Abstract
Objective
This study aimed to analyze the disease burden and risk factors of nasopharyngeal carcinoma (NPC) in China in 2019, assessing trends from 1990 to 2019 to inform prevention and treatment.
Methods
Utilizing the Global Burden of Disease Study 2019 (GBD 2019) Data, a descriptive analysis method was employed to analyze the disease burden and risk factors for NPC in China in 2019. Additionally, the disease burden of NPC in China from 1990 to 2019 was examined. The Joinpoint Regression Program was used to estimate the annual percent change (APC) and the average APC (AAPC).
Results
From 1990 to 2019, the number of new NPC cases in China increased from 47.49% to 62.57% of the global NPC cases, and the proportion of prevalence in China to the world rose from 45.29% to 70.81%. The total change rates of the age-standardized incidence rate (ASIR) globally and in China were 36.77% and 70.69%, respectively. The total change rates of the age-standardized prevalence rate (ASPR) globally and in China were 115.34% and 232.52%, respectively. The increase in ASIR and ASPR in China was significantly higher than the global average. The decrease in age-standardized death rate, standardized disability-adjusted life years rate, and standardized years of life lost due to premature mortality rate in China was much more pronounced than globally. From 1990 to 2019, the ASIR and ASPR in China showed an upward trend, with AAPCs of 1.80% and 4.19%, respectively. Over the past 30 years, the incidence among young and middle-aged individuals in China has increased, indicating a trend toward younger age at onset. In all periods, the risk of incidence, prevalence, and death in males was significantly higher than in females.
Conclusion
In summary, the disease burden of NPC in China remains significant. Therefore, continued attention and strengthening of risk factor control, along with strategies for early diagnosis and treatment, are essential.
Keywords
Graphical Abstract

Introduction
Nasopharyngeal carcinoma (NPC) is a type of squamous cell carcinoma that occurs in the epithelial mucosa of the nasopharynx. 1 This disease shows a significant regional aggregation tendency, especially prevalent in East and Southeast Asia, and particularly in Southern China. 2 NPC is highly sensitive to radiation therapy, and the widely used intensity-modulated radiotherapy (IMRT) has significantly improved local and regional control rates. 3
Due to the often indistinct early symptoms of NPC, ~80% of patients are diagnosed at middle or late stages. These patients require various treatments, including radiotherapy, chemotherapy, and immunotherapy, which are lengthy, expensive, and often have numerous side effects with limited effectiveness. 3 Once metastasis occurs, the prognosis of NPC is grim, with a death rate of 91% within the first year after initial metastasis, 4 imposing a significant disease burden in China. Currently, there is a relative scarcity of research on the disease burden and risk factors of NPC in China.
Previous studies have explored the trends in NPC incidence and mortality in China using age-period-cohort patterns, 5 while this study, utilizing data from the Global Burden of Disease Study 2019 (GBD 2019), aims to explore the current status and trends in the disease burden of NPC in China from 1990 to 2019. The objective is to provide a scientific basis for formulating targeted public health policies and for the rational allocation of medical resources.
Materials and Methods
Sources of Information
This study is a secondary analysis of the results of the GBD 2019 study. The data for this study were obtained from the Global Health Data Exchange database (https://gbd2019.healthdata.org/gbd-results/). 6 Standardized population data were obtained from the GBD world population estimates (https://ghdx.healthdata.org/record/ihme-data/gbd-2019-population-estimates-1950-2019).
Indicators for Evaluating the Burden of Disease
The number and rate of incidence, prevalence, death, and disability-adjusted life years (DALYs) were used as indicators to evaluate the disease burden of NPC in China. DALYs include 2 parts: years of life lost due to premature mortality (YLL) and years lived with disability (YLD), which comprehensively take into account the burden of premature death and disability caused by disease. 7
N is the number of deaths of a disease in different age groups and genders, and L is the life loss value of each age group, that is, the expected life value corresponding to the death age point in the standard life table.
Prev is the prevalence number with a disease; DW is the disability weight, 0 means complete health, and 1 means death. 8
The YLD rate, YLL rate, and DALYs rate are calculated by the ratio of YLD, YLL, and DALYs to the population of this group, respectively.
Risk Factor Evaluation Index
GBD used counterfactual analysis to calculate the disease burden attributed to risk factors. Assuming that the exposure level of other risk factors in the population remains unchanged, compare the exposure distribution of the target risk factors with the theoretical minimum risk exposure level, and calculate the proportion of the disease burden attributed to the risk factors, that is, the population attributable fraction (PAF). 9
The attributable DALYs rate is estimated to be the total DALYs rate for the outcome multiplied by the PAF for the risk-outcome pair for each age, sex, location, and year. 10
Classification of Risk Factors for NPC in the GBD 2019
Of the 87 risk factors for disease burden reported by the GBD 2019, a small proportion of NPC cases can be attributed to 3 risk factors: alcohol use, occupational exposure to formaldehyde, and smoking. Detailed definitions, along with the extraction process and data source references, can be found in the Supplement Materials.
Statistical Methods
First, the descriptive analysis method was used to analyze the disease burden and risk factors for NPC in 2019 in China. Second, the incidence, prevalence, death, and disease burden of NPC in China from 1990 to 2019 were analyzed by age and sex. The changing trend of the disease burden of NPC in China from 1990 to 2019 was analyzed by Joinpoint 4.7 (https://surveillance.cancer.gov/joinpoint/), and the annual percent change (APC) and average APC (AAPC) were calculated by a logarithmic linear regression model. The significance level is set to 0.05. In addition, we explored the main risk factors affecting the incidence of DALYs. The differences in risk factors between sexes and different age groups were investigated. The changes in risk factors for NPC from 1990 to 2019 were analyzed. DALYs are used to evaluate the disease burden. All data analyses were performed using the open-source software R (version 4.3.1; R Foundation for Statistical Computing, Vienna, Austria, https://www.r-project.org/).
Results
Disease Burden of NPC in the World and China in 1990 and 2019
From 1990 to 2019, while China’s proportion of the global population decreased, the number of new NPC cases in China increased from 47.49% to 62.57% of the global total. During the same period, the proportion of the prevalence number in China to the world increased from 45.29% to 70.81%. From 1990 to 2019, the proportion of deaths in China decreased from 49.70% to 40.02% of the global total. Due to the decline in death numbers from 1990 to 2019, the proportion of YLLs in China decreased from 49.81% to 37.87%, and the proportion of DALYs in China decreased from 49.74% to 39.06% of the global total. From 1990 to 2019, the proportion of YLDs in China increased from 45.37% to 66.60%. Concurrently, the global YLL/DALY No ratio of NPC decreased from 98.44 to 95.86, while in China, it decreased from 98.58 to 92.94, indicating a significant decline in China (Table 1).
1990 and 2019: The Number of NPC in the World and China.

Abbreviations: DALYs, disability-adjusted life years; NPC, nasopharyngeal carcinoma; YLD, years lived with disability; YLL, years of life lost due to premature mortality.
In 2019, the crude incidence rate, prevalence rate, and death rate of NPC in China were 7.76, 48.38, and 2.01/100,000, respectively. The crude rates for DALYs, YLD, and YLL were 64.13, 4.53, and 59.60/100,000, respectively, with the YLL rate being about 13.16 times higher than the YLD rate. Regarding total change rates from 1990 to 2019, the global and China-specific age-standardized incidence rates (ASIRs) changed by 36.77% and 70.69%, respectively. The total change rates for the age-standardized prevalence rate (ASPR) globally and in China were 115.34% and 232.52%. The change rates for ASIR and ASPR in China were significantly higher than the global average. The decline in China’s age-standardized death rate (ASDR), standardized DALYs rate, standardized YLL rate, and YLL rate/DALY rate was also much higher than the global average. In terms of standardized rates, China’s ASIR, ASPR, ASDR, standardized DALYs rate, standardized YLL rate, and standardized YLD rate in 1990 and 2019 were approximately twice the global average (Table 2).
Crude Rate and Standardized Rate (Per 100,000) of NPC in the World and China in 1990 and 2019.

Abbreviations: DALYs, disability-adjusted life years; NPC, nasopharyngeal carcinoma; YLD, years lived with disability; YLL, years of life lost due to premature mortality.
In 2019, the incidence number, prevalence number, death number, DALYs number, and the rates of incidence, prevalence, death, and DALYs in males were significantly higher than those in females. The highest incidence number for both men and women was in the 50 to 54 age group (Figure 1a). For individuals under 55 years old, the prevalence number and DALYs number increased with age in both genders (Figure 1b). The number of deaths was higher in the 50 to 70 age group (Figure 1c).

Disease burden of nasopharyngeal carcinoma in Chinese men and women in 2019. The numbers and rates of incidence (a), prevalence (b), deaths (c), and DALYs (d) of nasopharyngeal carcinoma per 100,000 population by age and sex in 2019. The figure shows the upper and lower limits of the 95% UIs. DALYs, disability-adjusted life years; 95% UIs, 95% uncertainty intervals.
The incidence rate trend for both men and women was similar, increasing with age in those under 60 and then showing a slow decrease followed by an increase in those over 60 years old (Figure 1a). The prevalence rate initially increased and then decreased with age (Figure 1b). The peak prevalence rates for males and females were at ages 50 to 54 and 55 to 59, respectively, with rates of 131.12 and 47.99/100,000 (Figure 1b). The death rate increased with age (Figure 1c). The DALYs rate initially increased and then decreased with age, peaking at 210.54/100,000 for males aged 65 to 69 and 73.73/100,000 for females aged 70 to 74 (Figure 1d).
Epidemic Trends and Joinpoint Regression Analysis of NPC in China From 1990 to 2019
From 1990 to 2019, the incidence and prevalence of NPC in China exhibited an increasing trend (Figure 2a and b). The ASIR and ASPR in China showed an upward trend during this period, with the AAPCs being 1.80% [95% confidence interval (95% CI): 1.30%-2.32%] and 4.19% (95% CI: 3.68%-4.70%), respectively, a statistically significant difference (P < .001). The most significant increases in ASIR and ASPR in China were from 2006 to 2009 (APC = 6.70%, APC = 11.19%; Table 1; Figures S1 and S2). Overall, the number of deaths and DALYs did not change substantially. The ASDR and age-standardized DALYs rate of NPC in China showed a decreasing trend from 1990 to 2019, with the AAPC being −2.45% (95% CI: −2.58% to −2.33%) and −2.39% (95% CI: −2.52% to −2.26%), respectively. The risk of incidence, prevalence, and death in men was significantly higher than that in women during all periods (Table 3; Figures 2c and d, S3, and S4).
The Age-Standardized Rates of Nasopharyngeal Carcinoma in China From 1990 to 2019 by Joinpoint Regression.

Abbreviations: AAPC, average annual percent change; APC, annual percent change; ASDR, age-standardized death rate; ASIRs, age-standardized incidence rates; ASPR, age-standardized prevalence rate; DALYs: disability-adjusted life years.
*P < 0.05.
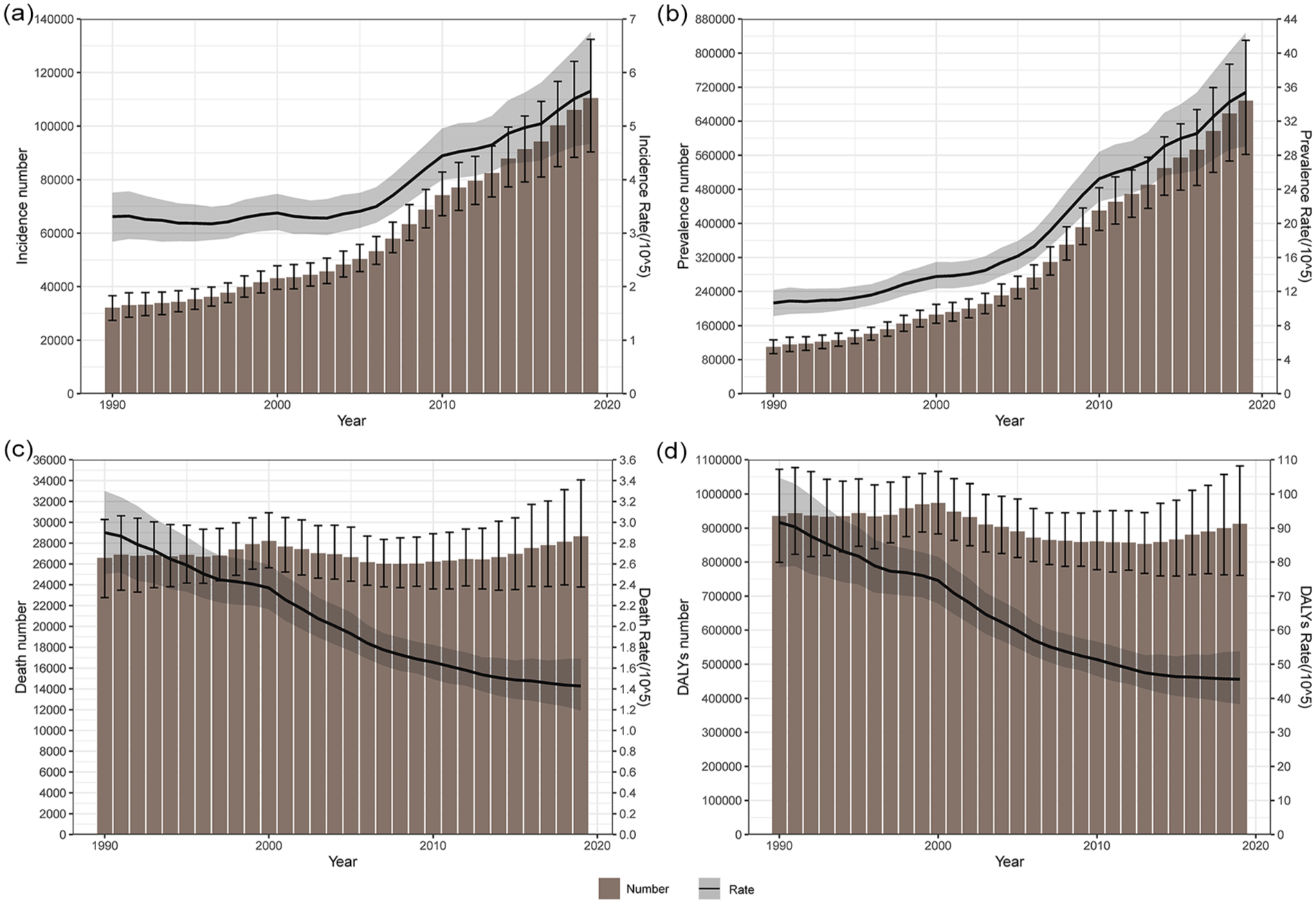
The age-standardized numbers and rates of incidence (a), prevalence (b), deaths (c), and DALYs (d) of nasopharyngeal carcinoma per 100,000 population from 1990 to 2019. The figure shows the upper and lower limits of the 95% UIs. DALYs, disability-adjusted life years; 95% UIs, 95% uncertainty intervals.
Trends of NPC by Age in China From 1990 to 2019
In terms of age groups, from 1990 to 2019, the incidence rate in the 25 to 59 age group showed an increasing trend, while in the over 60-year-old group, it decreased slowly before 2006 and then increased. The age group with the highest incidence rate shifted from those aged 80+ in 1990 to 55 to 59 years old in 2019 (Figure 3a).

The rates and numbers of incidence (a, b), prevalence (c, d), deaths (e, f), and DALYs (g, h) of nasopharyngeal carcinoma per 100,000 population in different age groups from 1990 to 2019. DALYs, disability-adjusted life years.
On the other hand, the number of incidence cases in the age group over 25 years old shows a yearly upward trend, with the 45 to 59 age group experiencing a rapid increase, which should receive special attention (Figure 3b).
From 1990 to 2019, the prevalence rate and number in the age group over 25 years old showed an increasing trend, with the prevalence number in the 30 to 69 age group increasing rapidly each year, which needs more attention (Figure 3c and d).
From 1990 to 2019, the death rate of all age groups showed a downward trend, while the number of death cases showed a downward trend in the younger age groups and a rapid upward trend in the age group aged 65 and above (Figure 3e and f).
From 1990 to 2019, the DALY rate of each age group showed a downward trend, with the number of DALY cases consistently high in the 45 to 64 age group over the years. The number of DALY cases has been increasing year by year since 2008 in the 65 to 69 age group (Figure 3g and h).
Risk Factors for NPC in China by Sex and Age in 2019
The DALYs rate attributable to risk factors and the percent DALYs attributable to risk factors in 2019 varied among different sexes and age groups, with rates and percentages significantly higher in males than in females. Among men, the contribution of smoking and drinking is approximately equal, while in women, the contribution from drinking is higher. Smoking affects only those over the age of 30.
In 2019, among males, the DALY rate attributable to the 3 risk factors increased with age and then decreased. The DALY rates attributed to alcohol use, occupational exposure to formaldehyde, and smoking peaked at ages 60 to 64, 45 to 49, and 65 to 69 (111.80, 2.77, and 95.03/100,000, respectively). In women, the attributable DALY rate at all ages is much lower than in men, and the DALYs rate caused by alcohol use is higher than that caused by smoking across all age groups (Figure 4a).
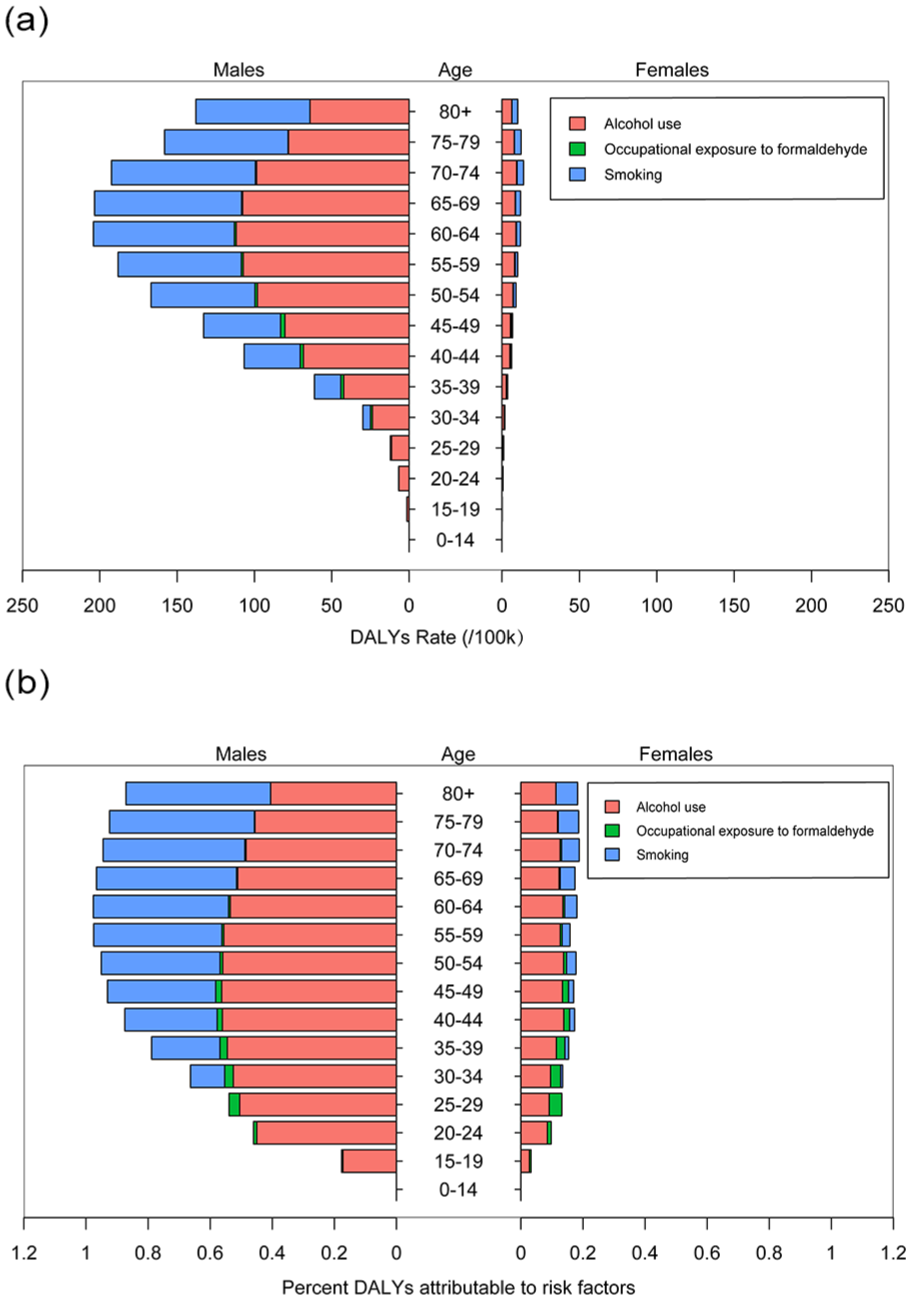
The DALYs rate attributable to the risk factors (a) and proportions of DALYs attributable to risk factors (b) by age and sex in 2019. DALYs, disability-adjusted life years.
The PAF of alcohol use in men is higher in the age group over 20, but there is no significant difference in PAF among different age groups. The PAF of smoking increases with age. In women, the PAF of alcohol use is higher than that of smoking, and the PAF of smoking increases with age. In addition, the PAF for exposure to formaldehyde in both men and women aged 25 to 29 accounted for the highest proportion among all age groups (Figure 4b).
Changes in Risk Factors for NPC in Men and Women From 1990 to 2019 in China
From 1990 to 2019, the standardized DALY rate attributable to all 3 risk factors showed a decreasing trend in both sexes, with the rate in males being significantly higher than in females (Figure 5a and b). The total PAF in both men and women displayed an increasing trend over the years. The male PAF for smoking changed little over time, while the PAF for alcohol use exhibited a slow upward trend (Figure 5c and d). Among the 3 risk factors, the standardized DALYs rate and PAF attributed to alcohol use were the highest in both men and women. The impacts of smoking and alcohol use cannot be ignored, nor can occupational exposure.

The DALYs rate attributable to the risk factors (a, b) and proportions of nasopharyngeal carcinoma due to specific risk factors (c, d) in China by sex from 1990 to 2019. DALYs, disability-adjusted life years.
Discussion
Compared to the world level, the disease burden of NPC in China has always been severe. The cause of the disease is still unclear, and it may be related to Epstein-Barr Virus (EBV) infection, genetic factors (tumor-related family history), unhealthy dietary habits (pickled food and high-salt diet), poor behavioral habits (smoking and drinking), environmental or occupational factors, race, sex, and age. 11 EBV infection contributes to 95% of NPC incidences in endemic regions and plays a significant role in its pathogenesis, particularly in Southern China, with a higher prevalence in males and certain age groups. The association between EBV and NPC was first linked to elevated IgG and IgA antibody titers to Viral Capsid Antigen (VCA) and Early Antigen (EA), which correlate with tumor burden and occur 1 to 2 years before tumor development, suggesting EBV reactivation may be involved in tumorigenesis. 12
This study analyzed the incidence, prevalence, death, and disease burden of NPC in China in 2019 (cross-sectional data) and over the period 1990-2019 (trend data). In 2019, the incidence number and rate, prevalence number and rate, death number and rate, DALYs number and rate of NPC in males were much higher than those in females, which may be related to the following reasons: in terms of risk factors, the standardized DALYs rate of the attribution of risk factors in males was higher than that in females. The sex ratio (male to female ratio) at birth since 1980 is higher than normal. 13
According to the age distribution of NPC in 2019, the incidence, prevalence, and DALY rates in men and women aged 40 to 69 were higher, peaking in the 50 to 54 age group, with a high number of deaths also in the 50 to 74 age group, which represents a significant portion of the working-age population. More attention should be given to early screening of NPC in these younger age groups. The trends of incidence rate, prevalence rate, and DALYs rate were the same between men and women. Except that the incidence rate increased sharply over 80 years old, the rate and number trend of prevalence and DALYs were similar. From the perspective of risk factors in 2019, the DALYs rate attributable to smoking plus alcohol use in men over 40 years old exceeded 100/100,000, with the DALYs rate and PAF for smoking and alcohol use being higher in men. Strengthening control of risk factors, such as tobacco and alcohol control, is necessary.
The results showed that the ASDR and DALY rates of NPC decreased from 1990 to 2019. This may be due to the great progress made by the medical community in early screening and treatment in recent years. There is a great difference in the treatment plan and therapeutic effect between early NPC and middle and advanced NPC. Patients with early NPC do not need chemotherapy; the 5-year survival rate is more than 90%, the treatment cycle is short, and there are fewer side effects. The double antibody regimen and Xia Ning-Shao P85-Ab biomarker regimen increased the rate of early diagnosis and early treatment of NPC. 4 Second, current treatment options for NPC include brachytherapy, external radiotherapy, stereotactic radiosurgery, nasopharyngectomy, chemotherapy, and photodynamic therapy (PDT), either alone or in different combinations.14 -16 NPC is highly sensitive to ionizing radiation, and radiotherapy is the basic treatment for NPC. With the passage of time, radiotherapy technology has developed from initial 2-dimensional (2D) radiotherapy to 3D conformal radiotherapy and then to IMRT. IMRT, a precision radiotherapy technique enabling the conformation of high doses to concave-shaped tumors while protecting normal tissues, is now the standard of care for NPC. 17 After improvement, local control and survival are enhanced, and toxicity is reduced. 2 With the wide application of IMRT and the addition of chemotherapy, targeting, and immunotherapy, the 5-year survival rate of NPC has reached 80%. Hyperfractionated IMRT can increase the survival rate by nearly 20%. 18 PDT is a minimally invasive technique that can be repeatedly applied at the same site, unlike ionizing radiation. It is particularly useful in oncology because it can be combined with chemotherapy, ionizing radiation, or surgery. PDT is effective for treating local failures of NPC with a depth of <10 mm and can be performed easily under local anesthesia. Furthermore, PDT has proven to be effective in treating residual disease, providing good results for patients with an incomplete response after initial treatment.15,16 At the same time, the promotion of smoking cessation programs and the increase in sports activities are also part of the reason. 19
The incidence number, ASIR, prevalence number, and ASPR of NPC in China all showed an increasing trend from 1990 to 2019. The AAPC of ASIR and ASPR were 1.80% and 4.19%, respectively. From 1990 to 2019, China’s proportion of the world’s incidence rate has increased significantly. At the same time, the change rate of ASIR and ASPR in China is nearly twice that of the world. This shows that the problem of NPC in China cannot be ignored and that there is no delay. China should strengthen 20 the medical investment in NPC.
Age is an important factor affecting the incidence and prevalence of NPC. From 1990 to 2019, the number and rate of incidence and prevalence in the 30 to 69 age group increased year by year, with the 40 to 44 age group showing the highest prevalence rate, and the prevalence growth rate in the 25 to 49 age group exceeding 50%. This suggests a trend of younger onset of NPC, which is consistent with the findings of Bai et al. 5 Bai et al attributed this trend to smoking and occupational exposure. Studies have shown that the smoking rate peaks in the 25 to 34 age group, where not only is the smoking prevalence higher, but the smoking volume is also significantly greater. 21 Although smoking is not the primary cause of NPC, it may contribute to an increased risk by compromising the immune system, promoting EBV reactivation, or interacting with other environmental carcinogens.20,22,23 In addition, the 25 to 49 age group has the highest occupational exposure to NPC-related risk factors. Many individuals in this age range are frequently exposed to carcinogenic substances such as cadmium, 24 smoke, dust, and various chemicals in their workplaces. Several studies have found that occupational exposure can increase the risk of NPC by 2 to 6 times.25,26 Prolonged exposure to these occupational hazards may lead to chronic inflammation and DNA damage in the nasopharynx, further contributing to EBV-related tumorigenesis. Despite the potential roles of smoking and occupational exposure, EBV infection remains the primary cause of NPC in China. Based on a real-world study in Southern China, the majority of NPC cases are EBV-related, with 94.8% of patients (239/252) testing positive for EBV-encoded small RNA (EBER), highlighting the strong association between EBV and NPC in this region. 27 Therefore, strengthening early screening and preventive measures for high-risk populations is crucial to reducing the burden of NPC. Furthermore, advancements in early screening and diagnostic methods may also contribute to the observed increase in NPC prevalence. In recent years, the widespread application of EBV detection techniques, such as serological testing, polymerase chain reaction for viral load quantification, and in situ hybridization of EBER in biopsy tissues, has significantly improved the early detection rate of NPC, particularly in high-incidence regions. 28 As screening programs expand and detection technologies become more accessible, the increased detection of subclinical or early-stage NPC may partly explain the rising prevalence in younger age groups. This suggests that the observed trend reflects not only a potential increase in NPC incidence but also the impact of improved medical screening and diagnostic capabilities.
From the changes of risk factors for NPC from 1990 to 2019, the standardized DALYs rates of both men and women showed a downward trend due to the decline in death and YLL rates, while the PAF of smoking remained almost unchanged from 1990 to 2019, whereas that of alcohol consumption in both men and women increased year by year, which should receive continuous attention. Although GBD 2019 has performed a correlation analysis of occupational exposure to formaldehyde as a risk factor for NPC, the role of formaldehyde in NPC risk is controversial, 29 with 1 multicenter study supporting the hypothesis that occupational exposure to formaldehyde increases the risk of NPC 30 and another study showing that no association between NPC and formaldehyde. 31 Chang et al also suggested that the association with occupational formaldehyde exposure is unknown. 23 At the same time, Song et al 29 proposed that occupational formaldehyde exposure had little effect on the etiology of NPC. However, it is worth noting that the GBD risk factor analysis for NPC is still insufficient. As we can see, even for the top 3 risk factors listed by GBD for NPC, the combined proportion of these 3 factors in the most affected gender and age groups is <1%. Additionally, in the year with the highest contribution from risk factors, the combined proportion remains below 1%. This analysis only covers the interannual changes and the gender-age distribution of these risk factors.
Bai et al 5 analyzed the period cohort effect of NPC in China. For period effects, the males’ RRs of NPC incidence increased continuously over all periods and increased in females after 2010. For cohort effects, the RRs of NPC incidence continually increased with later birth cohorts, and the increase stopped after the 1985 birth cohort. The period and cohort effects on NPC death rate continuously declined for both sexes. Song et al 29 predicted that the ASIR will increase by 41.2% in China between 2019 and 2035, indicating that NPC remains a major health challenge.
There are some limitations to this study. The availability of raw data is a major limitation of GBD data sources. 6 Although the GBD has integrated a large amount of raw data, the lack of more reliable cause-specific death data in some remote and impoverished areas may affect the accuracy of GBD estimates. In addition, the GBD does not provide site-specific data in China, and the distribution of NPC in China also varies greatly, so it is not possible to study the disease burden of NPC in China by province and region. Finally, this is an ecological study, and there are inevitably ecological fallacies, which means that conclusions drawn from groups may not apply to individuals.
Conclusion
In the past 30 years, the number of incidence cases, prevalence cases, and YLD in China has accounted for a large increase in the proportion of the world, and with the advancement of diagnosis and treatment methods, the proportion of the number of deaths, DALYs, and YLLs has decreased. In the past 30 years, the total growth rate of ASIR, ASPR, and age-standardized YLD rates in China has been approximately twice that of the world, showing a trend of increasing year by year, and may continue to increase in the future. In all periods, the risk of incidence, prevalence, and death in males was much higher than that in females. The incidence of young and middle-aged people in China has been increasing in the past 30 years, and the incidence is getting younger. We should pay more attention to and control modifiable risk factors, such as smoking, drinking, and so on. In summary, the disease burden of NPC in China is still heavy, so we should continue to pay attention to and strengthen the control of risk factors and the strategy of early diagnosis and treatment.
Supplemental Material
sj-docx-1-ohn-10.1177_19160216251375033 – Supplemental material for The Burden of Nasopharyngeal Carcinoma in 2019 and the Trend of Change From 1990 to 2019 in China
Supplemental material, sj-docx-1-ohn-10.1177_19160216251375033 for The Burden of Nasopharyngeal Carcinoma in 2019 and the Trend of Change From 1990 to 2019 in China by Kai Xu, Jianhua Chen, Huan Liu, Xiaoyu Lu, Mengya Liu and Xiujun Qin in Journal of Otolaryngology - Head & Neck Surgery
Footnotes
Acknowledgements
Not applicable.
Author Contributions
X.Q. and K.X. conceived and designed this project. K.X. and J.C. analyzed the data and drafted the manuscript. H.L., M.L., and X.L. critically revised the manuscript. All authors interpreted data and wrote the report.
Data Availability Statement
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Xiujun Qin was supported by the Natural Science Foundation of Shanxi Province (202203021211005), and Jianhua Chen was supported by the Youth Independent Project of the China Institute for Radiation Protection (YQ23000208).
Ethical Considerations and Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Supplemental Material
Additional supporting information is available in the online version of the article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.


