Abstract
Background
Suicide risk in Parkinson's disease (PD) remains understudied, with limited exploration of the impact of neuropsychiatric comorbidities and commonly prescribed PD and psychiatric medications.
Objective
To investigate the prevalence and correlates of suicide risk in PD.
Methods
This study comprised 129 people with PD (PwP) undergoing screening for clinical trial participation at a movement disorders clinic. Suicide risk and psychiatric diagnoses were assessed with the Mini International Neuropsychiatric Interview (MINI). The Parkinson Anxiety Scale (PAS) and the Beck Depression Inventory-II (BDI-II) were also administered. Logistic regression models were used to identify correlates of suicide risk.
Results
Suicide risk was present in 22.5% of the sample, with 3.9% reporting a lifetime suicide attempt. No associations were found between suicide risk and demographic or PD-related variables. Suicide risk was independently associated with higher PAS score (odds ratio (OR) = 1.17; 95% confidence interval (CI): 1.07–1.29; p = 0.001), higher BDI-II suicidal ideation item score (OR = 32.43; 95% CI: 7.78–135.12; p < 0.001), and benzodiazepine use (OR = 13.88; 95% CI: 2.77–69.57; p = 0.001). Furthermore, the BDI-II suicidal ideation item missed nearly 45% of at-risk individuals identified by the MINI, with only 16 scoring above 0.
Conclusions
Despite no documented suicide risk in participants’ medical charts or neurologists’ referrals, over one-fifth were found to be at risk. Correlates of suicide risk in PD warrant further investigation. This study highlights the importance of screening PwP for suicidality during routine care, and that a one-item screen might not adequately capture at-risk individuals.
ClinicalTrials.gov Identifier
NCT03968133
Plain language summary
Parkinson's disease (PD) is known for its motor symptoms, such as tremor, stiffness, and slowed movement. It can also affect mood, thinking, and gut health. These challenges can take a heavy toll on quality of life. Researchers have found that people with PD are more likely to have suicidal thoughts or behaviors, but the reasons for this are not well understood. In our study, we wanted to learn how common suicidal thoughts and behaviors are among people with PD, and what factors might increase their risk.
To do this, we collected data from 129 people with PD seen at a movement disorders clinic in Canada. Each participant took part in an in-depth interview about suicidal thoughts, past suicide attempts, and mental health conditions. They also completed questionnaires measuring anxiety and depression levels, and we reviewed their medical history and medication use. We then analyzed the data to see which factors were most related to suicide risk.
We found that about one in five participants were at risk of suicide, even though this was not recorded in their medical charts. Higher anxiety levels and the use of medications called benzodiazepines (a type of drugs that helps reduce anxiety symptoms) were linked to increased suicide risk.
Our results suggest that suicide risk in PD may often go unnoticed in regular medical care. Healthcare providers should actively ask people with PD about their mood, anxiety, and any thoughts of suicide during routine visits. When possible, input from family members or caregivers can also help identify signs of distress that might otherwise be missed or go unreported. Future research should continue to explore the role of anxiety and identify additional factors that may increase suicide risk in people with PD.
Introduction
Parkinson's disease (PD) is the second most prevalent neurodegenerative disorder worldwide and remains without a cure. 1 Beyond the cardinal motor features, PD involves a myriad of non-motor symptoms, including neuropsychiatric symptoms such as anxiety and depression, which diminish quality of life and contribute substantially to overall disability. 2 Psychiatric comorbidities, combined with physical disability and shared predisposing demographic characteristics, including male sex and advancing age, represent key factors that may place people with PD (PwP) at an elevated risk of suicidal ideation and behavior,3,4 broadly referred to as “suicidality”.
Suicidal ideation is defined as having thoughts about ending one's own life, which may be passive in the absence of a clear plan, or active in its presence. 5 Suicidal behavior includes suicide attempts and death by suicide. 5 While primary psychiatric disorders such as depression or schizophrenia are associated with high rates of suicidal thoughts and death by suicide, suicidal ideation and behaviors are also prevalent and a significant concern in other medical conditions. A recent meta-analysis identified a 22.2% prevalence of suicidal ideation and 1.25% prevalence of suicidal behavior across 14 and 21 studies in PwP, respectively, representing a two-fold increased risk of suicidal behavior relative to controls without PD. 6 These rates, however, are likely underestimates, as suicidality in PwP can be difficult to detect due to barriers to disclosure such as stigma and cultural factors,6–8 the current lack of validated screening tools, 3 and the under-recognition of neuropsychiatric manifestations in this population.9–11
Correlates of suicidality in PwP also remain understudied. 3 Among existing studies, suicidal ideation in PwP appears to be more strongly associated with neuropsychiatric than motor symptoms,12–17 with major depressive disorder emerging as a consistent correlate of suicidal ideation.12–17 In contrast, associations between major depressive disorder in PwP and completed suicide have not been consistently observed,18,19 whereas both high doses of and withdrawal from dopaminergic medications have been linked to death by suicide.3,18 Preliminary evidence suggests a potential link between anxiety and suicidal ideation in PD,13,14,20 although no studies have systematically investigated this link. Furthermore, the relationship between suicidality and the use of commonly prescribed non-dopaminergic medications in PwP represents another understudied area with salient clinical practice implications.
The present study aimed to examine the prevalence and correlates of current suicide risk in PwP, considering both present suicidal ideation and past attempts. We included clinical variables which have received limited attention in the literature to date, including anxiety disorders, as well as the use of antidepressant and anxiolytic medications. A better understanding of the characteristics of PwP at risk of suicide may help to refine screening procedures and guide management strategies.
Methods
This study is a secondary analysis of data collected during the screening process for a clinical trial investigating the effects of a multi-strain probiotic on anxiety in PwP. The trial was approved by the University of British Columbia Clinical Research Ethics Board (Protocol #H18-03083) and registered on ClinicalTrials.gov (NCT03968133). It was conducted at the tertiary Movement Disorders Clinic at the University of British Columbia, Canada, with recruitment occurring between December 2020 and February 2023. Potential participants were pre-screened based on the trial's eligibility criteria (Supplemental Table 1) through a review of recent consult notes in their medical charts and phone discussions. All participants provided electronic informed consent through the Research Electronic Data Capture (REDCap) system prior to undergoing any screening procedures.
Clinical assessments
A total of 143 individuals were consented, including 77 who were recommended for participation by their neurologist during weekly multidisciplinary clinical research rounds. The present report draws on data obtained from recruited PwP who completed a remote psychiatric examination during trial screening regardless of ultimate trial eligibility, thus including those both with and without clinical anxiety and other psychiatric comorbidities. All participants were maintained on stable doses of antidepressant or anxiolytic medications for a minimum of 4 weeks, and on stable doses of PD medications for a minimum of 2 weeks, prior to the screening examination. All participants demonstrated the cognitive capacity to understand and respond appropriately to examination questions. As active suicidality was an exclusion criterion for the trial, assessments for suicidality represented a key component of the screening process. Notably, individuals involved in the screening process were not suspected to have active suicidal ideation or depressive disorder based on chart review or verbal comments from their neurologist.
Demographic and clinical characteristics of those with a diagnosis of PD according to the UK Brain Bank Criteria, 21 confirmed by a movement disorders specialist, were obtained by self-report and verified by chart review. Disease duration was defined as the time since onset of first motor symptoms. The levodopa equivalent daily dose was calculated using commonly accepted conversion factors. 22 Remote psychiatric assessments, consisting of the Mini International Neuropsychiatric Interview (MINI), the Parkinson Anxiety Scale (PAS), and the Beck Depression Inventory-II (BDI-II), were performed in participants’ ON medication state. The MINI, version 6.0.0, is a short structured diagnostic interview for more than 15 common psychiatric disorders and disorder subtypes based on the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, and International Classification of Diseases, Tenth Revision criteria. 23 The suicidality module of the MINI assesses current suicide risk through dichotomous (yes/no) items on suicidal ideation, suicide plan and attempt within the past month, as well as lifetime suicide attempts. Scores for ten of 11 items are weighted according to their estimated contribution to risk level, and the sum score is used to classify suicide risk into low (1–8 points), moderate (9–16 points), and high risk (≥ 17 points). The module, often considered as the reference standard in validation studies of suicide assessment measures, has long been recognized for its practicality in assessing suicide risk in neurological conditions.24,25 The MINI was administered by one of three physicians (DM, FP, NJA) and used to assess the presence of psychiatric disorders and suicide risk.
The BDI-II is a widely used measure for assessing severity of depression in PD. 26 It is a 21-item self-report questionnaire that asks participants to reflect on their depressive symptoms over the past two weeks. Each item is rated on a 4-point Likert scale ranging from 0 to 3 and the total score ranges from 0 to 63. A higher score is indicative of more severe depressive symptoms. Item 9 of the BDI-II assesses one's suicidal thoughts or wishes and is rated as follows: 0 = I don't have any thoughts of killing myself; 1 = I have thoughts of killing myself, but I would not carry them out; 2 = I would like to kill myself; 3 = I would kill myself if I had the chance. A score ≥ 1 indicates the presence of suicidal ideation. One large study with more than 5300 psychiatric patients showed that this item is associated with both the risk of repeat suicide attempts and death by suicide, and can be used as a brief screening tool for suicide risk in clinical practice. 27 In this study, we considered both the BDI-II total score with item 9 removed (hereafter referred to as “adjusted BDI-II”) and the individual score for item 9 as separate covariates when assessing factors associated with suicide risk.
The 12-item self-rated version of the PAS was developed to assess the severity of anxiety symptoms in PwP. 28 It has three subscales that assess persistent anxiety, episodic anxiety, and avoidance behavior over a four-week period. Items are scored on a 5-point Likert scale, with 0 meaning “not or never” and 4 meaning “severe or nearly always”. The maximum total score is 48.
Suicide risk management protocol
A suicide risk management protocol was implemented as part of the trial procedures to ensure participant safety. The protocol was triggered in the following circumstances: (1) if a potential participant disclosed active suicidal ideation with a plan to carry it out during the pre-screening call; (2) if a participant endorsed a score of 2 or 3 on BDI-II item 9; or (3) if any degree of suicide risk was identified according to the MINI. In all such cases, irrespective of study eligibility, individuals were instructed to contact emergency services or visit the emergency department immediately if they felt at imminent risk of harming themselves or others. They were also provided with 24-h crisis hotline numbers and additional mental health resources. The principal investigator (SAC) was promptly notified of all identified cases for further clinical assessment, appropriate follow-up, and documentation in accordance with regulations and study procedures.
Statistical analysis
All statistical analyses, except for mediation analysis, were conducted using SPSS version 28.0. Normality of continuous data was assessed using the Shapiro-Wilk test. Demographic and clinical characteristics were compared between PwP with and without suicide risk using Fisher's exact test for categorical variables and Mann-Whitney U test for continuous variables. Cohen's kappa was calculated to assess the level of agreement between suicide risk as identified by the MINI suicidality module and the suicidal ideation item of the BDI-II (item 9).
Logistic regression analysis was used to assess the association between demographic and clinical characteristics (independent variables) and the presence of suicide risk (dependent variable, defined as ≥ 1 point on the MINI suicidality module). Univariable logistic regression was first used to calculate the odds ratio (OR) and 95% confidence interval (CI) for each independent variable. Variables with p < 0.10 in univariable analysis were entered into the multivariable logistic regression model, and backward stepwise selection was performed. Variance inflation factor (cut-off < 5) and tolerance (cut-off > 0.20) were used to check for multicollinearity. 29 The goodness of fit of the model was assessed using the Hosmer-Lemeshow test (p > 0.05 indicating a good fit) and the Nagelkerke R2 index. Statistical significance was set at p < 0.05 (2-tailed). Mediation analysis was performed using the R package regmedint (v1.0.1). 30
Results
A total of 129 PwP (88 males; 68.2%) completed the screening procedures and were included in this study. Based on the MINI suicidality module, 1 participant (0.8%) was at moderate risk of suicide, 28 (21.7%) were at low risk, and 100 (77.5%) were not at risk as indicated by a score of 0. We thus combined low and moderate risk groups into a single “at-risk” group for subsequent analyses. No deaths, hospitalizations, emergency room visits, or injuries attributable to suicidality were identified or reported during the study period. Among these 29 at-risk PwP, 16 (55.2%) had anxiety, depression, or other mood-related concerns documented in their most recent medical charts prior to study participation.
Demographics and clinical characteristics
Table 1 presents the demographic and clinical characteristics of participants with and without suicide risk. No significant differences between the two groups were observed in age, sex, or race/ethnicity. Both groups also had comparable PD-related characteristics, including disease duration, levodopa equivalent daily dose, initial extremity and side of motor symptom onset, and use of various antiparkinsonian medications.
Demographic and clinical characteristics of PwP with and without suicide risk.
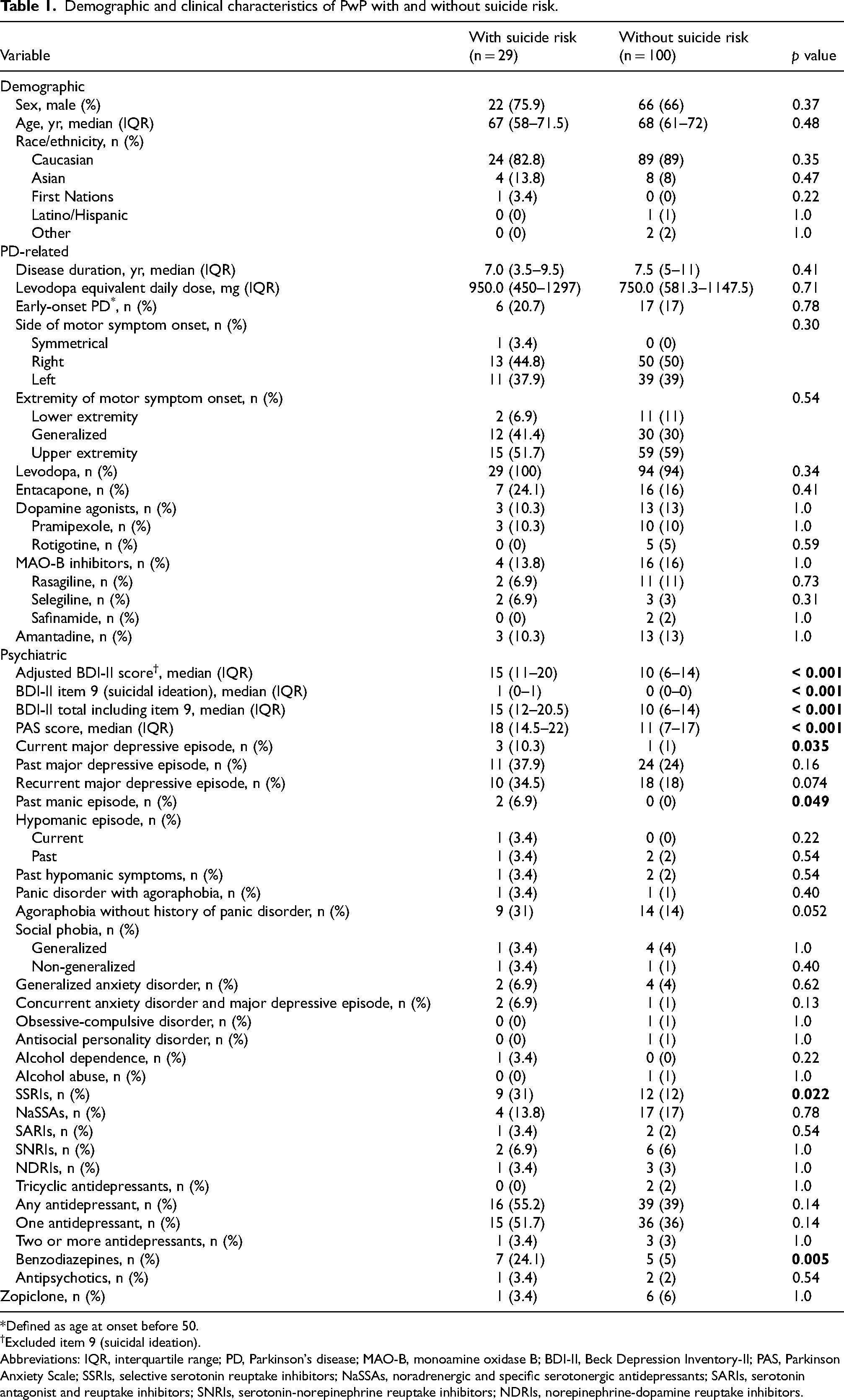
Defined as age at onset before 50.
Excluded item 9 (suicidal ideation).
Abbreviations: IQR, interquartile range; PD, Parkinson's disease; MAO-B, monoamine oxidase B; BDI-II, Beck Depression Inventory-II; PAS, Parkinson Anxiety Scale; SSRIs, selective serotonin reuptake inhibitors; NaSSAs, noradrenergic and specific serotonergic antidepressants; SARIs, serotonin antagonist and reuptake inhibitors; SNRIs, serotonin-norepinephrine reuptake inhibitors; NDRIs, norepinephrine-dopamine reuptake inhibitors.
Among the various psychiatric disorders, a current major depressive episode (p = 0.035) and a past manic episode (p = 0.049) were reported significantly more often by participants with versus those without suicide risk. At-risk participants also scored significantly higher on the PAS and on both unadjusted and adjusted BDI-II (all p < 0.001). With regard to medication regimens, significantly higher rates of selective serotonin reuptake inhibitor (SSRI) (p = 0.022) and benzodiazepine (p = 0.005) use were observed among participants at risk of suicide. No significant differences were detected in usage rates for other antidepressant classes, antipsychotics, or zopiclone (Table 1).
MINI suicidality module items
Table 2 shows the frequency of responses for individual MINI suicidality module items among those at risk of suicide. More than half of the 29 at-risk participants (15; 51.7%) thought about suicide within the past month of assessment: 14 occasionally and 1 often, with 12 of mild intensity and 3 of moderate intensity. Fourteen (48.3%) participants expressed feelings of hopelessness, and 7 (24.1%) thought they would be better off dead or wished they were dead. None reported a suicide plan or having taken active steps to hurt themselves within the past month. However, 5 (17.2%) participants reported a previous suicide attempt.
Frequency of responses for individual MINI suicidality module items (n = 29).

B1 (suffer any accident?) and its two sub-questions (B1a and B1b) are not scored and thus not shown here.
% of 29 PwP with suicide risk.
Suicide risk as assessed by MINI suicidality module versus BDI-II item 9
According to BDI-II item 9 (suicidal ideation), 20 PwP reported thoughts of killing themselves but would not carry them out (as indicated by a score of 1), and no participants scored above 1. Of note, the one participant deemed to be at moderate risk based on the MINI scored 1 on this item, indicating no active component to their suicidality. Among participants at risk of suicide according to the MINI, 16 (55.2%) scored 1 on this item (mean ± standard deviation, 0.55 ± 0.51; median [interquartile range], 1 [0–1]), while 4 (4%) participants without suicide risk had a score of 1 (0.04 ± 0.20; 0 [0–0]) (p < 0.001). Cohen's kappa for the level of agreement between suicide risk and BDI-II item 9 was 0.57 (95% CI: 0.40–0.75).
Factors associated with suicide risk
In univariable logistic regression analysis, factors associated with the presence of suicide risk included the following: higher adjusted BDI-II score (OR = 1.12; 95% CI: 1.04–1.20; p = 0.002), higher BDI-II item 9 score (OR = 29.23; 95% CI: 8.46–100.96; p < 0.001), higher PAS score (OR = 1.15; 95% CI: 1.07–1.23, p < 0.001), presence of a major depressive episode (OR = 11.42; 95% CI: 1.14–114.39; p = 0.038), presence of agoraphobia without history of panic disorder (OR = 2.76; 95% CI: 1.05–7.28; p = 0.040), SSRI use (OR = 3.30; 95% CI: 1.22–8.89; p = 0.018), and benzodiazepine use (OR = 6.05; 95% CI: 1.75–20.84; p = 0.004) (Table 3).
Univariable logistic regression analysis for suicide risk.
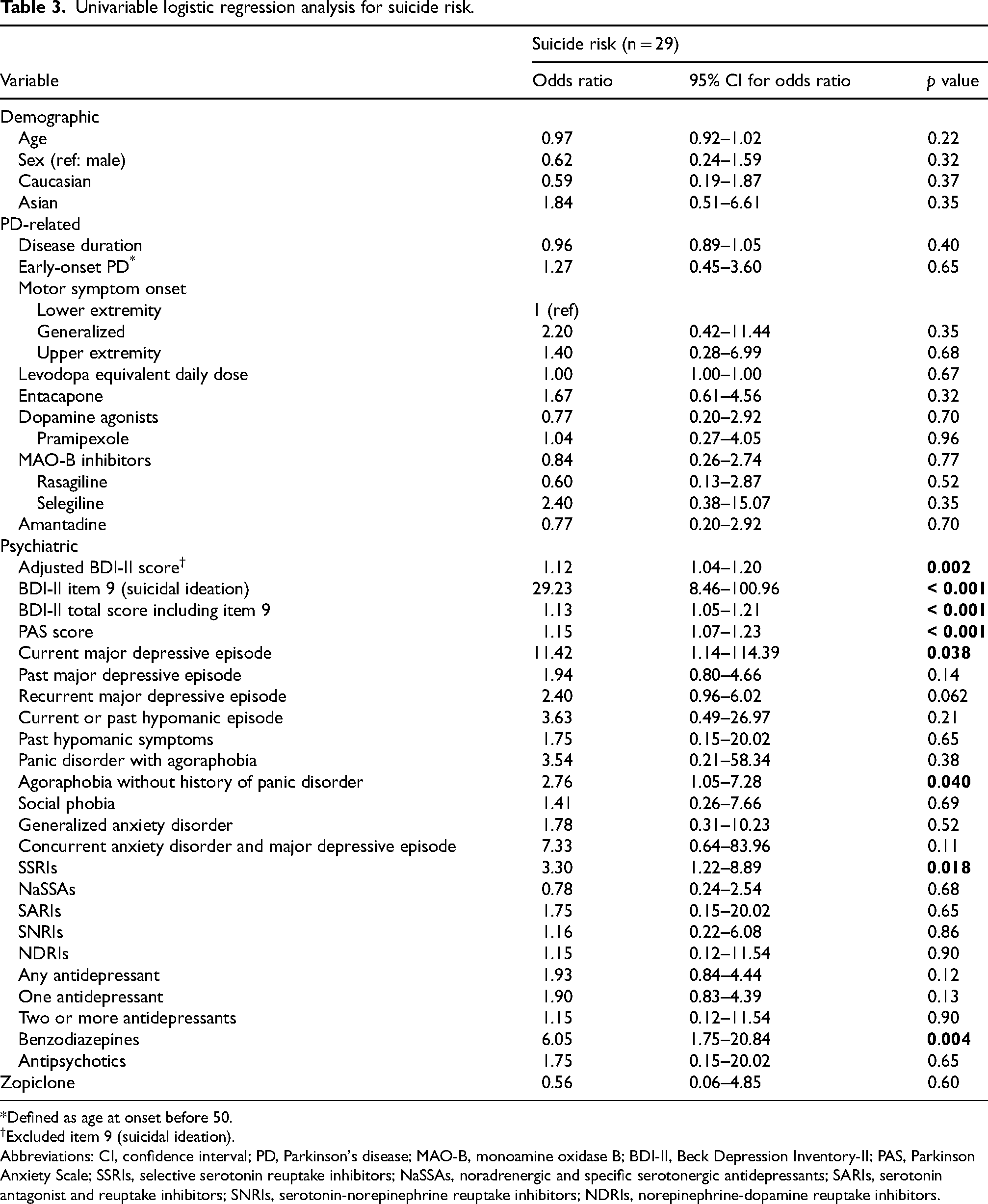
Defined as age at onset before 50.
Excluded item 9 (suicidal ideation).
Abbreviations: CI, confidence interval; PD, Parkinson's disease; MAO-B, monoamine oxidase B; BDI-II, Beck Depression Inventory-II; PAS, Parkinson Anxiety Scale; SSRIs, selective serotonin reuptake inhibitors; NaSSAs, noradrenergic and specific serotonergic antidepressants; SARIs, serotonin antagonist and reuptake inhibitors; SNRIs, serotonin-norepinephrine reuptake inhibitors; NDRIs, norepinephrine-dopamine reuptake inhibitors.
Multivariable logistic regression analysis revealed that higher PAS score (OR = 1.17; 95% CI: 1.07–1.29; p = 0.001), higher BDI-II item 9 score (OR = 32.43; 95% CI: 7.78–135.12; p < 0.001), and benzodiazepine use (OR = 13.88; 95% CI: 2.77–69.57; p = 0.001) were independently associated with suicide risk in this sample of PwP (Table 4). The variance inflation factors and tolerance for all candidate variables were below 2 and above 0.5, respectively, indicating that multicollinearity was not a concern (Supplemental Table 2). The logistic model demonstrated a good fit (Hosmer-Lemeshow test χ2 = 7.02; df = 8; p = 0.53; Nagelkerke R2 = 0.56), with 88.3% of cases being classified correctly.
Multivariable logistic regression analysis for suicide risk.

Abbreviations: CI, confidence interval; BDI-II, Beck Depression Inventory-II; PAS, Parkinson Anxiety Scale.
Given the potentially confounding relationship between anxiety and benzodiazepine use, we additionally performed a post hoc mediation analysis to examine the extent to which benzodiazepine use (mediator) mediated the association between anxiety symptoms (exposure) and suicide risk (outcome). Results show that use of benzodiazepine was not a statistically significant mediator of suicide risk through an indirect path (Supplemental Figure 1). The direct effect of anxiety severity on suicide risk remained significant after controlling for benzodiazepine use (OR = 1.17; 95% CI: 1.08–1.27; p < 0.001).
Discussion
Our report highlights the prevalence and correlates of suicide risk in a sample of 129 PwP undergoing screening for clinical trial participation at a tertiary movement disorders clinic in Vancouver, BC, Canada. Although no participants had recent or present suicide risk documented in medical charts reviewed during pre-screening, 22.5% of participants were identified as having low or moderate suicide risk based on the MINI, with 3.9% of the sample reporting a lifetime suicide attempt. This high prevalence of suicide risk is remarkably consistent with the 22.7% prevalence of suicidal ideation reported in a cohort study by Kostić et al., 14 and the 22.2% prevalence of suicidal ideation in PwP reported in Mai et al.'s recent meta-analysis. 6 Consistent with our observations, the higher prevalence of suicidal ideation detected in prospective compared with retrospective studies included in Mai et al.'s analysis suggests an under-documentation and likely under-detection of suicidality in routine clinical practice. This under-recognition may be attributable to a combined lack of awareness of the relationship between PD and suicidality on the part of clinicians, a low sensitivity of current screening methods, and suboptimal patient selection for screening due to limitations in current understanding of PD-specific correlates of suicidality.
Despite mounting evidence supporting an elevated prevalence of suicidal ideation in PwP, conflicting findings regarding the risks of suicidal behavior in PwP may lead some clinicians to perceive a relatively low risk of suicide among PwP, and thus a lack of need for routine screening.3,6 In our study, as in several others,13,31–33 a high prevalence of suicidality in general did not correspond with a markedly increased lifetime risk of suicidal behavior among PwP, as the 3.9% prevalence of past suicide attempts in our sample fell within the range of that reported for the general Canadian (3.1%) 34 and U.S. (4.6%) 35 adult populations. It has been suggested that suicidal ideation may represent a true depressive phenomenon in PwP, whereas factors such as executive dysfunction, high doses (or withdrawal) of dopaminergic agents, and subthalamic nucleus stimulation may facilitate the transition to suicidal behavior.3,13,36 Thus, the finding that rates of past suicide attempts in our sample were similar to the background population may reflect the fact that individuals with deep brain stimulation or clinically significant dysexecutive features were likely to have been excluded during pre-screening. 13 Regardless of the frequency with which suicidal thoughts manifest in suicidal behavior in PwP, early recognition of suicidal ideation is essential for addressing related quality of life concerns, and preventing the transition to suicidal behavior related to a change in clinical state or treatment regimen.
However, there is a lack of consensus recommendations on when, in whom, and how best to implement suicide risk screening in routine clinical care. Screening rates in primary care are low, reported to be 36–42% even in patients presenting with major depression,37,38 and are likely lower in specialty neurologic care. One study of epilepsy found that only 58% of healthcare providers would screen for suicidality if symptoms were spontaneously reported by patients or their relatives, while 6% never screened at all. 39 In PD, although such screening rates have not been examined, we found that documentation of anxiety, depression, or mood-related concerns was present in only 55% of the 29 at-risk PwP. This finding plausibly suggests that: (1) suicide risk may not be systematically assessed even when neuropsychiatric symptoms are identified, and (2) such symptoms are under-recognized, as previously reported.9,11 The latter may in turn reduce the likelihood of suicide risk screening. Indeed, routine screening for neuropsychiatric symptoms is infrequently undertaken, with only 50% of PwP with anxiety or depression being identified and treated, 10 while 24% are never screened. 40 Numerous challenges may underlie these screening gaps. Logistical and resource constraints such as limited time and lack of support staff are commonly cited.39,40 On the patient side, cultural or religious beliefs, public stigma, and self-stigma surrounding mental health and suicidality can further reduce the suicide risk screening rate.6–8,41 At the provider level, discomfort initiating conversations about suicidality may also contribute, potentially stemming from insufficient training and confidence, fear of causing distress, or uncertainty about how to respond.39,42,43 Evidence supports the value of structured training programs (such as the Recognizing and Responding to Suicide Risk 44 or the Question, Persuade, Refer 45 programs), clear protocols and greater institutional support, 43 along with supervision, guidance from senior colleagues, and peer consultation, 46 in reducing anxiety and improving confidence in suicide risk assessment.
In lieu of comprehensive suicide risk assessment methods such as the MINI suicidality module, in-office suicidality screening often occurs as one component of depression screening, such as with the BDI-II and the self-report Patient Health Questionnaire-9. The predictive validity of the BDI-II suicidal ideation item has been established in large psychiatric samples, with higher scores indicating greater risk. 27 A score ≥ 1 increases the risk of suicide fourfold, while a score ≥ 2 versus ≤ 1 doubles the risk of repeat attempts. In our sample, 15.5% of participants screened positive for suicidal ideation using BDI-II item 9, representing a markedly higher proportion than is seen in the general Canadian population (2.6%). 34 This finding is consistent with suicidal ideation rates of 13.3% and 11.1% reported in Chinese 15 and Brazilian 13 studies using BDI-II item 9 in PwP, respectively, and elevated relative to the finding of a 5.1% suicidal ideation rate using this single-item screen in a Spanish cohort. 16 Importantly, however, the single-item BDI-II screen failed to capture nearly 45% of individuals found to be at risk of suicide using the MINI suicidality module in our sample. Similarly, 3 of 13 patients (23%) assessed as having death or suicidal ideation on the MINI in the Brazilian study screened negative for suicidal ideation using BDI-II item 9. 13 Similar limitations pertaining to the suicidal ideation item of the Patient Health Questionnaire-9 have also been reported in neurological conditions such as multiple sclerosis, stroke, and epilepsy. 47 Collectively, these observations suggest that, despite their convenience and demonstrated predictive capacity, single-item screens such as BDI-II item 9 are insufficient assessment tools for suicidality in higher-risk patients and should not be used as the sole basis for risk determination or as a substitute for clinical judgement. 48
Beyond single-item screens, a range of brief tools is available to support suicide risk assessment. These have been reviewed previously,49–51 including in individuals with neurological conditions.52,53 While none have been validated in the PD population, 3 several widely used instruments may still be feasible for routine PD care, considering the screening challenges outlined above. For example, the clinician-administered Columbia-Suicide Severity Rating Scale (C-SSRS) assesses both the frequency and severity of suicidal ideation and behavior, 54 takes less than five minutes to complete, and is among the most commonly used tools in clinical trials, including those involving PwP. 3 Notably, administration does not require mental health training, and both the tool and training are publicly accessible at no cost. Brief 6-item screener, self-report, and computer-based versions of the C-SSRS are also available, offering flexibility across settings. 55 Furthermore, the Ask Suicide-Screening Questions, validated in both youth and adult medical populations, includes four yes/no items and a fifth acuity item for positive screens. 56 It can be administered in under two minutes by any clinical or nonclinical staff, with non-acute positive screens warranting a brief suicide safety assessment by a trained clinician to determine the need for further evaluation. 57 As well, the self-report or clinician-administered Geriatric Suicide Ideation Scale (GSIS) is a 31-item measure designed for older adults that assesses suicide and death ideation, loss of personal and social worth, and perceived meaning in life. 58 Although longer, the GSIS demonstrates strong psychometric properties and may be particularly relevant in PD, as it is a chronic condition closely tied to aging. Two abbreviated 5- and 10-item versions may represent more practical alternatives. 59 Ultimately, clinics and practitioners must consider their patient population, available resources, and workflow when choosing a screening approach and implementing an appropriate response plan to a positive screen.50,60
Identification of patients at risk of suicide with or without the aid of screening tools requires an awareness of the various potential contributors to risk of suicidal ideation and behavior in PwP. Links between depression and suicidal ideation are well-established, and the lack of association seen in our study likely reflects a floor effect as patients with a current depressive disorder were infrequent and the prevalence of antidepressant treatment was high, potentially treating suicidal ideation in those with a mood disorder or mood symptoms. Moreover, individuals with severe depression would mostly have been excluded in the pre-screening stage of the study. Despite our small sample size, however, we identified significant independent associations between suicide risk and scores on the PAS as well as benzodiazepine use. These observations are consistent with associations between anxiety disorders and suicidal ideation observed in the general population,61–64 as well as three previous studies in PwP.13–15 While major depressive disorder is one of the strongest predictors of suicide ideation, it has not emerged as a reliable predictor of suicidal behavior among those with existing ideation.61,63,64 In contrast, anxiety and impulse-control disorders predict both suicidal ideation and transition to suicide attempts.61–64 Links between benzodiazepine use and suicidality have been established in other cohorts, 65 and add to the rationale for increased caution around the use of benzodiazepines in PwP. 66 However, the use of benzodiazepines might be an expression of more intractable anxiety disorders, especially in a population at risk of cognitive impairment and postural instability. Furthermore, while post hoc mediation analysis showed a significant association between anxiety severity and suicide risk independent of benzodiazepine use, the nature of the present study and its small sample size do not allow for any causal inferences. Additionally, the MINI does not include a dedicated module for impulse-control disorders, thus precluding us from assessing their relationship with suicidality.
Similar to the study by Elfil et al., 67 none of the examined demographic or PD-related variables, such as antiparkinsonian medications, were associated with suicide risk in our sample. Studies analyzing the correlates of suicidal ideation in PD overall report a stronger association with psychiatric variables than with demographic or PD-related variables.12–17 In the two aforementioned retrospective studies, one found that an upper extremity onset of motor symptoms was associated with completed suicide, 18 while the other observed significantly more frequent entacapone use in the suicide group, although it did not reach statistical significance in the multivariable model. 19 Other literature suggests that higher doses of levodopa 18 or dopamine agonist use 3 may be associated with the escalation of suicidal ideation into suicidal behavior; however, our small sample size of individuals with previous suicide attempts prevented us from confirming this observation. Significant differences in treatment approaches and prescription practices of levodopa and other antiparkinsonian medications across countries and continents have been highlighted, 68 which should be taken into consideration when interpreting findings related to antiparkinsonian medications.
Several limitations should be noted. First, this study was a secondary analysis, which was likely underpowered to detect potentially important effects of variables such as depression, dopaminergic medication dosing, and ethnicity on suicide risk. Other variables of interest, such as apathy, the effects of deep brain stimulation, and cultural factors, were not assessed. Similarly, no causal inferences on the relationship between anxiety symptoms, benzodiazepine use, and suicidality can be drawn, and further well-powered studies designed to investigate this question are warranted. The lack of a healthy control group also precludes direct comparisons of the prevalence of suicidality in PwP versus an age-matched sample of the general population. Our sample was derived from PwP being screened for clinical trial participation at a tertiary center, reflecting a sample with inherent differences from the general population of PwP. 69 Selection bias was also present: while participants with documented anxiety symptoms were sought out for participation during pre-screening, those with more severe depression, anxiety, apathy, and/or suicidality may have self-excluded from trial participation when approached. The class balance between those with and without anxiety in our sample gives us confidence in the relative generalizability of our results in spite of these sources of bias. While our findings are preliminary, they support the inclusion of assessments of anxiety in future studies investigating suicide risk. Nevertheless, as no participants were classified as high risk, caution is warranted in extrapolating these findings to PwP with elevated suicidality. Future work will benefit from studies in which suicidality is the primary outcome and that include PwP recruited from the community, general neurology, and acute care settings to capture a broader clinical spectrum and higher-risk cases.
In conclusion, around 22% of PwP in our sample were at risk of suicide. These individuals had higher anxiety levels. Correlates of suicide risk in PD warrant further investigation. Our findings highlight the importance of screening PwP for suicidal ideation and behavior during routine clinical care, while a one-item screen might not adequately capture individuals at risk.
Supplemental Material
sj-docx-1-pkn-10.1177_1877718X251410887 - Supplemental material for Anxiety is associated with increased risk of suicidality in Parkinson's disease
Supplemental material, sj-docx-1-pkn-10.1177_1877718X251410887 for Anxiety is associated with increased risk of suicidality in Parkinson's disease by Joyce ST Lam, Kira N Tosefsky, Julie Zhu, Dylan Meng, Petra Uzelman, Fabricio Pio, Nicholas J Ainsworth, Fidel Vila-Rodriguez, Andrew K Howard and Silke Appel-Cresswell in Journal of Parkinson's Disease
Footnotes
Acknowledgements
We thank all participants for their valuable contributions to this study, as well as the physicians and staff members at the UBC Movement Disorders Clinic and the Pacific Parkinson's Research Centre for facilitating the recruitment process. The authors also thank the following for their support: JSTL has received a Parkinson Canada Graduate Student Award and a Parkinson's Foundation Visiting Scholar Fellowship. KNT is supported by the UBC MD/PhD Program and the Canada Graduate Scholarships-Doctoral Program. NJA receives salary support from the UBC Institute of Mental Health and from the Canadian Consortium of Clinical Trial Training (CANTRAIN). SAC is supported by the Marg Meikle Professorship in Parkinson's Research through the Pacific Parkinson's Research Institute.
Ethical considerations
The study was approved by the University of British Columbia Clinical Research Ethics Board (Protocol #H18-03083).
Consent to participate
All participants provided electronic informed consent through the Research Electronic Data Capture (REDCap) system prior to undergoing any screening procedures.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Weston Family Foundation (grant number GR015436).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability
The data that support the findings of this study are available from the corresponding author (SAC) upon reasonable request.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
