Abstract
Background
Early onset Parkinson's disease (EOPD), defined as Parkinson's disease (PD) diagnosed before age 50, often presents unique challenges compared to late-onset PD, particularly with regard to non-motor symptoms. Psychosis in EOPD is associated with increased functional impairment and may lead to a higher mortality risk.
Objective
Our study is aimed to determine the prevalence of psychosis in EOPD patients and its impact on all-cause mortality, along with examining the effects of antipsychotic medications and Selective Serotonin Reuptake Inhibitors (SSRIs) on mortality in EOPD patients.
Methods
Our retrospective cohort included EOPD patients diagnosed between 1990 and 2022 at Mayo Clinic, Rochester, Minnesota. Psychosis was defined using the National Institute of Neurological Disorders and Stroke/the National Institute of Mental Health (NINDS/NIMH) Work Group criteria. Cox proportional hazards models were used to analyze the association of psychosis and medications with mortality.
Results
Of 829 patients with EOPD, 158 (19.1%) developed psychosis at a median of 12.1 years after PD motor symptom onset. Psychosis was significantly associated with increased mortality in unadjusted (HR = 4.31, 95% CI: 2.59–7.18, p < 0.001) and adjusted (HR = 3.55, 95% CI: 2.10–6.01, p < 0.001) models. No significant difference in mortality risk was observed between patients treated with antipsychotics or SSRIs versus those who were not.
Conclusions
Psychosis is a possible complication in EOPD and is associated with a significant increase in all-cause mortality. The use of antipsychotics and SSRIs did not significantly alter the mortality risk in these patients. Further research is needed to understand the mechanisms driving this association and to develop tailored interventions.
Plain Language Summary
Parkinson's disease (PD) is a condition that affects movement and can also lead to mental health challenges, including psychosis—a condition where a person may experience hallucinations, delusions, or a loss of connection with reality. While PD usually affects older adults, some people are diagnosed before age 50, a form known as early-onset Parkinson's disease (EOPD). This study explored the occurrence of psychosis in EOPD and its impact on lifespan. We reviewed medical records of 829 patients diagnosed with EOPD at Mayo Clinic between 1990 and 2022. Nearly 20% of these patients developed psychosis, usually about 12 years after their first motor symptoms appeared. Patients with psychosis were found to have a threefold higher risk of death compared to those without psychosis. The study also examined whether treatments like antipsychotic medications or antidepressants (SSRIs) affected survival in these patients. The results showed that neither type of medication significantly reduced the risk of death. These findings highlight the serious impact of psychosis on people with EOPD and underline the need for better strategies to detect and manage this condition early. By improving understanding of EOPD and its complications, this research could help guide future treatment approaches and improve care for patients.
Keywords
Introduction
Parkinson's disease (PD) is the second most common neurodegenerative disorder after Alzheimer's disease, with an incidence of 16.5 cases per 100,000 person-years and affecting men more often than women. 1 PD is a progressive disorder characterized by the degeneration of dopaminergic neurons in the substantia nigra, leading to a number of motor symptoms.2,3 However, non-motor symptoms, including cognitive impairment and psychiatric manifestations, significantly impact the quality of life and disease management.4,5 Among these non-motor symptoms, psychosis stands out due to its complexity and the challenges it poses in treatment.6–11
Early onset Parkinson's disease (EOPD) refers to PD that manifests before the age of 50.12,13 Even though the motor symptoms in EOPD are similar to those in late-onset PD, the younger age of onset suggests differences in disease progression, questionable genetic predisposition, and response to treatment.12,14–16 Psychosis in the context of EOPD is particularly concerning, as it can lead to more severe functional impairments and psychosocial consequences compared to older patients.17,18
Our study aims to determine the prevalence of psychosis in EOPD patients, identify demographic and clinical factors associated with an increased risk of psychosis in EOPD patients, evaluate the impact of psychosis on all-cause mortality in EOPD patients, and examine the effects of medications on the mortality risk among EOPD patients with psychosis.
Methods
EOPD case selection
We selected all EOPD cases from January 1990 to October 2022 at Mayo Clinic, Rochester, Minnesota, using the Mayo Clinic Data Explorer system. We searched the indexes for 5 diagnostic codes potentially indicative of PD in a similar way used in Turcano et al. (2024). 19 A movement disorder specialist (R.S.) reviewed their medical records to confirm the clinical diagnosis of PD. The onset of PD was defined as the approximate date in which at least two of the four cardinal motor symptoms of PD (rest tremor, rigidity, bradykinesia, and impaired postural reflexes) were first noted by the patient, family members, or healthcare provider, as documented in the medical record. We applied the same diagnostic, inclusion, and exclusion criteria as those outlined in the study by Savica et al. (2013). 1
Exclusion criteria included unresponsiveness to levodopa (minimum 1 g per day combined with carbidopa), patients who developed psychosis but did not have an onset date in the medical record were excluded from the analysis, extensive nervous system involvement, identification of another cause for their parkinsonism (i.e., repeated head injury or stroke, history of encephalitis, neuroleptic treatment initiated less than 6 months before motor onset, etc.). 9 Patients with a PD onset at or before the age of 50 were classified as EOPD and included for this study, to comply with the recommendations of the International Parkinson and Movement Disorder Task Force. 20 Patients with a PD onset before the age of 21 were classified as juvenile PD. 21 Patients with a PD onset after the age of 50 were considered late-onset PD (LOPD) patients and therefore not included.
Review of medical records
A comprehensive review of the patients’ medical records was performed. Patients’ demographics, disease characteristics such as PD motor subtype, date of onset of parkinsonism and date of diagnosis of PD were recorded. The date and cause of death was recorded when applicable.
Identification of patients with psychosis
We used the National Institute of Neurological Disorders and Stroke/ the National Institute of Mental Health (NINDS/NIMH) Work Group clinical criteria for psychosis to classify patients with psychosis. 7 We defined psychosis as the presence of one or more of the following symptoms: illusions, false sense of presence, hallucinations, or delusions. Psychotic symptoms had to last at least 1 month or recur within 1 month and not be explained by another medical condition. 7 We excluded all cases of acute change in mental status such as acute dementia, confusion, and delirium due to medical conditions. Psychosis etiology was classified into drug-induced, PD-related, or other causes based on clinical documentation. Drug-induced psychosis was defined as psychotic symptoms emerging in the context of medication use, with improvement upon dose reduction or discontinuation. PD-related psychosis was identified when symptoms were attributed to disease progression rather than medication effects. This classification is summarized in Table 2.
If the symptoms persisted for 6 months or more, patients were considered to have unresolved psychosis. Patients with psychosis were regarded as treated if any antipsychotic prescription was used for psychosis at any time after their psychosis diagnosis. Available antipsychotic medications at the time of the study were Quetiapine, Olanzapine, Risperidone, and Haloperidol.
Statistical analysis
Continuous characteristics were summarized with medians and interquartile ranges; categorical characteristics were summarized with frequency counts and percentages. The association between psychosis and all-cause mortality was assessed using Cox proportional hazards regression. The development of psychosis was treated as a time-dependent covariate to account properly for the variable development of psychosis between patients. The primary outcome of interest was all-cause mortality, and patients were censored at the date of death or the date of chart abstraction. Cox models were both unadjusted and adjusted for patient age, sex, and race. Model results were reported with hazard ratios (HRs) and 95% confidence intervals.
Secondary analysis assessed the risk of all-cause mortality among patients who developed psychosis with treatment using anti-psychotic medications or selective serotonin reuptake inhibitors (SSRIs). This analysis only included patients who developed psychosis and indexed patient follow-up at the onset of psychosis instead of the onset of PD symptoms. Models were both unadjusted and adjusted for patient age, sex, and race. Patients with unknown date onset of psychosis were excluded from this analysis.
Results
We identify 829 patients with EOPD from January 1990 to October 2022. Table 1 summarizes patient demographics and PD disease characteristics. Median (IQR) age was 42 (37, 46) years; 519 (62.6%) patients were male, and 693 (83.6%) patients were white.
Cohort demographics and Parkinson's disease characteristics.
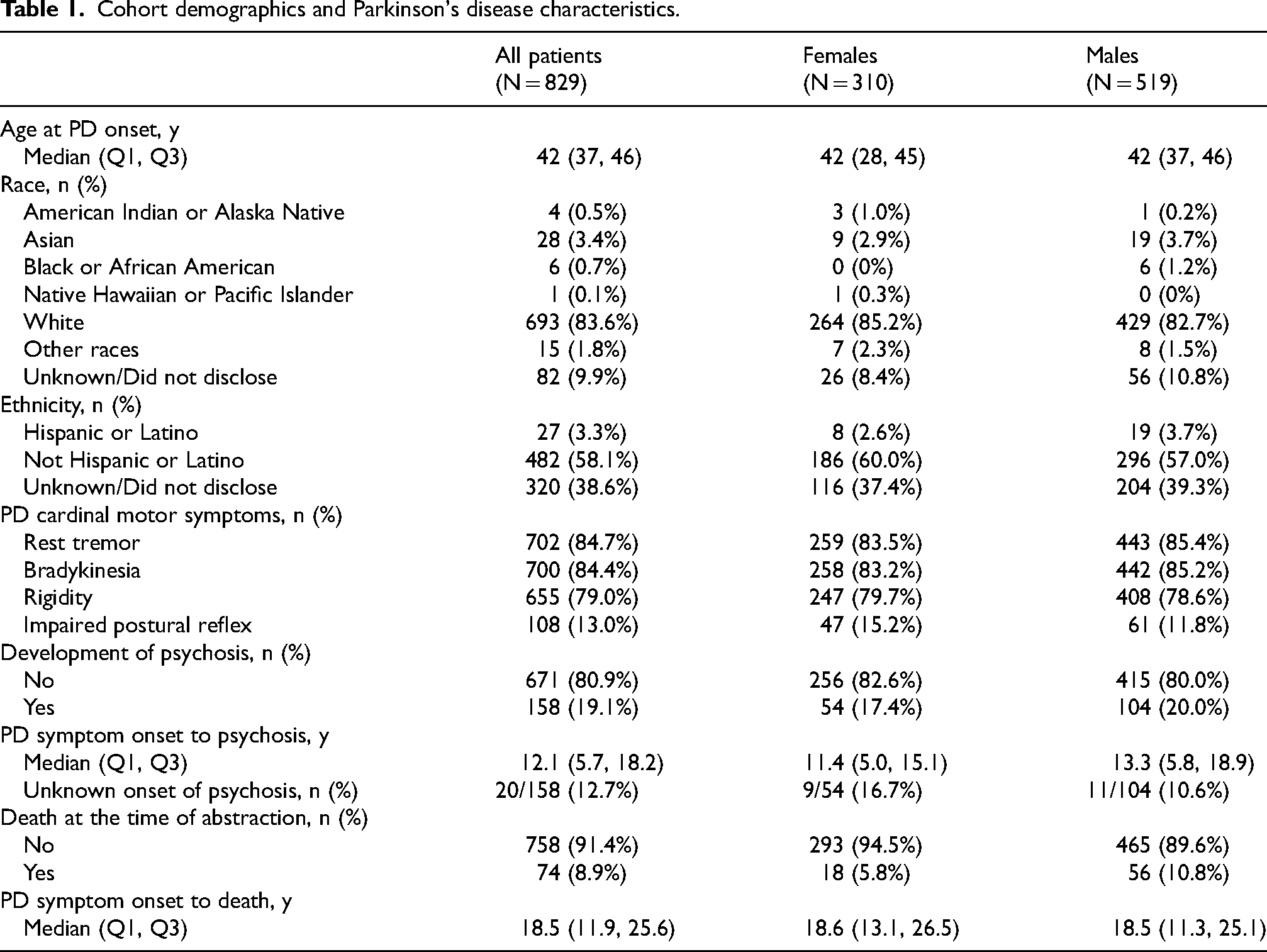
There were 158 (19.1%) patients who developed psychosis following the onset of PD motor symptoms (Table 2); these were 54 (17.4%) females and 104 (20.0%) males. The median (IQR) time from PD symptom onset to psychosis was 12.1 (5.7, 18.2) years. Drug-induced psychosis was the most common cause (52.5%), followed by psychosis related to PD or Parkinsonism (17.7%).
Characteristics of psychosis in early-onset Parkinson's disease.
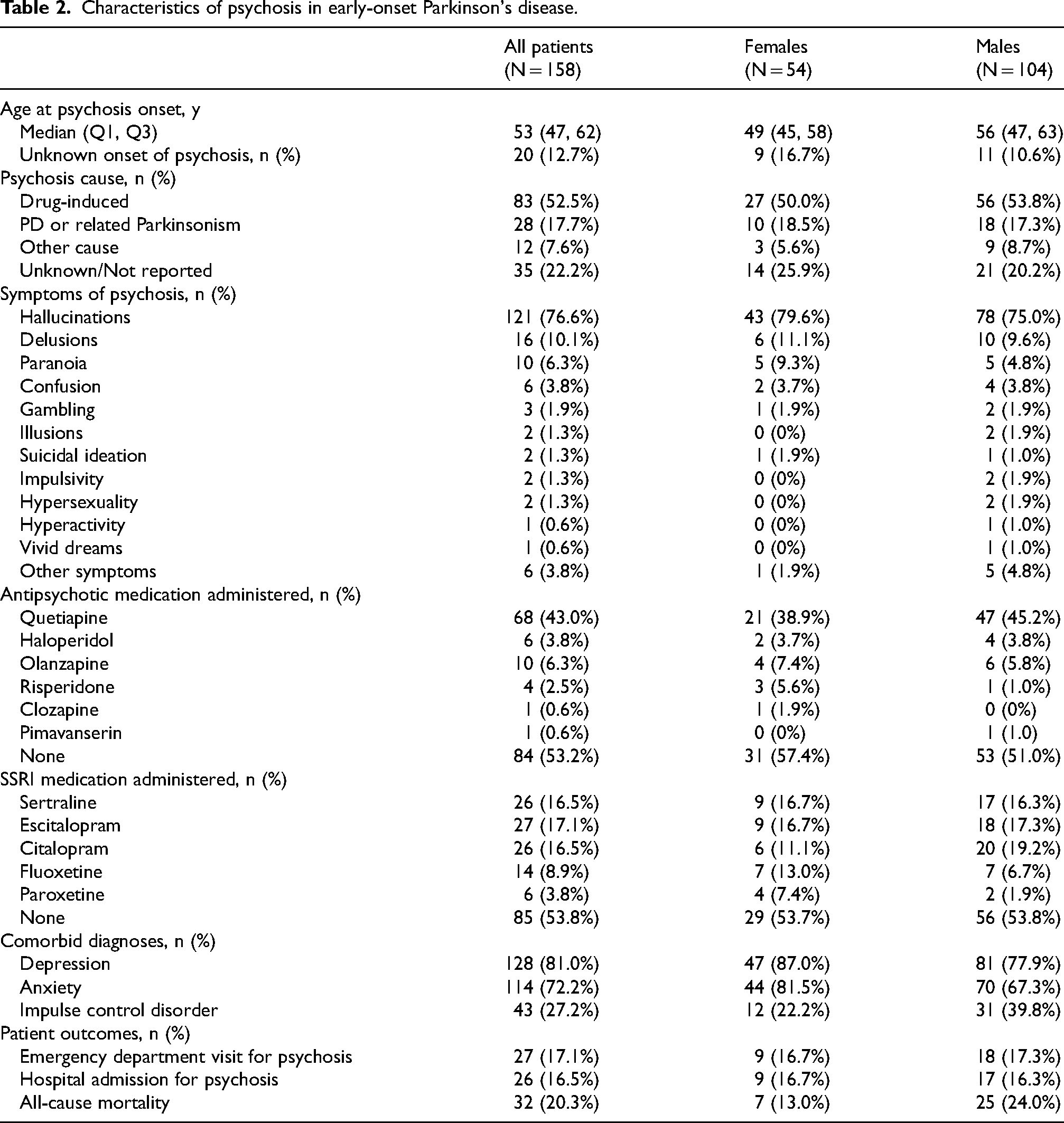
In unadjusted analysis, psychosis was associated with 4 times greater risk for death among EOPD patients (HR = 4.31, 95% CI: 2.59–7.18, p < 0.001) compared to EOPD without psychosis. After accounting for patient age, sex, and race, psychosis was associated with more than 3 times greater risk for death (HR = 3.55, 95% CI: 2.10–6.01, p < 0.001). The Kaplan-Meier cumulative incidence curve for all-cause mortality among patients with and without psychosis are reported in Figure 1.
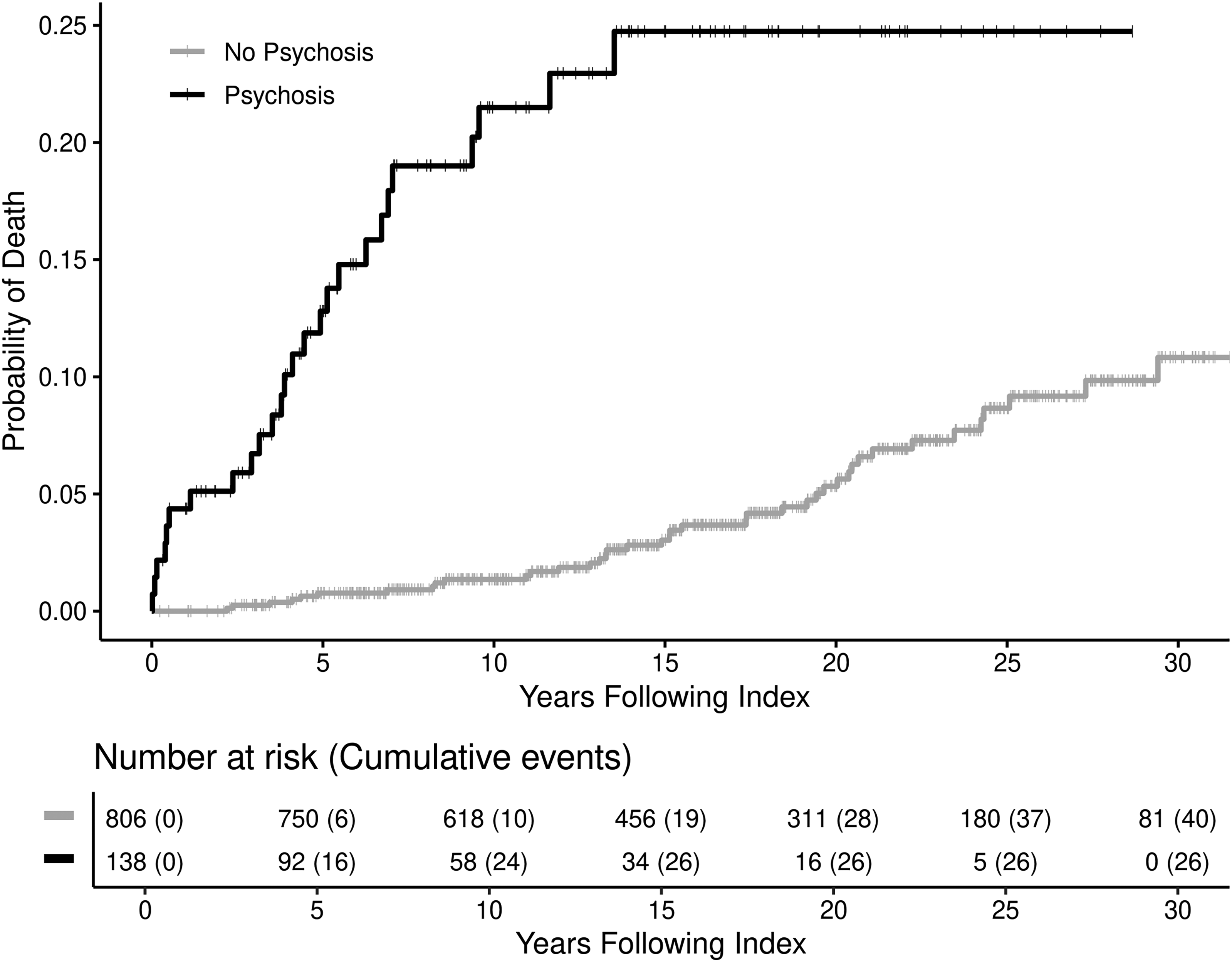
Kaplan-Meier cumulative all-cause mortality among early-onset Parkinson's disease patients. Index refers to the date of PD symptom onset (no psychosis) or the date of psychosis onset (psychosis) and the 20 patients with unknown psychosis onset were excluded from the figure.
Among the 158 patients who developed psychosis, 74 (46.8%) were prescribed antipsychotic medication at any point during the study after developing psychosis, and 73 (46.2%) used SSRIs either before or after developing psychosis. There was no significant difference in risk of death for patients who were taking anti-psychotic medications compared with patients not taking anti-psychotic medications in either the unadjusted (HR = 0.65, 95% CI: 0.29–1.43, p = 0.13) or adjusted (HR = 0.69, 95% CI: 0.31–1.53, p = 0.36) analyses. This suggests that taking antipsychotics does not increase mortality in EOPD patients. Similarly, there was no difference in risk of death associated with taking SSRIs in the unadjusted (HR = 0.55, 95% CI: 0.25–1.20, p = 0.13) or adjusted (HR = 0.60, 95% CI: 0.27–1.33, p = 0.22) models. Additionally, taking antipsychotics didn't increase the mortality for EOPD.
Discussion
Our study provides a analysis of the prevalence, clinical characteristics, and outcomes of psychosis in patients with EOPD. The findings highlight the strong impact of psychosis on the mortality of EOPD patients and contribute to the understanding of its clinical management.
We observed that psychosis occurred in 19.1% of EOPD patients, suggesting that it is a possible complication in this patient population, compared to 38.4% of LOPD patients. 9 The median time from PD motor symptoms onset to the development of psychosis was approximately 12.1 years, indicating that psychosis tends to manifest in the later stages of the disease. In contrast, the median time to the onset of psychosis in LOPD patients was 8.1 years after the onset of PD motor symptoms, suggesting a more rapid progression in these cases. 9 Additionally, psychosis was associated with a significantly increased risk of mortality. Patients with psychosis had a risk of death that was three times higher compared to those without psychosis, even after adjusting for age, sex, and race. LOPD patients have a 71.4% increase in the risk of death compared to PD patients. 9 The differences in psychosis presentation between EOPD and LOPD may be attributed to the brain's neuroplasticity and compensatory mechanisms in response to dopaminergic neuron loss. Research indicates that humans must lose approximately 48–68% of dopaminergic neurons in the substantia nigra pars compacta (SNc) and around 70 to 80% of dopamine content in the striatum before symptomatic Parkinson's disease manifests. 22 This highlights the brain's ability to compensate for early dopaminergic deficits, effectively delaying the onset of symptoms. 22 Alternatively, the differences may be due to mesolimbic involvement. Larkov et al. 2020 highlights the role of the mesolimbic pathway in PD, particularly in relation to cognitive and emotional deficits. It suggests that disruption of dopaminergic output from neurons in the ventral tegmental area (VTA) impairs the mesolimbic system, contributing to these deficits. 22
In our cohort, drug-induced psychosis was the most common cause (52.5%), followed by psychosis related to PD or Parkinsonism (17.7%). This distinction is important as it highlights the significant role of medication effects in the development of psychosis in EOPD. Identifying whether psychosis is primarily driven by medication or disease progression is crucial for treatment decisions, as medication adjustments may alleviate symptoms in drug-induced cases, whereas PD-related psychosis may require targeted therapeutic interventions. Moreover, the high prevalence of drug-induced psychosis may have contributed to the observed lack of significant mortality benefit with antipsychotic treatment. In cases where psychosis is medication-induced, modifying or discontinuing the causative agent may be a more effective approach than introducing an antipsychotic. Conversely, in PD-related psychosis, disease progression and underlying neurodegenerative changes may drive symptoms, making pharmacological intervention more relevant. The heterogeneity in psychosis etiology within this cohort may have diluted the potential survival benefit of antipsychotic use. Future studies should stratify outcomes based on psychosis cause to better assess treatment efficacy and optimize management strategies.
The prevalence of psychosis in our EOPD cohort aligns with prior studies reporting psychosis as a common non-motor symptom of PD; however, our focus on early-onset cases provides a specific perspective that has been less explored.8,23,24 Previous research has consistently demonstrated that psychosis in PD is associated with increased morbidity and mortality, but no information was available specifically in the EOPD population.9,25 The mechanism behind the occurrence of psychosis in PD remains unclear. Some studies have employed functional neuroimaging to explore this phenomenon. Visual hallucinations (VH) in PD patients were associated with functional changes in associative visual cortices, possibly linked to increased stability of resting-state networks. 23 Similarly, fMRI studies during active hallucinations in a PD patient, demonstrated that visual hallucinations are accompanied by marked desynchronization occurs between posterior and anterior cortical areas involved in visual processing. 26 The temporal relationship between PD onset and psychosis development in our study is also consistent with existing literature, suggesting psychosis typically occurs after many years of living with PD, often coinciding with disease progression and treatment complications.9,10,13 Some studies tried to explain the difference of presentation of psychosis in EOPD and LOPD.
The findings of this study highlight the need for heightened vigilance and proactive management of psychosis in patients with EOPD. Given the significant mortality risk associated with psychosis, clinicians should monitor EOPD patients closely for early signs of psychiatric symptoms and consider early intervention strategies. The lack of significant mortality reduction with antipsychotic or SSRI treatment in our study suggests that current pharmacological approaches may be insufficient, and that alternative or adjunctive therapies should be explored. Although no significant survival benefit was observed with antipsychotics or SSRIs, the relatively large effect sizes (antipsychotics aHR = 0.70; SSRIs aHR = 0.60) suggest a potential benefit that may not have reached statistical significance due to the limited sample size (158). Another limitation is the absent utilization for Parkinson's disease psychosis, such as Pimavanserin (not yet available in the study period) or Clozapine (not used because of the difficulties to be prescribed).24,27 Instead, most patients received either Quetiapine or other antipsychotics such as Haloperidol, Risperidone, and Olanzapine. 28 This prescription pattern may have contributed to the lack of benefit in mortality and highlights the need for clinicians to reconsider antipsychotic selection in PD-related psychosis. We emphasize that clinical decisions should be guided by symptom management and improvements in quality of life rather than mortality outcomes alone.
Our study has several strengths. First, it includes a large cohort of 829 patients with EOPD. By focusing specifically on EOPD, the study addresses an underexplored subgroup of Parkinson's disease, offering unique insights into the prevalence, characteristics, and outcomes of psychosis in this population. The use of the Mayo Clinic Data Explorer system allowed for the examination of comprehensive and longitudinal medical records, enabling an in-depth analysis of disease progression and outcomes. Psychosis was rigorously defined using the NINDS/NIMH Work Group clinical criteria, ensuring consistency and precision in case identification.
Despite these strengths, there are several limitations that should be considered when interpreting the results. First, the retrospective nature of the study design may introduce biases related to incomplete or inaccurate medical records. Additionally, the study population was predominantly Caucasian and of Northern European Ancestry, which may limit the generalizability of the findings to more diverse populations. Moreover, the exclusion of patients with unknown psychosis onset dates may have led to an underestimation of the true prevalence and impact of psychosis in this population. The lack of structured interviews and standardized data collection introduces variability in the clinical assessment of psychosis. Furthermore, the single-center nature of the study may not fully represent patient populations or clinical practices in other settings. In addition, our study did not include data on MAO-B inhibitor use, which may be relevant in the context of psychosis and mortality risk. Future studies should consider evaluating the potential impact of MAO-B inhibitors to better understand their role in this population. Lastly, the study focused primarily on pharmacological treatments, leaving the role of non-pharmacological or adjunctive therapies unexplored, which could be an area for future research.
Further research is needed to explore the underlying mechanisms that contribute to the increased mortality risk associated with psychosis in EOPD patients. Longitudinal studies with larger and more diverse cohorts could provide more definitive insights into the progression of psychosis and its impact on mortality. Additionally, exploring the effectiveness of alternative therapeutic interventions, including non-pharmacological approaches, could help identify more effective management strategies for psychosis in EOPD. Our study highlights the substantial prevalence and serious implications of psychosis in patients with EOPD. The association between psychosis and increased mortality underscores the need for early detection and improved management strategies. Addressing the challenges of treating psychosis in this population is essential for improving long-term outcomes and quality of life for EOPD patients.
Footnotes
Acknowledgements
We are grateful to the patients and their families for taking part in this cohort study. We thank the Mayo Data Explorer team for their support.
Ethical considerations
This study was approved by the Mayo Clinic Institutional Review Board.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
The data supporting the findings of this study are available on request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
