Abstract
The COVID-19 pandemic has claimed an extremely high number of lives worldwide, causing widespread panic and stress. The current research examined whether COVID-19 stress was associated with everyday cognitive failures, using data from a seven-day daily diary study of 253 young adults in Singapore. Multilevel modeling revealed that COVID-19 stress was significantly associated with cognitive failures even after adjusting for demographic factors, both at the within-person and between-persons levels. Specifically, individuals experienced more cognitive failures on days they experienced more COVID-19 stress (as compared to their own average levels of COVID-19 stress), and individuals who experienced more COVID-19 stress overall (as compared to individuals who experienced less COVID-19 stress overall) experienced more cognitive failures in general. While a large body of work has evidenced the detrimental effects of COVID-19 stress on individuals’ well-being, the current findings provide novel insights that these stressors may negatively impact individuals’ cognitive functioning as well.
COVID-19 stress and cognitive failures in daily life
The COVID-19 pandemic has claimed an extremely high number of lives worldwide. As of early April 2022, there have been more than 505 million confirmed cases of COVID-19 infection and more than 6 million deaths (World Health Organization, 2022). Beyond the loss of life, the fear of potential infection and constant worry about the health of loved ones have resulted in significant stress and anxiety for many individuals (Xu et al., 2020). Moreover, the resultant abrupt changes from higher unemployment rates and social isolation have caused widespread financial insecurity and loneliness, compounding the experienced stress during the pandemic (Vatansever et al., 2021). Furthermore, unlike other daily stressors that occur due to various context-dependent factors specific to each person (e.g., relationship stressors, work-related stressors), COVID-19 related stressors can be experienced by almost everyone concurrently in the world today (Arıcan & Kafadar, 2022). Thus, COVID-19 related stressors are a more widespread phenomenon in the current background that is particularly important to study. While the economic and socioemotional consequences of COVID-19 stress have been well established, little is currently known about its cognitive consequences.
One potential cognitive consequence of COVID-19 stress is related to daily cognitive failures. Cognitive failures are broadly defined as failures to perform simple tasks that a person is normally capable of completing without errors (Lange & Süß, 2014), such as stopping at the traffic light when it turns red or remembering to attend a work meeting. Cognitive failures can be distinguished from other cognitive errors as being the result of lapses of attention or slips of memory rather than a result of a lack of knowledge, and individuals who experience cognitive failure more often report frequent lapses of action, perception, and memory (Bridger et al., 2013). Although cognitive slips and errors are common in daily living, they have been found to have broad and potentially major implications in real-world outcomes. For example, cognitive failures make individuals more vulnerable to the effects of stress (Broadbent et al., 1982; Mahoney et al., 1998), leading to outcomes such as job impairment, workplace-related mishaps, and injuries and hospitalization (Abbasi et al., 2021; Wallace & Vodanovich, 2003a, 2003b). Cognitive failures have also been found to lead to increased susceptibility to driving error and car accidents (Allahyari et al., 2019; Larson & Merritt, 1991). Several studies also indicate that self-reported cognitive failures predict laboratory measures assessing cognitive abilities such as working memory or attentional control (Unsworth et al., 2012a; Unsworth et al., 2012b).
Research examining the antecedents of cognitive failures has suggested that stress can have detrimental effects on one's cognitive functioning (Mahoney et al., 1998). In particular, it is thought that the negative effect of stress on cognitive functioning may be explained through the mediating role of mind wandering (Hartanto & Yang, 2020), which refers to thoughts about one's goals that are not related to the primary task at hand (Morin & Racy, 2021; Smallwood & Schooler, 2006). While mind-wandering is not necessarily maladaptive, it can negatively affect cognitive functioning if driven by anxiety or stress, and lead to cognitive failures (Burdett et al., 2016; McVay & Kane, 2010). For example, stressful life events, such as the COVID-19 pandemic, may increase the likelihood of engaging in task-unrelated thoughts (e.g., worrying about potential infection) and decrease the effectiveness of disengaging from such thoughts (Klein & Boals, 2001). These mental diversions compete for limited cognitive resources and the attempts to suppress undesired thoughts consume even more resources (Smeekens & Kane, 2016). Indeed, as illustrated by literature on working memory, these mental diversions may result in poorer reasoning (Kane et al., 2005), multitasking (Colom et al., 2010), and learning (Noël, 2009). Given the literature on the implications of cognitive failure, as well as the pervasiveness of stress during this pandemic, it behooves us to properly examine the relationship between COVID-19 stress and cognitive failure.
The present study thus seeks to investigate the effect of COVID-19 stress on everyday cognitive failures. In order to reduce the possibility that individual differences may confound any observed associations between COVID-19 stress and cognitive failures, we employed a multilevel approach by utilizing a diary study design. This study design allowed us to examine day-to-day fluctuations in COVID-19 stress and cognitive failures, while controlling for several individual differences in the form of demographic factors (i.e., age, sex, race, household income, and subjective socioeconomic status) previously linked to our variables of interest.
Method
Participants and design
Data for the current study were collected as part of the second wave of a larger project broadly examining daily experiences and well-being (see Goh et al., 2023; Majeed et al., 2023; Ng, Lua et al., 2022; Ng, Majeed et al., 2023), conducted with young adults in Singapore with the daily diary portions running from June 24, 2021 to August 12, 2021 (i.e., during the country's partially relaxed “Phase 3 Heightened Alert” 1 and the stricter semi-lockdown “Phase 2 Heightened Alert” 2 of the COVID-19 pandemic; Abu Baker, 2021; Ang, 2021).
Undergraduate students from the last author's university were recruited for the study through the local subject pool system. 3 Participants completed a baseline questionnaire, followed by a seven-day self-administered diary survey taken nightly. Within one to two days of completing the baseline questionnaire, a link to the first diary survey was emailed to participants at 8.00 p.m., with the link to the consecutive diary surveys being sent each evening at 8.00 p.m. for the remaining six days. Each daily diary survey was left available for completion until 3.00 a.m. the next day. A total of 1,721 observations of daily data were obtained from 253 participants, where each participant provided an average of 6.80 days of observations (97% completion rate; see Table 1). The data collection procedure was approved by the Institutional Review Board at the last author's university (IRB-20-118-A075-M4[621]). All participants provided informed consent prior to data collection.
Summary of descriptive statistics
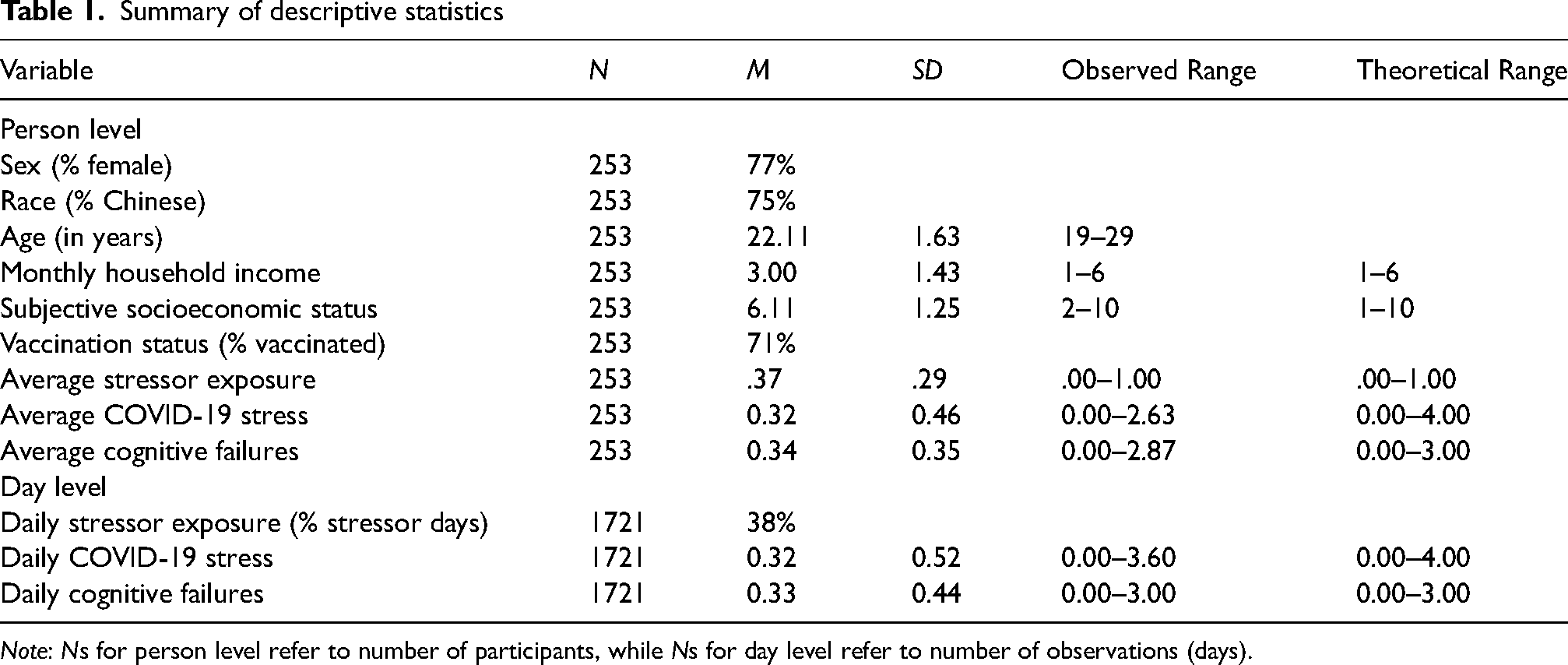
Note: Ns for person level refer to number of participants, while Ns for day level refer to number of observations (days).
Measures
Baseline
Demographic covariates. Participants were asked to report their sex (male or female), race (Chinese, Malay, Indian, or other), age, and monthly household income (1 = less than $2,000, 2 = $2,000–$5,999, 3 = $6,000–$9,999, 4 = $10,000–$14,999, 5 = $15,000–$19,999, 6 = more than $20,000). Subjective socioeconomic status was measured using a 10-point ladder scale (Adler et al., 2000), with the bottom rung (1) representing the lowest status and the top rung (10) representing the highest status.
COVID-19 vaccination status. Participants were asked to report their COVID-19 vaccination status (currently vaccinated or unvaccinated).
Daily
Daily stressor exposure. Daily stressor exposure was measured each day for each participant through the Daily Inventory of Stressful Events (Almeida et al., 2002). The inventory is a checklist of seven types of stressors (arguments, avoided arguments, discrimination, work/education stressors, home stressors, network stressors, and “others”), and participants were asked to indicate if any of the stressors occurred to them “since yesterday.” In line with existing work on daily stressor exposure (e.g., Majeed et al., 2021; Ng et al., 2022; Rush et al., 2019), the construct was operationalized as a binary variable. Specifically, if at least one stressor was experienced on that day, the day was categorized as a stressor day, and otherwise, it was categorized as a non-stressor day. The intra-class correlation for daily stressor exposure was .64.
Daily COVID-19 stress. COVID-19 stress was measured using five items selected from the COVID Stress Scales (Taylor et al., 2020), administered daily. The COVID Stress Scales have been validated across a number of different samples (e.g., Asmundson et al., 2022; Carlander et al., 2022; Khosravani et al., 2021; Taylor et al., 2020), and correlate strongly with other COVID-19 fear-related measures (e.g., Khosravani et al., 2021; Pakpour et al., 2021) while showing significantly greater correlations with anxiety-related measures rather than depression-related measures (Khosravani et al., 2021; Taylor et al., 2020). The current study used five items adapted from the COVID Stress Scales to measure COVID-19-related stress and anxiety symptoms on four factors: (1) danger and contamination, (2) xenophobia, (3) compulsive checking, and (4) traumatic stress symptoms. Participants were asked to indicate “how you have felt or behaved this way today” in relation to three worries and two behaviors on a 5-point Likert scale (0 = Not at all, 4 = Extremely for worries; 0 = Never, 4 = Almost always for behaviors). Specifically, the items on worries were: “Today, I was worried about catching the virus” (danger and contamination), “Today, I was worried that our healthcare system will be unable to keep me and my loved ones safe from the virus” (danger and contamination), and “Today, I was worried that foreigners are spreading the virus in Singapore” (xenophobia). The items on behaviors were: “Today, I checked online and offline media (e.g., Facebook, Straits Times) for information concerning COVID-19” (compulsive checking) and “Today, I had trouble concentrating because I kept thinking about the virus” (traumatic stress symptoms). All items were averaged such that higher overall scores reflected greater levels of daily COVID-19 stress (αwithin = .63, αbetween = .86). The intra-class correlation for daily COVID-19 stress was .74. A plot of average COVID-19 stress levels (per participant) over time, in comparison to the number of COVID-19 cases and deaths in Singapore (data retrieved from Mathieu et al., 2020), is provided in Figure 1.
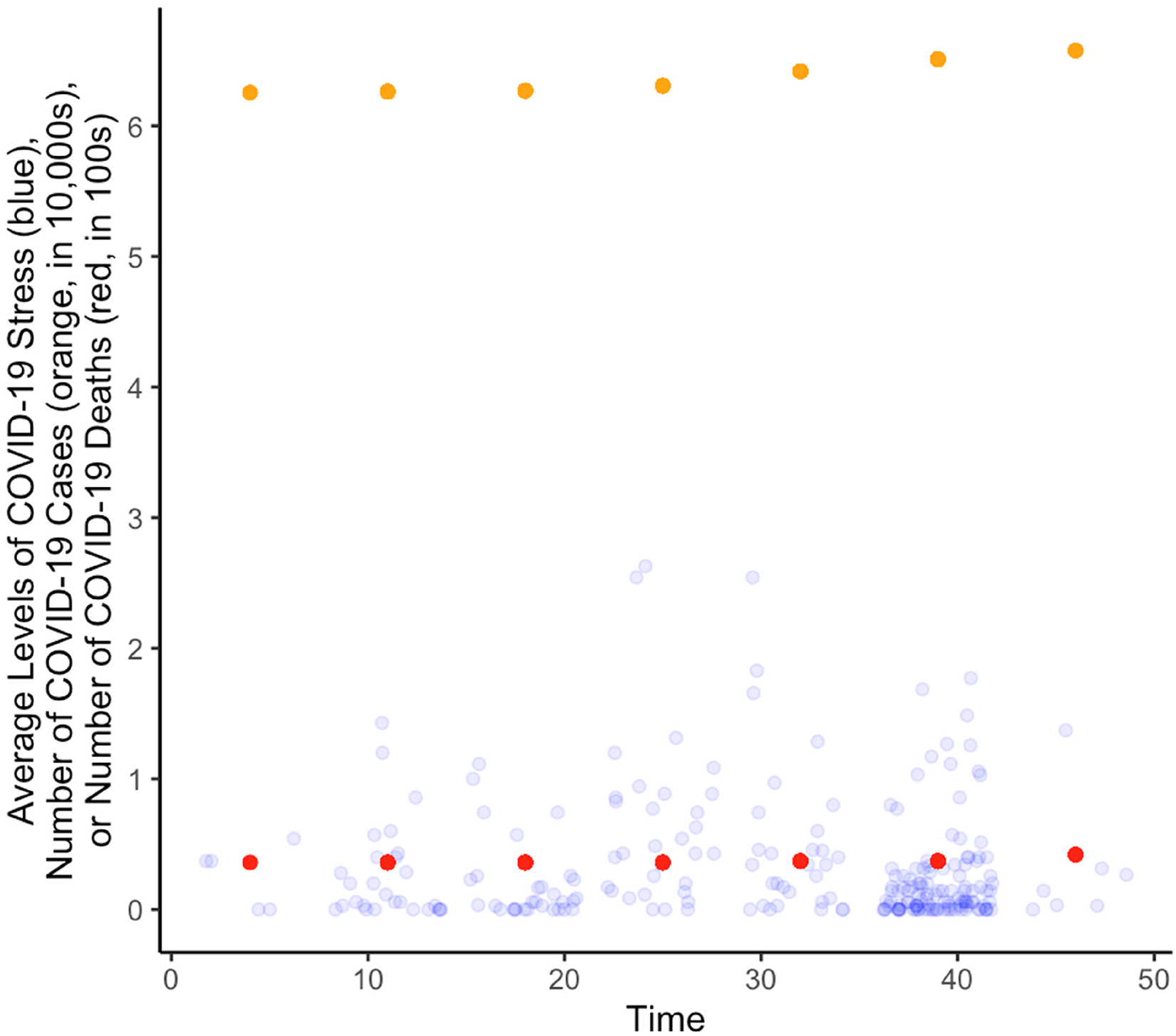
Participant-average levels of COVID-19 stress and national numbers of COVID-19 cases and deaths over time.
Daily cognitive failures. Cognitive failure was measured using the 13-item Cognitive Failures in Everyday Life Scale (Lange & Süß, 2014), administered daily. Each item (e.g., “Did your mind unintentionally wander, at any point of time today?”) was rated on a 4-point Likert scale (0 = Never, 3 = Several times), with higher scores reflecting greater daily cognitive failure (αwithin = .75, αbetween = .95). The intra-class correlation for daily cognitive failures was .57.
Analytic plan
Due to the two-level nature of the diary data (i.e., repeated measures nested within individuals), multilevel modeling 4 was conducted to examine the association between daily COVID-19 stress and daily cognitive failures across the seven days (Level 1) nested within participants (Level 2).
Main analyses
The Level 1 predictor, daily COVID-19 stress, was person-mean centered and entered as both a random and fixed predictor, and its person-level mean was reintroduced as a fixed predictor at Level 2 in order to fully decompose daily COVID-19 stress into its within- and between-persons components (Bolger et al., 2012). Time—in terms of number of days since the start of data collection for the whole sample—was included as a person-mean-centered Level 1 covariate with both random and fixed components with its person-level mean reintroduced as a Level 2-fixed covariate in order to account for changes over time due to the changing pandemic situation. The unadjusted model was thus as follows, with γ10 and γ01 representing the within-persons and between-persons parameters of interest respectively:
Level 1: (Daily cognitive failures) di = B0i + B1i(daily COVID-19 stress) di + B2i(time) di + ε di
Level 2: B0i = γ00 + γ01(average COVID-19 stress) i + γ02(average time) i + μ0i
B1i = γ10 + μ1i
B2i = γ20 + μ2i
An adjusted model was estimated with the inclusion of demographic factors, COVID-19 vaccination status, and daily stressor exposure. Age, sex, race, objective socioeconomic status (i.e., monthly household income), and subjective socioeconomic status were included as Level 2-fixed components in an adjusted model in order to rule out demographic confounds. Stressor exposure was included as random and fixed components at Level 1 in terms of stressor days versus non-stressor days, and as a fixed component at Level 2 in terms of average stressor exposure across the seven days. Categorical predictors (i.e., sex, race, and daily stressor exposure) were dummy-coded with male, majority race (i.e., Chinese), and non-stressor day serving as the reference categories respectively. The equations for the adjusted model are thus as follows:
Level 1: (Daily cognitive failures) di = B0i + B1i(daily COVID-19 stress) di + B2i(time) di + B3i(daily stressor exposure) di + ε di
Level 2: B0i = γ00 + γ01(average COVID-19 stress) i + γ02(average time) i + γ03(age) i + γ04(sex) i + γ05(race) i + γ06(objective SES) i + γ07(subjective SES)i + γ08(average stressor exposure)i + μ0i
B1i = γ10 + μ1i
B2i = γ20 + μ2i
B3i = γ30 + μ3i
At Level 1, B0i (the intercept coefficient for each participant i) indicates participant i's average level of cognitive failures. B1i shows the change in daily cognitive failures in relation to daily COVID-19 stress. At Level 2, B0i was modeled as a function of between-participant differences. This includes participant i's average COVID-19 stress over the duration of the seven days and other covariates. B1i represents the slope coefficient for each participant i. μ0i and μ1i indicate the deviation of each participant's intercept and slope respectively from the model-implied values.
Additional analyses
Leave-one-out multiverse analysis. As the daily COVID-19 Stress measure was adapted and had not yet been established in its current form, we conducted a leave-one-out multiverse analysis to evaluate plausible analytic alternatives in parallel and interpreted collectively. The purpose for this analysis was to see if our results were robust across the different operationalizations of COVID-19 stress. Specifically, we repeated the unadjusted and adjusted analyses previously mentioned but with all 31 possible combinations of the five items used to create the COVID-19 Stress measure.
Exploratory lagged analysis. We repeated the main analyses with a one-day time lag in a preliminary examination of whether the association between COVID-19 stress and cognitive failures could spill over onto the next day. Specifically, we modeled next-day cognitive failures as a function of today's COVID-19 stress and covariates.
Exploratory mediation analysis. We repeated the main analyses with COVID-19 vaccination status as a predictor of daily COVID-19 stress, resulting in a mediation model (for conceptual representation, see Figure 2).

Conceptual representation of mediation.
Transparency and openness
The current work's design and its analysis plan were not pre-registered. Relevant materials, data, analytic code, as well as a supplemental information (zero-order correlation matrix at Level 2 and residual QQ plot) have been made publicly available on Researchbox #466 (https://researchbox.org/466).
Unless otherwise stated, all analyses were conducted in R version 3.6.3 (R Core Team, 2020). Data cleaning and manipulation were performed using dplyr version 1.0.10 (Wickham et al., 2022). Descriptives were extracted using psych version 2.2.9 (Revelle, 2021). Multilevel scale reliabilities were calculated via semTools version 0.5-5 (Jorgensen et al., 2021). ICCs were calculated by merTools version 0.5.2 (Knowles et al., 2020). Multilevel modeling was conducted via lme4 version 1.1-28 (Bates et al., 2014) with significance testing by lmerTest version 3.1-3 (Kuznetsova et al., 2017), where maximum likelihood estimation was used to fit all models. Effect sizes in the form of standardized coefficients were calculated by effectsize version 0.6.0.1 (Ben-Shachar et al., 2020) using the “pseudo” method. Multilevel mediation was conducted via mlma version 6.2-1 (Yu & Li, 2022). Sensitivity power analyses were performed using Mplus version 8 (Muthén & Muthén, 2012).
Results
Main analyses
We found significant positive associations between daily COVID-19 stress and daily cognitive failures both at the within-persons and between-persons levels (Table 2). 5 Specifically, to a small extent, participants reported more cognitive failures on days they experienced more COVID-19 stress compared to their own average (unadjusted: β = .07, 95% CI = [.02, .12], γ10 = 0.08, SE = 0.03, p = .006; adjusted: β = .06, 95% CI = [.01, .11], γ10 = 0.07, SE = 0.03, p = .020). Additionally, to a moderate extent, participants who experienced higher levels of COVID-19 stress in general also reported more cognitive failures than participants who experienced lower levels of COVID-19 stress (unadjusted: β = .17, 95% CI = [.04, .30], γ01 = 0.12, SE = 0.05, p = .009; adjusted: β = .18, 95% CI = [.09, .27], γ01 = 0.13, SE = 0.03, p < .001).
Full results of main multilevel analyses

Note: Nparticipants = 253, Nobservations = 1721. Estimates for random effects indicate variances. Bolded rows indicate statistical significance at p < .050.
Leave-one-out multiverse analyses
Leave-one-out multiverse analyses revealed that our main findings were generally robust across the various operationalizations of daily COVID-19 stress (Figure 3). All point estimates were consistent with the main findings (i.e., positive in sign), although some combinations of items (e.g., the combination of items 1, 2, and 4 at the within-persons level, and the combination of items 1 and 4 at the between-persons level) produced nonsignificant associations (ps ≥ .050) with daily cognitive failures.

Summary of leave-one-out multiverse analyses.
Exploratory lagged analyses
We found that daily COVID-19 stress was not predictive of next-day cognitive failures (unadjusted: β = −.02, 95% CI = [−.07, .04], γ10 = −0.02, SE = 0.03, p = .525; adjusted: β = −.02, 95% CI = [−.07, .03], γ10 = −0.02, SE = 0.03, p = .455). This suggests that the association between COVID-19 stress and cognitive failures is short-lived, and does not spill over to the next day.
Exploratory mediation analyses
The mediation analysis revealed a significant indirect mediation pathway from COVID-19 vaccination status through COVID-19 stress in predicting cognitive failures (B = −0.01, 95% CI = [−.007, −.017]). This suggests that being vaccinated for COVID-19 is associated with decreased levels of COVID-19 stress, which in turn is associated with lower levels of cognitive failures.
Discussion
We analyzed data from a daily diary study of 253 young adults in Singapore across seven days during the COVID-19 pandemic. We found that COVID-19 stress was consistently associated with poorer cognitive functioning both at the within-persons and between-persons levels, such that individuals experienced more cognitive failures on days they experienced more COVID-19 stress (as compared to their own average levels of COVID-19 stress), and also that individuals who experienced more COVID-19 stress overall (as compared to individuals who experienced less COVID-19 stress overall) experienced more cognitive failures in general. Adjusting for demographic covariates did not change the observed patterns. Of note, leave-one-out multiverse analyses of the five items forming the COVID-19 stress measure preliminarily suggest that the associations observed in the current work are mostly driven by stress from two specific items (i.e., “Today, I was worried that foreigners are spreading the virus in Singapore” and “Today, I had trouble concentrating because I kept thinking about the virus”).
The current work is the first to empirically examine the associations between COVID-19 stress and cognitive failures. The use of a daily diary methodology allowed us to examine this relationship in an ecologically valid setting, and also allowed us to rule out stable individual differences that may account for the positive within-persons associations between COVID-19 stress and cognitive failure. Taken together, the findings of the current work suggest that the stress arising from the COVID-19 situation may indeed be associated with increased levels of cognitive failures among individuals both at the day-to-day level and in general. The positive associations observed in the current study are in line with much of the literature broadly examining stress on cognitive failures (Mahoney et al., 1998). Considering past works suggesting that mind-wandering mediates the positive relationship between stress and cognitive failures (Hartanto & Yang, 2020), we posit that mind-wandering may also be a possible explanation for the observed relationship between COVID-19 stress and cognitive failure. Further research into this potential mechanism is warranted, given the lack of direct examination of this mechanism in the current work. Nonetheless, our findings suggest that beyond detriments to affective and socioeconomic outcomes, COVID-19 stress may be associated with poorer cognitive outcomes as well.
In addition to our main results, we uncovered two notable exploratory findings. First, we did not observe any lagged associations or spillover of daily COVID-19 stress onto cognitive failures on the next day. This contrasts with existing works on other types of stress and cognitive failure—for example, daily work-related stress has been found to be associated with higher levels of next-day cognitive failure (Kottwitz et al., 2022). Situating our current exploratory findings within the existing literature suggests that the relationship between COVID-19 stress and cognitive failure may be more transient in nature, perhaps due to differences in the nature of the stressor experience itself. Second, vaccination against COVID-19 appeared to play a protective role, with our current data indicating that vaccinated individuals reported reduced levels of COVID-19 stress in general. Consequently, this reduction in stress might indirectly protect against cognitive failures. These exploratory findings, while brief, provide valuable insights that could guide future research and interventions not just within the context of COVID-19, but within the broader stress literature.
The current study is not without limitations. First, while the original version of the COVID-19 Stress Scale has been validated with two large North American samples (Taylor et al., 2020) and a large South American sample (Pulido & Jimenez, 2020), it has not been validated with any Asian samples, nor has the shortened daily version adapted for the current daily diary study been validated in any context. As such, future studies should be conducted to assess the psychometric properties of the five-item version employed in the current study. Second, while the daily diary method is high in ecological validity, minimizes issues of recall bias, and allows for the disentangling of within- and between-persons associations, its nonexperimental nature does not allow for causal conclusions to be drawn. Thus, it is possible—though not theoretically likely—that higher levels of cognitive failures drive higher levels of COVID-19 stress, 6 in opposition to our hypothesized direction.
In sum, the present work provides novel insights into the associations between daily COVID-19 stress and daily cognitive failures. While a large body of work has evidenced the detrimental effects of COVID-19 stress on individuals’ sense of well-being, the current findings suggest that these stressors may negatively impact individuals’ cognitive functioning as well. In turn, this may have unfavorable consequences on individuals’ day-to-day functioning (e.g., in logical reasoning and decision-making), as previously alluded to. Considering the pervasiveness of COVID-19 stress today and the high likelihood that the pandemic will continue affecting individuals’ lives in the near future (Chia & Hartanto, 2021), it is undoubtedly important to consider the downstream effects of the pandemic on individuals in the society. Beyond ensuring adequate medical support and infrastructure in the current pandemic, it is crucial for community leaders and policymakers to ensure that individuals have adequate resources to mitigate the stresses arising from the pandemic situation.
Footnotes
Acknowledgements
We are grateful to Frosch Quek, Gloria Lai, Harkiran Kaur, Harleen Kaur, Joax Wong, Manmeet Kaur, Wei Ming Ooi, and Xin Yi Poh for their assistance in data collection.
Authors contributions
NMM and AH developed the study concept and analytic plan. NMM and KTASK performed the data analysis and interpretation. NMM, KTASK, MYL, JLC, and VYQL drafted the paper, and all authors provided critical revisions. All authors approved the final version of the paper for submission.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article: This research was supported by a grant awarded to AH by Singapore Management University through research grants from the Ministry of Education Academy Research Fund Tier 1 (21-SOSS-SMU-023) and Lee Kong Chian Fund for Research Excellence. The funding body had no role in the design of the study and collection, analysis, and interpretation of data and in writing the manuscript.
Data availability statement
The materials and dataset analyzed during the current study have been made publicly available in the Researchbox repository (#466; https://researchbox.org/466).
