Abstract
Cerebrovascular diseases are pathological conditions involving impaired blood flow in the brain, primarily including ischaemic stroke, intracranial haemorrhage, and subarachnoid haemorrhage. The nucleotide-binding and oligomerisation (NOD) domain-like receptor (NLR) family pyrin domain (PYD)-containing 3 (NLRP3) inflammasome is a protein complex and a vital component of the immune system. Emerging evidence has indicated that the NLRP3 inflammasome plays an important role in cerebrovascular diseases. The function of the NLRP3 inflammasome in the pathogenesis of cerebrovascular diseases remains an interesting field of research. In this review, we first summarised the pathological mechanism of cerebrovascular diseases and the pathological mechanism of the NLRP3 inflammasome in aggravating atherosclerosis and cerebrovascular diseases. Second, we outlined signalling pathways through which the NLRP3 inflammasome participates in aggravating or mitigating cerebrovascular diseases. Reactive oxygen species (ROS)/nuclear factor kappa-light-chain-enhancer of activated B cells (NF-κB), ROS/thioredoxin-interacting protein (TXNIP) and purinergic receptor-7 (P2X7R) signalling pathways can activate the NLRP3 inflammasome; activation of the NLRP3 inflammasome can aggravate cerebrovascular diseases by mediating apoptosis and pyroptosis. Autophagy/mitochondrial autophagy, nuclear factor E2-related factor-2 (Nrf2), interferon (IFN)-β, sirtuin (SIRT), and phosphoinositide 3-kinase (PI3K)/protein kinase B (AKT) reportedly alleviate cerebrovascular diseases by inhibiting NLRP3 inflammasome activation. Finally, we explored specific inhibitors of the NLRP3 inflammasome based on the two-step activation of the NLRP3 inflammasome, which can be developed as new drugs to treat cerebrovascular diseases.
Keywords
Recently, in-depth investigations on the inflammasome complex have presented evidence indicating its association with cerebrovascular diseases. The NLRP3 inflammasome is one of the most extensively studied inflammasomes. Several researchers have reported that expression of the NLRP3 inflammasome promotes the progression of atherosclerotic lesions and increases the risk of stroke (Li et al., 2014; Kastbom et al., 2015; Paramel Varghese et al., 2016; Abdul-Muneer et al., 2017; Cheng et al., 2018). Activation of the NLRP3 inflammasome causes aggravation of stroke, while inhibition improves clinical symptoms and prognosis. The objective of this review is to summarise the pathological mechanism and signalling pathways of the NLRP3 inflammasome in aggravating cerebrovascular diseases to target these signalling pathways and the two-step activation of the NLRP3 inflammasome and develop new drugs for cerebrovascular diseases in the future.
Introduction to Inflammasome
The inflammasome is a protein complex composed of a sensor protein called pattern recognition receptors, an adaptor protein (an apoptosis-associated speck-like protein containing a caspase activation and recruitment domain [CARD], apoptosis-associated speck-like protein [ASC]) and an effector protein (caspase-1 in canonical inflammasome, caspase-4,5,11 in non-canonical inflammasome). The inflammasome is capable of regulating innate immune signalling. The pattern recognition receptors response to damage-associated molecular patterns (DAMPs) or pathogen-associated molecular patterns (PAMPs), results in the accumulation and activation of caspase-1, which cleaves pro-interleukin (IL)-1β and pro-IL-18 into their active forms. IL-1β, a pro-inflammatory cytokine, regulates inflammation in various disorders, especially chronic inflammatory diseases, including rheumatoid arthritis, neurodegenerative disorders, Crohn disease, asthma and so on (Wang, Hu, et al., 2018). IL-18 is a co-stimulatory cytokine that mediates adaptive immunity and is associated with Th1, Th2 and IFN-γ. IL-18 primarily mediates systemic lupus erythematosus, macrophage activation syndrome, rheumatoid arthritis, type 1 diabetes, Crohn's disease, psoriasis and graft-versus-host disease (Dinarello, 2009; He, Hara, et al., 2016; Kelley et al., 2019).
Inflammasome Category
According to the pattern recognition receptors, inflammasomes can be categorised into three categories, absent in melanoma 2 (AIM2), IFN-γ inducible protein 16 (IFI16), and various NLR subsets (Xiao, 2015; Shim and Lee, 2018). AIM2 and IFI16 proteins are double-stranded deoxyribonucleic acid (dsDNA) sensors containing the N-terminal PYD domain and the C-terminal DNA-binding domain of the haematopoietic interferon-inducible nucleus (Xiao, 2015). The difference between AIM2 and IFI16 is the number of DNA-binding domains of the interferon-inducible nucleus: AIM2 has one, and IFI16 has two (Latz et al., 2013). IFI16 induces the production of IFN-β and IL-1 through activation of stimulators of interferon genes and inflammasomes, respectively (Xiao, 2015; Chen, He, et al., 2018). AIM2 initiates inflammatory responses to dsDNA (Latz et al., 2013; Xiao, 2015; Chen, He, et al., 2018). Furthermore, pattern recognition receptors can be sub-classified into two main categories according to their cellular localisation. a) Toll-like receptors and C-type lectin receptors, which are located in the plasma membrane and endosomes, recognise PAMPs and DAMPs outside the cell. b) Retinoic acid-inducible gene-I-like receptors, AIM2-like receptors, NLRs and cytosolic sensor cyclic guanosine monophosphate-adenosine monophosphate synthase which are located intracellularly (Moossavi et al., 2018).
Structure of NLRs and NLRP3 Inflammasome
NLRs consist of three components: a) C-terminal. When the leucine-rich repeats (LRRs) are in the resting state, the C-terminus inhibits NLR protein function and alters the conformation after recognising stimuli to remove the inhibitory effect on the NLR protein (Menu and Vince, 2011). b) A central nucleotide-binding and oligomerisation domain (NACHT) exists in all NLRs. The NACHT domain has ATPase activity and is considered essential for NLRP3 oligomerisation (Latz et al., 2013; Kelley et al., 2019). c) An N-terminal effector domain consisting of either a CARD, Pyrin or baculoviral inhibitor of apoptosis protein repeat (BIR) domain before the NACHT domain (Ting and Davis, 2005). Furthermore, NLRs can be sub-classified into two groups based on the N-terminal domain: a) NLRP containing pyrin and b) NOD-like receptor subfamily C (NLRC), which contains CARD (Moossavi et al., 2018). These N-terminal domains initiate specific downstream signalling cascades through homotypic protein interactions. The NLRP3 inflammasome is a well-known inflammasome complex encoded by the Nlrp3 gene. NLRP3 is composed of three components: a) the NLRP3 scaffold (an innate immune receptor, composed of three domains: C-terminal LRRs, the NACHT domain, and an N-terminal PYD effector domain). NACHT consists of a nucleotide-binding domain (NBD), helical domain (HD) 1, winged-helix domain (WHD) and HD2 (Sharif et al., 2019). b) PYCARD (containing an N-terminal PYD and a C-terminal CARD), usually called ASC, activates caspase-1. c) The cysteine protease precursor pro-caspase-1 (containing a CARD and a caspase domain) (Figure 1) (Liu, Zeng, et al., 2018; Moossavi et al., 2018). The NLRP3 inflammasome is located in immune cells, including antigen-presenting cells macrophages, dendritic cells, and neutrophils in the spleen, as well as monocytes (Moossavi et al., 2018). In the brain, the activated NLRP3 inflammasome and ASC are mainly derived from microglia and neurons respectively (Lammerding et al., 2016).
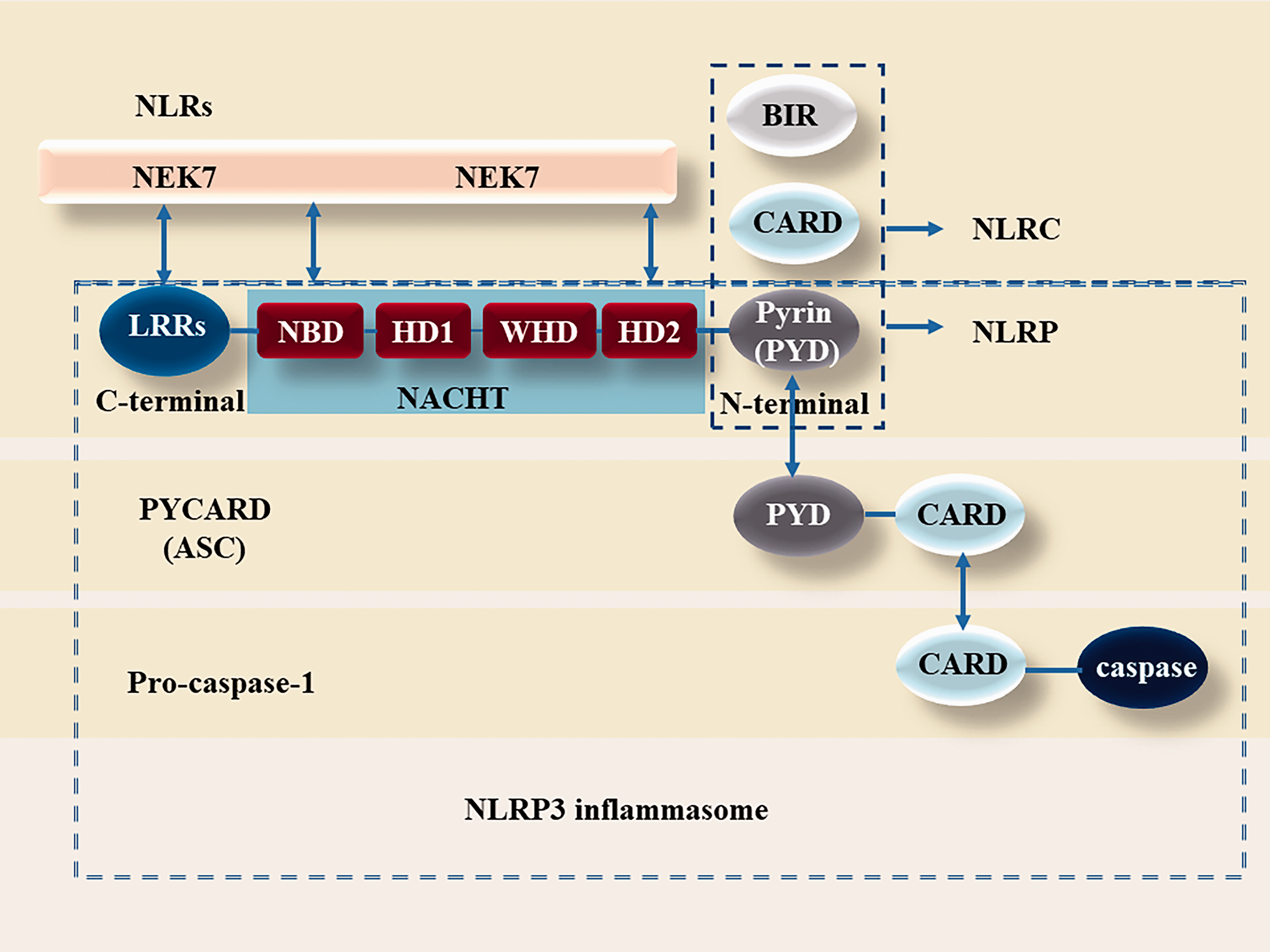
Structure of NLRs and NLRP3 Inflammasome. NLRs consist of three components, the C-terminal LRRs, the central NACHT, which consists of NBD, HD1, WHD, and HD2, and the N-terminal domain. The N-terminal domain can be Pyrin, CARD, or BIR. When the N-terminal part is CARD, it is called NLRC inflammasome, and when the N-terminal part is Pyrin, it is called NLRP inflammasome. The NLRP3 inflammasome is composed of three parts, the first part is NLRP3 composed of LRR-NACHT-Pyrin/PYD, the second part is PYCARD composed of PYD-CARD, also known as ASC, and the third part is pro-caspase-1 composed of CARD-Caspase. These three parts form NLRP3 inflammasome through the interaction of PYD-PYD and CARD-CARD. NEK7 is a newly discovered inflammasome component of NLRP3 in recent years, which is related to ROS-induced priming. Part of NEK7 binds to LRRs of NLRP3, and part of NEK7 binds to NBD and HD2 of NACHT. Abbreviations: NLRs: NOD domain like receptor, LRRs: leucine-rich repeats, NACHT: nucleotide binding and oligomerization domain, NBD: nucleotide-binding domain, HD1: helical domain 1, WHD: winged helix domain, HD2: helical domain 2, CARD: caspase activation and recruitment domain, BIR: baculoviral inhibitor of apoptosis protein repeat, NLRC: NOD-like receptor subfamily C, NLRP: NOD domain like receptor family contain pyrin domain, PYD: pyrin domain, PYCARD/ASC: apoptosis-associated speck-like protein containing a CARD, NEK7: NIMA-related kinase 7.
Recently, never in mitosis gene A-related kinase 7 (NEK7) has been identified as a component of the NLRP3 inflammasome to sense reactive oxygen species (ROS), which might activate NLRP3 by influencing the oxidation of protein thiol groups (Gross et al., 2016). Half of NEK7 was found to bind to LRR through its C-terminal lobe, while the other half was linked to the HD2 and NBD regions (Figure 1) (El-Sharkawy et al., 2020). ATP binds to the NBD domain, which phosphorylates S195 of NEK7 allowing NLRP3 to adopt its active conformation for oligomerization (El-Sharkawy et al., 2020). NEK7 binds to NLRP3 during the priming and activation interphase (El-Sharkawy et al., 2020). With the discovery of NEK7, new insights have emerged into the structure of the NLRP3 inflammasome. Hafner-Bratkovic et al. (2018) proposed that LRR is not necessary for NLRP3 inflammasome activation (Hafner-Bratkovic et al., 2018). The structure of the NLRP3 inflammasome may be more complex than currently understood and will require further exploration by researchers.
Activation of the NLRP3 Inflammasome—A Two-Step Process
Unlike other pattern recognition receptors, the basal level of the NLRP3 inflammasome is low in immune cells (Jo et al., 2016). NLRP3 can bind to the pyrin domain of ASC, consequently recruiting pro-caspase-1 through CARD-CARD interactions. Pro-caspase-1 recruitment results in the release of the active catalytic p20 and p10 caspase-1 fragments, cleaving the inflammatory cytokines pro-IL-1β and pro-IL-18 to its biologically active 17 kDa fragment (Menu and Vince, 2011).
Activation of the NLRP3 inflammasome is a two-step process consisting of “priming” and “activation.” The first signal in inflammasome activation, called “priming”, is induced by the TLR/nuclear factor kappa-light-chain-enhancer of activated B cells (NF-κB) pathway (Toma et al., 2010). NF-κB can be activated either by toll like receptors, which sense PAMPs and DAMPs or environmental stress, or by cytokines such as tumour necrosis factor α (TNF-α). Furthermore, NF-κB leads to the upregulation of NLRP3, pro-IL-1β, and pro-IL-18 expression (Saha et al., 2020). The activation threshold of NLRP3 is regulated by both post-translational and transcriptional activation of the NLRP3 gene (Latz et al., 2013). NLRP3 expression is a limiting step for NLRP3 inflammasome activation in macrophages (Bauernfeind et al., 2009). After priming, although NLRP3 remains inactive, it is more responsive to danger signals (Latz et al., 2013; Herman and Pasinetti, 2018; Ge et al., 2020). The second signal is called a “trigger” or “activation.” Under specific conditions, the NLR is activated and combined with ASC and pro-caspase-1 in a cascade reaction to form a complex structure. Simultaneously, this complex structure triggers pro-caspase-1 self-cleavage into caspase-1. Then, caspase-1 cleaves pro-IL-1β, pro-IL-18, and the pore-forming molecule gasdermin-D into their active forms (Gaidt and Hornung, 2017; Song and Li, 2018). Three main conditions trigger a second signal. a) Potassium efflux, considered the most crucial; b) ROS induced by DAMPs or PAMPs; c) Cathepsin B released by lysosomes (Shao et al., 2015). Furthermore, calcium, sodium, and chloride efflux, as well as mitochondrial dysfunction, play vital roles in the second signal of NLRP3 activation (Menu and Vince, 2011; Kelley et al., 2019). DAMPs that activate the NLRP3 inflammasome can be classified into host-derived DAMPs such as hyaluronan, cholesterol crystals, extracellular ATP, β-amyloid, DNA and gout-associated monosodium urate crystals, and environmental DAMPs including asbestos, silica, nanoparticles, skin irritants and alum adjuvant. PAMPs include pathogen-associated RNA, DNA, pore-forming toxins and peptidoglycans (Jo et al., 2016).
NLRP3 Inflammasome/Caspase-1/IL-1β Pathway Plays an Important Role in the Pathogenesis of Cerebrovascular Diseases
NLRP3 inflammasome/caspase-1/IL-1β pathway is an important pathway for the production of IL-1β. IL-1β levels are found to increase after cerebral infarction and cerebral haemorrhage (Yamasaki et al., 1995; Wei et al., 2014; Wei, Li, et al., 2019). Reportedly, IL-1β promotes cerebral oedema and increases the cerebral infarct size by inducing neutrophil infiltration and adherence at the infarct site (Yamasaki et al., 1995). The infarct size, cerebral oedema, and neurological deficit of middle cerebral artery occlusion were significantly improved by inhibiting or knocking out IL-1β (Yamasaki et al., 1995; Boutin et al., 2001; Caso et al., 2007). IL-1β may be associated with cerebral oedema following intracerebral haemorrhage (Wei et al., 2014). The primary cause of a subarachnoid haemorrhage (SAH) is an aneurysm. IL-1β is reportedly expressed in cerebral arteries of early aneurysm model mice (Moriwaki et al., 2006), and the expression of IL-1β can aggravate SAH (Fontanella et al., 2010). IL-1β gene knockout reduces the incidence of mature experimental cerebral aneurysms (Moriwaki et al., 2006). Activation or blocking of NLRP3 inflammasome or capase-1 can affect the production of IL-1β, and thus affect cerebrovascular diseases.
Caspase-1 is the only enzyme in mice that activates IL-1β, termed the IL-1β converting enzyme (Friedlander et al., 1997). Knockout of the IL-1β converting enzyme family significantly reduced the infarct volume, cerebral oedema, and neurological deficits in middle cerebral artery occlusion (Friedlander et al., 1997; Schielke et al., 1998). Inhibition of caspase-1 activation can reduce cerebral oedema after intracerebral haemorrhage, downregulate IL-1β levels, and improve neurological function deficits (Liang et al., 2019).
The NLRP3 inflammasome is an activator of caspase-1. Levels of the NLRP3 inflammasome are found to be increased in cerebral infarctions (Wang, Yao, et al., 2020). In SAH, activation of the NLRP3 inflammasome/caspase-1/IL-1β pathway increases blood-brain barrier permeability, microglial accumulation, and neuronal apoptosis (Li, Dong, et al., 2020). Inhibition of the NLRP3 inflammasome/caspase-1/IL-1β pathway can reduce the volume of the cerebellar infarct, reduce secondary brain injury and inflammation after cerebral hemorrhage, protect the integrity and permeability of the blood-brain barrier, reduce cerebral oedema of cerebral infarction, cerebral haemorrhage and SAH, and reduce the loss of neurological functions (Ismael et al., 2018; Song and Zhang, 2019; Xu, Li, et al., 2019).
It has been suggested that the NLRP3 inflammasome/caspase-1/IL-1β pathway plays an important role in the pathogenesis of cerebrovascular diseases and is an effective target for the treatment of cerebrovascular diseases.
Pathogenic Mechanisms Following Cerebrovascular Diseases
The pathological basis of both ischaemic and haemorrhagic stroke involves changes in the structure and function of arterioles, including fibrinoid changes, lipohyalinosis, necrosis, and microaneurysm formation (Prabhakaran and Naidech, 2012). Similar risk factors such as hypertension, diabetes mellitus, dyslipidaemia, and smoking can induce the above pathological changes in the arterioles, resulting in arteriole occlusion and/or rupture (Prabhakaran and Naidech, 2012). The typical cause underlying a SAH is an intracranial aneurysm, and unlike cerebral infarction and intracerebral haemorrhage, blood enters into the subarachnoid space of the brain and spinal cord (Tso and Macdonald, 2014). However, different types of stroke present unique pathological changes, which will be briefly introduced in the following subsections.
Ischaemic Stroke
Focal cerebral ischaemia refers to a sudden decrease or loss of blood supply to a specific brain region, resulting in neurological impairments. Based on differences in residual blood flow, focal cerebral ischaemia can be divided into the ischaemic core and penumbra. Embolism, thrombosis, and relative hypoperfusion can result in an absolute cerebrovascular blood flow of less than 1 mL/g/min, leading to almost immediate ischaemic hypoxia in the brain tissue (Nedergaard and Dirnagl, 2005; Lakhan et al., 2009). This area is referred to as the ischaemic core, surrounded by brain tissue with reduced blood flow, known as the penumbra. Blood flow in the penumbral area is usually maintained at 2–4 mL/g/min (Nedergaard and Dirnagl, 2005). The penumbra is characterised by the preservation of ion channel function and metabolism, with no electrical activity (Nedergaard and Dirnagl, 2005; Ramos-Cabrer et al., 2011).
Pathology of the Ischaemic Core: Oxidative Stress and Excitatory Toxicity
In the ischaemic core, the decreased blood flow leads to insufficient oxygen and glucose supply in the brain tissue, triggering a series of cascading reactions, including sodium-potassium pump dysfunction, extensive depolarisation of neuronal cell membranes, activation of glutamate and voltage-gated calcium channels, the influx of calcium ions in neurons, and release of glutamate into the synaptic cleft (Zhang et al., 2006; Rashidian et al., 2007; Alishahi et al., 2019). Intracellular calcium overload promotes nitric oxide and ROS production, mitochondrial dysfunction, endoplasmic reticulum stress responses, activation of calpain proteases, and ultimately neuronal death (Rashidian et al., 2007; Hossmann, 2009; Ramos-Cabrer et al., 2011). Oxidative stress plays an important role in neuronal injury following cerebral ischaemia. Several factors can lead to oxidative stress during cerebral ischaemia, including intracellular calcium, zinc, extracellular glutamate elevation, anaerobic glycolysis, and mitochondrial dysfunction (Hossmann, 2009; Alishahi et al., 2019). Oxidative stress can mediate neuronal death by destroying mitochondria, the endoplasmic reticulum, and cellular components, promoting calcium overload, excitotoxicity, reperfusion injury, and inflammation (Hossmann, 2009; Lakhan et al., 2009; Alishahi et al., 2019).
Glutamate is an excitatory neurotransmitter. Following the release of glutamate into the synaptic cleft, the presynaptic neuronal reuptake of glutamate occurs. Glutamate reuptake is an energy-intensive process, and energy consumption leads to severe disruption of glutamate transporters, causing excitotoxic effects that trigger neuronal death (Castillo et al., 2016; Perez-Mato et al., 2019). Glutamate can also overstimulate glutamate receptors, promote calcium ion influx, and induce mitochondrial ROS production (Castillo et al., 2016; Alishahi et al., 2019; Perez-Mato et al., 2019).
Ischaemic Penumbra—The Region Whose Progression Is Affected by the Ischaemic Core
Penumbra formation is influenced by several factors, including excitotoxicity, peri-infarct depolarisations, spreading depression, lactacidosis, microcirculatory disturbances, and flow-metabolism uncoupling (Back and Schuler, 2004; Nedergaard and Dirnagl, 2005; Lakhan et al., 2009). In the ischaemic core, glutamate can mediate peri-infarct depolarisations or spreading depression, cause acidosis, increase energy demand and neurotransmitter leakage, affect the survival of penumbral cells, and gradually expand the infarct size (Ramos-Cabrer et al., 2011). The ischaemic core can also promote penumbral cell death through numerous mechanisms, including oxidative stress, apoptosis, inflammatory cytokine release, adhesion molecule expression, and matrix metalloproteinase production (Ramos-Cabrer et al., 2011). Penumbral tissues can tolerate several hours of hypoperfusion, and neurological function can be fully restored with timely restoration of blood flow (Lakhan et al., 2009); Therefore it is crucial to restore blood flow before irreversible damage occurs to penumbral tissues.
Post-Ischaemic Inflammation—A Double-Edged Sword
Post-ischaemic inflammation is a dynamic process involving various inflammatory cells, chemokines, and proteases, which play an important role during the course of cerebral ischaemia. Post-ischaemic inflammation is a double-edged sword, which not only aggravates cerebral oedema in the early stage of ischaemia but also promotes tissue recovery during the recovery stage (Zheng and Yenari, 2004; Shichita et al., 2012). During the early stages of ischaemia, excitotoxic events and cytotoxic substances appear to be involved in the induction of an in situ post-ischaemic inflammatory reaction (Zheng and Yenari, 2004). In situ inflammation induces the expression of adhesion molecules on endothelial cells of the blood-brain barrier, which further promotes the migration and adhesion of white blood cells from the peripheral blood into brain tissues (Lakhan et al., 2009). Increased expression of chemokines is also involved in the aggregation of inflammatory cells (Lakhan et al., 2009). The aggregation and adhesion of inflammatory cells can damage the integrity of the blood-brain barrier endothelial cells and microvessels. Furthermore, proinflammatory cells can increase the blood-brain barrier permeability directly through endothelial cells (Lakhan et al., 2009; Shichita et al., 2012). Increased matrix metalloproteinases reportedly impair the blood-brain barrier integrity after stroke and are associated with vasogenic oedema (Lakhan et al., 2009). During the recovery period, inflammatory cells infiltrating the brain tissue can remove necrotic cells and tissue fragments, promoting tissue repair and regeneration (Shichita et al., 2014).
Intracerebral Haemorrhage
Pathology of Early Intracerebral Haemorrhage: Toxicity of Blood, Oxidative Stress, Brain Edema and Mass Effect
Primary intracerebral haemorrhage occurs in the absence of vascular malformation or brain parenchymal lesions, blood vessel rupture, blood into the brain parenchyma, and may spread to the ventricular system; simultaneously, blood components such as leucocytes, haemoglobin, thrombin, plasmin, complement components, plasma, and fibrin degradation products enter the brain parenchyma (Bai et al., 2020). A few minutes after intracerebral haemorrhage occurrence, toxic components in the blood, such as blood-derived coagulation factors, complement components, immunoglobulins, and other bioactive molecules, present a potent toxic effect on brain cells and promote inflammation and oxidation (Aronowski and Zhao, 2011). After 24 h, red blood cell lysis produces cytotoxic haemoglobin, haem, and iron, which also induce intense oxidative damage to the brain cells (Aronowski and Zhao, 2011). In the early stage of intracerebral haemorrhage, serum protein deposition can lead to cytotoxic oedema, whereas in the late stage, cerebral oedema is mainly vasogenic (Badjatia and Rosand, 2005). The mass effect of haematoma and secondary edema can lead to tissue compression and displacement. Compression of adjacent blood vessels results in local hypoperfusion of brain tissues (Kingman et al., 1987), resulting in pathological changes similar to those in the penumbra area of cerebral infarction.
Secondary Brain Injuries: Toxic Effects of Heme Metabolites and Thrombin
Secondary brain injuries include inflammatory responses, oxidative stress, cytotoxicity and excitotoxicity (Zhu, Wang, et al., 2019). Haem in erythrocytes is released into the brain tissue and metabolised by haem oxygenases. Metabolite iron can result in neuronal loss around blood clots through oxidative damage (Egashira et al., 2015; Dang et al., 2017). Thrombin produced immediately after intracerebral haemorrhage is not only involved in the hemostasis cascade reaction but also the formation of brain oedema. High-dose thrombin can induce inflammation, excitotoxicity, apoptosis, complement system activation, mesenchymal cell proliferation, scar tissue formation, and increase the blood-brain barrier permeability, while extremely low-dose thrombin has a protective effect (Lee et al., 1997; Xi et al., 2006; Zhu, Wang, et al., 2019). Damage to brain tissue by the thrombin-activated complement system is associated with the formation of membrane attack complexes and typical inflammatory responses (Xi et al., 2006). After intracerebral haemorrhage, microglial activation induces an inflammatory response by releasing matrix metalloproteinases, ROS, active nitrogen, inflammatory cytokines, and chemokines, inducing extensive neuronal death (Bai et al., 2020).
Subarachnoid Haemorrhage
Pathology of Early Subarachnoid Hemorrhage—A Vicious Circle Formed by Increased Intracranial Pressure, Hypoperfusion, Cerebral Edema, and Neuroinflammation
SAH is a condition in which blood enters the subarachnoid space of the brain and spinal cord. Blood release, acute reactive congestion, and acute vasospasm during the first 72 h after a SAH can cause early brain damage including increased intracranial pressure, cerebral edema, neuroinflammation, oxidative stress, cell death, neuronal dysfunction, blood-brain barrier disruption, microvascular changes, and transient global cerebral ischaemia (Cahill et al., 2006; Zheng and Wong, 2017; Pang et al., 2019); these pathological changes are mutually promoting. The blood entering the subarachnoid space, together with vasoparalysis and obstruction of cerebrospinal fluid drainage, contribute to increasing the intracranial pressure. Increased intracranial pressure, cerebral vasospasm, and inflammatory cascades lead to whole-brain hypoperfusion (Cahill et al., 2006; Tso and Macdonald, 2014). NLR correlates with cerebral perfusion in the early phase of SAH (Wu et al., 2019). After SAH occurs, microthrombosis formed by platelet aggregation can also aggravate local cerebral hypoperfusion (Tso and Macdonald, 2014; Pang et al., 2019). Whole-brain hypoperfusion can cause a series of pathological changes, including neuronal cell and vascular endothelial cell death, sodium-potassium pump dysfunction, activation of inflammation and apoptosis cascade, oxidative stress response, and matrix metalloproteinase-9 activation, all of which can induce the destruction of the blood-brain barrier and lead to brain oedema (Cahill et al., 2006; Tso and Macdonald, 2014; Pang et al., 2016; Pang et al., 2019). Brain oedema further increases intracranial pressure, forming a vicious circle. Neuroinflammation plays an important role in early brain injury. Following the occurrence of SAH, microglia are activated and release inflammatory factors, which further activate glial cells and aggravate brain injury. Whole-brain hypoperfusion, oxidative stress, and blood-brain barrier destruction also increase neuroinflammatory responses (Pang et al., 2019).
Delayed Brain Injury: Cerebral Vasospasm, Inflammatory Cascade, Epilepsy, Rebleeding, and Hydrocephalus
SAH can result in delayed brain injury, including cerebral ischaemia associated with cerebral vasospasm, seizures, rebleeding, and hydrocephalus (Welty and Horner, 1990; Miller et al., 2014). The pathology of delayed cerebral ischaemia includes angiographic vasospasm, arteriole contraction, microthrombosis, cortical diffusion depolarisation, and self-regulation dysfunction (Macdonald, 2014). These factors cause cerebral vasospasm, which in turn causes delayed cerebral ischaemia (Macdonald, 2014; Veldeman et al., 2020). Inflammation plays a vital role in both early and delayed brain injury. Degradation products of red blood cells, such as haemoglobin, methaemoglobin, oxyhaemoglobin haem, and haem, increase oxidative stress in brain tissues, triggering an inflammatory cascade (Welty and Horner, 1990; Zheng and Wong, 2017). Inflammatory cascades, neuronal excitotoxicity, and blood-brain barrier disruption can lower the seizure threshold and increase susceptibility to epilepsy (Wang, Liang, et al., 2021). Rebleeding after SAH is associated with hypertension. Some studies have observed that larger aneurysms are a greater risk of rebleeding (van Donkelaar et al., 2015). However, few reports have found that the rebleeding rate of small, ruptured aneurysms is not lower than that of large, ruptured aneurysms (Zheng et al., 2019). Hydrocephalus after SAH is associated with inflammation, apoptosis, autophagy, oxidative stress and blood-brain barrier destruction (Chen, Luo, et al., 2017).
In general, cerebrovascular diseases are accompanied by oxidative stress. Oxidative stress is one of the main activators of NLRP3 inflammasome activation. Therefore, the generation of oxidative stress may be the main mechanism of activation of NLRP3 inflammasome in cerebrovascular diseases. Finally, activation of NLRP3 inflammasomes aggravates cerebrovascular diseases through multiple pathways.
The Mechanism Underlying NLRP3 Inflammasome Aggravation of Cerebrovascular Diseases
Following brain injury, a series of pathological changes can activate the NLRP3 inflammasome, and the activation of the NLRP3 inflammasome further aggravates brain injury through an inflammatory response, especially neuroinflammation in association with the NLRP3 inflammasome. Moreover, the NLRP3 inflammasome plays an important role in atherosclerosis and increases the risk of cerebrovascular diseases. Herein, we introduce the pathological mechanism underlying NLRP3 inflammasome-induced aggravation of cerebrovascular diseases, improving our understanding of the role of the NLRP3 inflammasome in cerebrovascular diseases.
NLRP3 Inflammasome in Neuroinflammation
Neuroinflammation is a complex innate immune inflammatory response of the central nervous system, mediated by cytokines, chemokines, ROS, and secondary messengers. These mediators are produced by central neuroglial cells (astrocytes, microglia, oligodendrocytes, and neuron-glial antigen-2 glia), endothelial cells, and peripheral immune cells (Yang and Zhou, 2019). Microglia and astrocytes are primary immune cells involved in neuroinflammation (DiSabato et al., 2016; Schain and Kreisl, 2017; Yang and Zhou, 2019; Hung et al., 2020). Microglia play a macrophage-like role in the central nervous system and are the centre of neuroinflammation (DiSabato et al., 2016). After the occurrence of a lesion, microglial cells are the first to be activated and migrate to the lesion site to initiate innate immunity, release inflammatory factors and chemokines, promote neuronal apoptosis, and phagocytose dead cells, cell debris, and invading pathogens (Yang and Zhou, 2019). Inflammatory mediators produced by microglia, in turn, promote the proliferation of astrocytes and amplify the inflammatory response by secreting inflammatory mediators, such as cytokines and chemokines (Freeman et al., 2017; Yang and Zhou, 2019; Hung et al., 2020). Neuroinflammation leads to the aggregation of immune cells, oedema, tissue damage, and cell death (DiSabato et al., 2016).
The NLRP3 inflammasome plays a vital role in neuroinflammation by promoting the production of IL-1β by microglia and is involved in neuroinflammation in various diseases (DiSabato et al., 2016; Freeman et al., 2017; Yang and Zhou, 2019), including Parkinson's disease (Rui et al., 2020), Alzheimer's disease (Shen, Guan, et al., 2020), multiple sclerosis (Liu, Li, et al., 2019), stroke (Tong et al., 2015), depression (Zhang et al., 2015), traumatic brain injury (Xu, Yin, et al., 2018), HIV-associated neurocognitive disorder (He et al., 2020) and postoperative cognitive dysfunction (Wei, Yang, et al., 2019). In demyelinating disease, NLRP3 inflammasomes promote microglial accumulation and astrocyte proliferation (Freeman et al., 2017). After brain ischaemia/reperfusion injury, NLRP3 inflammasomes are first activated in microglia (Gong et al., 2018). Activation of P2X7R and opening of the pannexin 1 channel activates the NLRP3 inflammasome in microglial cells. Furthermore, TLRs on glial cells activate NLRP3 inflammasomes by recognising DAMPs and PAMPs (Yang and Zhou, 2019).
Both NLRP3 inflammasome and neuroinflammation are involved in the pathogenesis of cerebrovascular diseases. Following intracerebral haemorrhage, neuroinflammation destroys the blood-brain barrier, increases brain edema, aggravates the mass effect, promotes degeneration and loss of axons, and promotes neuronal apoptosis, while inflammatory mediators released after cell death further aggravate neuroinflammation (Xiao et al., 2020). NLRP3 inflammasomes are required for complementary-induced neuroinflammation after intracerebral haemorrhage; in mice, activation of NLRP3 inflammasomes amplifies the inflammatory response after intracerebral haemorrhage (Xiao et al., 2020).
NLRP3 Inflammasome in Atherosclerosis
Atherosclerosis is a complex chronic inflammatory disease that is influenced by cholesterol deposition at the arterial subendothelium. The balance between pro-inflammatory and inflammation-resolving factors determines the progression of atherosclerosis through immunity. Intrinsic atherosclerosis strokes are strongly associated with a high risk of stroke recurrence (Psychogios et al., 2015). It is important to control the development of atherosclerosis to prevent cerebrovascular diseases.
NLRP3 Inflammasome Is Closely Related to the Development of Atherosclerosis
Cholesterol crystals and oxidised low-density lipoprotein (ox-LDL) act as stimuli, activate the NLRP3 inflammasome and the oxidative stress response and cause an inflammatory response, promoting atherosclerosis lesion development (Freigang et al., 2011; Li et al., 2014; Paramel Varghese et al., 2016; Abdul-Muneer et al., 2017; Liu, Zeng, et al., 2018). In atherosclerotic plaques, mRNA expression levels of P2X7R, NLRP3 inflammasome, ASC, caspase-1, IL-1β, and IL-18 are significantly increased when compared with those in normal arteries (Xiao et al., 2013; Peng et al., 2015; Paramel Varghese et al., 2016). Numerous studies have shown that enlarged atherosclerotic lesions are accompanied by the activation of the NLRP3 inflammasome (Yamaguchi et al., 2015; Tumurkhuu et al., 2016; Couchie et al., 2017; Tumurkhuu et al., 2018; Wu et al., 2018), and suppression of the NLRP3 inflammasome and ROS attenuates atherosclerotic plaques (Leng et al., 2016). In Nlrp-/- mice, atherosclerosis stimuli such as cholesterol crystals and ATP were unable to induce IL-1β release; accordingly, atherosclerotic plaques were alleviated (Abderrazak et al., 2015; Deng et al., 2015; Bode et al., 2016; He, Wang, et al., 2016; Leng et al., 2016; Zhou et al., 2016; Fuster et al., 2017; Ma et al., 2018; Zhang, Han, et al., 2018; Zhang, Liu, et al., 2018). These results indicate that the NLRP3 inflammasome-mediated inflammatory response accelerates the formation and development of atherosclerosis. Herein, we explore the role of the NLRP3 inflammasome in atherosclerosis.
NLRP3 Inflammasome Increases the Susceptibility of Macrophages to Lipid Deposition and Promotes Macrophage Recruitment and Transfer Into Foam Cells
Macrophage recruitment and transfer into foam cells is the key process involved in the development of atherosclerosis, and high-density lipoproteins (HDL) play a protective role in atherosclerosis by suppressing inflammatory monocyte cell recruitment and IL-1β secretion (Thacker et al., 2016). CD68-positive macrophages are reportedly located in atherosclerotic lesions with NLRP3 inflammasome expression (Paramel Varghese et al., 2016). NLRP3 inflammasome activation accelerates neutrophil and macrophage recruitment and neutrophil extracellular trap formation, increases the susceptibility of macrophages to lipid deposition, and promotes foam cell formation (Figure 2), while Nlrp3-/- reduces the atherosclerotic lesion size, prevents plaque progression and reduces macrophage infiltration (Li et al., 2014; Zheng et al., 2014; Leng et al., 2016; Tumurkhuu et al., 2016; Wang et al., 2017; Wang, Wu, et al., 2018; Westerterp et al., 2018; Yan et al., 2018). Furthermore, inhibition of the NLRP3 inflammasome plays an anti-inflammatory role by promoting M1 macrophage transfer into the M2 phenotype (Abderrazak et al., 2015). The downstream factor, IL-1β, of the NLRP3 inflammasome promotes foam cell formation. Ox-LDL upregulates the expression of pro-IL-1β and ROS induced by phagocytosis of ox-LDL through the cathepsin B pathway to activate the NLRP3 inflammasome, induce macrophages to secrete IL-1β, and promote macrophage transfer into foam cells during atherosclerosis (Figure 2) (Jiang et al., 2012; Ding et al., 2014). IL-1β inhibits cholesterol efflux through negative feedback, resulting in the accumulation of intracellular cholesterol and foam cell formation (Tumurkhuu et al., 2018).
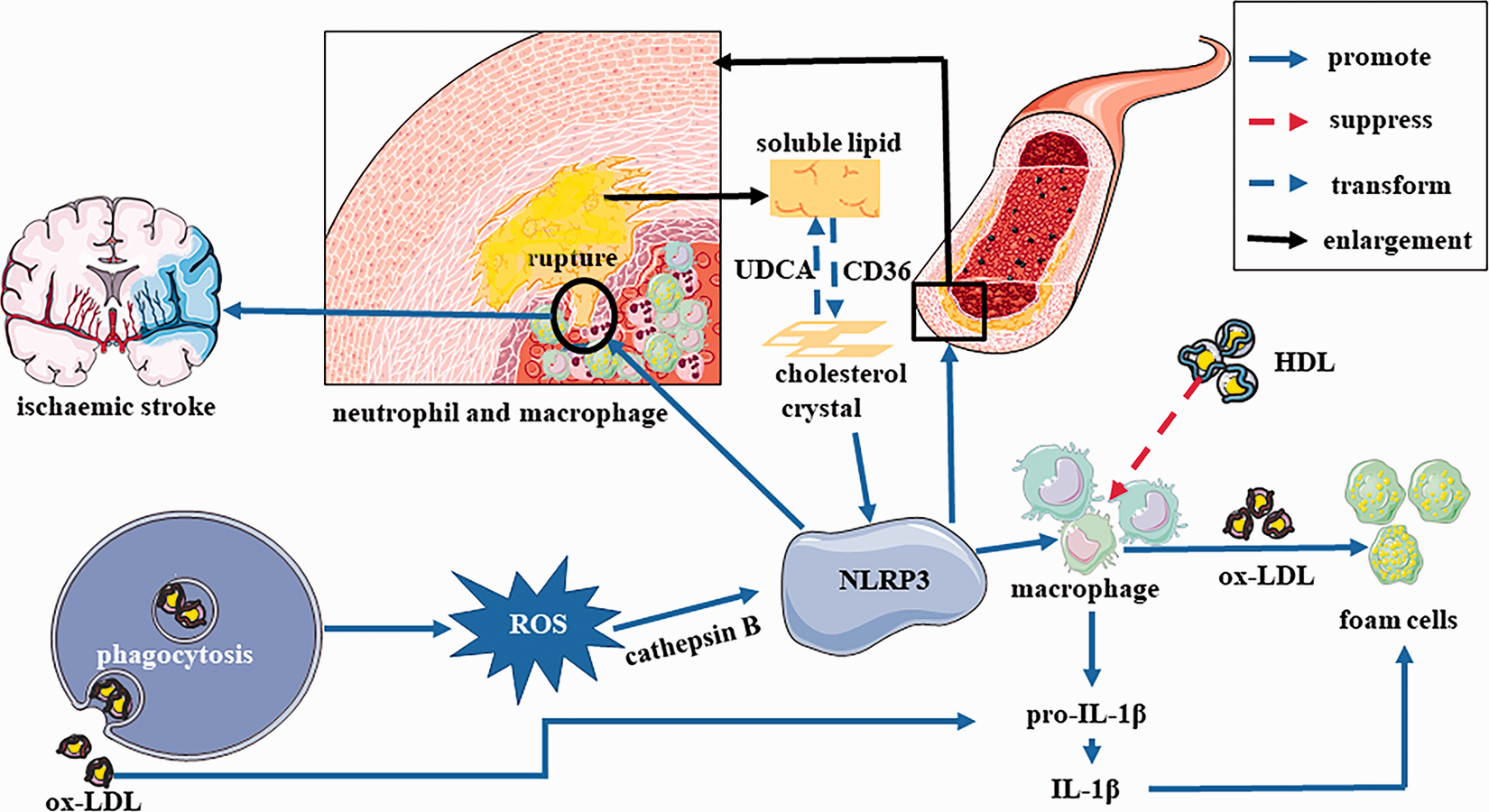
Main Mechanism of NLRP3 Inflammasome in Development of Atherosclerosis. The phagocytosis of ox-LDL generates ROS through the cathepsin B pathway to activate the NLRP3 inflammasome. Activation of the NLRP3 inflammasome accelerates neutrophil and macrophage recruitment, increases the susceptibility of macrophages to lipid deposition, promotes foam cell formation, induces macrophages secreting IL-1β, and impairs plaque stability. Rupture of atherosclerotic plaques can cause stroke. Ox-LDL also upregulates the expression of the pro-IL-1β. IL-1β inhibits cholesterol efflux through a negative feedback, results in accumulation of intracellular cholesterol and foam cell formation. CD36 converts intracellular soluble ligands into crystals or fibrils, while UDCA increases cholesterol solubility, decreases cholesterol crystals-depositions, and inhibits NLRP3 inflammasome dependent inflammation. HDL play a protective role in atherosclerosis by suppressing monocyte cell recruitment and IL-1β secretion. Abbreviations: ox-LDL: oxidized low-density lipoprotein, ROS: reactive oxygen species, UDCA: ursodeoxycholic acid, HDL: high-density lipoproteins.
NLRP3 Inflammasome Influences Cholesterol Solubility and Disrupts Atherosclerotic Plaque Stability
In atherosclerotic mice, cholesterol crystals that accumulate in atherosclerotic plaques activate the NLRP3 inflammasome in phagocytes. Thus, decreasing cholesterol crystal deposition in atherosclerotic plaques by employing ursodeoxycholic acid (UDCA) could increase cholesterol solubility in macrophages, impair NLRP3 inflammasome-dependent inflammation, and diminish atherosclerotic plaque development (Figure 2) (Bode et al., 2016). In atherosclerosis, an increase in the pattern recognition receptors CD36 is accompanied by NLRP3 inflammasome activation (Du et al., 2018). Studies have reported that CD36 converts intracellular soluble ligands into crystals or fibrils (Duewell et al., 2010; Sheedy et al., 2013), and targeting CD36 downregulated serum IL-1β concentrations and suppressed cholesterol crystal accumulation in plaques (Sheedy et al., 2013). NLRP3 inflammasome activation also disrupts plaque stability, whereas atherosclerotic plaque rupture leads to stroke (Hutcheson et al., 2014). Studies have observed that inhibition of the NLRP3 inflammasome enhances atherosclerotic plaque stability, reduces plaque volume and maximal stenosis, as well as the average plaque size of atherosclerotic lesions, preventing plaque progression (Zheng et al., 2014; Leng et al., 2016; van der Heijden et al., 2017; Ma et al., 2018). It can be seen that the improvement of atherosclerosis induced by inhibition of NLRP3 inflammasome is also beneficial for cerebrovascular diseases.
NLRP3 Inflammasome in Ischaemic Stroke
Notably, activation of the NLRP3 inflammasome after cerebral ischaemia aggravates brain injury. The NLRP3 inflammasome, caspase-1, IL-1β and IL-18 levels increase in cerebral ischaemia/reperfusion animal models and patients with stroke (Fann et al., 2013; Zhang et al., 2014; He et al., 2017). A previous study found that the NLRP3 inflammasome was increased in the hippocampus, striatum, and thalamus of the neonatal hypoxia-ischaemic brain (Ystgaard et al., 2015), and the upstream factory of the NLRP3 inflammasome, P2X7R, was markedly upregulated in the hippocampus (Thakkar et al., 2016). A genetic investigation revealed that the NLRP3 rs4612666 gene polymorphism enhanced the susceptibility of large artery atherosclerosis ischaemic stroke by altering plaque vulnerability and was involved in large artery atherosclerosis ischaemic stroke and microembolic signal occurrence (Cheng et al., 2018). NLRP3-Q705K minor allele carriage is associated with an increased risk of stroke/transient ischaemic attack (Kastbom et al., 2015). Inhibition of NLRP3 inflammasome and IL-1β improves neurological deficits, alleviates brain tissue damage (Ito et al., 2015; Wang, Wang, et al., 2015; Lammerding et al., 2016; Thakkar et al., 2016; Hong et al., 2018; Ismael et al., 2018; Teng et al., 2018; Qu et al., 2019; Mo et al., 2020; Zhang, Zhao, et al., 2020), decreases infarct volume, and alleviates the brain oedema post-ischaemic stroke (Yang et al., 2014; Zhang et al., 2014; Wang, Li, et al., 2015; Lu et al., 2016; Qiu et al., 2016; He et al., 2017; Chen, Xu, et al., 2018; Ismael et al., 2018; Ma et al., 2019).
NLRP3 Inflammasome Is Associated with Increased Proinflammatory Cytokines and Inflammatory Infiltration
Ischaemia/reperfusion or oxygen-glucose deprivation/reoxygenation can induce the first-step signal of NLRP3 activation, resulting in increased proinflammatory cytokines and NLRP3 expression in injured tissues (Ito et al., 2015; Wang, Wang, et al., 2015; Chen, Dixon, et al., 2018; Lemarchand et al., 2019; Zhang, Zhao, et al., 2020). Reportedly, the NLRP3 inflammasome was first activated in microglia cells after brain ischaemia/reperfusion injury and then expressed in neurons and microvascular endothelial cells, but mainly in neurons (Gong et al., 2018). The NLRP3 inflammasome not only releases inflammatory cytokines such as IL-1β and IL-18, but also promotes microglial activation, infiltration of neutrophils, and the aggravates neurotoxicity of microglia in ischaemia/reperfusion (Figure 3) (Wang, Li, et al., 2015; Zhao et al., 2015; Li, Wang, et al., 2016; Lu et al., 2016; Qiu et al., 2016; Yu et al., 2017; Chen, Xu, et al., 2018; Liu, Cen, et al., 2018; Ma et al., 2019; Sha et al., 2019; She et al., 2019; Tang et al., 2019; Wang et al., 2019). A recent discovery has confirmed that Smad6 is a target for NLRP3 to interact with microglia cells in neonatal rat hypoxic-ischaemic encephalopathy model (Chen, Hu, et al., 2020). Chen et al. (2020)'s findings suggest that Smad6 may be a target for the treatment of nervous system diseases by intervening NLRP3 inflammasome (Chen, Hu, et al., 2020).
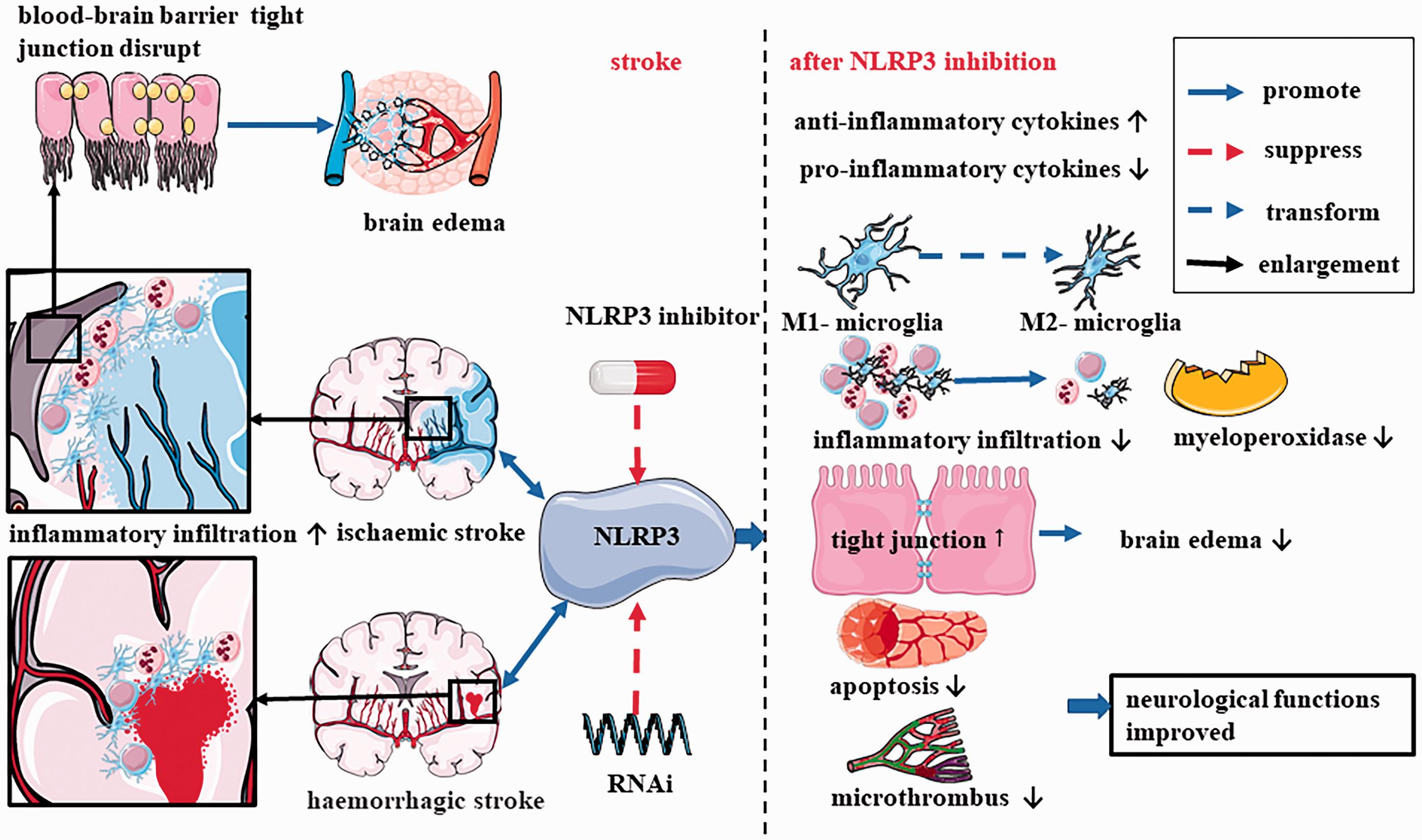
The Mechanism Underlying NLRP3 Inflammasome Aggravation of Cerebrovascular Diseases. NLRP3 inflammasomes are activated after brain injury. Activation of NLRP3 inflammasome aggravates brain edema by increasing inflammatory cell infiltration, destroying tight junction proteins, and enhancing permeability of brain microvessel endothelial cell. Inhibition of NLRP3 inflammasome with inhibitors or RNAi reduces proinflammatory cytokines levels, promotes the transformation of M1-type microglia cells to M2-type, inhibits the aggregation and activation of inflammatory cells, and reduces myeloperoxidase level. M2-type microglia have anti-inflammatory effects, and the level of anti-inflammatory cytokines is up-regulated after phenotypic transformation of microglia. Inhibition of NLRP3 inflammasome also increases tight junction proteins expression, reduces cerebral edema and blood-brain barrier permeability, reduces neuronal degeneration and apoptosis, and reduces microthrombosis. All of these lead to improvement of neurological functions.
NLRP3 Inflammasome Is Associated With Increased Blood–Brain Barrier Permeability and Brain Oedema
The blood-brain barrier is formed by specialised brain endothelial cells interconnected by tight junctions. Tight junctions in the blood-brain barrier are essential for maintaining the microenvironment (Sozen et al., 2009). Brain oedema mediated by the NLRP3 inflammasome is associated with increased blood-brain barrier permeability. Studies have shown that the NLRP3 inflammasome enhances the permeability of brain microvessel endothelial cells via IL-1β (Yang et al., 2014) and downregulates the expression of tight junction proteins, occludin and zona occludens-1, after ischaemia/reperfusion injury (Figure 4) (Cao et al., 2016; Qu et al., 2019). Occludin degradation renders the blood-brain barrier more vulnerable to reperfusion injury in vitro (Zhang, Li, et al., 2020). A recent study observed that the NLRP3 inflammasome influences the distribution of aquaporin-4 in the infarct area (Wang, Chen, et al., 2020). Similarly, diabetes reportedly stimulates NLRP3 inflammasome activation, disrupts the polarity of aquaporin-4 and increases the blood-brain barrier permeability after ischaemia (Ward et al., 2019). Moreover, NLRP3 inflammasome-mediated pyroptosis is related to brain oedema following ischaemia/reperfusion (An et al., 2019). The mechanisms underlying the association between pyroptosis and brain oedema warrant further study. In ischaemic tissues, recruited neutrophils can contribute to dramatic blood-brain barrier disruption and tissue damage, ultimately resulting in haemorrhagic transformation (Guo et al., 2018). NLRP3 inflammasome may disrupt the blood-brain barrier and promote brain oedema through various factors. Inhibition of NLRP3 inflammasome is expected to reduce the degradation of tight junction protein in blood-brain barrier and the permeability of blood-brain barrier, thus having a protective effect on cerebrovascular diseases.
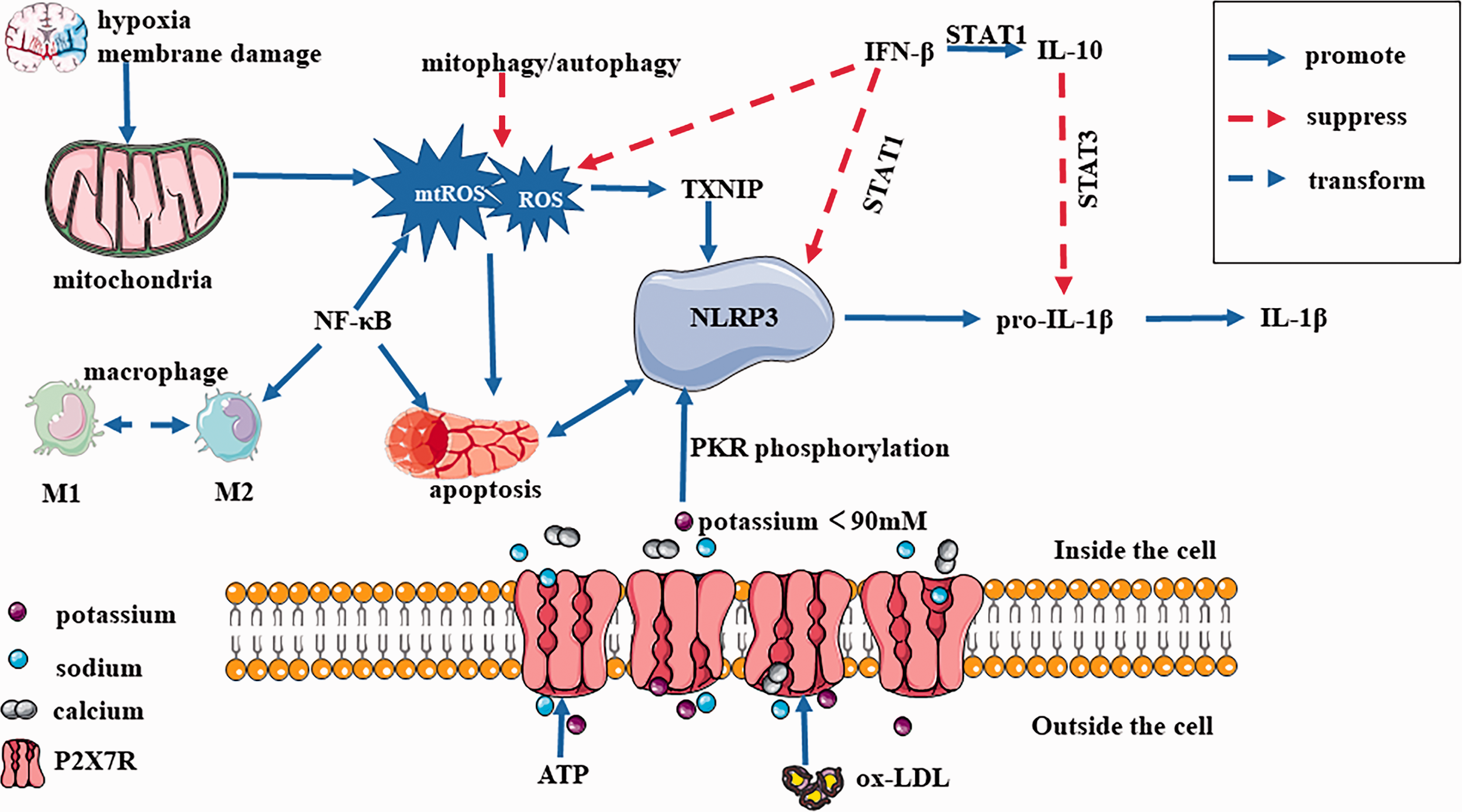
Signalling Pathways of NLRP3 Inflammasome Activation in Cerebrovascular Diseases. Hypoxia and membrane damage induce mtROS production. ROS leads to NLRP3 inflammasome activation and IL-1β secretion through inducing the binding of TXNIP to NLRP3. ROS also activates NLRP3 inflammasome via NF-κB and apoptosis. The mitophagy/autophagy system removes mtROS and suppresses NLRP3 inflammasome activation. NF-κB regulates both pyroptosis and oxidative stress, it also influences macrophage differentiation into M1 or M2 cells. IFN-β inhibits NLRP3 in three pathways: (A) represses the activity of the NLRP3 inflammasome via the signal transducer and activator of transcription (STAT)1 transcription factor; (B) induces IL-10 in a STAT1-dependent manner, while IL-10 reduces pro-IL-1β production via STAT3 signalling; (C) suppresses ROS generation in antigen presenting cells. The opening of P2X7R allows potassium ions to efflux from cells and sodium and calcium ions to influx into cells. The NLRP3 inflammasome is activated when the intracellular potassium ion level is below the threshold of 90 Mm. ATP leads to neuroinflammation through activating the P2X7R/cryopyrin inflammasome axis. Ox-LDL upregulates the expression levels of P2X7R, NLRP3 inflammasome and IL-1β via phosphorylation of protein kinase R. Abbreviations: mtROS: mitochondrial ROS, ROS: reactive oxygen species, TXNIP: thioredoxin-interacting protein, IFN-β: interferon-β, STAT: signal transducer and activator of transcription, P2X7R: purinergic receptor-7.
NLRP3 Inflammasome in Intracranial Haemorrhage
Haemorrhagic stroke is a devastating disorder with high morbidity and mortality rates. Recent studies have shown that intracranial haemorrhage activates and exacerbates inflammatory progression (Cheng et al., 2017). The NLRP3 inflammasome plays a key role in secondary brain injury following intracranial haemorrhage (Yang, Sun, et al., 2018). Yuan et al. (2017) found that NLRP3 expression and the levels of ROS, lipid peroxides, and NF-κB-p65 were increased in an animal model of intracranial haemorrhage (Yuan et al., 2017). NLRP3 RNAi, encoded by a recombinant adenovirus, relieved inflammation and brain injury after intracranial haemorrhage (Yuan et al., 2015). Moreover, inflammasomes play a vital role in hypertension, which is a risk factor for intracranial haemorrhage. Blockade of NF-κB inhibited hypertension by suppressing NLRP3 inflammasome activation, pro-inflammatory cytokine production, and oxidative stress reactions (Liu, Zeng, et al., 2018). Inhibition of the NLRP3 inflammasome ameliorated neurological dysfunction, relieved brain oedema, and decreased the haemorrhagic volume (Cheng et al., 2017). Activation of NLRP3 inflammasome plays a devastating role in intracerebral haemorrhage, and it is involved in the pathology of intracerebral haemorrhage through the following aspects.
NLRP3 Inflammasome Regulates Immune Cells and Cytokines
Microglial activation is critical for intracranial haemorrhage-induced secondary brain injury (Li, Wang, et al., 2018). Activated microglia release cytokines in response to haemorrhagic stroke and ultimately lead to neuroinflammation and brain injury. Disturbing the co-localisation of the NLRP3 inflammasome with microglial cells improved neurological functions (Yang, Sun, et al., 2018), and NLRP3 inflammasome expression increased in microglia in a time-dependent manner; NLRP3 inflammasome increases gradually and peaks at day 5 after intracranial haemorrhage (Yao et al., 2017; Miao et al., 2020). Suppression of the NLRP3 inflammasome is followed by inhibition of microglial accumulation and activation, as well as amelioration of neurological dysfunction post intracranial hemorrhage (Figure 3) (Zhao, Pan, et al., 2017; Li, Wang, et al., 2018; Wang, Nowrangi, et al., 2018). Furthermore, selective inhibition of caspase-1 could promote the polarisation of M1-type microglia into M2-type around the haematoma and ameliorate neurological dysfunction of limb movement (Figure 3) (Lin et al., 2018). The role of NLRP3 inflammasome in intracerebral haemorrhage is not only related to microglia, but also related to the release of inflammatory factors.
P2X7R plays a damaging role in intracranial haemorrhage through NLRP3 inflammasome-dependent neutrophil infiltration and IL-1β and IL-18 release (Feng et al., 2015). Reportedly, the suppression of the NLRP3 inflammasome downregulates levels of myeloperoxidase, a heme-containing peroxidase expressed primarily in neutrophils and monocytes, and inhibits recruitment and infiltration of leucocytes and neutrophils (Ma et al., 2014; Guo et al., 2018; Wang, Nowrangi, et al., 2018). Furthermore, inhibition of NLRP3 inflammasome attenuates neurological deficits, downregulates cytokine levels, including IL-1β, IL-6, TNF-α and lactate-dehydrogenase (Yang et al., 2015; Cheng et al., 2017; Zeng et al., 2017; Li, Wang, et al., 2018; Lin et al., 2018; Ren et al., 2018; Xu, Shen, et al., 2019). The proinflammatory effect of NLRP3 inflammasome may be related to neuroinflammation in intracerebral haemorrhage. Inhibition of NLRP3 inflammasome is beneficial to reduce neuroinflammation and the subsequent pathological changes caused by neuroinflammation.
NLRP3 Inflammasome Is Involved in Blood–Brain Barrier Disruption
NLRP3 inflammasome expression is accompanied by blood-brain barrier component destruction in delayed recombinant tissue-type plasminogen activator-induced haemorrhagic transformation, while NLRP3 shRNA decreases haemorrhage score and haemorrhage volume during haemorrhagic transformation (Guo et al., 2018). Neutrophil recruitment may be the mechanism underlying of NLRP3 knockdown-attenuated haemorrhagic transformation and motor deficits (Ma et al., 2014). IL-1β injected into the brain parenchyma increased the blood-brain barrier permeability. The IL-1β-induced increase in blood-brain barrier permeability was neutrophil-dependent (Blamire et al., 2000). In intracranial haemorrhage, accumulating evidence shares a similar conclusion that inhibition of the NLRP3 inflammasome maintains the blood-brain barrier integrity, attenuates brain oedema and alleviates neurobehavioral disorders in intracranial haemorrhage (Ma et al., 2014; Feng et al., 2015; Cheng et al., 2017; Yao et al., 2017; Zeng et al., 2017; Li, Wang, et al., 2018; Ren et al., 2018; Yang, Sun, et al., 2018; Xu, Shen, et al., 2019; Miao et al., 2020). Yang et al. (2015) reported that miR-223 inhibited NLRP3 expression, consequently relieving brain oedema via 3′ UTR sites on NLRP3 mRNA in intracranial hemorrhage (Yang et al., 2015). The destruction of the blood-brain barrier by NLRP3 inflammasome in intracerebral haemorrhage may be related to inflammatory infiltration. Inhibition of NLRP3 inflammasome is helpful to reduce cerebral edema after intracerebral haemorrhage.
NLRP3 Inflammasome Is Associated With Neuronal Degeneration and Apoptosis
Intracranial haemorrhage is associated with the activation of different cell death pathways. These cell death pathways lead to the removal of inactivated and damaged cells, resulting in neuronal cell damage (Lin et al., 2018). A previous study observed that inhibition of NLRP3 inflammasome assembly reduces neuronal cell degeneration and ameliorates histological damage (Cheng et al., 2017; Zeng et al., 2017; Li, Wang, et al., 2018), as well as decreases apoptosis in intracranial haemorrhage (Figure 3) (Lin et al., 2018; Xu, Shen, et al., 2019).
NLRP3 Inflammasome in SAH
SAH is an emergent neurological disease known to present a poor prognosis and markedly high morbidity and mortality. Early brain injury, brain injury that occurs within 72 hours of SAH, has been reported to play a vital role in the prognosis of SAH (Zhou et al., 2018). The NLRP3 inflammasome acts as an important mediator of the inflammatory response in SAH-induced early brain injury. SAH-induced oxidative stress activates NF-κB, consequently promoting the translocation of the p65 subunit into the nucleus and increasing its downstream proinflammatory cytokines (IL-1β, IL-6, TNF-α) and NLRP3 mRNA levels (Shao et al., 2016; Li et al., 2017; Zhou et al., 2017), exacerbating neurological deficits of SAH (Chen et al., 2013). Inhibition of the NLRP3 inflammasome alleviates neurological deficits and improves neurobehavioral outcomes after SAH (Shao et al., 2016; Liu et al., 2017; Zhou et al., 2017; Zhou et al., 2018). Understanding the role of NLRP3 inflammasome in SAH is of great significance for prevention and treatment of SAH.
NLRP3 Inflammasome Is Involved in Inflammatory Infiltrates, Autophagy, and Apoptosis
In SAH, inhibition of the NLRP3 inflammasome upregulates the rate of survival and surviving neurons (Dong et al., 2016; Cao et al., 2017). Suppression of NLRP3 reportedly decreases neutrophil infiltration, microglial activation, and production of proinflammatory factors (Figure 3) (Yin et al., 2018). The NLRP3 inflammasome may also be associated with autophagy and apoptosis. Li et al. (2017) reported that NLRP3 inhibition increased autophagy marker beclin-1 expression (Li et al., 2017), and caspase-1 inhibition reduced neural necrotic cell death in SAH (Li et al., 2017). In another study, Li et al. (2016) observed that minocycline inhibited NLRP3 inflammasome activation and repressed neural apoptosis induced by P53-associated apoptotic proteins in early brain injury following SAH (Li, Chen, et al., 2016).
Blocking of NLRP3 Inflammasome Improves the Blood–Brain Barrier Permeability and Relieves Brain Oedema
NLRP3 inflammasomes are associated with disruption of the blood-brain barrier in SAH. ATP activates the NLRP3 inflammasome through the P2X7R/NLRP3 inflammasome axis, exacerbating neurological deficits and brain oedema following SAH (Chen et al., 2013). Inhibition of the NLRP3 inflammasome improved the blood-brain barrier permeability, reduced the brain water content, and exerted neuroprotective effects after SAH (Figure 3) (Li, Chen, et al., 2016; Li et al., 2017; Liu et al., 2017; Zhou et al., 2017). Additional studies have observed that NLRP3 inflammasome inhibition is accompanied by increased tight junction protein expression (Dong et al., 2016; Yin et al., 2018). The effect of NLRP3 on the blood-brain barrier may be attributed to the regulation of IL-1β-induced matrix metalloproteinase-9 expression, which opens the blood-brain barrier by degrading tight junction proteins (Sozen et al., 2009).
Inhibition of NLRP3 Inflammasome Reduces Microthrombosis
A previous study reported that SAH induced microcirculatory dysfunction and microthrombosis in vivo (Friedrich et al., 2012). Microcirculatory dysfunction contributes to delayed cerebral ischaemia following SAH, and the number of microthrombi correlates with the number of apoptotic neuronal cells and prognosis of SAH (Sabri et al., 2012). Zuo et al. (2020) found that inhibition of the NLRP3 inflammasome reduced microthrombosis and improved neurobehavior following SAH (Figure 3) (Zuo et al., 2020). Currently, research on the NLRP3 inflammasome and microthrombosis remains scarce, and the study of microthrombosis is of great significance to improve the prognosis of SAH.
It appears that the NLRP3 inflammasome plays a crucial role in cerebrovascular diseases and atherosclerosis, and inhibition of NLRP3 inflammasome activation may have therapeutic significance in cerebrovascular diseases. Understanding the activation pathway of the NLRP3 inflammasome in cerebrovascular diseases can help assess suitable NLRP3 inflammasome inhibitors.
Signalling Pathways of Nlrp3 Inflammasome Activation in Cerebrovascular Diseases
Following brain injury, NLRP3 inflammasome activation reportedly underlies the aggravation of cerebrovascular disease pathology mediated via the NLRP3 inflammasome. Multiple signalling pathways are involved in the activation of NLRP3 inflammasomes after brain injury, and we will discuss these pathways from the perspective of two-step activation of NLRP3 inflammasome.
The Signal Pathway That Aggravates Cerebrovascular Diseases
ROS/NF-κB/NLRP3 Inflammasome Pathway-Signalling Pathway Involved in the Priming
NF-κB is a heterodimeric protein involved in inflammatory responses (Sabir et al., 2017). Activation of NF-κB in brain injury plays an important role in the priming of the NLRP3 inflammasome, increasing the mRNA level of NLRP3 and creating conditions for NLRP3 inflammasome activation. Suppression of the NF-κB/NLRP3 inflammasome pathway plays a protective role in both haemorrhagic and ischaemic stroke (Li, Wang, et al., 2016; Shao et al., 2016; Zeng et al., 2017; Chen, Xu, et al., 2018; Fann et al., 2018; Li, Wang, et al., 2018; Liu, Cen, et al., 2018; Yin et al., 2018; Tang et al., 2019; Miao et al., 2020).
ROS induced by SAH and intracranial hemorrhage activates NF-κB, thus translocating the p65 subunit into the nucleus and increasing the mRNA levels of NLRP3 and proinflammatory cytokines (Figure 4) (Shao et al., 2016). Activation of the ROS/NF-κB/NLRP3 inflammasome led to early brain injury after SAH and intracranial hemorrhage (Shao et al., 2016), while inhibition of the ROS/NF-κB/NLRP3 inflammasome pathway improved neurological deficits following ischaemia/reperfusion injury (Zhang, Zhao, et al., 2020). Zeng et al. (2017) reported that nuclear factor E2-related factor-2 (Nrf2) is upstream of the ROS/NF-κB/NLRP3 inflammasome pathway or ROS/NLRP3 inflammasome pathway in intracranial haemorrhage (Zeng et al., 2017). Xu et al. (2018) observed that Nrf2 activation decreased ROS, inhibiting NLRP3 inflammasome activation in oxygen-glucose deprivation/reoxygenation-induced BV2 cells (Xu, Zhang, et al., 2018). However, the mechanism associating Nrf2 with the ROS/NF-κB/NLRP3 inflammasome pathway in cerebrovascular diseases remains to be elucidated. A previous report has observed Nrf2 activation attenuated oxidative stress and neuronal inflammation via the nicotinamide adenine dinucleotide phosphate oxidase 4/ROS/NF-κB pathway (Saha et al., 2020). Nrf2 negatively regulates the NF-κB signalling pathway via the following mechanisms: a) Nrf2 decreases intracellular ROS levels by upregulating antioxidant genes and mitophagy-activating genes, resulting in the inhibition of NF-κB activation (Liu, Zeng, et al., 2020). b) Nrf2 prevents IκB-α proteasomal degradation by increasing heme oxygenase-1 levels and inhibiting the nuclear translocation of NF-κB. c) Nrf2 inhibits NF-κB by competing with the transcription co-activator cyclic adenosine monophosphate response element-binding protein (Saha et al., 2020). Further studies need to assess whether the regulation of Nrf2 on NF-κB in cerebrovascular diseases is identical to the above-listed mechanisms.
Signalling Pathway Involved in the Activation
ROS/TXNIP/NLRP3 Inflammasome Pathway
ROS not only affects the priming of the NLRP3 inflammasome through NF-κB but also affects the activation of the NLRP3 inflammasome. Recognition of ROS by TLR is vital for inflammasome activation (Fernandes-Alnemri et al., 2013). In cerebral ischaemia, ROS production and oxidative stress mediate proinflammatory effects via the NLRP3 inflammasome (Ma et al., 2014; Zhao et al., 2019). Inhibition of the ROS/NLRP3 inflammasome pathway plays a protective role in atherosclerosis, ischaemic stroke and SAH (Sun et al., 2015; Wang, Li, et al., 2015; Leng et al., 2016; Li, Chen, et al., 2016; Liu et al., 2017; Peng et al., 2017; Wang et al., 2017; Zhou et al., 2017; Yao et al., 2019). Hypoxia and membrane damage induce mitochondrial ROS (mtROS) production, which leads to unprompted NLRP3 activation (Jiang et al., 2018). Both Zhang et al. (2020) and Gong et al. (2018) demonstrated that mitochondrial dysfunction activates the NLRP3 inflammasome in microglia after oxygen-glucose deprivation/reoxygenation (Gong et al., 2018; Zhang, Zhao, et al., 2020). The role of ROS and NLRP3 inflammasomes in cerebrovascular diseases may be related to thioredoxin-interacting protein (TXNIP), a widely expressed protein that interacts with thioredoxin. Nrf2, the upstream signalling molecule of ROS, inhibits the NLRP3 inflammasome by regulating the thioredoxin/TXNIP complex and has protective effects on oxygen-glucose deprivation/reoxygenation and ischaemia/reperfusion injury (Li, Chen, et al., 2016; Liu et al., 2017; Hou, Wang, et al., 2018). A study found that increased expression of TXNIP activated the NLRP3 inflammasome and exacerbated brain damage after neonatal hypoxic ischaemia (Figure 4) (Chen, Dixon, et al., 2018). Inhibition of the TXNIP/NLRP3 inflammasome pathway reportedly alleviates brain injury (Wang, Li, et al., 2015). However, the precise functional relationship between TXNIP and ROS in cerebrovascular diseases has not been investigated. There are two pathways of interaction between TXNIP and ROS based on hyperglycaemic diseases. a) TXNIP combines with thioredoxin in the absence of stimulus, ROS dissociates TXNIP from thioredoxin and induces the binding of TXNIP to NLRP3 via the LRR domain (Han et al., 2018). The direct protein-protein interaction between TXNIP and NLRP3 inflammasome leads to the release of IL-18 and IL-1β. b) The combination of TXNIP with the NLRP3 inflammasome triggers ROS production and accumulation (Amin et al., 2020). The ROS/TXNIP/NLRP3 inflammasome is widely observed in several diseases and plays a proinflammatory role, especially in vascular complications caused by high glucose (Amin et al., 2020), including diabetic retinopathy (Lu et al., 2018; Du, Wang, Tu, et al., 2020), diabetic nephropathy (Han et al., 2018; Du, Wang, Chen, et al., 2020), myocardial ischaemia/reperfusion injury (Wang, Yan, et al., 2020) and nonalcoholic steatohepatitis (Bai et al., 2019), as well as in conditions not associated with high glucose levels, such as the mouse model of osteoarthritis (Gu et al., 2019) and endothelial senescence-related cardiovascular diseases (Yin et al., 2017). As diabetes is a risk factor for stroke, it is reasonable to speculate that the ROS/TXNIP/NLRP3 inflammasome pathway confirmed in high glucose diseases remains a concern in cerebrovascular diseases. Future studies could validate this pathway in patients with cerebrovascular diseases.
P2X7R/NLRP3 Inflammasome Pathway
P2X7R is a ligand-gated cation channel. The opening of P2X7R allows potassium ions to efflux from cells and sodium and calcium ions to influx into cells (Di Virgilio et al., 2017; Hou, Dong, et al., 2018). Potassium ion efflux and calcium ion influx are common pathways leading to NLRP3 inflammasome activation, especially potassium ion efflux from cells (Di Virgilio et al., 2017). The NLRP3 inflammasome is activated when the intracellular potassium ion level is below the threshold of 90 mM (Figure 4) (Schorn et al., 2011; Wang, Hou, et al., 2018; Ribeiro et al., 2019). The effect of P2X7R on the NLRP3 inflammasome is related to potassium ions, as well as protein kinase R phosphorylation. Ox-LDL upregulates the expression levels of P2X7R, NLRP3 inflammasome and IL-1β via phosphorylation of protein kinase R (Peng et al., 2015). P2X7R-/- suppresses NLRP3 inflammasome activation by inhibiting protein kinase R phosphorylation (Peng et al., 2015). In SAH, the activation of P2X7R by ATP aggravated neuroinflammation through the cryopyrin inflammasome (Chen et al., 2013). Altered ion channel status and protein kinase R phosphorylation may afford a protective effect on cerebrovascular diseases by inhibiting the P2X7R/NLRP3 inflammasome.
In summary, current studies have shown that activation of ROS/NF-κB/NLRP3 inflammasome signalling pathway, ROS/TXNIP/NLRP3 inflammasome signalling pathway and P2X7R/NLRP3 inflammasome signalling pathway are associated with exacerbation of cerebrovascular diseases. ROS/NF-κB was associated with the first step of NLRP3 inflammasome activation, and ROS/TXNIP and P2X7R were associated with the second step of NLRP3 inflammasome activation. Nrf2 is an upstream molecule of ROS, which can simultaneously participate in the first step and the second step activation of NLRP3 inflammasome. However, there are few studies on the molecular mechanisms of the signalling pathways in cerebrovascular diseases. In cerebrovascular diseases, the mechanism of NF-κB promoting NLRP3 mRNA expression has been proposed. The mechanisms by which Nrf2 interacts with ROS/TXNIP were demonstrated in oxygen-glucose deprivation/reoxygenation and ischaemia/reperfusion injury. At present, the molecular interaction mechanisms between Nrf2 and ROS/NF-κB have been proposed, but whether those mechanisms are applicable to cerebrovascular diseases need further study. Similarly, whether the interaction mechanisms between TXNIP and ROS proposed in hyperglycaemic diseases are applicable to cerebrovascular diseases require further exploration. Exploring the mechanisms of the signalling pathway can help develop inhibitors that target the molecules in the signalling pathway.
Cerebrovascular Disease Aggravation after NLRP3 Inflammasome Activation
Pyroptosis
Pyroptosis is a mode of programmed cell death and is characterised by the formation of plasma membrane pores mediated by caspase-1 and inflammatory cytokines release (She et al., 2019). Inhibition of pyroptosis induced by the NLRP3 inflammasome exerts neuroprotective effects after cerebral ischaemia/reperfusion injury (An et al., 2019; Zhu, Zhang, et al., 2019). NLRP3 inflammasome-mediated epithelial pyrotosis accelerates the development of atherosclerotic plaques and increases plaque size (Wu et al., 2018; Zhang, Liu, et al., 2018). In certain diseases, the NLRP3 inflammasome mediated pyroptosis is associated with TLR4-mediated myeloid differentiation primary response protein 88/NF-κB including hepatic ischaemia/reperfusion injury (El-Sisi et al., 2020) and necrotising enterocolitis (Chen, Zhang, et al., 2020). TLR4-mediated myeloid differentiation primary response protein 88/NF-κB/NLRP3 inflammasome-induced pyroptosis is associated with the formation of gasdermin-D, a substrate of caspase-1 (Chen, Zhang, et al., 2020; Liu, Yao, et al., 2020). Caspase-1 cleaves gasdermin-D into N-terminal and C-terminal fragments. N-terminal of gasdermin-D was sufficient to promote cell lysis and inflammasome activation without the C-terminal of gasdermin-D (Downs et al., 2020). Reportedly, N-terminal of gasdermin-D inserts into the lipid bilayer by interacting with inner membrane glycerophospholipids, including phosphatidylinositol phosphates, phosphatidic acid, and phosphatidylserine; this results in pores of approximately 20 nm that cause the cell to swell and burst, releasing inflammatory cytokines IL-1β and IL-18 (Downs et al., 2020; El-Sharkawy et al., 2020). In models of myocardial infarction, NF-κB-mediated pyroptosis has been associated with oxidative stress (Lei et al., 2018), suggesting that NF-κB pathways are not entirely in parallel with each other. Moreover, the adenosine monophosphate-activated protein kinase (AMPK)/glycogen synthase kinase 3β signalling pathway has been associated with NLRP3 inflammasome-mediated pyroptosis (An et al., 2019).
Apoptosis
Neuronal apoptosis is associated with cognitive impairment in cerebrovascular diseases. Activation of the ROS/NF-κB/NLRP3 inflammasome can induce neuronal apoptosis (Yu, Zhang, et al., 2019; Long et al., 2020). Simultaneously, neuronal apoptosis can activate the NLRP3 inflammasome (He et al., 2017; Teng et al., 2018; Wang et al., 2019; Ward et al., 2019). Inhibition of the NLRP3 inflammasome injury decreases neuronal apoptosis in ischaemia/reperfusion and SAH (Qiu et al., 2016; Liu et al., 2017; Yin et al., 2018; Ma et al., 2019; Qu et al., 2019; She et al., 2019; Mo et al., 2020). Other studies have reported that the anti-apoptotic effects depend on upregulated expression levels of anti-apoptotic protein B-cell lymphoma-2 and downregulated levels of the pro-apoptotic factor, building information modelling (Fann et al., 2013; Dong et al., 2016; Fann et al., 2018).
In short, NLRP3 inflammasomes promote neuronal death by mediating pyroptosis and apoptosis. NLRP3 inflammasomes-mediated pyroptosis is associated with NF-κB, and the molecular mechanisms have been identified. NF-κB not only promotes the expression of NLRP3 mRNA, but also participates in NLRP3 inflammasome-mediated pyroptosis. NLRP3 inflammasome-mediated apoptosis can further activate the NLRP3 inflammasome and amplify damage. It is suggested that the role of NLRP3 inflammasome in cerebrovascular diseases is complex. Inhibition of NLRP3 inflammasomes activation is important for saving neuronal death.
The Signal Pathway That Alleviates Cerebrovascular Diseases
Autophagy/Mitophagy
Autophagy maintains cell homeostasis by engulfing damaged and dysfunctional organelles. Autophagy dysfunction is associated with various diseases, including neurodegenerative diseases and cancer. In cerebrovascular diseases, the autophagy markers, including light chain 3-II/light chain 3-I, beclin-1, and autophagy-related gene 5, and the mitophagy marker Parkin, as well as phosphatase and tensin homolog-induced putative kinase 1 (PINK-1) expression, are negatively correlated with the NLRP3 levels (Cao et al., 2017; He et al., 2017; Li et al., 2017; Wang et al., 2019). Autophagy regulates the NLRP3 inflammasome through the following three mechanisms (Figure 4): Autophagy removes the intracellular activator of the NLRP3 inflammasome, such as mtROS, which is the primary source of mtROS, a major source of ROS (90%) (Figure 4). b) Autophagy removes components of the NLRP3 inflammasome. c) Autophagy removes intracellular pro-IL-1β (Zhou et al., 2011). Mitophagy is defined as autophagy that occurs in the mitochondria and can remove mtROS. Parkin/mitophagy plays a protective role in cerebral ischaemic injury and atherosclerosis by inhibiting the NLRP3 inflammasome (Ma et al., 2018; He et al., 2019). The mechanism underlying the Parkin/mitophagy pathway is relatively well established. PINK-1 protein assists the recruitment of Parkin into the dysfunctional mitochondria, and induces mitochondrial outer membrane protein ubiquitination; p62 recognises ubiquitin mitochondria and binds to light chain 3 to initiate mitophagy (He et al., 2019). However, few studies have assessed the mechanism of PINK-1 activation. Investigating the activation mechanism of PINK-1/Parkin is expected to provide a new method for treating cerebrovascular diseases.
IFN-β/NLRP3 Inflammasome Pathway
IFN-β plays an anti-inflammatory role by inhibiting the NLRP3 inflammasome in experimental autoimmune encephalomyelitis (Inoue and Shinohara, 2013) and tuberculosis (Sabir et al., 2017). IFN-β also plays an anti-inflammatory role in cerebrovascular diseases. IFN-β attenuates tight junction protein degradation in brain endothelial cells and affords protection against ischaemic stroke (Kuo et al., 2020). In intracranial hemorrhage, elevated levels of IFN-β and signal transducer and activator of transcription (STAT) 1 are accompanied by reduced levels of NLRP3 inflammasomes, caspase-1, and IL-1β (Wang, Nowrangi, et al., 2018). However, the mechanism underlying IFN-β effects in cerebrovascular diseases have not been directly evaluated. IFN-β is thought to inhibit NLRP3 inflammasome-mediated inflammatory response via three possible pathways (Figure 4): a) It represses the activity of NLRP3 inflammasomes via the STAT1 transcription factor. b) IFN-β induces IL-10 in a STAT1-dependent manner, while IL-10 reduces pro-IL-1α and pro-IL-1β production via STAT3 signalling (Guarda et al., 2011; Sabir et al., 2017). c) IFN-β can inhibit the NLRP3 inflammasome by suppressing ROS generation in antigen-presenting cells (Inoue and Shinohara, 2013). Although these three pathways have not been assessed in cerebrovascular diseases, we postulate that they might be applicable in cerebrovascular disease as STAT-1 activation is associated with neuronal cell death (Jung et al., 2015; Xu et al., 2015), and inhibition of STAT1 or STAT3 plays a protective role in stroke (Jiang et al., 2013; Tian et al., 2018; Cai et al., 2019; Cheng et al., 2019; Liu, Ran, et al., 2019; Li, Lv, et al., 2020). It is worth exploring the interaction between IFN-β and NLRP3 inflammasomes in future investigations. Understanding the relationship between the IFN-β/NLRP3 inflammasome and cerebrovascular diseases is crucial for the treatment of stroke.
Sirtuin (SIRT)/NLRP3 Inflammasome Pathway
SIRT is a class of NAD+ dependent deacylases related to cell metabolism. SIRT activation has an inhibitory effect on the NLRP3 inflammasome. SIRT acts on NLRP3 inflammasomes via two strategies: a) oxidative stress, including SIRT1-AMPK-sterol regulatory element-binding protein/NLRP3 inflammasome (Li et al., 2013) and SIRT3-superoxide dismutase 2-mtROS/NLRP3 inflammasome in atherosclerosis (Chen, Zhu, et al., 2017). b) Apoptosis and autophagy, including SIRT1/autophagy/NLRP3 inflammasome in ischaemic stroke, the SIRT3/class O of forkhead box 3a/Parkin/NLRP3 inflammasome signalling pathway in atherosclerosis, and the APMK/SIRT1/NF-κB pathway in diabetic nephropathy (He et al., 2017; Ma et al., 2018; Li, Chen, et al., 2020). However, the mechanism of action of SIRT and NLRP3 inflammasome remains unclear and requires further study.
PI3K/AKT/NLRP3 Inflammasome Pathway
The role of the PI3K/AKT pathway in stroke is well-known. It regulates downstream anti-apoptotic molecules and plays a protective role in rats after ischaemic stroke (Li, Liu, et al., 2019; Lu et al., 2019; Meng et al., 2020; Wei et al., 2020; Yang et al., 2020). However, PI3K/AKT has not been associated with the NLRP3 inflammasome in cerebrovascular diseases. Wang et al. (2020) observed that the ROS/PI3K/AKT/NLRP3 inflammasome alleviates acute lung injury (Wang, Zhang, et al., 2020), suggesting that PI3K/AKT has an inhibitory effect on the NLRP3 inflammasome. However, Cruz et al. (2007) reported that ATP-mediated, ROS-dependent PI3K activation is involved in the activation of caspase-1 and processing of IL-1β and IL-18 (Cruz et al., 2007). The findings of Cruz et al. (2007) suggest that the PI3K/AKT pathway promotes NLRP3 inflammasome activation, and the difference results between Cruz et al. (2007) and Wang et al. (2020) may be attributed to differences in models employed (Cruz et al., 2007; Wang, Zhang, et al., 2020). Accordingly, the relationship between PI3K/AKT and NLRP3 inflammasomes needs to be further explored, especially in cerebrovascular diseases.
Notably, ROS and Nrf2 can simultaneously affect “priming” and “activation.” However, ROS plays a stimulatory role, while Nrf2 plays an inhibitory role. NF-κB activates “priming” of the NLRP3 inflammasome, while P2X7R activates “activation” of the NLRP3 inflammasome. Activation of NLRP3 inflammasomes mediates damage to the nervous system through pyroptosis and apoptosis. In contrast, autophagy/mitophagy inhibits NLRP3 inflammasome activation by clearing NLRP3 inflammasome activators. The effect of the PI3K/AKT pathway on inflammasomes remains controversial, and the inhibitory mechanism of IFN-β and SIRT on NLRP3 inflammasome in cerebrovascular diseases is also unclear, necessitating further investigations. The interaction mechanism between IFN-β and NLRP3 inflammasome has been proposed, but whether this mechanism is applicable to cerebrovascular diseases needs further study. Inhibition of ROS, NF-κB, and P2X7R mediated signalling pathways and activation of autophagy, mitochondrial autophagy, Nrf2, IFN-β, and SIRT mediated signalling pathways can inhibit the NLRP3 inflammasome and play a protective role in cerebrovascular diseases. However, as these signalling pathways are not exclusively involved in NLRP3 inflammasome activation, inhibiting these signalling pathways may simultaneously affect other responses. In other words, inhibitors that target these signalling pathways are not specific. So we are going to talk about specific inhibitors of NLRP3 inflammasome.
Specific Inhibitors of NLRP3 Inflammasome
Numerous of drug studies have observed that inhibition of the upstream NLRP3 inflammasome pathway and IL-1β has a protective effect on NLRP3 inflammasome-mediated diseases, but these drugs are less specific and may evade the target. Currently available clinical therapies for NLRP3-associated diseases include drugs that target IL-1β, such as the recombinant IL-1 receptor antagonist anakinra, the neutralising IL-1β antibody canakinumab, and the soluble decoy IL-1β receptor lilonapil (Jiang et al., 2017; Dai et al., 2021). However, the suppression of NLRP3 expression is more efficient and economical. Herein, we introduce inhibitors proposed in recent years from the perspective of NLRP3 two-step activation.
Inhibitors of the Priming Step
When unstimulated, the mRNA expression levels of NLRP3 were not high. The mRNA levels of NLRP3, pro-caspase-1, and pro-IL-1β were significantly increased when DAMPs and PAMPs activated the priming response. Priming is mainly mediated by NF-κB and TLR, and inhibition of NF-κB and TLR can inhibit the inflammatory response by downregulating mRNA levels. NF-κB is involved in multiple signalling pathways; hence, this method is not specific. Reportedly, a number of extracted chemicals can improve NLRP3 inflammasome mediated disease by inhibiting NLRP3 expression.
In a mouse model of ulcerative colitis, an ethanol extract of Canna x generalis rhizome inhibited the expression of ASC mRNA, as well as the expression of NLRP3 and cleaved caspase-1 proteins, thereby inhibiting the activation of NLRP3 inflammasomes (Mahmoud et al., 2021). Notably, the ethanol extract of Canna x generalis rhizome can up-regulate the expression of intestinal occludin and claudin-1 (Mahmoud et al., 2021). Occludin and claudin-1 were impaired following cerebral ischaemia/reperfusion injury (Qu et al., 2019); hence, it may be possible to explore whether the ethanol extract has any effect on tight junction proteins of the blood-brain barrier.
ER2.4 and ER2.7, derived from Hibiscus noldeae, had similar effects on IL-1β and IL-6 when compared with AC-YVAD-CHO (a caspase-1 inhibitor) and dexamethasone, with more potent effects on IL-1β than those of dexamethasone (Tomani et al., 2020). Tomani et al. (2020) observed that the inhibitory effect of ER2.4 and ER2.7 on the NLRP3 inflammasome may be mediated via the inhibition of pro-caspase-1 expression or through some unknown mechanism, inducing the degradation of the NLRP3 inflammasome (Tomani et al., 2020).
The water extract of Artemisia scoparia inhibited NF-κB and extracellular signal-regulated kinase-mediated expression of NLRP3 and IL-1β precursor genes and proteins (Ahn et al., 2021). Furthermore, the water extract of Artemisia scoparia participated in the activation response of NLRP3 inflammasome activation, inhibiting cleavage of caspase-1 and IL-1β, and inhibiting ATP- and monosodium uric acid-mediated IL-1β production (Ahn et al., 2021).
Similarly, some compounds from the ginger plant, including 6-shogaol, 8-shogaol, and 10-gingerol, inhibited lipopolysaccharide-primed expression of pro-IL-1β and NLRP3 and inhibited ATP-mediated activation of caspase-1. Among them, 6-shogaol demonstrated the most potent inhibitory effect on IL-1β secretion and could inhibit the NLRP3 inflammasome (Ho and Chang, 2018).
In addition, traditional Chinese medicines, such as Baicalin, also have inhibitory effects on the first-step activation of NLRP3 inflammasome. In mouse atherosclerosis models, Baicalin treatment at 50 and 100 mg/kg significantly reduced NLRP3 and caspase-1 mRNA levels and delayed atherosclerosis progression (Zhao et al., 2020).
In summary, lipopolysaccharide stimulation simulates the first-step activation of the NLRP3 inflammasome, and this approach can be used to study inhibitors targeting priming. Priming is mainly mediated by NF-κB and TLR. NF-κB is involved in multiple signalling pathways; therefore, targeting priming is not specific. At present, the ability of these small molecule compounds to transport in the blood-brain barrier has not been studied, so whether these drugs have a protective effect on cerebrovascular disease is not certain. However, these small molecule compounds are promising for the treatment of cerebrovascular diseases, especially ethanol extract of Canna X generalis rhizome, because ethanol extract of Canna X generalis rhizome has an effect on the expression of tight junction proteins.
Inhibitors of the Activation Step
Drugs That Target NEK7
NEK7 is a recently discovered protein that may be involved in NLRP3 inflammasome activation. The decreased expression of NEK7 can assist MCC950 in altering the active conformation of NLRP3; however, MCC950 may disrupt the interaction between NLRP3 and NEK7 (Tapia-Abellan et al., 2019). One of the components of ginsenoside, Rg3, is a specific inhibitor of the NLRP3 inflammasome. Although it does not affect the upstream regulation of the NLRP3 inflammasome and does not affect the NLRC4 or AIM2 inflammasome, Rg3 inhibited the interaction between NEK7 and NLRP3, further inhibited the interaction between NLRP3 and ASC, inhibited the oligomerisation of ASC, and ultimately blocked the NLRP3 inflammasome cascade (Shi et al., 2020). Inhibition of NLRP3 by Rg3 is independent of ATP and has inhibitory effects in vivo. Rg3 also inhibited the priming of NLRP3, but not as potently as the interaction of NEK7-NLRP3. Furthermore, Rg3 inhibited both potassium ion efflux-independent activation of the NLRP3 inflammasome and the potassium ion efflux-dependent interaction of NEK7-NLRP3 (Shi et al., 2020). The possibility that Rg3 inhibits potassium ion outflow cannot be excluded, warranting further investigations (Shi et al., 2020). As NEK7 is a newly discovered component of the NLRP3 inflammasome, limited studies on inhibitors targeting it are available, and exploration of NEK7 inhibitors can be undertaken in the future. Aalinkeel et al. (2018) used nanotechnology to increase the transport of Rg3 on blood-brain barrier, which had a protective effect on Alzheimer's disease (Aalinkeel et al., 2018). The application of nanotechnology to other NLRP3 inflammasome inhibitors is expected to boost the ability of drugs to cross the blood-brain barrier and thus treat neurological diseases.
Drugs That Target NLRP3
Targeting NLRP3 is the most investigated strategy, especially targeting the NACHT structure. The NACHT domain is vital for NLRP3 oligomerisation, a key step in the assembly of NLRP3 inflammasomes (Huang et al., 2018).
MCC950
MCC950, also known as CP-456773 or CRID3 (Guzova et al., 2019; Kuwar et al., 2019), is widely known as the most potent and specific NLRP3 inhibitor (Dai et al., 2021). It is often used as a positive control to compare the efficacy of novel NLRP3 inhibitors; for instance, the discovery of nitrostitu-quinazolin-4 (3H)-one 2 K to inhibit the activation of NLRP3 inflammatory body by occupying the ATP-binding site of NLRP3 protein (Abdullaha et al., 2019). MCC950 has demonstrated a beneficial effect in mouse models of several NLRP3 related diseases (Jiang et al., 2017). Multiple studies have reported that MCC950 inhibited the NLRP3 inflammasome in the NACHT domain (Tapia-Abellan et al., 2019; Vande Walle et al., 2019; Dai et al., 2021). The binding of MCC950 to NACHT required a complete (d)ATP-binding pocket, but (d)ATP-binding pocket was significantly reduced in most cap-associated NLRP3 mutants (Vande Walle et al., 2019). Blockade of the mutant p.D305N NLRP3 in cryopyrin-associated periodic syndrome monocytes required a higher concentration of MCC950 (Tapia-Abellan et al., 2019). In vivo, MCC950 showed weak inhibition of NLRP3 inflammasomes in two cryopyrin-associated periodic mouse models (Vande Walle et al., 2019). MCC950 partially blocked the interaction between NLRP3 and NEK7 in ischaemia/reperfusion-induced lung injury models (Xu, Wu, et al., 2018). Instead of binding to NEK7, MCC950 directly targets an NLRP3 site, in or near the Walker B motifs to block ATP hydrolysis, resulting in the formation of an inactivated NLRP3 structure, thereby preventing the activation of NLRP3 (Tapia-Abellan et al., 2019). In recent years, it has been observed that MCC950 inhibits ASC oligomerization and inhibits the cleavage of caspase-1 (p20) (Chow et al., 2020; Dai et al., 2021). Guzova et al. (2019) proposed that mitochondrial transporters ABCb7 and ABCb10 are the pharmacological targets of CP-453773; although this hypothesis has been proven incorrect, they found that undifferentiated THP1 cells can serve as a reliable and simplified model for investigating NLRP3 inflammasomes (Guzova et al., 2019). MCC950 was found to increase serum liver enzyme levels in a phase II clinical trial in rheumatoid arthritis; hence, it was not further developed (Agarwal, Pethani, et al., 2020). Abdullaha et al. (2020) reported that IIIM-1266 and IIIM-1270 inhibited NLRP3 inflammasomes at the same locus as MCC950, and IIIM-1266 could be developed as a novel drug (Abdullaha et al., 2020).
MCC950 was once considered a specific inhibitor of NLRP3, but recent studies have found that MCC950 may be involved in the priming process of the NLRP3 inflammasome. In a dose-dependent manner, MCC950 enhanced TNF-α secretion in peripheral blood mononuclear cells of Muckle-Wells syndrome patients (Kaneko et al., 2020) and inhibited bleomycin-induced chloride effusion of NLRP3−/− bone marrow-derived macrophages (Jiang et al., 2017). In the liver of old mice, MCC950 can inhibit the PI3K/AKT/mammalian target of rapamycin and enhance autophagy activity (Marin-Aguilar et al., 2020). These findings could be attributed to different cell and reaction conditions, and further investigations assessing the inhibitory effect of MCC950 on NLRP3 are needed. MCC950 has been extensively studied in NLRP3 inflammasome-associated diseases. In mice with hypertension, MCC950 reduced blood pressure and limited renal inflammation, fibrosis, and dysfunction (Krishnan et al., 2019). In a porcine liver transplantation model, MCC950 improved the prognosis of organs from donors after circulatory death (Yu, Cheng, et al., 2019). In ischaemia/reperfusion-induced lung injury, reduced the production of IL-1β and IL-18 and inhibited neutrophil infiltration and apoptosis (Xu, Wu, et al., 2018). In a traumatic brain injury model, treatment with MCC950 alleviated brain oedema, reduced lesion volume, improved long-term motor and cognitive function, and improved neurological function after traumatic brain injury by reducing microglial activation, leucocyte recruitment, proinflammatory cytokine production, compaction protein loss, and cell death (Xu, Yin, et al., 2018).
Oridonin
Oridonin has demonstrated anti-inflammatory, anti-tumour, antioxidant, and neuroregulatory effects and has been shown to possess preventive or therapeutic effects in mouse models of peritonitis, gouty arthritis, and type 2 diabetes (Zhao, Zhang, et al., 2017; He et al., 2018). Zhao et al. (2017) reported that oridonin inhibited NF-κB p65, as well as the secretion of IL-1β, IL-6, and TNF-α (Zhao, Zhang, et al., 2017), suggesting that oridonin may affect priming. Oridonin reportedly inhibits NLRP3 inflammasome assembly and activation by forming covalent bonds with cysteine 279 of the NACHT domain of NLRP3, presenting no association with NF-κB-mediated priming (He et al., 2018). Like MCC950, it blocked the interaction between NLRP3 and NEK7 (He et al., 2018), suggesting that a molecule targeting NACHT can inhibit the interaction between NEK7 and NLRP3. As NEK7 was only recently discovered, there are no further studies supporting this hypothesis, warranting verification in future investigations.
CY-09
CY-09 is considered a specific inhibitor of the NLRP3 inflammasome, demonstrating no effect on the lipopolysaccharide-induced expression of TNF-α, IL-1β, and NLRP3, indicating that it does mediate its effect on the NLRP3 inflammasome via priming (Jiang et al., 2017). CY-09 does not affect potassium effusion and chlorine effusion, nor does it affect the status of the AIM2 or NLRC4 inflammasome. It acts upstream of ASC oligomerisation and inhibits NLRP3-ASC interaction (Jiang et al., 2017). By directly binding to the Walker A motif of the NLRP3 NACHT domain, CY-09 blocks the binding of NLRP3 to ATP and inhibits the ATPase activity of NLRP3, thus inhibiting the assembly and activation of NLRP3 inflammasomes (Jiang et al., 2017). In vivo, CY-09 actively prevented NLRP3 mediated acute inflammation, with significant therapeutic effects in cryopyrin-associated periodic syndrome and mouse models of type 2 diabetes (Jiang et al., 2017). Sun et al. (2020) reported that inhibition of the NLRP3 inflammasome by CY-09 could reverse the increase in neuronal pyroptosis caused by the low-density lipoprotein receptor−/− after ischaemia (Sun et al., 2020). In a mouse model of epilepsy, CY-09 reportedly inhibited astrocyte activation and neuronal loss (Shen, Jiang, et al., 2020). In a study assessing nonalcoholic fatty liver disease, CY-09 was found to downregulate blood triglyceride levels in mice (Wang, Sun, et al., 2021). Triglyceride levels play an important role in the pathogenesis of atherosclerosis and stroke. Based on effects on nervous system diseases and triglycerides, CY-09 could be utilised in cerebrovascular diseases. Furthermore, Jiang et al. (2017) found that the CY-09 analogue, C172, was also a specific inhibitor of NLRP3 (Jiang et al., 2017).
OLT1177
OLT1177 is a novel oral small-molecule specific inhibitor of NLRP3 (Lonnemann et al., 2020). OLT1177 did not affect the mRNA expression levels of NLRP3, ASC, caspase-1, IL-1β and IL-18, with no impact on NLRC4 and AIM2 inflammasomes (Marchetti et al., 2018). OLT1177 binds to the NLRP3 nucleotide-binding domain and inhibits ATPase activity and the interaction of NLRP3-ASC and NLRP3-caspase-1, thus inhibiting the polymerisation of NLRP3 inflammasomes (Marchetti et al., 2018). OLT1177 can alleviate myocardial ischaemia/reperfusion injury in mice (Toldo et al., 2019), and improve cognitive impairment in a mouse model of Alzheimer's disease (Lonnemann et al., 2020). Marchetti et al. (2018) revealed that oral administration of 1000 mg OLT1177 daily for 8 days was safe in healthy individuals (Marchetti et al., 2018). OLT1177 is currently in phase II clinical trials for treating inflammation and is expected to be developed as a targeted agent for NLRP3 inflammasomes in the future (Marchetti et al., 2018; Lonnemann et al., 2020). Lonnemann et al. (2020) observed that OLT1177 could inhibit the release of TNF-α by microglial cells (Lonnemann et al., 2020); however, Marchetti et al. (2018) found that OLT1177 did not affect TNF-α or “priming” (Marchetti et al., 2018). The difference in the results of these two experiments may be due to different cell types, Lonnemann et al. (2020) used microglia from a mouse model of Alzheimer's disease (Lonnemann et al., 2020), while Marchetti et al. (2018) used macrophages from murine and human (Marchetti et al., 2018). Additional studies are needed to determine whether OLT1177 affects priming.
Tranilast
Tranilast, an analogue of a tryptophan metabolite, was initially used as an anti-allergy treatment and has since been employed to treat various diseases (Darakhshan and Pour, 2015). Tranilast is considered an effective and extensive inhibitor of both canonical and non-canonical NLRP3 inflammasome activation, with no inhibitory effects on the NLRC4 or AIM2 inflammasomes (Huang et al., 2018). Reportedly, the sites of action of tranilast on NLRP3 inflammasomes are downstream of potassium ion efflux, mitochondrial damage, and chlorine efflux, and upstream of caspase-1 and ASC oligomerization (Huang et al., 2018). Additional studies have revealed that tranilast directly binds to the NACHT domain of NLRP3 and inhibits the formation of the NLRP3‐ASC complex, further blocking the oligomerisation and assembly of NLRP3 and inhibiting the activation of NLRP3 inflammasome (Huang et al., 2018). Moreover, tranilast inhibited the direct interaction between NLRP3 and NLRP3. Tranilast also inhibited the cytokine-induced activation of NF-κB (Huang et al., 2018). Zhuo et al. (2019) found that tranilast could reduce neuronal apoptosis in a rat ischaemia/reperfusion model, affect NF-κB, and decrease the mRNA and protein expression of cytokines (Zhuo and Zhuo, 2019). This suggests that tranilast may also have an inhibitory effect on priming. The effect of NF-κB was excluded in the study by Huang et al. (2018) (Huang et al., 2018); hence, the relationship between tranilast and NF-κB needs to be further investigated. Moreover, tranilast inhibited the activation of the NLRP3 inflammasome in vivo, demonstrating a protective effect on NLRP3 mediated acute inflammation and tissue damage, which could be employed in clinical practice (Huang et al., 2018).
Tetrahydroquinoline Inhibitors
Compound 6, a tetrahydroquinoline inhibitor synthesised by Dai et al. (2021), inhibited NLRP3 inflammasome activity in vivo and in vitro, but did not affect AIM2 and NLRC4 inflammasomes (Dai et al., 2021). Regarding the mechanism of action, compound 6 did not block potassium extravasation and did not bind to the PYD or LRR domain. Instead, compound 6 directly binds to the NLRP3 NACHT domain and blocks NLRP3 ATPase activity (Dai et al., 2021). Finally, it inhibited the activation of the NLRP3 inflammasome and relieved NLRP3 inflammasome-induced colitis (Dai et al., 2021).
Drugs That Target ASC
ASC oligomerisation is an upstream event in inflammasome activation and is involved not only in the activation of NLRP3 but also in the activation of AIM2; hence, inhibitors targeting ASC also affect AIM2 inflammasomes. Furthermore, inhibition of ASC weakly inhibits NLRC4 inflammasomes (Franklin et al., 2014; Chen, Li, et al., 2020).
Dehydrocostus Lactone
Dehydrocostus lactone is a natural sesquiterpene lactone that inhibits the activation of NLRP3 inflammasomes in THP-1 cells and human peripheral blood mononuclear cells, improving the inflammatory response in lipopolysaccharide-induced inflammatory mice (Li, Yuan, et al., 2019; Chen, Li, et al., 2020). Furthermore, dehydrocostus lactone significantly inhibited the aggregation of ASC and affected the activation of NLRP3, AIM2, and NLRC4 inflammasomes, with the strongest effect on NLRP3 inflammasomes (Chen, Li, et al., 2020). Dehydrocostus lactone also inhibited potassium outflow, which may be responsible for the potent inhibition of NLRP3 and the weak inhibition of AIM2 (Chen, Li, et al., 2020). Dehydrocostus lactone is reportedly involved in regulating NF-κB pathways in acute lung injury and bone metabolic disease (Hu et al., 2019; Nie et al., 2019). Chen et al. (2020) observed that dehydrocostus lactone inhibited the expression of NF-κB-dependent NLRP3 and IL-1β, and therefore inhibited the initiation of NLRP3 inflammasome activation (Chen, Li, et al., 2020).
Sulforaphane
Oral sulforaphane reduced symptoms and inflammatory infiltrates in a mouse model of acute foot gout, attributed to inhibition of the NLRP3 inflammasome by sulforaphane (Yang, Yeon, et al., 2018). This inhibition is not dependent on the ROS pathway or any stimulus-specific pathway, such as lysosomal rupture, P2X7, or potassium release, but is rather related to the inhibition of ligand-independent activation of the NLRP3 inflammasome (Yang, Yeon, et al., 2018). Furthermore, sulforaphane inhibited ATP- or bleomycin-induced ASC oligomerisation and blocked the activity of various NLRP3 inflammasome activators without inhibiting the AIM2 inflammasome (Yang, Yeon, et al., 2018). Additionally, sulforaphane inhibited the activity of the NLRP3 inflammasome by regulating the inflammasome complex itself and the AMP-activated protein kinase-autophagy axis (Yang, Yeon, et al., 2018).
KN3014
Cell-based screening using normal human peripheral blood mononuclear cells revealed that 50 µm KN3014 strongly inhibited IL-1β secretion. Additionally, KN3014 inhibited the constitutive autologous secretion of IL-1β from peripheral blood mononuclear cells derived from patients with Muckle-Wells syndrome (Kaneko et al., 2020). KN3014 presented no serious cytotoxicity and could be developed for clinical application (Kaneko et al., 2020). Reportedly, KN3014 did not affect the activity of NF-κB and did not affect priming. Instead, it targeted the interaction between NLRP3 and ASC through PYD, thereby inhibiting the inflammatory activation of NLRP3 (Kaneko et al., 2020).
Thiazolo-Alkenyl Sulfonylurea Derivative 7
Agarwal et al. (2020) reported that thiazolo-alkenyl sulfonylurea derivative 7 inhibited the activation of NLRP3 by inhibiting ASC oligomerisation (Agarwal, Pethani, et al., 2020). Unlike other ASC inhibitors, thiazolo-alkenyl sulfonylurea derivative 7 does not affect the AIM2 inflammasome, but its inhibitory effects on CYP2C8 and CYP2C9 limit its in vivo application, despite its good pharmacokinetic properties (Agarwal, Pethani, et al., 2020).
Drugs That Target Caspase-1
Currently, Z-YVAD-FMK is the most commonly employed irreversible caspase-1 inhibitor with cell permeability (Li, Yan, et al., 2018). It blocks necrosis and the release of IL-1β and IL-18 by inhibiting caspase-1 p20 cleavage (Li, Yan, et al., 2018; Gao et al., 2019; Nyiramana et al., 2020). Chow et al. (2020) observed that Z-YVAD-FMK had a poor inhibitory effect on human caspase-1 and reduced cell death to a certain extent, but failed to completely inhibit NLRP3 inflammasome-mediated cell death (Chow et al., 2020). Other molecules were also found to inhibit caspase-1, such as Z-VAD-FMK (Chow et al., 2020) and Q-VD-OPH (Altaee and Gibson, 2020; Butkevych et al., 2020), thereby inhibiting the downstream caspase-1 reaction.
X-linked inhibitor of apoptosis protein is considered a caspase-1 inhibitor; however, Gao et al. (2019) proposed that X-linked inhibitor of apoptosis protein may be located downstream of caspase-1 and participate in the regulation of cytokine secretion (Gao et al., 2019). They also found that blocking caspase-1 p20 cleavage was associated with the preservation of the X-linked inhibitor of apoptosis protein (Gao et al., 2019). Inflammasome-mediated IL-1β and IL-18 release also depended on the expression of the X-linked inhibitor of apoptosis protein (Gao et al., 2019). Reports regarding NEK7 and X-linked inhibitor of apoptosis protein suggest that some unknown molecules may be involved in activating the NLRP3 inflammasome. Furthermore, exploring the NLRP3 inflammasome structure could help increase targets for future NLRP3 inflammasome therapy.
To sum up, inhibitors that inhibit the second-step activation of the NLRP3 inflammasome, especially those targeting NLRP3, have been studied extensively. Currently, there are few inhibitors targeting the newly discovered structure NEK7. Nanotechnology has promoted the transport of NEK7 inhibitors across the blood-brain barrier, and the application of nanotechnology is expected to broaden the range of therapeutic drugs for cerebrovascular diseases. MCC950 is the most widely used NLRP3 inflammasome specific inhibitor. The interaction mechanism between MCC950 and NACHT has been well defined. In recent years, there has been new understanding of the interaction between MCC950 and NLRP3, for example, it also affects NEK7 and ASC, and may even affect the priming of NLRP3 inflammasome. Unfortunately, the clinical trial found that MCC950 had an effect on serum liver enzyme levels, so the clinical trial was not further developed. However, MCC950 is still widely used as a specific inhibitor of NLR3 inflammasome, and has been used to compare the efficacy against NLRP3. Based on MCC950, several inhibitors of NLRP3 inflammasome have been identified. In the study of MCC950, THP1 cells were found to be a reliable and simple model for the study of NLRP3 inflammasome specific inhibitors. The interaction mechanism of oridonin on NLRP3 is similar to that of MCC950 and also related to NACHT and NEK7. The effects of MCC950 and oridonin on NACHT and NEK7 suggest that there may be a relationship between NACHT and NEK7, which requires further exploration. Other small molecule compounds also target NACHT, such as CY-09. It has been proved in animal models that CY-09 has a protective effect on cerebrovascular diseases, but whether it can be applied in clinical practice still needs further study. OLT1177 is also a small molecule targeting NACHT, and whether it affects priming is controversial. Phase II clinical trials of OLT1177 are currently underway and have found that OLT1177 is safe orally. OLT1177 has been shown to protect against cardiac ischemia/reperfusion injury and central nervous system diseases in animal models. The effect of OLT1177 on central nervous system diseases suggests that OLT1177 can penetrate the blood-brain barrier. Therefore, OLT1177 is expected to be applied in the treatment of cerebrovascular diseases. At present, there is no study on OLT1177 and cerebrovascular diseases, so it is of great significance to further study the role of OLT1177 in cerebrovascular diseases. Tranilast was initially used as an anti-allergy treatment. In recent years, a study found that tranilast has a protective effect in animal models of cerebral ischemia, and more evidence is needed. ASC is involved not only in the activation of NLRP3 inflammasome, but also in the activation of AIM2 inflammasome, so inhibitors targeting ASC may inhibit both AIM2 and NLRP3. There are relatively few drugs targeting ASC and caspase-1.
Specific Inhibitors With No Identified Targets
Currently, some drugs with specific inhibitory effects on NLRP3 inflammasomes have been identified; however, their exact mechanisms of action require further research.
Compound 17 (YQ128) identified from HL16 is a selective inhibitor of the NLRP3 inflammasome (Jiang et al., 2019). As it can cross the blood-brain barrier in vitro and in vivo and is unlikely to be affected by efflux transport, it demonstrates potential as a treatment for central nervous system diseases (Jiang et al., 2019). However, its low oral bioavailability (10%) limits its application in vivo, and further analogue development based on this new chemical scaffold could be possible in the future (Jiang et al., 2019).
Ethyl pyruvate has a specific inhibitory effect on NLRP3 inflammasomes but not on AIM2 and NLRC4, acting independently of potassium efflux and lysosomal rupture (Li, Liang, et al., 2018). Reportedly, the inhibitory effect of ethyl pyruvate on NLRP3 inflammasomes could be partially achieved by inhibiting mitochondrial damage; however, this inhibitory effect on mitochondrial damage occurs independently of mtROS production (Li, Liang, et al., 2018).
In colitis-associated cancer, arctigenin inhibited α-tubulin acetylation by downregulating the expression of carnitine palmitoyltransferase 1, thereby disrupting NLRP3 assembly (Qiao et al., 2020). Arctigenin also inhibited the expression of NLRP3 mRNA, but the effect was weaker than that on NLRP3 assembly (Qiao et al., 2020).
Glibenclamide is an ATP-sensitive K+ channel inhibitor used in the treatment of type 2 diabetes (Carvalho et al., 2020). Additionally, glibenclamide demonstrates neuroprotective effects, which can reduce infarct volume, brain oedema, activation of microglial cells, production of inflammatory factors, protection of the blood-brain barrier, and restoration of tight junction expression in the brain (Hou et al., 2020). Glibenclamide inhibited the NLRP3 inflammasome by inhibiting the ATPase activity of NLRP3 and downregulating TNF and IL-17 levels (Carvalho et al., 2020); however, the high doses needed to achieve the inhibitory effects in vivo may cause fatal hypoglycaemia (Kuwar et al., 2019).
A novel NLRP3 inflammasome-specific inhibitor, JC124, was developed based on the glibenclamide structure. JC124 selectively inhibits the NLRP3 inflammasome pathway both in vivo and in vitro (Kuwar et al., 2019). The JC124 target on NLRP3 inflammasome is yet to be determined, demonstrating effects on ROS and TNFα levels; thus, JC124 may be involved in regulating the priming response of NLRP3. Further analysis of the components of JC124 revealed that compounds 14 and 17 had similar inhibitory effects as MCC950 on NLRP3 in vivo (Fulp et al., 2018). Moreover, JC124 can improve cognition and myocardial infarction (Fulp et al., 2018) and could be developed for clinical applications in cardiovascular and cerebrovascular diseases.
In a word, there are also some specific inhibitors whose specific targets are unknown at present and need to be further determined. Some drugs that have been used clinically have specific inhibitory effects on NLRP3, such as glibenclamide, but glibenclamide produces fatal hypoglycemia at doses that inhibit NLRP3. A new compound based on glibenclamide, JC124, was developed without the side effect of fatal hypoglycemia. At the same time, JC124 can also improve myocardial ischemia and cognition, and is expected to be used in cerebrovascular diseases.
Promising Directions for Drug Research
Based on findings reported by Agarwal et al. (2020), compounds generated after structurally modifying the sulfonylurea part of MCC950 also demonstrated inhibitory effects on the NLRP3 inflammasome (Agarwal, Sasane, et al., 2020); hence, it was possible to develop novel NLRP3 inflammasome inhibitors based on the sulfonylurea structure. Virtual screening of large compound libraries is an ideal strategy to develop new drugs (Abdullaha et al., 2020). Aalinkeel et al. (2018) used nanotechnology to increase the transport of Rg3 on blood-brain barrier (Aalinkeel et al., 2018). For inhibitors that are hard to cross the blood-brain barrier, nanotechnology may give them a promising application in central nervous system diseases. On investigating specific inhibitors, the effects of drugs on the upstream regulation of NLRP3, including K+ effusion, ROS production, and mitochondrial membrane potential, should be avoided. The drug effects on other inflammasomes should also be evaluated.
We concluded that inhibition of the NLRP3 inflammasome significantly improved neurological deficits and prognosis in cerebrovascular diseases. Although some drugs and molecules have not been employed in the study of cerebrovascular diseases, their inhibition of the NLRP3 inflammasome suggests their potential for improving cerebrovascular diseases. Overall, the most promising of the NLRP3 inflammasome specific inhibitors for the treatment of cerebrovascular disease may be molecules that target NACHT. Due to the few molecular studies targeting NEK7, ASC, and caspase-1, the potential therapeutic effect of drugs targeting these structures cannot be ruled out and further studies are needed to determine this. Notably, the NLRP3 inflammasome inhibitor derived from H. noldeae is often used to treat inflammatory diseases of the respiratory system, including asthma (Tomani et al., 2020). Moreover, coronavirus disease 2019 remains widespread worldwide, and the NLRP3 inflammasome is also thought to play a crucial role in coronavirus disease 2019 (Freeman and Swartz, 2020). The use of NLRP3 inflammasome inhibitors may benefit patients with coronavirus disease 2019; however, further studies are warranted.
Conclusions
The NLRP3 inflammasome is a vital component of the immune system and plays an important role in cerebrovascular diseases.
NLRP3 Inflammasome in Ischaemic Stroke
Oxidative stress in the ischaemic core after ischaemic stroke is the main stimulator of NLRP3 inflammasome activation, and NLRP3 inflammasome-mediated neuroinflammation is related to post-ischemic inflammation. In ischaemic stroke, NLRP3 inflammasomes mediate infiltration of inflammatory cells and cytokines, and destroy tight junction proteins on the blood-brain barrier, finally aggravates brain injury.
NLRP3 Inflammasome in Intracerebral Haemorrhage
Oxidative stress plays a major role in the activation of NLRP3 inflammasome in early brain injury after intracerebral haemorrhage. Activation of NLRP3 inflammasome mediates secondary brain injury in intracerebral haemorrhage. Furthermore, NLRP3 inflammasomes mediate infiltration of inflammatory cells and cytokines, damage the blood-brain barrier, mediate neuronal degeneration and apoptosis, and aggravate the neurological function deficit.
NLRP3 Inflammasome in SAH
NLRP3 inflammasome activated by oxidative stress injury in SAH can promote infiltration of inflammatory cells and cytokines, mediate neuronal apoptosis, destroy the blood-brain barrier, and aggravate brain oedema. Unlike ischaemic stroke and intracerebral haemorrhage, NLRP3 inflammasome is associated with microthrombosis in SAH. Microthrombosis plays an important role in SAH. Microthrombosis may aggravate local cerebral hypoperfusion in the early stage of SAH and is also a major pathological change in secondary brain injury. However, there are few studies on the relationship between microthrombosis and NLRP3 inflammasome, and further studies are needed.
Signalling Pathways of NLRP3 Inflammasome in Cerebrovascular Diseases
NLRP3 inflammasome is involved in multiple signaling pathways of cerebrovascular diseases, among which ROS/NF-κB/NLRP3 inflammasome pathway, ROS/TXNIP/NLRP3 inflammasome pathway and P2X7R/NLRP3 inflammasome pathway have a clear aggravation effect on cerebrovascular diseases. Autophagy/mitophagy, IFN-β/NLRP3 inflammasome pathway and SIRT/NLRP3 inflammasome pathway have clear ameliorative effects on cerebrovascular diseases. The role of PI3K/AKT/NLRP3 inflammasome pathway in cerebrovascular diseases is controversial. The mechanism of interaction between NF-κB and autophagy/mitophagy on NLRP3 inflammasomes has been relatively well established. The interaction mechanisms between Nrf2 and NF-κB, TXNIP and ROS, and IFN-β and NLRP3 have been proposed, but whether these mechanisms are applicable to cerebrovascular diseases needs further study. Inhibition of the activation of NLRP3 inflammasome in these signaling pathways has a protective effect on cerebrovascular diseases, but this inhibition is not specific.
Specific Inhibitors of NLRP3 Inflammasome
Currently, many small molecule specific inhibitors of NLRP3 inflammasome have been developed. These compounds target the different structures of NLRP3 inflammasome and have specific inhibitory effects on NLRP3 inflammasome, which are expected to be applied in the treatment of cerebrovascular diseases. Virtual screening of large compound libraries, THP1 cells, and nanotechnology are helpful for the development of NLRP3 inflammasome specific inhibitors for cerebrovascular diseases.
Supplemental Material
sj-pdf-1-asn-10.1177_17590914211018100 - Supplemental material for The Role of NLRP3 Inflammasome in Cerebrovascular Diseases Pathology and Possible Therapeutic Targets
Supplemental material, sj-pdf-1-asn-10.1177_17590914211018100 for The Role of NLRP3 Inflammasome in Cerebrovascular Diseases Pathology and Possible Therapeutic Targets by Rongrong Bai, Yue Lang, Jie Shao, Yu Deng, Reyisha Refuhati and Li Cui in ASN Neuro
Footnotes
Acknowledgments
Figures 2 to 4 were produced using Servier Medical Art (www.servier.com). We would like to thank Editage (![]() ) for English language editing.
) for English language editing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
