Abstract
Background:
Accurate calculation and adjustment of insulin doses is integral to maintaining glycemic control in insulin treated patients. Difficulties with insulin dose calculations may lead to poor adherence to blood glucose monitoring and insulin treatment regimes, resulting in poor metabolic control. The main objective of this study was to evaluate ease of use and user preference of a high specification touch screen blood glucose meter, which has an in-built insulin calculator, compared to patients’ usual method of testing blood glucose and deciding insulin doses.
Methods:
Patients with diabetes on a multiple daily injection insulin regime used the Test Meter without the insulin calculator and 1 of 3 comparator meters, each for a 7-day period. They then used the Test Meter with the in-built calculator for 10 days. Patients completed an ease of use questionnaire after each 7-day period, a preference questionnaire after the second 7-day period, and a questionnaire comparing the Test Meter with their usual method after the final 10-day period.
Results:
Of 164 patients who completed the study, 76% stated a preference for the Test Meter as a diabetes management tool compared to their usual method. A small number of patients preferred familiar methods and/or calculating insulin doses themselves. The log book function of meters was important to most patients.
Conclusions:
The Test Meter system with in-built insulin calculator supports people to better manage their diabetes and increases their confidence. Patients have different needs and preferences which should be acknowledged and supported in a patient centered health service.
Patient self-management through blood glucose monitoring and accurate calculation and adjustment of insulin doses is integral to glycemic control in patients with insulin treated diabetes. This is a challenge for many patients as multiple variables need to be considered. There is evidence in adolescents suggesting that poor compliance with insulin regimes due to a lack of understanding of and/or frustration with the complexity of insulin dose calculations may contribute to poor metabolic control. 1 A recent study of patients with type 2 diabetes (T2D) showed that many lack the understanding and skills to apply self-monitoring data to aid therapy adjustments. 2 High avoidance (avoiding thinking about blood glucose values and diabetes) and a sense of pointlessness of self-monitoring were associated with infrequent self-monitoring and use of self-monitoring data for insulin dose adjustments, and lack of sharing data with health care professionals. The authors suggested that if patients were guided in seeing the value of self-monitoring blood glucose it could improve adherence to self-monitoring.
A blood glucose meter (BGM) which is easy to use with features to assist patients with dose calculations may promote increased frequency of glucose testing and improved diabetes self-management. The FreeStyle InsuLinx BGM contains an in-built bolus insulin dose calculator. Insulin, medication doses, food intake, physical activity, and health information can be logged. In “easy” mode the meter suggests the insulin dose based on a “usual” prescribed meal dose, current and target glucose levels. In “advanced” mode carbohydrate intake and insulin-to-carbohydrate ratios are also taken into account. The main objective of this study was to evaluate ease of use and user preference of this meter compared to patients’ usual method of testing blood glucose and deciding insulin doses. A secondary objective was to compare the ease of use of the meter with other leading BGMs.
Patients and Methods
This was a randomized, 2-arm, cross-over study conducted at 7 sites in the United Kingdom from September 2011 to April 2012. The clinical protocol “Ease of Use of New BGM with In-Built Insulin Calculator at Home Study” (ADC-PMS-INX-11011) was approved by the National Research Ethics Committee. The study was registered on ClinicalTrials.gov (NCT01432275).
Study Participants
Eligible patients were adults with type 1 diabetes (T1D) or T2D on a multiple daily injection (MDI) insulin regime (insulin adjusting) for at least 6 months, regularly doing 3 or more blood glucose tests per day, and willing to do at least 4 tests daily, who had no previous experience of the FreeStyle InsuLinx meter (Abbott Diabetes Care, Alameda, CA; Test Meter) or the assigned comparator meter. All patients gave written informed consent.
Study Design and Plan
Patients used the Test Meter without the insulin calculator (BG mode) and 1 of 3 assigned comparator BGMs (Accu-Chek Aviva Nano [Roche Diagnostics, Mannheim, Germany; Comparator 1], Bayer Contour USB [Bayer Consumer Care, Basel, Switzerland; Comparator 2], LifeScan Verio Pro [LifeScan Europe, Zug, Switzerland: Comparator 3]) each for a 7-day period (Figure 1).
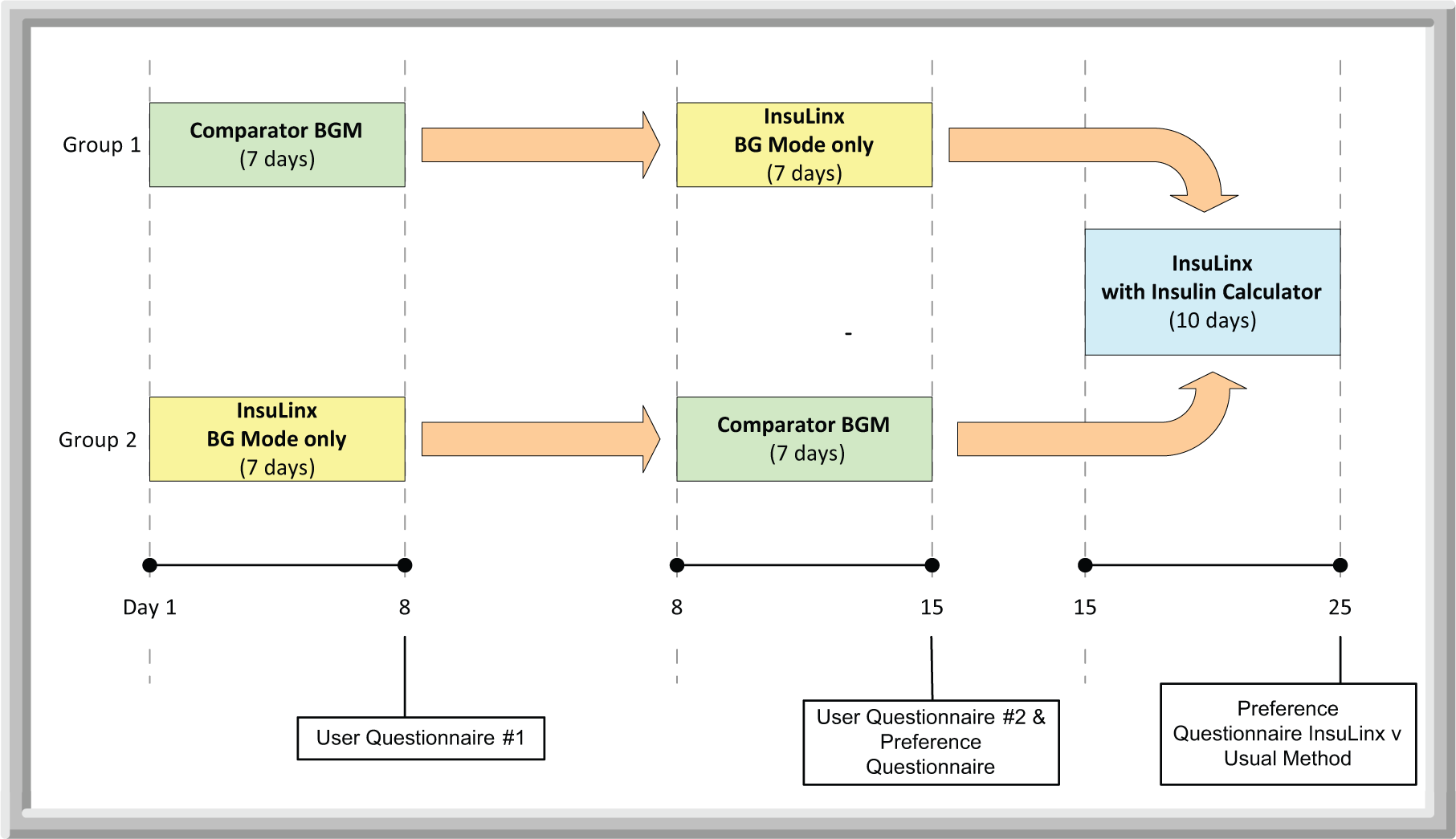
Study design.
They completed an ease of use questionnaire after each 7-day period for the BGM used, and after the second 7-day period a preference questionnaire comparing the 2 BGMs used. They then used the Test Meter with the in-built insulin dose calculator (IC mode) for 10 days, after which they completed a 2-part questionnaire, part A comparing the Test Meter with their usual method of testing blood glucose and calculating insulin dose, and part B evaluating specific features of the Test Meter.
Patients were randomized into 1 of 2 groups, to use either the Test Meter or comparator BGM first. A 1-hour training session was given to patients on use of the Test Meter in BG Mode and the comparator BGM, supported by use of a structured training checklist for each meter.
A half-hour training session on use of the Test Meter in IC mode was given after completing the first 14 days of the study. Easy mode setup was used in patients using a pattern-based insulin regime. Advanced mode setup was used for patients who used a carbohydrate-counting based insulin regime. No changes were made to patients’ usual insulin regimes.
Statistical Analysis
The exact binomial test for proportion was performed to determine the statistical significance of the inequality in preference, or inequality in agreement and disagreement with ease of use statements, in those patients stating a preference or an opinion. All analyses were conducted using SAS version 9.2. 3
Results
A total of 178 eligible adult patients were enrolled, of whom 164 completed the study. Baseline characteristics of these patients are shown in Table 1.
Baseline Characteristics of Patients (n = 164).
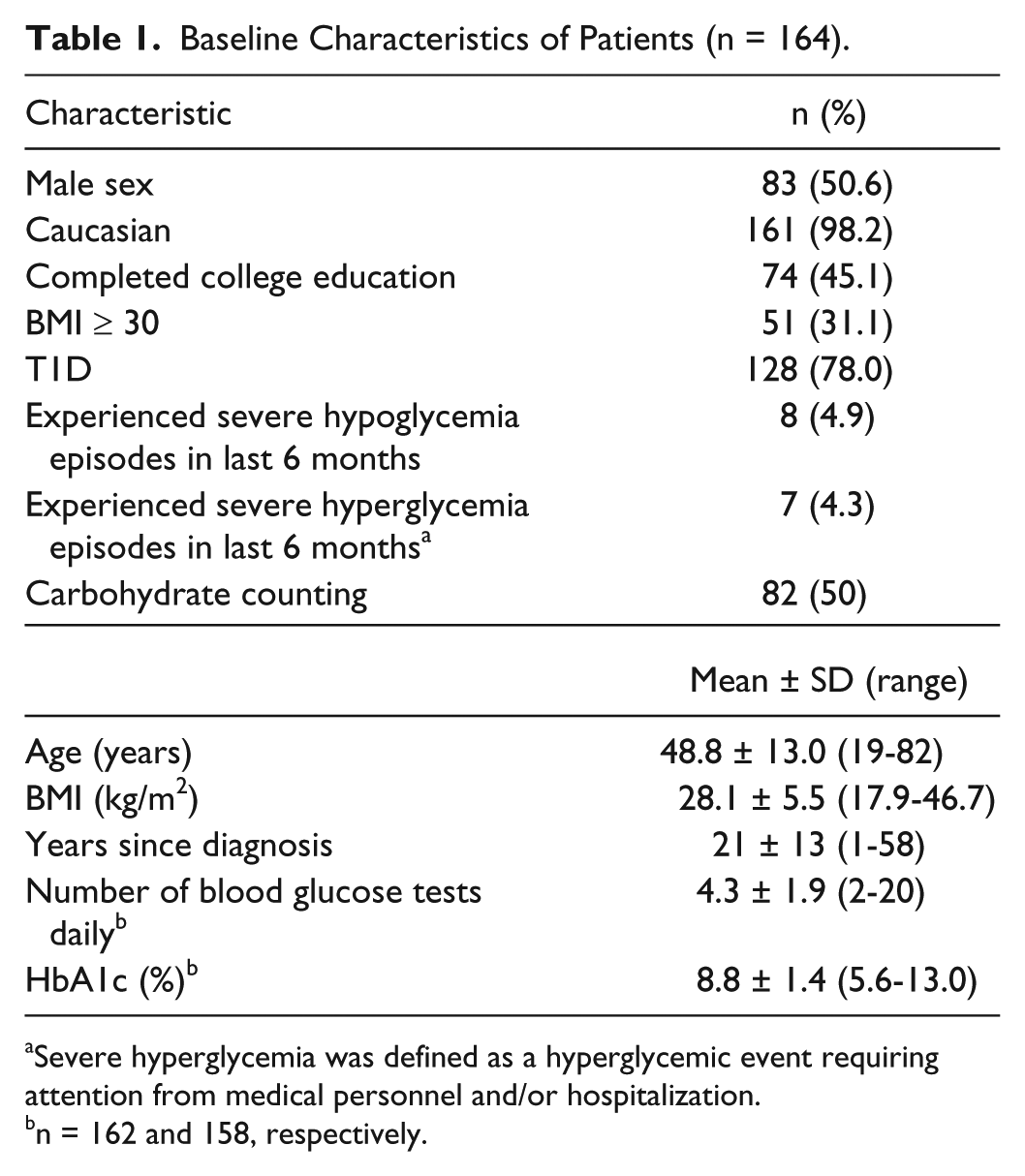
Severe hyperglycemia was defined as a hyperglycemic event requiring attention from medical personnel and/or hospitalization.
n = 162 and 158, respectively.
Ease of use questionnaires showed that most patients found all 4 study meters with their test strips easy to use and gave them information on how they were doing with their blood glucose. A significant majority of patients also considered that the Test Meter and Comparators 2 and 3 gave them information on how they were doing with managing their diabetes as well as how they needed to manage their blood glucose (Table 2).
Responses From Ease of Use Questionnaires About Study Meters.
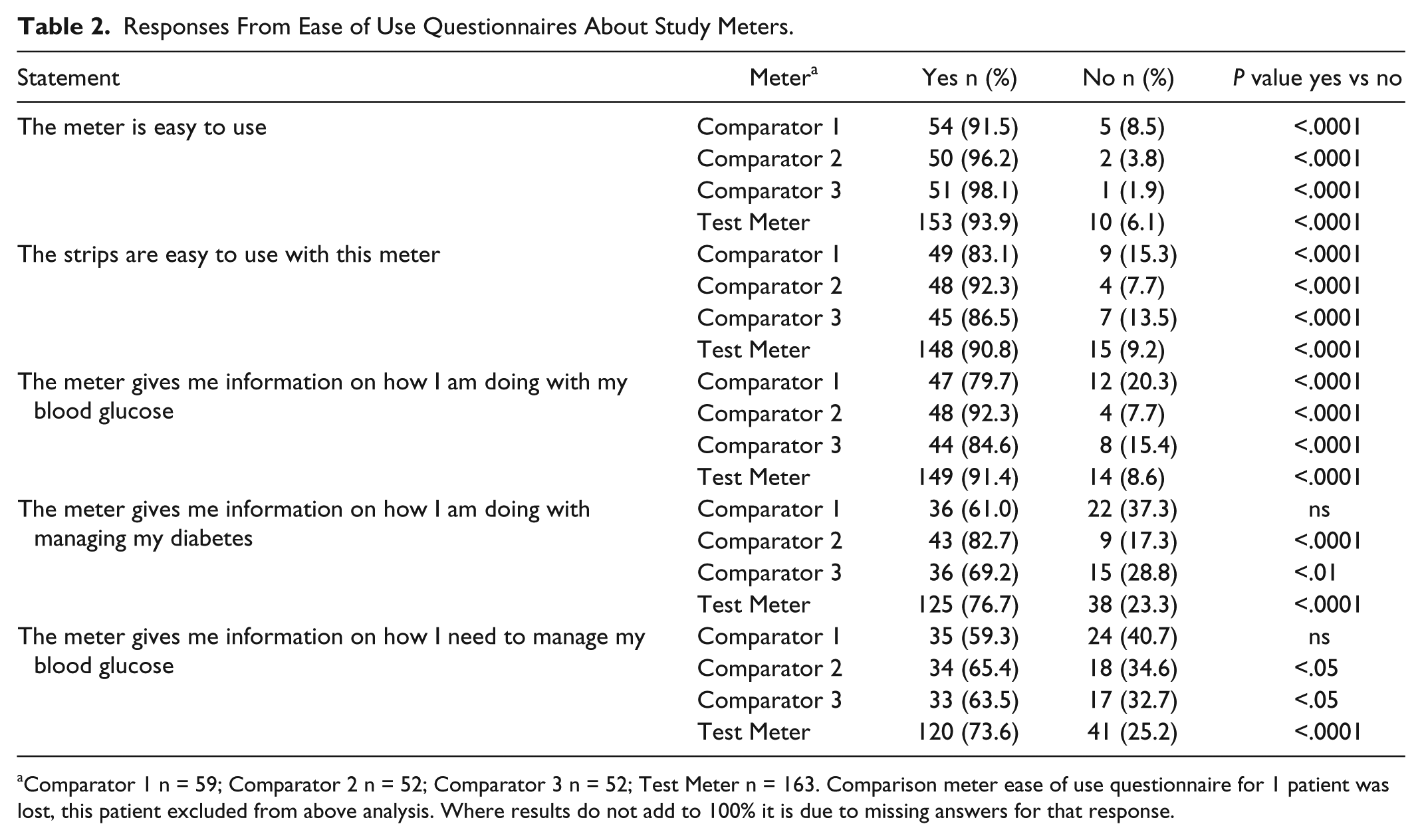
Comparator 1 n = 59; Comparator 2 n = 52; Comparator 3 n = 52; Test Meter n = 163. Comparison meter ease of use questionnaire for 1 patient was lost, this patient excluded from above analysis. Where results do not add to 100% it is due to missing answers for that response.
The results of the preference questionnaire between the 2 meters used by each patient are shown in Table 3. The Test Meter was significantly favored over Comparator 1. There was no significant difference in patient preference between the Test Meter and Comparators 2 and 3. The meters were rated as about the same in questions on individual aspects of use by 23-73% of patients. Among patients who expressed a preference in these questions, the Test Meter was significantly favored over Comparator 1 for all responses except for the number of error messages, and over Comparator 3 for easier set up of date, time and language, and for wasting fewer strips. Altogether 133 patients (81%) said they would definitely or probably change their meter for a study meter; 98 patients (60%) would definitely or probably change for the Test Meter.
Responses to the Preference Questionnaire Test Meter vs Comparator Meter.
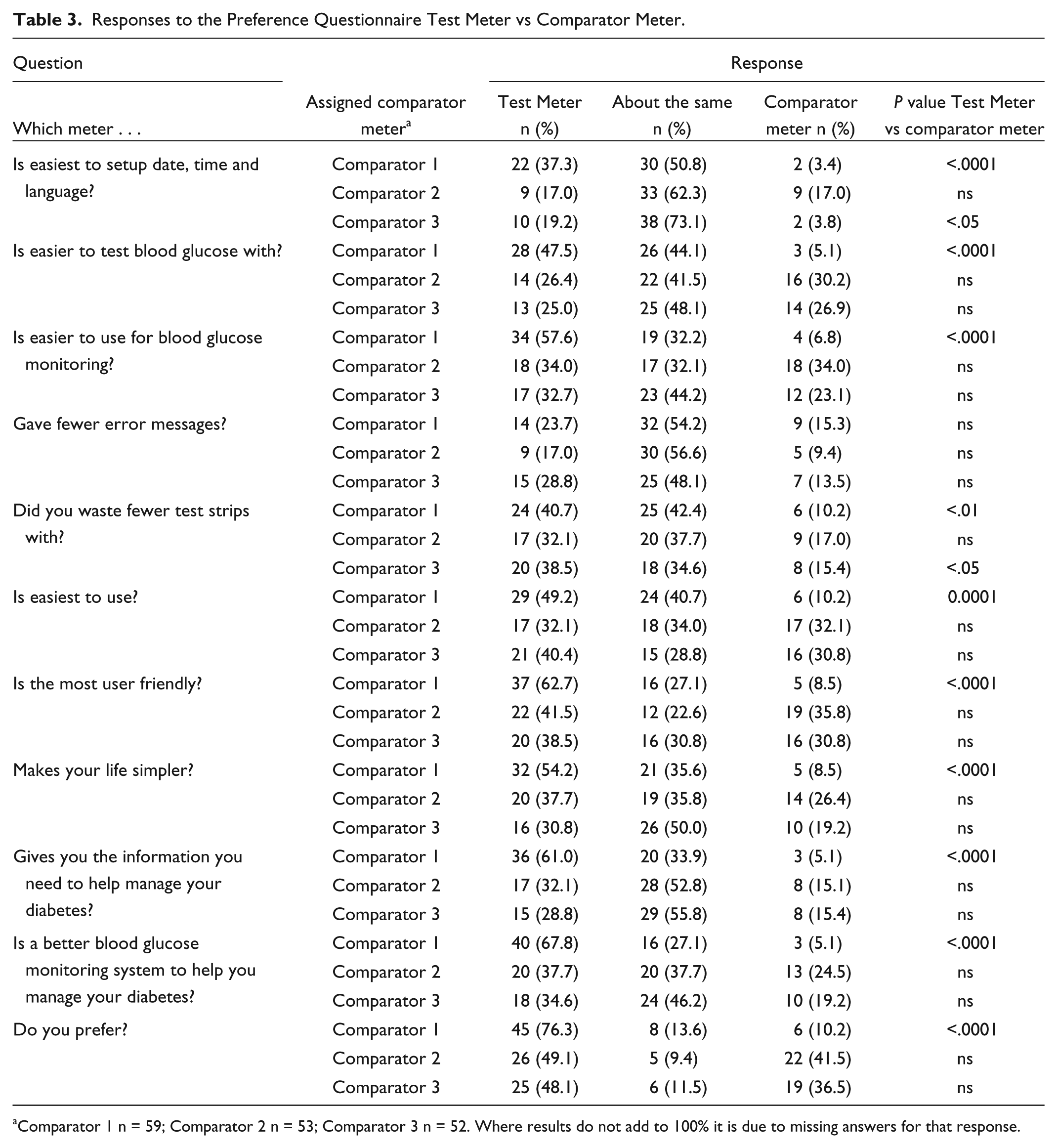
Comparator 1 n = 59; Comparator 2 n = 53; Comparator 3 n = 52. Where results do not add to 100% it is due to missing answers for that response.
Table 4 shows the meter features other than testing blood glucose levels indicated by patients to be important to them. The log book was by far the most valued feature.
Blood Glucose Meter Features Important to Patients.
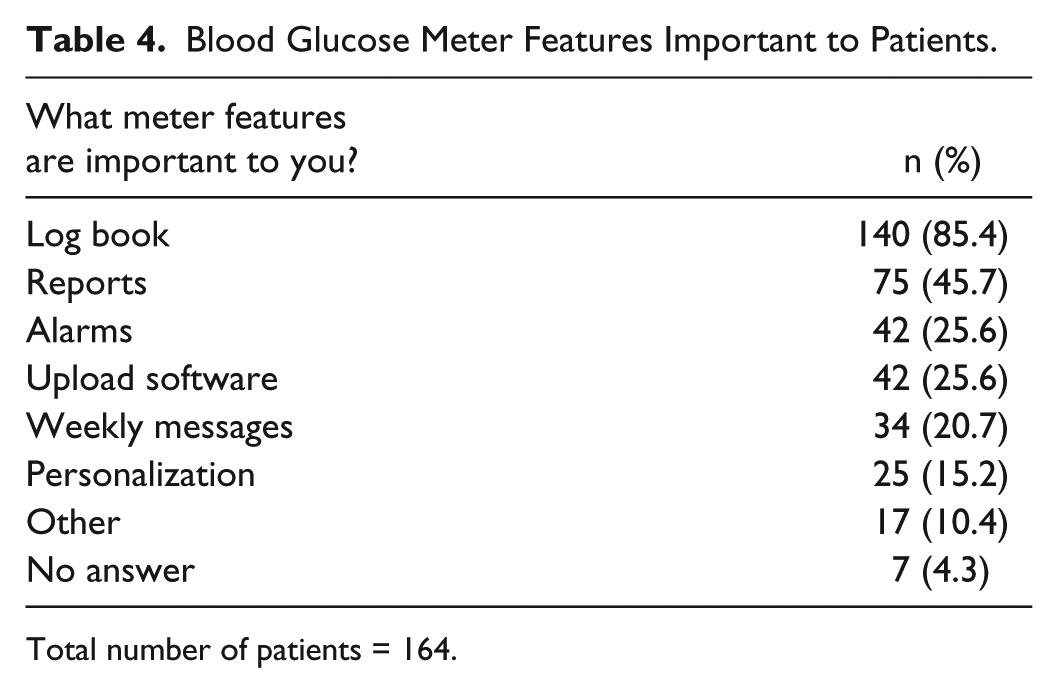

Total number of patients = 164.
Table 5 shows patients’ evaluation of specific features of the Test Meter. Most patients considered that the touch screen was easy to use; the system helped them decide their insulin dose and feel more confident about it and about managing their diabetes.
Patients’ Evaluation of Specific Features of the Test Meter.
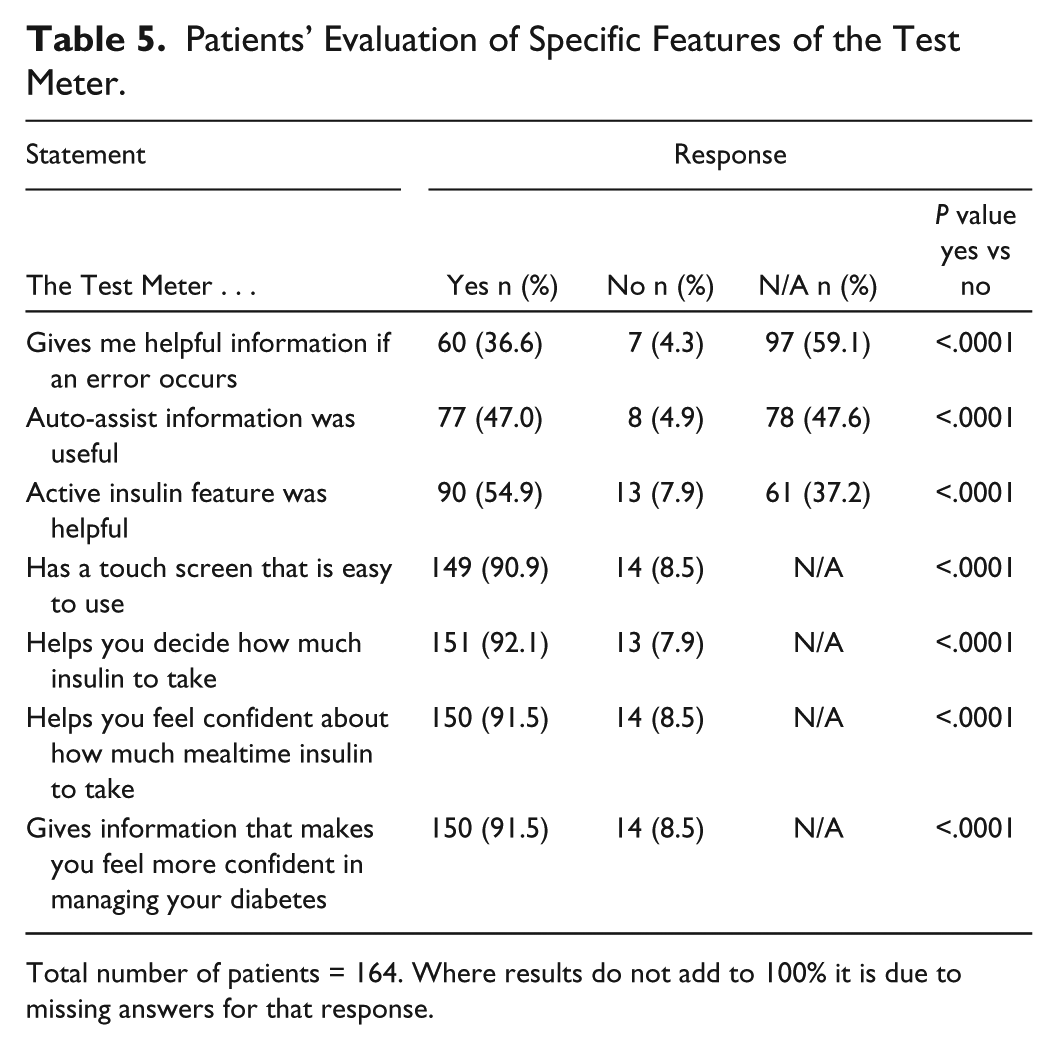
Total number of patients = 164. Where results do not add to 100% it is due to missing answers for that response.
Table 6 shows the results of the questionnaire comparing the Test Meter as a diabetes management tool compared to the patients’ usual method of testing blood glucose and calculating insulin dose. There was a significant preference for the Test Meter over patients’ usual method (76% vs 17%, P < .0001). Over 70% of patients considered the Test Meter was a better system to manage their diabetes, gave them the information they need to help manage their diabetes, made them feel more confident when adjusting their mealtime insulin and about managing their diabetes, and was more helpful and easier to decide and log an insulin dose.
Comparison of Test Meter to Patients’ Usual Method.
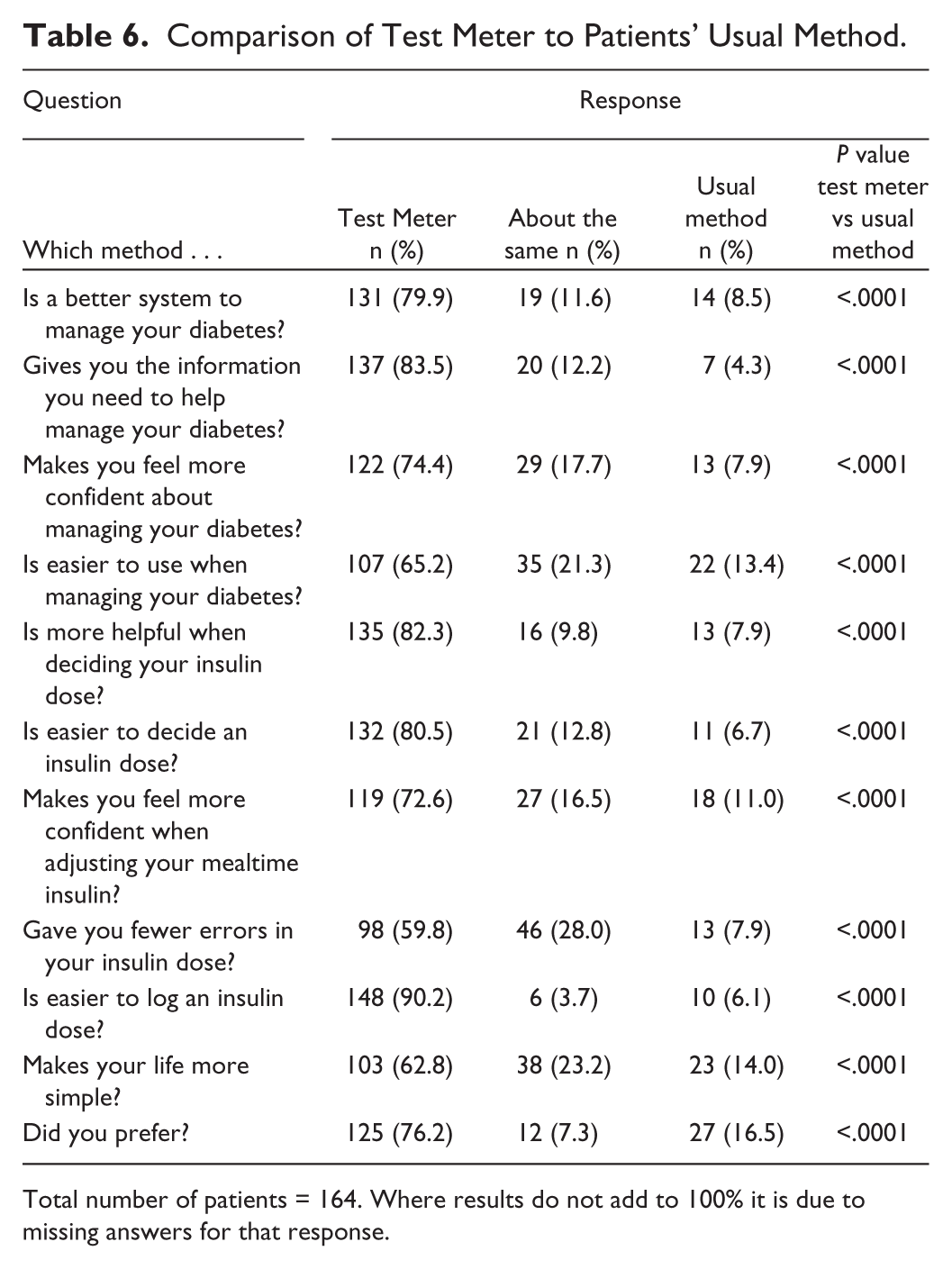
Total number of patients = 164. Where results do not add to 100% it is due to missing answers for that response.
Among the 125 patients expressing a preference for the Test Meter, the commonest reason cited in the free text section of the questionnaire related to the insulin calculator function (n = 55, 44%), followed by overall and specific aspects of ease of use (n = 40, 32%), and log book and other information functions (n = 26, 21%). Conversely, among the 27 patients who preferred their usual method, the most common cited reason (n = 9, 33%) also related to the insulin calculator, such as ability or preference to calculate own insulin doses or use prescribed doses, lack of trust in or inability to adapt to the insulin calculator, and self-reported hypoglycemia after taking the insulin dose recommended by the Test Meter. Four (15%) patients expressed not liking change, preferring or feeling more comfortable with usual routine.
Two patients had an episode of severe hypoglycemia during the study; 1 of these was assessed as not related to study device met serious adverse event (SAE) criteria; the other was assessed as possibly related to the study device. Both patients were using the Test Meter. Another patient reported an increased frequency of hypoglycemia throughout the study, during use of both Comparator Meter and Test Meter, in BG or IC mode.
Discussion
The main objective of the study was to evaluate the user preference and ease of use of a meter with an in-built insulin dose calculator, compared to patients’ usual method of testing blood glucose and deciding insulin doses, when used by patients on a MDI insulin regime. Of patients, 76% stated a preference for using the Test Meter system as a diabetes management tool over their usual method.
Over 70% of patients felt more confident adjusting their insulin and managing their diabetes, and over 90% considered the system easy to use, and gave them information on how they were doing with their blood glucose.
The fact that patients found the system helped in the interpretation of blood glucose test results and in using these to decide an insulin dose could help overcome the feelings of avoidance and pointlessness identified as obstacles to blood glucose self-monitoring. 2
A previous study showed that using the bolus calculator built into the Test Meter minimized errors in insulin dose determination. 4 Glaser et al observed a higher frequency of errors with conventional bolus calculation methods compared with an insulin dose calculation device. 1 They suggested that consistent use of the insulin dose calculation device may help to improve metabolic control. Maurizi et al demonstrated that using an insulin dose calculator did improve HbA1c levels in T1D patients compared to manual calculation. 5 A recent review on the use of BGMs with built-in bolus calculators concluded that these are effective motivational tools which empower the patient through an increased capability to translate self-monitored blood glucose values into appropriate therapeutic decisions. 6
A small proportion of patients, however, prefer familiar routines, calculating their own or using prescribed insulin doses; this must be acknowledged and supported. Potential risks of hypoglycemia in any automated system must also be borne in mind, and appropriate patient education in this respect is important.
In recent years much progress has been made in BGM technology, which now provides an array of features additional to blood glucose testing. This study gave further insight into patients’ views on such additional features. The log book feature was overwhelmingly the additional feature most valued by patients. Among patients who stated a preference for the Test Meter over their current method, the calculator function, ease of use and log book and other information functions were the most frequent cited reasons for their preference.
Budget constraints in many health care systems have resulted in restrictions on meter and test strip availability and choice, cost considerations being paramount irrespective of additional features. This study demonstrates patients’ different needs and preferences in respect of blood glucose monitoring, which should be acknowledged in any patient centered health care service. Clinicians should be supported to meet these individual needs and preferences, and thus promote patient collaboration, involvement and empowerment in managing their diabetes.
Conclusion
Over 70% of patients on a MDI insulin regime preferred the Test Meter, a BGM system with in-built insulin calculator, over their usual method of testing blood glucose and deciding insulin doses. They found it easy to use and felt more confident adjusting their mealtime insulin dose and managing their diabetes. This study has highlighted that patients have different preferences. Greater flexibility should be allowed by health care systems in supporting patients’ choices.
Footnotes
Acknowledgements
We thank the following for assistance: Study personnel at the 7 clinical sites for execution of this study; Walter Amor and Zoe Welsh (Abbott Diabetes Care) for assistance with statistical analysis.
Abbreviations
BGM, blood glucose meter; MDI, multiple daily injection; SAE, serious adverse event; T1D, type 1 diabetes; T2D, type 2 diabetes.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The trial was designed by Abbott Diabetes Care with input from the chief investigator. FreeStyle and related brand marks are trademarks of Abbott Diabetes Care Inc in various jurisdictions.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was sponsored by Abbott Diabetes Care Ltd.
