Abstract
Background:
Research underpins and informs a profession’s growth. Research and practice have a fundamental relationship involving knowledge production and its applications to a profession’s work.
Objectives:
To investigate health information management professionals’: interest in investigator involvement in research; exposure to, or opportunity for, research investigator involvement; areas of research interest; barriers to research investigator involvement.
Method:
A cross-sectional study design was utilised. An online survey elicited data on respondents’: demographics, employment, roles; access to research information; interest and experience in research engagement; experience of barriers to research investigator involvement.
Results:
Of 112 respondents: 64.3% reported no research involvement; 35.7% had research team experience; 83.9% retrieved research information from the web; 73.9% had no role-based research component; 51.3% had been approached by other (workplace-based) researchers to access and analyse data. Barriers to investigator involvement were personal, organisational and logistical, with lack of time the greatest impediment (62.5%) followed by cost (33.9%), lack of confidence (33%) and not knowing who to approach, or how (31.3%). Research skill development was important for 14.1%. Clinical Coding and Classification Systems (13.3%) and eHealth (12.6%) were considered likely to benefit most from health information management-related research.
Conclusion:
Health information management practitioners generally have interest in research engagement; barriers include time, money and confidence.
Implications for practice:
Provision of research skills and the anomaly of requests for facilitation of data access and analyses alongside absence of a research component in their formal roles require attention. The professional association should actively encourage collaborative academic-practitioner research and showcase new evidence for practice.
Keywords
Introduction
Research is a critical element for propelling the growth of a profession since it promotes the development of knowledge. Professional competencies, observed King et al (2018: 122) “can only remain current if practitioners continually engage with new knowledge.” Research is particularly vital in professions that are undergoing significant, rapid changes to professional practice. Mdletshe (2023) cited challenges to the medical imaging profession including the introduction (and rapid expansion) of technology, divergence into new roles that align with the profession’s skill set and changing needs of the profession’s stakeholders; these challenges mirror those currently affecting the health information management profession. In all professions, research and practice have a fundamental, but often unrecognised, symbiotic relationship at the nexus between knowledge production and its applications to the profession’s work (King et al., 2018). Research provides the decision-making evidence for the direction of a profession in many vital areas such as education and training (initial and continuing), credentialing, policy and governance.
Ideally, both academics and practitioners should contribute to a profession’s research activities and outputs. Their involvement as research investigators ensures a focus on relevant areas of practice, given the practitioners’ capacity to contribute context-specific knowledge (Laustsen, Petersson et al., 2021). Practitioners can capacitate the exchange of knowledge by engaging in its dual translation from research to practice and practice to research (Laustsen, Westergren et al., 2021). Inevitably, however, research relationships in what Bartunek and Rynes (2014: 1195) described as the “academic-practitioner dialectic,” must negotiate the oppositional concepts of theory and practice and rigour and perceived relevance to professional practice. In their systematic review of the literature, King et al. (2018) identified interrelated factors in these research relationships involving (a) academics, practitioners and healthcare and educational organisations, (b) the need for academics to support practitioners in research and (c) requirements for practitioners to acquire research confidence, knowledge and skills.
The profession of health information management is a vital contributor to the global health system, particularly in the areas of clinical treatment and decision-making, patient safety, research, health policy, service planning and funding. Health information managers (HIMs) plan, develop, implement and manage health information services and systems, and clinical and administrative data, to meet the medical, legal, ethical and administrative requirements of healthcare delivery (Health Information Management Association of Australia [HIMAA], 2022). In Australia’s hospital system, HIMs are the custodians of data relating to every episode of care. Outside the hospital system, they work across the health sector, managing and protecting patient data in government health departments, statutory bodies, clinical registries, health screening centres, primary and community health services and facilities, research centres, universities, health insurance funds, private information technology (IT) firms, health classification and other health services companies and not-for-profit healthcare organisations. A considerable proportion of HIMs also contribute as expert HIM-clinical coders (HIM-CCs). HIM-CCs and clinical coders (CCs) assign codes from recognised classification systems to narrative descriptions of patients’ diseases and clinical and surgical procedures, to accommodate storage, protection, retrieval, analysis and applications of health data (HIMAA, 2022). HIMs and CCs are highly involved in the pursuit of health data quality, including accuracy, timeliness and correctness.
Historically, while all patient records existed in paper form, there was clear delineation of professions regarding patient information: entry of notes into patient records was the domain of the clinical professions (doctors, nurses and allied health professionals), and the cleaning, classification (coding), analysis and protection of patient data and information were the domain of the health information management professional. Since the advent of electronic medical records (EMRs) and related health information systems, health “data” have become more readily accessible and of sufficient value that multiple professions (clinical professionals as well as data scientists [data architecture, machine learning, analytics] and software engineers) have assumed a vested interest, such that it is becoming more challenging to define the boundaries of the broader “health information workforce” and impossible to enumerate it (Health Workforce Australia, 2013).
There is a degree of risk in the blurring of these professional boundaries. EMRs have provided the opportunity to aggregate patient data “to answer clinical and policy questions in a systematic, timely and reproducible way” (Jackson, 2014: 4). The demand for data has never been higher within all levels of government, local health districts/networks and primary health networks, and by researchers, health economists, academics, medical educators, the pharmaceutical and health insurance industries and health and legal consultants. The possibility of linking datasets provides greater opportunities for answering clinical and policy questions, and HIMs have the best skill-set to inform about data quality, coding and other specialist aspects of classification, privacy and security of health data and medico-legal implications surrounding the ethical handling of such datasets (Henderson, 2015). Many technological advances in health have been introduced well ahead of considered legal protections for patient privacy and governance of these processes. Similarly, private companies are involved in the development of online booking systems to access health care and are subject to existing privacy legislation, but the lack of governance has already resulted in significant fines for breaches (Henderson, 2021; Henderson and Robinson, 2021). These data and other developments all require evidence to support related practice.
HIMAA has existed for over 75 years (Watson, 2013) and its international peer-reviewed journal, Health Information Management Journal (HIMJ), for over 50 years (Robinson and Lee, 2020). A 2021 examination of articles published in HIMJ in 2016–2020 found that only 34.5% involved at least one HIM as an author; the remainder were published on health information management professional knowledge domains by clinicians, pharmacists, public health specialists, non-profession specific health researchers, health informaticians and nursing and allied health professionals (Robinson et al., 2021). In their scoping review of the literature on the applications of ICD-10 and ICD-10-AM data in research published in 2012–2022, Riley et al. (2024) found that only 3.8% of the studies included HIM or CC authors. In addition, only 5.7% of the studies acknowledged the assistance of expert HIMs or CCs, or mentioned the involvement of hospital health information services (Riley et al., 2024). These findings suggest a great need to engage more HIMs in research and publication.
HIMs in Australia are the data custodians for the vast bulk of patient administrative data and are the curators to whom researchers apply for access to patient data, subject to ethics approval. HIMs and CCs are specialists within their domains of expert work and would be an asset as collaborators on any research project involving these patient data. It is crucial for the positioning of the health information management profession, and the expansion and currency of its knowledge base, that both HIMs and CCs share, demonstrate and disseminate their knowledge and experience via publication of their ethically approved workplace-based studies and research project outcomes (Robinson et al., 2021; Henderson and Callen, 2018). In 2015, in recognition of the need to increase HIMs’ participation in research, the Association included the following statement in the HIMAA Professional Practice Guidelines for Health Information Management Professionals, cross-referenced to the HIM professional competency domains: Members of the Health Information Management Association of Australia (HIMAA) shall: . . . 8. Advance health information management knowledge and quality practice through continuing participation in education, research, publications, presentations, and interdisciplinary collaboration (emphasis added). (HIMAA, 2015)
The HIMAA board of directors requested its Research Advisory Committee (RAC) to undertake a survey of HIMAA members, with the purpose to discover the extent of, and barriers to, their participation in research.
Aims
The aims of this study were to investigate HIMAA members’:
Interest in investigator involvement in research projects,
Exposure to, or opportunity for, investigator involvement in research projects,
Areas or topics of research interest for research projects and
Barriers to investigator involvement in research projects.
Method
Study design and sample
A cross-sectional study design was utilised. The study population comprised all members of HIMAA at 31 July 2022: the entire population of 960 members was invited to participate. The estimated required sample size was 275 (95% Confidence Interval; 5% Margin of Error). The HIMAA membership comprises HIMs (having a bachelor or profession-entry master degree in health information management), including HIMs who work as clinical coders (HIM-Coders). The senior associate and associate membership comprises clinical coders (CCs), who are not qualified HIMs and mostly do not have university-level education that contains research training, and those qualified in health information management-related fields, such as health data analysts and health informaticians.
Survey instrument
A purposely designed survey instrument containing 18 items was created in REDcap (Appendix A, Online Supplemental) by the authors, who were members of the RAC. The survey included four characteristic variables (aggregated to test for representation of the membership), and 14 questions to elicit information about types of organisations and roles in which participants were employed (categorical responses based on four domains of specialist professional knowledge) (Riley et al., 2020); level of education; current and previous experience as an investigator in research; interest in future research participation, including as a professional development activity or for a higher education degree and/or mentorship and what barriers impeded involvement in research projects. Most questions (15) were categorical, and three were open-ended to accommodate free-text responses.
Data collection
The eligible population was alerted via notices in HIMAA’s electronic member newsletter, distributed directly to all members, and its social media fora (Linked In, Facebook) to watch for the forthcoming survey. An electronic link to the Participant Information Form and Survey was subsequently distributed to the HIMAA membership by the membership officer so that none of the research team needed access to the membership email list, thereby protecting the privacy of individual members and ensuring participant anonymity. Recipients were requested to complete the survey only once.
Data analysis
Descriptive analyses of categorical variables were performed in Microsoft Excel. HIMAA provided de-identified summary data on the membership: age group, member type, gender and member country. Using characteristics of age, sex and state/territory, the achieved sample was compared to the membership population to test how representative the respondents were of the national sample frame. Qualitative analyses of open-ended questions were undertaken using a process of data categorisation, wherein similar responses were grouped under broader categorical headings based on their content.
Ethics approval
The project was approved by the Human Research Ethics Committee of The University of Sydney (Protocol No. 2022/385).
Results
One hundred and sixty-eight HIMAA members submitted a response to the survey; of these, 24 completed only the items requesting demographic details and 22 provided no data, leaving a sample of 122 respondents who fully completed the survey. Ten (10) of these were undergraduate or masters students, who reported having had no experience in the profession; these data were analysed separately. The remaining 112 responses constituted the denominator for the figures provided in this article.
Table 1 outlines the demographic characteristics of the respondents. To determine the representativeness of the sample, the test of representation using demographic variable comparisons produced the following (where p < 0.05 = significant difference): members’ age χ2 = immeasurable; members’ sex χ2(1) = 3.026; p = 0.082; member’s state/territory χ2(7) = 5.504; p = 0.599; membership status χ2(5) = 6.673; p = 0.144.
Demographic characteristics of respondents (excluding students).

Other*: Associate Diploma in Medical Record Administration (n = 3); Bachelor Honours (n = 1).
HIS**: (Hospital) Health Information Service.
Almost 91% (n = 102) of respondents had completed university qualifications, the majority being health information management degrees. The remaining 9% (n = 10) had completed a Vocational Education and Training (VET)/Technical and Further Education (TAFE) clinical coding certificate. Almost 50% of respondents had 20 or more years of professional experience, and almost 70% had 10 or more years of professional experience. The majority of respondents (53%) worked in public health services, 12% in private health services and 10% in each of private information technology/health companies and the academic/higher education sector. When roles were grouped within the six broad domain categories of health classification, health informatics, health information science and management, health data analytics/research, academic/higher education and “other,” it was found that over one-third of respondents (37.5%) worked in health classification or clinical coding. Almost 30% (n = 32) were engaged in the area of health information science and management; and 13% (n = 15) of respondents identified as working in “other” broad role categories: these responses included three people who worked across multiple domains, three who worked in allied health or nursing roles and others in ad hoc positions, ranging from Chief Executive Officer to Product Manager to Safety and Quality Manager.
Research experience
Most respondents (64.3%, n = 72) reported no research involvement, while 35.7% (n = 40) had experience as part of a research team. Among those with experience, most had limited involvement in research, with 62.5% (n = 25/40) participating in fewer than five studies, while a smaller group (37.5%, n = 15/40) had high involvement with five or more studies. Respondents could nominate up to three areas of previous research, with the total number of previous research topics documented equalling 86. The most commonly reported area of research was Clinical Research and Patient Outcomes (30.2%, n = 26) with foci on areas such as oncology, cardiology and clinical trials research (Table 2). Clinical Coding and Classification Systems (15.1%, n = 13) constituted the second most commonly reported area, with foci on topics including advancements in coding practices, accurate medical data, clinical costing and audit roles. Similarly, 14.0% (n = 12) of responses indicated experience in Health Information Technology and Systems research, focusing on health data interoperability, the impact of IT systems on patient care and the use of EMRs. Workforce Development and Education represented another area of research (14.0%, n = 12), with respondents reporting involvement in topics relating to education delivery, training and workforce planning, specifically related to health information management and coding.
Areas of previous research.

Research interest and motivation
Respondents were asked whether or not they were interested in undertaking research and, if so, why were they were interested. It was possible to select more than one reason, and an average of 1.2 “reasons” were selected per respondent. Of those interested in research, the motivation varied. The most common reason was workplace-related, with 38.4% (n = 43) citing industry and organisational information solutions. Approximately 20% (n = 22) were driven by educational goals, such as pursuing a master’s degree, PhD, or professional doctorate and 27.7% (n = 31) expressed personal interest outside formal education. Another 38.4% (n = 43) were unsure or not interested in research involvement.
Access to research information, workplace research requirements and practical research involvement
Respondents were asked to indicate how they access research information for their usual work activities. Multiple responses were allowed: as shown in Figure 1, the most frequently utilised method was general web searches, with 83.9% (n = 94) of respondents indicating this as their primary source. Reputable research databases such as PubMed and MEDLINE were the second most utilised resource, and 39.3% (n = 44) of respondents accessed research information through the HIMJ. A smaller proportion (8.9%, n = 10) reported that accessing research information was not applicable to their work.
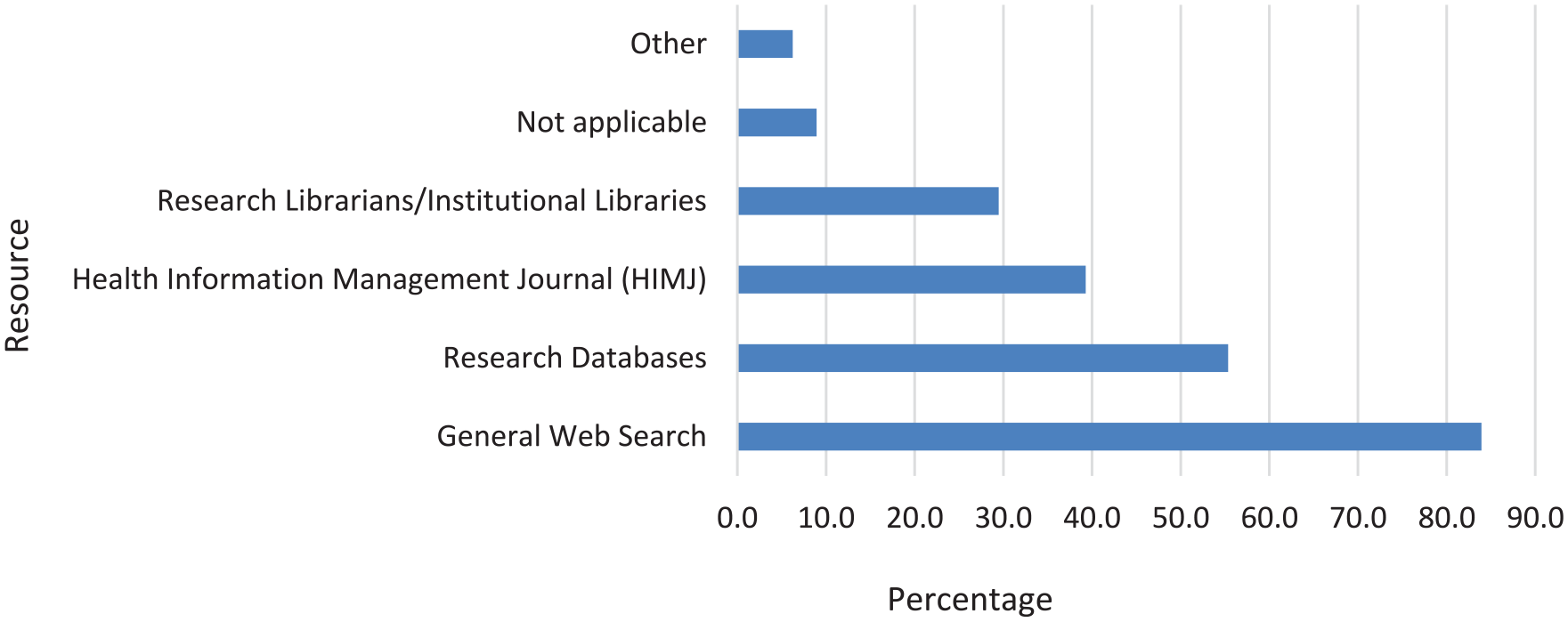
How research information is accessed for work.
The majority (73.9%, n = 82) of respondents indicated that research was not a component of their role; however, just over half (51.3%, n = 61) of all respondents reported being approached, often or sometimes, by other researchers to access and analyse data in the workplace. Research was a requirement of the job for 18.9% (n = 21) of respondents. A minority (7.2%, n = 8) were unsure whether research was a component of their role.
Barriers to research
Barriers to respondents’ engagement in research projects comprised personal, organisational and logistical challenges, with an average of 2.7 barriers nominated per respondent. Thirteen respondents reported no barriers and 22 nominated a single barrier, indicating that over 70% of the respondents faced multiple challenges when considering participation in research activities. As shown in Table 3, the most commonly reported barrier was lack of time, cited by 62.5% (n = 70) of respondents. Financial barriers, lack of confidence and uncertainty about who to approach or how to become involved in research were each cited as challenges by approximately one-third of the respondents. Approximately 28% of respondents reported lack of mentorship as a barrier; correspondingly, a substantial proportion (62.5%, n = 70) were unsure or not interested in being mentored by HIM researchers. Lack of organisational support was a barrier for 21% of respondents.
Barriers to research involvement.

Topics of research interest or research for professional development?
In response to the question, “Would you participate in research as a Professional Development activity?” 59.2% (n = 71) of respondents provided a positive response. A further 9.2% of respondents expressed disinterest, and a notable 31.7% were unsure.
Respondents were invited to nominate up to three areas of interest in their professional practice that would benefit from research (Table 4). A diverse range of areas emerged within the field of health information management. These included Clinical Coding and Classification Systems (13.3%, n = 18) and eHealth (12.6%, n = 17). Governance/Legislation/Standards were nominated by 9.6% (n = 13). Finally, 10.5% (n = 14) of responses were categorised as “not elsewhere classified” as they were not clearly aligned with a distinct area of research interest. They included non-viable or non-specific responses such as “unsure,” “none that I can think of right now,” “skill development” and “knowledge base”; and 14% (n = 19) of respondents indicated interest in developing their own research skills, particularly in areas such as data analytics, statistics, database searching and scientific writing.
Respondents’ perceptions of areas of professional practice that would benefit from research.

Discussion
Our study aimed to identify the research investigator involvement, experience and aspirations of Australia’s health information management workforce. The findings highlight the diversity of health sector organisations and roles in which HIMs and other health information practitioners are employed, thereby reflecting the wide applicability of the professional skill-set(s).
It is encouraging that approximately two-thirds of the respondents expressed interest in participating in, or reported having had some experience of, research and that 59% were interested in participating in research as a professional development activity. The fact that 41% of the respondents were unsure or disinterested in participating in research as a professional development activity suggests an opportunity for future exploration of the factors contributing to this uncertainty. The findings suggest that the respondents’ acknowledged lack of research-related skills constitutes a “barrier” to their research involvement, and that HIMs’ greater knowledge of, and confidence in, applying research methods would support increased research investigator involvement.
An increased volume of research by health information management practitioners within their workplace context on topics relevant to their roles (e.g., clinical classification and EMRs) is necessary to increase the evidence-based knowledge of the profession. This is especially pressing in light of the findings of Riley et al (2024) that HIMs and CCs were included as authors in only 3.8% of studies that used ICD-10 or ICD-10-AM codes in peer-reviewed research undertaken in Australia between 2012 and 2022.
The main reason for the respondents’ interest in undertaking research was related to finding information solutions for their industry or organisation. The current work situation of one-fifth of the respondents required their involvement in research. At the other end of the spectrum, a similar proportion reported “lack of organisational support” as a barrier, which may signify that such support plays a crucial enabling role in research engagement; it also suggests that, given a conducive environment, this sub-group might potentially engage in workplace-based research activities. Notwithstanding the finding that almost four-fifths of the respondents’ work roles did not require them to undertake research, over half of all respondents reported being asked by researchers within their workplace to access and analyse data. This discrepancy points to a disjunction between the formal role/position requirements of HIMs, who comprised the large majority of the respondents, and the reality of the actual need for their practical involvement in workplace-based research activities.
The finding that respondents predominantly referred to undertaking a general web search to source research information rather than utilising reliable, evidence-based sources that may or may not be peer-reviewed, suggests a need for practitioners to be upskilled in research techniques. It also reinforces the need for the existing research-related competencies in HIMAA’s (2023) profession-entry level HIM Professional Competency Standards, which closely inform university curricula for HIM-qualifying degrees. Likewise, the fact that almost 40% of the respondent HIMs accessed research information from the HIMJ reflects the journal’s importance for the profession.
Over 30% of the research topics reported by the 35.7% of respondents who had research investigator experience related to “Clinical research and patient outcomes.” Given that 75% of the roles of all respondents related to HIMs’ core professional functions of clinical coding, health information technology work and health information science and management, this statistic may represent, in part, the work of HIM-respondents involved in disease registry, hospital- or university-based research, which may be more likely to be clinical in focus and to incorporate the HIM in the broader clinical research team.
Where the HIM practitioner role in research has been explored, their input has been acknowledged positively. Seeley et al. (2010), in the United Kingdom, found co-ordination, setting-up mechanisms for collaborative learning through information sharing and using the theoretical frameworks (taken from their literature review) to help guide implementation, were important elements of the health information management role in a large multidisciplinary research project to improve services for head injury. Notwithstanding this, the dearth of literature specific to health information management professionals’ participation in research prompts the broader consideration of this concern in other health professions. In examining the factors that constrained nurses from research investigator participation, Roxburgh (2006) found similar reasons to some reported in our study, that is, lack of time, lack of peer support, and limited skills and knowledge about the research process. Lorenzetti et al (2012), while focused on clinical librarians as “information professionals,” similarly reported barriers to their research investigator participation including the lack of time, organisational support, competencies and confidence in engaging with members of research teams on an equal footing.
Comparisons with the findings of a previous convenience survey of the HIMAA membership (Kemp et al., 2020) that investigated the research culture of the health information management profession, were anecdotally informative, but as that survey was extended through snowball sampling (potentially to other non-HIMAA members), the representativeness of the sample could not be established, and the reliability therefore unable to be assessed. While the respondents to the current survey reported various barriers to their research investigator involvement, historically health information management practitioners have made a significant contribution to the body of knowledge, both through research participation as an investigator (Campbell and Giadresco, 2020; Kwan et al., 2020; Shepheard et al., 2019; Considine et al., 2017) and by sharing their practice-based expertise and experiences (Hay et al., 2020) through publication. The level of support given to these authors within their organisations is unknown, but should be encouraged to the benefit of the entire profession.
Mdletshe (2023) cited similar challenges to the medical imaging profession as those affecting areas of the health information management profession and a parallel lack of professional involvement in research output. He proposed the establishment of a “research culture” that involves commitment and support from management within organisations; creating an environment of reflective evidence-based practice; appointing research postdoctoral leads that promote research through helping students develop awareness of the research process and the value of evidence-based practice; supporting and taking pride in colleagues who undertake research, with a positive discourse and attitude towards research activities in the profession; supporting continuing academic education and professional development through management support for Masters- and PhD-levels of education and creating a culture of valuing research across knowledge fields and mutual interest in collaboration in research. It is encouraging that HIMAA is already well progressed in implementing one of the key strategies recommended by King et al. (2018: 133), namely, encouragement of its members’ research “through funding opportunities”; however, there remains scope to adopt the King et al. (2018: 133) recommendation for “showcasing new evidence for practice.”
The recommendations of Lorenzetti et al (2012) may also be pertinent to the health information management profession: building research capacity may require organisational support; peer-mentoring can enhance individual research skills; willingness to work “outside one’s comfort zone” may be a prerequisite for involvement in interdisciplinary research and developing the competencies and confidence necessary to engage as an equal with other researchers can positively impact successful research team participation.
Limitations
The low response rate (12.7%) presented a potential limitation; however, when a standard error of ±10%, rather than ±5%, was applied, the response rate was demonstrated to be representative. Another limitation concerned possible selection bias, whereby members of the study population who were already interested in research were possibly predisposed to participate in a survey about research interest and opportunities. It was also possible that, owing to hospital firewalls and other security mechanisms, members had provided HIMAA with more than one email address; in the event that some members may have received more than one invitation to participate, this limitation was mitigated by the provision of written advice to complete the survey only once.
Conclusion
Following our determination of the facilitators and barriers to research participation, strategies can now be developed to build the enablers and resolve the barriers to this significant aspect of HIMs’ and other health information management practitioners’ professional development. The HIMs’ unique professional skill-set underpins the profession’s identity, and research into the profession’s competency domains should be undertaken by HIMs. The potential significance of this study will lie in the expansion of the profession’s knowledge base to build capacity for relevant investigations about health information management and clinical coding and classification, to be undertaken by these practitioners, about their own profession. We therefore recommend increased efforts in HIMAA’s formal recognition, promotion and support for HIMs’ and other health information management practitioners’ involvement in research as part of their professional role. Greater recognition of research as an advantageous, valuable professional development activity will strengthen the health information management profession by enriching the next generation of its practitioners, educators and researchers.
Supplemental Material
sj-docx-1-him-10.1177_18333583251322985 – Supplemental material for Health information management professionals’ investigator involvement in research: barriers and facilitators
Supplemental material, sj-docx-1-him-10.1177_18333583251322985 for Health information management professionals’ investigator involvement in research: barriers and facilitators by Joan Henderson, Merilyn Riley, Benjamin Brown, Mary Lam, Stephanie Gjorgioski, Melanie Tassos, Jenny Davis and Kerin Robinson in Health Information Management Journal
Footnotes
Acknowledgements
The authors thank Nicole Payne (Healthscope, Australia) for assistance in the survey design, and Ms Jae Redden (former Chief Executive Officer, HIMAA) and her staff for distributing the survey.
Accepted for publication February 8, 2025.
Author contributions
JH, ML, KR, BB, JD designed the study; JH, KR researched the literature; JH, BB, ML, MR, JD, KR, SG, MT contributed to the survey; BB set up and managed REDCap; JH, MR, SG, MT, ML provided statistical advice; MR, JH, KR, SG, MT extracted and analysed the data; MR, ML, JH, KR, SG, MT reviewed the analyses; JH, MR, KR, SG, MT, JD contributed to the manuscript drafts and KR finalised the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors received a small competitive grant from the Health Information Management Association of Australia to support the conduct of this research.
ORCID iDs
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
