Abstract

From a meta-analysis of 12 studies totaling 2260 patients, Horigan et al 1 concluded that diabetes education is underutilized for a variety of reasons. The results of their study highlight the failed systems in several countries that must be reformed to help patients with diabetes fully understand the significance of this chronic disease. The number of Americans with diagnosed diabetes is projected to increase 165%, from 11 million in 2000 to 29 million in 2050, and this trend is reflected worldwide. 2 Since patient education efforts have had little impact on the incidence of diabetes and its complications, the need for effective diabetes monitoring should be evaluated.
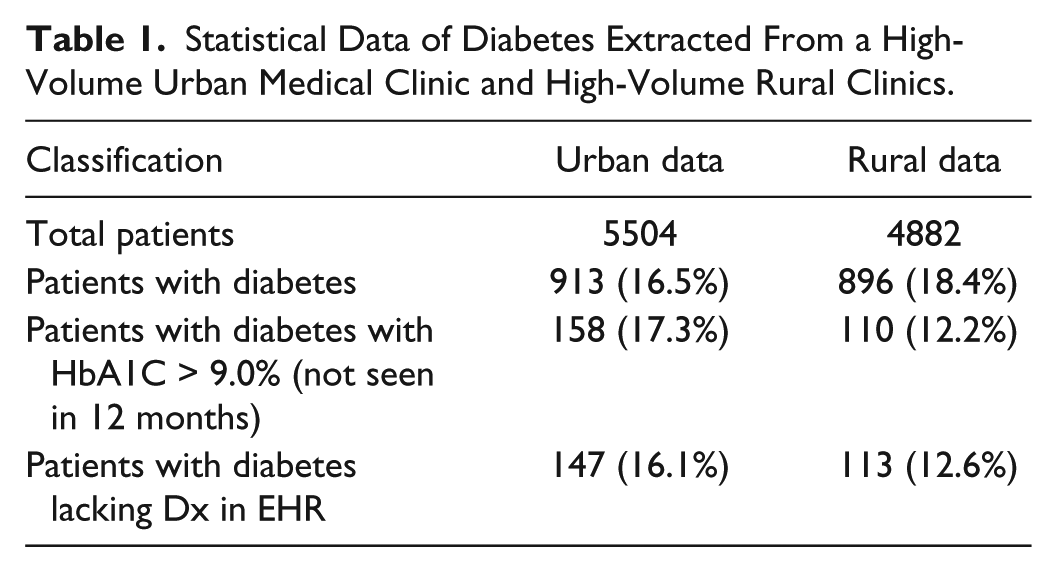
After receiving approval for institutional review board exemption status, a baseline medical records study was conducted on a large primary care, metropolitan clinic in the southeastern part of the United States. In addition, a series of 12 clinics in a rural area had identical baseline medical study conducted. Data were extracted using proprietary software (iMorpheus, a middleware search engine owned by Sonic Healthcare, Austin, Texas, USA). Urban and rural clinic data were separately analyzed. The time window designated for the extraction for the urban clinic was November 12, 2014, to April 1, 2016, which resulted in a total of 13 881 laboratory accessions representing 5504 individual patients. The time window for the rural clinics was March 9, 2015, to May 13, 2016, which resulted in 4882 individual patients. Among these 5504 urban patients, 913 (16.5%) were identified as having diabetes using either the American Diabetes Association diabetes parameters 3 or documented diagnoses based on International Classification of Disease level 9 or 10 (Table 1). Of these 913 patients, 16.1% did not have a diabetes diagnosis documented in their electronic medical records and 45.6% had not undergone HbA1C measurement for over 12 months. A total of 17.3% patients had HbA1C > 9% at last visit, but no follow-up testing was performed within the 12 months. Among the rural 4882 patients, 18.4% were identified as having diabetes and 12.6% did not have a diabetes diagnosis documented in their electronic medical records (Table 1). Among the urban patients with diabetes, 53.8% had not undergone HbA1C measurement for over 12 months. A total of 12.2% of rural patients had HbA1C >9.0% at last visit, but no follow-up testing was performed within the 12 months (Table 1). Further study will be done to extract the compliance with annual eye examinations. In the urban clinic, a preliminary data assessment of potential kidney involvement showed that 64.6% of the 913 patients had not been tested for microalbumin. Kidney involvement was not fully assessed on the rural population. In summary, current technology offers great opportunity for data mining to help primary care providers identify patients with diabetes and prediabetes, to manage patients to improve compliance status, and to further complete necessary kidney assessment and annual eye examinations for retinopathy and other ocular/visual complications of diabetes mellitus.
Statistical Data of Diabetes Extracted From a High-Volume Urban Medical Clinic and High-Volume Rural Clinics.
Horigan et al 1 clearly are on point that diabetes education is necessary to emphasize the frequent monitoring and interventions required to maintain lowered glycemic levels and prevent the secondary impacts of retinopathy and chronic kidney disease. The lack of patient follow-up in our study confirms their findings and further identifies that use of electronic medical records alone does not facilitate the provision of effective follow-up by primary care providers, even when patients visit health care providers within a timely period. For the patient with diabetes to engage with health care providers to monitor and maintain the glycemic levels that mitigate damage from the disease, patient education must be modified, perhaps even personalized, to promote understanding of the disease and improve compliance with the monitoring required to prevent disease evolution.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
