Abstract
Background:
The COVID-19 pandemic has added to the pre-existing challenges of diabetes management in many countries. It has accelerated the wider use of digital health solutions which have tremendous potential to improve health outcomes for people with diabetes. However, little is known about the attributes and the implementation of these solutions.
Objective:
To identify and describe digital health solutions for community-based diabetes management and to highlight their key implementation outcomes.
Methods:
We searched Ovid Medline, CINAHL, Embase, PsycINFO, and Web of Science for relevant articles. A purposive search was also used to identify grey literature. Articles that described digital health solutions that aimed to improve community-based diabetes management were included in this review. We applied a thematic synthesis of evidence to describe the characteristics of digital health solutions, and to summarize their key implementation outcomes.
Results:
We included 15 articles that reported digital health solutions that primarily focused on community-based diabetes management. Nine of the 15 innovations involved were mobile applications and/or web-based platforms, and five were based on social media platforms. The majority of the digital health solutions were used for diabetes education and support. High engagement, utilization, and satisfaction rates with digital health solutions were observed. The use of digital health solutions was also associated with improvement in self-management, taking medication, and reduction in glycated hemoglobin (HbA1c) levels.
Conclusion:
COVID-19 triggered digital health solutions have tremendous potential to improve health outcomes for people with diabetes. Further studies are needed to evaluate the sustainability and scale-up of these solutions.
Introduction
Over the last few decades, the burden of non-communicable diseases (NCDs) has increased rapidly globally including in low- and middle-income countries (LMICs). Non-communicable diseases are now responsible for more than 70% of deaths worldwide, three-quarters of which occur in LMICs. 1 Cardiometabolic conditions are one of the major NCDs of public health importance worldwide. In 2021, an estimated 537 million adults were living with diabetes and 3 in 4 adults with diabetes live in LMICs.2,3 Several previous studies have reported that Disability-adjusted Life Years (DALYs) attributed to diabetes showed an increasing trend in developing countries. 4
Besides the increasing prevalence of type 2 diabetes, the gaps between awareness of diabetes, treatment, and control rates are substantial. For instance, based on the 2017-2018 NCD monitoring survey in India, among those with diabetes, only 45.8% were aware of their status and 36.1% were on diabetes treatment. Of this, 15.7% had their blood glucose under control. 5 Control rates were similar in China—among people with diabetes, 40.3% were aware of their status, 62.9% were receiving treatment, and 16.9% had controlled diabetes. 6 Substantial gaps between awareness, treatment, and control rates were also observed in Africa and Latin America.7,8 A complex interaction of factors, including lack of diabetes awareness, behavioral risk factors, and limited access to and quality of health services, are the contributing factors to the high prevalence of diabetes. 9
Before COVID-19, the management of diabetes both at community and health facility levels had multiple challenges including low rates of taking medications as prescribed and implementation of recommended lifestyle changes. 10 The COVID-19 pandemic has aggravated these pre-existing challenges in diabetes management. 11 The need for a rapid shift of focus of the entire health system to COVID-19 prevention and control created a disruption in the continuum of care significantly impacting the delivery of care to achieve optimal glycemic control levels among people with diabetes. 12
On the other hand, the COVID-19 pandemic has also accelerated many digital health innovations that had the potential to improve diabetes management. 13 To cope with the challenge posed by the COVID-19 pandemic, health systems in many low- and middle-income countries rapidly pivoted to develop and implement various digital health innovations for community-based diabetes management. These innovations aim to mitigate the health system impacts of the COVID-19 pandemic and have the potential to improve the accessibility and equity of service delivery in the long term if they are appropriately implemented and scaled up.
However, the design and implementation of digital health solutions for community-based diabetes management during the COVID-19 pandemic were rapid. As a result, most of the innovations haven’t been well integrated into the health system. Moreover, strategies for long-term sustainability and wider scale-up of the innovations have not been put in place. To strategically align digital health innovations within health systems, it is crucial to generate strong evidence that can inform the sustainability and scale-up of these innovations. This review applied an implementation science lens to identify and describe key digital health solutions targeted at community-based diabetes management and to summarize their implementation outcomes.
Methods
Study Design
In this study, we applied a scoping review of implementation outcomes to identify and describe digital health innovations for community-based diabetes management in the COVID-19 context. This design was chosen as it helps identify knowledge gaps and scope a body of literature using a broad range of evidence from both published sources and gray literature. 14
Scope of the Review
This review purposively focused on digital health solutions (telephone-based, web/applications, and social media). The specific digital health solutions of interest were those primarily aimed at community-based diabetes management—the management of diabetes through community-based interventions. In this synthesis, the characteristics of the innovations, their primary purposes, implementation outcomes, and success and challenges, were described. After the synthesis of evidence, this review also proposed strategies to improve sustainability and scale-up of digital health solutions.
Search Strategy
The search strategy included a broad systematic search of literature from Ovid Medline, CINAHL, Embase, PsycINFO, and Web of Science for relevant articles. We limited the search to the publication period between January 1, 2020, and February 22, 2022, as COVID-19 the pandemic period was our focus. The search terms included keywords for digital health solutions (synonyms of Digital health solutions), problem (diabetes, NCDs), and context (COVID-19). In addition, a purposive search was conducted from general search engines, references of review articles, and web pages of relevant organizations.
The preliminary screening of titles and abstracts was broad enough to capture articles potentially relevant to the study. Potentially relevant articles were retrieved in full text for a more detailed review. Two authors (T.H. and A.I.), in consultation with the wider team, conducted title and abstract screening.
Inclusion/Exclusion Criteria
To be included in this review, articles and other sources were expected to
Address community-based diabetes management (peer support, community health worker-led interventions, or self-management by people with diabetes).
Involve digital health solutions (applications, online platforms, or telephone-based services).
Developed, adapted, or scaled up in response to the impacts of COVID-19.
Designed to be applied or applied at the community-level.
Studies that report on the use of digital health solutions primarily between healthcare providers and people with diabetes for clinical treatment were excluded. Studies that reported the use of digital health solutions for community-based diabetes management before the emergence of COVID-19 were also excluded.
Extraction of Evidence
We included various characteristics of the innovations in the data abstraction templates. Besides, data related to the study/program characteristics, intervention, target population, implementation outcomes challenges/facilitators and outcomes were extracted.
Synthesis of evidence
We conducted a thematic synthesis of the extracted evidence to describe the characteristics of digital health solutions and their implementation outcomes. Using interpretive synthesis, we proposed potential strategies for further adaptation and scale-up of digital health solutions. Specific digital health innovations were used as an example to illustrate implementation outcomes, challenges, and success factors.
Findings
Characteristics of Included Articles
A total of 3765 citations were identified from the systematic search of the literature for January 1, 2020, and February 22, 2022. From these, 745 duplicates were removed. After screening the title and abstract 69 articles were retained. Additional purposive and retrospective searches from references of systematic and scoping reviews resulted in 14 additional articles. As shown in Figure 1 below, 83 articles underwent a detailed review.
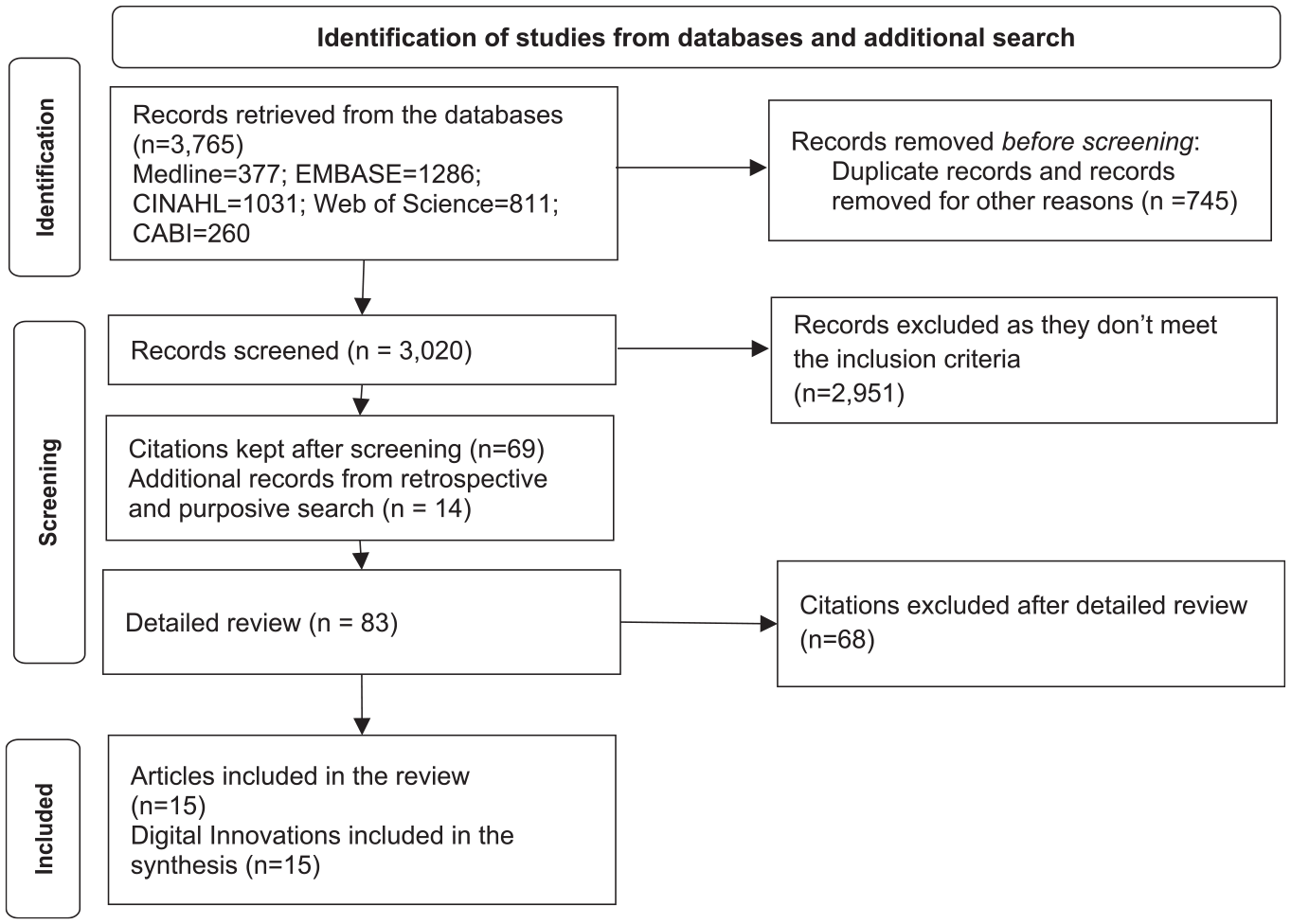
Flow chart of study identification, screening, and selection.
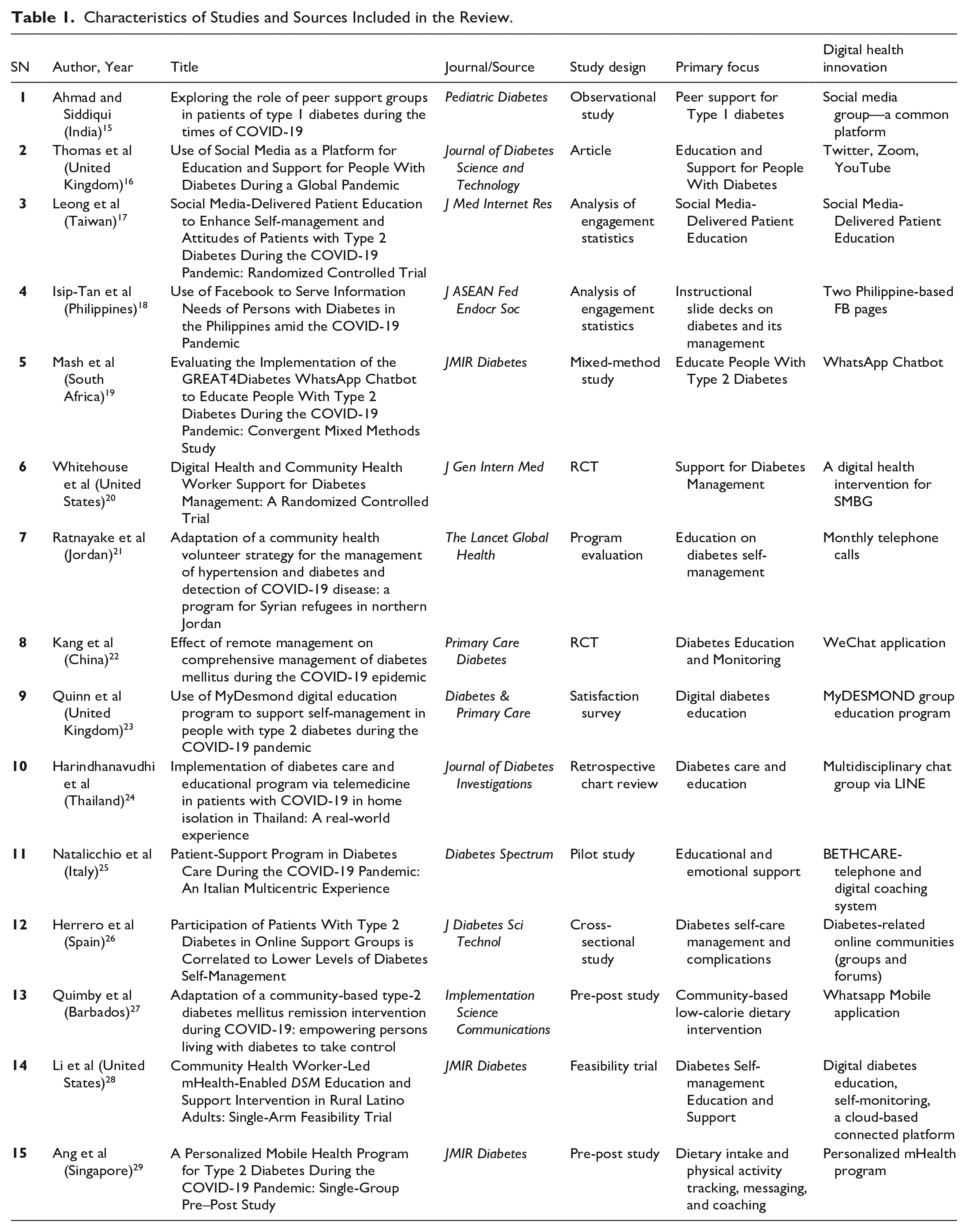
A total of 15 relevant articles from 13 countries that reported digital health solutions focusing on community-based diabetes management were included in this review. Of these, 14 were journal articles and 1 was a conference abstract. From the review of the 15 digital health solutions, 9 were based on common social media platforms. Two of the 15 digital health solutions have applied a telephone-based approach (1 along with a digital coaching system). Five digital health solutions were based on apps or online platforms. However, most of these studies were small-scale feasibility and pilot studies. Details of the included articles are shown in Table 1 below.
Characteristics of Studies and Sources Included in the Review.
Core Functions of Innovations
From the detailed review of the identified digital health solutions, 7 core functions related to their primary purpose were identified and described. Some of the digital health solutions served two or more of these core functions.
Education and support: Most of the digital health solutions that were based on social media platforms provided structured health information (audio, video, text) to people with diabetes. Digital health solutions, such as the GREAT4Diabetes WhatsApp Chat bot, had a primary focus on delivering messages that were essential for people with diabetes.17,19
Peer support and coaching: Digital health solutions enabled people with diabetes to interact with peers, volunteers, or coaches.15,26 This can provide a virtual peer support mechanism for people with diabetes.
Self-monitoring of blood glucose: Digital health solutions, such as Way to Health Platform, can monitor blood glucose, interpret the values, and communicate the information to health providers. 20
Diabetes self-management: Digital health innovations, such as telephone-based support and online support groups, enabled people with diabetes to manage their diabetes.23,26
Taking medication: Expanding the role of Community Health Workers to deliver medications at home improved access to medications during COVID-19 lockdowns. 21
Tracking physical activity and diet: Digital health solutions such as Personalized Mobile Health Program integrated physical activity and diet tracker for people with diabetes. 29
Community-based dietary intervention: An online intervention using a low-calorie diet for weight loss and diabetes remission implemented within the community and supported by trained community health advocates in Barbados was an example of this. 27
Implementation Outcomes
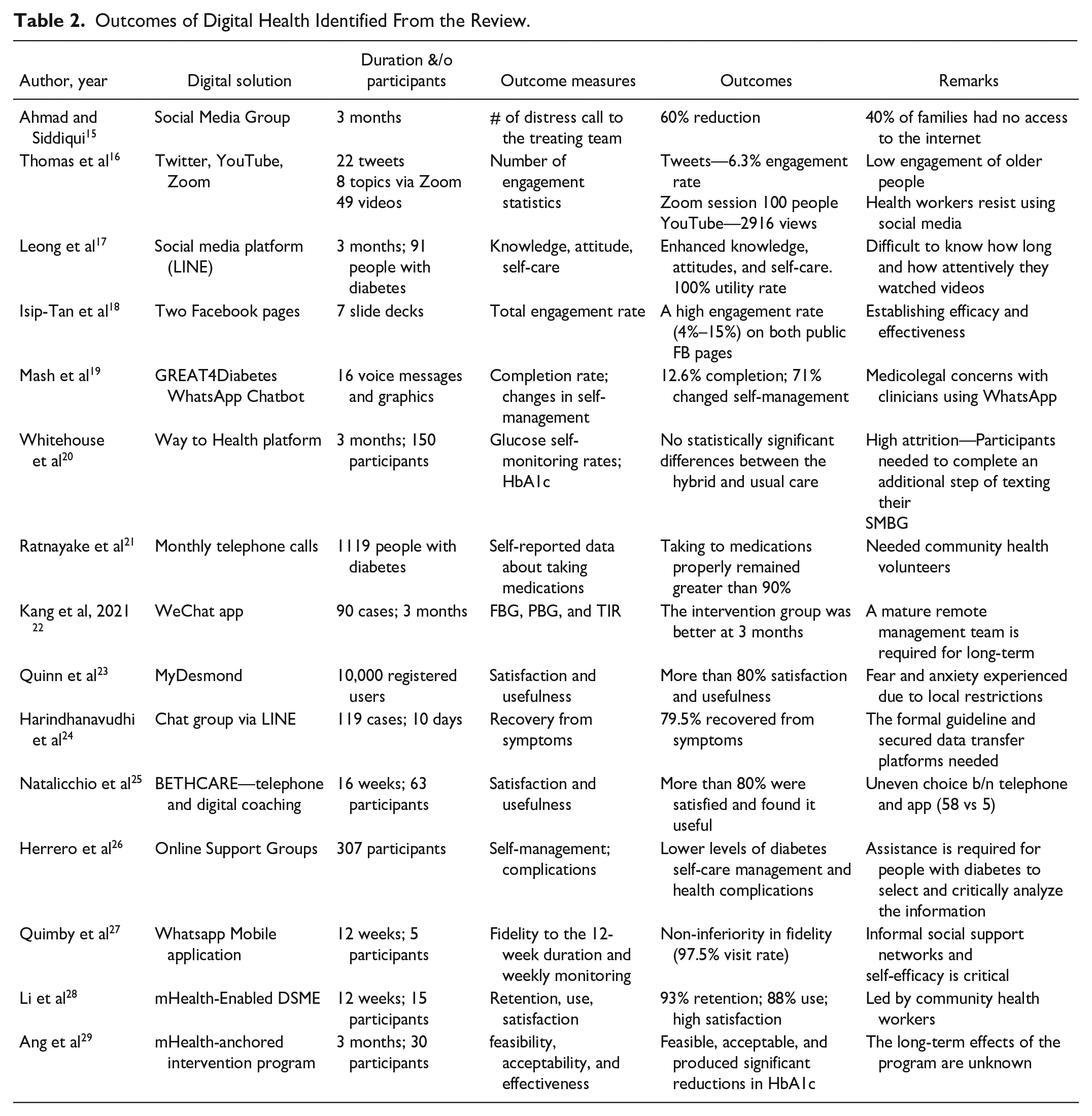
We identified 3 categories of outcomes from a detailed review of digital health solutions (see Figure 2). The first category was implementation outcomes related to peoples’ interaction with digital health solutions. This included engagement statistics (eg, number of views, hours watched) and utility rates. The second category was implementation outcomes related to the adoption of diabetes management interventions delivered through digital platforms. These included improvements in self-monitoring and self-management practices. The last category was effectiveness outcomes, that is, changes in clinical outcomes. As shown in Table 2, there was a promising level of engagement of people living with diabetes with digital health solutions. Outcomes related to the adoption of diabetes management intervention delivered using digital health solutions demonstrated non-inferiority to the usual care. However, the findings on diabetes management outcomes were only suggestive that these interventions could be effective as the evidence on effectiveness outcomes was limited.
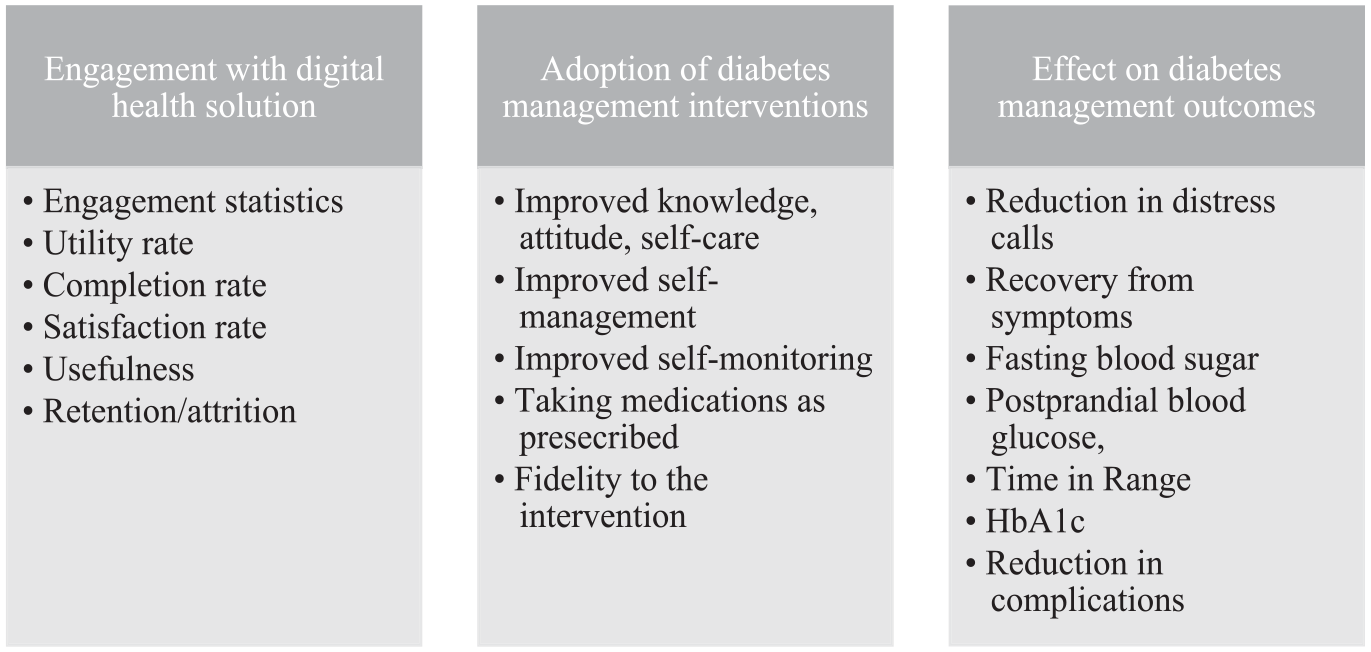
Categories of outcomes.
Outcomes of Digital Health Identified From the Review.
Challenges and Success Factors
There were several challenges associated with the implementation of digital health solutions for diabetes management (see Table 2). The most common challenges include the following:
Internet access: Lack of internet access was one of the challenges in the implementation of peer support intervention via social media in low- and middle-income countries. In the study that involved parents of children with type 1 diabetes, about 40% of families could not be enrolled as they did not have any internet access. 15
Digital literacy: People who access social media tend to be younger. Older people and those with limited digital literacy would be excluded from diabetes services delivered via social media. Similarly, people from ethnic minorities or deprived backgrounds with low digital literacy are less likely to access services delivered through social media. 16
Medicolegal concerns: Some health workers resisted using social media for service delivery. 16 They were also concerned about the transfer of data through digital platforms due to medicolegal reasons. The absence of formal guidelines and a secured platform for data transfer has created this challenge. 19
Ascertainment of efficacy and effectiveness: For videos delivered via social media platforms, it was difficult to know how attentively participants watched the videos and establish the efficacy and effectiveness of the education and support.17,28
Additional steps: An effort to improve access to digital health services through basic cell phones required participants to text their self-monitored blood glucose values via SMS. These additional steps involved in the use of digital health solutions increased the attrition of participants. 20
Required assistance: Assistance from community health workers and/or a matured support system was also required to facilitate the use of digital health solutions and help people with diabetes navigate and analyze the information delivered through these platforms.21,26
Unknown long-term effects: Most of the digital health solutions were applied for a short period of time (<3 months). Though they were found to be feasible, acceptable, and effective in the short term, their long-term effects after the decline of the COVID-19 pandemic are unknown. 29
Discussion
In this review, 15 digital health solutions that have the potential to improve diabetes outcomes, if they are further adapted and scaled up, are described. While most the digital solutions focus on the remote delivery of health services, some of which needed to be assisted by community health workers. Though infrastructural and operation challenges have affected their implementation, these solutions have resulted in promising outcomes during COVID-19 lockdowns and other restrictions. The wider application of the innovations would improve a more decentralized approach to health service delivery for people with diabetes.
Our findings indicated that digital health solutions, especially those based on social media platforms, have high engagement and utilization for community-based management of diabetes, including in low- and middle-income countries. As shown in this review, digital health solutions that involved Whatsapp Chatbots (South Africa and Barbados), WeChat (China), and LINE (Thailand and Taiwan) had high utilization rates and positive effects on diabetes management and reduction of complications. They could be scaled up to support diabetes management in other low- and middle-income countries. Our findings show that diabetes education and self-management are the main areas where these solutions can be most useful.
Access to reliable internet connectivity and readiness for the adoption of virtual services were among the challenges in the implementation of digital health solutions in low- and middle-income countries. A similar study in Canada reported that these were also the main challenges among minority groups living in high-income countries. 30 Another study stated that interoperability guidelines for semantics and data management are essential for the integration of digital health into routine health service delivery. 31 These are also important issues in the integration of the digital health solutions described in this review. As several medicolegal concerns and unintended consequences of the implementation of digital health innovations are possible, 32 future scale-up of digital health solutions need to give due attention to ethical issues, especially on handling and transferring people with diabetes information. Although digital health solutions improved access to and continuity of care, without proactive efforts to ensure equity, their implementation may increase disparities in healthcare access for vulnerable populations with limited digital literacy or access to the internet and digital devices. 33
The findings of this study have important implications for policy, practice, and research. From a policy perspective, the findings imply the need for advancing the lessons learned from the implementation of these solutions in the COVID-19 normal period as the future of healthcare delivery will be increasingly digital. 34 This could be by using a “hybrid” model of both virtual and face-to-face health service provision for people with diabetes and hypertension. Policy attention is also needed for further adaptation and scale-up of the innovations to the wider population. From a practice perspective, the findings call for the integration of crucial elements of the innovations, such as the expanded role of community health workers, remote monitoring of people with diabetes, and virtual peer support, into the health system. From a research perspective, it would be crucial to evaluate the effectiveness in terms of health outcomes, the potential for scale-up, and the sustainability of their implementation and benefits in the future.
There are some limitations associated with this review. First, most of the included studies were small-scale feasibility studies, and the long-term effectiveness of the included digital health solutions couldn’t be ascertained. Second, there was a very high level of heterogeneity among the included studies in terms of content and context and this could affect the generalizability of the findings. Third, this review focused on community-based diabetes management during the COVID-19 pandemic and the digital health innovations included in this review may not be representative of all digital health solutions for diabetes management. Finally, detailed information about implementation challenges and success factors was not available for some of the digital health solutions.
In conclusion, the evidence on implementation outcomes showed that digital health solutions for community-based diabetes management have tremendous potential to improve health outcomes for people with diabetes. Further studies are needed to evaluate the long-term sustainability and scale-up of digital health solutions.
Footnotes
Abbreviations
DALYs, disability-adjusted life years; HbA1c, glycated hemoglobin; LMICs, low- and middle-income countries; NCDs, non-communicable diseases.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
