Abstract
Objective:
Dietary self-management is one key component to achieve optimal glycemic control. Advances in mobile health (mHealth) technology have reduced the burden of diabetes self-management; however, limited evidence has been known regarding the status of the current body of research using mHealth technology for dietary management for adults with type 2 diabetes.
Methods:
Literature searches were conducted electronically using PubMed, CINAHL (EBSCO), Web of Science Core Collection, PsycINFO (Ovid), EMBASE (Ovid), and Scopus. Keywords and subject headings covered dietary management, type 2 diabetes, and mHealth. Inclusion criteria included studies that applied mHealth for dietary self-management for adults with type 2 diabetes and were published in English as full articles.
Results:
This review (N = 15 studies) revealed heterogeneity of the mHealth-based dietary self-management or interventions and reported results related to physiological, dietary behavioral, and psychosocial outcomes. Twelve studies applied smartphone apps with varied functions for dietary management or intervention, while three studies applied continuous glucose monitoring (CGM) to guide dietary changes. Among 15 reviewed studies, only three of them were two-arm randomized clinical trial (RCT) with larger sample and 12-month study duration and 12 of them were pilot testing. Nine of 12 pilot studies showed improved HbA1c; most of them resulted in varied dietary changes; and few of them showed improved diabetes distress and depression.
Conclusion:
Our review provided evidence that the application of mHealth technology for dietary intervention for adults with type 2 diabetes is still in pilot testing. The preliminary effects are inconclusive on physiological, dietary behavioral, and psychosocial outcomes.
Approximately 37.1 million (~14.7%) of US adults have diabetes, with 90% to 95% having type 2 diabetes. 1 Globally, a total of 387 million people worldwide have diabetes, and the number is expected to rise to 592 million by 2035. 2 The estimated total cost (direct and indirect) attributed in the United States was 327 billion in 2017. 3 Substantial evidence supports aiming for HbA1c <7% as the glycemic goal for decreasing the incidence of diabetic complications (eg, cardiovascular disease, retinopathy, nephropathy, and neuropathy). 2 However, the American Diabetes Association has suggested that less than 30% of individuals achieve the recommended glycemic goal (HbA1c < 7%). 4 The strategies for achieving HbA1c < 7% involve performing dietary self-management, which requires data organization and arithmetic skills, including tracking food intake, estimating food portion size, and calculating carbohydrate intake. 5 Mastering such skills for ideal dietary self-management are usually burdensome and challenging for most of individuals with diabetes. 6
Advances in mHealth technology (eg, mobile phones, patient monitoring devices, personal digital assistants, and other wireless devices)
7
have reduced the burden of diabetes self-management.
8
Reviews by Wu
Presently, there has been limited synthesis of the research evidence regarding the use of mHealth technology for dietary management for adults with type 2 diabetes. There are no current or underway systematic or scoping reviews that have explored the types and key components of the mHealth technologies used in the research on dietary interventions for type 2 diabetes. Moreover, there has not been a review of how these mHealth dietary interventions impact physiological (eg, HbA1c and weight), dietary behavioral (eg, dietary behavior changes and healthy eating), and psychosocial (eg, distress, quality of life, and depressive symptoms) outcomes. Thus, this review will seek to synthesize the current body of published research on the use of mHealth technology for dietary management for adults with type 2 diabetes to characterize these interventions and their outcomes.
Methods
Protocol
Because the purpose of this review is to systematically scope the current body of research literature on this topic to characterize the interventions and outcomes that are under investigation in the field, a scoping review was selected as the most appropriate methodology. 14 This review was conducted in accordance with the protocol registered at https://osf.io/edwz6.
Search Strategies
The search strategy aimed to locate published studies, beginning with an initial limited search of PubMed, CINAHL, and Web of Science Core Collection. The text words contained in the titles and abstracts of relevant articles, and the index terms used to describe the articles were then used to develop a full search strategy for PubMed (Table 1). The PubMed search strategy, including all identified keywords and index terms, was then adapted for CINAHL (EBSCO), Web of Science Core Collection, PsycINFO (Ovid), EMBASE (Ovid), and Scopus (search queries for each database are available at https://osf.io/s5xqh). The reference lists of all included sources of evidence were screened for additional studies. Studies published in English between January 2011 and June 2022 were eligible for inclusion.
Search Strategy.
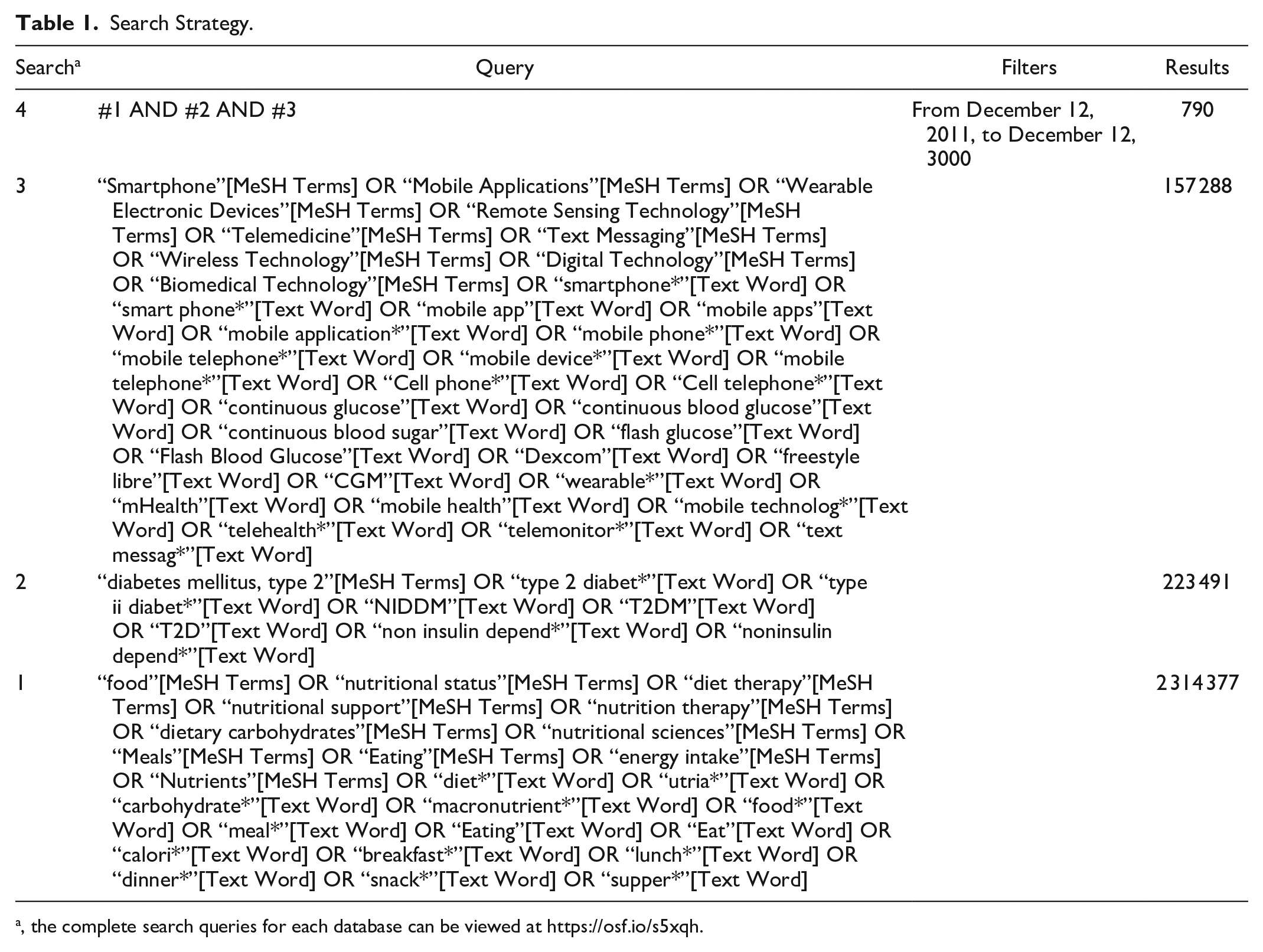

, the complete search queries for each database can be viewed at https://osf.io/s5xqh.
Inclusion and Exclusion Criteria
To be eligible for inclusion in this scoping review, studies included (1) adult participants with type 2 diabetes; (2) the application of mHealth technology for diabetes dietary self-management; and (3) experimental and quasi-experimental study designs, including randomized controlled trials, nonrandomized controlled trials, pre-post studies, interrupted time-series studies, and feasibility studies.
Studies were excluded if: (1) the participants were exclusively patients with type 1 diabetes and/or gestational diabetes; (2) they focused on pediatric patients, patients with cancer or HIV, patients who had gone through gastric bypass, and inpatients, as the dietary intake for these conditions need special attention in nutrition; (3) the technological component was limited to the use of telephones or the Internet; and (4) they were qualitative studies, technology algorithm testing/safety studies, study protocols, review articles, dissertations, and commentaries/opinion pieces and conference abstracts/posters.
Study Selection
Following the database searches, all identified citations were collated and uploaded into EndNote 20, and duplicates were removed. The pooled set of records were uploaded into Covidence for eligibility screening. Following a pilot test of the screening criteria, titles and abstracts were screened by two independent reviewers for assessment against the inclusion criteria for the review. Potentially relevant sources were retrieved in full, with the exception of three records for which the full text could not be located. The full texts of relevant citations were assessed in detail against the inclusion criteria by two independent reviewers. Any disagreements that arose between the reviewers at each stage of the selection process were resolved through discussion, and with an additional reviewer.
The results related to the identification of eligible studies are summarized in Preferred Reporting Items for Systematic Reviews and Meta-Analyses (Figure 1). Database searches yielded 3874 citations, leaving 1559 titles and abstracts to be screened for eligibility after removing duplications. Following full-text retrieval of 134 potentially relevant articles, 120 were subsequently excluded, leaving 14 articles that applied mHealth for dietary management for individuals with type 2 diabetes that were eligible for inclusion in the review. The references of the included articles were searched manually, resulting in an additional 1263 references to review. This relevance screening of these results located five additional relevant records, from which one additional eligible article was found. As a result, a total of 15 articles were included in this review. Studies were summarized based on the following categories: authors/country, sample size/characteristics, study design, intervention components, and outcomes (Table 2).
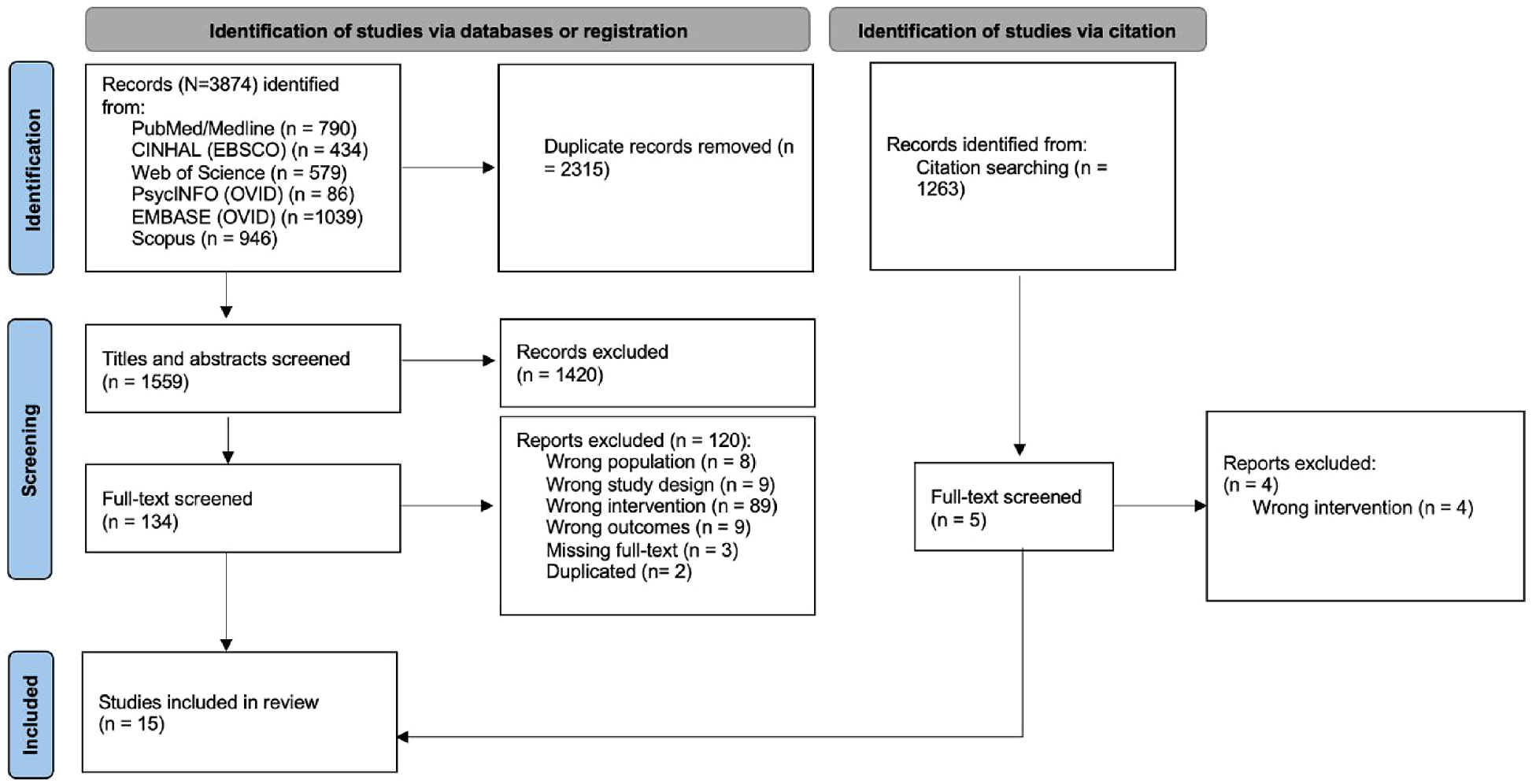
Preferred Reporting Items for Systematic Reviews and Meta-Analyses flow chart.
Studies on Dietary Self-management Using mHealth Technology.

Abbreviations: SD, standard deviation; BMI, body mass index; SMS, short message service; FBS, fasting blood sugar; GLP, glucagon-like peptide-1; CI, confidence interval; RCT, randomized clinical trial; GEM, glycemic excursion minimization; IG, intervention group; CG, control group;
Results
Description of Included Studies
Among 15 reviewed studies, four were conducted in the United States,19,23,24,30 seven were in Asia,15,18,25 -29 two were in Australia,17,20 and two were in Europe.22,31 The sample sizes ranged from 10 to 800. The participants aged from 42.3 to 60.8 years and 25.9% to 81.4% were females. Of the three studies that reported on race, the percentage of non-white participants ranged from 15% to 47.6%.23,24,30 A total of 35.5% to 100.0% participants took oral antihyperglycemic medication,19,15,22,25,26,28,29,31 11.8% to 37.8% participants injected insulin,22,25,29,31 and 23.5% to 30% had mixed oral medication and insulin.25,26 A total of six studies reported the duration of diabetes, ranging from 2.6 to 13.7 y15,19,23,27,29,31 Among 15 reviewed studies, a total of eight studies were two-arm RCT intervention,15,20,22,23,25 -28 two studies were two-arm quasi-experimental studies,18,24 and five studies were single-group intervention.17,19,29 -31 A total of 12 studies lasted less than or equal to three months,15,17 -20,23 -26,29 -31 and three lasted 12 months.22,27,28
Types of Mobile Health and the Key Components of Dietary Intervention
Among 15 reviewed studies, 12 studies applied smartphone apps with varied functions for dietary management or intervention. These apps included those with speech-recognition device and photographs of meals (ie, DialBetic), 15 image-based dietary assessment, 17 diet intake record, alarm systems, and displays of nutrient intake. 18 Smartphone apps are also used for other purposes, such as to facilitate the learning and adoption of plant-based meals, self-monitoring habits, and scheduling of coaching calls, 19 create meal plans and find recipes with nutrient information (ie, EasyNutrition), 24 act as a dietary diary (ie, Noom), 25 a mobile game player that educated the participants on healthy food intake (ie, Amoo), 26 log food and provide analysis with a graph of daily energy intake and the intake of different nutritional components being displayed (ie, Calomeal), 29 promote the Mediterranean diet (ie, EVIDENT II), and track dietary habits (ie, Vitadio). 31 Two studies provided short message service (SMS) for tailored feedback as dietary alerts and reminders, 27 or for educational tips about dietary intake. 28 Three studies applied real-time continuous glucose monitoring (RT-CGM)20,30 or blinded CGM 23 with sessions on reducing carbohydrate intake and providing substitutions.
Intervention Effects on Physiological, Dietary Behavioral, and Psychosocial Outcomes
Overall, the impact of dietary interventions using mHealth on outcomes was mixed. Among 15 reviewed studies, only three of them were two-arm RCT with larger sample and longer study duration,22,27,28 which lasted 12 months. All these three full RCTs only reported physiological outcomes (one reported HbA1c 22 and two reported glucose changes)27,28 and dietary behavioral outcomes (eg, dietary behavior changes and healthy eating), but none of these three studies reported psychosocial outcomes (eg, distress, quality of life, and depressive symptoms).
Alonso-Dominguez
Of the two-arm RCT pilot studies that lasted less than or equal to three months,15,20,23,25,26 three studies resulted in a significant reduction in HbA1c,15,23,25 one resulted in reduction in carbohydrate food consumption, 23 improvement in dietary information scores, 26 attention to high carbohydrate food, high calorie food, 26 and diet behavior, 20 and significant improvement in diabetes distress20,23 and depression. 23 However, others did not result in HbA1c reduction, 20 fasting blood glucose changes,20,26 did not resulted in improving diet self-management skills.15,25 Of the two two-arm quasi-experimental studies,18,24 one resulted in a significant reduction in HbA1c, 24 and the other achieved a BMI reduction and improved dietary behavior and dietary attitude. 18 However, these two-arm studies did not show significant change in eating habits. 24 Of the five single-group interventions,17,19,29 -31 four resulted in a significant reduction in HbA1c19,29 -31 and BMI29 -31 or weight, 17 others resulted in improved in healthy dietary habits, 31 reduced in consumption of food portion size, 31 carbohydrate,30,31 protein and fat, 31 and improved dietary self-efficacy,19,31 diabetes distress, 30 and depression. 30
Discussion
This scoping review aimed to synthesize the status of the current body of research using mHealth technology for dietary management for adults with type 2 diabetes. Fifteen studies reported using either mHealth apps or CGM for dietary self-management or intervention; however, the use of mHealth technology for dietary intervention for adults with type 2 diabetes was largely in the pilot testing stage. The pilot testing showed promise in improving glucose or weight control, improving dietary management behaviors, reducing carbohydrate intake, or reducing diabetes distress and depression. However, the preliminary effects were inconclusive on physiological outcomes (eg, HbA1c and weight), dietary behavioral outcomes (eg, dietary behavior changes and healthy eating), and psychosocial outcomes (eg, distress, quality of life, and depressive symptoms), because the dietary interventions using mHealth and reported outcomes were heterogeneous, which made it difficult to synthesize the outcomes.
Although dietary self-management is a key component of glycemic control and mHealth is advancing for diabetes management, the current body of research using mHealth technology for dietary management for adults with type 2 diabetes is limited. Wu
Our review showed heterogenous types of mHealth and components of dietary interventions. Most of studies applied smartphone apps with features such as speech recognition and photographs of meal, image-based dietary assessment, diet intake record, alarm systems, and displays of nutrient intake. These features provide the opportunity to reduce the burden of dietary management for individuals with diabetes. Three studies applied CGM with sessions on reducing high carbohydrate choices and suggesting substitutions, indicating that CGM may be a useful and educational tool to allow individuals with diabetes to understand how their dietary intake impacts their postprandial glucose levels and glucose variability, particularly the consumption of high carbohydrate food.
One limitation of this review is that the mHealth-based interventions for dietary self-management were conducted in a less diverse population. Among 15 reviewed studies, only three studies reported race and seven studies were conducted in Asian populations, indicating that such types of interventions need to be tested in other race/ethnic populations, particularly in African Americans and Hispanics, due to the high prevalence of type 2 diabetes in these populations. 1 To the best of our knowledge, this is the first scoping review to synthesize the status of the current body of research using mHealth-based intervention for dietary self-management for adults with type 2 diabetes.
Conclusions
The present scoping review provided evidence that the application of mHealth technology for dietary intervention is still in the pilot testing stage. The preliminary effects are inconclusive on physiological, dietary behavioral, and psychosocial outcomes, largely due to the heterogeneous mHealth-based intervention for dietary self-management and the heterogeneous reported outcomes. Future full-scale studies are needed to further test the effectiveness of application of mHealth for dietary management in adults with type 2 diabetes. Future studies are also needed to test the effectiveness of application of mHealth for dietary management in diverse populations.
Footnotes
Acknowledgements
The authors acknowledge Marie Claire R Mortejo, BSN, and undergraduate student Jenelle Marius for their assistance with pilot article screening.
Abbreviations
CGM, continuous glucose monitoring; mHealth, mobile health; RCT, randomized clinical trial.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project is supported by NIH/NCATS UL1TR001445 CTSI Collaborative Translational Pilot Project Award (Yaguang Zheng, PhD), P30DK111022-08 New York Regional Center for Diabetes Translation Research (NY-CDTR) Pilot and Feasibility (P&F) Program Funding (Director: Judith Wylie-Rosett, EdD, RD; awardee: Yaguang Zheng, PhD), and R25 HL145323-01A1 Research and Education in Cardiovascular (RECV) training program (Contact PI: Victoria Vaughan Dickson, PhD, CRNP, FAHA, FHFSA, FAAN; trainee: Jenelle Marius and YiLan Zhang).
