Abstract
Background
Emerging evidence suggests preoperative opioid use may increase the risk of negative outcomes following orthopedic procedures. This systematic review evaluated the impact of preoperative opioid use in patients undergoing shoulder surgery with respect to preoperative clinical outcomes, postoperative complications, and postoperative dependence on opioids.
Methods
EMBASE, MEDLINE, CENTRAL, and CINAHL were searched from inception to April, 2021 for studies reporting preoperative opioid use and its effect on postoperative outcomes or opioid use. The search, data extraction and methodologic assessment were performed in duplicate for all included studies.
Results
Twenty-one studies with a total of 257,301 patients were included in the final synthesis. Of which, 17 were level III evidence. Of those, 51.5% of the patients reported pre-operative opioid use. Fourteen studies (66.7%) reported a higher likelihood of opioid use at follow-up among those used opioids preoperatively compared to preoperative opioid-naïve patients. Eight studies (38.1%) showed lower functional measurements and range of motion in opioid group compared to the non-opioid group post-operatively.
Conclusion
Preoperative opioid use in patients undergoing shoulder surgeries is associated with lower functional scores and post-operative range of motion. Most concerning is preoperative opioid use may predict increased post-operative opioid requirements and potential for misuse in patients.
Level of evidence
Level IV, Systematic review.
Introduction
The opioid crisis is a major public health issue that has resulted in widespread overdose and addiction with recent estimates suggesting that no less than 289 million opioid prescriptions are filled yearly in the United States. 1 Recent studies suggest that at least 1.9 million Americans have developed opioid use disorder,2,3 and at least 530 people die weekly from opioid overdose. 4 Over 50% of opioid-related deaths occur despite acceptable prescription of the medications with respect to medical board guidelines. 5 Additionally, complications arising from opioid misuse and overuse result in significant healthcare expenses, estimated at an annual cost of $78.5 billion in US. 6
Optimal pain control for patients with shoulder disorders or following surgical intervention is an area of ongoing research. 7 Current practices of orthopedic surgeons are highly variable and opioids are commonly relied upon or prescribed without individualizing the needs of patients. 8 As many patients expect to be pain-free postoperatively and satisfaction of treatment is associated with such an expectation, orthopedic surgeons have been keen to achieve this goal, resulting in overreliance on discharge opioid prescriptions. This is reflected in the fact that orthopedic surgeons file 7.7% of all US opioid prescriptions, representing the third-largest provider of opioids among clinicians.9,10
Opioid medications have traditionally been widely prescribed as a non-operative management of chronic joint pain. However, emerging evidence has shown that preoperative opioid use is associated with an increased risk of negative outcomes and increased postoperative demand for opioids following total joint arthroplasties.11,12 As such the utility of preoperative opioid use in such patients has come under significant scrutiny.11,13,14 Preoperative opioid use has been shown to be associated with increased readmission rates and risk of early revision among patients undergoing total knee or hip arthroplasty. 12 Although increased revision rates and readmission were also evident in patients undergoing shoulder arthroplasty and rotator cuff repair,15,16 the effects of preoperative opioid use on revision surgery, readmission, and costs after shoulder surgeries are mixed. Some studies show no link between preoperative opioid use and complications, increased duration of stay, or readmission rates following shoulder arthroplasty.17,18
The objective of this systematic review is to evaluate currently available evidence on the association between preoperative opioid use in patients undergoing shoulder surgery with respect to perioperative clinical outcomes, postoperative complications, and postoperative dependence on opioids.
Materials and methods
The study was conducted according to the Cochrane Handbook for Systematic Reviews 19 and reported as per the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. 20
Search strategy
EMBASE, MEDLINE, PubMed, Cochrane Central Register of Controlled Trials (CENTRAL), and Cumulative Index to Nursing and Allied Health Literature (CINAHL) database were searched from date of inception to April 15th, 2021.
The search strategy, adapted to each database, included terms representing preoperative opioid use and its association with postoperative outcomes or opioid use. MeSH and EMTREE terms were used, along with free text, in several combinations to increase search sensitivity. We consulted with experts in the field, manually reviewed the reference lists of articles that fulfilled the eligibility criteria and used the “related articles” feature in PubMed. The search strategy was adapted in PubMed to search for articles published online ahead of print (Appendix 1).
Eligibility criteria
In order to maximize potentially eligible data, no restrictions was made on publication date or follow-up. The criteria for inclusion were: (1) Studies on shoulder arthroplasty or scope procedures evaluating preoperative use of opioids; (2) Adult patients (3) Studies that reported at least one outcome related to shoulder arthroplasty or scope procedures; (4) Studies focused on postoperative opioid use; (5) any randomized or non-randomized studies were included.
The exclusion criteria were: (1) Studies that did not report on pre-operative opioid use; (2) Studies that included less than five patients; (3) Reviews and conference abstracts were excluded; (4) Studies without adequately reported functional outcomes or postoperative opioid use; (5) We excluded patients with functional pain syndromes. (6) Non-English language studies were excluded.
Study screening
Study selection was performed by two authors (OAM, CP) using Covidence (Covidence systematic review software, Veritas Health Innovation, Melbourne, Australia). The selection of studies was performed in a stepwise manner, first by title and abstract, then full-text review. A resolve-by-consensus strategy was utilized for all discrepancies. If consensus could not be reached, a third senior researcher (MK) was consulted. Manual screening of the references of included studies was done to identify additional articles which may have eluded the initial search strategy (Figure 1).
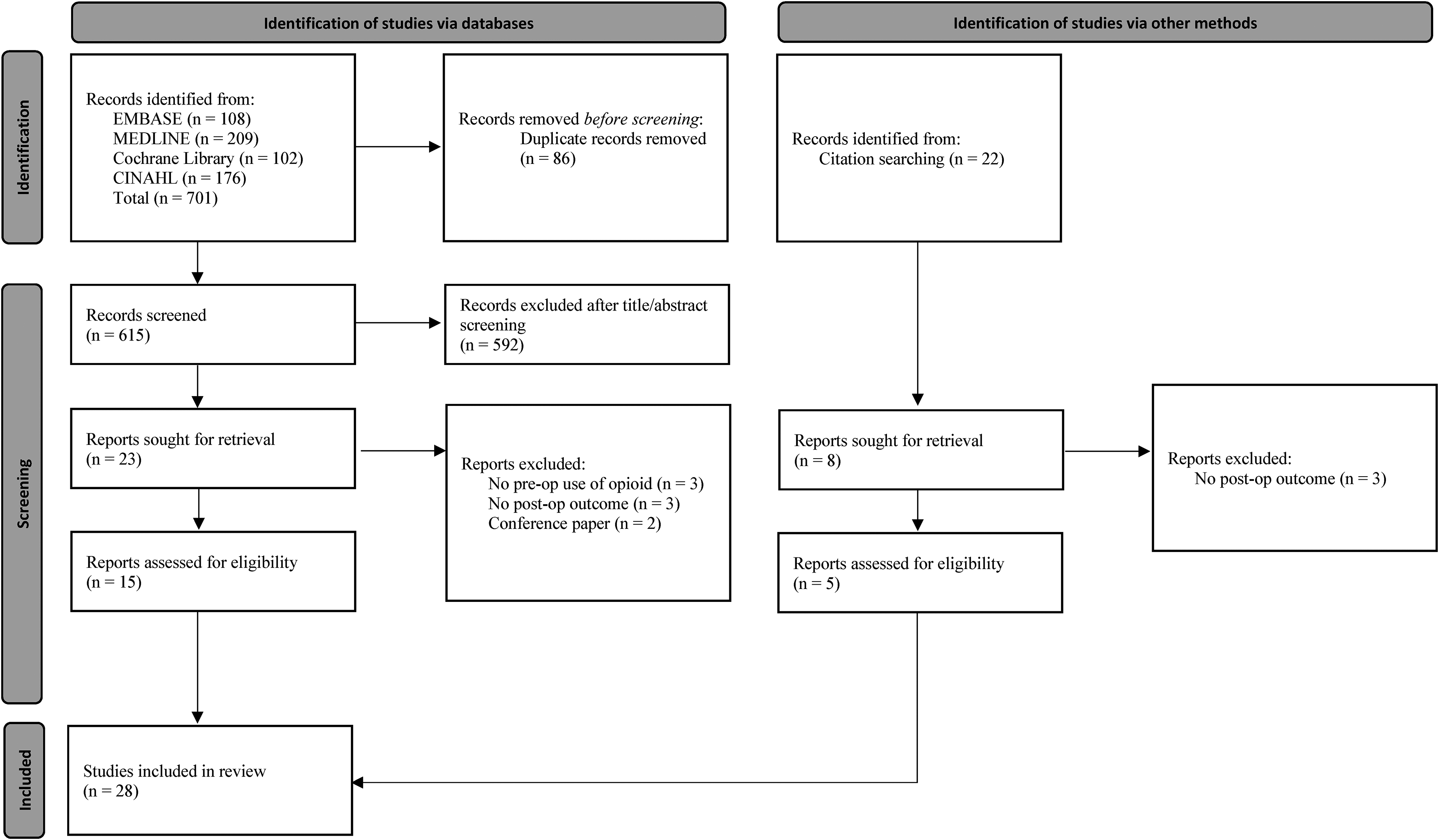
PRISMA flow diagram.
Extraction of data
Data were extracted by two reviewers (OAM, CP) independently from each other into a collaborative pre-defined data abstraction web-based spreadsheet (Google Sheets, 2021. California, United States: Google LLC.). To ensure accuracy, the results were audited by both reviewers (OAM, CP) and reviewed by the principal investigator (MK).
Extracted data included information on basic study characteristics (authors, publication year, country, journal of publication, study type), demographic data (age, sex, sample size, diagnosis, intervention type), preoperative opioid use, period of follow-up, study outcomes, and complications. The authors of included studies were contacted if there were any uncertainties regarding the data.
Risk of bias and quality assessment
The Methodological Index for Non-Randomized Studies (MINORS) was used by two independent reviewers (OAM, CP) to assess risk of bias in the included studies. 21 The MINORS scale assigns a score of 0, 1, or 2 for a list of 8 and 12 questions in non-comparative, and comparative studies, respectively.
Statistical analysis
Descriptive statistics were calculated to reflect the frequency and percentage of abstracted study data. Using Cohen's Kappa (κ), inter-reviewer agreement at each stage of the screening process was calculated. Agreement was categorized a priori, as per Landis and Koch, 22 with k of 0.81 to 1.0 for near perfect agreement; k of 0.61 to 0.80 for substantial agreement; k of 0.41 to 0.60 for moderate agreement; and k of 0.21 to 0.40 as fair agreement. Interobserver agreement for methodologic quality assessment was calculated using the intraclass correlation coefficient (ICC); a value of ≥0.65 was considered adequate. 23
Results
Study characteristics
The search strategy retrieved 701 studies, of which 28 were identified to undergo full-text review. Twenty-one studies which met all of the inclusion criteria and were included in the final qualitative synthesis (Figure 1).15–18,24–40 There was substantial agreement for both title and abstract screening (Cohen's kappa = 0.71) and full-text review (Cohen's kappa = 0.72).
There was a near perfect level of agreement among quality assessment scores using the MINORS criteria (ICC, 0.93). The mean MINORS score for the included studies was 12 ± 0.7 out of 16 for non-comparative studies and 19.9 ± 1.3 out of 24 for comparative studies. Characteristics of included studies can be found in Table 1.
Characteristics of included studies.
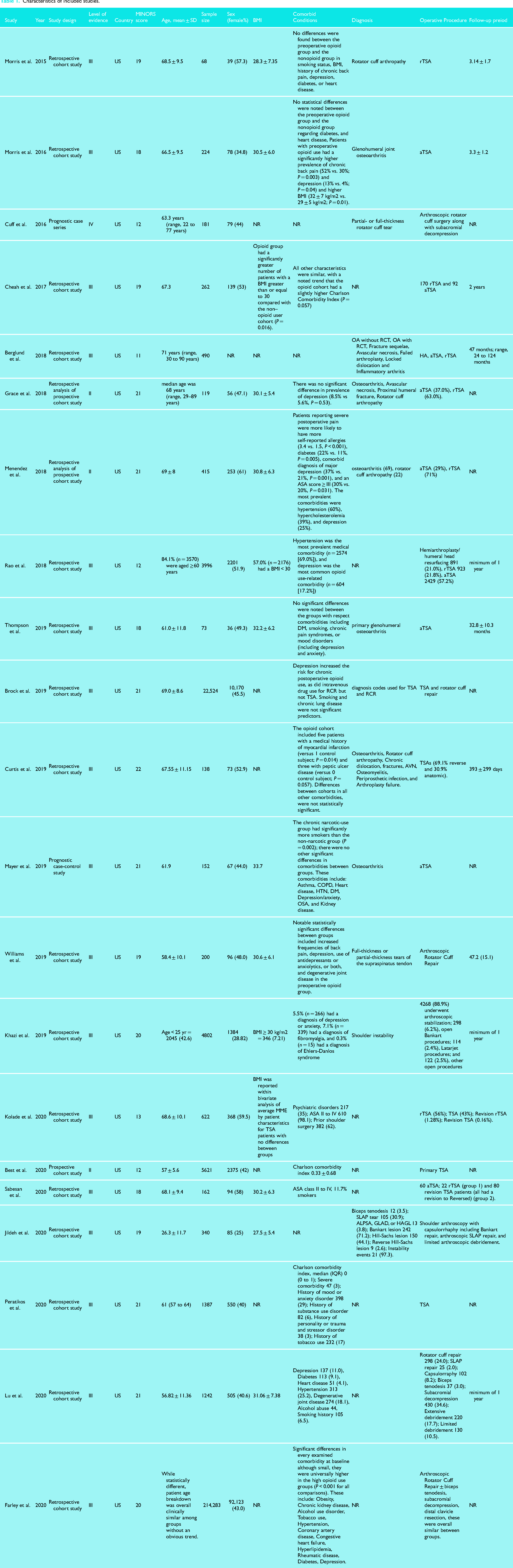
The included studies were conducted between 2015 and 2020, with 17 (81.9%) studies published within 3 years of the search. Three of the studies were of level II evidence (n = 6155),17,30,34 one was level IV evidence (n = 181) and 38 17 were level III evidence, (n = 250,965). All of the included studies were performed in the United States.
This review includes a total of 257,301 patients. The median sample size was 378 participants (interquartile range: 167 to 2692). Of those, 110,771 (43.1%) were female (range: 39 to 92,123). The median age of the included participants was 66.9 (range: 22 to 90). Shoulder arthroplasty was evaluated in 14 studies, while shoulder arthroscopy was assessed in 6 studies. Brock et al. reported on outcomes of both types of procedures. 27 The follow-up was reported in 10 studies, with a mean of 2.3 years. Regarding body mass index (BMI), the median was 30.5 kg/m2 (range: 27.5 to 32.2).
Diagnosis
Partial- or full-thickness rotator cuff tears (RCTs), glenohumeral joint osteoarthritis with and without RCT, fracture sequelae, avascular necrosis (AVN), locked dislocation, inflammatory arthritis, osteomyelitis, and periprosthetic infection were reported pathology in the included studies. Seven studies did not report diagnosis of included patient populations.
Opioid use
Preoperative: Of the included studies, 51.5% (n = 132,524) of the patients reported pre-operative opioid use. Also, 8 studies reported the opioid types, and 10 studies reported doses expressed as Oral Morphine Equivalent (OME) (Table 2).
Preoperative opioid use.
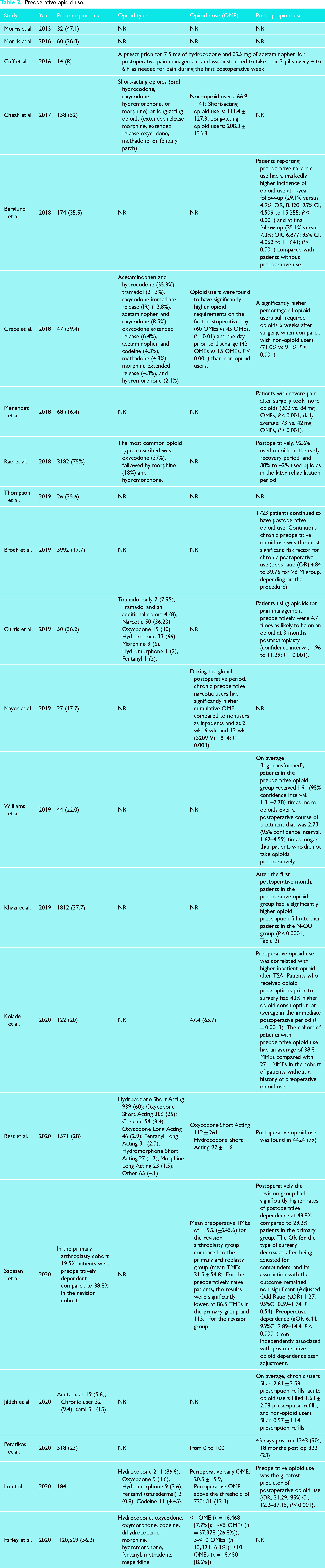
Postoperative: Fourteen studies (66.7%) reported a higher likelihood of opioid use at follow-up among those prescribed opioids preoperatively compared to preoperative opioid-naïve patients.
For instance, Grace et al. 17 reported that opioid users were found to have significantly higher opioid requirements on the first postoperative day (60 OMEs vs 45 OMEs, P = 0.01) and the day prior to discharge (42 OMEs vs 15 OMEs, P < 0.001), than non-opioid users. Curtis et al. 15 reported that patients using opioids for pain management preoperatively were 4.7 times as likely (95% CI 1.96 to 11.29; P = 0.001) to be on an opioid at 3 months post-arthroplasty. This was also found in a 1-year follow-up as per Berglund et al. in which patients reporting preoperative opioid use had a markedly higher incidence of opioid use (29.1% versus 4.9%; odds ratio, 8.320; P < 0.001). 40
Type of opioids
A wide variety of opioid medications were included, although they were reported in less than 50% of included studies. Cuff et al. 38 reported only postoperative opioid regimen as a prescription for 7.5 mg of hydrocodone and 325 mg of acetaminophen during the first postoperative week. On the other hand, 4 studies reported preoperative use of opioids which included acetaminophen and hydrocodone, tramadol, oxycodone immediate release, acetaminophen and oxycodone, oxycodone extended release, acetaminophen and codeine, methadone, morphine extended release, and hydromorphone.15,17,24,30
Comorbid conditions
In the majority of included studies reporting comorbidies, no statistical differences were noted between the preoperative opioid and non-opioid groups.15–17,29,36,37
However, Farley et al. 24 identified significant differences in every examined comorbidity at baseline as they were universally higher in the high opioid use groups (P < 0.001 for all comparisons). Two studies linked between preoperative opioid use and prevalence of one of the following comorbidities: chronic back pain, depression, obesity, self-reported allergies and an ASA score ≥ III.27,34 Three studies did not report comorbid conditions.28,38,40
Pain reporting, functional scores and range of motion (ROM)
Pain reporting and functional assessment scores were reported in eight studies (38.1%). The American Shoulder and Elbow Surgeons (ASES) score was the most commonly used (8 studies) followed by Visual Analogue Scale (VAS) for pain which was reported in 6 studies. Four studies assessed ROM at final follow up (Table 3).
Pain reporting, functional scores and range of motion.
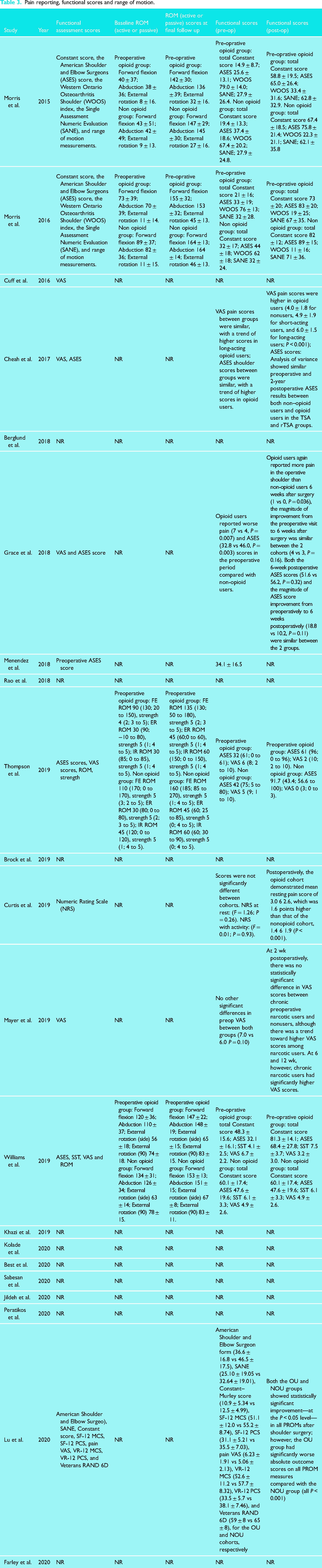
Grace et al. 17 reported that opioid users had worse VAS (7 vs 4, P = 0.007) and ASES (32.8 vs 46.0, P = 0.003) in the preoperative period compared with non-opioid users. Morris et al. 37 found that the non-opioid group had significantly greater preoperative forward flexion (average 16° greater; P = 0.005) and abduction (average 12° greater; P = 0.03). Although both groups significantly improved on ROM measurements from preoperative to most recent follow-up (P < 0.001), the opioid group demonstrated significantly lower ROM measurements, except for external rotation (P = 0.58), compared to the non-opioid group post-operatively.
Complications and revision surgery
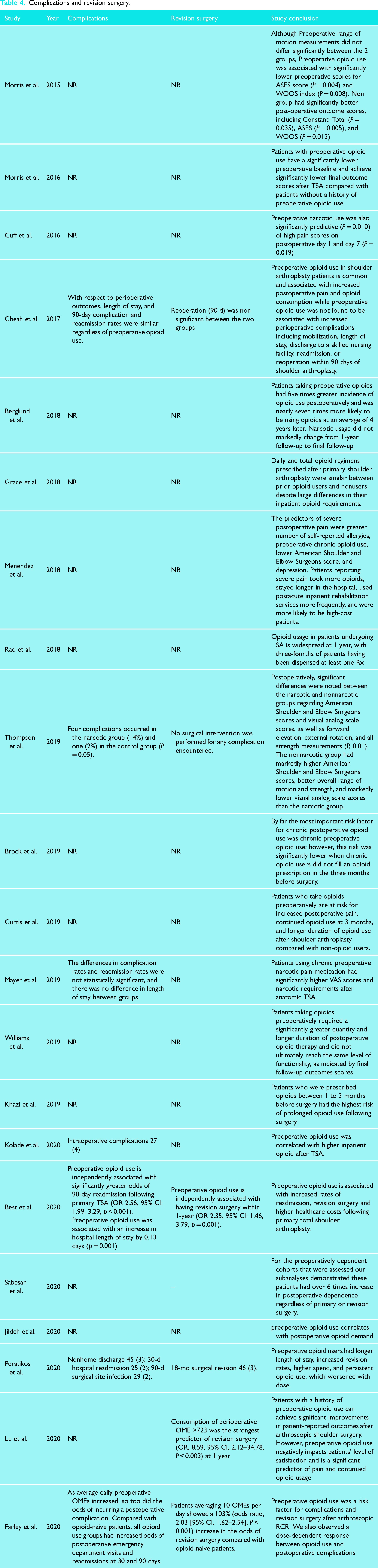
Complications reported among included studies were of heterogeneous conclusion. Best et al. found that preoperative opioid use is independently associated with significantly greater odds of 90-day readmission following primary TSA (OR 2.56, 95% CI: 1.99, 3.29, p < 0.001) and with an increase in hospital length of stay of 0.13 days (p = 0.001). 30 On the other hand, Mayer et al. 18 found that the differences in complication rates and readmission rates were not statistically significant, and no difference in length of stay between both groups was seen.
Again, Best et al. 30 reported preoperative opioid use is independently associated with having revision surgery within 1-year (OR 2.35, 95% CI: 1.46, 3.79, p = 0.001), which is consistent with the report of Peratikos et al. who showed an 18-month surgical revision of 3% in the opioid group. 26 (Table 4).
Complications and revision surgery.
Discussion
The association between preoperative opioid use and clinical outcomes is complex. The primary finding of this review is that the preoperative use of opioids is associated with inferior clinical outcomes and increased postoperative opioid use in patients undergoing shoulder surgeries.
It has been proposed that preoperative opioid use in orthopedic surgery increases the risk of chronic opioid use, thereby contributing to the ongoing “opioid crisis” in North America. 41 Indeed, opioid use has become a central focus of orthopedic research in recent years. 42 Preoperative opioid use has been identified as a predictor of prolonged postoperative use after many orthopedic procedures.43,44 Bartels et al. 45 and Kim et al. 46 identified multiple predictors of long-term opioid use during follow-up such as high in-hospital opioid use, procedure type, anesthesia type, age, and insurance type.
One of the problems that exists when analyzing the literature in this topic, is the lack of standardization of the definition of “chronic opioid use” leading to a wide variety in terminology used and outcome reporting suggesting the need of standardization. 47 Nevertheless, we noted that there is a higher likelihood of ongoing opioid use at follow-up among those prescribed opioids preoperatively compared to preoperative opioid-naïve patients. Most of the studies included in this review report that those patients given opioids prior to their shoulder surgery were more likely to continue using opioids after surgery and reported higher pain scores and lower functional outcomes. Opioid stewardship is very important as it seems likely that preoperative opioid use leads to opioid tolerance and a diminished analgesic effect which ultimately leads to worse postoperative pain and greater opioid consumption.48,49
Although our study suggests that prescribing patients an opioid before surgery is associated with ongoing long-term opioid use, we cannot exclude the possibility that this is an artifact arising from underlying patient characteristics (e.g. patients with chronic pain conditions or psychiatric disorders).50–53 In a large retrospective study involving 29,827 arthroscopic rotator cuff repair patients, Westermann et al. 54 found that those patients prescribed opioids preoperatively were more than 7 times more likely to continue using opioids after discharge. Other factors (e.g. psychiatric conditions and lower back pain) were also identified as contributing to ongoing opioid use. Although most of the studies showed no statistical differences were noted between the preoperative opioid and non-opioid groups regarding comorbidities, it is possible that the worst outcomes associated with preoperative use of opioids might be linked with certain comorbidities and/or the presence of chronic pain in this population, with the subsequent impact on clinical outcomes. However, there is an urgent need for standardized, evidence-based postoperative opioid prescribing protocols, 55 as well as the development of strategies to reduce prolonged opioid use following surgery that consider a multimodal analgesic approach. 56 This can be achieved by identifying patients preoperatively and try to use strategies to decrease their preoperative opioid use. 57
Goplen et al. 43 reported that total joint arthroplasty patients that received opioids preoperatively have worse overall pain and function than opioid-naïve patients. This was also found in patients undergoing ACL reconstruction, where the preoperative opioid group scored more poorly in patient-reported outcomes (at baseline and 1-year follow-up) and were more likely to fail to reach a patient acceptable symptomatic state. 58 Chronic opioid use before cervical arthrodesis has also been associated with worse functional outcomes following surgery. 59 In the context of shoulder surgery outcomes, most of the studies found that patients with preoperative opioid use had poor functional scores throughout the postoperative period. However, it is noteworthy that the preoperative opioid group tended to start with lower functional scores, so that the magnitudes of improvement did not differ greatly when comparing the preoperative opioid and non-preoperative opioid groups.18,26,30 In a subsequent work, Cozowicz et al. found that those patients with the most opioid prescriptions were at increased risk of treatment complications. 60 Although this review was carefully designed to focus on functional outcomes, these data were missing from many of the included studies. Nevertheless, these results highlight important points regarding functional outcomes and ROM in patients undergoing shoulder surgeries, which develops earlier work questioning the benefit of prescribing opioids preoperatively to orthopedic surgery patients.
Recently, there has been a trend towards the use of non-opioid pain regimens favoring multimodal analgesia schemes. In fact, opioids are no longer a part of standard procedures in the treatment of athletes,61,62 and have been proposed as the second or third-line pharmacological option for the management of chronic painful joint conditions such as osteoarthritis.63,64 Multimodal analgesia can improve pain control and lessen reliance on opioids.57,65 Also, it was recently reported that a multimodal pain protocol could improve recovery (patient-reported) following arthroscopic shoulder surgery, with reduced opioid use relative to a conventional opioid-receiving group. 66 Despite the importance that multimodal analgesia schemes might have in decreasing postoperative opioid use, future studies should ideally have as their key measure the improvements in patient-related outcomes instead of decreased opioid usage. 67
Limitations
There are several limitations in this review. First, we could not establish causality between preoperative opioid use and its effects on the outcomes of shoulder surgeries. This is due to many confounders, such as chronic pain, which were not adequately addressed in included studies. Furthermore, the indications of the preoperative opioid use were not mentioned since these medications might be taken for other causes of pain such as back pain or cancer pain.
Also, this review lacked any level I type of evidence. Because of this, some groups may have been imbalanced concerning gender, severity of back pain, mood disorders, and other chronic pain conditions.
Second, our analyses were constrained by the availability of published data as most of the studies included in this review did not include data on patient-reported outcomes, ROM, or strength. This was due to the older studies lacking access to the big data registries currently available, and the absence of certain information which was probably omitted during the surgeon's routine follow-up assessments. This limits the applicability of our results when shoulder surgeons have their preoperative counseling with their patients who are chronic users of opioids.
Despite these limitations, our findings are consistent with those reported in other orthopedics studies.43,68–70 Nevertheless, further research is required to better understand the influence that preoperative opioids have on postoperative outcomes in shoulder surgery.
Taken together, our findings agree with the previous orthopedic literature regarding preoperative use of opioids. This work and prior studies have identified major associations with preoperative opioid use: inferior outcomes, greater ongoing opioid use, depression, anxiety, and psychiatric conditions. Collectively, these data are likely to help guide clinical and surgical decision-making when planning orthopedic patient care protocols. Even if those patients given opioids preoperative are likely to experience an equal magnitude of improvement as those not given opioids. Also, postoperative programs and pain management counseling should be considered to help patients achieve adequate analgesia, thereby reducing the opioid burden.
Conclusion
Our review suggests that in patients undergoing shoulder surgery, the preoperative use of opioids is associated with inferior clinical outcomes and increased postoperative opioid use and misuse. It is unclear to what degree this influence is due to the opioid use itself and to what extent it is related to comorbidities, severity of the preoperative condition leading to surgery, and/or chronic pain prevalence. Future prospective studies controlling for comorbidities, severity of the pathology and chronic pain, and OME are needed.
Supplemental Material
sj-docx-1-sel-10.1177_17585732211070193 - Supplemental material for The role of preoperative opioid use in shoulder surgery—A systematic review
Supplemental material, sj-docx-1-sel-10.1177_17585732211070193 for The role of preoperative opioid use in shoulder surgery—A systematic review by Omar A Al-Mohrej, Carlos Prada, Kim Madden, Harsha Shanthanna, Timothy Leroux, and Moin Khan in Shoulder & Elbow
Footnotes
Acknowledgements
None.
Contributorship
OAM: Study design, data analysis, processing, writing—original draft, and approval of final draft. CP: Data collection, processing and reviewing—original draft. KM: methodology reviewing—original draft and approval of final draft. HH: reviewing, editing and approval of final manuscript. LL: reviewing, editing and approval of final manuscript. MK: Data curation, methodology, validation, visualization, project administration, and approval of final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Ethical approval
Not applicable.
Informed Consent
Not applicable.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
