Abstract
Purpose
The purpose of this matched cohort study was to determine the impact of intensive, multidisciplinary neurorehabilitation on functional independence following pediatric acquired brain injury.
Methods
Cohorts receiving lower-intensity (n = 19) and higher-intensity multidisciplinary neurorehabilitation (n = 19) were matched on age, injury characteristics, and admission functional status. Intensity was measured by time in physical, occupational (OT), and speech therapy over length of stay (LOS). Outcome measures included WeeFIM efficiency, WeeFIM developmental functional quotients (DFQs), and LOS.
Results
There were no significant between-cohort findings in 1) WeeFIM efficiency, 2) WeeFIM DFQs or 3) LOS. There was a significant difference between admission and discharge WeeFIM DFQs for all participants (p < 0.001), demonstrating significant functional recovery regardless of intensity. Hierarchical linear regressions were significant for OT intensity and discharge WeeFIM DFQs (p = .003, ΔR2 = .22). Total admission WeeFIM DFQs significantly predicted LOS in the lower-intensity (p = 0.016, R2 = 0.29) and higher-intensity (p < 0.001, R2 = 0.51) cohorts, indicating a greater variance explained with increased intensity.
Conclusion
While significant functional outcomes were not correlated with intensity, OT intensity did significantly predict variations in functional independence. Investigation into definitive parameters for intensive treatment, including the amount and context of therapeutic interventions, is needed.
Introduction
Acquired brain injuries (ABIs), both traumatic and non-traumatic injury mechanisms, are the leading cause of mortality and disability in pediatric populations. Brain injuries account for the highest hospitalization rate among pediatric populations. 1 Pediatric brain injuries represent the largest number of individuals receiving inpatient rehabilitation (IPR). An estimated 145,000 children and adolescents live with substantial and long-lasting limitations in social, behavioral, physical, or cognitive functioning following a brain injury. The overall associated cost with an ABI sustained under the age of 14 is around $60.4 billion. 2 Aside from the societal and financial burden, pediatric ABIs have a substantial caregiver burden and a long-standing impact on family functioning. 3
Moderate to severe ABIs are associated with acute and persistent detrimental effects on age-appropriate functional independence and developmental activities of daily living.4,5 Pediatric patients with moderate to severe ABI often participate in intensive neurorehabilitation to address functional deficits. Pediatric-focused multidisciplinary neurorehabilitation optimizes functional independence and improves functional recovery.6–11 An essential parameter for treatment efficacy during pediatric IPR is dosage. 12 Emerging evidence suggests dose is defined as frequency, intensity, time, and type of intervention.12,13 Defining intensity is an established problem in rehabilitation research.5,13,14 With no definitive definition, most studies report intensity as the number of minutes in active or scheduled therapy.5,15 While time spent in therapeutic intervention may not be the most robust measurement of intensity, it remains the dominant measure of intensity in research.10,13,14 Timing and intensity are crucial parameters of dosage impacting the efficiency of neurorehabilitation for ABI populations.12,16 The optimal timing of neurorehabilitation is well-supported in the literature, but there is a lack of evidence regarding the intensity required to initiate experience-dependent plasticity.
Low-intensity stimulation can weaken synaptic responses, while high-intensity stimulation can induce long-term potentiation. 17 Overall, early-onset and more intensive neurorehabilitation in the IPR setting promotes functional recovery following moderate to severe traumatic brain injury (TBI) in adult populations. 5 Higher-intensity multidisciplinary rehabilitation is associated with functional outcomes, discharge destination, and length of stay (LOS) in adult brain injury populations.5,18–20 Additionally, higher levels of effort during interventions and duration of engagement in more complex therapy activities are associated with better functional outcomes. 18 As evidence continues to emerge for adult populations regarding intensity, measured by active time in therapy, there remains a lack of literature examining therapeutic intensity during pediatric neurorehabilitation following ABI.
There are drastic variations in the intensity of therapeutic interventions provided during IPR following ABI. Variations in intensity exist from one to two hours daily up to eight hours per day based on the facility. 21 A recent scoping review synthesizing the evidence on dosage characteristics and rehabilitation efforts on recovery in pediatric ABI populations reported variations in intervention characteristics, including ranges in frequency, duration, and type. However, the studies included in the review did not specify intensity and reported ranges in time between 25 min to six hours a day, acknowledging a well-established problem with defining intensity in rehabilitation research. 13 These variations could significantly impact recovery trajectories and functional outcomes.
The lack of definitive parameters for intensity, including the variations in intensity and inconsistent outcomes following IPR, has resulted in scrutiny of rehabilitation services for all populations and ages, including pediatric ABI. Policy changes can impact reimbursement, and the continued scrutiny creates a critical need for evidence to support the optimal intensity and effectiveness of rehabilitation services. 22 Furthermore, more recent studies report insufficient evidence for the “three-hour rule” recommendation based upon the Centers for Medicare and Medicaid Services Intensity of Therapy requirement.23,24 There are limited clinical practice guidelines (CPGs) for pediatric IPR, since the variability in intensity, duration, and type remains unknown. 10 Investigating intensity during pediatric neurorehabilitation following ABI could significantly impact the quality and efficacy of neurorehabilitation and impact payer reimbursement. The development of CPGs for intensity and dosage in pediatric populations during IPR is needed to promote optimal outcomes and minimize costs to families, providers, and society. 25
Focus on pediatric populations is needed due to the established associations between age and the greater potential for neural plasticity.5,17 Pediatric patients with brain injuries who received care at a specialized pediatric hospital had higher cognitive scores than non-specialized centers. 6 Quality indicators, including specialized pediatric training, are predictive of outcomes; however, the parameters for intensity during specialized rehabilitation remain unknown. Further evidence is needed to establish the most cost-effective intensity of inpatient therapy to create sustainable patient outcomes. 22 Overall, there is limited evidence for the corresponding dose-response relationship between intensity and functional gains during and following neurorehabilitation, especially in pediatric populations.
The purpose of the study was to determine the impact of an intensive, multidisciplinary neurorehabilitation approach on overall functional independence following ABI in pediatric populations at the time of discharge from IPR. The secondary aims of the study were 1) to determine the impact of intensive, multidisciplinary neurorehabilitation on motor skills (self-care and mobility) and cognitive functioning based on the motor and cognitive domains of Functional Independence Measure for Children (WeeFIM®); 2) to determine the effect of intensive, multidisciplinary neurorehabilitation on IPR LOS; 3) to examine the impact of discipline-specific intensive approaches (occupational therapy [OT], physical therapy [PT], speech therapy [SLP]) on functional outcomes; and 4) to identify any predictors of functional outcomes with consideration to intensity.
Methods
Study design and participants
The study was a matched cohort study investigating the effect of intensity, measured as total minutes in skilled, direct therapy over length of admission, during multidisciplinary neurorehabilitation on functional independence following ABI in pediatric populations as measured by WeeFIM scores converted to WeeFIM efficiency and developmental functional quotients (DFQs). A cohort of participants receiving lower-intensity multidisciplinary neurorehabilitation (n = 19) was matched and compared to a cohort of participants receiving higher-intensity multidisciplinary neurorehabilitation (n = 19) based on age, injury characteristics, and admission WeeFIM scores, as a marker of severity.
The study was approved by the Institutional Review Board at Rocky Mountain University of Health Professions. Participants were admitted to a designated pediatric-specialized IPR accredited by the Commission on Accreditation of Rehabilitation Facilities® (CARF) between February 8, 2019, and October 22, 2021.
All pediatric patients admitted with a primary diagnosis of ABI were screened for eligibility (n = 106). Pediatric participants were included in the study (n = 81) based on the following inclusion criteria: age 12 months to <228 months; injury coded 1.0–1.9 (stroke), 2.0–3.0 (all brain dysfunction/injury) including 2.1–2.2 (non-traumatic injury) or 2.2–2.30 (traumatic brain dysfunction) in the Uniform Data System for Medical Rehabilitation (UDSMR®) database; admission to designated IPR center. Participants were excluded from the study for the following (n = 25): missing information on impairment code or incorrect diagnosis coding; missing evaluation scores; code 14.2 (brain injury with multiple fractures for WeeFIM and FIM) or non-weightbearing status for lower extremity at time of admission to IPR due to impact of trauma on WeeFIM scoring; clinically implausible functional scores; pre-existing disability; admission from home with secondary complications of initial injury; less than one week of admission to IPR (less than six nights, seven days of skilled therapy provided); sequential admissions (not initial admission); total dependence at the time of admission and discharge. See Table 1 for inclusion and exclusion criteria and Table 2 for individuals excluded from the study.
Inclusion and exclusion criteria.
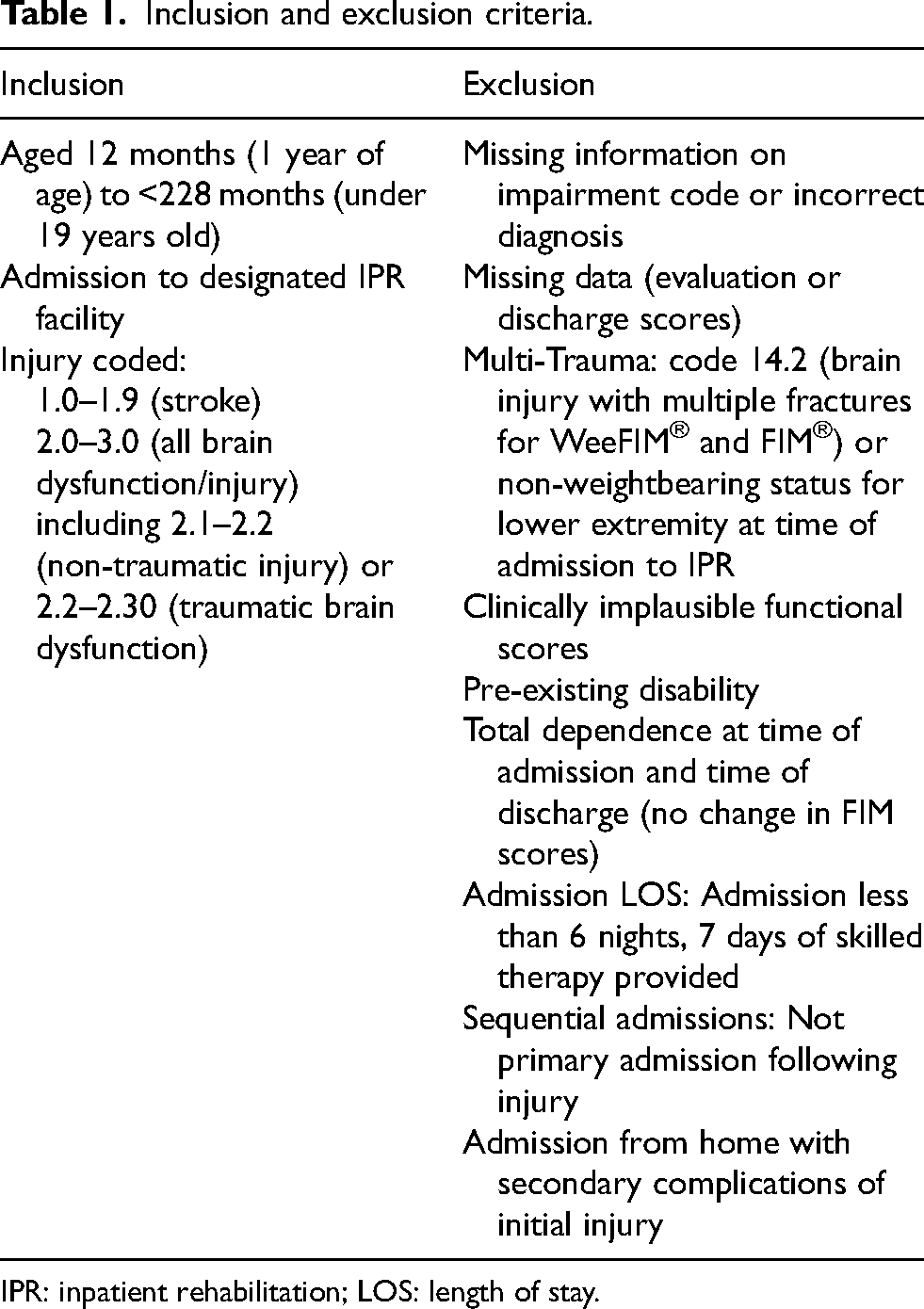
IPR: inpatient rehabilitation; LOS: length of stay.
Exclusion table.
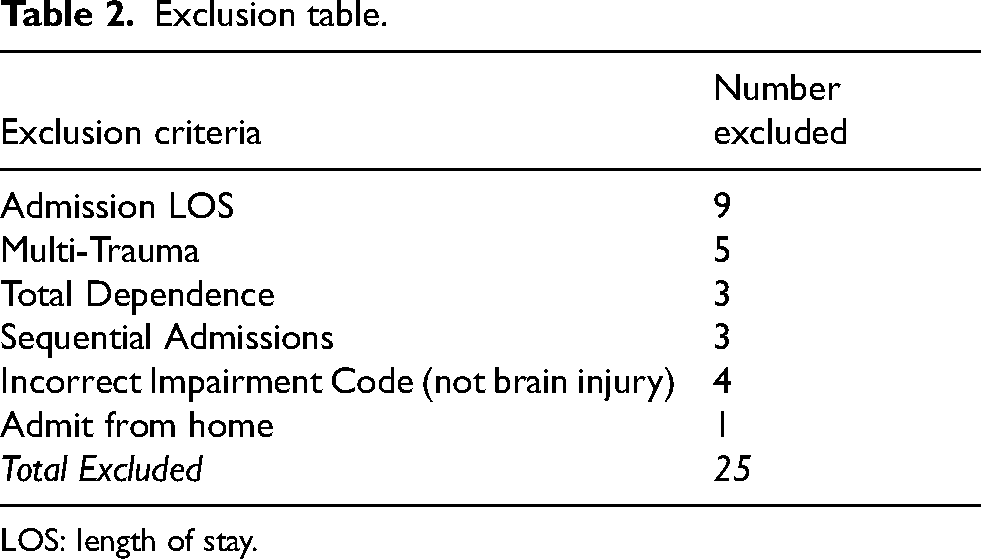

LOS: length of stay.
Procedures
Individuals who met the inclusion criteria were enrolled in the study (n = 81) based on consecutive sampling. Individuals were matched based on intensity parameters and identified clinical characteristics impacting functional outcomes (n = 38). Within 72 h of admission to IPR, the credentialed multidisciplinary team members assessed participants using the WeeFIM instrument, assessing self-care, mobility, and cognitive abilities as part of routine care. All recorded WeeFIM data was scored by credentialed nursing staff, occupational therapist(s), speech therapist(s), physical therapist(s), and neuropsychologist(s), ensuring a comprehensive evaluation process. To enhance inter-rater reliability, all raters underwent a credentialing process aligned with the guidelines of the UDSMR. During admission, participants participated in skilled OT, PT, and SLP interventions, as well as neuropsychology, recreational therapy, art counseling therapy, and school. In this early IPR setting, the participants participated in targeted early neurorehabilitation efforts, including individualized interventions to maximize functional independence for community re-integration. The direct, skilled interventions were provided by licensed and trained occupational therapists, physical therapists, and speech-language pathologists, experienced in brain injury rehabilitation with pediatric populations under the supervision of a physiatrist. The multidisciplinary team determined appropriate interventions, including timing and effort levels, based on individualized care and individual goal-directed therapeutic interventions. Within 72 h of discharge, the WeeFIM instrument was re-administered by credentialed multidisciplinary team members. If an individual unexpectedly discharged from IPR for any duration longer than three days, the WeeFIM scores collected on the final day of admission were utilized. The total and domain (self-care, mobility, and cognition) WeeFIM measurements were documented and converted to WeeFIM efficiency scores, DFQs, and DFQ percentage changes for matched intensity cohort comparison, measuring functional independence.
Demographic and injury-specific clinical characteristics were extracted from electronic medical records (EMRs) upon the participant's discharge. Daily minutes of OT, PT, and SLP were obtained from each participant's EMR, recorded as therapists’ documentation of daily minutes of billable therapy. The total minutes per discipline were verified with internal recorded source, with variations addressed during data collection, to eliminate confounding errors with intensity parameters.
Primary and secondary measures throughout the participant's admission to the designated center were recorded, including (1) WeeFIM scores from admission and discharge, including subscales and domains, (2) demographic information and injury characteristics, (3) calculated LOS, and (4) daily minutes of therapeutic interventions including discipline-specific minutes. The multidisciplinary team was blinded to the study design by the systematic inability to identify matched comparisons.
Based on the literature and clinical expertise, the following variables were selected for optimal matching prior to observed outcome measures to avoid variable selection based on estimated effects. A computer algorithm was utilized to maximize intensity differences, accounting for matching parameters.
Matched variables
Lower and higher intensity cohorts were matched based on (1) age, (2) mechanism of injury and injury characteristics, and (3) admission WeeFIM scores, as a marker of severity – significant factors impacting functional outcomes.7,26–30
Age
Based on the principles of neuroplasticity, age significantly impacts experience-dependent synaptic potentiation, synaptogenesis, and cortical reorganization. 17 In previous studies, younger children had reduced functional improvements than older children during IPR following TBI, as well as a significant reported effect of age on motor and cognitive DFQs. 6 Other evidence suggests that age impacts functional recovery and should be considered in predictive recovery models for pediatric brain injuries. 31 Older age is associated with better functional outcomes in pediatric TBI populations.9,32 For pediatric nontraumatic brain injuries in IPR, age provided the strongest models for predicting functional outcomes per WeeFIM efficiency. 33 Among patient pre-injury characteristics, an individual's age at the time of injury accounts for significant variance in functional outcomes.6,9,10 In general, children under the age of seven are at increased risk for adverse outcomes, impacting functional recovery, compared to older children and adolescents. 34
Based on the available evidence, matching by age ranges between the two cohorts aided in controlling variability in functional outcomes, specifically WeeFIM scores. The participants were matched into two age brackets: (1) less than or equal to 72 months and (2) greater than 72 months. These groups are consistent with transitions within the developmental lifespan and identified in the literature to impact functional outcomes based on an established effect of age on functional ratings on WeeFIM for children younger than seven years of age.9,10,11,33
Mechanism of injury and injury characteristics
Evidence depicts a confounding impact of the mechanism of injury on recovery rate, trajectory, and prognosis. Literature suggests variations in functional outcomes based on the mechanism of injury in pediatric populations, with noted significant improvements in WeeFIM scores6,9–11,35 and functional recovery 36 in TBI compared to non-traumatic injuries. Other evidence suggests no significant difference in functional outcomes following IPR between abusive and non-abusive brain injuries. However, non-abusive injuries had greater independence with ambulatory status at time of discharge. 37 Due to the mechanism of injury and principles of neuroplasticity, the functional recovery and recovery trajectory are different between non-traumatic and traumatic injuries.
Participants from each cohort were matched based on the mechanism of injury: stroke, non-traumatic, or traumatic. The mechanism of injury was collected from the chart and identified as the admitting physician's prescribed injury coded. An injury code of 2.0–3.0 identifying brain dysfunction/injury was considered for matching based on the inclusion of 2.1–2.2 (non-traumatic injury), 2.2–2.30 (traumatic brain dysfunction), and stroke coded as 1.x (1.1, 1.2, 1.3, 1.4, and 1.9) by the UDSMR database. Within each code, the mechanism of injury was further stratified for matching by etiology and location based on medical chart review, diagnostic imaging, and investigating team's discretion. Considerations for optimal matching included focal verse diffuse injuries, lesion location, and other injury characteristics impacting functional recovery. Matching included posterior fossa masses; diffuse axonal injury; left focal lesions; hypoxic-ischemic encephalopathy; non-accidental trauma; arteriovenous malformation/stroke; moderate to severe focal TBI with location considered; mild TBI; and brainstem involvement.
Severity: Admit WeeFIM
Several significant factors could impact the functional trajectory and recovery following an ABI. The severity of injury based on Glasgow Coma Scale, the time from injury to admission to IPR, the time to following commands, length of post-traumatic amnesia, admission functional independence, and many other variables have been noted in the literature to impact functional independence and WeeFIM scores.7,9,11,38 Evidence suggests that admission levels of dependence following TBI were the most powerful predictor of LOS and WeeFIM motor score (p < 0.001). 39 LOS was significantly associated with admission WeeFIM score, with shorter LOS in children who had higher functional ratings on admission (P < .001). 9 Admission WeeFIM scores significantly predict levels of functional gain throughout IPR in non-traumatic brain injuries, and significantly predict the likelihood of gains in self-care and mobility in TBI participants. 27 Of the reported 69.5% variance in discharge FIM motor scores, the greatest variance was contributed to admission FIM scores (p < 0.001), an indicator of functional independence in adult brain injury populations. 39
Participants were matched based on WeeFIM total admission scores, as a marker of severity, to within +/- 10 points of admission WeeFIM scores.
Intensity
Intensity was measured as active minutes of billable OT, PT, and SLP services. The total minutes spent in each discipline-specific intervention were recorded daily in the chart by licensed providers. The total minutes in each discipline were included in the calculations of total time in multidisciplinary rehabilitation per day. Minutes per discipline were included in secondary review of discipline-specific intensity through statistical analysis. Only internal resources providing direct patient care were utilized. Indirect time spent in care-related activities such as patient care conferences, multidisciplinary team meetings, and documentation were not included. Time spent in co-treatments between disciplines was split equally amongst the disciplines involved. For statistical analysis, intensity was the participant's total minutes of OT, PT, and SLP for the participant's duration of admission divided by total LOS. The calculated intensity represented the participant's daily average minutes of billable services. Discipline-specific intensity was measured by minutes engaged in each discipline-specific intervention over LOS. A computer algorithm created by an author maximized intensity differences between participants while remaining within matching parameters. The algorithm grouped participants by age and diagnosis, resulting in 56 cases across 13 groups. For matching procedures, pairs within each group were required to have their admission WeeFIM scores within 10 points of each other and at least a 15-min difference in their average active minutes of therapy. Pairwise combinations were generated to maximize the difference in therapy intensity between matched participants. The algorithm presented the capability to prioritize grouping with the smallest range in therapy-minute differences, as needed.
Outcome measures
WeeFIM
The WeeFIM® instrument measures functional abilities and the need for assistance associated with levels of disability in pediatric populations aged six months to seven years and older. 40 It is an 18-item performance-based instrument that assesses mobility (five items on transfers and locomotion), self-care (eight items on self-care and sphincter control), and cognitive abilities (five items on communication and social cognition) and weighs the burden of care for individuals across time.40,41 Each item is scored on an ordinal scale reflecting complete independence without modifications or assistance from a caregiver (7) to total dependence and assistance from a caregiver (1). 40
The WeeFIM is more suitable for the IPR setting and is quicker to administer with minimal ceiling effects than the Pediatric Evaluation of Disability Inventory. 42 It is a valid measurement of functional outcome and caregiver burden in children with ABI.9,43 In pediatric populations with disabilities, studies report excellent test-retest and inter-rater reliability,44,45 excellent test-retest reliability for each domain, and high internal consistency for motor and cognitive domains. 46 Literature depicts early improvements on the WeeFIM provide clinically meaningful insight into functional status at discharge. 42
WeeFIM efficiency
WeeFIM efficiency is the gross change in WeeFIM scores from admission to discharge divided by the length of rehabilitation stay. WeeFIM efficiency has been utilized in various pediatric functional outcome studies.8,10,11,33
WeeFIM DFQs
While the matched cohort grossly accounted for age, DFQs were used as an outcome measure to consider the known effect of age on functional abilities and development in children under the age of six.6–8,31,41 DFQs utilize a quotient score based on age-normative values reported by UDSMR 47 to reflect percent of ‘age-appropriate’ functioning, ranging from 14 for a child scoring below age-based norms to greater than 100 for a child who performs at a level exceeding the age-based norms.8,31,41 Secondary outcomes for the study included 1) DFQs for total, self-care, mobility, and cognitive domains, and 2) DFQs percent change from admission to discharge (change in admission to discharge DFQs divided by admission DFQs, multiplied by 100).
Data analysis
Descriptive statistics were performed to examine demographic, clinical, and injury-specific characteristics based on matched intensity cohort allocation. Preliminary analyses were performed to ensure the assumptions of normality (Rule of 1 for skewness) and homogeneity of variance were met. If the variable violated assumptions of normality, the degree of skewness was determined, and the data was log-transformed accordingly. Independent t-tests or Mann-Whitney U tests (if assumptions were not met) were used to examine any significant differences between groups based on clinical characteristics and functional independence at admission.
For between-cohort analysis, independent t-test or Mann-Whitney U test was used to examine whether there was a significant difference in WeeFIM efficiency, raw WeeFIM scores, and LOS.
A mixed-model ANOVA was used to determine whether there were significant differences in DFQs between the matched intensity cohorts at the time of admission and discharge. Assumptions of normality, homoscedasticity, and multivariate outliers were met for analysis. The percentage change in DFQs violated the normality assumption and, therefore, was transformed based on natural logarithms before conducting an independent t-test.
Univariate linear regression models were calculated to determine if total intensity significantly predicted LOS. Additional analysis for the prediction of intensity on LOS included stratification based on matched intensity cohorts.
Correlation analyses were calculated using Spearman's rho (r) to determine correlations between discipline-specific intensities and functional outcomes. Secondary analyses using hierarchical linear regression models were conducted to assess the moderating effect of discipline-specific intensity on functional outcomes. Cohen's standard was used to evaluate the strength of the relationships, where coefficients between 0.10 and 0.29 represent a small effect size, between 0.30 and 0.49 represent a moderate effect size, and above 0.50 indicate a large effect size. Steps within hierarchical regression were compared to the previous step using F-tests. Assumptions of normality, homoscedasticity, multicollinearity, and outliers were met for analysis.
Correlation analyses were calculated using Spearman's rho (r) to examine predictors of functional outcomes, with stratification for matched-intensity cohorts. Assumption for monotonic relationship was met. Linear regression models were conducted to assess whether predictors and total intensity significantly predicted functional outcomes. Assumptions of normality, homoscedasticity, and multivariate outliers were met for analysis.
All statistical analysis were performed using Intellectus Statistics™. 48 Alpha levels were set at p ≤ 0.05 for all analyses.
Results
Participant characteristics
See Table 3. There were no significant differences between the matched intensity cohorts for baseline clinical characteristics including age, time from injury to admission, and admission WeeFIM scores. The average age was 114.63 months (standard deviation [SD] = 71.06, minimum [Min] = 14.00, maximum [Max] = 220.00, median [Mdn] = 123.00) in the lower-intensity cohort and 106.58 months (SD = 68.01, Min = 24.00, Max = 214.00, Mdn = 81.00) in the higher-intensity cohort. There were no significant differences between admission WeeFIM scores for the matched cohorts, including total score, motor (self-care and mobility), and cognitive domains.
Clinical characteristics by matched intensity cohort.
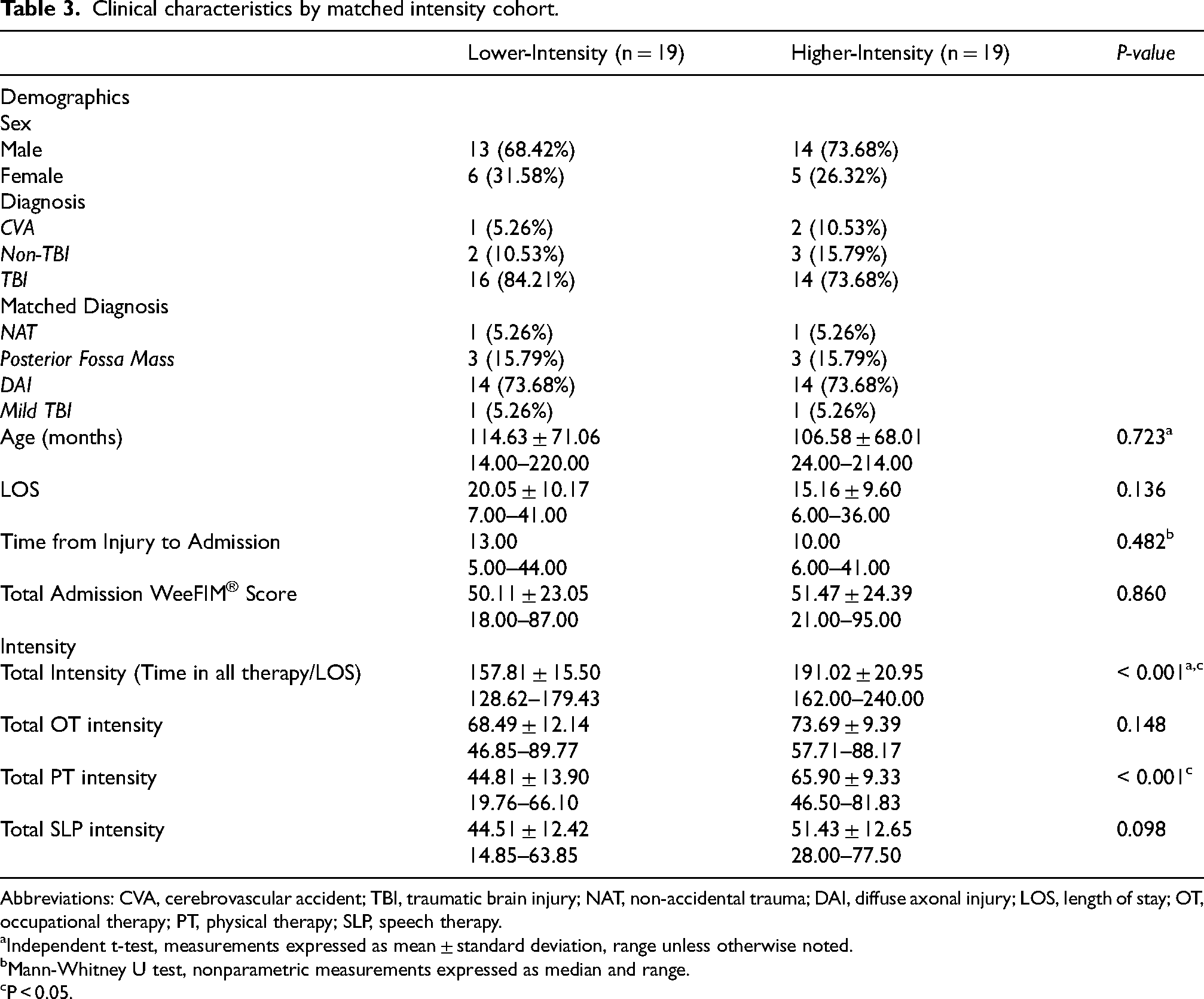
Abbreviations: CVA, cerebrovascular accident; TBI, traumatic brain injury; NAT, non-accidental trauma; DAI, diffuse axonal injury; LOS, length of stay; OT, occupational therapy; PT, physical therapy; SLP, speech therapy.
Independent t-test, measurements expressed as mean ± standard deviation, range unless otherwise noted.
Mann-Whitney U test, nonparametric measurements expressed as median and range.
P < 0.05.
The average intensity, measured as minutes of therapy over LOS, was significantly lower in the lower-intensity cohort (157.8, SD = 15.50, Min = 128.62, Max = 179.43, Mdn = 161.73) than the higher-intensity cohort (191.02, SD = 20.95, Min = 162.00, Max = 240.25, Mdn = 188.57), (α=0.05, t(36) = −5.55, p < .001). Examining time in discipline-specific activities, the matched cohorts had significantly different PT intensities (α=00.05, t(36) = −5.49, p < .001), but no significant differences in OT (p = 0.148) or SLP intensities (p = 0.098). The average PT intensity was 44.81 (SD = 13.90, Min = 19.76, Max = 66.10, Mdn = 49.44) in the lower-intensity matched cohort and 65.90 (SD = 9.33, Min = 46.50, Max = 81.83, Mdn = 65.00) in the higher-intensity matched cohort. The mean difference between cohorts was 33.21 min of therapy over LOS (SD = 17.75, Min = 15.38, Max = 81.27, Mdn = 27.17). See Figure 1.
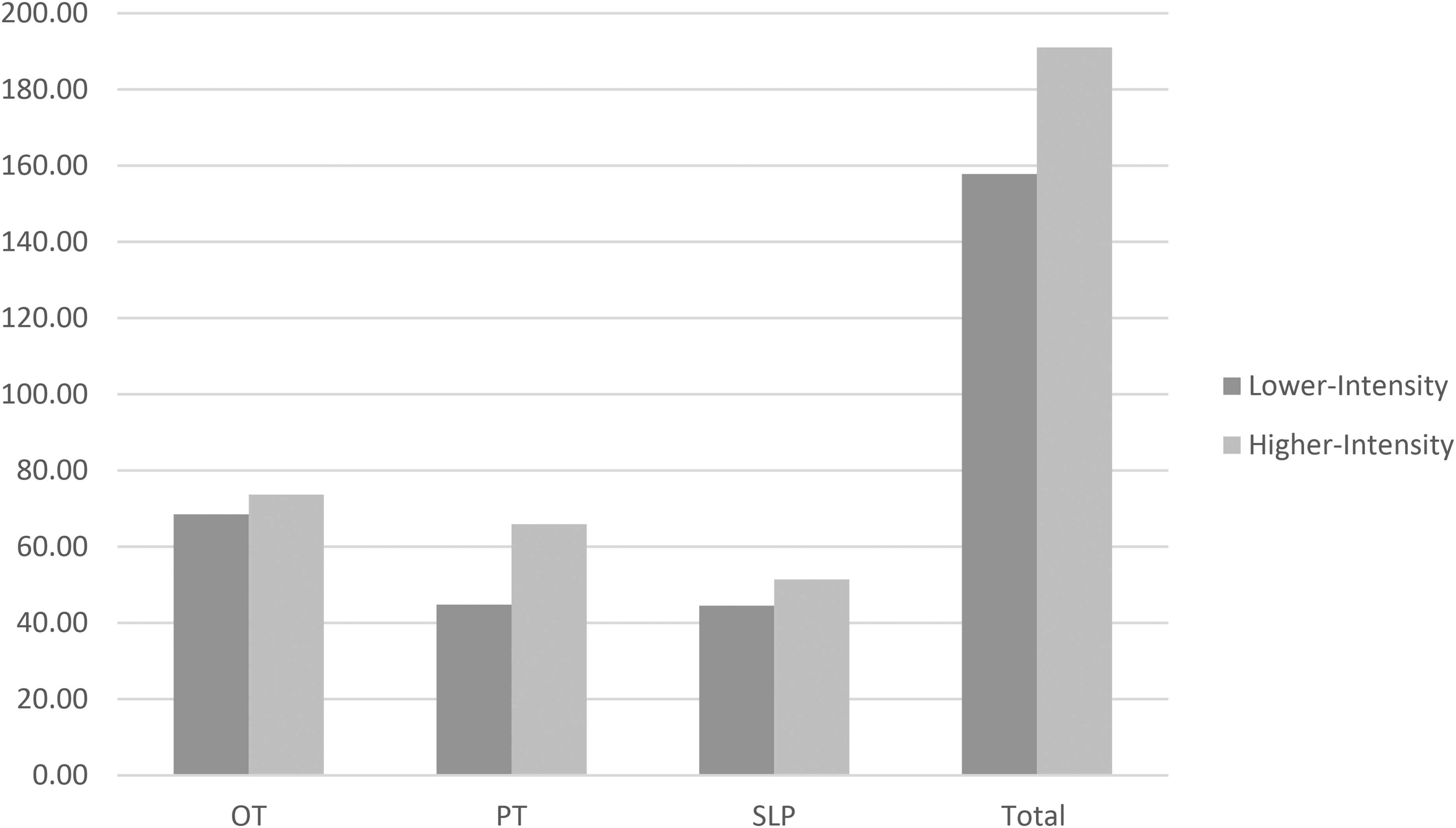
Average intensity by discipline, measurements reported as mean intensity (total number of minutes/length of stay). Abbreviations: SLP, speech-language pathology; PT, physical therapy; OT, occupational therapy.
Primary analysis
WeeFIM efficiency
There were no significant differences in WeeFIM efficiency between the lower-intensity (Mdn = 1.69) and higher-intensity (Mdn = 1.83) matched cohorts via Mann-Whitney U test (α=0.05, U = 146.5, z = −0.99, p = 0.321). Examining the domains of WeeFIM to determine potential differences in efficiency based on total intensity, there was no significant difference in motor (self-care and mobility) (p = 0.397) or cognitive domain efficiencies (p = 0.405). See Table 4.
Functional outcomes.
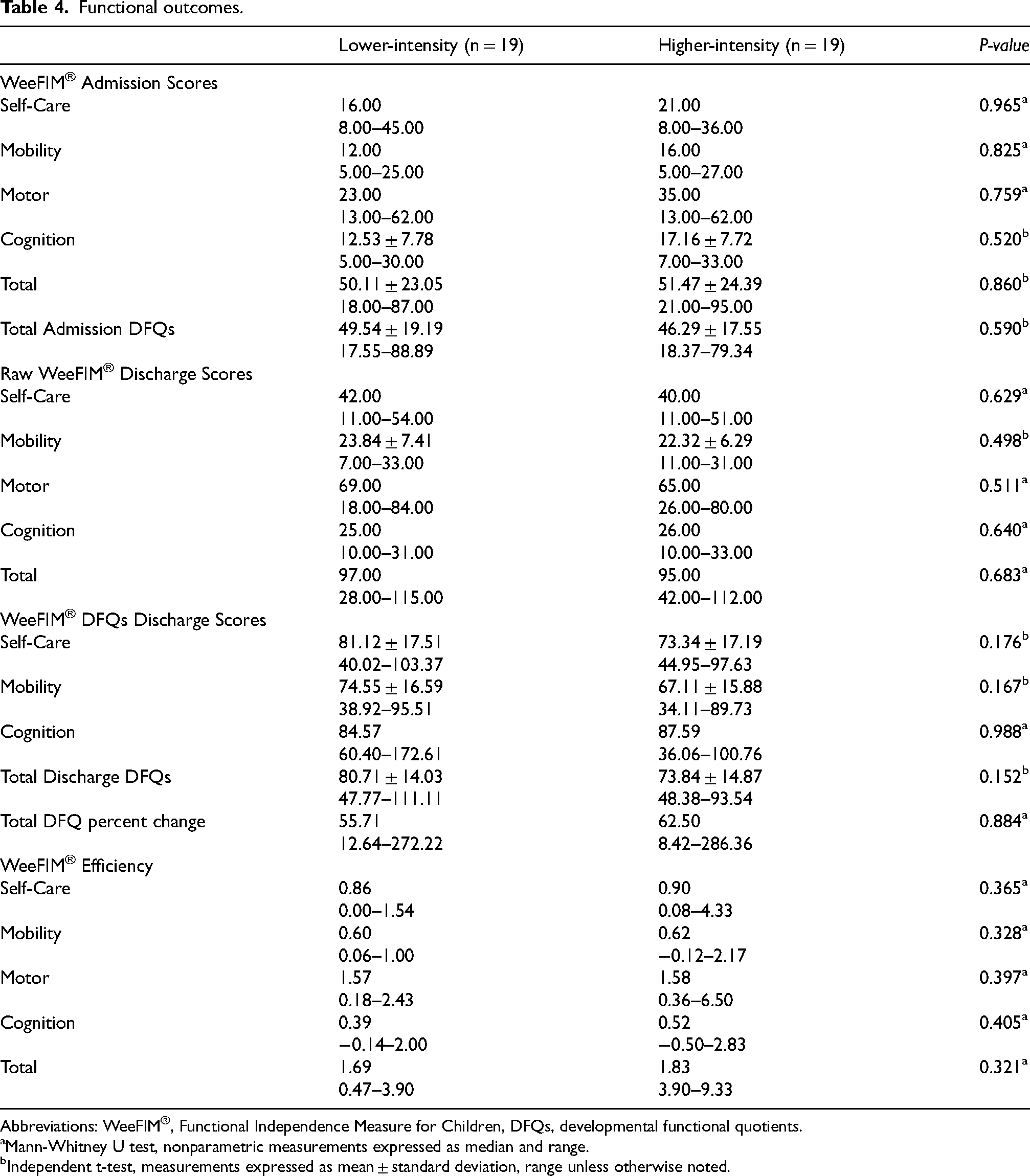

Abbreviations: WeeFIM®, Functional Independence Measure for Children, DFQs, developmental functional quotients.
Mann-Whitney U test, nonparametric measurements expressed as median and range.
Independent t-test, measurements expressed as mean ± standard deviation, range unless otherwise noted.
Discharge functional status (WeeFIM scores and WeeFIM DFQs)
There were no significant differences in raw WeeFIM discharge scores for total score and all domains (self-care, mobility, motor, or cognition) and total DFQs at the time of discharge between the matched cohorts. The total DFQs percent change was also not significant between the matched intensity cohorts for total percent change (α=0.05, U = 185.5, z = −0.15, p = 0.884), self-care, mobility, and cognition domains.
Examining the difference between DFQs at the time of admission and discharge, there was no significant interaction effect (F(1, 36) = 0.67, p = 0.417), indicating the relationship between total admission and total discharge DFQs were not significantly different between matched intensity cohorts. However, there was a significant difference between the total admission DFQs and discharge DFQs for all participants (F(1, 36) = 176.77, p < 0.001), demonstrating significant functional recovery for both cohorts.
LOS
There was no significant difference between matched cohorts for LOS. The mean LOS in the lower-intensity cohort was 20.05 days (SD = 10.17, Min = 7.00, Max = 41.00, Mdn = 19.00); while the higher-intensity cohort's mean LOS was 15.16 (SD = 9.60, Min = 6.00, Max = 36.00, Mdn = 10.00). The results of the linear regression model were not significant for LOS based on total intensity (F(1,36) = 2.21, p = .146, R2 = .06), indicating intensity did not explain a significant proportion of variation in LOS.
Secondary analysis
Discipline-specific analysis
A significant negative correlation was observed between 1) PT intensity and total discharge DFQs (r = −0.41, p = 0.011, 95.00% confidence interval [CI] = [−0.64, −0.10]), and 2) PT intensity and discharge motor DFQs (r = −0.47, p = 0.003, 95.00% CI = [−0.69, −0.18]). Both correlations indicated a moderate effect size. A hierarchical regression analysis was conducted to assess whether the addition of PT intensity to total intensity significantly predicted 1) total discharge DFQs scores and 2) discharge motor DFQs. The initial step of the hierarchical regression was not significant for total intensity and variations in discharge DFQs, controlling for total intensity in regression. The second step was significant for 1) total discharge DFQs (F (1, 35) = 8.20, p = 0.007, ΔR2 = 0.19) and 2) discharge motor DFQs (F (1, 35) = 28.69, p < 0.001, ΔR2 = 0.45), indicating that the consideration of PT intensity explained an additional 18.84% variation in total discharge WeeFIM DFQs and 44.98% variation in discharge motor DFQs. There were no significant relationships found between PT intensity and other functional outcomes, including LOS, or WeeFIM efficiency.
Examining the relationship between OT-specific intensity on functional outcomes, there was a significant positive correlation between OT intensity and total discharge DFQs (r = 0.38, p = 0.019, 95.00% CI = [0.07, 0.62]). The initial step of the hierarchical regression was not significant for total intensity and variations in discharge WeeFIM DFQs (p = 0.603). The second step was significant for OT intensity and discharge WeeFIM DFQs (F(1, 35) = 9.81, p = 0.003,ΔR2 = 0.22), suggesting the addition of OT intensity to the model explained an additional 21.72% variation in the total discharge WeeFIM DFQs. There were no significant relationships found between OT intensity and other functional outcomes, including self-care domain, LOS, or WeeFIM efficiency. See Table 5.
Summary of hierarchical regression analysis for variables predicting functional outcomes.
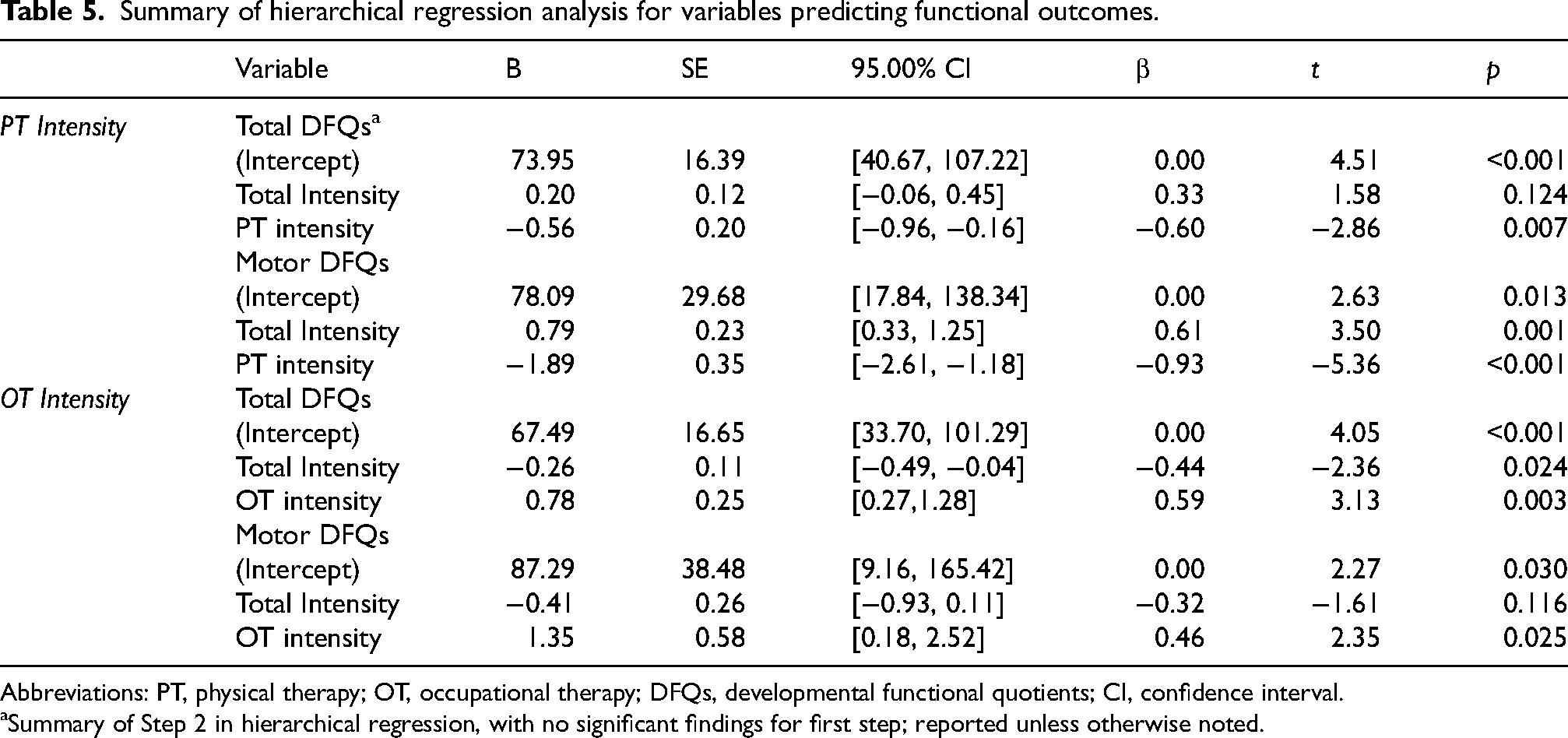
Abbreviations: PT, physical therapy; OT, occupational therapy; DFQs, developmental functional quotients; CI, confidence interval.
Summary of Step 2 in hierarchical regression, with no significant findings for first step; reported unless otherwise noted.
No significant correlations between SLP intensity and functional outcomes were established (SLP and total discharge DFQs [r = 0.24, p = 0.386], SLP and cognition DFQs [r = −0.12, p = 0.469], SLP and LOS [r = −.030,p = 0.070]).
Predictors of functional outcomes with consideration to intensity
Secondary analysis of predictors of functional outcomes included Spearman correlation analysis of admission DFQs; time from injury to admission; LOS; and age in months with matched intensity stratification. Overall, there was a significant negative correlation found between total admission DFQs and LOS (r = −0.61), indicating a large effect size (p < 0.001, 95.00% CI = [−0.78, −0.36]). When examining correlations within matched intensities, total admission WeeFIM DFQs were significantly correlated to LOS with a correlation of −0.58 in the lower-intensity cohort (p = 0.009, 95.00% CI = [−0.82, −0.18]), while the correlation between admission DFQs and LOS in the higher-intensity cohort was −0.73 (p < .001, 95.00% CI = [−.89, −.42]).
Linear regression models were conducted to assess whether admission DFQs significantly predicted LOS in each matched intensity cohort to examine predictive models considering intensity. In the lower-intensity cohort, linear regression models were significant (F(1,17) = 7.08, p = 0.016, R2 = 0.29). Total admission DFQs explained approximately 29.40% of variance in LOS for participants receiving lower intensity. Linear regression models were significant in the higher-intensity cohort regarding admission DFQs and LOS (F(1,17) = 17.89, p < 0.001, R2 = 0.51), indicating 51.27% of variance in LOS was explained by admission DFQs.
Discussion
The study uniquely employed optimal matching to create relatively homogenous groups, enabling a focused examination of the impact of intensity on functional outcomes in children receiving IPR following an ABI. Matching within the study aimed to address confounding variables noted as limitations in previous research, allowing for a more focused analysis of intensity parameters measured by the time spent in therapeutic activities over LOS. The matching process was the first identified in the literature related to intensity and pediatric brain injuries involving matching methodology, including consideration for lesion location, severity, and mechanism.
Overall, there was no significant difference in functional independence between matched intensity cohorts measured by WeeFIM efficiency and changes in WeeFIM DFQs. The lack of global differences in WeeFIM scores between the matched cohorts was consistent with findings in adult brain injury populations.23,49–51 These studies report limitations with the heterogeneity of brain injury diagnosis, intensity allocation, and consideration for between facility variances. However, most studies that did not find statistical differences based on total FIM scores found significant findings regarding recovery rate and significant impacts in motor and cognitive domains of functional independence.
There were statistically significant differences in intensities provided between the matched cohorts for 1) total intensity (OT, PT, and SLP) and 2) PT-specific intensity. While the minutes of therapy provided were diluted due to the division over the entire LOS, the variation in total intensity was approximately 33.21 min per day between the cohorts, with the lower-intensity cohort receiving around 83% of the intensity of the higher cohort. The difference in PT intensity was 21.09 min per day, accounting for the majority of the overall variation between total intensities. Both cohorts had higher OT intensities compared to PT or SLP intensities. While the intensity variation in the study may not reflect the level of intensity required to significantly impact functional outcomes, it does reflect feasible changes within the current rehabilitation structure, especially regarding the impact of discipline-specific intensities.
The significant negative correlation between (1) PT intensity and total discharge DFQs and (2) PT intensity and discharge motor DFQs counterintuitively suggests increases in PT intensity result in a decrease in discharge DFQ scores. These findings are inconsistent with the literature regarding time in PT and functional outcomes in brain injury populations, with PT intensity significantly relating to mobility or motor changes during IPR for pediatric TBI populations.52,53 However, PT intensity was weakly correlated (r = 0.11, p > 0.05) to motor outcomes following IPR in adult populations. 54 Additionally, evidence suggests time spent in basic or complex PT activities is not significantly associated with either cognitive or motor outcomes. 55 The inability to determine variations in complexity or consistency of interventions represents a limitation of the study, as these factors may have influenced outcomes.
Using hierarchical regressions allowed the isolation of PT intensity, controlling for total intensity on DFQs, indicating 44.98% of variance in the motor DFQ is explained by PT intensity. Clinically, the relationship between PT intensity and discharge DFQs is likely the result of individualized treatment planning, with the rehabilitation team adapting to the lack of functional progress by increasing time in PT. While the admission WeeFIM scores were part of the matching to aid in controlling functional status between groups, the individualized recovery trajectory, including individualized treatment planning and individualized dosage considerations, was not controlled in this study. These findings highlight the potential impact of rehabilitation trajectory, including individualized recovery rate, and rehabilitation intensity variations, warranting further investigation.
OT intensity accounted for an additional 21.72% variation in the total discharge DFQs, while controlling total intensity. The significant positive correlation between OT intensity and discharge DFQs suggests that more time in OT interventions significantly impacts functional independence at the time of discharge, consistent with previous findings for OT intensity.10,24,55 Based on the study's sample, an additional one-unit increase in OT intensity increased the total DFQs by around one point on average (0.78 units). These findings indicate a need to consider quality and type of interventions over quantity. Time in OT interventions significantly impacted functional outcomes more than total intensity, PT-specific, or SLP-specific intensities. Evidence suggests that more time spent in complex OT activities than basic OT interventions is significantly associated with better motor scores. 55 Additionally, participation in contextualized interventions, a key aspect of intensity, resulted in greater functional outcomes, specifically self-care and mobility at the time of discharge from IPR following TBI. 56 The findings from this study and supporting literature highlight the impact of occupational-based, contextualized interventions. While the current study did not examine therapeutic interventions directly, the scope of OT is occupation-based with client-centered goals and key considerations for client factors, context, and environment. 57 Time spent in real-life, functional activities is a critical aspect of occupation-based interventions, including activities of daily living, and may contribute to functional recovery compared to decontextualized therapy. Additionally, the WeeFIM is weighted in self-care, occupation-based constructs. Future investigation into functional-based, contextualized interventions associated with intensity as a predictor of functional outcomes is needed to determine rehabilitation efficacy. Additionally, consideration of other parameters of dosage, including type of therapy, need to be considered in future research.
While there was no significant difference from admission to discharge WeeFIM DFQs based on intensity, there was a significant difference between admission and discharge functional outcomes for all participants, depicting a significant recovery for all participants following rehabilitation at a pediatric-specialty, CARF-accredited facility. The improvement of all participants highlights the value of IPR and is consistent with the literature regarding pediatric brain injuries and IPR.6,9,33,58 This finding aligns with the emerging evidence regarding quality over quantity of therapy. Literature indicates that quality indicators, including specialized pediatric training, pediatric-specific equipment, and rehabilitation structure impact functional outcomes.6,8,59,60 The lack of significant differences during IPR based on intensity suggests the parameters for intensity may need to be greater than the average 33.21 min for this study to establish a clinically significant intensity difference. Additional consideration of quality indicators at specialized pediatric rehabilitation centers needs to be addressed in future research. Additionally, future investigation should address consistent delivery of interventions across providers, as variations in therapeutic approach, experience, and adherence to treatment protocols may influence functional outcomes.
Intensity did not explain a significant proportion of variation in LOS (p = 0.136), which is consistent with the literature.11,19,23,49 However, insufficient power for LOS cannot be excluded, indicating the potential impact of intensity on LOS in future studies. While not statistically significant, a four-day reduced LOS (25%) does have substantial clinical and financial considerations. A four-day reduction in LOS could significantly benefit families across diverse socioeconomic backgrounds, by alleviating the financial burden associated with hospitalization, supporting a faster return to routine life, and reducing other indirect costs such as parental return to work. From a staffing perspective, the decrease in LOS in the higher-intensity cohort endorses the feasibility of implementing higher intensity, with the total staffing demands higher in the lower-intensity cohort. The outcomes demonstrated that higher intensity may be a viable and efficient approach for optimizing rehabilitation within a shorter timeframe.
Examining predictors of functional outcomes with consideration to intensity, admission DFQs were significantly correlated with LOS based on matched cohorts. Admission DFQs in the higher-intensity cohort accounted for 51.27% variance in LOS, indicating a clinically significant relationship, while admission DFQs only explained 29.40% of the variance in LOS in those receiving lower intensity levels. Therefore, admission DFQs were predictive of LOS, with admission DFQs predicting a clinically meaningful variance in LOS for those individuals receiving higher amounts of therapy compared to the lower-intensity cohort. Further investigation into the relationship between dosage and functional outcome predictors is needed.
These findings suggest the critical need for continued investigation into the impact of neurorehabilitation following ABIs in pediatric populations, including intensity, as one parameter of dosage, with increased attention to complexity, type, and focus of interventions. This study was one of the first identified to create diagnostic and functionally homogenous matches, considering the impact of heterogeneity of brain injuries on functional recovery. As with previous research, the study has limitations with the complexity of multidisciplinary rehabilitation and dosage parameters, impacting the generalizability of findings. However, the study does provide evidence for the need for continued investigation with additional considerations for study design and statistical analysis. Rehabilitation effectiveness and efficacy following pediatric brain injuries need further investigation, including considerations for more significant differences in intensity parameters. Additionally, the findings from this study suggest a need to identify quality indicators that could impact functional recovery aside from dosage.
Limitations
This study was conducted in a clinical setting as a matched cohort study, which introduces inherent limitations to the methodology. While the optimal matching created near homogenous cohorts, it also excluded a large number from the initial enrollment (n = 43), creating a small sample (n = 38). The small sample size, as well as the use of one facility, limits the generalizability of the findings. Another limitation was the variability in discipline-specific intensity within the clinical setting. Individualized goals and interventions influenced the ethical delivery of service intensity, impacting conclusions. The study did not consider the type or complexity of activities during interventions, limiting the prediction of discipline-specific activities. The lack of minimal clinically important difference (MCID) for the WeeFIM measurement limited reporting of clinically significant findings. Another limitation was the use of minutes in therapy as a definition for intensity, as emerging evidence suggests that time may not be the most robust intensity measurement. Future studies utilizing the WeeFIM should consider establishing inter-rater reliability during joint therapy sessions across multiple timepoints, in addition to assuring all providers are WeeFIM credentialed. Data collection was restricted to billable services (OT, PT, and SLP), limiting the impact of additional rehabilitation services such as neuropsychology, recreational therapy, or art therapy on functional outcomes.
Conclusion
All participants in the study demonstrated significant gains in functional outcomes from the time of admission to discharge. These significant gains in DFQs were not isolated to intensity, as measured as time in therapy over LOS, indicating the impact in functional recovery may be related to the quality indicators of the IPR facility, the type or complexity of interventions, or participant's effort during IPR. OT intensity, or duration of time spent in OT over LOS, did significantly predict variations in functional independence at discharge from IPR as measured by discharge WeeFIM DFQs. Future research should investigate a broader range of intervention intensities, including low, moderate, and high levels, to better understand intensity's impact on functional outcomes. Occupation-based, functional interventions and cognitive-specific interventions regarding intensity should be further investigated. Other aspects of dosage, including the complexity and type of interventions, should be considered in future research to guide evidence-based practice effectively.
Footnotes
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
