Abstract
Introduction
Premature rupture of membranes (PROM) is one of the most common and important causes of premature births and peripartum mortality. Maternal antibiotic treatment affects the infantile prognosis. This study was conducted to compare the efficacy of Ampicillin and Cefotaxime administered for the parturients on neonatal outcomes.
Material and Methods
A comparison between the effects of Cefotaxime and Ampicillin on infantile complications of PROM was done in this clinical trial. Two hundred and twenty parturients with PROM who needed antibiotic therapy were randomized in two groups of control (Ampicillin) and intervention (Cefotaxime) treatments. The maternal/fetal statuses up to accouchement and the infants’ status up to transfer to neonatal intensive care unit, death, or discharge from hospital were followed. The Apgar score, cardiac, respiratory and nervous systems, infection, immaturity, asphyxia, and mortality rates were compared in both groups.
Results
The differences between the two groups were significant in: Apgar score min1 and min5, need for resuscitation, asphyxia, need for hospitalization, infection, and mortality rate.
Conclusion
Administration of Cefotaxime in parturients with PROM improved the Apgar scores and decreased respiratory complications, infection, asphyxia, mortality rate, and need for ICU hospitalization in infants.
Introduction
Premature rupture of membranes (PROM) is observed in 1%–3% of pregnancies. The incidence of PROM depends on ANC visit, history of PROM, history of abortion, abnormal vaginal discharge, and UTI (Tiruye et al., 2021). And 30%–40% of premature deliveries (Acop, 2007; Modarres and Moshrefy, 2002; Ghazvini K et al., 2008); causes severe problems for pregnant women and fetuses (Boskabadi and Zakerihamidi, 2019; Boskabadi and Zakerihamidi, 2018); and may be followed by long-term complications and morbidity in infants. According to Boskabadi, the most important risk factors for PROM are the mother’s diabetes and hypertension, which are associated with neonatal and maternal complications. Infection is the most important maternal and neonatal complication (Boskabadi and Zakerihamidi, 2019). According to the findings of one study, the maternal risk factors in pregnancy included diabetes, hypertension, prior PROM, smoking, urinary tract infection, thyroid disorders, history of premature birth, and cerclage, respectively. The labor complications consisted of cesarean, oligohydramnios, chorioamnionitis, placenta abruption, fetal distress, fever, and placenta previa. The neonatal problems in that study consisted of jaundice, infection, respiratory distress syndrome (RDS), and asphyxia. The common infections in infants with PROM included clinical infection, sepsis, and meningitis (Boskabadi et al., 2016).
Inflammation and infection of the choriodecidua is referred as the mechanism of PROM. There is a strong correlation between PROM and intrauterine infection/inflammation (chorioamnionitis), especially in preterm pregnancies (Romero et al., 2003). Women who experience PROM are at high risk for chorioamnionitis, which can be due to the increased bacterial colonization before or after the rupture of the membranes (Stock et al., 2015).
The source of maternal genital tract infection is different in different parts of the world (Hamedi et al., 2012). A meta-analysis study on the effect of antibiotics on preterm labors with/out PROM emphasized that vaginal colonization should be considered as a criterion in selection of antibiotics; and Ampicillin is an appropriate medication wherever group B streptococcus is the most common vagina colonizing microorganism (Segel et al., 2003). In a study the risk of neonatal infection in mothers with PROM who receive cefotaxime is clearly less than mothers who receive ampicillin (Boskabadi et al., 2014a). However, they have failed to address regions such as Iran, where other microorganisms like Gram-negative bacteria are more common. Regional differences in the microbiology of sepsis suggest a revision in the use of Ampicillin and its substitution with more appropriate antibiotics for Gram-negative bacteria. Cefotaxime, a 3rd generation cephalosporin, acts through prevention of the bacterial cell wall synthesis in a wide spectrum of Gram-negative and Gram-positive germs; whereas, Ampicillin, a penicillin group member, binds to penicillin binding proteins on the bacterial cell wall and inhibits its formation. The current study was designed to evaluate the suitable antibiotic through a comparison of the effects of Cefotaxime versus Ampicillin on maternal and neonatal complications of PROM.
Methods
Trial design
A comparison between the effects of Cefotaxime and Ampicillin on infantile complications of PROM was done in this clinical trial. This study was funded by University of Medical Sciences (grant numbers: 89647). A comparison between the effects of Cefotaxime and Ampicillin on infantile complications of PROM was done in this clinical trial.
Participants
A total of 220 pregnant women with premature rupture of membranes at gestational ages≥26 (Boskabadi et al., 2014b) weeks requiring antibiotics were volunteered in this clinical trial at Ghaem Hospital, Mashhad, Iran, between June 2016 and October 2018. All participants with watery vaginal discharge for more than 12 h were examined by an obstetrician/gynecologist and included in the study after confirmation of PROM and need for antibiotics. Other inclusion criteria were live fetus and parental consent to enter the study. Cases with congenital anomalies, delivery in less than 6 h from taking antibiotics, and antibiotic use due to other reasons such as concurrent urinary tract infections, vaginal infections or clinical chorioamnionitis (fever, uterine tenderness, mother tachycardia) were excluded from the study. The study was conducted for the first time and was considered a pilot study (Figure 1). Participant flow chart.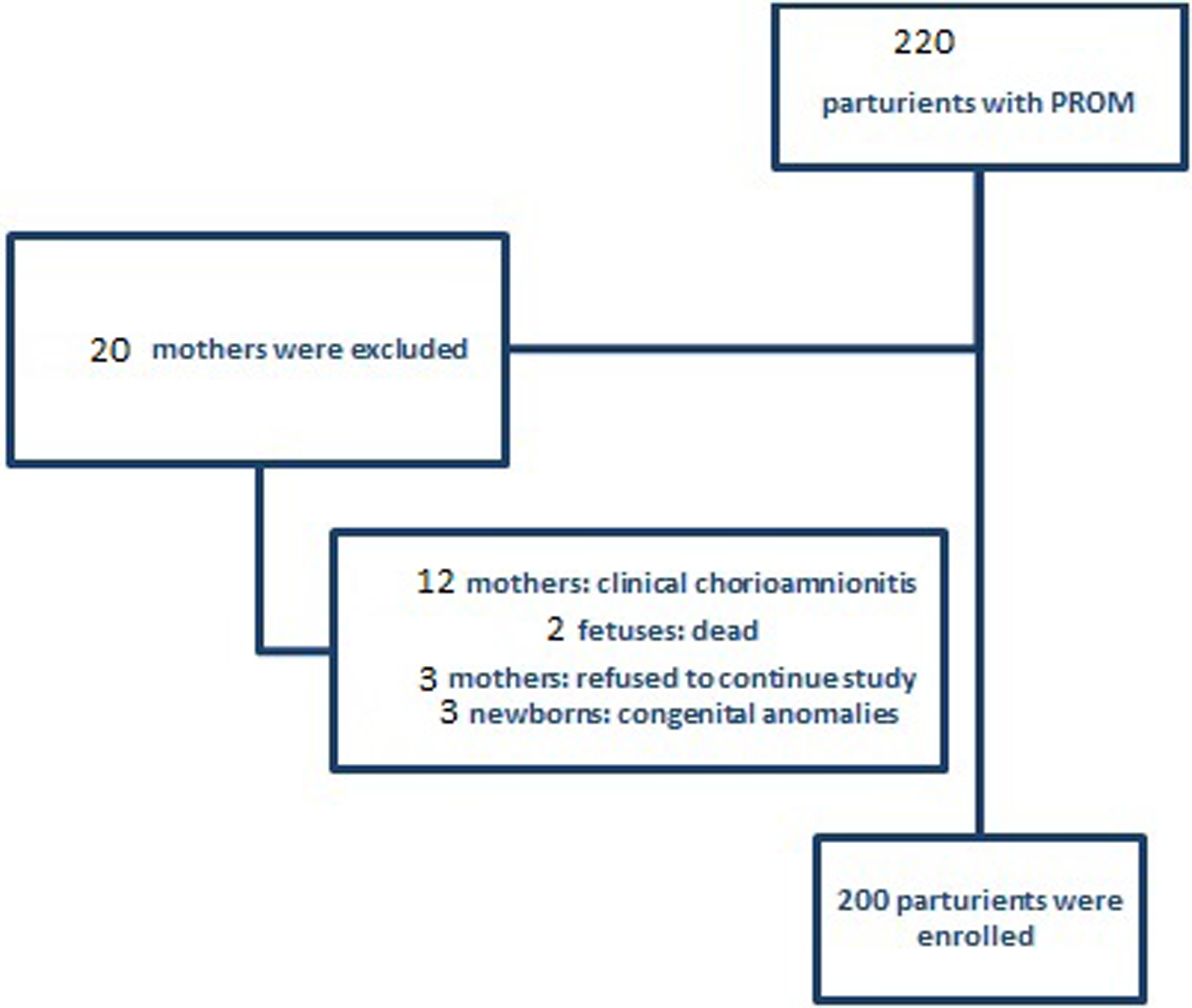
The participants were assigned to treatment groups via the block randomization method. To this end, a web-based online software package was utilized to identify the number of random blocks. We introduced 25 blocks of different sizes of 6 and 10 for 200 samples. The numbers 1-25 were assigned to the blocks. Each block included an equal number of intervention and control cases based on the block size. One of the blocks was randomly selected after the selection of the first mother; thereafter, it was assigned to one of the groups. We selected the next item of the same block by referring to the next mother. The sampling was completed by similar processing of the remaining blocks. The process continued till the completion of the first block. The next block was randomly selected from the remaining blocks, and the above process was repeated until the completion of sampling. Upon the admission of mother, the Obstetricians accidentally opened one of the blocks and, without knowing the grouping, presented one of the numbers to a nurse who was aware of the grouping. The nurse injected cefotaxime in mother of the intervention group or Ampicillin in control group. The neonate was followed-up by the resident of pediatric, who was blind to the grouping of mother. Data were classified as A and B in SPSS software (version 23). Moreover, to avoid any bias, the statistical analyst interpreted the results without knowing the grouping.
Interventions
The parturients in the control group received intravenous injections of Ampicillin, 2 gr every 6 h, until 24 h after delivery according to obstetrics and midwifery references; while, intravenous injection of Cefotaxime 1 gr every 8 h until 24 postpartum was performed for participants in the case group.
Outcomes
Data collection was performed by means of observation and a researcher-made questionnaire including maternal and neonatal demographic information. The content validity of the questionnaire was confirmed through literature review.
After obtaining an informed consent, initial questionnaire was filled containing the mother’s blood group, age and occupation, history of thyroid disorders, number of pregnancies and abortions, gestational diabetes and hypertension, eclampsia, history of PROM in previous pregnancies, infection, maternal amniotic fluid status, history of corticosteroid–antibiotic co-treatment, type of delivery, and duration of rupture of membranes.
The newborn’s gender, weight, height, head circumference, 1- and 5-min Apgar scores, need for cardiopulmonary resuscitation (CPR), and health status (respiratory, cardiologic, and nervous system as well as skin and abdomen) were evaluated. Neonates with poor health conditions were evaluated further in the NICU regarding the respiratory (tachypnea, grunting, nasal flaring, retraction, crackles and decreased lung volumes, need for respiratory support, oxygen hood and intubation, and need for ventilation, problems of respiratory distress syndrome (RDS), pneumonia, asphyxia, pneumothorax, pulmonary collapse), cardiovascular (heart murmur, bradycardia, arrhythmias, cyanosis), and neurological (decreased reflexes or normal neurological reflexes) statuses as well as infections (sepsis, positive-culture meningitis, urinary tract infection, clinical infection or R/O sepsis) and neonatal complications, necrotizing enterocolitis, hypoglycemia, jaundice, prematurity, cerebral hemorrhage, associated anomalies, and hypocalcemia. The gestational age was defined according to the Ballard maturational assessment of neonates at birth and/or the ultrasonography information of the first trimester of pregnancy. ESR, CRP, platelet count, Hb, Hct, and WBC tests as well as blood culture were performed during the hospitalization of neonates in NICU. Apgar score and VBG of cord were also used to assess asphyxia.
Statistical methods
SPSS version 21 was used for data analysis. Descriptive statistic indices including frequency distribution tables, mean, and standard deviation were used to describe the characteristics of the study samples. To ensure the homogeneity of the two groups Chi-square test was used for qualitative variables, independent t test for normal quantitative variables and Mann–Whitney test for non-normal quantitative variables. Analysis of covariance and univariate logistic regression model was used to control the variable of mode of delivery. A p < .05 was considered as statistically significant.
Results
Baseline data: The characteristics of the studied neonates in the two groups are compared in Figure 2. Comparison of (a) clinical and (b) gender charcteristics in two groups of infants born to mothers with PROM who were treated with either ampicillin or cefotaxime.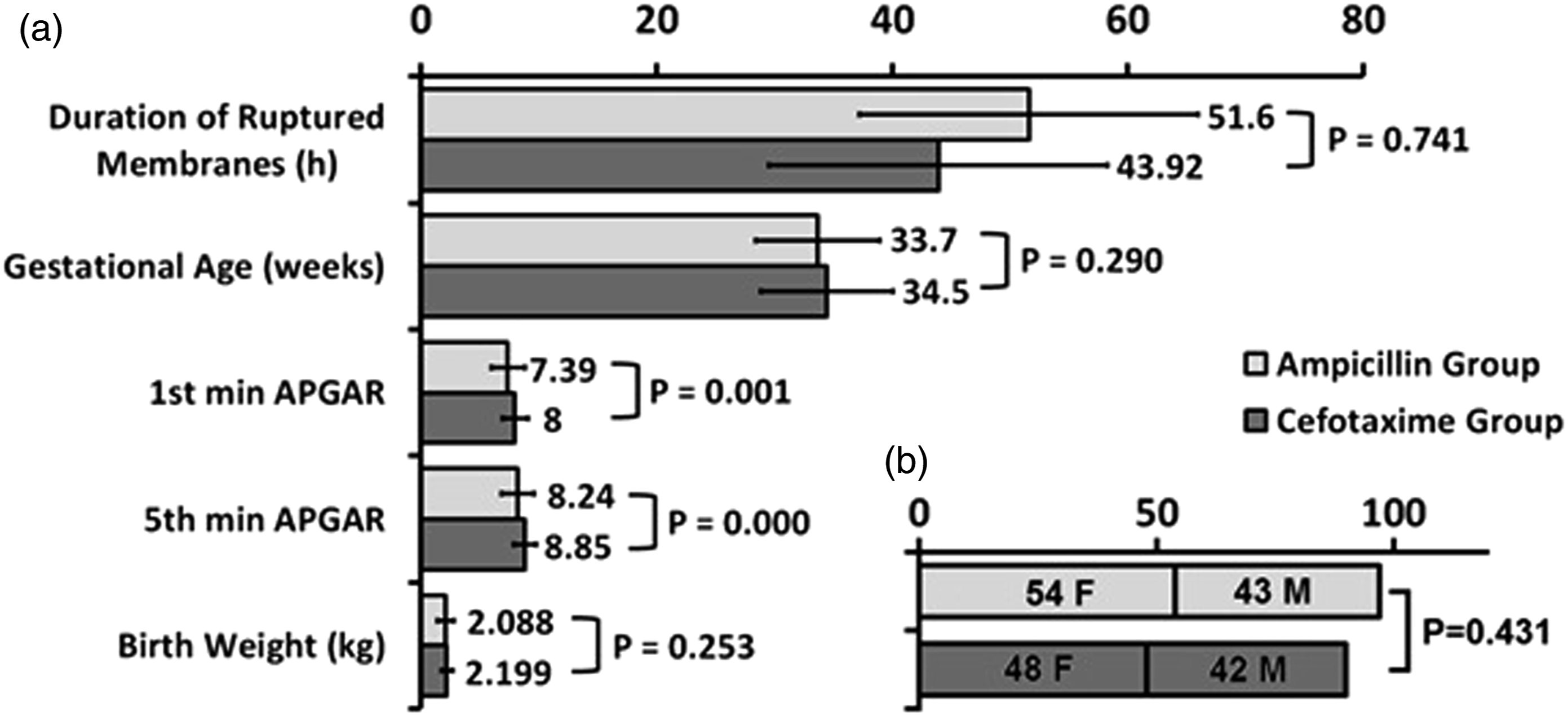
Numbers analyzed
Twelve mothers were excluded due to clinical chorioamnionitis; two fetuses were born dead; three mothers refused to continue with the study; and three newborns had congenital anomalies.
The mean age of the parturients was 27.15 ± 5.6 (Cefotaxime and Ampicillin groups were 27.2 ± 5.7 and 27.1 ± 5.5 years, respectively) (p = 0.98). The course of pre-partum corticosteroid consumption was 21.3 ± 5.6 and 22.4 ± 8.5 h in Cefotaxime and Ampicillin groups, respectively (p = 0.78). No significant differences was found between the two groups in terms of maternal education level (p = 0.56), number of pregnancies (p = 0.46), smoking (p = 0.16), gestational diabetes (p = 0.97), gestational hypertension (p = 0.79), eclampsia (p = 0.49), history of abortion in previous pregnancies (p = 0.29), history of previous PROM (p = 0.56), history of premature delivery in previous pregnancies (p = 0.62), genital infection (p = 0.22), urinary tract infection (p = 0.27), hemorrhage during pregnancy (p = 0.98), placental abruption (p = 0.37), placenta previa (p = 0.62), fetal distress (p = 0.21), and fever (p = 0.65). Most of the Cefotaxime-receiving women delivered naturally, whereas cesarean delivery was more common in the group receiving Ampicillin (p = 0.01). After adjusting for the route of delivery as a possible confounding factor by Analysis of covariance, the difference in the infection rate between the two groups remained statistically significant (p = 0.025). On the other hand, by performing the univariate logistic regression model test, it was determined that the mode of delivery was not clinically significant in the final result of the incidence of infection {OR: 0.320, 95% CI (0.067–1.524), p = 0.153}.
Although a total of 118 neonates (63%) were born preterm, no significant difference was observed comparing the control and case groups (p = 0.451). A total of 42% of the neonates (84 infants) were hospitalized among which, 67 infants had respiratory symptoms (tachypnea, retraction, grunting, and nasal flaring); 20 neonates experienced some degree of asphyxia at birth; and 4% of the neonates (all from the control group) died during the first week of their life. RDS, asphyxia, and infection were the underlying causes of death. Comparing the neonatal complications suggests that respiratory problems, asphyxia, sepsis, and need for hospitalization and resuscitation were significantly lower in the Cefotaxime group (Figure 3). Comparison of neonatal complications in control (neonates born to mothers with PROM who received ampicillin) and case (neonates born to mothers with PROM who received cefotaxime) groups.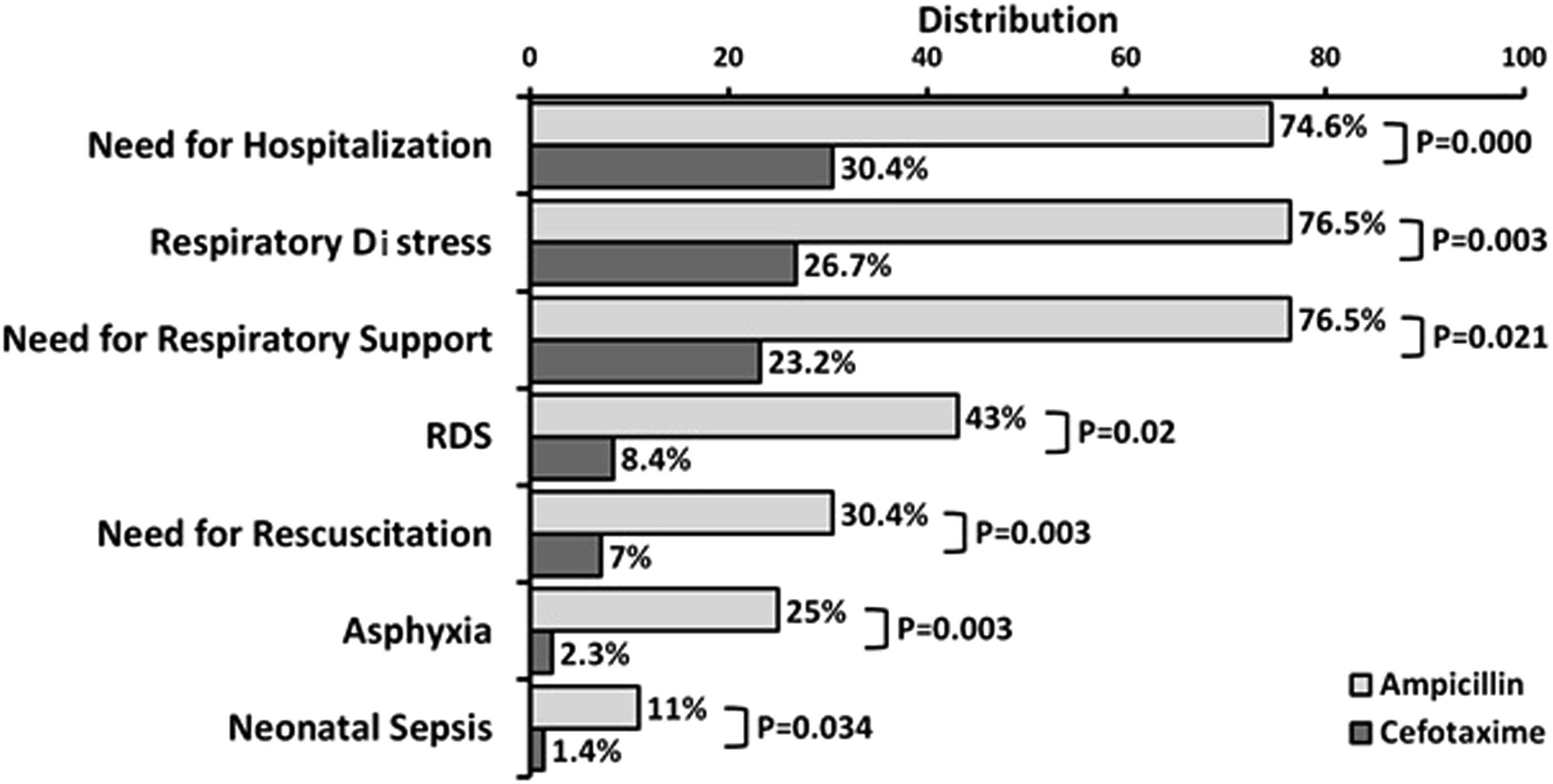
Outcomes and estimation
The two treatment groups were homogeneous regarding the predisposing factors (smoking, gravidity, abortion history, gestational diabetes, hypertension, eclampsia, history of previous PROM, history of premature delivery in previous pregnancies, genital tract infections, UTI, placental abruption, placenta previa, fetal distress, and amniotic fluid volume) (p > 0.121). The two groups were also homogeneous regarding gestational age, birth weight and duration of rupture of membranes (p > 0.290).
Ancillary analyses: Neonates in Ampicillin group required significantly more resuscitation in the delivery room compared to those in Cefotaxime group (p = 0.003). Respiratory difficulties and asphyxia were the main reasons for CPR in these neonates. The incidence of asphyxia in neonates in Ampicillin group was significantly greater than those in Cefotaxime group (p = 0.003). A total of 42% of neonates (57.2% in Ampicillin group and 23.3% in the Cefotaxime group, (p < 0.0001)) were transferred to NICU. The neonatal mortality rate in this study was 4.4%. Eight neonates (18.6%) died after birth in the Ampicillin group whereas no mortality was observed in the Cefotaxime group.
Discussion
Recent studies have shown that vaginal colonization by Gram-negative bacteria, especially E. coli, is on the rise in PPROM patients (Jeong et al., 2015; Mikula et al., 2023; Wolf et al., 2015). Rectovaginal colonization of Escherichia coli (E. coli) and other Gram-negative bacteria has been shown to be more common in mothers with preterm delivery (Javanian et al., 2017). Several other studies in Iran have shown that the most common vaginal germs in pregnant mothers are gram negatives (Boskabadi et al., 2014a; Hamedi et al., 2012).
In a coincident study in our center, Gram-negative germs were reported as the most common vaginal colonizing germ in mothers with PROM, while only 2% of mothers were infected with group B Streptococcus (GBS) (Saghafi et al., 2018). Coliforms, including E. coli, often colonize the mother’s vaginal canal and are thus acquired by infants before or during delivery (Simonsen et al., 2014). Vaginal bacterial colonization can increase the incidence of NICU hospitalization. Increased incidence of sepsis due to Gram-negative organisms may be associated with the increased consumption of prophylactic antibiotics by mothers to prevent GBS. The main factors in neonatal mortality are positive neonatal blood culture and neonatal sepsis (Saghafi et al., 2018). Due to the reduction in GBS colonization cases, the appropriate antibiotic treatment for PROM should be prescribed according to the common microorganisms in the endocervical bacterial colonization (Saghafi et al., 2018). In cases of bacteremia with pathogenic species, single-drug treatment with Ampicillin or Cefotaxime would be appropriate (Murphy and Weiner, 2012). In Lorthe’s study, in preterm premature rupture of membranes at 24–31 weeks, antibiotic prophylaxis based on third-generation cephalosporin may be associated with improved survival without severe neonatal morbidity when compared with amoxicillin, with no evidence of increase in neonatal sepsis related to third-generation cephalosporin-resistant pathogen (Lorthe et al., 2022). A former study in our center reported that Ampicillin was ineffective in the incidence of neonatal sepsis and decreasing the mortality rate of neonates of PPROM (Hamedi et al., 2012). Ampicillin-resistant E. coli is initially treated with beta-lactamases, such as Cefotaxime. The current study was designed based on the aforementioned considerations. Our results showed that antibiotic management of parturients with PROM with Cefotaxime compared to Ampicillin reduces neonatal pulmonary complications, NICU admission rate, incidence of infection, asphyxia, and mortality rate, while improves the neonatal Apgar score. Substitution of Ampicillin with Cefotaxime in treatment of parturients with PROM is proposed in geographical areas where group B streptococcus (GBS) is not the most common vagina colonizing microorganism. Among a total of 13 neonates with confirmed positive blood culture, 11 were in control groups, whereas two were in intervention group. The microbial germs in two of the neonates born from mothers receiving Cefotaxime were Staphylococcus, whereas the microbial germs in neonates born from mothers receiving Ampicillin were: Klebsiella pneumoniae (n = 5 cases), coagulase negative Staphylococci (n = 2 cases), E-Coli (n = 1 case), and Corynebacterium (n = 1 case).
PROM as a serious source of maternal-fetal/neonatal morbidity and mortality has a strong correlation with intrauterine infections. Ampicillin has been suggested and used for vaginal infections caused by group B streptococcus as the most common vagina colonizing microorganism. However, the source of maternal genital tract infection is different at different regions of the world (Hamedi et al., 2012). It seems that the antibiotics used in our region are most likely inappropriate as most cases of infections in our study were possible or clinical infections. The results of our study are consistent with previous studies in our geographical area (Boskabadi et al., 2011, 2014a; Hamedi et al., 2012; Ghazvini et al., 2008); however, lack of vaginal microbiological data in this study can still be a considerable limitation. Our results suggest Cefotaxime as a good choice in reducing the incidence of fetal problems and need for resuscitation. The results of study comparing Cefotaxime with Ceftriaxone showed that although both antibiotics are similar in terms of neonatal complications and infection prevention in mothers with PROM, Cefotaxime is more effective in deferring the delivery until at least 48 h, which helps the fetus lung maturation (Rasti et al., 2020). The findings of another study demonstrated that Cefotaxime is more cost-effective and therefore preferred to Ceftriaxone (Illahi et al., 2018).
While the incidence of asphyxia in neonates born to mothers with PROM has been reported to be 8.6% (Romero et al., 2003), our results showed a far higher incidence in Ampicillin group, but a much lower incidence in Cefotaxime group. This confirms the inefficacy of Ampicillin and rationalized use of Cefotaxime in parturients with PROM in our geographical area. Salan et al. showed that the Apgar score is affected by the time between the rupture of the amniotic sac and delivery, such that the reduction of this time increases the risk of a low Apgar score by 8.5 times (Salan, 2017).
Our results showed a lower NICU admission rate (42%) for neonates born to mothers with PROM compared to two previous studies in 2003 (65.3% and 75.8%) (Romero et al., 2003; Tanir et al., 2003). This lower total NICU admission rate in our study can be attributed to improvements in care technics (use of antibiotics in all neonates, differences in the patient selection, and higher gestational age in neonates in our study), as, this rate was notably lower even in our Ampicillin group. The newborns in Cefotaxime group showed a significantly lower NICU transfer rate, reconfirming the beneficial role of Cefotaxime administration in parturients with PROM.
In this study the incidence of sepsis in neonates of mothers receiving Ampicillin was 6 times higher than those in Cefotaxime group. Cefotaxime has shown suitable concentrations in the umbilical cord sera of neonates born to mothers colonized with E. coli and treated with Cefotaxime (Lepercq et al., 2009). On the other hand, in a study in Mashhad Ampicillin administration for 3 and 7 days in mothers with PROM showed no significant differences in the duration of gestation as well as the rates of chorioamnionitis, endometritis, and neonatal morbidity, suggesting the ineffectiveness of Ampicillin therapy on maternal problems and neonatal morbidity (Hamedi et al., 2012). In Ou-Yang’s study, Ampicillin plus cefotaxime should be casually prescribed only in selected critically ill neonates because they were associated with a higher risk of infections caused by MDR (multidrug-resistant) pathogens and final worse outcomes (Ou-Yang et al., 2023).
The incidence of sepsis in previous studies has been reported as 5.2%–14% (Medina and Hill, 2006; Mercer et al., 2003; Rathore et al., 2020). According to a study, antibiotic therapy decreased the incidence of sepsis (Romero et al., 2003). The incidence of sepsis has been shown to decrease in neonates born to mothers receiving Ampicillin while meningitis and pneumonia had an increased incidence (Romero et al., 2003). Compiling the results of the two mentioned reports with the current study suggests that Cefotaxime is an appropriate antibiotic against sepsis.
Neonates in this study were also examined for tachypnea, grunting, retraction, nasal flaring, and crackles. All these disorders were found to be more prevalent in neonates in Ampicillin group. Since bacterial agents are the major causes of PROM, appropriate antibiotics with higher penetration into the infants’ lungs can reduce the risk of respiratory disorders (Romero et al., 2003). Our findings confirmed the results of the previous studies where antibiotic therapy led to a decrease in the incidence of RDS and prematurity in neonates born to mothers with PROM (Bahasadri and Nateghi, 2006; Romero et al., 2003). Respiratory distress syndrome was seen in 22.6% of all neonates and in 34% of premature neonates. The prevalence of RDS in PROM in preterm neonates has been reported to be 54%–90% (Ehsanipoor et al., 2008; Medina and Hill, 2006). This lower incidence of RDS compared to the previous studies can be ascribed to the higher gestational age of neonates examined in our study, as, 1/3 of all neonates were full-term with apparently lower prevalence of RDS. Contradictory results from various studies are in part due to inhomogeneity of the samples and the difference in the antibiotics used.
The reason for the difference in infant mortality rates in other studies (4%–19%) (Boskabadi et al., 2014a; Medina and Hill, 2006) compared to our study (4.4%) can be ascribed to the fact whereas both treatment groups in the current study have received antibiotics which reduced the mortality rate, other studies have compared the results of prescription and non-prescription of antibiotics. Our findings are consistent with a previous study that reported a neonatal mortality rate of 4.6% due to preterm birth because of PROM (Romero et al., 2003).
Limitations: As a noticeable limitation, the colonization of germs was not performed simultaneously in vaginal canal of mothers. Regarding the low GBS colonization rate in our center, appropriate antibiotic regimens should be considered in PPROM cases according to the most prevalent microorganisms of endocervical bacterial colonization. Future studies are suggested to evaluate the presence of other responsible germs as well as assessing the efficacy of other suitable antibiotics on maternal and neonatal complications of PROM.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
