strengths of the current solution include the no-cost access to the Dexcom API, minimal technical requirements to establish data sharing connection with the API, and CGM values that are not restricted by proprietary reporting software. The integration supports meaningful use criteria of Certified Electronic Health Record Technology 16 and documentation for insurance billing.2,17 While the API integration described here is specific to Northwestern Medicine’s instance of Epic, it was built on open web standards and technologies that are amenable to wider use with most EHR vendors in the United States. Future studies are needed to monitor the implementation of this CGM-EHR integration model in clinical practice and its impact on ongoing care of the individual with diabetes.
Footnotes
Abbreviations
CGM, continuous glucose monitoring; CGM-RPM, CGM remote physiologic monitoring; EHR, electronic health record; iCoDE, integration of continuous glucose monitoring data into the electronic health record project.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: GA has received research support to her institution Northwestern University from Fractyl Health, Insulet, Tandem Diabetes, and Welldoc. GA has received consulting fees from Dexcom and Insulet. RC, RB, PC, and NN have nothing to disclose. AZ, SBA, JW, and AH are employees of Dexcom.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
