Abstract
Purpose:
The aim was to evaluate which clinical and radiographic variables are independent (true) risk factors for hip subluxation in nonambulatory children below 5 years of age with cerebral palsy.
Methods:
Patients were recruited from a population-based hip surveillance program. Inclusion criteria were birth during 2002–2006, age below 5 years, and gross motor function classification system levels III–V. In all, 121 children (71 boys) met these criteria. Gross motor function classification system was level III in 29 patients, level IV in 28, and level V in 64. Anteroposterior radiographs at diagnosis and during follow-up were assessed, and only the worst hip of each patient was used for the analyses. The mean age at the initial radiograph was 2.5 years (range: 0.7–4.9 years), and the mean follow-up time was 4.0 years (range: 0.5–11.8 years).
Results:
At the last follow-up, 67 children had a clinically significant hip displacement, defined as migration percentage ≥40%. Univariable regression analysis defined these risk factors: gross motor function classification system level V, spastic bilateral cerebral palsy, initial migration percentage, yearly rate of migration percentage progression, and initial acetabular index. When these variables were analyzed with multivariable regression in 107 patients with initial migration percentage <50% and follow-up ≥1.0 year, the independent risk factors were initial migration percentage (p = 0.003) and yearly rate of migration percentage progression (p < 0.001).
Conclusion:
The parameters that need to be assessed in hip surveillance in children below 5 years of age are initial migration percentage and rate of migration percentage progression. Acetabular index and femoral head–shaft angle might be useful later for decision-making regarding choice of treatment.
Level of evidence:
Level II, development of diagnostic criteria.
Introduction
Nonambulatory children with cerebral palsy (CP) have an increased risk of hip displacement that over time can lead to complete dislocation, deformities, and pain.1–3 Therefore, surveillance programs for early detection and management have been developed.4,5 A proper surveillance can provide early surgical treatment and ultimately lead to better outcomes than those of neglected dislocations. 6 The children should be enrolled in the screening program as soon as the diagnosis of CP has been established, usually at an age of 1–2 years.4,7
Reliable predictors of subluxation are important for surveillance and treatment. Previous studies have shown a clear relationship between impaired motor function as determined by gross motor function classification system 8 (GMFCS) and progression of hip displacement.5,6 Reduced femoral head coverage, measured as increased migration percentage (MP), predisposes to increasing subluxation if left untreated.7,9,10 There is, however, no consensus regarding other radiographic variables. Valgus position of the proximal femur is a common deformity in children with CP, and a high femoral head–shaft angle (HSA) has been reported to be a predictor of hip displacement.11,12 However, others found no significant association between initial HSA and later subluxation in children below the age of 5 years. 13 A dysplastic acetabulum with an increased acetabular index (AI) is often seen in hips with subluxation, but the prognostic value in small children is controversial.10,14 Thus, in order to improve hip surveillance, further research is needed. Since the variables may be interdependent and since hip displacement occurs early in life, multivariable analysis is required to find the independent (true) risk factors. We have found only one previous study with this approach, but not all potential predictors were analyzed. 15
The purpose of this longitudinal, population-based study was to analyze which clinical and radiographic parameters are independent risk factors for hip displacement in nonambulatory children during the first years of life. We think such data could be relevant for modification and improvement of existing surveillance programs.
Patients and methods
The patients were recruited from our population-based surveillance program for children with CP. The inclusion criteria were as follows: children with bilateral CP born during the 5-year period 2002–2006, GMFCS levels III–V, and age at diagnosis below 5 years. All the 121 children (71 boys and 50 girls) who met these criteria were included in the study. The mean age at the initial pelvic radiograph was 2.5 years (range: 0.7–4.9 years). GMFCS levels and type of CP were determined by physiotherapists and neuropaediatricians. GMFCS distribution was level III in 29 patients, level IV in 28, and level V in 64 patients. The type of CP was spastic bilateral in 93 patients (quadriplegia in 58 and diplegia in 35 patients), dyskinesia in 26 patients, and uncertain type in 2 patients; 49 of the 58 patients (84%) with spastic quadriplegia were at GMFCS level V, showing the strong association between CP type and gross motor function.
Radiographic measurements
An anteroposterior (AP) radiograph of the pelvis was taken at the time of diagnosis and yearly during follow-up. The radiographic measurements were performed by one of the authors (T.T.), who is a pediatric orthopedic surgeon with long experience in assessment of hip radiographs in children. The radiographic approach and the measurements of MP 9 and HSA 11 were similar to those in our earlier report 13 and are shown in Figure 1. AI is the slope of the acetabular roof, which is the angle between the line through the medial and lateral edges of the acetabular roof and Hilgenreiner’s line. 16 In patients who had been operated for hip displacement, the last preoperative radiograph was used for the last (final) radiographic measurements. Patients who had not undergone surgical treatment were followed until the last available radiograph in our radiographic archive.
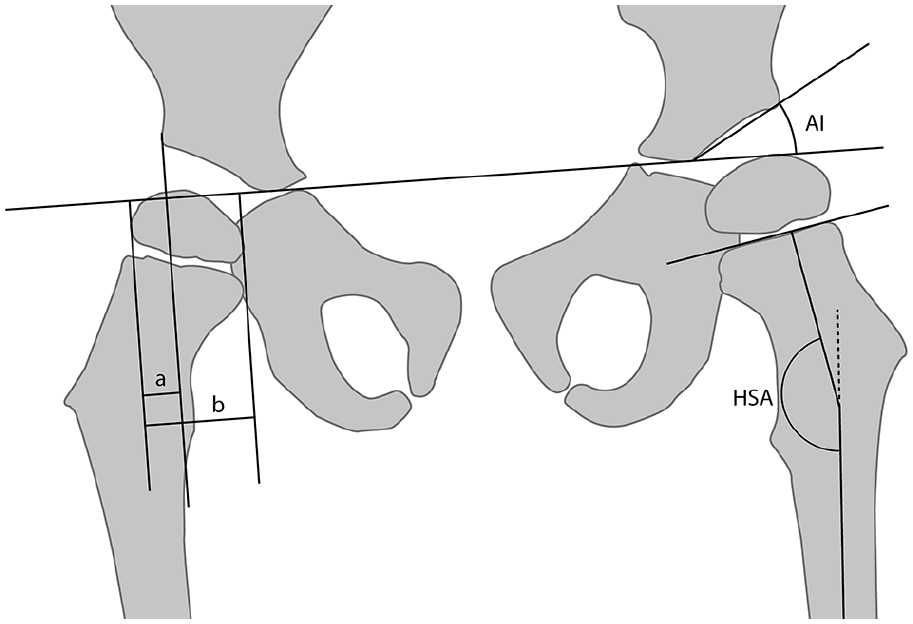
Schematic drawing showing the radiographic measurements. Migration percentage (MP; shown in the right hip) is the percentage of distance a to distance b (a/b × 100). Acetabular index (AI) is the slope of the acetabular roof, as indicated in the left hip. The head–shaft angle (HSA) is the medial angle between a line perpendicular to the proximal femoral physis and a line through the middle of the femoral shaft.
Statistics
SPSS (version 26) was used for the statistical analysis (IBM, Armonk, New York). Continuous variables were analyzed with Student’s t tests for independent samples and paired samples. Correlation between parameters was evaluated by Pearson’s correlation coefficient (r). In order to avoid the statistical problem of bilaterality since the hips of the two sides are not independent of each other, only the worst hip of each patient (the hip with the largest MP at the last radiograph) was used for the analysis. Since an MP > 40% is usually considered an indication for surgical correction in order to restore femoral head coverage,17,18 this MP value was chosen as cutoff for clinically relevant hip subluxation. Potential risk factors for MP ≥ 40% at the last radiograph were first analyzed with univariable binary logistic regression. Variables with a p value <0.1 were then analyzed with multivariable logistic regression. Differences were considered significant when the p value was <0.05.
Results
The mean MP at the initial radiographic examination was 24.1% (SD: 20.4%). The mean follow-up time was 4.0 years (range: 0.5–11.8 years) and the mean patient age at the last radiograph was 6.5 years (range: 2.1–13.8 years). At the last follow-up, the mean MP was 46.0% (SD: 25.4%), and 67 patients (55%) had clinically relevant hip displacement (MP ≥ 40%). The last AI was larger in patients with last MP ≥ 40% than in those with lower MP (27.6° and 18.2°, respectively; p < 0.001), and the same applied to the last HSA (171.3° vs 167.4°; p = 0.018).
Progression per year in MP was analyzed in 107 patients with initial MP < 50% and follow-up time ≥1.0 years. The mean MP progression was 6.5% per year (SD: 7.6%), with increasing rates with more severe functional level (2.2% per year at GMFCS level III, 4.7% at level IV, and 9.3% at level V; Figures 2 and 3). Yearly progression was greater in children who had MP ≥ 40% at the last radiograph than in those with MP < 40% (10.8% vs 2.2%; p < 0.001). Children who underwent hip operations had shorter mean follow-up than nonoperated patients (3.5 years vs 5.0 years; p < 0.001) because follow-up ended with the last preoperative radiograph in the former group as opposed to continued follow-up in the latter group. MP progression rate was larger in operated than in nonoperated patients (10.4% vs 2.3% per year; p < 0.001).
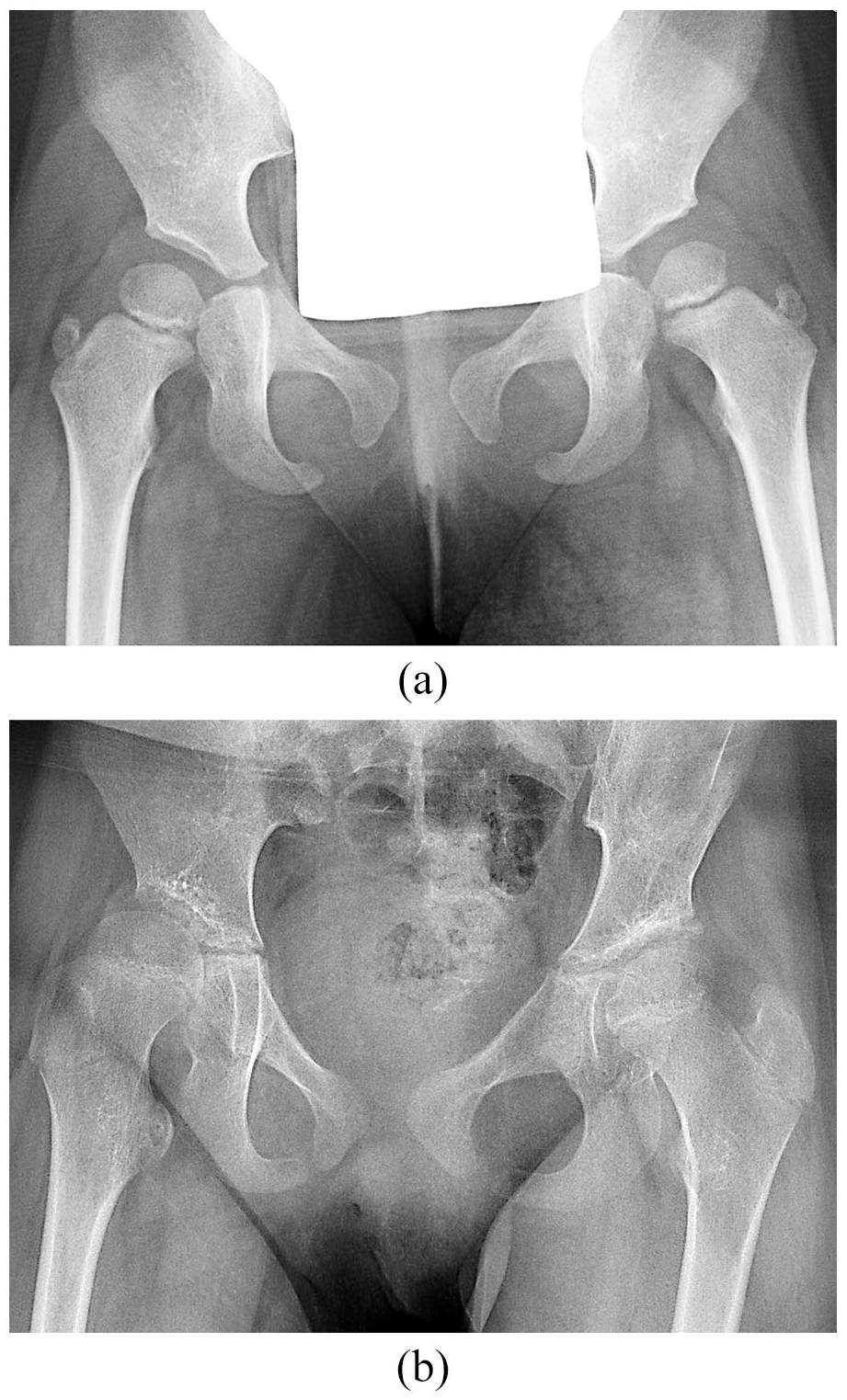
Radiographs of a girl with spastic diplegia, GMFCS level IV. (a) Initial radiograph at the age of 3.1 years, when MP of the right hip was 34%. (b) Radiograph at the age of 9.3 years (follow-up 6.2 years), which shows a moderate deterioration of the right hip with MP 40%. The mean increase in MP was 1.0% per year.
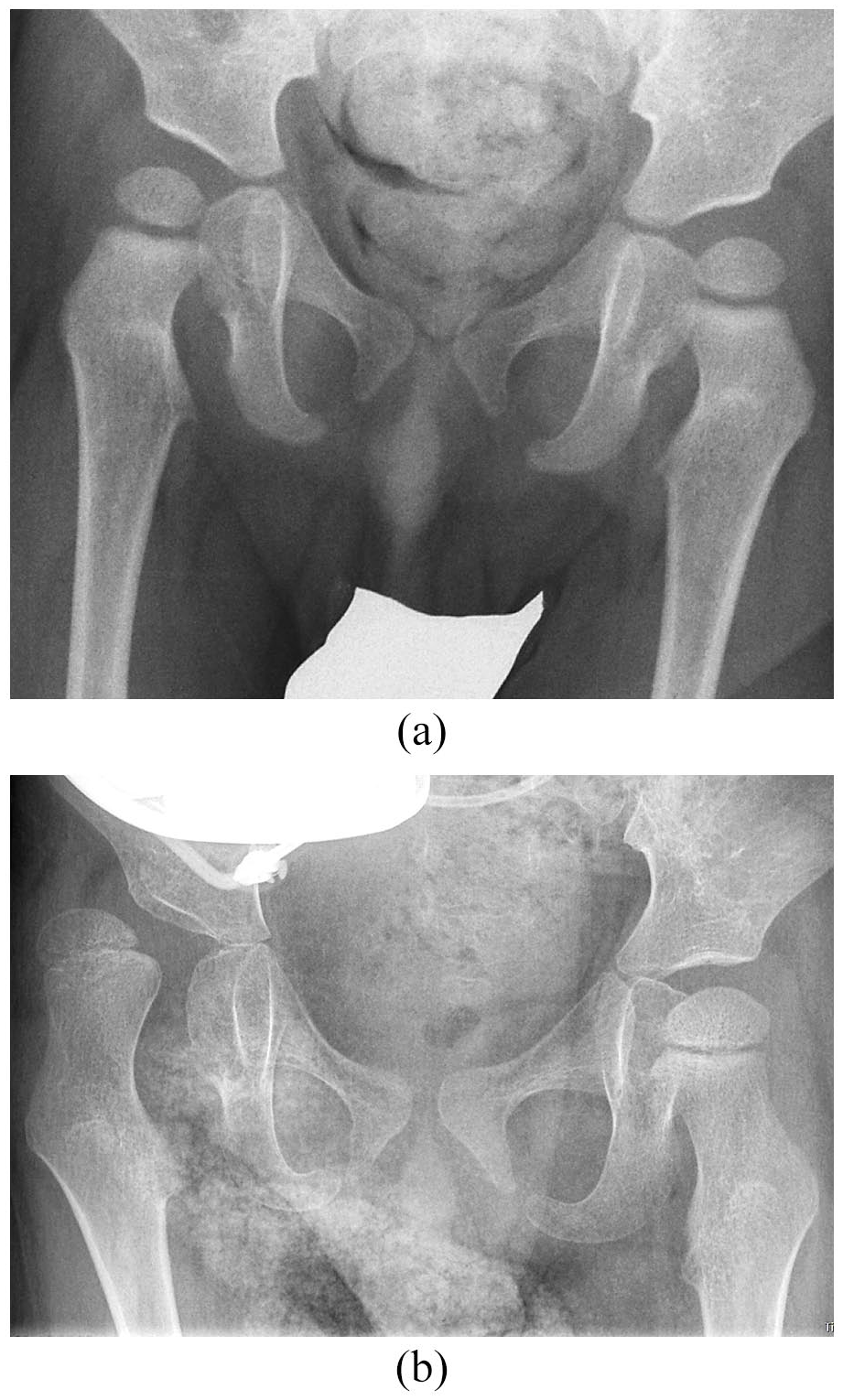
Radiographs of a boy with spastic quadriplegia, GMFCS level V. (a) Initial radiograph at the age of 1.1 years. Radiographic measurements of the right hip: MP 23%, AI 25°, and HSA 173°. (b) Radiograph at the age of 3.4 years (follow-up: 2.3 years), showing a very rapid deterioration of the right hip, which is severely subluxated with MP 89%.
Possible predictors for hip displacement (last MP ≥ 40%) were analyzed with binary logistic regression in 107 patients with initial MP < 50% and follow-up time ≥1.0 years. The following variables were predictors in univariable analysis: GMFCS level V, spastic bilateral CP, initial MP, yearly progression of MP, and initial AI (Table 1). These variables were not risk factors: gender (p = 0.293), patient age (p = 0.341), and initial HSA (p = 0.640). Multivariable regression analysis was performed of the variables with a p value <0.1 in the univariable analysis. Initial MP and yearly progression rate of MP were independent risk factors, whereas GMFCS level, CP type, and initial AI were not (Table 2).
Univariable binary logistic regression analysis of possible risk factors for hip displacement (MP ≥ 40% at the last follow-up) in 107 patients with initial MP < 50% and follow-up time ≥1.0 years.
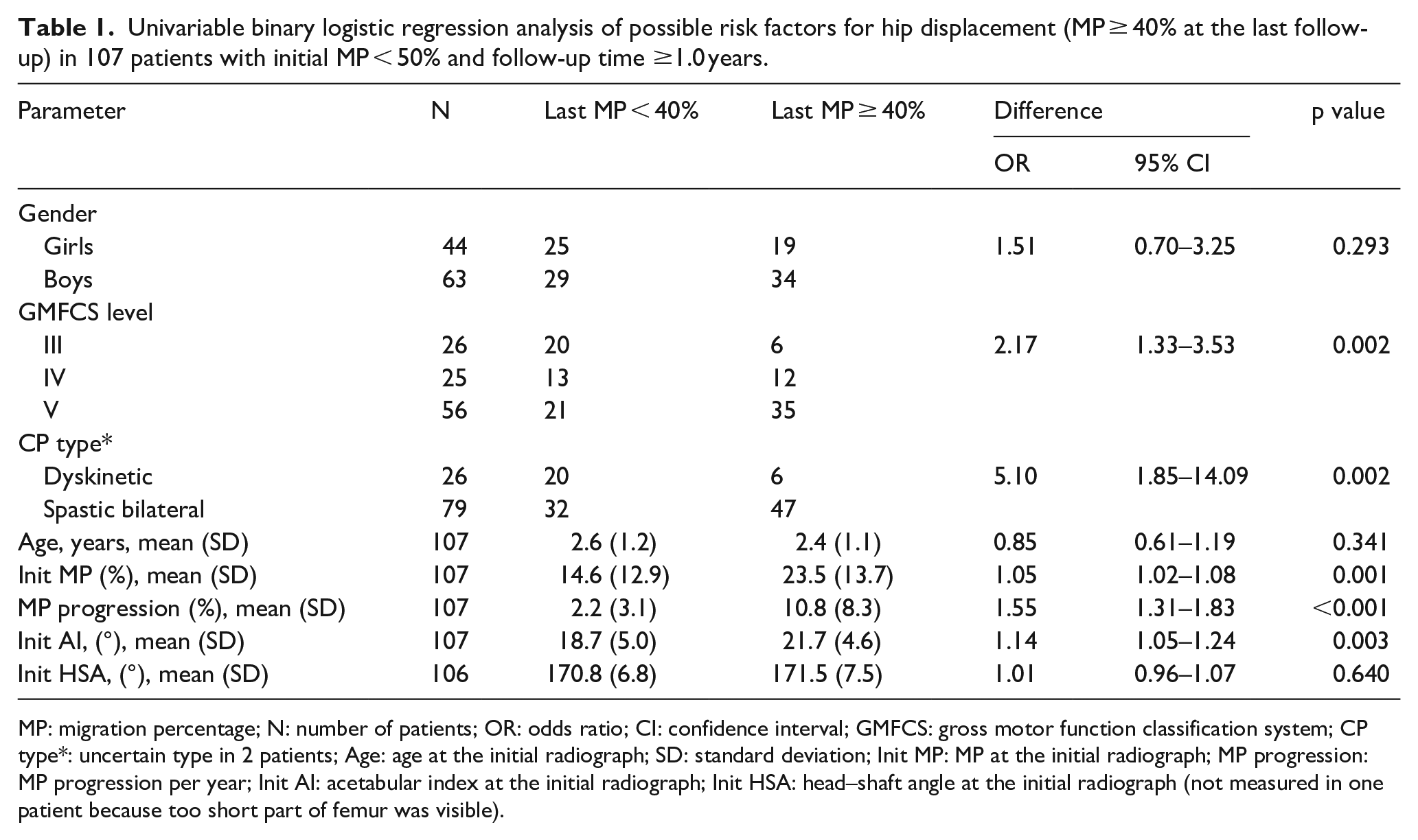
MP: migration percentage; N: number of patients; OR: odds ratio; CI: confidence interval; GMFCS: gross motor function classification system; CP type*: uncertain type in 2 patients; Age: age at the initial radiograph; SD: standard deviation; Init MP: MP at the initial radiograph; MP progression: MP progression per year; Init AI: acetabular index at the initial radiograph; Init HSA: head–shaft angle at the initial radiograph (not measured in one patient because too short part of femur was visible).
Multivariable binary logistic regression analysis of risk factors for hip displacement (MP ≥ 40% at the last follow-up) in 107 patients with initial MP < 50% and follow-up time ≥1.0 years.
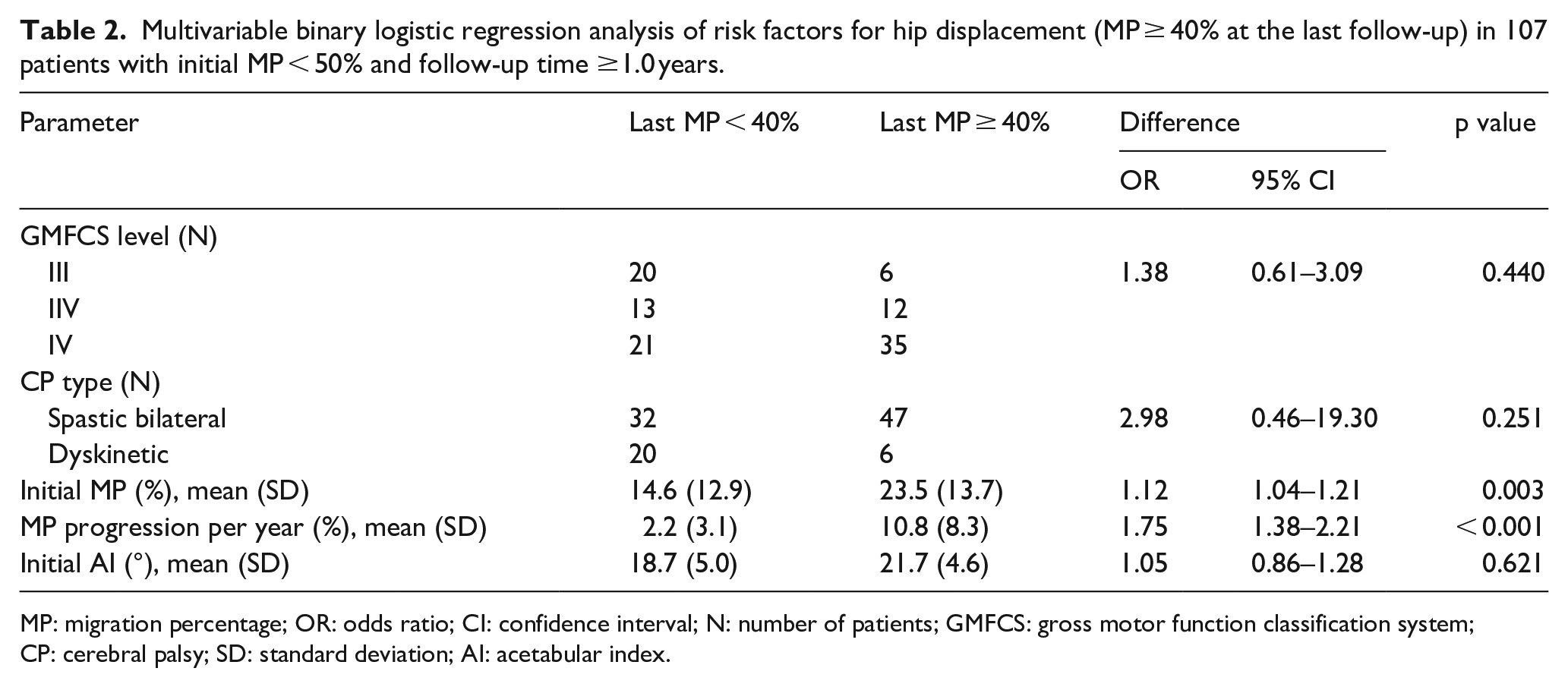
MP: migration percentage; OR: odds ratio; CI: confidence interval; N: number of patients; GMFCS: gross motor function classification system; CP: cerebral palsy; SD: standard deviation; AI: acetabular index.
The correlations between the variables that were significant at the univariable regression analysis are shown in Table 3. Initial MP was significantly correlated with type of CP and initial AI, but not with MP progression per year or GMFCS level. Yearly MP progression was correlated with GMFCS level, but not with type of CP or initial AI.
Correlation coefficients (r) between the parameters that were statistically significant risk factors for hip displacement at the univariable regression analysis.
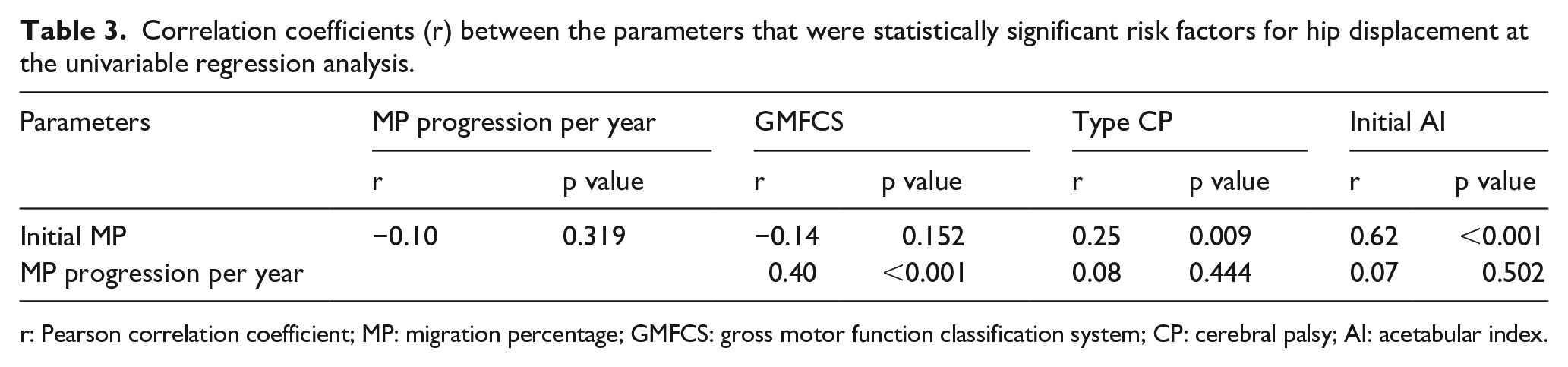
r: Pearson correlation coefficient; MP: migration percentage; GMFCS: gross motor function classification system; CP: cerebral palsy; AI: acetabular index.
The radiographic results at the first and last examinations are shown in Table 4. The mean MP increased during the follow-up period and the increase was significant at all the GMFCS levels. Whereas there were no differences in initial MP between the GMFCS levels, MP at the last follow-up was larger at GMFCS level V compared with levels III and IV (p < 0.001 and 0.049, respectively). There were no significant differences in initial AI between the GMFCS levels. AI increased during follow-up at GMFCS levels IV and V, but not at level III (Table 4). There were no significant differences in the last AI between GMFCS levels V and III (p = 0.122) or between levels V and IV (p = 0.684). There were no significant differences in initial HSA between the GMFCS levels. The mean HSA decreased during the study period at GMFCS levels III and IV, whereas there was no significant change at level V (Table 4). The last HSA was significantly higher at GMFCS level V compared with those at level III (p = 0.004) and level IV (p = 0.010).
Radiographic measurements at the initial and last examinations (mean values with SD in parentheses) in 107 patients with initial MP < 50% and follow-up time ≥1.0 years.
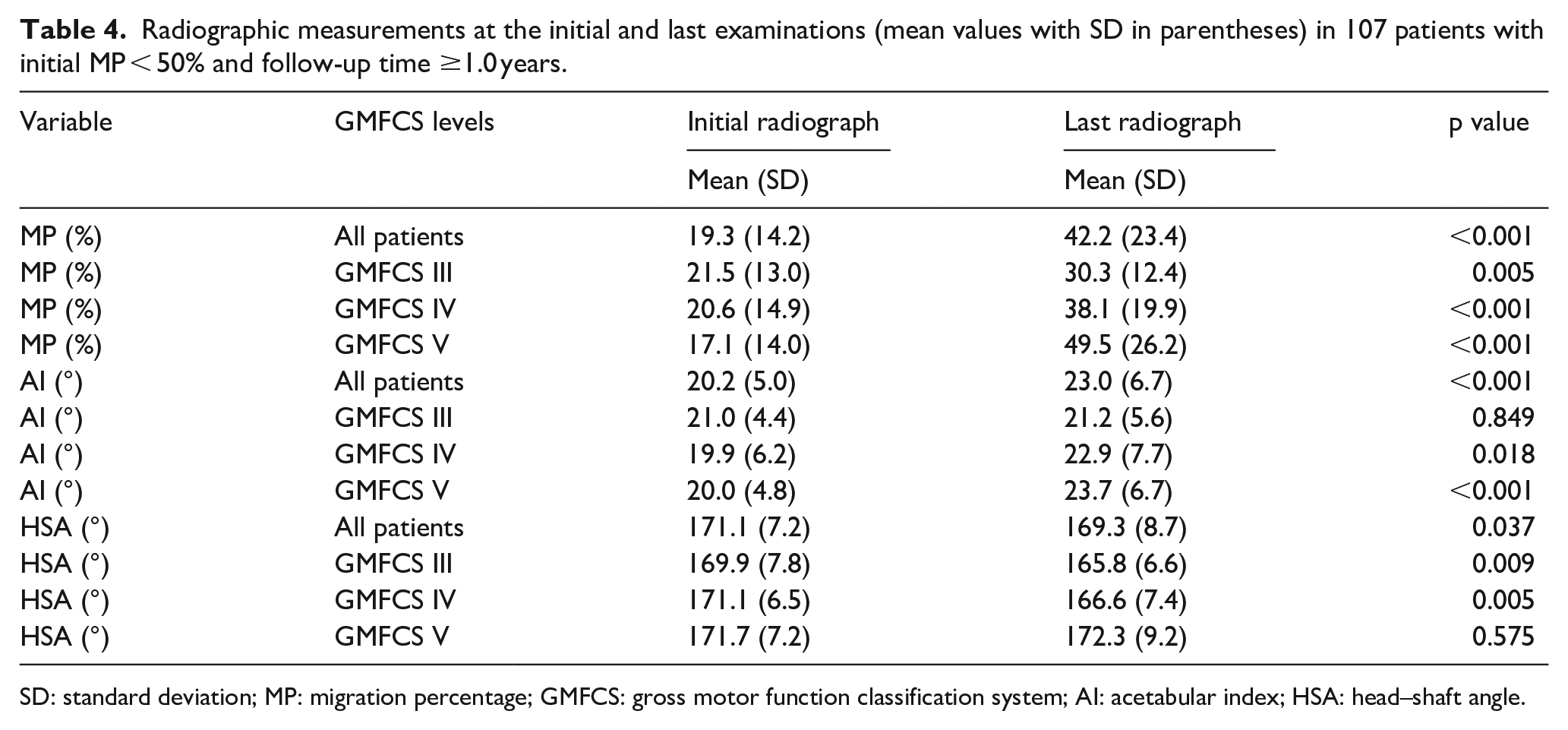
SD: standard deviation; MP: migration percentage; GMFCS: gross motor function classification system; AI: acetabular index; HSA: head–shaft angle.
Discussion
This population-based study of children at GMFCS levels III–V showed that the independent (true) risk factors for clinically significant hip displacement, defined as MP ≥ 40% at the last follow-up, were high initial MP and large rate of yearly MP progression.
Previous studies have reported that hip subluxation is strongly related to the severity of motor impairment as assessed by the GMFCS.5,6 In the present study, GMFCS level V was a risk factor for hip displacement in univariable, but not in multivariable analysis. The reason was probably that GMFCS level was significantly correlated with yearly MP progression rate, which was an independent risk factor. Another reason was that we studied children at GMFCS levels III–V. If children at levels I and II also had been included, GMFCS would probably be a significant factor in multivariable analysis. We thought this was less relevant from a clinical point of view, since hip displacement is rather infrequent in levels I and II. Our findings are in accordance with those of a recent study of children at GMFCS levels III to V, where the development of MP during the last 3 preoperative years was not significantly associated with GMFCS level. 19
Spastic bilateral CP was also a predictor in univariable analysis. The reason why spastic CP was not a predictor in multivariable analysis, was probably that it was significantly correlated with initial MP. Since it is easier to determine the correct GMFCS level than to decide type of CP in small children, GMFCS level is probably a more reliable parameter in hip screening programs, although Pruszczynski et al. 6 pointed out that GMFCS is not a reliable measure for 2- to 3-year-old children.
MP measures the coverage of the femoral head by the acetabular roof, which probably is the most important single qualification of a hip joint. Our study showed that the initial MP was an independent predictor of hip displacement, which supports previous studies.5,15,17 MP is considered to be the most useful radiographic parameter in screening for hip displacement,3,4,7,10 because it is little influenced by the rotational position of the femur 9 and has sufficient interobserver reproducibility. 20
The yearly progression rate of MP was also an independent predictor of hip displacement. This is in accordance with the findings of Wagner and Hägglund, 19 who reported an increasing displacement rate during the 3 years preceding hip operation. Although the rate of MP progression cannot be determined at the time of the initial radiograph, it is an important prognostic factor during follow-up. The mean rate of MP progression per year at GMFCS level V in the present study was 9.3%, which is in keeping with the yearly progression of 7% to 9% in quadriplegic patients. 10 Our progression rate was moderate in children who ended with MP < 40% (2% per year) but was pronounced (almost 11% per year) in hips with final MP ≥ 40%. The practical implication for hip surveillance is that a radiograph should be taken every 6 months (rather than every 12 months) in children with MP progression >10% per year.
There is no consensus regarding other radiographic predictors. AI is one of the controversial parameters. Whereas Cooke et al. 14 found that AI was the most powerful single predictor of hip displacement, Vidal et al. 10 maintained that AI should not be considered as a prognostic indicator before the age of 5 years. Hägglund et al. 4 reported that hip displacement preceded acetabular dysplasia. Moreover, the reliability of the AI has been questioned because the index varies with the orientation of the pelvis. 21 The present study showed that AI was a risk factor in univariable regression analysis, but not in multivariable analysis. The reason was probably that initial AI was strongly correlated with initial MP. Thus, AI is hardly an independent predictor in children <5 years of age.
Another controversial predictor is HSA. The initial HSA was found to be a risk factor for later hip displacement by Hermanson et al., 11 but this was not supported by others.13,22 van der List et al. 12 reported that HSA at the age of 2 years was predictive of later hip displacement, whereas HSA was not a predictor at patient age of 4 years. The present findings are inconsistent with these results, since there was no significant association between the initial HSA in children below 5 years of age and later clinically relevant hip displacement.
A hip surveillance program would be most efficient if only independent (true) predictors of subluxation were used. Since some of the variables are significantly correlated, multivariable analysis is required to define the most important risk factors. We have found only one study that analyzed the predictors with multivariable logistic regression. 15 This Swedish study found that independent risk factors were GMFCS level V, lower age at diagnosis, higher initial MP, and higher initial HSA. We confirmed initial MP as independent risk factor, but not age, GMFCS and HSA. Although both studies were population based, they can hardly be directly compared since AI and progression rate of MP were not included in the analysis of Hermanson et al., 15 and age at diagnosis was higher in the Swedish study (mean age: 3.6 years (range: 0.6–9.7 years) vs 2.5 years in our study). We think age at diagnosis should not exceed 5.0 years in studies of predictors of hip displacement aimed at early diagnosis and treatment.
Nonambulatory children usually have normal hips at birth and develop hip displacement during the first years of life (Figure 3). In a population-based study of the natural history, the mean age at subluxation was 3.6 years and at complete dislocation 4.4 years. 7 This shows the importance of an early initial radiograph, preferably at the age of 2 years. Since moderate degrees of hip displacement is asymptomatic, 23 yearly radiographs are necessary to define the natural history and to find the appropriate time of operative correction, which usually is shortly after the MP exceeds 40%.17,18 At that time, soft-tissue procedures are usually sufficient to provide good long-term outcome.24,25
The mean patient age at the last follow-up was 6.5 years. At this age, the mean AI and HSA were significantly larger in hips with final MP ≥ 40% than in hips with final MP < 40%. This shows that there is an association between both AI and HSA and hip displacement at this age, which probably is caused by the development of secondary deformities in the acetabulum and femur as the child grows. Although AI and HSA at a young age (<5 years) are not independent predictors of hip displacement, these variables may be useful later for the choice of surgical procedures. In hips with moderate subluxation and a particularly large HSA, a varus femoral osteotomy should be considered rather than soft-tissue releases alone. A large AI in hips with more severe subluxation would indicate that a pelvic osteotomy is needed to correct the acetabular dysplasia.
There are a few limitations of this study. First, the number of patients in some of the subgroups was rather small. Second, although the radiographic parameters are easy to measure in hips with well-defined landmarks, measurements can be demanding if the most important landmark (the lateral acetabular rim) is difficult to define. However, the good intra- and inter-rater agreement in previous studies indicates that the measurements are sufficiently reliable in clinical use.13,20,22 The main strength of the study is its population-based design, which should imply good generalizability of the results. Moreover, the study was longitudinal, with follow-up of all the patients.
The aim of this study was not to propose a new hip surveillance program, but to present data aimed at modification and improvement of existing programs. The clinical significance of our results is that the only radiographic parameter that needs to be measured in routine hip surveillance in children below 5 years of age is the MP. Other parameters like AI and HSA are not independent predictors of subluxation at that age. They are, however, useful later for decision-making regarding the choice of surgical correction.
Footnotes
Acknowledgements
The authors would like to thank the photographer Ine Eriksen for help with the illustrations. We also thank the statistician Are Hugo Pripp for help with the statistical analysis.
Author contributions
T.T. planned and executed the study and wrote the manuscript. J.H. executed the study and revised the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Regional Ethics Committee and by our institutional review board.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Formal consent is not required in this type of work (retrospective study, anonymized radiographs).
