Abstract
Background:
Access to timely, accurate health-related information can protect migrants’ health during public health crises. However, unmet language needs, social alienation and mistrust were among the barriers that migrants faced in accessing official information about COVID-19 and recommended vaccines. This study aimed to explore information-seeking behaviour about COVID-19 vaccines among Eastern Mediterranean Region (EMRO) born migrants in Australia.
Methods:
With an explanatory mixed-method approach, we employed an online survey followed by semi-structured interviews. Survey and interviews were advertised through migrants-specific organisations' websites and social media posts, and Facebook advertisements. The survey collected data on socio-demographics, sources of information, preferred communication channels and information-gathering capacity from 300 individuals between September and November 2021. Seventeen adults participated in interviews between December 2021 and February 2022. The qualitative data were analysed using inductive thematic analysis.
Results:
The survey participants’ mean age was 41.4 ± 11.8 years and 52% were male. Around 70% reported that the Australian government was among their main sources of information, and 37% preferred receiving information via email or SMS. Around 70% agreed that they can easily access the information they need, feel included in government communications, and can distinguish between fake and good information. Around 60% agreed they could access information in their language, while approximately 50% of respondents indicated they had difficulty understanding vaccine information. Analysis of the interview transcripts revealed that the information sources used depended on their perceived need, their information-gathering capacity, ease of access and trust in sources. Lack of trust in official sources made it more difficult to accept uncertainty. Sources of information favoured included community networks and personal experience.
Conclusion:
To ensure equitable access to health information, health communications should be tailored to migrants’ specific needs, preferences and information-gathering capacity. Such communication should be practised in all aspects of health, not only during a public health crisis, to improve trust in official sources.
Introduction
Access to reliable and accurate health information is a core component of the right to health (1). There is no doubt that official sources should be the main source of health information. However, these sources may not always be accessible, acceptable, or meet people’s needs (2,3). This is especially highlighted where people with different cultural and linguistic backgrounds are the audiences for one-size-fits-all official health communication (4).
In multicultural societies, health communications routinely assume a one-size-fits-all approach in which disease-specific information is produced in the official language based on assumed generalisable information needs and information-gathering capacity (5,6). However, during a public health emergency, when there is a need for communal action to protect all of society, officials may implement strategies to make health information more accessible (7). One of the commonly used strategies is translating the information into different languages with the expectation that people access the information and take the recommended actions (7). The acceptability, and therefore effectiveness, of health messages is closely associated with trust (8). However, as observed during the COVID-19 pandemic in many multicultural societies, the sudden change from a one-size-fits-all approach to a more culturally and linguistically targeted official health communication may not necessarily make them a trusted source of information (10,11).
Australia is a multicultural society with 30% of its population born overseas and about a quarter speaking a language other than English at home (9). In Australia, health information is typically provided in English, in written form, and is disseminated digitally. This approach excludes some members of society from health communications (10,11). Collecting, analysing and using health information is more complex for migrants whose first language is not the official language of the destination country (12,13). Unmet language needs, the government’s reliance on digitally disseminated information, social alienation and mistrust of authorities were among the barriers migrants faced in accessing official information about COVID-19 and recommended vaccines (11).
In Australia, all migrant groups except those born in northwest Europe and Sub-Saharan Africa (mostly South Africa) had higher age-standardised death rates compared to the Australia-born population, with the highest rate observed among people born in North Africa and the Middle East (14). Part of this disparity can be attributed to the inequity in accessing timely, accurate information about COVID-19 and vaccines (15,16). With some delays, many initiatives in Australia targeted migrants to provide culturally and linguistically appropriate information (17). However, such initiatives have since been wound back, with effects on migrants’ ability to access information about booster doses and decide whether to accept booster doses.
To design strategies to ensure equitable access to health information in multicultural societies, it is important to understand migrants’ information-seeking behaviours and information-gathering capacity. This study aimed to explore information-seeking behaviour about COVID-19 vaccines among migrants in Australia to guide effective communications related to not only the COVID-19 vaccines but also other public health crises management and preparedness in a multicultural society.
Methods
The study population was migrants born in the Eastern Mediterranean Region (EMRO) living in Australia. EMRO includes countries in the Middle East, North Africa and South Asia. This population was selected for this study because these groups of migrants had the highest COVID-19-related age-standardised death rate, and the lead researcher has lived experience as a migrant from EMRO living in Australia during the COVID-19 pandemic.
We employed an explanatory mixed-method approach where the findings from the quantitative component were explained by the qualitative findings. In this study, we used an online survey followed by semi-structured interviews for data collection. Participants for the survey and interviews were recruited by advertising online, primarily posts on targeted communities' Facebook pages, Facebook advertising and social media posts, and websites of organisations that provide social and health services for migrants in Australia. These organisations included migrants and refugees-specific and community-specific organisations managed by prominent members of communities. At the end of the survey, we also invited participants to the interview and provided a link to the interview expression of interest form. The interview expression of interest form collected potential participants’ contact details and data on their country of birth and whether they identified as health professionals or were studying to become health professionals. In selecting participants for interview, we used a maximum variation approach. For this approach, we used data on country of birth and health profession background to include people born in different countries of the EMRO and prevent over-representation of people with health profession backgrounds. We did not collect any other socio-demographic data before or during the interview to protect participants’ privacy and encourage participation.
Quantitative data
The survey was available in English, and Arabic and Farsi languages, the two main languages spoken in the EMRO countries, and collected data on socio-demographics, sources of information about COVID-19 vaccines, preferred channels for receiving information about COVID-19 vaccines and vaccination programmes, and items related to information-gathering capacity. The data were collected between September and November 2021 and analysed descriptively using R Version 4.2.2.
Qualitative data
Semi-structured telephone interviews were carried out by DP between December 2021 and February 2022. Interviews were in English and lasted between 20 and 40 minutes. Participants were asked about the sources that they and the people around them used to learn about COVID-19 vaccines and their experiences with those sources. Audio recordings of the interviews were transcribed verbatim and analysed using inductive thematic analysis by PF and DP. In this article, participants are presented with a code that includes M for man or W for woman.
Integration of findings
We have integrated quantitative and qualitative findings in this article using narrative contiguous presentation. We have reported quantitative and qualitative findings in different subsections in the Results section and provided a mixed method integration section that reports the summary of integrated findings. In the Discussion section, the findings of the quantitative and qualitative parts are merged and discussed together (18).
Results
Quantitative findings
A total of 300 people participated in the survey. The participants’ ages ranged from 18 to 74 years (mean ± standard deviation (SD): 41.4 ± 11.8). Years lived in Australia ranged from <1 to 40 years (8.8 ± 6.6). Key demographic data is presented in Table 1. Around 37% reported email or SMS as their most preferred channels. Approximately 70% reported using Australian government information as one of their three main sources. Australian-only sources were selected by 156 (61%), a mix of country-of-origin and Australian sources by 90 (35%) and country of origin by 10 (4%). About 40% (101/256) reported family members and friends as one of their three main sources.
Participants’ socio-demographic characteristics, sources of information and preferred channels to receive information about COVID-19 vaccines and vaccination programme.

The question asked was: ‘From the list below, please select up to three sources that you think you have received most of your information about the COVID-19 vaccines.’ Number of participants responded: 256.
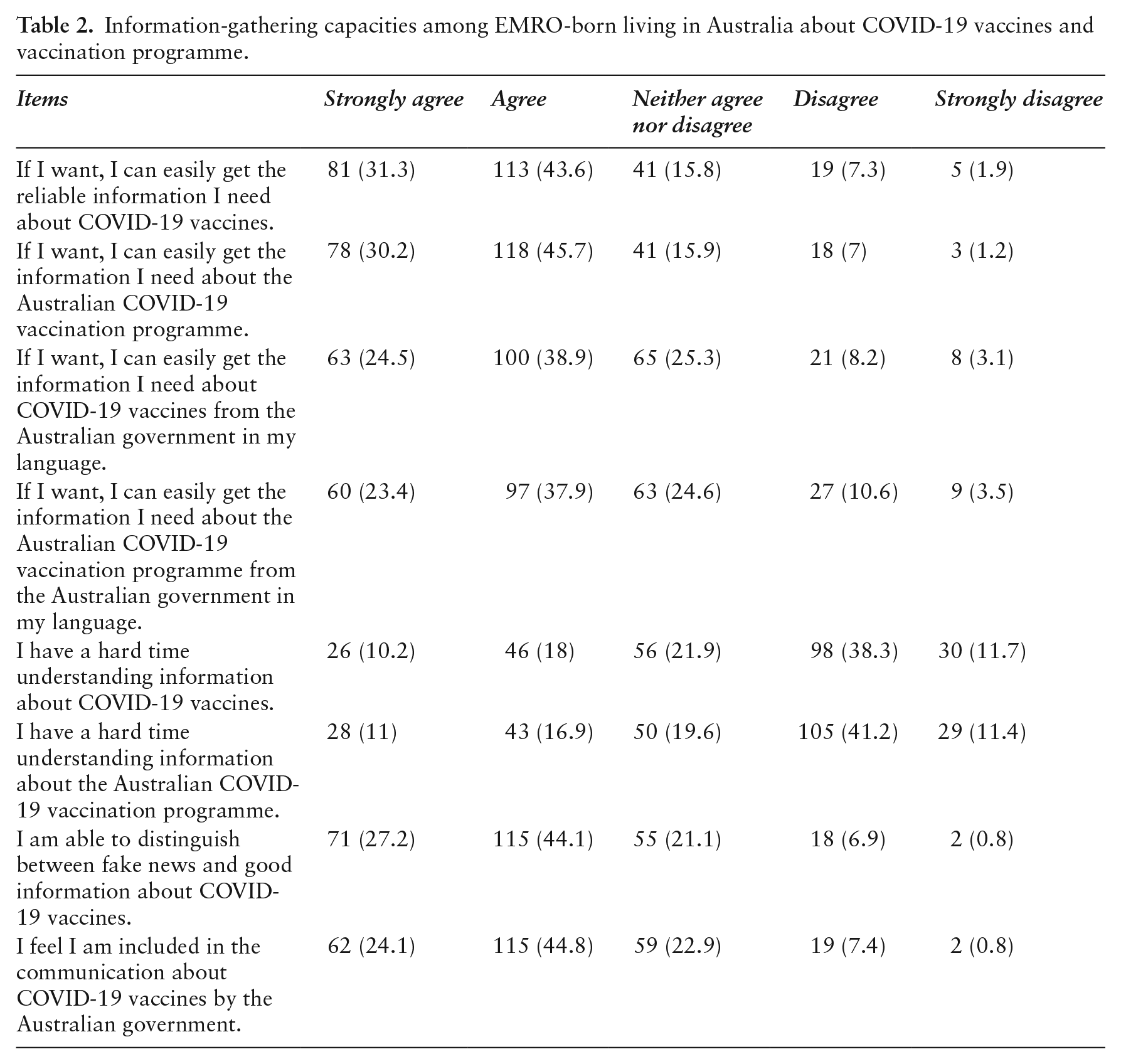
Around 70% of participants agreed that they can easily access the information they need, distinguish between fake and good information, and feel included in the Australian government's communications. Around 60% of participants agreed that they can access information in their own language from the Australian government. Approximately 50% of respondents indicated they had difficulty understanding vaccine information (Table 2).
Information-gathering capacities among EMRO-born living in Australia about COVID-19 vaccines and vaccination programme.
Qualitative findings
Nine men and eight women born in 11 countries participated in interviews. Four participants either were, or were studying to become, health professionals. During the interview, four participants self-identified as community leaders. We did not ask participants if they were community leaders or prominent members.
Participants reported that because the vaccine was new, and they had little experience with it they and others in their community lacked sufficient information to make decisions about whether to accept it. They defined their information need as knowing all the details about the vaccine to be secure.
This is not something . . . like the normal cold and flu vaccine, people are scared these days they don't know what they really haven't experienced . . . They don't want to go in something like do a mistake by taking a vaccine . . . So I think they should know each and everything so that they feel they're secure. [M06]
A lack of trust in Australian authorities and, therefore, in the communications disseminated by officials contributed to their perceived information needs.
They [government] don't disclose everything . . . So there are things which we don't know. Mostly the government or the people in the higher authority, they know it very well. [M06] I think that side effects are listed somewhere on the [government] web. But . . . in real ground, you see very different side effects and stories from people than what you see on the web, like on the web, it's very mild side symptoms and stuff like that. And . . . some people are having it really hard. So I think that's where the fear factor comes in. [W06]
Perceived information needs led people to use a variety of sources to collect information to guide their decisions about the COVID-19 vaccine. These sources were a combination of official and unofficial sources.
These sessions [for migrants about COVID vaccinations] with the organisation I’m volunteering for, coincided with when I started to think about getting the vaccine. So I’ve got some of the information from these sessions. And also, I have some friends – doctors, whom I sometimes contact them ask them their opinions. Part of my information was from researchers, but also from the media, the TV and the news and parts are from, like, word of mouth, from my friends. [W07]
Official organisations
Official communication about the COVID-19 vaccine was based on generalisable information needs and required audiences to accept some level of uncertainty. This approach did not satisfy the information needs of those who defined their needs as being beyond the information available through official channels.
I think that the basic information is available [through the Australian Health System] . . . like what COVID is, like the amount of doses you need . . . like clinics . . . But sometimes when people want more information that can be very difficult to access . . . no one can give you a straight answer. [W04]
Health professionals
To obtain details about the vaccines that were absent from public health messages, such as information about risk, people consulted health professionals. People preferred to obtain this information within the context of trusted relationships.
My mother . . . came to Australia at the very end of her life . . . she gets all her information from a GP, who she trusts. If she didn't trust . . . I think it's going to be a very difficult thing to convince her to take booster or even the actual vaccination. [M09]
The need to know everything about the vaccines was particularly highlighted for people with specific circumstances, such as pregnant or breastfeeding women and those with chronic conditions, who often access multiple health professionals as information sources.
Because I was breastfeeding, I didn't have any information from my GP or even the people at the call centre where you book your appointment . . . when I asked my GP, my GP said that it was safe, but they didn't give me any reasoning behind it . . . So I had to book with my daughter's paediatrician and then I also booked with my endocrinologist to ask if it was safe to get the vaccine . . . I was very vaccine hesitant. I didn't want to get it until I was sure that it was safe. [W02]
Receiving information from health professionals was not only through the traditional appointment-based sessions but also included seeking information from health professionals from the same cultural and linguistic backgrounds through social media and community-organised events.
I have joined a very nice [WhatsApp] group. It's called the Australian Islamic Medical Association . . . I've received a few videos made by the GPs, doctors themselves, and they belong to different languages . . . And it was really good to know that they are telling us in our own languages, so yeah, so I got this information from there. [W05]
When information from official organisations and health professionals was not accessible, did not satisfy people’s needs, or people did not trust the source – as one of the participants put it, ‘they don't want to consume more information from the people that are confusing them even more’ – they sought information from alternative sources.
Social media
People sought information from social media managed by community groups or leaders. Their trust in community leaders gave them confidence in information obtained through these networks.
So there's a few Facebook websites [managed by the community] that always give an update in Arabic . . . we have a lot of trust in community leaders and majority of the time, that's where people go to. [W08]
Participants preferred to obtain vaccine-related information from social media for several reasons, including that the effort needed to become informed is decreased because the visual element aids in communicating meaning, and social media content can be passively consumed rather than actively sought. However, there is the associated risk that people will be exposed to information that is incorrect or contradicts official information, and the risk that information will be disseminated through the wider community.
Those videos that come in through WhatsApp are actually the source of information, rather than, you know, most of the government things are on the website . . . you have to click on the website, but doesn't come through like our WhatsApp . . . now the anti-vaccination are getting really smart in working with the elderly people, the immigrants those that can't read have . . . access [to] information you can share and run. [W03]
Personal networks
Participants obtained vaccine information through personal networks including family members, friends and community members. ‘We use people as resources, and that makes sense. Our community as resources.’ Using personal networks as a source of information overcame the problems of mistrust and barriers posed by lack of English proficiency, literacy and digital literacy among some migrants.
I’ve just noticed that a lot of people when they’re confused, and they don’t understand, that they’ll ask family members, who are just more well versed in that sort of lingo and language . . . A lot of people that I had to talk to, they didn’t have that level of education . . . And I had to kind of use my own sort of thing to like, explain it as simply as possible . . . They’re like . . . what it is. What are they putting in my body? [W04]
Experiential
People drew upon personal experience with the vaccine and anecdotes about others’ experiences to evaluate the validity of information distributed through official and unofficial sources.
People talk, you know, different things, negativity, about the COVID vaccine. When I had my vaccine, people were ‘Oh tell me six months later what happened.’ Now and nothing happened. [M03]
People who had experienced serious side effects that were not communicated by official sources, or witnessed them in others, re-evaluated their trust in official information in light of their experiential information.
So when my dad got the vaccine, he had very severe side effects . . . when we did go to get him the vaccine, they said that it's a very small chance that he'll have side effects, but they didn't really list what the side effects would be . . . I feel like not all the information was disclosed to us. [W02]
People who witnessed breakthrough infections among family and community members were more likely to seek and rely on experiential information to decide about getting the vaccine.
I was confused. People are getting the vaccine and they still get sick. And we didn't know what was the point of getting vaccine as I get sick again. [M03]
People reported that experiences with the vaccine and anecdotes of others’ experiences ‘makes it real’. Experiential information was more likely to shape people’s decisions about vaccines than information provided through official sources.
And a huge factor is . . . the people around them, if they're getting it and it's like talking about their experience . . . it's like okay, someone has got it . . . I'm also gonna get it. [W04]
Combining information
Participants sought information from multiple sources to weigh up the risks of contracting COVID-19 against the risks of being vaccinated, and considered vaccine mandates to make decisions.
Because there are lots of rumours about this vaccine . . . I wasn't really keen to have it but then because of the lots of calls to have the vaccine I start to believe that I need to take it because lots of people have already had it . . . Because I have a special heart condition . . . So if I get the virus, the virus could kill me. the only option I have is to get a vaccine . . . And I might bring the virus and I might expose like, one of my family members . . . and my plan to travel back home country were the reasons I had to have the vaccine. [W07]
Final mixed methods integration
Findings from both quantitative and qualitative phases showed that migrants use information from multiple sources to guide their decisions about COVID-19 vaccines. These sources included official and unofficial sources. Migrants’ information-gathering capacity and perceived information needs affected the type of sources used. The newness of the vaccine and the lack of trust in officials influenced migrants’ perceived information needs. Personal network and experiential information were perceived as more compelling, accessible and trustworthy sources.
Discussion
Based on our findings, migrants use information from multiple sources to guide their decisions about COVID-19 vaccines. Despite most participants reporting official sources as one of their main sources, only 60% reported using only Australian sources. Information sufficiency tended to be unfulfilled using only Australian official sources. Lack of trust in official sources and incomplete information because of the newness of the vaccine increased concern about the vaccine and made it more difficult to accept uncertainty.
Uncertainty is part of public health crises. Officials try to manage their audiences' information demand in making decisions about subsequent introduced interventions. Part of this management is relying on the public’s trust in officials (19). The more an individual trusts the health authority, the more likely they are to comply with health recommendations to mitigate risks (20). Previous studies reported trust in authorities as a key factor for COVID-19 vaccine uptake among migrants (11,21,22). However, officials may not be always trusted by all members of society. This can be more prominent among migrants, especially those whose health information needs and health information-gathering capacity were not considered in routine health communication practices but who suddenly became a target group for health communications during a public health crisis (11,23). In these circumstances, despite official reassurance messaging, our participants reported they wanted to know everything about the proposed vaccination by seeking details from multiple sources. When a particular channel does not meet users’ information needs or is not trusted, they will select other information channels, if they believe they have the capacity to successfully do so (26).
Navigating the complex environment surrounding COVID-19 vaccines required a high information-gathering capacity. For migrants, this capacity is determined by their level of literacy, digital literacy, proficiency in the destination country’s official language, and health system literacy (11,24 –26). People consider their capacity to gather information and analyse the costs and benefits of using particular sources to determine which are more likely to provide them with sufficient and trusted information with the least amount of effort (27 –29). When access to official information requires a high level of information-gathering capacity and is costly in terms of time and money, other, easier-to-access sources may play a more important role in shaping migrants' decisions about health interventions. Based on our findings, personal networks were the main sources, and many people prefer passive consumption of information, using email and SMS instead of searching for information. Previous studies reported migrants’ reliance on informal oral communication and easy-to-access and familiar channels to gather information about COVID-19 and its vaccines (25,30,31). This may be explained by unfamiliarity with the destination health system and health communication strategies and the limited capacity of some to define their questions based on their information needs and search for answers. It is also important to note that changes in COVID-19 vaccines information require people to regularly find and analyse information, which may have affected the way people prefer to receive information.
Our findings showed the importance of personal networks and experiential information in shaping migrants’ understanding of COVID-19 vaccines as they were perceived as more compelling, accessible and trustworthy sources. Previous work similarly showed that interpersonal channels are perceived as far more useful than others, which may be due to the greater likelihood that the interpersonal exchange may assist the user to evaluate information and ensure that the information provided will be relevant to their specific needs (28). Given that migrants’ personal and social networks may largely be limited to those from the same cultural and language backgrounds, there should be opportunities for migrants to improve their exposure to official information through unofficial sources. Presenting official information through stories and referring to people’s experiences and observations can be used for this purpose. In Australia, with some delay, the engagement of trusted members of the communities was one of the successful strategies in improving COVID-19 vaccination uptake among migrants (17). Previous studies reported the effectiveness of using personal networks to disseminate health information among migrant communities (32 –34). Meaningful engagement with prominent and trusted members of migrant communities in designing and disseminating health messages when used in combination with other methods of health communication can improve access to health information (11,21).
Strengths and limitations
The mixed methods approach of this research provided opportunities to develop a deeper understanding of migrants’ experiences in obtaining information about COVID-19 vaccines. The use of an online questionnaire may have excluded some individuals, specifically those with limited literacy and digital literacy, from participating. The availability of the questionnaire in only English, Arabic and Farsi and interviews conducted in English may have affected some people’s ability to participate or share their experiences. However, Arabic and Farsi are the languages of the majority of the migrants from EMRO and the inclusion of participants who self-identified as influential community members who could share the experiences of their community members might have reduced the effect of these limitations.
Conclusion
Migrants define their information needs and seek information from a variety of sources including official organisations, health professionals, social media, personal networks and experiential information. Our study highlighted the importance of trust and information-gathering capacity in accessing information sources. Personal networks and experiential information played critical roles in shaping migrants’ understanding of COVID-19 vaccines. The use of personal networks including engagement with influential community members in sharing official information may improve migrants' access to accurate information. There is a need for multiculturalism in health communication strategies in multicultural societies. Health information needs and preferred communication channels of people from various cultural and linguistic backgrounds should be considered in all health communications. Building trust takes time; the sudden change to a more culturally and linguistically appropriate approach during public health crises is not sufficient to improve access to health information. Routine assessment of migrants’ health information needs and information-gathering capacity and design of various health communication strategies can improve health equity in a multicultural society. The findings of this study can assist health officials in engaging with migrant communities in all stages of COVID-19 control and in the management of other health issues and crises in Australia and similar multicultural societies.
Footnotes
Acknowledgements
This study was funded by a project grant from the Australian Partnership for Preparedness Research on Infectious Disease Emergencies (APPRISE). The research team thanks the participants of this study. The authors thank Keely Allen for her support in quantitative data collection for this study and the people and organisations who assisted with participants’ requirements.
Author contributions
DP and SL contributed to the conceptualisation and design of the study. DP performed data collection and quantitative data analysis. DP and PF contributed to qualitative data analysis. MM contributed to the development of the manuscript. Original draft was written by DP and all authors contributed to data interpretation and editing of the article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by a project grant from the Australian Partnership for Preparedness Research on Infectious Disease Emergencies (APPRISE). The funding body was not involved in the design of the study, collection, analysis, and interpretation of data or the writing of the article.
Ethical considerations
Ethics approval was obtained through the Australian National University Human Research Ethics Committee (2021/224).
