Abstract
Purpose:
Sports-related concussion (SRC) cases have increased among children in the last decade. Differences in concussion symptoms, presentation, and follow-up care exist when comparing demographics. The aim of this study was to explore SRC within the pediatric population.
Methods:
A retrospective chart review of patients ≤18 years old diagnosed with SRC at a New Orleans stand-alone children's hospital from January 2007 to December 2021 was performed. T-test and Fisher's exact test were used for relationship between outcomes and sports, demographics, setting, insurance, and follow-up care.
Results:
Children who sustained SRC at practice were more likely to be male (p = 0.0311) and younger (p < 0.0001). Cheerleading was more likely to have injuries during practice (p < 0.0001). Medicaid/uninsured patients were more likely to be referred from the emergency department (ED) (p = 0.001), have longer length of follow-ups (p = 0.0489), and have more missed appointments (p = 0.0062). However, the total number of follow-ups between insurance types did not differ (p = 0.3084).
Conclusion:
SRC incidence is situation and time dependent. Medicaid/uninsured patients are more likely to be evaluated at the ED, miss appointments, and have a longer length of follow-up to attain the same number of appointments. Exploring the nuances of SRC within this population will improve management and outcomes.
Introduction
Sports-related concussions (SRC) in the pediatric population have become a topic of unique interest in the last decade as participation in sports has increased drastically. SRC are defined as mild traumatic brain injury (TBI) during athletics resulting in the onset of neurological impairments and a constellation of symptoms such as headache, nausea, vomiting, dizziness, confusion, and lethargy. 1 Concussions account for approximately 75% of all pediatric TBIs, with SRC accounting for 65% of pediatric concussions. 2 In the United States, over 44 million children participate annually in sports with an estimated 1.6 to 3.8 million suffering SRC. 1 With the rise in sports participation among youth, it has become imperative to dissect the pathophysiology of the condition and potential outcomes for this population.
When comparing concussion presentation and post-concussion care, previous studies have revealed differences among demographic groups. Zuckerman et al. found that individuals with private insurance had more missed days of school post-concussion when compared with those having public insurance. 3 Other studies revealed that females remained symptomatic for longer periods of time when compared to their male counterparts.4–6 Reasons for this are unknown but could be due to females having greater basal rate of glucose metabolism. 7 Moreover, disparities in presentation and follow-up care have been found among pediatric patients who are publicly insured and self-identify as Black.8,9 Pate et al. revealed that Black and/or publicly insured patients were more likely to initially present at the emergency department (ED), while White and/or privately insured patients were more likely to present at the concussion clinic. 9
The aim of this study was to stratify the incidence and follow-up of SRC within the pediatric population by type of sport, time of year, setting (i.e., practice or in-game), initial presentation location (i.e., ED or clinic), insurance type, and sociodemographic characteristics. The authors hypothesized that there would be significant differences in temporal and situational injury patterns in pediatric patients with SRC. Significant differences in SRC incidence and follow-up were also predicted when grouping by initial presentation location, insurance type, and sociodemographic. Exploring the nuances of SRC within this population could help design a plan for efficient allocation of resources. This would potentially address the influx of children with SRC and identify disparities among certain demographic groups, improving management and outcomes for these populations.
Methods
A retrospective chart review of patients younger than 18 years old who were diagnosed with SRC at a New Orleans stand-alone children's hospital from January 2007 to December 2021 was performed. Demographics (age, sex, race), sports played, setting (practice or in-game) of SRC, location (clinic or ED) of initial presentation, insurance type (Medicaid/uninsured, private), number of follow-ups, date of initial presentation, and date of last follow-up visit were collected. Patients older than 18 years, with TBI from non-sports activities, with more severe TBI including hemorrhage or seizures, and with incomplete medical records were excluded. Data was analyzed with t-test and Fisher's exact to compare outcomes between sports, demographics, setting, insurance types, and follow-up care.
Results
Temporal and situational differences in SRC
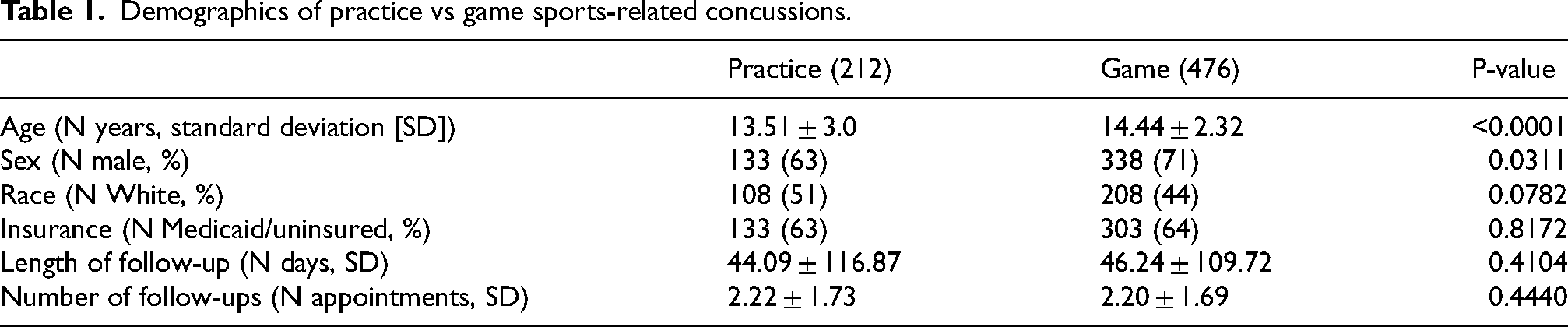
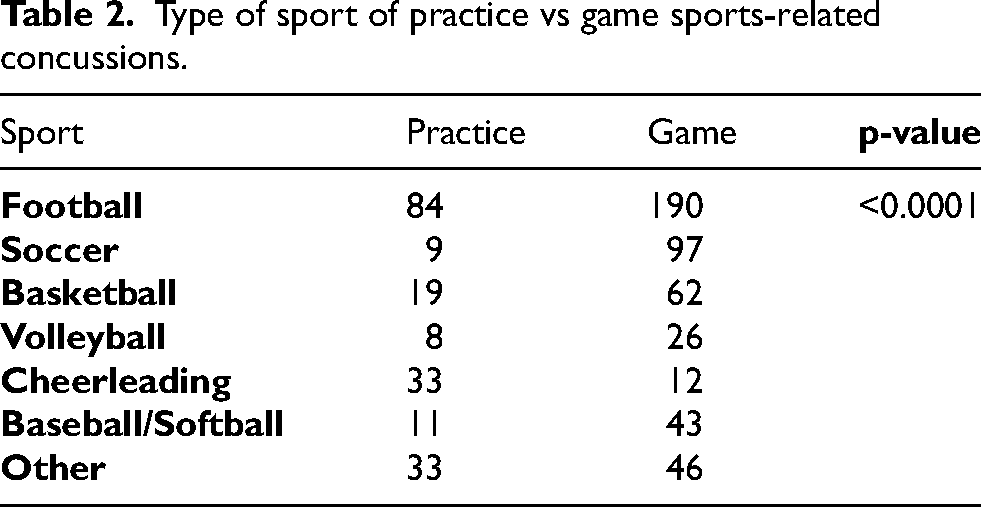
Six hundred and eighty-eight patient charts had information regarding the situation under which they sustained SRC. SRC incidence among all sports followed the timing of their respective seasons (Figure 1). Football was associated with the most concussions (Figure 2) and had the largest incidence during the fall months (Figure 1). The sport with the second highest incidence of concussion was soccer, followed by basketball, volleyball, cheerleading, and baseball/softball (Figure 2). Children who sustained SRC at practice were more likely to be male (p = 0.0311) and younger than those who sustained SRC during competition (13.51 ± 3.0 vs 14.44 ± 2.32 years, p < 0.0001) (Table 1). Additionally, most SRC occurred during competition; however, cheerleading was more likely to have SRC during practice (p < 0.0001) (Table 2).
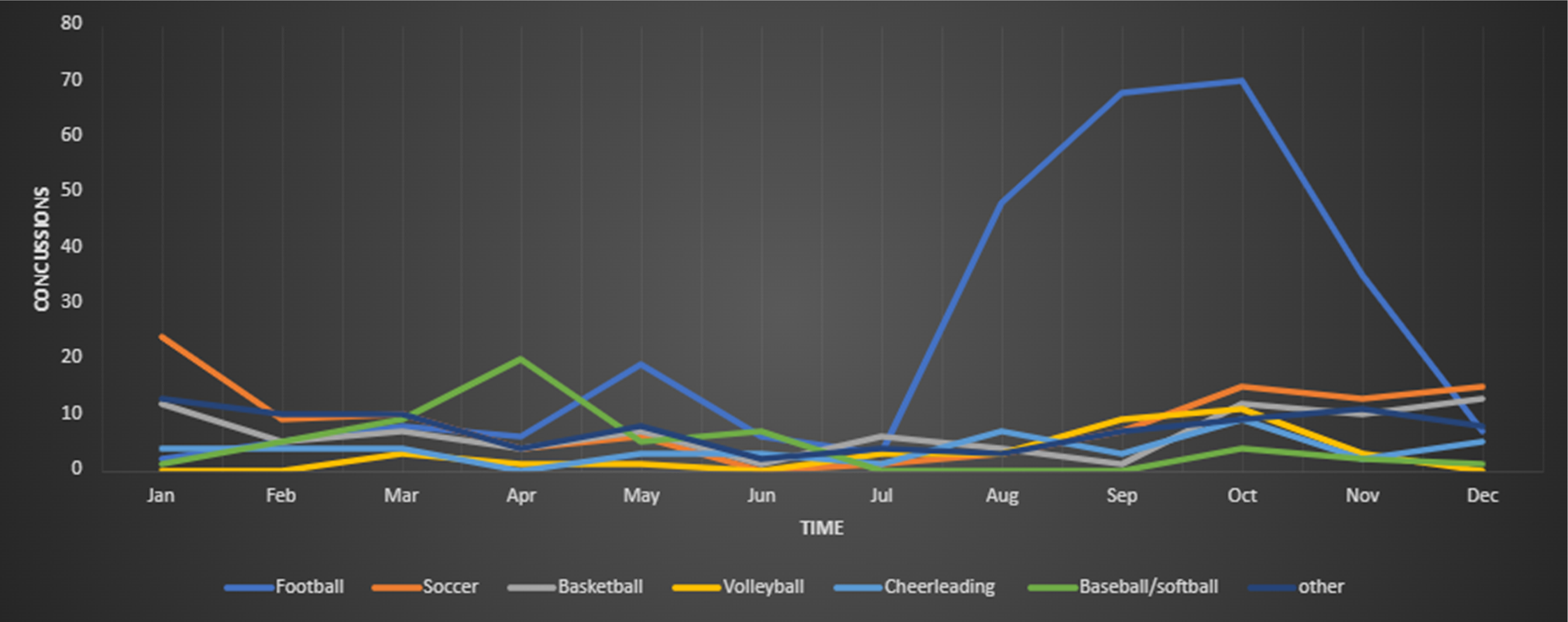
Temporal distribution (by month) of concussions by sport.
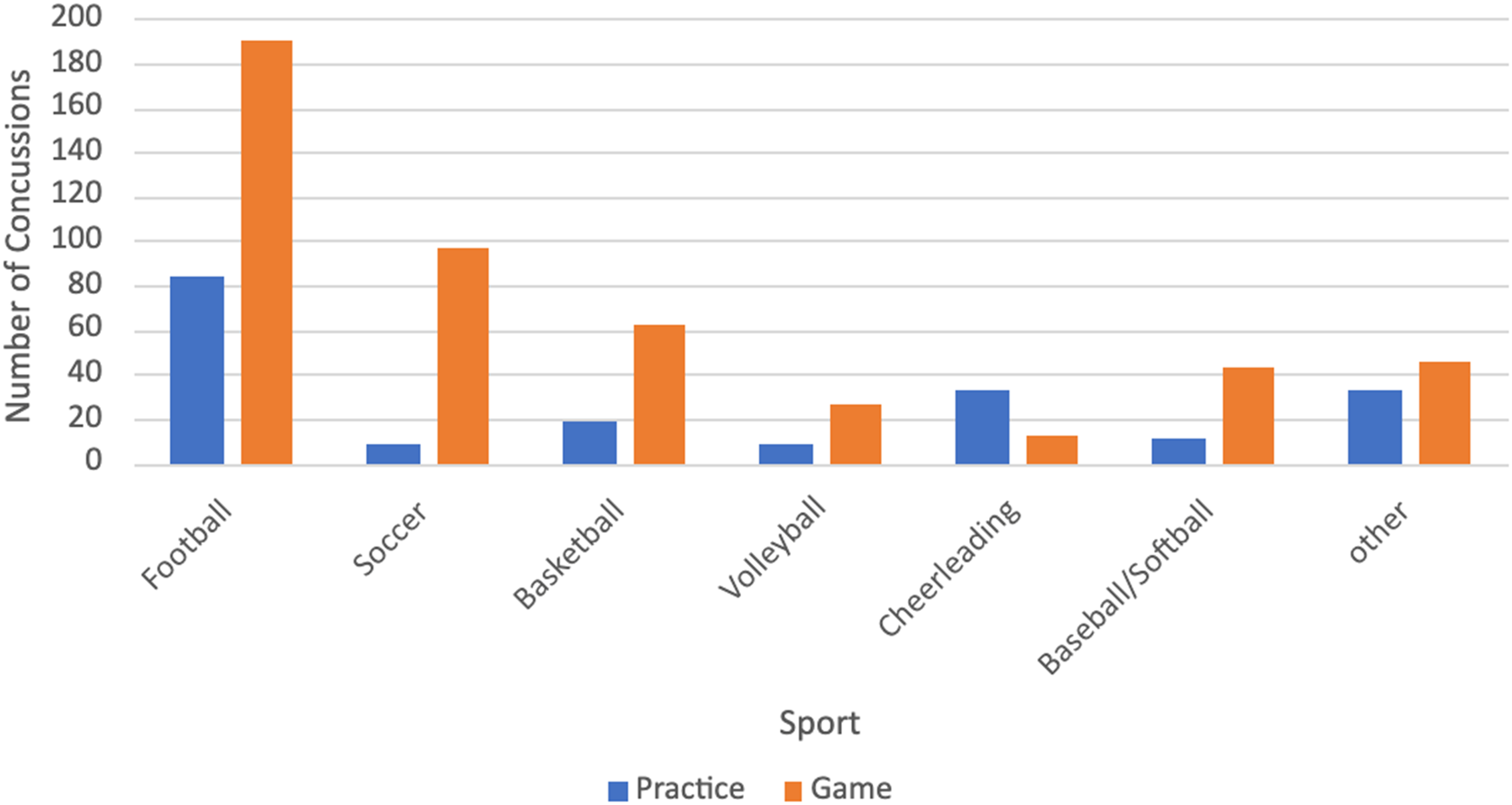
Sports-related concussions incidence in practice vs in game by sport.
Demographics of practice vs game sports-related concussions.

Type of sport of practice vs game sports-related concussions.
Initial presentation location and follow-up rates based on insurance status
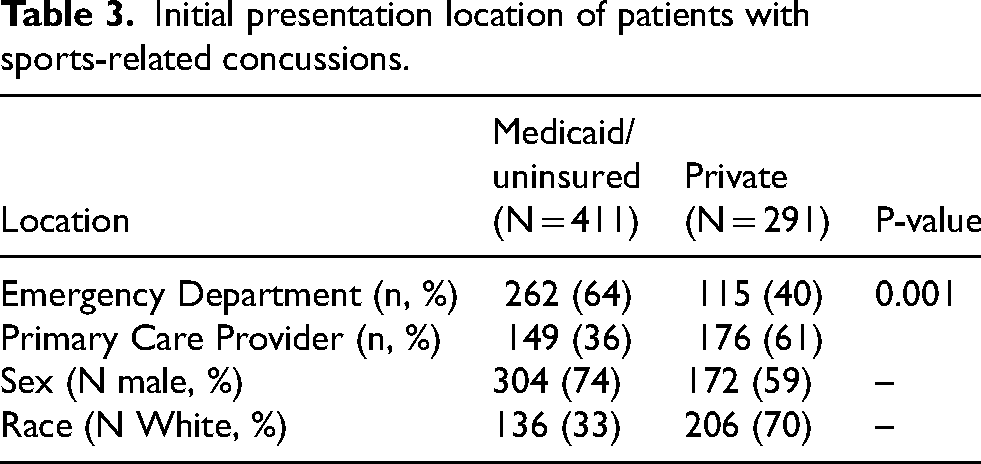
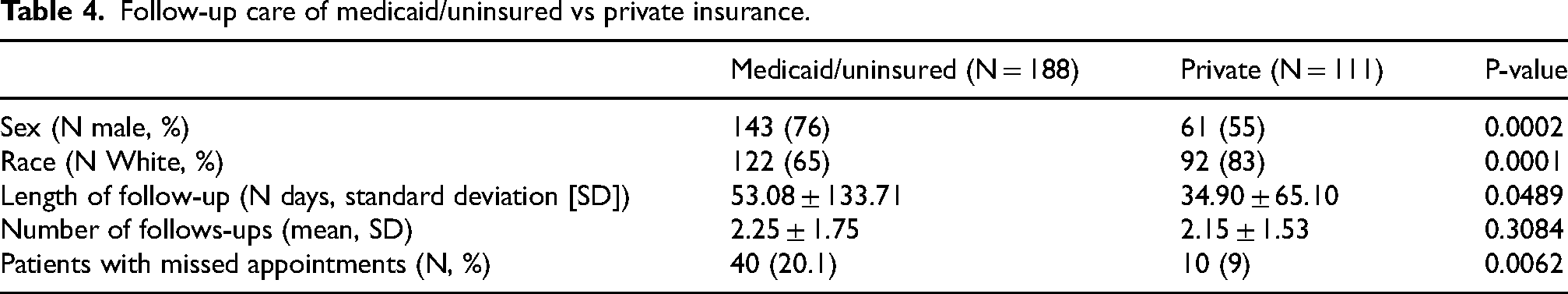
Seven hundred and eight patients with information regarding referral and follow-up were included. Four hundred and seventeen had Medicaid or were uninsured and two hundred ninety-one had private insurance. At initial presentation, 74% of Medicaid/uninsured patients were male as compared to 59% of privately insured patients, and 33% of Medicaid/uninsured patients were White, as compared to 70% of privately insured patients (Table 3). Medicaid/uninsured patients were more likely to be referred from the ED (63.7% vs 39.5%, p = 0.001) (Table 3). Of the two hundred ninety-nine children who were seen in follow-up, Medicaid/uninsured patients were more likely to be male (76% vs 61%, p = 0.0002) and less likely to be White, with the percentage of White patients being 65% vs 83% (p = 0.0001) in Medicaid/uninsured vs private, respectively. Medicaid/uninsured patients also had a longer length of follow-up (53.08 ± 133.71 vs 34.90 ± 65.10 days, p = 0.0489) and more missed appointments (20.1% vs 9%, p = 0.0062). However, the total number of follow-ups between insurance types did not differ (2.25 ± 1.75 vs 2.15 ± 1.53, p = 0.3084) (Table 4).
Initial presentation location of patients with sports-related concussions.

Follow-up care of medicaid/uninsured vs private insurance.

Discussion
In this study, the incidence and follow-up care of SRC in the pediatric population was explored. SRC incidence among children has steadily increased over the last decade 1 ; therefore, it is imperative to dissect the nuances of the condition to improve education on prevention, symptomology, and treatment in those most susceptible populations.
Temporal and situational differences of SRC
When looking at the temporal distribution, SRC incidence followed each sport's season in the region (Figure 1). Football and cheerleading SRC were more prevalent in the fall semester, while soccer-related SRC peaked toward the winter months, and baseball SRC increased in the spring semester. This follows the trends of school-associated athletics in the region. In agreement with previous studies,10–12 football was the sport with the most concussions in this cohort, but it is unclear from this data if football is more dangerous than other sports or if more children play football in this cohort. The data also suggest that in most of the sports, concussions occurred during in-game settings instead of during practice. Marar et al. found similar results while looking at nationally dispersed US high school data from 2008–2012. 10 In contrast, supported by Zachery et al., 13 the data revealed that concussions during cheerleading were more prevalent during practice than in-game settings. These concussion rates could be explained by the repetitive nature of cheerleading practice or the process of learning of new routines compared to competition.
Moreover, in the current study's patient cohort, children who sustained SRC at practice were more likely to be younger and male than those who sustained SRC during competition. These findings follow published trends, 14 which have identified that there is an increase in concussion incidence during practice at the high school level when compared to the collegiate level. Interestingly, in this cohort, males were more likely to sustain SRC, in contrast with current literature which suggests that females have a greater propensity toward SRC. However, to the authors’ knowledge, previous studies have not examined differences in incidence of SRC when controlling for both gender and setting.
Referral source for concussion follow-up
Regardless of complaint, the number of Medicaid/uninsured patients presenting to the ED continues to increase while the number of privately insured patients decreases every year. 2 Similar trends were seen in the pediatric patient population that was studied here. Medicaid/uninsured patients were more likely to present to the ED for concussion care, whereas privately insured patients were often evaluated by their primary care provider (PCP). Whether a patient with a concussion presents to the ED or to their PCP, the care plan remains the same and for many patients it does not require emergent treatment. Both sets of patients received the same questioning and were discharged home with the same precautions and referral for follow-up in the multispecialty concussion clinic. The greater number of patients presenting to the ED may reflect social disparity and lack of access to consistent healthcare; however, it may also illustrate a gap in public health literacy on diagnosis and management of concussions.
Follow-up care of SRC
Lack of adherence to concussion care recommendations has been shown to prolong recovery times and worsen outcomes. 2 Disparities in follow-up care have been shown particularly among pediatric patients who are publicly insured and identify as Black. 15 However, limited data was present on the effect of socioeconomic status on follow-up concussion care. Specifically, it is not clear whether a discrepancy in follow-up care is due to missed follow-up visits by the patient or decreased number of follow-ups scheduled by the provider. 3 In terms of demographics, the data revealed similar findings as Medicaid/uninsured patients were less likely to be White. Medicaid/uninsured patients were found to have a longer length of follow-up even though their total number of follow-up appointments was the same on average as privately insured patients. This difference may be due to the increased number of missed appointments by Medicaid/uninsured patients which lengthened the follow-up period. These missed appointments may be attributed to known causes of health disparities such as access to adequate transportation and resources. 3
Limitations
There are several limitations to this study. It was a retrospective review, and no patients were contacted. Therefore, this study could not determine reasons why patients initially presented to the ED or what contributed as barriers to follow-up care. Implementation of a standardized questionnaire at the initial multidisciplinary visit would help to obtain this information for future studies. Although this center is one of a few comprehensive multidisciplinary concussion clinics for children and adolescents in the region, this study did not capture the entire population, nor does it explore how many children sustain SRC but do not seek medical care. Since the study only examined patients at this single institution, it was unable to address SRC patterns on a city, region, or statewide basis.
Future directions include a needs assessment of the current practice pattern to better address any gaps in current care that contribute to sequelae of SRC. Additionally, partnering with local high school athletic program associations to address SRC prevention and treatment at the state level can lead to policy and system changes to benefit young athletes.
Conclusions
SRC incidence is situation and time dependent. Medicaid/uninsured patients are more likely to utilize the ED for SRC evaluation and are more likely to miss appointments and have longer length of follow-up to attain the same number of appointments. Studying the intricacies of concussion incidence, presentation, and diagnosis can provide insight into expanding community, school-based, and parent education on SRC. Moreover, healthcare institutions can optimize resource utilization and improve ease of referral for multidisciplinary follow-up care.
Footnotes
Ethical considerations
Institutional Review Board approval was sought and received for this project. Approved in July 2022 with exempt status. No informed consent was obtained.
Author contributions
J.A.C.A., S.K., H.M., E.C. performed literature review, data design and extraction, analysis, and drafting of manuscript. A.S., S.S., and L.E. provided guidance on study design and critical review of manuscripts. J.A.Z. provided study concepts, analysis and data interpretation, and critical revisions.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
