Abstract

Accurate insulin dosing can contribute to glycemic control, 1 but calculating mealtime insulin doses is challenging for many patients.2,3 The advent of blood glucose (BG) monitoring systems with built-in insulin bolus calculators enables patients to manage complex insulin dose calculations and minimize errors. 3 A multicenter, observational study was conducted to determine whether use of the FreeStyle InsuLinx Blood Glucose Monitoring System (Abbott Diabetes Care, Alameda, CA) in regular clinical practice could improve glycated hemoglobin (HbA1c) in patients with diabetes self-managing multiple daily injections (MDI) of rapid-/short-acting insulin.
In total, 203 patients (64% type 1 diabetes; 67% with baseline HbA1c ≥ 7.5%) were instructed in the use of the system, which was set up according to each patient’s preferred dose-calculation method: easy mode for fixed doses of mealtime insulin plus correction doses based on premeal BG levels, or advanced mode for carbohydrate counting. HbA1c was determined at baseline, and at 3 and 6 months. At each time point, patients completed a questionnaire to assess confidence in insulin calculation and changes in self-management.
Overall, mean HbA1c declined significantly from 8.25% at baseline to 8.08% at 6 months (P = .0333). In patients with baseline HbA1c ≥ 7.5% (ie, those with most clinical need for glycemic control), 4 the reduction was already significant at 3 months, and even greater by 6 months (Figure 1). In total, 73% of patients used the system in easy mode. In the overall population, there were no differences in HbA1c response between patients using the easy or advanced modes. However, among patients with baseline HbA1c ≥ 7.5%, significant reductions were only observed in those using easy mode (Figure 1). With advanced mode, there was no change in HbA1c at 3 months, although at 6 months the reduction was of a similar but nonsignificant magnitude to that seen in the easy mode subgroup (Figure 1). The lack of statistical significance might be a function of the small population of evaluable advanced-mode patients, or may reflect that these patients originally required less support for insulin management and had less benefit to gain than those using easy mode.
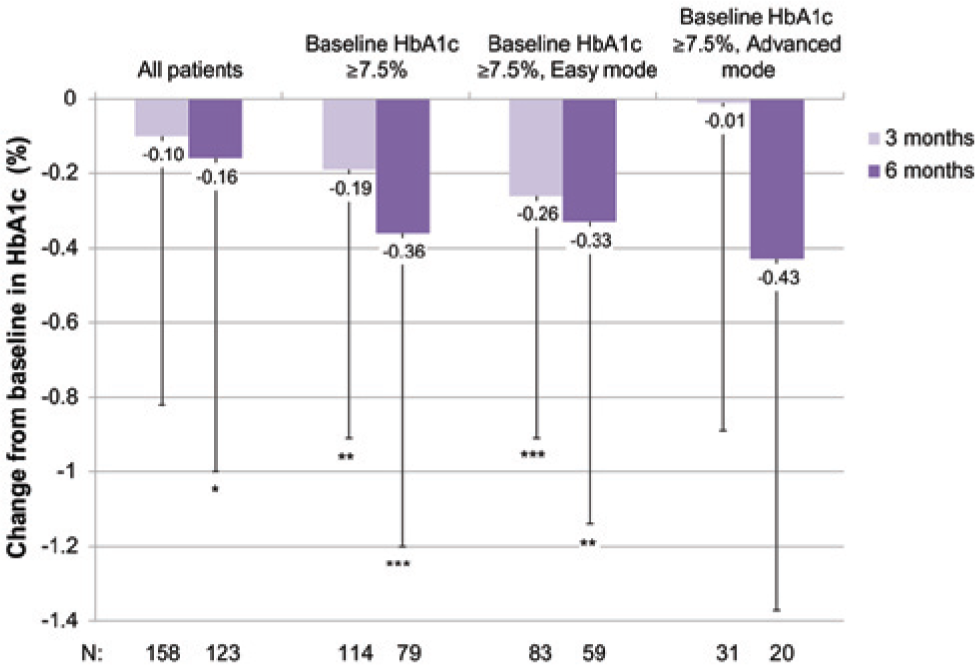
Change in HbA1c (%) from baseline in evaluable patients overall and in study subpopulations. N, evaluable patients for each analysis, defined as those with HbA1c values at baseline and at the specified visit assessment. Bars indicate standard deviation. *P < .05. **P < .01. ***P < .001.
Compared with prestudy behaviors, 57% of patients tested their glucose more frequently after 6 months’ use of the insulin calculator, 53% had a greater understanding of the need for glucose measurements, and 38% injected insulin more appropriately. Patients also expressed greater confidence in their ability to correct BG levels: Mean confidence score on a scale of 1 to 10 increased from 7.05 to 7.97 at 3 months (P < .0001, n = 174) and was maintained at 6 months. Furthermore, 95% of participants still using the system after 6 months indicated a preference to continue using Freestyle InsuLinx as their BG monitoring system.
We conclude that use of a BG monitoring system with built-in automated insulin bolus calculator in a real-world setting improved glycemic control and self-management in patients with diabetes routinely receiving MDI of insulin, and increased confidence in calculating accurate insulin doses. A randomized controlled trial is warranted to confirm these findings.
Footnotes
Acknowledgements
We thank the following for their invaluable assistance in the execution of this study: the diabetes teams of the participating Hospitals (Medisch Centrum Haaglanden, The Hague; Lange Land Ziekenhuis, Zoetermeer; Atrium Medisch Centrum Parkstand, Heerlen; Elkerliek Ziekenhuis, Helmond; Zorgsaam Ziekenhuis, Terneuzen; Meander Medisch Centrum, Amersfoort; Orbis Medisch Centrum, Geelen; Joren Bosch Ziekenhuis, Den Bosch; Amphia Ziekenhuis, Breda).
Abbreviations
BG, blood glucose; HbA1c, glycated hemoglobin; MDI, multiple daily injections.
Declaration of Conflicting Interests
Judith van Niel was a member of the FreeStyle InsuLinx Advisory Boards for Abbott Diabetes Care and received fees for lectures. Petronella H. Geelhoed-Duijvestijn received a fee for a lecture at FEND 2012. FreeStyle and related brand marks are trademarks of Abbott Diabetes Care Inc in various jurisdictions.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was sponsored by Abbott Diabetes Care, Alameda, CA, USA and CZ Health insurance Company (Netherlands). Medical writing support was provided by Joanne Fitz-Gerald, ACUMED® (Tytherington, UK), with funding from Abbott Diabetes Care.
