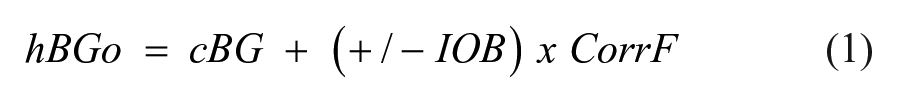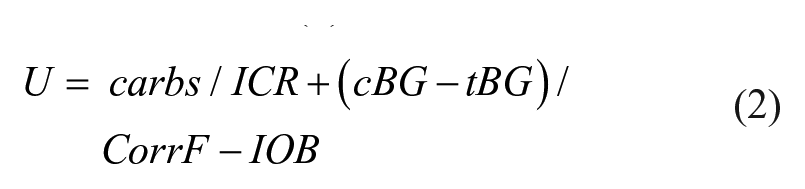Abstract
The accompanying article by Groat et al in this issue presents a methodology to compare glucose outcomes from insulin bolus dose recommendations observed retrospectively from a novel iDecide bolus calculator with glucose outcomes from the prospective bolus recommendations provided by a current insulin pump. The methodology in this article evaluates a bolus calculator algorithm and also evaluates calculations for two additional lifestyle behaviors, exercise and alcohol intake, that are modifiable risk factors associated with diabetes. This methodology for evaluation of glycemic outcomes from bolus calculators could be expanded further using much larger existing bolus calculator databases. This would complement current verifications done through in-silico testing with the University of Virginia/Padua 300 patient type 1 diabetes simulator. This approach merits serious consideration, yet the actual dose recommendations provided by the iDecide calculator introduce wider lessons on how bolus calculator glucose outcomes might be better optimized.
Keywords
Optimal management of daily glucose profiles with reduced glucose variability remains a key aim in daily life with diabetes. To improve success in this endeavor, a variety of tools such as self-monitoring of blood glucose, multiple daily insulin injections, advances in the types and action times of basal and bolus insulins, insulin pump therapy, and continuous glucose monitoring are utilized. One tool that provides improved estimates for safe and effective doses for prandial and corrective bolus insulin is the bolus calculator (BC) that was patented by Medtronic in 1999 (#6554798) and first implemented within the Deltec Cozmo insulin pump in 2002. This article discusses a variety of BC issues with special reference to the article in this issue by Groat et al on “A Methodology to Compare Insulin Dosing Algorithms in Real-Life Settings.”
Research studies have documented that bolus dose math errors that occur in over 60% of manual dose calculations made by patients are substantially reduced when a BC is used.1,2 Even though other advances, such as hypo/hyper minimizer and artificial pancreas systems, are in development and entering the market, BCs are expected to remain a primary tool in the foreseeable future for the millions of patients with diabetes who utilize them in IP (insulin pumps), glucose meters, and phone apps. They simplify the math required to calculate prandial boluses and correction boluses, while accounting for residual bolus insulin activity to partially minimize insulin stacking.
The article by Groat et al at Arizona State University and the Mayo Clinic introduces a novel approach to verify BC apps under real life circumstances. The authors compare bolus doses recommended by the iDECIDE (iD) BC app with those given by an insulin pump, and also expand BC functionality further through optional inputs regarding physical activity and alcohol intake that impact bolus dose requirements. With the iD’s bolus recommendations masked to users during the study, researchers retrospectively compared the actual bolus doses delivered by the insulin pump with the simultaneous bolus doses calculated by the iD BC app. Success or failure was determined in relation to the actual postbolus glucose outcomes from the BC currently in use. The undelivered bolus doses from the iD BC were evaluated based on whether the iD’s bolus dose recommendations were more than 10% smaller, similar (±10%), or more than 10% larger than those of the standard BC when the user’s glucose ended up below, within, or above the pump’s glucose target range. In other words, theoretically would the iD BC have improved postbolus glucose results?
The FDA currently allows BCs to receive approval after undergoing in-silico testing with the University of Virginia’s type 1 diabetes simulator that currently operates with a 300 patient database. 3 Even though this provides a relatively easy and inexpensive way to test and obtain approval for a new BC, obtaining FDA approval for equivalence with existing BCs represents a rather low bar since many of these comparator BCs utilize nonphysiologic settings or use algorithm logic that delivers inappropriate bolus dose recommendations. 4 BCs help many type 1 patients improve their glucose control as shown by improved A1c levels either with the BC alone 5 or when combined with accurate carb counts. 6 However, outcomes in general have been limited, suggesting that BCs have not been fully optimized. 4 The ideal goal of the BC would focus on enhancements that bring about demonstrable improvements in glycemic control rather than a goal that merely replicates the meager glycemic performances seen in many of today’s BCs.7 -9
By comparing a new BC’s performance with prospective data inputs from an existing BC under real life circumstances, the iD approach expands on the certainty of in silico testing . However, testing of new BCs would be more effective if the accuracy of BC settings and the logic in existing algorithms were improved through direct comparisons with much larger patient-approved anonymous raw data outcomes now available within large BC databases available at Glooko, CareLink, Tidepool, and T1D Exchange.
The Groat article introduces an interesting and useful methodology for BC research. Although the design of the iD protocol has weaknesses that reduce effectiveness, it is informative for Arizona State University and other researcher teams who are performing BC research. As one example, the iD BC uses each pump’s internal glucose target range to evaluate glucose outcomes. Although all of the subjects’ target ranges in this study are relatively normal at 90 to 120 mg/dL, other subjects and clinicians might select wider target ranges. For example, one subject’s target range might be 90 to 90 mg/dL while another’s might be 70 to 180 mg/dL. Using the narrow glucose targets in this study, results were skewed with only 13% of the study’s glucose results ending up within the “target range” and 77% “above the range” although not necessarily outside a desirable glucose range.
The choice to use the IP’s target range handicaps the evaluation of outcomes for both the IP BC and the iD BC. To improve understanding of actual glucose outcomes, the variable target glucose range against which the IP BC’s actual and the iD BC’s projected glucose outcomes are compared could be replaced with consistent glucose range outcomes, such as <50, 50 to 80, 81 to 140, 141 to 180 mg/dL, and so on. Even though not ideal, projected glucose outcomes from a nonoperational BC can be reasonably estimated for various points in time with equation 1:
Here, the hypothetical glucose outcome (hBGo) is determined from the current BG (cBG) plus the deficit or excess in insulin on board (± IOB) times the individual’s correction factor (CorrF). Keys to success with equation 1 include measuring IOB accurately, using a duration of insulin action (DIA) of 4 hours or more, and ensuring the CorrF is appropriately based on an accurate TDD. 10
Another weakness noted by the authors arises from the evaluation of outcomes based on glucose readings taken 3 hours ± 15 minutes after the bolus is delivered, at a time when significant actual IOB may still exist. 11 For example, with a range of 90 to 90 mg/dL, a glucose of 91 mg/dL 3 hours later would be “above range” and an iD bolus might be judged superior if it recommends a bolus dose that is more than 10% larger than the pump’s recommended bolus, even though this bolus may later generate hypoglycemia once the residual IOB has fully acted.
The IP BC to which iD is compared only subtracts IOB in excess of that needed to correct the current glucose from carb boluses when the user’s glucose goes below their target. Even when the glucose goes low, only enough of the excess IOB is subtracted to bring the glucose back to the bottom of the user’s target range. Thus, excess IOB is ignored under most circumstances and can lead to bolus overdoses unless a user is aware of this issue and manually subtracts the excess IOB from carb bolus recommendations when IOB is greater than the correction bolus. The aggressive nature of BCs found in most IPs to my awareness has never been explained or justified.
In contrast, the iD BC uses a conservative bolus equation originally used in the Cozmo insulin pump below to determine bolus recommendations that subtracts IOB from the sum of the carb and correction (±) boluses:
where U = bolus units recommended, ICR is the insulin to carb ratio, cBG is the current glucose, tBG is the target glucose, CorrF is the correction factor, and IOB is the residual bolus insulin activity.
Equation 2 fully subtracts IOB from correction boluses and any excess IOB beyond that needed to correct the current glucose is then subtracted from carb boluses. Given that basal rates and pump settings were unchanged in this retrospective study, the conservative iD BC algorithm would be expected to deliver smaller bolus recommendations than those delivered by the pump bolus algorithm to which iD was compared. Even so, the iD BC app generated larger bolus doses than the IP BC 13% of the time when the glucose was low and 20% of the time when BGs were within the target range. The authors of the Groat article do not fully explain the modifications that allow the iD BC to increase its bolus dose recommendations. The system appears to be doing this through reduced estimates for residual IOB.
This raises a serious issue in that the study relies on modification of DIA times as the primary tool to modify the iD BC’s recommended doses. This does not address the actual sources for insulin dosing errors, such as basal rate or ICR settings, or unreliable carb counting on the part of the user. Adjustment of the IOB is a circuitous way to fix glucose problems that typically are unrelated to IOB or a DIA time setting. Most control issues related to insulin doses originate from incorrect basal rates (long-acting insulin doses) and/or from an incorrect ICR. When a user or clinician shortens the DIA time to correct insulin deficits that originate in the basal or carb doses, they complicate control issues by introducing hidden insulin stacking. This, in turn, can further deteriorate the accuracy of BC settings in the subsequent efforts to eliminate the hypoglycemia that it generates. Less commonly, an excessively long DIA can generate hyperglycemia.
The most important insulin dose for creating an accurate BC is the TDD. This determines the frequency of hypo and hyperglycemia, and along with a patient’s weight can be used to determine very accurate initial BC settings. In an earlier article regarding the iD BC, a patient’s TDD is stated to equal wt(lbs) × 0.23 u/lb. 12 However, this equation is not intended to select an individual’s TDD but instead provides a theoretically “ideal TDD” for a person of that weight against which an individual’s actual TDD can be taken into account to evaluate their insulin sensitivity. In addition, this 2016 article uses an old equation for the I:Carb ratio (450/TDD) rather than 2.6 × wt(lbs)/TDD where weight and insulin sensitivity are accounted for. The CF or CorrF equation (1700/TDD) also does not account for the current deficit or excess in the TDD (A1c and hypoglycemia frequency) where 1300/TDD may be more appropriate with an A1c of 10% and 2400/TDD may work better for an A1c of 6%. It is not clear which equations were used to select the initial IP BC settings against which the iD BC was compared.
Summary
In its current form, the iD algorithm outperforms the IP BC at preventing lows with 43% of bolus recommendations being reduced compared to 19% being increased when the glucose went below the target range. It shows mixed results for readings above the target range with 27% lower and 34% higher bolus recommendations, and creates more glucose variability within the narrow target range with 52% lower and 39% higher bolus recommendations. The algorithm performed reasonably well for exercise and alcohol events when the glucose was above target, but for unexplained reasons did not go as well when glucoses were in or below the target glucose.
The stated aims of the Groat article were to
Develop a method to analytically compare BC algorithms
Test the iD (or other) BC with an existing insulin pump BC
Share lessons learned
They succeed on numbers 1 and 2, but disappointment exists for the third aim. The authors acknowledge that modifications to the iD BC will be needed but specifics on these modifications are not provided. It is unclear how the iD algorithm modified standard bolus recommendations, and limited information is provided for how the iD algorithm failed or the modifications that might be made to improve glucose outcomes. Fitness devices with Bluetooth technology, as the authors note, will more quickly and appropriately adjust for changes in physical activity than manual entry. Adjustments for other factors may eventually find their way into BC dose calculations, such as for CGM trend lines (or even more precise projections of 30- to 60-minute glucose values), changes in weight, menses for women, a meal’s fat and protein content, 13 the glycemic index of foods, illness, and medications.
Correct BC settings are critical for optimal glucose outcomes. Even the soon-to-arrive AP systems provide bolus doses from the pump’s BC settings and, therefore, will be more difficult to optimize when BC settings contain errors. Optimization of insulin pump basal rates or long-acting insulin doses and BC settings is a critical first step to obtain optimal performance while an AP system is operational. BC optimization is even more important during interruptions in AP service when the AP returns to being a standard pump.
Large BC databases exist that could be utilized to advance BC technology through improved algorithms that deliver more accurate bolus doses and through selection of more physiologic BC settings, as well as basal rates or LAI doses. Multiple research projects are underway to enhance the accuracy of bolus and basal dose recommendations through selection of more physiologic BC settings and accompanying basal rates or long-acting insulin doses. This article by researchers and clinicians at Arizona State University and Mayo Clinic takes some beginning steps in providing a helpful methodology to evaluate new bolus calculators.
Footnotes
Abbreviations
BC, bolus calculator; BG, blood glucose; CGM, continuous glucose monitoring; CorrF, correction factor or mg/dL decline per unit of insulin; DIA, duration of insulin action; ICR, insulin:carb ratio; iD BC, iDECIDE bolus calculator app; IOB, bolus insulin on board or active bolus insulin; IP BC, insulin pump bolus calculator.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.