Abstract
Objective:
Develop workflows and billing processes for a Certified Diabetes Care and Education Specialist (CDCES)-led remote patient monitoring (RPM) program to transition the Teamwork, Targets, Technology, and Tight Control (4T) Study to our clinic’s standard of care.
Methods:
We identified stakeholders within a pediatric endocrinology clinic (hospital compliance, billing specialists, and clinical informatics) to identify, discuss, and approve billing codes and workflow. The group evaluated billing code stipulations, such as the timing of continuous glucose monitor (CGM) interpretation, scope of work, providers’ licensing, and electronic health record (EHR) documentation to meet billing compliance standards. We developed a CDCES workflow for asynchronous CGM interpretation and intervention and initiated an RPM billing pilot.
Results:
We built a workflow for CGM interpretation (billing code: 95251) with the CDCES as the service provider. The workflow includes data review, patient communications, and documentation. Over the first month of the pilot, RPM billing codes were submitted for 52 patients. The average reimbursement rate was $110.33 for commercial insurance (60% of patients) and $46.95 for public insurance (40% of patients) per code occurrence.
Conclusions:
Continuous involvement of CDCES and hospital stakeholders was essential to operationalize all relevant aspects of clinical care, workflows, compliance, documentation, and billing. CGM interpretation with RPM billing allows CDCES to work at the top of their licensing credential, increase clinical care touch points, and provide a business case for expansion. As evidence of the clinical benefits of RPM increases, the processes developed here may facilitate broader adoption of revenue-generating CDCES-led care to fund RPM.
Keywords
Introduction
Continuous Glucose Monitoring (CGM) is the standard of care for pediatric patients with type 1 diabetes (TID).1,2 The 4T (Teamwork, Targets, Technology, and Tight Control) program uses evidence-based guidelines to provide early and equitable access to diabetes technology (CGM) to sustain tight glycemic management from the onset of TID diagnosis. The 4T study design and results have been previously published.3,4 Briefly, the 4T program includes early CGM initiation within 30 days of TID diagnosis, followed by monthly remote patient monitoring (RPM) and patient-reported outcomes surveys.
All patients diagnosed with TID are offered the program regardless of insurance status or type, language spoken, or provider referral. The 4T program increased patients meeting HbA1c targets of <7% from 28% to 64% and achieved a mean time-in-range (70-180 mg/dL) of 68% at 12 months. 4 Here, we focus on our development of workflows and billing processes for a Diabetes Care and Education Specialist (CDCES)-led RPM program as part of the transition and sustainability of the 4T Study from research to our clinic’s standard of care.
The 4T team (pediatric endocrinologists, diabetes educators, diabetes research scientists, biostatisticians, and program coordinators) implemented RPM as a tool to improve glucose and provide regular education and insulin adjustments to patients. During RPM, the CDCES reviews CGM data and provides clinically indicated diabetes education or insulin dose adjustments via asynchronous electronic health record (EHR) messaging between routinely scheduled diabetes care visits to increase time in range.5,6
Due in part to routine (at least monthly) RPM, the 4T program achieved significant improvements in glucose management with a decrease in HbA1c of −1.10% at 12 months post-TID diagnosis compared with historical controls. 4 RPM is pivotal to fully utilize CGM, which allows for increased CGM data interpretation, tailored education, and insulin dose adjustments. Remote patient monitoring allows personalized care tailored to a patient’s needs and does not have to correspond to endocrinology visits. However, billing workflows must be developed, implemented, and utilized to sustain an RPM program. Specifically, revenue-generating CDCES-led workflows are needed for RPM of CGM.
The CGM interpretation codes that can be used for RPM are currently in use in diabetes clinics. Specifically, the Current Procedural Terminology (CPT) code 95251 (ambulatory continuous glucose monitoring of interstitial tissue fluid via a subcutaneous sensor for a minimum of 72 hours; analysis, interpretation, and report), 7 is used by clinicians if they perform CGM interpretation during a routine diabetes care visit. This manuscript describes the development of workflows and billing processes for a CDCES-led RPM program.
Methods
We identified stakeholders within the institution to support the process, including hospital compliance, system analysts, clinical informatics and billing analysts, and financial counseling. Hospital compliance reviewed the various RPM CPT codes available and provided compliance billing integrity guidance for appropriately using the CPT codes identified. The EHR system analysts and clinical informatics provided expertise on how the billing workflow and associated progress notes in the EHR system can be designed, accessed, and completed by the billing provider (CDCES in this case). Billing analysts and revenue management ensured the back-end billing infrastructure was utilized appropriately. They tracked the bill flow from when it was submitted to when it was sent to the insurance company and the revenue generated. If there were any patient-related costs (copays or deductibles) and any billing errors (eg, duplicate bills), they were also tracked. Financial counseling services worked with the 4T team to develop a workflow to support patients and families with financial challenges paying for RPM-related copays or deductibles. The CDCES team, as the end users, were involved from the beginning to ensure the processes developed were relevant and efficient. We started with the existing CGM interpretation code 95251, recommended by billing compliance as the most specific code to accurately describe the service being performed. A workflow with the CDCES as the billing provider was developed, which was novel for the clinic. The schematic below shows how RPM billing was built into our clinic’s data flow in the 4T program (Figure 1).
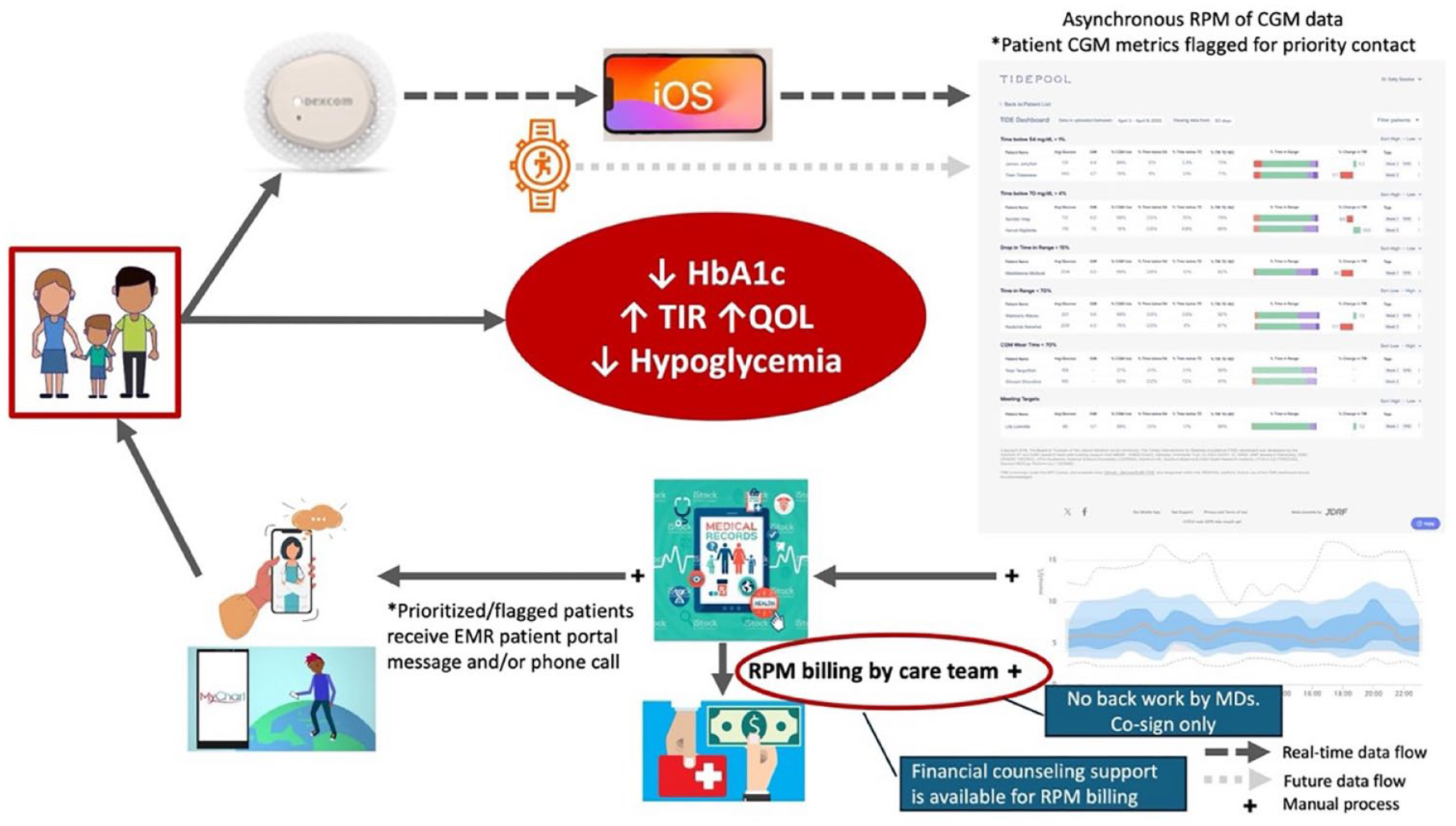
4T data flow overview.
A patient is started on CGM within a month of T1D diagnosis, and CGM data flows via Bluetooth to the CGM app on a compatible smart device (iOS devices were provided if needed). The app transmits data to the manufacturer’s cloud, which is then retrieved by hospital servers using custom code and prioritized for review via the Timely Intervention for Diabetes Excellence (TIDE) platform.
The TIDE platform prioritizes patients based on CGM data. The CDCES locates the patient for RPM in TIDE and creates a billing progress note and any associated patient-facing message in the EHR patient message portal with potential insulin dose adjustment and/or diabetes education. Remote patient monitoring allows for the review of CGM data that would benefit from diabetes care team intervention in between quarterly clinic visits. During RPM, the CDCES reviews CGM data and provides clinically indicated diabetes education or insulin dose adjustments in between care visits when indicated by CGM data (Figure 2). Training in CGM interpretation and insulin dose adjustment is required for CDCES credentialing, with additional shadowing by senior team members for RPM workflows in the clinic.
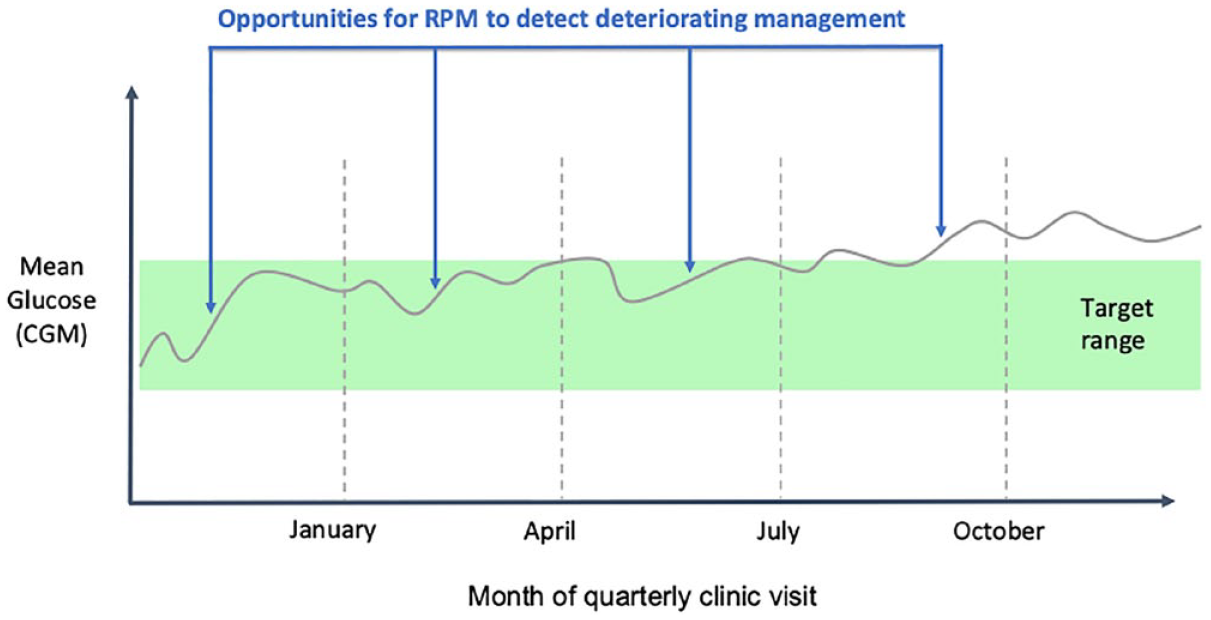
Opportunities for RPM.
RPM codes
Stipulations of billing codes were considered, such as the timing of CGM interpretation, the scope of work, providers’ licensing, and necessary EHR documentation to meet billing compliance standards. Online resources were used from the Endocrine Society, CGM manufacturers, the Association of Diabetes Care & Education Specialists, 7 and others. Billing compliance identified codes and the potential limitations of each code, which was discussed to optimize the billing workflows in development. We assessed various situations where the RPM billing workflow could be used and answered the following questions to correctly identify the appropriate code and its usage (Table 1).
Helpful Questions to Identify Appropriate RPM Codes.

Abbreviations: APP, advanced practice provider; CDCES, Certified Diabetes Care and Education Specialist; RPM, remote patient monitoring; CGM, continuous glucose monitoring.
After identifying and discussing the billing codes, the compliance group noted provisions that made certain codes feasible or unfeasible, depending on the institution. For example, a meeting of “incident-to guidelines” for a Registered Nurse-CDCES or Registered Dietitian Nutritionist-CDCES to perform the service (RPM) directed by a physician or other qualified health care provider and the location of the service. Finally, we considered whether the code provided relative value units (RVUs) based on reimbursement structure and our institution’s billing systems.
Once a code was identified, billing compliance provided a compliance billing integrity guidance document describing the code, details, and documentation requirements. For the documentation requirements, billing compliance provided an example of the billing report and what needed to be included in the billing workflow in the EHR. This helped the clinical informatics team build the documentation template and design the workflow in the EHR.
Workflow development
Once the billing compliance department released the “compliance billing integrity guidance” document related to the use of 95251 by a CDCES, the team met regularly to design the workflow in the EHR. The “compliance billing integrity guidance” outlined the documentation requirements and an example of a report that needed to be integrated into the billing or progress note in the EHR. We had to comply with “incident-to” billing compliance, a set of CMS guidelines stipulating the provider type, supervision, and service location. 8 “Incident-to” billing allows nonphysician practitioners, including CDCES, to perform and bill certain services. Then, the code can be billed under the supervising physician’s National Provider Identifier (NPI) number at the full physician reimbursement rate. The guidance document noted specific documentation requirements to meet “incident-to” services, such as a cosignature by the supervising/attending physician or APP if not personally performing the service. Part of “incident-to” is related to where the service is performed, even if the service is non-patient-facing. For 95251, a place of service 11 (freestanding physician’s office) must be the location of the service as 95251 cannot be billed by a facility (Hospital Outpatient Provider-Based Department [place of service 22]) since it is a professional service. As a professional service, it is not payable under the outpatient prospective payment system (OPPS). Therefore, to use CPT 95251, the CDCES team had to perform their RPM at a freestanding physician’s office or, in our situation, one of the “satellite clinics” that was not a Hospital Outpatient Provider-Based Department. The clinical informatics team then created a workflow in the EHR to accurately meet the compliance documentation requirements with a thorough review of how the CDCES engages with the EHR system including their current documentation practices. The workflow consisted of the following steps: The CDCES selected the patient for review in TIDE and created a documentation “encounter.” A standard “reason for visit” was entered as “Continuous Glucose Remote Monitoring” to enable these encounters to be easily distinguished within the vast electronic medical record. The CDCES completed the progress note according to the billing compliance guidelines and added a cosigner. The progress note needed to include the following: duration that the patient wore the CGM device (must be >72 hours); current HbA1c (if available); CGM metrics (all CGM data must be >72 hours) including time in target range, time above and below target range, and patterns of hypo/hyperglycemia; interpretation of results, any recommended changes to treatment plan including insulin dose changes and copy of the device download (e.g., AGP) (Supplemental Material 1). CGM metrics were reviewed and interpreted, copied and pasted from TIDE or the CGM manufacturer’s platform, and a copy of the AGP report was added to the progress note. Per billing compliance, the service provider needed to engage in “active decision making” with proof that unique and newly entered information was reported for the specific data in the progress note. Progress note templates were created with placeholders to ensure CDCES captured all the necessary data points and information was presented consistently and met all billing compliance standards. Then, the CDCES added the RPM code (95251). The CDCES listed themselves as the “service provider” and indicated the “billing provider” as the supervising/authorizing provider who would complete their review. The full encounter, including the progress note, was routed to the indicated supervising attending MD/APP, who completed their attestation, re-stated any recommended treatment changes, and cosigned the note. The charges were not submitted until the Attending MD/APP reviewed and cosigned the encounter.
Results
From February 2024 through May 2024, a CDCES charged monthly CGM RPM as the service provider and an MD as the billing provider (completed attestation and cosign). Fifty-two patients were successfully billed for a monthly RPM using CPT code 95251. Patients had a mix of commercial (60%) and public (40%) insurance (Table 2). The average reimbursement rate was $110.33 for commercial insurance and $46.95 for public insurance (Medi-Cal) per code occurrence. The percentage of claims paid by commercial insurance was 94%, and 43% for public insurance. The average cost for patients on public insurance was $0 (no deductible or copay/coinsurance). For patients with commercial insurance, the average cost was $51.04 per billing occurrence. Of these, 35% paid a deductible averaging $117.12, 29% paid a copay averaging $21.31, and 29% paid nothing. If a patient deductible was charged, then a copay/coinsurance was not.
Billing Revenue and Patient Costs (Patients Billed for a Single RPM 95251 Code, N = 52).
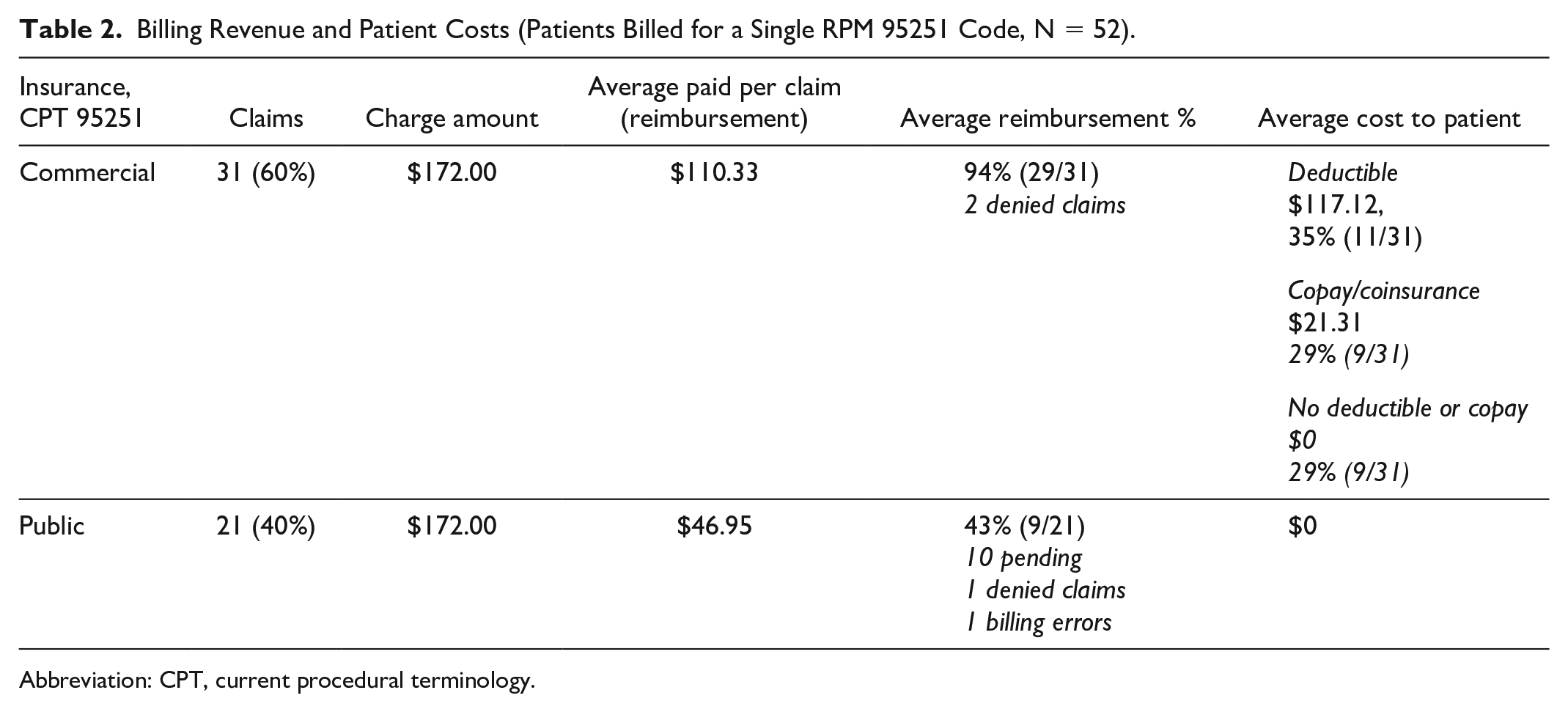
Abbreviation: CPT, current procedural terminology.
Two commercial insurance claims were denied and are under appeal. Ten public insurance claims were rejected for lack of authorization and are currently pending retroactive authorization. One public insurance claim was denied and is being appealed, and another was denied as a duplicate, causing a billing error.
On average, the CDCES took 15 minutes per patient to perform the RPM for the CGM interpretation, complete the billing documentation requirements, including the progress note and routing to the billing provider, and send an EHR message portal to the patient. On average, the billing provider took three minutes to attest the progress note, which includes reviewing, confirming, or editing the treatment section and cosigning.
Discussion
The 4T program improves T1D diabetes outcomes and3,4,9 -11 provides equitable, value-based, precision diabetes care.5,12 Translating proven interventions to clinical practice requires sustainability through integration into clinical workflows and billing. Furthermore, a barrier to optimizing diabetes care in the United States is the health care system in which the reimbursement for diabetes education and management frequently does not cover the total cost of services.
Having demonstrated the benefits of the 4T program in research protocols,3,4 we describe pilot data establishing RPM billing to sustain the 4T program within our institution. It has been over 30 years since the Diabetes Control and Complications Trial (DCCT) demonstrated the benefits of intensive management of T1D, 13 but clinical practice has not been able to replicate the intense engagement of that study in clinical practice. Expansion of diabetes education and care is unlikely without a positive or neutral business case. The improved glycemic outcomes in the 4T program support the monthly RPM charges required to sustain this precision approach to diabetes care in practice.
Implementing a diabetes care program, such as 4T, into clinical care requires close partnership and collaboration with the CDCES team. The focus on developing a billing workflow with the CDCES as the service provider allowed CDCES to bill for RPM being performed and work at the top of their license by providing diabetes care and education. The CDCES providers rarely bill for time spent on CGM interpretation, and this is a lost opportunity for these providers to bill for care being delivered and to support a financially sustainable diabetes care model.
Since RPM billing is novel and not used routinely for asynchronous review of CGM data outside of routine endocrinology visits, understanding the stipulations of various CPT codes and close collaboration with an institution’s billing compliance is needed. Depending on the institution, it can be a lengthy process to identify the different groups and departments that will need to be involved in designing an RPM program (hospital compliance, system analysis, clinical informatics, billing analysis, revenue management). Identifying a point person or small core team to lead the efforts is advised. Remote patient monitoring codes continue to be modified. 14 In addition, different RPM codes can also be stacked, for instance, 99454 (general RPM device code for collection and transmission of data), 95251 (CGM interpretation), and 99457 (direct RPM care management). Another consideration is that some codes may provide RVUs to the providers submitting the code and revenue generation for the clinic/division, and other codes can be added that provide no or lower RVUs but a higher payment and revenue back to the institution.
As this RPM billing workflow was developed, we also consulted the Stanford Children’s Diabetes Family Advisory Council (FAC). The 4T program was presented with the goal of starting monthly billing for RPM of CGM. The FAC supported RPM billing and highlighted the importance of the monthly patient portal messages to families explaining RPM and any diabetes care recommendations. In addition, the FAC noted the importance of communicating CGM interpretation to all families, regardless of whether a family was in range with their CGM metrics, so as not to unintendedly be punitive and perform RPM for those not meeting CGM glycemic goals. Finally, the FAC noted that they would consider an acceptable copay (if a copay applies) of up to $35 per month for patients and their families, given the benefits of the 4T program. Hesitation to bill for between-visit services due to negative patient feedback has been a perceived barrier by many diabetes practitioners.
Part of the RPM billing pilot includes connecting with financial counseling to identify how to support patients and their families who may find RPM fees (deductibles or copays) financially burdensome. The 4T program obtained philanthropic support to ensure accessibility to all patients with T1D, which included funds to support RPM patient costs. The challenge was how to develop a system to use the philanthropic/gift funds, which includes considering how to flag or identify patients that may need support, how to link the gift funds, and how to monitor the use of the gift funds accurately and according to the parameters of the gift fund. Once the 4T program was incorporated as the standard of care, we developed a workflow with revenue managers, EHR engineers, and patient financial counseling services to use the gift funds to support patients’ associated bills. This workflow only applies to patients with commercial insurance that have a deductible or copay charged, as public insurance in the pilot had zero associated patient charges. All families are given financial counseling information. Once a patient is started on a CGM, then they are given a “guarantor” flag in the EMR, which identifies them as potentially eligible for RPM bill support. If families apply for financial assistance and are approved, their Stanford Children’s medically necessary services (nonelective) are covered, including any RPM charges. The gift fund can pay RPM charges if the family is denied financial assistance. The RPM charges must be related to the CPT code 95251 with the CDCES as the service provider to isolate the monthly RPM charges by the CDCES team and not when the pediatric endocrinologist uses 95251 during routine in-person visits.
Furthermore, using the TIDE platform 5 has enabled clinicians to prioritize CGM data for clinical review and develop an efficient workflow for routine RPM. The TIDE platform was created at Stanford and has now been deployed in Tidepool to facilitate sustainability and scalability. 15 Tidepool adds increased functionality and features for data review and workflows to support RPM billing and reporting. Our next step is to share the 4T program with other diabetes centers and ensure that TIDE in Tidepool is readily available and can be tailored to clinic needs to disseminate and implement the 4T program.
Conclusion
The 4T program currently has 366 patients receiving RPM of their CGM data monthly. The goal is to expand clinical workflows and staffing to support monthly RPM review and billing by the CDCES team. This will generate revenue for the program directly to the division as well as the hospital to support this additional diabetes care. To expand billing to every patient with T1D seen at Stanford Children’s, the CDCES team needs enough members to allow for the time it takes to perform RPM and bill, as well as program coordinators or clinic administrators to support the CDCES team by assisting with CGM supply or connectivity issues. This support is vital to ensure the CDCES team has the bandwidth to perform and bill for RPM. Billing for RPM will allow diabetes clinics to create revenue for services that improve care for patients with TID and ensure the best practices are being utilized sustainably.
Supplemental Material
sj-docx-1-dst-10.1177_19322968241308920 – Supplemental material for Building a Diabetes Educator Program for Remote Patient Monitoring Billing
Supplemental material, sj-docx-1-dst-10.1177_19322968241308920 for Building a Diabetes Educator Program for Remote Patient Monitoring Billing by Franziska K. Bishop, Annette Chmielewski, Jeannine Leverenz, Shannon Lin, Barry Conrad, Anjoli Martinez-Singh, Laura Pike, David Scheinker, Priya Prahalad and David M. Maahs in Journal of Diabetes Science and Technology
Footnotes
Acknowledgements
We thank all the young people who participated in the 4T Study. We thank the other members of the research team, including the research coordinators, clinical staff, students in the Systems Utilization for Stanford Medicine group, the Quantitative Sciences Unit, and the T1DWorking Group in Statistics and Informatics at Stanford Medicine Children’s Health. We especially thank all staff and team members who are involved in the 4T Study including D Naranjo, C Guestrin, M Tannenbaum, E Fox, A Cortes, E Pang, R Tam, I Balistreri, A Loyola, N Alramahi, E Frank, J Lin, K Clash, J Senaldi, K Seeley, G Keoung, Kim MS, P Dupenloup, J Kurtzig, R Sesanayake, M Petel, P-A Laforcade, V Ritter, B Shaw, B Bunning, B J Zou, A Wang, Y Jeong, N Pageler, S Ghuman, C Brown, B Watkins, and G Loving.
Abbreviations
APP, advanced practice provider; CMS, Centers for Medicare & Medicaid Services; CDCES, Certified Diabetes Care and Education Specialist; CGM, continuous glucose monitoring; HER, electronic health record; HCPS, Healthcare Common Procedure Coding System; RN, registered nurse; RDN, registered dietitian nutritionist; RVU, relative value unit; RPM, remote patient monitoring; 4T, teamwork, targets, technology, and tight control; T1D, type 1 diabetes.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: DMM, DS, and PP have received support from NSF, Stanford MCHRI, and Stanford HAI. DMM has received funding from the Helmsley Charitable Trust. DMM has had research support from the NIH, and his institution has received research support from Dexcom. PP has consulted for Sanofi. DMM has consulted for Abbott, the Helmsley Charitable Trust, Lifescan, Sanofi, Medtronic, Provention Bio, Kriya, Biospex, and Bayer. The remaining authors declare no competing interests.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported in part by the NIH (grant no. P30DK11607401) via the Stanford Diabetes Research Center and grant no. R18DK122422 to DMM. Funding support was also received from the Stanford Human-Centered Artificial Intelligence (HAI) and Stanford Maternal & Child Health Research Institute (MCHRI) grants to PP. The MOCA foundation, which funds financial assistance for remote patient monitoring medical bills for families in need. The NSF (grant no. 2205084) provided additional support. The Stanford REDCap platform (![]() ) is developed and operated by Stanford Medicine Research Technology team. The REDCap platform services at Stanford are subsidized by (1) Stanford School of Medicine Research Office, and (2) the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health, through grant UL1 TR003142. The funders had no role in study design, data collection and analysis, the decision to publish, or the preparation of the manuscript.
) is developed and operated by Stanford Medicine Research Technology team. The REDCap platform services at Stanford are subsidized by (1) Stanford School of Medicine Research Office, and (2) the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health, through grant UL1 TR003142. The funders had no role in study design, data collection and analysis, the decision to publish, or the preparation of the manuscript.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
