Abstract
Background:
This network meta-analysis assessed the comparative risk of grade 3–5 and grade 5 treatment-related adverse events (TRAEs) for immune checkpoint inhibitors (ICIs), either alone or in combination with other modalities, for cancer treatment.
Methods:
PubMed, Embase, Cochrane Library, Web of Science, and recent predominant oncology congresses were searched for relevant phase II and phase III randomized controlled trials (RCTs). As outcomes, grade 3–5, and grade 5 TRAE outcomes were reported as odds ratios and 95% confidence intervals.
Results:
In 67 RCTs involving 36,422 patients and 19 ICIs, the incidence of grade 3–5 and grade 5 TRAEs was 17.9% and 0.8% with ICI monotherapy and 46.3% and 1.4%, respectively, with combinatorial therapy. Pneumonitis was the most common cause of grade 5 TRAEs following either monotherapy (16.3%) or combinatorial therapy (11.4%). Regarding grade 3–5 TRAEs, atezolizumab + chemotherapy (CT) and antiangiogenic therapy (AT) (atezolizumab + CAT), pembrolizumab + CT, ipilimumab + CT, and atezolizumab + CT were more toxic than any ICI monotherapy, pembrolizumab or nivolumab + radiotherapy (RT), and ICIs dual therapy (durvalumab + tremelimumab and nivolumab + ipilimumab). Tremelimumab, ipilimumab, durvalumab, and pembrolizumab were, however, associated with higher grade 5 TRAEs than combinatorial treatments. Atezolizumab + CAT was the most toxic and nivolumab + RT was the least toxic of combinatorial treatments; among monotherapies, tremelimumab and avelumab were the most and least toxic, respectively. The toxicity ranking changed with type of grade 3–5 TRAEs.
Conclusions:
Compared with combinatorial therapy, ICI monotherapy caused lower grade 3–5 TRAEs, but some monotherapies resulted in a higher incidence of fatal TRAEs. Atezolizumab + CAT and nivolumab + RT were the most and least toxic of combinatorial treatments, respectively, and tremelimumab and avelumab were the most and least toxic of the monotherapies, respectively.
Keywords
Introduction
Immune checkpoint inhibitors (ICIs), including programmed cell death-1 (PD-1), programmed cell death ligand-1 (PD-L1), and cytotoxic T lymphocyte antigen-4 (CTLA-4) inhibitors, have revolutionized the treatment of many cancers. These agents can upregulate T cell activity, leading to an immune response against cancer cells. However, the increased activity of T cells can also induce autoimmune toxicities by unbalancing the immune system. 1 ICIs have been reported to cause a wide spectrum of immune-related adverse events (irAEs), such as skin, gastrointestinal, endocrine, hepatic, pulmonary, and cardiovascular toxicities. 2 In general, most irAEs are mild and can be well controlled with supportive treatment and glucocorticoids. However, the incidence of irAEs appears to have increased with the rapidly growing number of patients receiving ICIs, and some irAEs are serious with fatal outcomes.
Currently, the United States Food and Drug Administration (FDA) has approved several ICIs for the treatment of various cancers, including two PD-1 inhibitors (nivolumab and pembrolizumab), three PD-L1 inhibitors (atezolizumab, avelumab, and durvalumab), and two CTLA-4 inhibitors (ipilimumab and tremelimumab). As individual ICIs influence different immunologic mechanisms, the frequencies, severities, and profiles of the irAEs may vary.2–6 Moreover, ICIs in combination with conventional therapy [chemotherapy (CT), antiangiogenic therapy (AT), or their combinations] or with a second ICI, are being increasingly used, and these combinations have demonstrated survival advantage over monotherapy in several tumors.7–10 However, combinatorial therapy may also result in an increased risk of treatment-related adverse events (TRAEs). To date, evidence regarding head-to-head comparisons among ICIs is lacking, and therefore, determining which monotherapy or combinatorial therapy has the most or the least toxicity remains undefined.
Safety is the critical factor for drug evaluation. A better understanding of the comparative safety profiles between the ICIs would be helpful in clinical decision making. In this study, we performed a systematic review and network meta-analysis to assess the comparative risk of grade 3–5 and grade 5 TRAEs among 19 ICIs used in cancer treatment.
Methods
Literature search strategy
This network meta-analysis was performed according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) criteria (Supplemental Table S1). 11 We systematically searched PubMed, Embase, the Cochrane Library, Web of Science, and the most recent oncology congresses (American Society of Clinical Oncology, American Society of Radiation Oncology, European Society for Medical Oncology, and World Conference on Lung Cancer) for available studies published before 1 November 2019. The search strategy is detailed in Supplemental Table S2. The reference lists of all relevant publications were also assessed for additional eligible studies.
Inclusion and exclusion criteria
Studies were included if they met all of the following criteria: (a) phase II or phase III randomized controlled trials (RCTs) of patients with cancer; (b) at least one treatment arm received an FDA-approved ICI, alone or in combination with another ICI or conventional therapy; (c) reported data of grade 3–5 and/or grade 5 TRAEs in each arm; and (d) published in English. When multiple publications covered the same study population, the one with the most recent and comprehensive data was used. Studies that failed to meet the above criteria were excluded from the network meta-analysis.
Data extraction
To better assess the toxicity of ICIs, especially in combinatorial treatments, we evaluated TRAEs instead of irAEs as the outcomes of interest. Two investigators independently extracted the following data from each study: the first author or the name of the RCT, year of publication, region, cancer type, study design, follow-up time, number of patients, interventions, and the number of grade 3–5 and grade 5 TRAEs.
Quality assessment
Two investigators independently assessed the risk of bias of the included RCTs using the Cochrane Collaboration’s tool, 12 which includes the following five domains: sequence generation, allocation concealment, blinding, incomplete data, and selective reporting. Blinding cannot be applied in studies with specific designs (such as open-label or cross-over) owing to unavoidable reasons. If such reasons were clearly stated in the included studies, these studies were rated as “+.” An RCT was judged to have a “low risk of bias,” a “high risk of bias,” or an “unclear risk of bias” if all domains indicated low risk, one or more domains indicated high risk, or more than three domains indicated as unclear risk, respectively.
Statistical analysis
The outcomes of interest were grade 3–5 and grade 5 TRAEs. Odds ratios (ORs) and their 95% confidence intervals (CIs) were used as summary statistics to estimate treatment effects. If a study reported zero grade 5 TRAEs in any arm, a half integer continuity correction (adding a 0.5 to each cell) was applied to calculate ORs. For direct comparisons, a standard pairwise meta-analysis was performed using R (version 3.5.0). The heterogeneity among studies was assessed using the chi-squared (χ2) and I-squared (I2) tests. A p value greater than 0.10 or an I2 value greater than 50% indicated substantial heterogeneity, and a random-effects model was used; otherwise, a fixed-effects model was used.
The Bayesian network meta-analysis was conducted using a random-effects model (generalized linear model) using the Markov chain Monte Carlo method in OpenBUGS (version 3.2.3). 13 For each outcome measure, four independent Markov chains were simultaneously run for 20,000 burn-ins and 100,000 inference iterations per chain to obtain the posterior distribution. The traces plot and Gelman–Rubin method were used to assess the convergence of the model. 14 Relative toxicity rankings were assessed according to the surface under the cumulative ranking curve (SUCRA) method. 15 SUCRA equals one if the treatment is certain to be the worst, and zero if it is certain to be the best. The transitivity assumption was assessed by comparing the distribution of potential effect modifiers (sample size, median age, and median follow-up time) across treatment comparisons. 16 Global inconsistency was evaluated by comparing the fit of the consistency and inconsistency models using a design-by-treatment test 15 ; local inconsistency was assessed by calculating the difference between the direct and indirect estimates in the treatment loops using the loop-specific approach, 15 and by testing between direct and indirect results within the treatment loops using node-split models 17 ; p < 0.05 indicated significant inconsistency. We assumed a common heterogeneity parameter for all comparisons and used the between-study heterogeneity variance, τ², to assess the extent of heterogeneity for each outcome.18,19 We conducted subgroup meta-regressions (sample size, treatment line, tumor type, drug dose, control arm, and study risk of bias) to search for the sources of heterogeneity.
Sensitivity analyses were conducted to assess the stability of the results by omitting studies with a high overall risk of bias, a sample size <100, or a placebo-controlled trial as well as by dividing the trials of nivolumab + ipilimumab into two dose groups [nivolumab (3 mg) + ipilimumab (1 mg) and nivolumab (1 mg) + ipilimumab (3 mg)] and the trials of pembrolizumab into three dose groups (200 mg, 2 mg/kg, 10 mg/kg). In addition, we performed subgroup analyses based on the nature and severity of TRAEs. Publication bias was examined using funnel plots. 20
Results
Literature search results and characteristics of included RCTs
The details of our literature search and study selection process are shown in Figure 1. The initial literature search identified 38,457 studies, of which 244 were deemed potentially eligible and were thus retrieved for detailed assessment. The relevant references were also reviewed for any missed studies. Finally, 67 RCTs involving 36,422 patients and evaluating 22 treatments (including CT, AT, placebo, and 19 ICIs) were included in the network meta-analysis.8–10,21–95 Among the 19 ICI-based treatments, 7 were monotherapies (nivolumab,21–31 pembrolizumab,32–43 atezolizumab,44–47 avelumab,48,49 durvalumab,91,93,95 ipilimumab,50,51 and tremelimumab52,53) and 12 were combinatorial therapies (nivolumab + RT, 54 pembrolizumab + AT, 55 pembrolizumab + CT,56–61 pembrolizumab + RT,62,63 atezolizumab + AT,64,65 atezolizumab + CT,66–70 atezolizumab + CT + AT (atezolizumab + CAT), 71 avelumab + AT, 72 durvalumab + CT, 73 ipilimumab + CT,74–80 nivolumab + ipilimumab,8–10,81–90 and durvalumab + tremelimumab91–95). The baseline characteristics of the included trials are shown in Table 1. A total of 46 studies (68.7%) were phase III trials, and 64 (95.5%) were multinational trials. Cancer types assessed in the trials included lung (n = 30), melanoma (n = 10), gastric and esophageal (n = 8), head and neck (n = 6), renal cell (n = 5), urothelial (n = 3), prostate (n = 2), breast (n = 1), endometrial (n = 1), and malignant mesothelioma (n = 1). The mean sample size for toxicity analysis was 515 participants (range, 36–1274). The mean age was 62.3 years (range, 55.5–69.5 years). The median follow-up time was 13.9 months (range, 5.1–57.7 months).

Literature search and selection.
Characteristics of included trials.
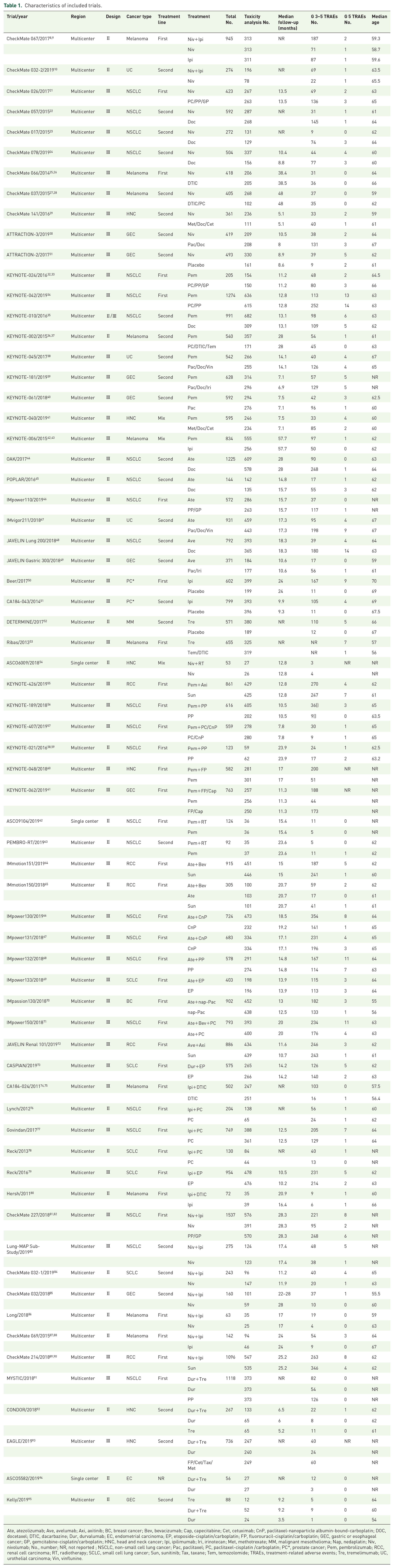
Ate, atezolizumab; Ave, avelumab; Axi, axitinib; BC, breast cancer; Bev, bevacizumab; Cap, capecitabine; Cet, cetuximab; CnP, paclitaxel-nanoparticle albumin-bound-carboplatin; DOC, docetaxel; DTIC, dacarbazine; Dur, durvalumab; EC, endometrial carcinoma; EP, etoposide-cisplatin/carboplatin; FP, fluorouracil-cisplatin/carboplatin; GEC, gastric or esophageal cancer; GP, gemcitabine-cisplatin/carboplatin; HNC, head and neck cancer; Ipi, ipilimumab; Iri, irinotecan; Met, methotrexate; MM, malignant mesothelioma; Nap, nedaplatin; Niv, nivolumab; No., number; NR, not reported ; NSCLC, non-small cell lung cancer; Pac, paclitaxel; PC, paclitaxel-cisplatin /carboplatin; PC*, prostate cancer; Pem, pembrolizumab; RCC, renal cell carcinoma; RT, radiotherapy; SCLC, small cell lung cancer; Sun, sunitinib; Tax, taxane; Tem, temozolomide; TRAEs, treatment-related adverse events; Tre, tremelimumab; UC, urothelial carcinoma; Vin, vinflunine.
Assessment of included trials
The risks of bias for the included RCTs are summarized in Supplemental Figure S1. Overall, the risk of bias across studies was relatively low; 12 RCTs were rated with a high risk of bias.22–24,35,42–45,48,55,72,86,92 The funnel plot analysis did not indicate any evident risk of publication bias for grade 5 TRAEs, but it did suggest a probability of publication bias for grade 3–5 TRAEs (Supplemental Figure S2).
Incidence of grade 3–5 and grade 5 TRAEs
The overall incidence of grade 3–5 and grade 5 TRAEs were 34.4% (12,297 of 35,778 patients from 66 studies) and 1.0% (352 of 34,288 patients from 63 studies), respectively, and, for patients receiving ICIs, the incidence rates were 30.5% (6,793 of 22,256 patients) and 1.1% (221 of 20,946 patients) for grade 3–5 and grade 5 TRAEs, respectively. Further analysis revealed that, with monotherapy, the incidence of grade 3–5 and grade 5 TRAEs were 17.9% (2220 of 12,373 patients from 47 studies) and 0.8% (98 of 11,875 patients from 44 studies), respectively, and combinatorial therapy resulted in 46.3% (4573 of 9883 from 39 studies) and 1.4% (123 of 9071 from 36 studies), respectively.
The causes of the grade 5 TRAEs are presented in Supplemental Table S3. Of the 98 cases of grade 5 TRAEs that occurred in the monotherapy cohort, the leading causes were respiratory (n = 36; 36.7%), gastroenteropancreatic (n = 10; 10.2%), and cardiovascular (n = 9; 9.2%) diseases. Of the 123 cases in the combinatorial treatment cohort, the leading causes were respiratory (n = 26; 21.1%), cardiovascular (n = 10; 8.1%), and infectious (n = 10; 8.1%) diseases. Pneumonitis was the most common cause of grade 5 TRAEs in patients receiving either monotherapy (16 out of 98; 16.3%) or combinatorial therapy (14 out of 123; 11.4%).
Conventional pairwise meta-analysis
The results of the pairwise meta-analysis are shown in Table 2. In terms of grade 3–5 TRAEs, monotherapies, including atezolizumab (OR = 0.25, 95% CI: 0.21–0.29), avelumab (OR = 0.14, 95% CI: 0.10–0.19), durvalumab (OR = 0.34, 95% CI: 0.25–0.45), nivolumab (OR = 0.21, 95% CI: 0.13–0.34), and pembrolizumab (OR = 0.27, 95% CI: 0.20–0.36), and the combination of durvalumab + tremelimumab (OR = 0.57, 95% CI: 0.47–0.74) were safer than CT. In addition, ICIs in combination with CT, including atezolizumab + CT (OR = 1.59, 95% CI: 1.37–1.84), ipilimumab + CT (OR = 2.24, 95% CI: 1.13–4.47), and pembrolizumab + CT (OR = 1.89, 95% CI: 1.15–3.09) were more toxic than CT alone. The durvalumab + tremelimumab combination was more toxic than durvalumab monotherapy (OR = 1.76, 95% CI: 1.33–2.34), the nivolumab + ipilimumab combination was more toxic than ipilimumab monotherapy (OR = 4.04, 95% CI: 2.96–5.51) and nivolumab monotherapy (OR = 2.69, 95% CI: 1.69–4.28), and the pembrolizumab + CT combination was more toxic than pembrolizumab monotherapy (OR = 12.57, 95% CI: 9.40–16.80). Atezolizumab and avelumab caused less grade 5 TRAEs than CT alone (OR = 0.38, 95% CI: 0.15–0.98 and OR = 0.26, 95% CI: 0.09–0.76, respectively); the nivolumab + ipilimumab combination caused more grade 5 TRAEs than nivolumab monotherapy (OR = 2.64, 95% CI: 1.13–6.14). Obvious heterogeneity was observed for grade 3–5 TRAEs in avelumab versus CT, nivolumab versus CT, pembrolizumab versus CT, durvalumab versus tremelimumab, ipilimumab + CT versus CT, pembrolizumab + CT versus CT, nivolumab + ipilimumab versus nivolumab monotherapy, and durvalumab + tremelimumab versus tremelimumab monotherapy (I2 = 56–90%). No heterogeneity was observed for grade 5 TRAEs in all comparisons, except atezolizumab + AT versus AT (I2 = 51%).
Results of direct comparison meta-analysis.

Significant results are in bold.
AT, antiangiogenic therapy; Ate, atezolizumab; Ave, avelumab; CI, confidence interval; CT, chemotherapy; Dur, durvalumab; E/C, experimental/control; Ipi, ipilimumab; Niv, nivolumab; No., number; OR, odds ratio; Pem, pembrolizumab; TRAEs, treatment-related adverse events; Tre, tremelimumab; RT, radiotherapy.
Network meta-analysis
Figure 2 shows the network of eligible comparisons for grade 3–5 and grade 5 TRAEs. Results of the network meta-analysis are presented in Figure 3. In terms of grade 3–5 TRAEs, ICIs in combination with CT (atezolizumab + CAT, pembrolizumab + CT, ipilimumab + CT, and atezolizumab + CT) were more toxic than all monotherapies (pembrolizumab, nivolumab, durvalumab, atezolizumab, avelumab, ipilimumab, and tremelimumab); pembrolizumab + AT, avelumab + AT, and nivolumab + ipilimumab were more toxic than all ICI monotherapy regimens except tremelimumab and ipilimumab; durvalumab + CT and atezolizumab + AT were more toxic than atezolizumab, nivolumab, and avelumab; and durvalumab + tremelimumab was more toxic than durvalumab and avelumab. CT was more toxic than all ICIs when used as monotherapy (except tremelimumab), and pembrolizumab + RT. Pembrolizumab + CT and ipilimumab + CT were more toxic than CT. Among the combinatorial treatments, ICIs in combination with CT (except durvalumab + CT) were more toxic than dual ICI therapy (nivolumab + ipilimumab and durvalumab + tremelimumab) as well as ICI + RT (pembrolizumab + RT and nivolumab + RT). Moreover, pembrolizumab + AT and avelumab + AT were more toxic than pembrolizumab + RT and nivolumab + RT, respectively. Among ICIs used as monotherapies, tremelimumab was more toxic than avelumab. With regard to grade 5 TRAEs, atezolizumab + CAT, ipilimumab + CT, atezolizumab + CT, and nivolumab + ipilimumab showed higher risk of grade 5 TRAEs than nivolumab, atezolizumab, and avelumab; atezolizumab + CAT also had a higher risk of grade 5 TRAEs than pembrolizumab, CT, and pembrolizumab + AT; durvalumab + CT, pembrolizumab + CT, and CT alone were associated with a higher risk of grade 5 TRAEs than atezolizumab and avelumab. Tremelimumab was more toxic than the other ICIs when used as monotherapy, except durvalumab and ipilimumab; pembrolizumab was more toxic than atezolizumab and avelumab. All results mentioned above were statistically significant with the ORs and lower limits of 95% CIs greater than 1.

Network of eligible comparisons for the network meta-analysis. (A) Grade 3–5 TRAEs. (B) Grade 5 TRAEs.
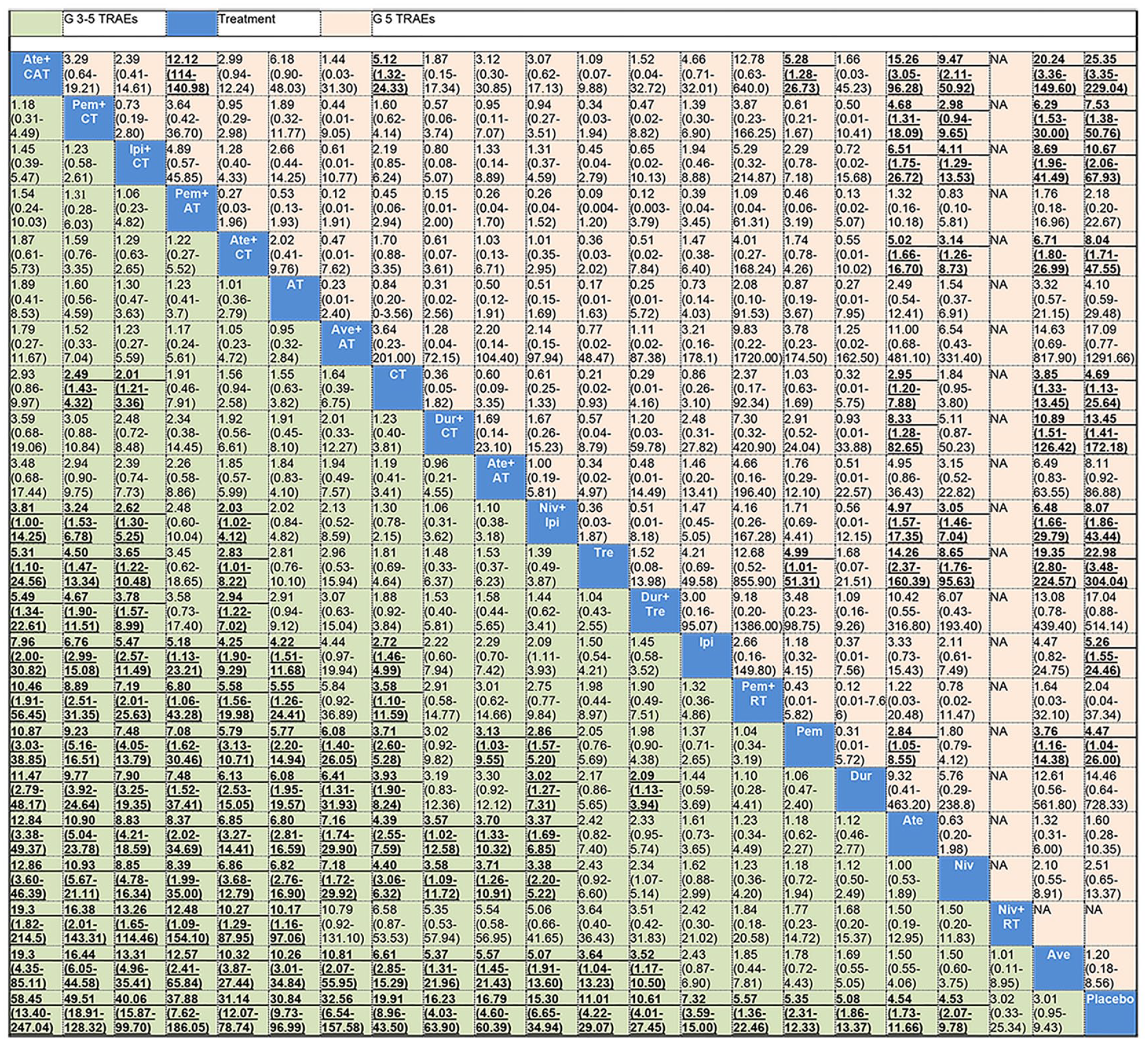
Treatments are reported in order of risk of grade 3–5 TRAEs ranking from high to low according to SUCRAs. Comparisons should be read from left to right. Data are ORs (95% CI) in the column-defining treatment compared with the row-defining treatment. An OR over 1 favors the row-defining treatment. Significant results are in bold and underlined.
Results of the toxicity ranking based on SUCRA are presented in Table 3, and ranking curves are shown in Supplemental Figure S3. Atezolizumab + CAT (91.2%) was ranked the most toxic treatment in terms of grade 3–5 TRAEs, followed by pembrolizumab + CT (90.9%), ipilimumab + CT (85.7%), pembrolizumab + AT(81.9%), and atezolizumab + CT (78.2%); avelumab (11.6%) was the least toxic treatment except placebo; and the nivolumab + RT combination was the least toxic combinatorial treatment. In terms of grade 5 TRAEs, atezolizumab + CAT (86.6%) was the most toxic treatment, followed by tremelimumab (84.5%), avelumab + AT (74.2%), durvalumab + CT (72.9%), and durvalumab + tremelimumab (72.2%); avelumab (10.6%) was also the least toxic treatment except placebo.
SUCRA values of grade 3–5 and grade 5 TRAEs for overall and sensitivity analysis.

AT, antiangiogenic therapy; Ate, atezolizumab; Ave, avelumab; CAT, CT+AT; CT, chemotherapy; Dur, durvalumab; Ipi, ipilimumab; Niv, nivolumab; Pem, pembrolizumab; RT, radiotherapy; SUCRA, surface under the cumulative ranking; TRAEs, treatment-related adverse events; Tre, tremelimumab; a, Niv(3 mg)+Ipi(1 mg); b, Niv(1 mg)+Ipi(3 mg); c, Pem(200 mg); d, Pem(2 mg/kg); e, Pem(10 mg/kg).
Transitivity, inconsistency, heterogeneity, and sensitivity analysis
Assessment of transitivity for grade 3–5 TRAEs indicated that the sample size, median age, and median follow-up times across treatment comparisons were relatively similar (Supplemental Figure S4). There were 13 independent closed loops with 32 comparisons in the network for grade 3–5 TRAEs, and 15 independent closed loops with 31 comparisons for grade 5 TRAEs. The design-by-treatment test for grade 3–5 TRAEs showed that there was no significantly global inconsistency (p = 0.102). However, tests of local inconsistency (loop-specific method and node-split model) showed that two of the loops (ipilimumab-nivolumab-placebo, p = 0.003; and pembrolizumab + CT-pembrolizumab-CT, p = 0.009) (Supplemental Table S4) and three of the comparisons (nivolumab + ipilimumab versus nivolumab, p = 0.017; nivolumab + ipilimumab versus ipilimumab monotherapy, p = 0.005; and ipilimumab versus placebo, p = 0.018) (Supplemental Table S5) were inconsistent. No significantly global (p = 0.976) or local inconsistencies (Supplemental Tables S4 and S5) were observed for grade 5 TRAEs.
The median heterogeneity, τ², were estimated at 0.29 (95% CI: 0.17–0.49) for grade 3–5 TRAEs, suggesting moderate heterogeneity; and 0.02 (95% CI: 0.01–0.23) for grade 5 TRAEs, suggesting low heterogeneity. The common heterogeneity standard deviation (SD) was 0.54 (95% CI: 0.41–0.70) for grade 3–5 TRAEs, and 0.14 (95% CI: 0.01–0.48) for grade 5 TRAEs. Subgroup meta-regression analyses for grade 3–5 TRAEs (Supplemental Table S6) revealed that the treatment choice and tumor type were the main sources of heterogeneity. Exclusion of patients receiving first-line therapy or including only patients with lung cancer resulted in 24.1% or 20.4%, respectively, relative reduction in heterogeneity SD. Sample size, control arm, and drug dose were also potential sources of heterogeneity. Excluding trials with a sample size <100 participants, or trials with a placebo-controlled design, or dividing treatments of nivolumab + ipilimumab into two dose groups resulted in 3.7%, 3.7%, or 5.6% relative reduction in heterogeneity SD, respectively.
Sensitivity analysis (Table 3) conducted by omitting trials with high risk of bias (n = 12), with sample size <100 (n = 6), or with placebo-controlled arms (n = 4) did not affect the main results of toxicity ranking substantially for both grade 3–5 and grade 5 TRAEs. Sensitivity analysis dividing treatments of nivolumab + ipilimumab into two dose groups or pembrolizumab into three dose groups resulted in slight changes in the ranking order of nivolumab + ipilimumab or pembrolizumab for either grade 3–5 or grade 5 TRAEs, without obvious changes in the ranking order of other treatments.
Subgroup analysis according to the type and severity grade 3–5 TRAEs
Results of the subgroup analyses are shown in Supplemental Tables S7–14. In term of grade 3–5 respiratory TRAEs, pembrolizumab was more toxic than CT. In terms of grade 3–5 gastroenteropancreatic TRAEs, atezolizumab + CAT, pembrolizumab + CT, ipilimumab + CT, atezolizumab + CT, pembrolizumab + AT, atezolizumab + AT, avelumab + AT, nivolumab + ipilimumab, ipilimumab monotherapy, pembrolizumab monotherapy, CT, and AT were more toxic than monotherapy with nivolumab, atezolizumab, or avelumab; atezolizumab + CAT, pembrolizumab + CT, ipilimumab + CT, atezolizumab + CT, nivolumab + ipilimumab, and CT were also more toxic than pembrolizumab monotherapy; atezolizumab + CAT, pembrolizumab + CT, and ipilimumab + CT were also more toxic than durvalumab + CT; the combination of ipilimumab + CT was also more toxic than atezolizumab + CT, nivolumab + ipilimumab, CT, ipilimumab monotherapy, atezolizumab + AT, and pembrolizumab + RT; atezolizumab + AT was more toxic than avelumab monotherapy; tremelimumab was also more toxic than monotherapy with avelumab or atezolizumab. As for grade 3–5 hepatic TRAEs, ipilimumab + CT and nivolumab + ipilimumab were more toxic than monotherapy with ipilimumab, pembrolizumab, nivolumab, avelumab, or CT; durvalumab + CT and atezolizumab + CT were more toxic than CT. Regarding grade 3–5 neurological TRAEs, atezolizumab + CT was more toxic than monotherapy with pembrolizumab, nivolumab, atezolizumab, or avelumab; CT was more toxic than monotherapy with pembrolizumab or atezolizumab. As for grade 3–5 endocrine TRAEs, durvalumab + CT, nivolumab + ipilimumab, pembrolizumab + CT, atezolizumab + CT, ipilimumab, and pembrolizumab monotherapy were more toxic than CT; nivolumab + ipilimumab and ipilimumab monotherapy were also more toxic than nivolumab monotherapy; pembrolizumab + AT was more toxic than AT. For grade 3–5 skin TRAEs, nivolumab + ipilimumab and ipilimumab + CT were more toxic than monotherapy with pembrolizumab, nivolumab, CT, and AT; ipilimumab monotherapy was also more toxic than CT. With regard to grade 3–5 hematological TRAEs, durvalumab + CT, atezolizumab + CT, pembrolizumab + CT, ipilimumab + CT, CT, and AT were more toxic than avelumab monotherapy; durvalumab + CT, atezolizumab + CT, ipilimumab + CT, and CT were also more toxic than monotherapy with nivolumab or pembrolizumab. All results mentioned above were statistically significant with the ORs and lower limits of 95% CIs greater than 1. No significant differences were observed in grade 3–5 renal TRAEs among all treatments.
The safety ranking based on SUCRA (Table 4) showed that pembrolizumab monotherapy, atezolizumab + CAT, durvalumab + CT, avelumab, nivolumab + ipilimumab, pembrolizumab + AT, atezolizumab + CT, and AT were ranked the most toxic regimens for respiratory, gastroenteropancreatic, hepatic, renal, skin, endocrine, neurological, and hematological grade 3–5 TRAEs, respectively.
SUCRA values according to type of grade3–5 TRAEs.

AT, antiangiogenic therapy; Ate, atezolizumab; Ave, avelumab; CT, chemotherapy; Dur, durvalumab; Ipi, ipilimumab; Niv, nivolumab; Pem, pembrolizumab; RT, radiotherapy; SUCRA, surface under the cumulative ranking; TRAEs, treatment-related adverse events; Tre, tremelimumab.
Discussion
To our knowledge, this is the largest and most comprehensive network meta-analysis conducted to assess the comparative safety of ICIs. Compared with the previous meta-analysis on this subject, our network meta-analysis included more recent studies, as well as the information reported in the predominant oncology congresses of 2019, more patients, and compared nearly all ICI-based treatments used in cancers. Moreover, this network meta-analysis focused on individual ICIs rather than ICI classes, selecting TRAEs instead of irAEs as the outcome of interest, and assessing the risk of grade 3–5 and grade 5 TRAEs separately. This network meta-analysis included 67 RCTs involving 36,422 patients and compared 19 ICIs. The incidence of grade 3–5 and grade 5 TRAEs were 17.9% and 0.8%, respectively, for monotherapy with an ICI, and were 46.3% and 1.4%, respectively, for combinatorial therapy. Pneumonitis was the most common cause of grade 5 TRAEs for patients receiving either monotherapy (16 out of 98; 16.3%) or combinatorial therapy (14 out of 123; 11.4%). Most of combinatorial treatments (ICI + CT, or AT, or another ICI) showed a significantly higher risk for grade 3–5 TRAEs than most of ICI-based monotherapy regimens. However, no significant differences were observed between several monotherapy regimens (tremelimumab, ipilimumab, durvalumab, and pembrolizumab) and combinatorial treatments in risk of grade 5 TRAEs, and tremelimumab was ranked the second-most toxic treatment among all treatments. Compared with grade 3–4 TRAEs, grade 5 TRAEs are uncommon. Individual clinical trials cannot characterize these rare toxic effects comprehensively, and the comparative risk of fatal TRAEs in ICI-based therapies is still not fully understood. Our findings suggested that although monotherapy was generally safer than a combinatorial treatment, a number of them seemed to be associated with an even higher risk of grade 5 TRAEs, which suggests that monitoring for adverse events is important.
Although CTLA-4 inhibitors are generally considered to be more toxic, and PD-L1 inhibitors are generally considered to be better tolerated because of their programmed cell death ligand-2-sparing ability that preserves the normal immunological homeostasis among ICIs used as monotherapy,3,5,96,97 the lack of head-to-head comparisons prevents us from making a firm conclusion. In a systematic analysis of the toxicity profile of PD-1 versus PD-L1 Inhibitors in non-small cell lung cancer, 98 patients treated with PD-1 inhibitors had an increased rate of irAEs (16% versus 11%, p = 0.07) and pneumonitis (4% versus 2%, p = 0.01) compared with patients who received PD-L1 inhibitors. However, in our network meta-analysis, no significant differences in the risk of grade 3–5 TRAEs were observed between PD-1 and PD-L1 inhibitors. Tremelimumab showed a significantly higher risk of grade 3–5 TRAEs than avelumab. The toxicity of ICIs as monotherapy, in terms of grade 3–5 TRAEs ranked from high to low was: tremelimumab, ipilimumab, pembrolizumab, durvalumab, atezolizumab, nivolumab, and avelumab. In terms of grade 5 TRAEs, tremelimumab was more toxic than other ICIs except durvalumab and ipilimumab; and pembrolizumab was more toxic than atezolizumab and avelumab. The toxicity ranking of ICIs as monotherapy based on the risk of grade 5 TRAEs from high to low was: tremelimumab, durvalumab, ipilimumab, pembrolizumab, nivolumab, atezolizumab, and avelumab. These results suggested that tremelimumab and avelumab seemed to be the most and least toxic ICIs monotherapy, respectively, and that different ICIs in the same class might be related to different risks of serious TRAEs.
To date, few trials have directly compared the safety between ICI-based combinatorial treatments. In their network meta-analysis, Xu et al. concluded no significant difference was observed in the risk of all-grade and grade 3–5 TRAEs between the combination of two ICIs and one ICI with conventional therapy. 6 In our network meta-analysis, 12 combinatorial treatments were compared. There were no significant differences in either the risk of grade 3–5 or grade 5 TRAEs among combinatorial treatments with CT or AT, while two ICIs (durvalumab + tremelimumab or nivolumab + ipilimumab) showed lower risk of grade 3–5 TRAEs than ICIs in combination with CT (except durvalumab + CT). Based on toxicity rankings, atezolizumab + CAT, pembrolizumab + CT, and ipilimumab + CT were ranked the most, second-most, and third-most toxic regimens in term of grade 3–5 TRAEs, respectively. Moreover, we found that the comparative risk of grade 3–5 TRAEs for ICIs based treatments varied depending on the nature and degree of severity TRAEs. Pembrolizumab, atezolizumab + CAT, durvalumab + CT, avelumab, nivolumab + ipilimumab, pembrolizumab + AT, atezolizumab + CT, and durvalumab + CT were ranked the most toxic treatments in risk of respiratory, gastroenteropancreatic, hepatic, renal, skin, endocrine, neurological, and hematological grade 3–5 TRAEs, respectively. These findings will be helpful for physicians to tailor an ICI-based therapy strategy for patients with different clinical backgrounds. For example, although the overall risk of grade 3–5 TRAEs for pembrolizumab and avelumab monotherapy were lower than combinatorial treatments, they seemed to have the highest risk of respiratory and renal grade 3–5 TRAEs in our study respectively, and should be used with caution in patients with chronic lung or kidney diseases.
Several recent clinical trials have evaluated combinations of ICIs with RT in cancers.54,62,63,99 The available data suggests that the combination has significantly improved survival compared with ICIs or RT alone. However, it is still not clear if combining ICIs with RT will increase the risk of TRAEs. In the present network meta-analysis, the risk of grade 3–5 TRAEs for pembrolizumab + RT or nivolumab + RT was similar to ICI monotherapy and was lower than other combinatorial treatments. Of note, current trials only represent a small fraction of the potential therapeutic combinations of ICIs with RT. Some factors such as treatment schedules of ICIs plus RT (concurrent or sequential), RT technique (SBRT or conventional RT), anatomic location irradiated (internal organs, bone, or brain), interval between treatments, and type of ICI used might affect the outcomes. Further clinical studies are needed to address these issues.
Some limitations of our network meta-analysis should be stated. First, heterogeneity was observed in the results of grade 3–5 TRAEs. Subgroup meta-regression analyses revealed that trials with a sample size <100 patients, cancer type, treatment line, and drug dose were potential sources of heterogeneity. However, sensitivity analysis showed that the main results for both grade 3–5 and grade 5 TRAEs were not markedly altered when removing trials of high risk of bias, sample size <100, or placebo-controlled, or dividing treatments of nivolumab + ipilimumab and pembrolizumab into different dose groups. Second, some trials reported TRAEs without the necessary details, and excluded reporting on TRAEs which occurred underneath a certain threshold (for example 1% or 5%). The missing information might result in bias. Moreover, different CT regimens and schedules used in individual trials might also lead to heterogeneity. Third, some of the newer data were extracted from recent conference abstracts. This could lead to a selection bias because the comprehensive toxicity data might be reported in the full publication. Fourth, TRAES refer to those adverse events which occur during the treatment, while irAEs mean those which have a putative immunological basis, and irAEs/TRAEs incidence might differ from each other. We selected TRAEs instead of irAEs as the outcome of interest in this study because TRAEs are more suitable for identifying and describing the safety profiles of chemo-immunotherapy combinations. However, not using the irAEs profiles might result in missing/overlooking the true nature of the monotherapy safety profile (at least for clinical practice). Finally, the network meta-analysis was conducted based on results reported from trials rather than individual patient data, and they were based on indirect comparisons but not direct comparisons. Thus, interpretation of the network meta-analysis results and drawing conclusions should be done with caution.
Conclusion
Compared with ICI-based combinatorial therapy, monotherapy with an ICI had a lower risk of grade 3–5 TRAEs, but some of them resulted in an even higher risk of fatal TRAEs. Some ICIs combined with CT seemed to be more toxic than the combination with RT or combination of two ICIs. Atezolizumab + CAT seemed to be the most toxic and nivolumab + RT seemed to be the least toxic among the combinatorial treatments, and among the monotherapy regimens, tremelimumab and avelumab seemed to be the most and least toxic, respectively. The toxicity ranking of some treatments changed depending on the nature and degree of severity of grade 3–5 TRAEs.
Supplemental Material
Supplementary_File – Supplemental material for Comparative risk of serious and fatal treatment-related adverse events caused by 19 immune checkpoint inhibitors used in cancer treatment: a network meta-analysis
Supplemental material, Supplementary_File for Comparative risk of serious and fatal treatment-related adverse events caused by 19 immune checkpoint inhibitors used in cancer treatment: a network meta-analysis by Tingting Liu, Bo Jin, Jun Chen, Hui Wang, Shuiyu Lin, Jun Dang and Guang Li in Therapeutic Advances in Medical Oncology
Footnotes
Author contributions
DJ contributed to the conception and design, data interpretation, and statistical analysis. LT and JB contributed to data acquisition, data interpretation, and statistical analysis and drafting of the manuscript. CJ, WH, LS, and LG contributed to data acquisition, data interpretation, and drafting of the manuscript. All authors read and approved the final manuscript.
Conflict of interest statement
The authors declare that there is no conflict of interest.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
