Abstract
Important
Trimming perforation margins is the basic procedure for any myringoplasties; however, to date, little literature has been reported on the effect of no trimming perforation margins on sandwich graft tympanoplasty.
Objective
The objective of this study was to compare the graft success rate, hearing improvement, and complications of endoscopic cartilage-perichondrium Sandwich technique (CPST) and cartilage-perichondrium underlay technique (CPUT) for repairing chronic large perforations.
Study Design
Prospective randomized controlled trial.
Setting
Tertiary referral center.
Participants and Intervention
One hundred two patients with chronic large perforations with 50% to 75% of tympanic membrane (TM) were recruited and randomly allocated to CPST (n = 51) and CPUT (n = 51), raising tympanomeatal flap and trimming perforation margins were not performed in both techniques.
Main Outcome Measurers
The graft success rate, air-bone gap (ABG) gain, operation time, and postoperative complications were evaluated at 12 months.
Results
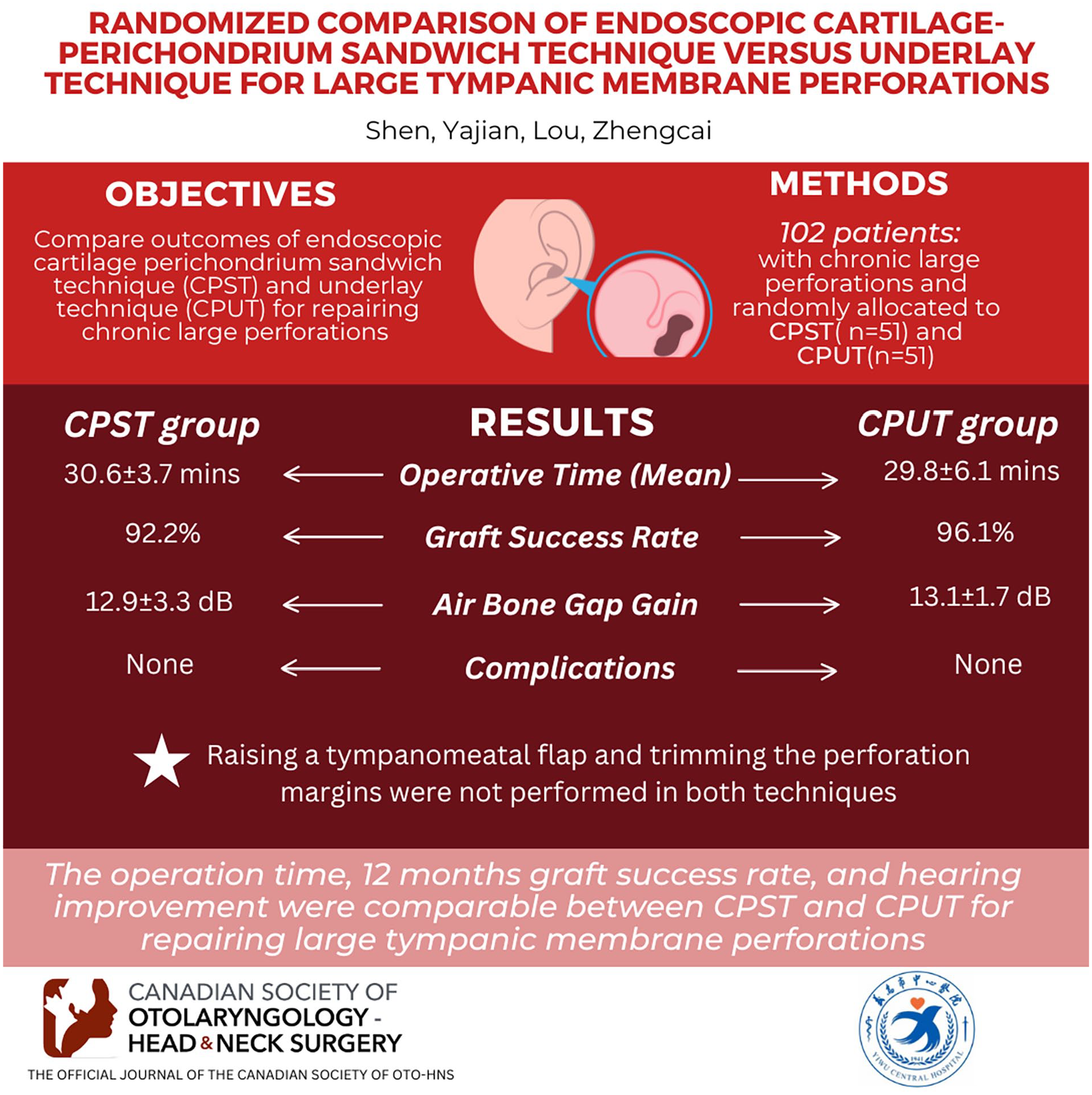
All the patients complete 12 months follow-up. The mean operation time was 30.6 ± 3.7 minutes in the CPST group and 29.8 ± 6.1 minutes in the CPUT group (P = .751).The graft success rate was 92.2% in the CPST group and 96.1% in the CPUT group (P = .979). Endoscopic examination revealed the perichondrial flap gradually became scab in the CPST group, 70.6% patients had the absence of typical cone-shaped TM. However, no scab was seen on the surface of graft, and all the patients had cone-shaped TM in the CPUT group. The ABG gain wasn’t significantly different (12.9 ± 3.3 dB vs 13.1 ± 1.7 dB, P = .689).The successful surgery was 94.1% in the CPST group and 96.1% in the CPUT group, the difference wasn’t significant among the 2 groups (P = .932). In addition, no procedure-related complications and no graft cholesteatoma were found in both groups during the follow-up period.
Conclusions and Relevance
The operation time, 12 months graft success rate, hearing improvement were comparable between CPST and CPUT for repairing large perforation, although raising tympanomeatal flap and trimming the perforation margins were not performed in both techniques.
Keywords
Introduction
Conventional under-overlay technique requires removal of epithelium layer and raising tympanomeatal flap for repairing large perforations of tympanic membrane (TM), which results in long operation and healing time, damage of chorda tympani nerve, and the risk of external auditory canal cholesteatoma.1,2 In 1989 years, Farrior first, introduced Sandwich graft tympanoplasty with trimming perforation margins to repair subtotal perforations. 3 In this technique, temporalis fascia was placed both medial and lateral to the fibrous TM remnant. 3 Recently, we created a under-overlay technique without raising tympanomeatal flap and no removal of epithelium to repair large perforation and obtain high graft success rate and no middle ear cholesteatoma.4-6 Although a few graft cholesteatomas occurred, it was also found in the underlay technique or conventional under-overlay technique.7,8 In addition, trimming perforation margins is the basic procedure for any myringoplasties; however, the necessity and amount of trimming performation tissues remains controversy.9-11 Overmuch trimming perforation margins would increase the perforation size and the possibility of graft failure. Nevertheless, recent clinical controlled trials showed that no trimming perforation margins did not affect the graft success rate of medium sized perforations for underlay technique.12,13 This graft outcomes were similar to previous techniques reported by other scholars, which the perforation margins were trimmed.4,9,10,14-16 However, to date, little literature has been reported on the effect of no trimming perforation margins on sandwich graft tympanoplasty.
The objective of this study was to compare the graft success rate, hearing improvement and complications of endoscopic cartilage-perichondrium Sandwich technique (CPST) and cartilage-perichondrium underlay technique (CPUT) for repairing large perforations.
Subjects and Methods
Ethical Considerations
Ethical approval for the performance of the present study was obtained from the Medical Ethical Committee of the Yiwu Central Hospital. Informed consent was obtained from all of the participants.
Patient Selection
Study subjects were recruited from consecutive patients diagnosed with chronic large perforation with 50% to 75% of TM who visited the Department of Otorhinolaryngology, Head and Neck Surgery. Cases that met the following criteria were analyzed: adult large perforation with 50% to 75% of TM, a dry ear at least 3 months prior to surgery, and air-bone gas (ABG) less than 40 dB. Exclusion criteria were revision cases, cholesteatoma, ossicular chain abnormity, middle ear acute inflammation, fungal otitis externa, and patients with other underlying diseases. Age, gender, perforation duration, myringosclerosis, and presence of diabetes were recorded at first visit. Computed tomography (CT) was performed prior to surgery.
Pure-tone averages (PTAs) were calculated for both air conduction (AC) and bone conduction (BC) by averaging the thresholds at 500, 1000, 2000, and 3000 Hz. In most cases, a threshold of 4000 Hz was used to interpolate the threshold of 3000 Hz per the standards of the Hearing Committee of the American Academy of Otolaryngology-Head and Neck Surgery. Pre- and postoperative air-bone gap (ABG) was calculated by subtracting the AC PTA from the BC PTA. ABG closure was calculated as preoperative ABG minus postoperative ABG.
Randomization and Blinding
All the patients underwent endoscopic cartilage-perichondrium myringoplasty without raising tympanomeatal flap and trimming perforation margins. The graft technique allocation was performed by the principal investigator, with the aid of a registered operating room nurse, using simple random sampling. Specifically, consecutive subjects who met the inclusion criteria and signed the consent form assigned random numbers generated by the SPSS for Windows software package (ver. 19.0; SPSS, Inc, Chicago, IL, USA) that allocated them to 1 of the 2 groups: endoscopic CPST group or CPUT group. The perichondrial flap was placed lateral to the epithelium of TM remnant in the CPST group, while the perichondrial flap was placed medial to the TM remnant in the CPUT group. The patients and assessor were blinded to the treatment arm.
Surgical Approach
All the patients underwent endoscopic cartilage-perichondrium myringoplasty without raising tympanomeatal flap under general anesthesia. The epithelium was removed from the distal malleus handle, but the perforation margins were not de-epithelialized in both groups. Any myringosclerotic plaques and epithelium of the TM remnant were preserved. The cartilage composite graft with one side perichondrium was harvested from the ipsilateral tragus; the perichondrium was circumferentially elevated with the pedicle attached to the cartilage. The full thickness cartilage graft was not thinned but trimmed larger than perforation margins and partially removed to accommodate the malleus handle if any, while the perichondrial flap was trimmed circumferentially so that it was larger than the cartilage graft. The graft was supported medially and laterally by Biodegradable NasoPore in both groups.
Cartilage-Perichondrium Sandwich Technique
The cartilage graft was placed transperforation medial to the TM remnant and annulus, but the perichondrial flap was placed lateral to the epithelial layer of the TM remnant (Figures 1 and 2).4-6

Schematic drawings. CPST group: (A) graft harvesting. (B) Graft shaping. (C) Graft placement, cartilage medial to but the perichondrium lateral to TM remnant. CPUT group: (A) graft harvesting. (B) Graft shaping. (D) Graft placement, cartilage graft and perichondrium graft medial to TM remnant. Yellow: cartilage. Orange-yellow: perichondrium. CPST, cartilage-perichondrium Sandwich technique; CPUT, cartilage-perichondrium underlay technique; TM, tympanic membrane.

Surgical procedures of 2 techniques. (A) Preoperative perforations; (B) middle ear packing; (C) graft placement; (D) graft localization.
Cartilage-Perichondrium Underlay Technique
The cartilage graft was placed trans-perforation medial to the TM remnant and annulus, the perichondrial flap was also placed medial to the remnant TM but lateral to the cartilage gaft and the malleus handle (Figures 1 and 2).
Postoperative Follow-Up and Outcome Measures
The patients were discharged on the day after surgery and follow-ups were scheduled at postoperative 2 and 4 weeks and 2, 3 and 12 months. Endoscope was performed at each follow-up. Audiometric evaluations were performed 12 months after surgery. The operation time was defined as from anesthesia success to complete placement of graft. Any intraoperative or postoperative complications were recorded. Graft success was defined as an intact graft without retraction, lateralization, significant blunting, or medialization, and successful surgery was defined as a postoperative ABG ≤20 dB. The assessors were blinded to the treatment arm.
Statistical Analyses
Statistical analyses were performed with the aid of SPSS ver. 21 (SPSS, Inc, IBM, Chicago, IL, USA). Data are expressed as means (with standard deviations) or percentages (%). The chi-squared test was used to compare categorical data. The Wilcoxon and Mann–Whitney U-tests were employed to compare nonparametric variables, and the independent and paired samples t-tests were used to compare parametric variables. A P-value <.05 was considered to indicate statistical significance.
Results
Demographic Characteristics of Patients
A total of 102 patients were included in the study (Figure 3), comprising 51 and 51 patients in the CPST and CPUT groups, respectively. All the patients complete 12 months follow-up. The demographic and preoperative data among 2 groups showed in the Table 1. The sex, age, side, perforation duration, myringosclerosis, and presence of diabetes were matched among 2 groups (Table 1). The mean operation time was 30.6 ± 3.7 minutes in the CPST group and 29.8 ± 6.1 minutes in the CPUT group, the difference was not significant (P = .751).

Enrollment, randomization, and follow-up of study participants.
Demographic Characteristic of Patients.

Abbreviations: CPST, cartilage-perichondrium Sandwich technique; CPUT, cartilage-perichondrium underlay technique; F, female; L, left; M, male; R, right.
Chi-square test.
Independent samples t-test.
Graft Success Rates
Endoscopic examination revealed the perichondrial flap gradually became necrosis and scab at postoperative 2 to 3 months in most of cases in the CPST group, 36 patients (70.6%) showed the mild bulge of the cartilage graft and the absence of typical cone-shaped TM. However, no scab was seen on the surface of graft and all the patients showed normal cone-shaped TM in the CPUT group.
At postoperative 12 months, residual perforation was observed in 5 (9.8%) cases in the CPST group, while only 2 (3.9%) in the CPUT group, the difference was not significant (P = .433). Nevertheless, residual perforation was spontaneously closed in 1 patient in the CPST group at postoperative 12 months (Figure 4). Thus, the graft success rate was 92.2% (47/51) in the CPST group and 96.1% (49/51) in the CPUT group, the difference was not significant (P = .979).

CPST group: (A) postoperative; (B) post 2 weeks; (C) post 4 weeks; (D) post 12 months. CPST, cartilage-perichondrium Sandwich technique.
Hearing Gain
The postoperative ABG showed significant improvement compared to preoperation (Table 2). In the CPST group, of the 51 patients, postoperative ABG was less than 10 dB in 13 (25.5%), 11 to 20 dB in 35 (68.6%), and more than 20 dB in 3 (5.9%). However, in the CPUT group, of the 51 patients, postoperative ABG was less than 10 dB in 17 (33.3%), 11 to 20 dB in 32 (62.7%), and 21 to 30 dB in 2 (3.9%) patient. The successful surgery was 94.1% in the CPST group and 96.1% in the CPUT group, the difference wasn’t significant among the 2 groups (P = .932).
Comparison of Hearing Gains, the Air-Bone Gap, and Bone Conduction.

Abbreviations: BC: bone conduction; CPST, cartilage-perichondrium Sandwich technique; CPUT, cartilage-perichondrium underlay technique; dB, decibel; PTA, pure-tone average; SD, standard deviation.
Paired samples test: Comparison between the same groups in regard to Air-bone gap or BC, pre- and postoperatively.
Mann–Whitney U test: Comparison between 2 groups in terms of gain, pre- or postoperatively.
P < .01.
When reported in accordance with the AAO-HNS guidelines, the preoperative ABG was 28.3 ± 2.6 dB in the CPST group and 27.9 ± 5.8 dB in the CPTU group (P = .741). Postoperatively, the ABG significantly improved to 16.8 ± 3.1 dB (P<.001) in the CPST group and 15.7 ± 7.6 dB (P<.001) in the CPTU group. However, the change in ABG wasn’t significantly different among the 2 groups (12.9 ± 3.3 vs 13.1 ± 1.7 dB, P = .689).
Postoperative Complications
No graft medialization, lateralization, or significant blunting was seen in any of the group. In addition, no procedure-related complications and no graft cholesteatoma were found in both groups during the follow-up period.
Discussion
Although the graft technique has not obviously changed, the surgical procedures are constantly improved for repairing chronic perforations, including no raising tympanomeatal flap,17,18 the graft placing lateral to the epithelial layer,4-6 and no trimming perforation margins,12,13,18 which significantly shortened the operation time. This study first compared the graft outcomes and TM morphology of endoscopic CPST and CPUT for repairing large perforations. In this study, the graft material (cartilage-perichondrium composite graft) and no trimming perforation edges are the same in both groups. The only difference is that the perichondrial flap was placed lateral to the epithelial layer of the remnant TM in the CPST group but medial to the remnant TM in the CPUT group. Theoretically, the mean operation time was similar in both techniques, which had been confirmed by the present study. Also, there was no significant difference in the graft success rate at postoperative 12 months between the 2 techniques (92.2% vs 96.1%). The graft success rate in this study was comparable to the techniques with trimming the perforation edges reported by recent some authors.14-16,19-22 Takahashi et al 14 reported the success rate of 98.0% using interlay technique. Bedri et al 19 reported the graft success rate of 90% using double-layer graft technique, and other scholars reported that the graft success rate was 95.1% using lateral underlay technique, 20 94.4% using L-shaped cartilage technique, 15 and 95.1% using circumferential subannular technique. 21
Why were the perforation margins not de-epithelialized in both groups? In our early study of cartilage graft underlay technique, we found that no de-epithelialized perforation margins did not affect the graft success and hearing gain following myringoplasty compared with de-epithelialized perforation margins.12,13,18 Therefore, we speculated that the perforation margins did not affect inosculation of the graft and the TM remnant and neovascularization of the graft. Additionally, the cartilage graft was placed medial to the TM remnant in both groups in this study; the only difference was that the perichondrial flap was placed lateral to the TM remnant in the CPST group but medial to the remnant TM in the CPUT group. Essentially, only the cartilage graft can achieve the inosculation with the TM remnant in the CPST group, the perichondrial flap mainly plays a pulling role in the cartilage graft in early postoperative phase but gradually forms the crust over time.4-6 Thus, the perforation margins were not de-epithelialized in both groups.
Although the graft success rate was not significantly different among 2 techniques in present study, CPST group had high residual perforation compared with the CPUT group (9.8% vs 3.9%). Endoscopic follow-up found the perichondrial flap gradually became necrosis and scab at postoperative 2 to 3 months in the CPST group, only the cartilage graft actually closed the perforations. Thus, it may result in the residual perforation because of movement and insufficient size of the cartilage graft. On the contrary, the perichondrium and cartilage grafts play a role of double insurance in the CPUT technique, and the perichondrial flap can reinforce the cartilage graft, thereby constituted actual double graft.
In addition, the gap between graft and remnant TM or annulus was filled with excessive perichondrial flap and thereby insured the close contact between the graft and remnant TM in the CPUT technique. Some scholars suggested that any residual gap between graft and perforation edge was filled with free perichondrial grafts (“tuck grafts”), creating a continuous surface between the graft and tympanic remnant.23,24 The perichondrial flap could reach the intimate contact with the remnant TM even if the cartilage graft was insufficient or moved. In addition, the crust formation affected the postoperative observation of graft in the CPST group, and the cartilage graft movement could not be early found and corrected during follow-up. On the contrary, the graft movement or extrusion could be early corrected in the CPUT group. Therefore, theoretically, CPUT technique is superior to the CPST technique.
Theoretically, the development of middle ear cholesteatoma is almost impossible for both 2 techniques, the underlay cartilage graft prevented the inward growth of epithelium of perforation margin and remnant TM in 2 techniques. 25 However, unfortunately, the follow-up time was short and only 12 months, and postoperative CT or magnetic resonance was not performed in this study. In addition, no graft cholesteatoma was seen in any group in this study. Although our previous study reported the graft cholesteatoma,4,5 graft cholesteatomas seem to be irrelevant to trimming the epithelial layer and perforation margins.7,8
Surprisingly, 70.6% patients showed the mild bulge of the cartilage graft and the absence of cone-shaped TM in the CPST group. However, no scab was seen on the surface of graft and all the patients showed normal cone-shaped TM in the CPUT group. The mild bulge of the cartilage graft may be related to the traction of lateral perichondrial flap in the early period of postoperation. The conical shape of TM may play a role in high frequency sound conduction, the cone-shaped eardrum allows it to have a larger area for the same canal size, which increases sound transmission to the cochlea.26,27 Nevertheless, no significant difference was observed among 2 groups for the ABG gain or successful surgery in this study, it could be related to older age, large perforation and longer perforation duration, thereby resulting in no improvement of postoperative high-frequency hearing. Recent study also found that low-frequency ABG improved but high-frequency conductive hearing loss persists after tympanoplasty for large perforation. 28
The study advantages include no patient was lost to follow-up from either group, thus supporting the results; this is a prospective, randomized controlled trial. However, our study had several limitations: a small sample size, enrollment of all patients from a single institution, a short follow-up time of 12 months, the absence of postoperative CT or magnetic resonance, and the absence of long-term follow-up data. Thus, this study needs more numbers and longer follow-up.
Conclusion
The operation time, 12 months graft success rate, hearing improvement were comparable between CPST and CPUT for repairing large perforation, although raising tympanomeatal flap and trimming the perforation margins were not performed in both techniques.
Footnotes
Author’s Contributions
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by Technology Agency of Jinhua City, China (Grants#2022-3-042) and Technology Agency of Yiwu City, China (Grants#23-3-80).
