Abstract
Objective
To assess the applicability of albumin (ALB) and C-reactive protein (CRP) concentrations in the diagnosis of sepsis in neonates on the day of admission, and to help with early identification and intervention in the development of sepsis.
Methods
This retrospective study included all neonates who were admitted to the neonatal intensive care unit from January 2020 to June 2023. We studied 160 full-term neonates, including 80 with sepsis and 80 healthy controls. A multivariate analysis was conducted to evaluate the associations between ALB, CRP, and sepsis.
Results
CRP concentrations were significantly higher in neonates with sepsis than in controls (26.5 ± 8.6 vs. 3.6 ± 1.2 ng/L). At a cut-off point of 10.8 ng/L, CRP showed a sensitivity of 74.3% and a specificity of 80%. Moreover, ALB concentrations were significantly lower in neonates with sepsis than in controls (25.4 ± 2.5 g/L vs. 29.2 ± 2.6 g/L). At a cut-off point of 26.8, ALB showed a sensitivity of 75.6% and a specificity of 84.2%.
Conclusions
Our findings suggest that ALB and CRP concentrations on the first day of admission are different between neonates who do and those who do not develop sepsis. Higher CRP concentrations and lower ALB concentrations may indicate an increased risk of sepsis.
Keywords
Introduction
Sepsis is a cause of morbidity and mortality in newborns and has a high incidence despite advances in intensive care. Sepsis is a complex, life-threatening disease that is attributed to a dysregulated host response to infection, eventually leading to acute multiorgan dysfunction.1–3 An early diagnosis of neonatal sepsis remains a major challenge because of the non-specific clinical signs and symptoms. Therefore, early recognition and prompt treatment are essential to improve the prognosis of neonatal sepsis.
Among the diagnostic tests for sepsis that are currently used, blood culture is the gold standard for the diagnosis of bacteremia. 4 However, blood culture is time-consuming and a false-negative result can weaken its clinical application, especially in neonates. Recently, certain parameters have been used as markers of inflammation and infections. C-reactive protein (CRP) is a well-characterized indicator of systemic inflammation. CRP is considered a good indicator to evaluate the severity of sepsis, but its serum concentration may be affected by trauma, malignant diseases, and the physiological condition of patients.5,6 Several studies have shown that albumin (ALB) concentrations are decreased during sepsis.7,8 In addition, ALB is closely related to inflammation, and hypoalbuminemia is frequently observed in patients with inflammatory diseases.9,10 Qian and Liu 11 also found that the rate of hypoalbuminemia was common among children with sepsis and serum albumin concentrations were negatively correlated with the prognosis, but its use among neonates has not been well studied.
Therefore, this study aimed to assess the applicability of CRP and ALB as diagnostic markers in neonates with neonatal sepsis. Combined use of CRP and ALB may help identify sepsis, and allow intervention in a timely manner.
Methods
Population
This retrospective study included neonates with a gestational age of 37 to 42 weeks. The neonates were admitted to Linping Branch, The Second Affiliated Hospital of Zhejiang University and to the People’s Hospital of Zhuji from January 2020 to June 2023.
The diagnostic criteria for sepsis were as follows. (1) In the clinical diagnosis, we included neonates with ≥2 of the following abnormalities in non-specific blood tests: (i) a white blood cell count ≥30 × 109/L at 6 hours to 3 days after birth, ≥20 × 109/L at ≥3 days, or <5 × 109/L at any day of age; (ii) CRP concentrations ≥3 mg/L at 6 hours after birth, ≥5 mg/L at 6 to 24 hours, or ≥10 mg/L at any day of age; (iii) and procalcitonin concentrations ≥ 0.5 mg/L at >3 days. (2) Neonates were included if a cerebrospinal fluid examination was positive for bacterial meningitis. (3) Neonates were also included if DNA of the causative organism was detected in blood. The diagnosis of sepsis was determined by clinical manifestations, positive blood culture, or positive cerebrospinal fluid (or other sterile cavity fluid) culture. 12 Healthy neonates with no risk factors for infections who had been hospitalized for physiological jaundice in the neonatal unit were included in the control group. The exclusion criteria were (1) congenital anomalies or genetic metabolic abnormalities (2) severe asphyxia, and (3) intrauterine growth restriction (Figure 1).

Flowchart of patient selection. NICU, neonatal intensive care unit.
This study was approved by the medical ethics committee of Linping Branch of The Second Affiliated Hospital of Zhejiang University. The requirement for informed consent was waived because of the retrospective nature of this study. Verbal informed consent for participation in the study was obtained from the patients’ guardians. The reporting of this study followed the relevant STROBE guidelines, and all patients’ details have been de-identified. 13
Data collection
The following data were gathered from the hospital’s electronic medical record system: maternal age, mode of conception, premature rupture of membranes, chorioamnionitis, gestational age, birth weight, and sex. Blood tests for CRP and ALB were conducted using samples taken from the newborns’ veins within 24 hours of admission.
Statistical analysis
Statistical analyses were performed using IBM SPSS for Windows Version 26 (IBM Corp., Armonk, NY, USA). Normally distributed variables are expressed as the mean ± standard deviation, and the t-test for two independent samples was used for comparison between the groups. In a multifactor logistic regression model, the risk factors with statistical significance in the univariate analysis were selected as covariates, and the presence of sepsis and no sepsis were used as dependent variables to analyze the independent risk factors for sepsis. A receiver operating characteristic (ROC) curve was used to analyze the predictive value of CRP and ALB concentrations on the first day of admission for sepsis, to determine the best cut-off point, and to calculate the sensitivity and specificity of CRP and ALB for predicting sepsis. Differences were considered statistically significant at P < 0.05.
Results
A total of 160 neonates who were admitted to the neonatal intensive care unit were included in the study (Figure 1). There were 80 neonates in the sepsis group and 80 neonates in the control group. Patients in the sepsis group were significantly more likely to be complicated by PROM and chorioamnionitis than those in the control group (both P < 001). With regard to laboratory data, CRP concentrations were significantly higher, but ALB concentrations were significantly lower, in the sepsis group than in the control group (both P < 001, Table 1).
Baseline characteristics of the neonates.

Data are shown as n (%), median (interquartile range), or mean ± standard deviation.
SGA, small for gestational age; GA, gestational age; BW, birth weight; CS, cesarean section; GDM, gestational diabetes mellitus, PROM, premature rupture of membranes; CRP, C-reactive protein; ALB, albumin.
The logistic regression analysis showed that CRP concentrations (odds ratio [OR]: 2.20; 95% confidence interval [CI]: 1.34–3.26; P < 0.001), ALB concentrations (OR: 0.73; 95% CI: 0.64–0.94; P < 0.001), and chorioamnionitis (OR: 8.24; 95% CI: 2.35–12.48; P < 0.001) were independent risk factors for sepsis (Table 2). The optimal cut-off value of CRP concentrations was 10.8 ng/L, with a sensitivity of 74.3%, specificity of 80%, and area under the ROC curve of 0.68 (95% CI: 0.57–0.78). The optimal cut-off value of ALB concentrations was 26.8 g/L, with a sensitivity of 75.6%, specificity of 84.2%, and area under the ROC curve of 0.78 (95% CI: 0.68–0.89). Moreover, the area under the ROC curve of CRP+ALB was 0.84 (95% CI: 0.76–0.91), with a sensitivity of 88.4% and a specificity of 90.2% (Figure 2).
Logistic regression analysis showing independent predictors of sepsis.

PROM, premature rupture of membranes; ALB, albumin; CRP, C-reactive protein.
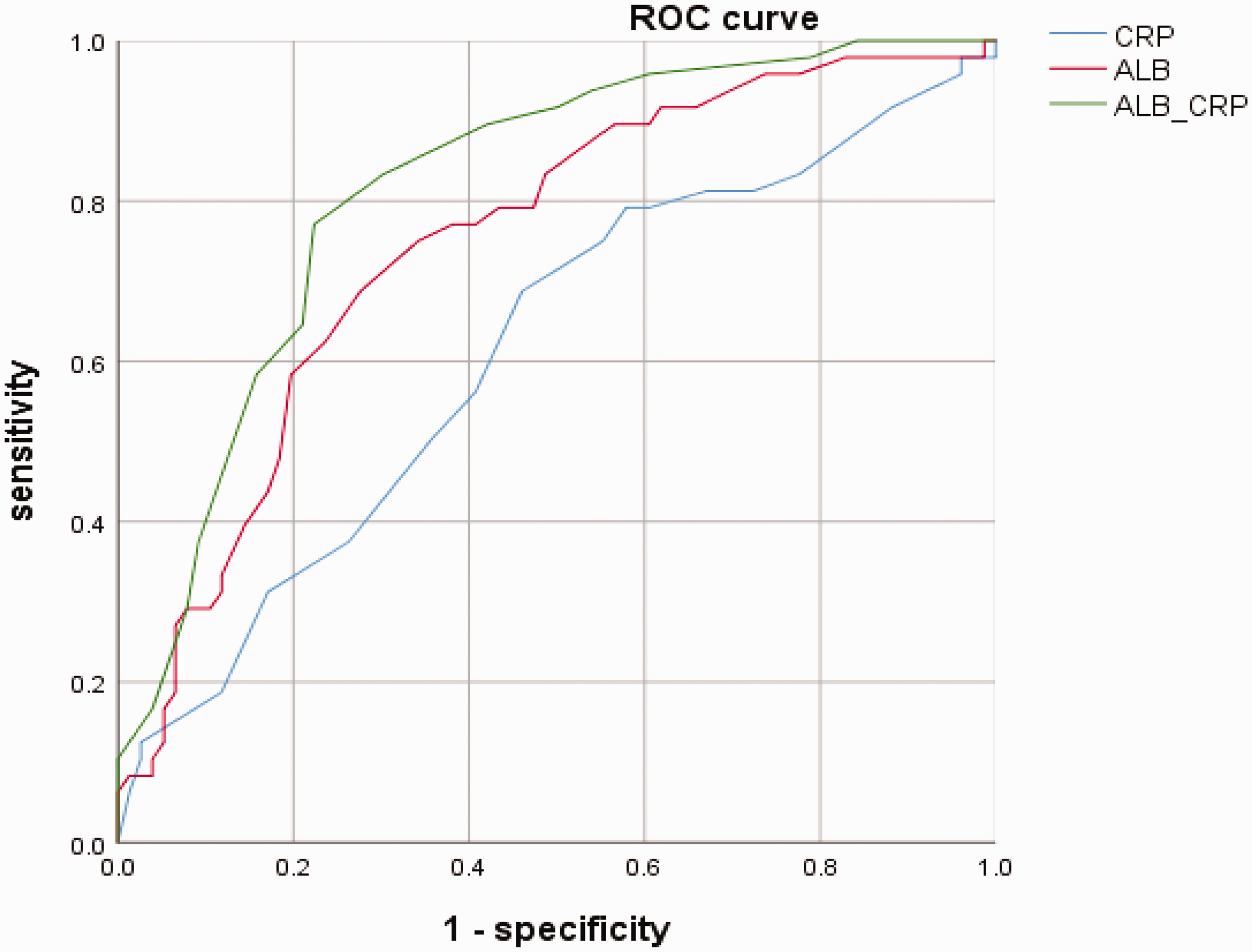
ROC curve analyses of CRP and ALB. ROC, receiver operating characteristic; CRP, C-reactive protein; ALB, albumin.
Discussion
The present study systematically analyzed CRP and ALB concentrations at admission in a cohort of neonates, and further evaluated the association between these features and the risk of sepsis. We found that CRP concentrations were significantly higher in neonates who developed sepsis than in those who did not. However, ALB concentrations were significantly lower in neonates who developed sepsis than in those who did not. Therefore, measuring CRP and ALB concentrations can help identify sepsis and provide intervention if necessary at an early stage. In addition, chorioamnionitis was an independent risk factor for the occurrence of sepsis.
Chorioamnionitis increases the risk of neonatal sepsis. 14 A meta-analysis also showed that chorioamnionitis was associated with blood culture-confirmed and clinically diagnosed neonatal sepsis. 15 A retrospective study in Sweden showed that chorioamnionitis increased the risk of neurodevelopmental disorders, especially cerebral palsy, autism spectrum disorders, attention deficit hyperactivity disorder, and intellectual disability. 16 Our study confirmed that chorioamnionitis was a significant risk factor for developing sepsis in neonates.
CRP is an acute-phase protein produced and secreted by hepatocytes. 17 To date, despite the detection of new markers of infection, the wide availability and rapid, simple, and cost-effective determination of CRP make it one of the preferred indices in many neonatal intensive care units. CRP concentrations may also be useful for the identification of neonates with bacterial infection, monitoring the response to treatment in infected neonates, and determining the duration of antibiotic therapy. 18 Our study showed significantly higher CRP concentrations in neonates with sepsis than in uninfected controls.
ALB is a multifunctional plasma protein synthesized in the liver. Some studies have shown that serum ALB concentrations on the first day of life are associated with severe infections in preterm infants. 19 In a prospective study of 199 very preterm infants with a gestational age <32 weeks, Torer et al. 20 found that the incidence of sepsis and morbidity and mortality increased as ALB concentrations on the first day of life decreased. The findings in these previous studies are consistent with our findings.
The main limitation of this study is the small patient population. Furthermore, because this was a retrospective, observational study, ensuring consistency of the clinical data was challenging because not all patients were treated by the same physicians. Finally, serum ALB concentrations could have been affected by the presence of jaundice in neonates who were included in the control group. 21
In conclusion, this study provides initial evidence for the usefulness of CPR and ALB concentrations in the diagnosis of neonatal sepsis. However, these findings still need to be confirmed by future studies with a larger number of neonates and different categories of infections using rigorous methods. Further studies could fully establish the role of CRP and other tested markers in the diagnosis of neonatal sepsis.
Footnotes
Author contributions
W. Yin wrote the manuscript. C. Fang prepared the figures. Y. Chen prepared the tables. All authors reviewed the manuscript.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
