Abstract
Introduction:
We conducted a meta-analysis (MA) to investigate the effects of furosemide on the prognosis of extracorporeal shockwave lithotripsy (SWL) therapy to remove renal (RS) and ureteric stones (US).
Methods:
We screened scientific databases including PubMed, Clinicalkey, Google Scholar, Medline, Embase, and Cochrane, from the date of establishment until March 2022, to search for randomized controlled trials evaluating SWL, in combination with furosemide (experimental group) or with SWL alone (control group), in treating RS or US. Our search terms included furosemide, extracorporeal SWL, and urolithiasis. For this MA, we employed the Cochrane Collaboration’s RevMan version 5.3.0.
Results:
Six trials, involving 1344 participants, with RS (n = 1097) and/or US (n = 247), met our predefined criteria. This included 137 proximal ureteral stones (PUSs), 35 mid-ureteral stones (MUS), and 75 distal ureteral stones (DUS). In case of RS, the experimental group exhibited significantly enhanced clearance, relative to controls (risk ratio [RR] = 1.16, 95% confidence interval [CI] = 1.07–1.25, p = 0.0002), yet there was no obvious difference in the PUS, MUS, and DUS (RR = 1.14, 95% CI = 0.97–1.33, p = 0.10; odds ratio [OR] = 1.26, 95% CI = 1.40–3.95, p = 0.69; RR = 1.21, 95% CI = 0.99–1.49, p = 0.06). There was also no marked difference between fragmentations in either group. Only reports of SWL treatment of RS provided adequate data on shocks, sessions, and complications for our analysis. Unfortunately, there was no significant alteration between the two groups.
Conclusion:
According to our analysis, furosemide strongly accelerates the clearance rate of SWL-treated RS. However, it does not enhance the fragmentation rate. Given this evidence, we propose that furosemide does not significantly improve the efficacy of SWL therapy in removing US.
Registration:
Our work is registered with PROSPERO (CRD42020204780).
Introduction
The global incidences of urinary stones ranges between 5% and 9% in Europe, 7% and 13% in North America, and 1% and 5% in Asia, and it is increasing in countries like Japan, United States, and Iceland. 1 The discrepancies in prevalence rates can be attributed to the following factors: age, race, socioeconomic status, dietary habits, sex, genetics, fluid intake, occupation, and education. Urinary stones rank third among urinary tract–related diseases, and have an approximately 50% recurrence rate throughout a patient’s life. 2
The high morbidity and recurrence rates of urinary stones increase the cost of stone management. Treatment options, based on size and location, include extracorporeal shock wave lithotripsy (SWL), ureteroscope (URS), percutaneous nephrolithotomy (PCNL), and flexible ureteroscopy (FURS).
Since 1980, SWL, a non-invasive and outpatient procedure, has been used as a common intervention for patients with renal (RSs) and/or ureteral stones (USs). 3 Currently, SWL is the optimal therapy for RS (<2 cm) and US (<1 cm). 4 Nevertheless, SWL limitations, compared to URS, PCNL, and FURS, include multiple treatments with a relatively low stone-free rate (SFR).5,6 Thus, the development of a novel stone clearing procedure is urgently needed to improve SWL outcomes.
Randomized controlled trials (RCTs) revealed that furosemide exposure enhances outcome of SWL treatment. However, the current data on furosemide supplementation of SWL treatment is conflicting. Moreover, prior multi-center investigations demonstrated that the SFR of SWL was significantly different based on varying locations of US. Thus, we conducted an extensive review and meta-analysis (MA) to verify the influence of furosemide administration on SWL outcomes in varying locations of US. Our conclusions will provide insight into the true nature of furosemide-based enhancement of SWL treatment.
Materials and methods
Study design
The preferred reporting items for systematic reviews and meta-analyses (PRISMA) criteria were employed while reporting the eligible studies. 7 Our work is registered with PROSPERO (CRD42020204780).
Search strategy
We searched scientific databases including PubMed, Clinicalkey, Google Scholar, Medline, Embase, and Cochrane, from the date of establishment until March 2022, for articles on SWL, either with furosemide (experimental group) or used alone (control group), in the treatment of RS or US. The following search words were used: furosemide, extracorporeal SWL, and urolithiasis. Our literature search was limited to ‘human studies’ and ‘English’, with no limitation on the publication year.
Inclusion/exclusion criteria
The following studies were included in our analysis: (1) RCT, (2) clinical intervention involving SWL alone (or with placebo) or in combination with furosemide, (3) full-text manuscript with the possibility of obtaining unpublished data, and (4) studies reporting the total number of subjects and appropriate results. The studies that were excluded from our analysis are as follows: (1) trials that explored the impact of different doses of furosemide on SWL exclusively and (2) trials that studied the combined effects of furosemide and other drugs (such as, α-blocker). Two authors (KI and SQH) were employed to assess the initially selected articles, based on the aforementioned criteria.
Data extraction
Two authors (FY and XLJ) conducted independent data extraction of the following information: study characteristics (author name, nationality, description of calculus, publication year, sample size, and detail methods), intervention [SWL with furosemide and SWL alone (or with placebo)], outcome (the rate of stone removal and fragmentation and the total number of sessions and shocks), and complications. Any conflicts in data collection were resolved by discussion and agreement.
The proximal ureteral stones (PUSs) were described as stones between the ureteropelvic junction and the top margin of the sacroiliac joint. The ‘lower ureter’ was defined as the region between the bottom margin of the sacroiliac joint and the ureterovesical junction. Stones in this region were termed as distal ureteral stones (DUSs). Finally, the mid-ureteral stones (MUSs) were defined as being in the region between the top and bottom margin of the sacroiliac joint.
Assessment of bias risk
The Cochrane Collaboration tool was used for calibration. 8 Using this tool, two reviewers (XSC and XLJ) examined and reported the bias risk and performed an independent assessment of each study. The risk was reported as ‘unclear’ if the reported data were inadequate and, therefore, a clear judgment could not be achieved. Any disputes regarding screening, selection of eligibility, or risk assessments, were settled by the reviewers through discussion and mutual consensus.
Statistical analysis and MA
RevMan v5.3.0 (The Cochrane Collaboration, Oxford, UK) was employed for all data analyses. A p value < 0.05 was regarded as significant. The Mantel–Haenszel method was employed for the exploration of categorical outcomes and risk ratios (RRs) with 95% confidence interval [CI]. The inverse variance method was used to compare continuous outcomes and mean difference (MD) with 95% CI. The chi-square test and I2 statistic were employed for heterogeneity assessment among the publications. In the presence of heterogeneity (I2 > 50%), the random-effects model was employed; otherwise, the fixed-effects model was employed. The impact of an individual study on the overall prediction was assessed using sensitivity analysis, where one study was omitted sequentially or subgroup analysis was conducted. Finally, publication bias was not evaluated since the number of analyzed studies was relatively low (<10).
Results
Characteristics of each study
Among the 525 articles retrieved from each database, 515 were excluded based on their titles and abstracts. In addition, four articles were eliminated based on their study design and lack of data availability. Finally, we included six RCTs that examined the synergistic action of SWL and furosemide against the actions of SWL alone.9–14 A flowchart of our inclusion/exclusion process is presented in Figure 1, and the demographics of the six eligible articles are summarized in Table 1.
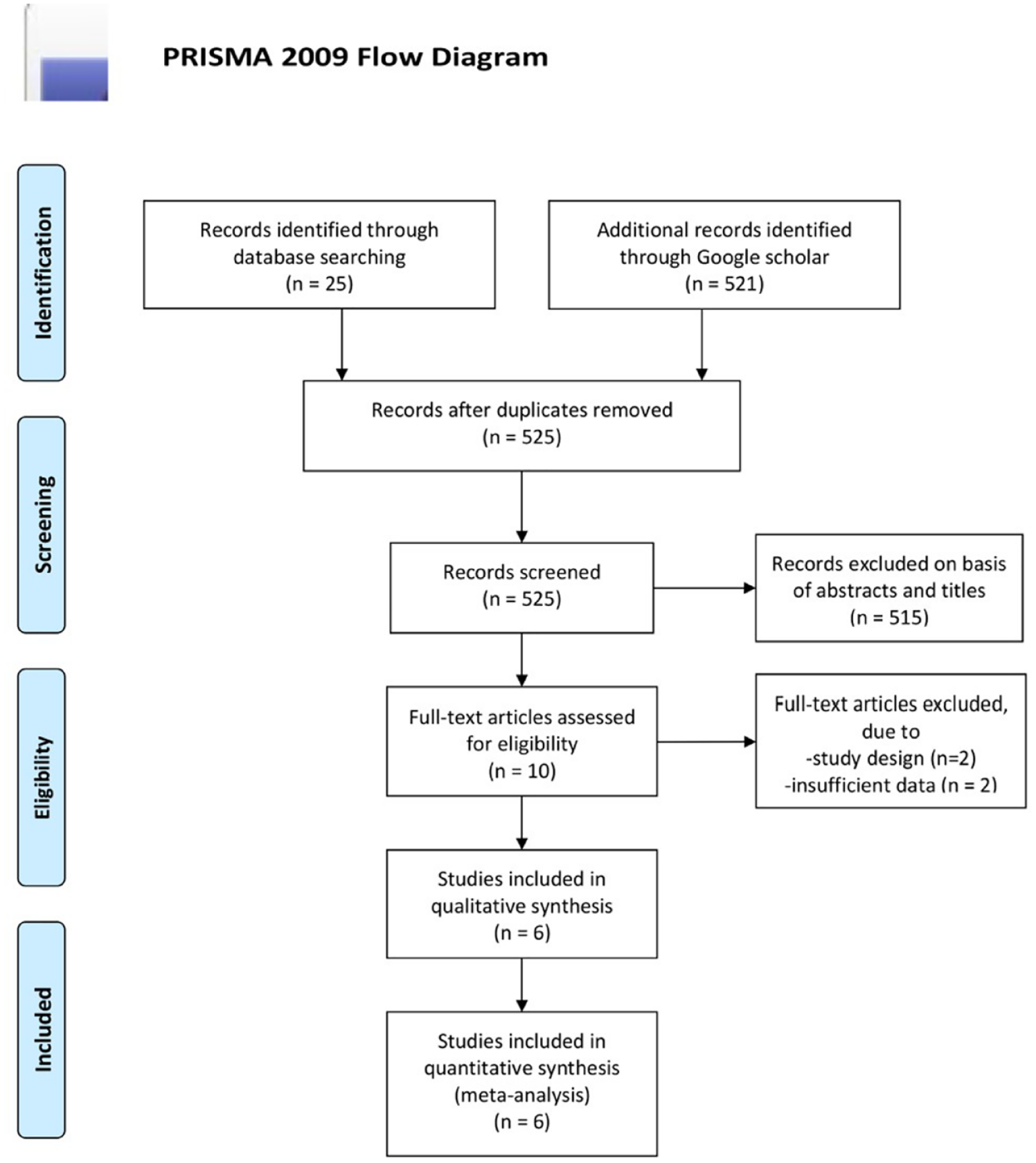
A flowchart summarizing our search criteria.
Characteristics of the included studied and quality assessment.

F, furosemide; NR, not reported; RCT, randomized controlled trials; SWL, extracorporeal shock wave lithotripsy.
Quality of each study
Among the six RCT studies, one failed to elaborate on the randomization procedure. 9 Four studies failed to report the allocation concealment procedure.9–12 All studies had relatively low performance, attritions, and bias in reporting.9–14 Four studies had unclear risk for detection bias,9–11,13 and all studies were free of other biases (Table 1). The study quality was not a criterion in our study selection process.
Primary outcome: stone clearance and fragmentation
The stone clearance and fragmentation rates in the enrolled studies were all based on X-ray and/or ultrasound image analysis. All patients underwent follow-ups every 2 weeks for 3 months. The fragmentation was assessed as good.
Four studies, with complete RS clearance data, were analyzed for RS removal.11–14 Owing to the presence of insignificant heterogeneity, we employed the fixed-effect model (p = 0.43; I2 = 0%). Based on our analysis, there was a significant improvement in RS clearance rate after furosemide + SWL administration (RR = 1.16, 95% CI = 1.07–1.25; p = 0.002), relative to controls. Three studies were used for RS fragmentation analysis, since they provided corresponding data.11–13 Due to the presence of insignificant heterogeneity, we employed the fixed-effect model (p = 0.86; I2 = 0%). Based on our analysis, an insignificant improvement was observed in RS fragmentation after furosemide + SWL administration (RR = 1.05, 95% CI = 0.94–1.16; p = 0.42), compared to controls.
Three studies were used for PUS clearance and fragmentation analyses, as they provided corresponding data.9,10,13 Due to the presence of insignificant heterogeneity, we employed the fixed-effects model for PUS clearance (p = 0.2; I2 = 39%) and fragmentation (p = 0.55; I2 = 0%) analyses. Based on our analysis, an insignificant improvement was observed in PUS clearance (RR = 1.14, 95% CI = 0.97–1.33; p = 0.10) and fragmentation (RR = 1.10, 95% CI = 0.97–1.24; p = 0.14) after furosemide + SWL administration, compared to controls.
Two studies were used for MUS clearance and fragmentation analysis, since they provided corresponding data.9,10 Due to the presence of insignificant heterogeneity, we employed the fixed-effects model for MUS clearance (p = 0.06; I2 = 72%) and fragmentation (p = 0.30; I2 = 6%) analyses. Based on our analysis, an insignificant improvement was observed in MUS clearance (RR = 1.26, 95% CI = 0.40–3.95; p = 0.69) and fragmentation (RR = 1.08, 95% CI = 0.86–1.35; p = 0.51) after furosemide + SWL administration, compared to controls.
Two studies were used for DUS clearance and fragmentation analyses, since they provided corresponding data.9,10 Due to the presence of insignificant heterogeneity, we employed the fixed-effects model for DUS clearance (p = 0.86; I2 = 0%) and fragmentation (p = 0.19; I2 = 42%) analyses. Based on our results, an insignificant improvement was noted in DUS clearance (RR = 1.21, 95% CI = 0.99–1.49; p = 0.06) and fragmentation (RR = 1.16, 95% CI = 0.98–1.38; p = 0.08; Figures 2 and 3) after furosemide + SWL administration compared to controls.

(a)–(d) Forest plot of SFR: (a) renal stone; (b) proximal ureteric; (c) mid-ureteric; and (d) lower ureteric.
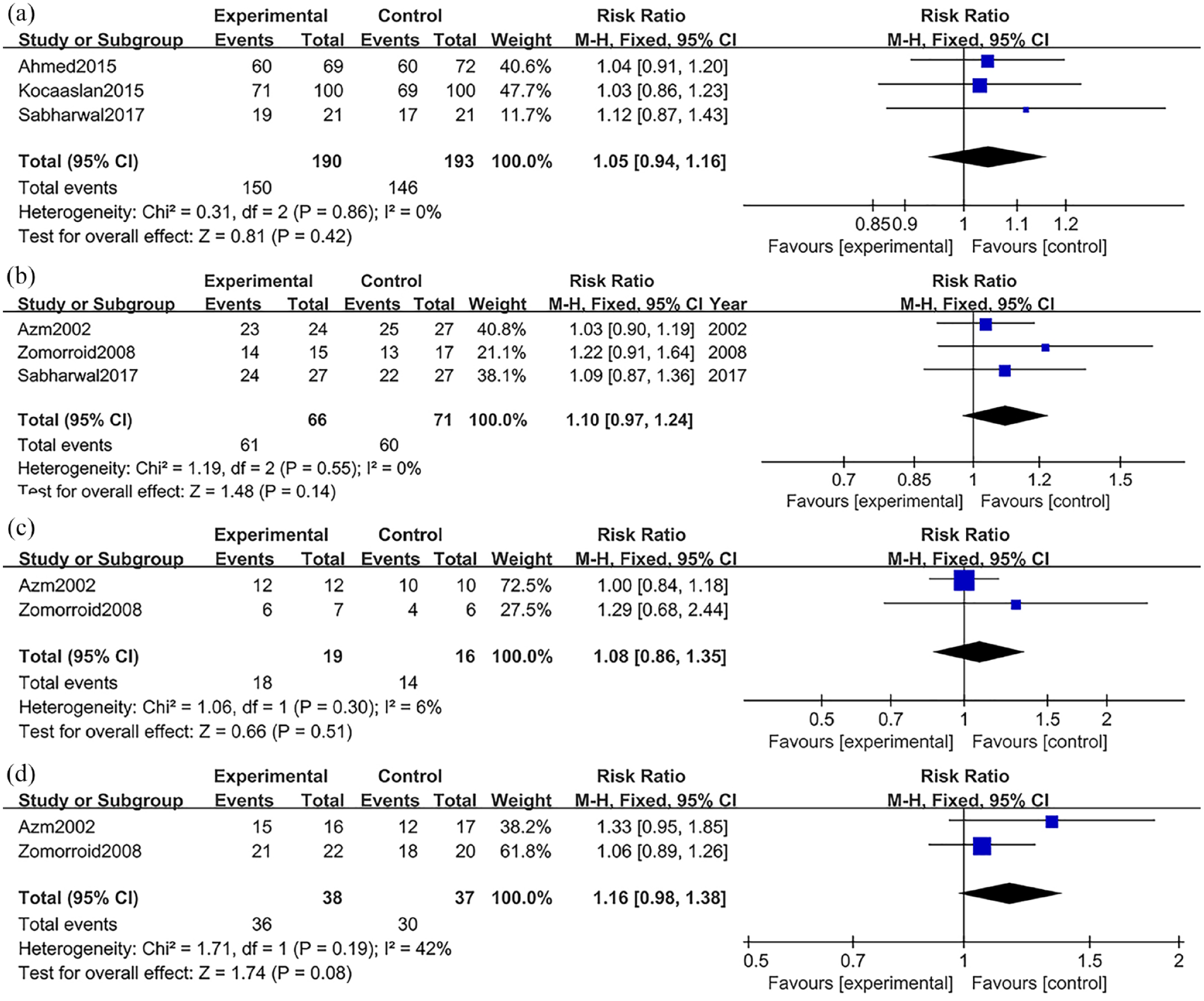
(a)–(d) Forest plot of fragmentation: (a) renal stone; (b) proximal ureteric; (c) mid-ureteric; and (d) lower ureteric.
Secondary outcomes: total amount of sessions and shocks needed
Half of the studies included in our MA had incomplete data regarding the required SWL shocks and sessions to completely treat US. Hence, only three studies were used for the analysis of the amount of shocks and sessions needed for RS removal, as they provided corresponding data. Since these studies revealed no heterogeneity regarding shocks and sessions (p = 0.95; I2 = 0%) (p = 0.83; I2 = 0%), we employed the fixed effects model for both analyses. Our results revealed that the number of shocks (MD = −134.18, 95% CI = −419.66 to 151.30; p = 0.36) and sessions (MD = −0.11, 95% CI = −0.24 to 0.03; p = 0.11) needed by the SWL + furosemide group were considerably lower than controls (Figure 4).

(a) Forest plot depicting alterations in SWL shocks in renal stone; (b) Forest plot depicting alterations in SWL sessions in renal stone.
Adverse effects and complications
The adverse effects of furosemide were not reported in all six studies.9–14 Only one study failed to mention complications. 13 Thus, we evaluated the complications in the remaining five studies.9–12,14 No complications were observed in the Azm and Higazy 9 and Zomorrodi et al. 10 studies, whereas the remaining three studies reported complications after SWL treatment to remove RS. Due to insignificant heterogeneity among the studies, we employed the fixed-effects model for complications analysis (p = 0.42; I2 = 0%). Based on our results, an insignificant decrease in complications was observed in the SWL + furosemide group, relative to controls (RR = 0.82, 95% CI = 0.64–1.04, p = 0.10; Figure 5).

Forest plot depicting alterations in SWL complications in RS.
Sensitivity analysis
The I2 statistic results revealed significant heterogeneity in the MUS clearance data among studies. However, we were unable to perform sensitivity analysis owing to the low quantity of eligible publications.
Discussion
Although SWL has been the primary intervention for US since 1980, 4 advancements in minimally invasive technology offers a faster and more effective stone clearing effect, with fewer complications. 6 However, SWL has advantages that make it irreplaceable by other treatments. For example, there is no need for anesthesia, it can be offered as outpatient treatment, and it is associated with minimal complications. Hence, The European Association of Urology still endorses SWL as the optimal intervention for RS < 2 cm or US < 1 cm. 4 Several factors, including kidney function (obstruction degree and renal unit functionality) and stone features (site, burden, and type) influence SWL success. In addition, more frequent treatments are often necessary, thus weakening SWL efficacy. Therefore, it is crucial to include adjuvant therapy that reduces need for retreatment. Prior studies revealed that adjuvant therapies, such as, DJ stenting prior to SWL, as well as oral α-receptor blocker administration after SWL can markedly improve SWL outcomes. However, it was also reported that the disadvantages of DJ stenting overpower its benefits, 15 and α-receptor blockers are only effective against crushed stones. 16 Therefore, it is necessary to develop better auxiliary methods.
Herein, we carried out an MA to investigate the significance of furosemide administration on SWL prognosis. Our systematic review revealed that SWL with furosemide provides a better stone clearance rate for patients with RS than SWL alone. The results also revealed that furosemide does not significantly enhance SWL effects on US.
Recent research proposed several theories, including spallation, tear, and shear forces, quasi-static squeezing, dynamic squeezing, and cavitation, that explain the principles of SWL, and all these theories have a very close relationship with the stone–water interface. 17 In particular, the cavitation activity is crucial for augmentating SWL efficiency. It is especially critical for producing fine fragments.17,18 The negative pressure phase of SWL generates cavitation within the fluid surrounding the stones and within the microcracks/cleavage interfaces. However, if there is not enough water surrounding the stones, cavitation bubbles can form, which can result in the depletion of maximum energy related to the SWL tensile pressure. This, in turn, can minimize cavitation activity around the target stone, and drastically reduce stone comminution. 18 Therefore, once the stone begins to crack, the powdering of the stone depends on the amount of water that enters the cracks. Powdered stones are easier to pass out of the body than cracked stones.
Furosemide exposure generates more urine during SWL. This promotes the formation of a liquid interface on stone. Simultaneously, the presence of excess fluid enhances penetration into the stone, which may reduce cavitation bubbles between the damaged shell and the core, thus enhancing the impact of successive SWLs on the stone core. Our research results are similar to an earlier reported RCT involving 714 patients, which reported that furosemide significantly improves the SWL-mediated clearance of RS. 14 However, other studies do not report any statistical significance likely due to small sample populations.12,13
Unlike the renal pelvis, where there is enough space for stones to be surrounded by water, US is usually surrounded by soft tissue, and, is therefore, difficult to penetrate with water, particularly, within the allocated time. It was reported that SWL efficacy is markedly enhanced at a reduced treatment rate (70–80 shocks per minute) when eliminating RS; however, it is not significant for US. 19 Interestingly, shock waves of 60 shocks per minute is more effective against US as there is more time for the water to enter cracked stones. 20 Hence, a diuretic agent generates more urine which may enhance SWL efficacy in US. Prior studies from 2002 and 2008 reported that furosemide supplementation is both beneficial and safe for patients undergoing SWL for distal and middle US.9,10 However, when treating upper US, diuretics usage with SWL treatment, showed no significant difference, compared to SWL treatment alone. 13
In our MA, furosemide did not enhance SWL treatment of US. The sample size included in our MA was relatively small. It was previously reported that the degree of ureteral obstruction is crucial to SWL success. 21 Due to severe stone-related ureteral obstruction, the amount of urine reaching the stone fissure may not be enough to produce a significant effect. In the Hans-Göran Tiselius et al. 22 study, increasing urine production via pressure infusion of around 1 L of Ringer acetate solution, in combination with furosemide, during SWL, did not produce any significant difference in US treatment outcome. Therefore, diuretics may not significantly enhance the effect of SWL on US.
Based on our analysis, furosemide did not significantly increase the fragmentation rate of SWL in both the kidney and ureter. SWL success depends on multiple factors, namely, stone size, location, Hounsfield units, technique, and distance of skin to stone. 6 In the studies,11–14 they do not find furosemide + SWL significant improvement in RS fragmentation. It is possible that stones not crushed by SWL possess higher Hounsfield units. 23 Therefore, even though furosemide increases the amount of water surrounding the stone, the seepage of fluid below the cracks will not happen, further disintegration of the core will not be enhanced. Hence, it may have no effect on SWL fragmentation rate, or number of sessions and shocks.
Both furosemide and high fluid intake before SWL, which can produce large amounts of urine, may able to enhance the efficacy of SWL. In Cheng et al.’s 24 study, they reported that administering 0.9% NaCl prior to SWL may be an effective measure to improve the treatment efficacy of SWL. However, in another study, 14 it was revealed that the efficacy of furosemide along with hydration is superior to hydration alone during SWL.
Due to the lack of data related to the effect of furosemide + SWL on impacted versus nonimpacted ureteric stones, the effect of furosemide + SWL on inferior calyceal RS versus other location RS and the effect of separate furosemide doses + SWL versus SWL alone on RS or US, a detailed subgroup analysis was not possible. Thus, additional studies are warranted.
Prior multi-center studies demonstrated that SWL treatment for stones in varying locations produce significantly different success rates.25,26 Diuretics may significantly improve the therapeutic effect of SWL on stones located within certain regions of the urinary tract, while having no effect on others. If the treatment effects of SWL in varying locations are analyzed in a unified manner, it is likely to cause deviations in result. A strength of this study is that we analyzed the effects of furosemide supplementation on SWL treatment of stones in various locations.
The included studies possessed adequate methodological quality. Nevertheless, there were a few potential limitations. The adverse effects related to furosemide were not reported in any of the enrolled studies, and non-contrast computed tomography scan was not used in any of the studies. These may lead to inaccurate assessments of the stone clearance and fragmentation rates. Various factors like stone type, stone density, stone size, stone location, skin to stone distance, and stone impaction in ureter affect the fragmentation and stone clearance rates. The lack of uniformity in these variables in the enrolled studies can, therefore, influence the overall results. Differences in the SWL machine used might also affect the outcome. In addition, there was no consistency in the rates of shock delivery (60–90/min) and gravel energy. Finally, the number of research cases in most RCTs was small.
Conclusion
Based on the present MA, furosemide significantly accelerates the clearance rate of RS following SWL treatment. However, it does not enhance the fragmentation rate. Moreover, furosemide does not improve the US clearance rate after SWL treatment. Future, high-quality RCTs are warranted to establish the true effect of diuretics on SWL-based intervention of urolithiasis.
Supplemental Material
sj-doc-1-tau-10.1177_17562872221128473 – Supplemental material for Furosemide improves the stone clearance rate of extracorporeal shockwave lithotripsy for kidney stones but not ureteral stones: a systematic review and meta-analysis
Supplemental material, sj-doc-1-tau-10.1177_17562872221128473 for Furosemide improves the stone clearance rate of extracorporeal shockwave lithotripsy for kidney stones but not ureteral stones: a systematic review and meta-analysis by Feng Yao, Ke Li, ShiQuan Huang, XueSong Cheng and XiaoLiang Jiang in Therapeutic Advances in Urology
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
