Abstract
Background:
Migraine inflicts substantial personal, social, and economic tolls on many adults in the United States (US). Acute and preventive medicines can offer some relief, but most patients are untreated or experience treatment failures. How preventive-treatment failures affect outcomes for patients no longer on preventive treatments or for patients with migraine is insufficiently understood.
Objective:
To measure the patient-reported health and economic burdens associated with increasing preventive-treatment failures among US adults with diagnosed migraine.
Design:
Retrospective, cross-sectional study.
Methods:
Data analyzed were from the 2023 US National Health and Wellness Survey. Participants were adults diagnosed with migraine, having ≥4 monthly migraine or headache days, having taken acute or preventive prescription migraine medications or currently taking acute prescription migraine medications, and taking no preventive migraine medications. Participants were categorized as never treated with preventive medicines, having failed 1 preventive medicine, or having failed ≥2 preventive medicines. Health-related quality of life (HRQoL) was assessed with the Migraine Disability Assessment, RAND’s 36-Item Short Form Survey Instrument, 5-Level EuroQoL instrument (EQ-5D), Work Productivity and Activity Impairment General Health version, 9-Item Patient Health Questionnaire, and 7-Item Generalized Anxiety Disorder scale. Details about medication use and health care resource use (HCRU) were collected. Data were adjusted by inverse probability of treatment weighting and compared using two-sided two-sample t-tests or Chi-square tests.
Results:
Patients who had failed preventive treatments had poorer HRQoL, greater work productivity loss, greater nonwork activity impairment, and greater HCRU than patients who had never taken preventive treatments. The number of preventive-treatment failures scaled with disease burden. Patients with ≥2 treatment failures had significantly lower EQ-5D scores (0.69 vs 0.73) than those for prevention-naïve patients; patients with ≥2 treatment failures had significantly higher overall work productivity loss (45.9% vs 34.9%), activity impairment (46.8% vs 36.7%), and higher rates of emergency room visits (37.0% vs 25.2%), hospitalization (23.5% vs 12.3%), and neurologist visits (17.6 vs 10.9%) than those of prevention-naïve patients. Medication overuse rates were similar among patients with any treatment failures and prevention-naïve patients (migraine-specific: 34.4%-39.3%; overall: 59.2%-62.3%).
Conclusion:
US adults with frequent migraines who failed preventive treatments have significantly greater unmet needs and different acute medication use patterns than adults who never took treatments.
Introduction
Migraine is a neurological disease that affects about 1 in 10 people worldwide, with a 1-year prevalence of 12% in the United States (US)1,2; it is associated with poor health-related quality of life (HRQoL) and costs the US economy almost $80 billion per year. 3 People with migraine are significantly more likely to have worse overall health, greater disease burden, and severe comorbidities, as well as to experience difficulties with interpersonal relationships and daily activities.4 –7 More frequent migraine attacks are associated with greater work productivity loss, greater health care costs, and greater costs to employers.8 –11
Acute and preventive therapies are available to treat migraine. Acute agents, such as serotonin 5-HT-receptor agonists (triptans, ditans), ergotamine derivatives, calcitonin gene-related peptide (CGRP) antagonists, nonsteroidal anti-inflammatory drugs (NSAIDS), and nonprescription analgesics, are taken when symptoms occur to relieve pain and restore functioning. In contrast, preventive treatments, including angiotensin inhibitors, CGRP antagonists, beta-blockers, and neurotoxins, can help to reduce the severity of future migraines, prevent migraines from occurring, or both. Preventive treatments are believed to benefit 4 in 10 patients with migraine and almost all patients with chronic migraine, but as few as 3 of every 100 patients eligible for preventive treatment will receive it (3%–13%).12,13 Furthermore, of those who initiate preventive treatment, up to half will either switch medications or discontinue treatment within 2 months.14,15
Preventive-treatment failure can happen due to lack of efficacy, tolerability concerns, or side effects, among other reasons, and is correlated with greater health and economic burden for patients, including worse HRQoL, greater depression and anxiety, and higher medical costs and health care resource use (HCRU).9,16,17 Additionally, a recent study showed that European adults who experience preventive-treatment failures report significantly greater impact on HRQoL, work productivity, and functioning. 18 Another recent study showed that among American adults with episodic migraines who were taking preventive treatments, those who failed prior preventive treatments had greater disease burden than those who had never taken preventive treatments. 19 However, data are limited on the impact of preventive-treatment failure on outcomes for US patients with chronic migraine who are no longer on preventive therapy. This cross-sectional study aimed to expand prior research by assessing the incremental patient-reported health and economic burden associated with increasing preventive-treatment failures compared to those who were never treated with preventive medicines among US adults with diagnosed migraine, which can facilitate a better understanding of unmet needs in this patient population.
Methods
Study design
A retrospective, cross-sectional study was conducted by using data from the 2023 US National Health and Wellness Survey (NHWS). The Pearl Institutional Review Board (Indianapolis, IN, USA) granted exemption status for this study.
Data source
The NHWS is an annual, self-reported survey of the US adult (aged ≥18 years) general population. Participants completed the survey online, answering not only a core set of questions about demographics and general health but also a set of expanded questions tailored to any self-reported disease from a predefined list of conditions. For example, participants who reported having migraines (one of the prespecified conditions) in the core section also answered other questions about their migraines in the expanded section. To ensure that the NWHS sample was representative of the adult US population, participants were recruited via a quota sampling approach to mirror the US general adult population distribution for age, sex, and race/ethnicity in the US Census.
Study population
Out of the total 75,002 total NHWS participants, eligibility criteria included those who reported being diagnosed with migraine by a physician (n = 8,439); had either at least 4 monthly migraine days (MMDs) or at least 4 monthly headache days (MHDs; n = 3,998); and had previously or were currently treated with a prescription migraine medication (n = 3,101). Last, participants who (1) were currently on preventive migraine medication (n = 738), (2) had 0 preventive-treatment failure (n = 707), or (3) were missing for marital status, body mass index, or time since migraine diagnosis (n = 99) were excluded from the analysis, resulting in a final sample of 1,557 participants.
Demographics and health characteristics
The core module of the NHWS comprises questions about participant demographics (i.e., age, sex, gender, race/ethnicity, education, income, insurance type, marital status) and overall health (i.e., alcohol use, body mass index, exercise habits, smoking status, comorbidities). Self-reported comorbidities were used to calculate Charlson Comorbidity Index (CCI) scores to predict burden of comorbid conditions and mortality. 20 The extended, migraine-specific survey section also includes time since physician diagnosis of migraine.
Comparison groups
To evaluate the incremental burden associated with failure of past migraine preventive medicines, participants were categorized as “prevention-naïve” (never treated with preventive medicines; n = 779), “1 failure” (n = 373), or “≥2 failures” (n = 504), based on number of self-reported failure due to nonresponse to preventive medication. Participants who were missing data for marital status, body mass index, and time since migraine diagnosis were excluded from the inverse probability of treatment weighting (IPTW; Figure 1).
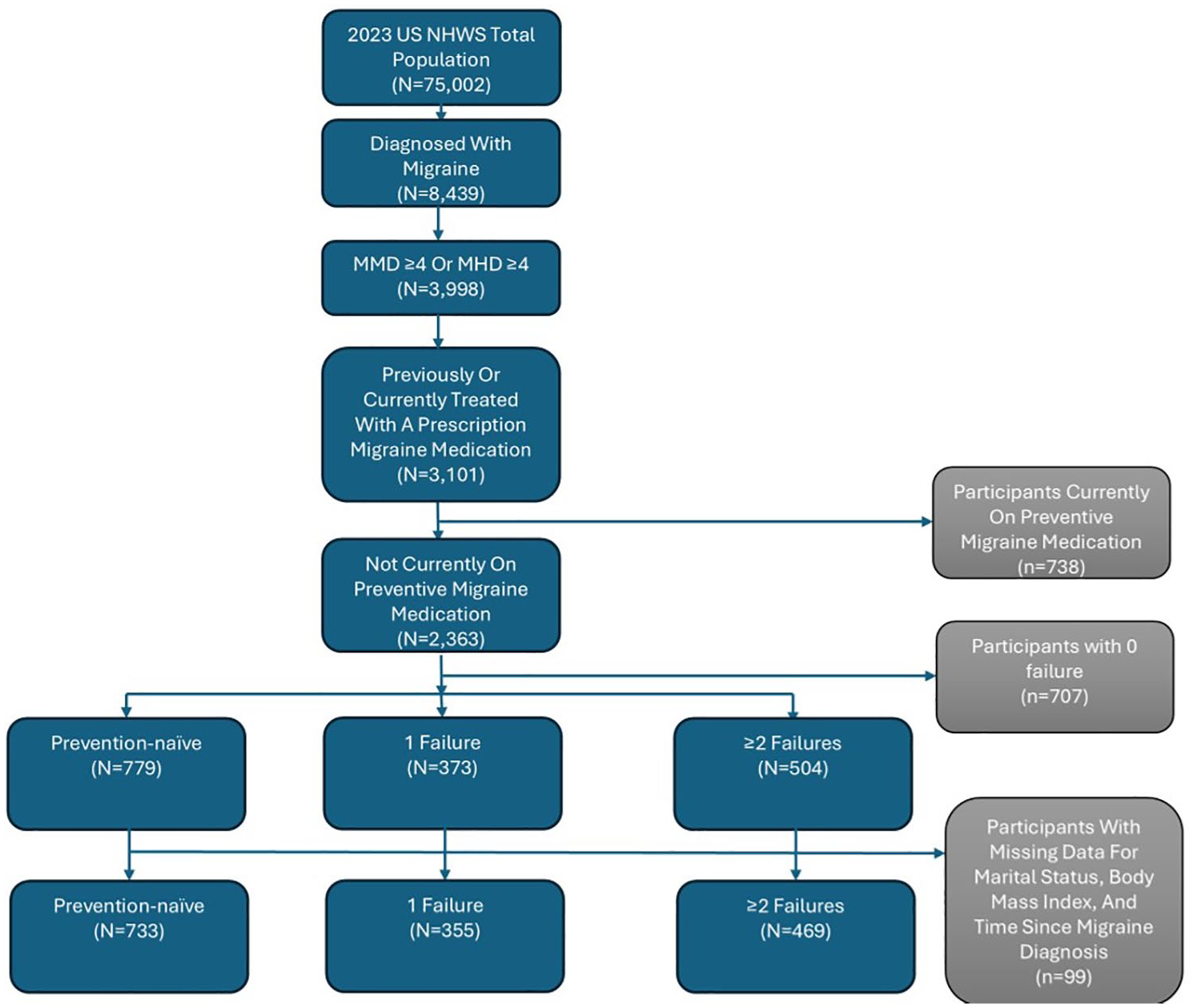
Flow chart of sample selection.
Outcomes
HRQoL and functional impairment
HRQoL and functional impairment outcomes included both migraine-burden characteristics (scores from the Migraine Disability Assessment, MIDAS); whether or not the participant experienced migraine related to menstrual cycle; scores from the 36-Item Short Form Survey Instrument, RAND-36; 5-Level EuroQoL instrument, EQ-5D-5L; the Work Productivity and Activity Impairment General Health version, WPAI-GH; the 9-Item Patient Health Questionnaire, PHQ-9; and the 7-Item Generalized Anxiety Disorder scale, GAD-7.
The MIDAS questionnaire evaluates headache-related disability and is commonly used as a scale of migraine severity. MIDAS measures the impact of headaches among five key dimensions (numbers of days absent from work or school activities; number of days less productive at work or school; numbers of days unable to do household activities; number of days less productive at doing household activities; number of days unable to participate in social, family, or leisure activities). 21 Impact of headaches on each dimension are scored as “no or minimal disability” (score, 0–5); “mild disability” (6–10); “moderate disability” (11–20); or “severe disability” (>20). The MIDAS also uses a 10-point visual analog scale (VAS) to measure frequencies and intensities of headaches, ranging from “no pain” to “pain as bad as it can be.” Scores for these dimensions and the VAS pain score were reported.
RAND-36 is a generic questionnaire that measures overall HRQoL. 22 Global, Physical, and Mental Health Composite (GHC, PHC, MHC) scores are transformed into scores ranging from 0 to 100 (mean, 50; standard deviation (SD), 10). EQ-5D-5L is a generic questionnaire that measures overall HRQoL by describing five key dimensions (anxiety and depression, mobility, pain and discomfort, self-care, and usual activities), each with a 5-point scale. 23 Ratings on the five dimensions are used to derive the EQ-5D index score. The EQ-5D-5L also measures overall HRQoL by presenting respondents with a VAS, ranging from “worst-imaginable” to “best-imaginable” health states. Both EQ-5D index scores and VAS scores were reported. The WPAI-GH measures how overall health affects work productivity and daily activities by using four metrics: absenteeism, presenteeism, overall work productivity impairment, and activity impairment. 24 For each metric, scores are expressed as the mean percentage of impairment in the past 7 days with higher numbers indicating greater impairment and less productivity. PHQ-9 was used to assess depressive symptom severity 25 by measuring each sign on a 4-point scale, from 0 (“none”) to 3 (“almost daily”). PHQ-9 scores can range from 0 to 27, with scores of 0–4 indicating no depressive symptoms; 5–9, mild depressive symptoms; 10–14, moderate depressive symptoms; 15–19, moderate-to-severe depressive symptoms; and 20–27, severe depressive symptoms. Scores ≥10 indicate a positive screen for depression. The GAD-7 was used to assess anxiety symptom severity. 26 Ratings on the seven items are summed, yielding a score that ranges from 0 to 21. GAD-7 scores of 0–4 indicate no anxiety symptoms; 5–9, mild anxiety symptoms; 10–14, moderate anxiety symptoms; and 15–21, severe anxiety symptoms. Scores ≥10 indicate a positive anxiety screen.
Medication use
Patients were asked about their use of migraine medications, including whether they were on prescription medications or over-the-counter (OTC) medications. For prescription medications, they selected from a prompted list, and for OTC medications, they provided the names in an open text question. Medications were also identified from medication-use questions in all pain-related disease modules to which patients responded. Migraine prescribed and OTC medications for acute use are listed in Supplemental Table 2. In addition, medication overuse (including migraine-specific medications and all medications) was defined as taking ergots, triptans, opioids, or combinations for more than 10 days, or taking analgesics or NSAIDs for more than 15 days over the past month. 27 Medication use data from the past month was used as past 3 months data were not available.
Health care resource use
HCRU was reported as the proportion of participants who had any hospitalizations, neurologist visits, and emergency room (ER) visits, as well as the number of hospitalizations, general practitioner or family practitioner visits, neurologist visits, health care provider (HCP) visits, and ER visits over the past 6 months because of personal health. The average number of visits among those who had any visits was also reported for hospitalization, neurologist visit, and ER visit.
Statistical methods
IPTW was conducted to adjust for potential confounding due to differences in participants’ likelihood of preventive treatment use. Participants missing for marital status, body mass index, and time since migraine diagnosis (n = 99) were removed before IPTW (Figure 1). Weights were estimated by multinomial logistic regression using all the previously identified demographics and health characteristics in the model. Stabilized weights were used to address extreme weight values. To verify that distributions of demographics and health characteristics were balanced between groups, distributions of covariates were assessed both before and after weighting. Means and SDs were reported for continuous variables, and numbers and percentages were reported for categorical variables. Standardized mean differences (SMDs), reflecting the difference in means between groups in SD units among the prevention-naïve group and the two treatment-failure groups (1 failure, ≥2 failures), were also compared. An SMD of <0.1 is considered a negligible imbalance between groups. 28
HRQoL, HCRU, and medication use for categories of patients with different numbers of treatment failures were compared after weighting by using two-sided two-sample t-tests or Chi-square tests, setting alpha at 0.05.
Manuscript preparation
STROBE guidelines, for cross-sectional studies, were consulted when preparing the manuscript (Supplemental Checklist 1).
Results
From the NHWS dataset, 1557 participants were included in analyses: prevention-naïve participants, 733; participants with 1 previous preventive treatment failure, 355; and participants with ≥2 previous preventive treatment failures, 469 (Figure 1). Before weighting, participants with preventive medication failure were more likely than prevention-naïve participants to be in the 30–49 age group (1 and ≥2 prevention failures: 53% and 45%, respectively, vs prevention treatment naïve: 38%), but they were less likely to be aged <30 or >49 years and more likely to be male (1 and ≥2 prevention failures: 24% and 30%, respectively, vs prevention treatment naïve: 21%); participants with preventive medication failure were more likely to be Black (17.2% and 14.1% vs 12.4%), married or living with a partner (55.8% and 58.4% vs 53.2%), have an annual household income above the median (38.6% and 43.1% vs 34.5%), be employed (67.9% and 63.1% vs 60.4%), and be current smokers (29.0% and 29.6% vs 21.8%) than prevention-naïve participants. The average time since migraine diagnosis was similar by number of treatment failures (prevention treatment naïve, 16.0 years; 1 and ≥2 prevention failures: 15.2 and 16.5 years). After weighting, all SMDs were <0.1, indicating that the distribution of covariates was well balanced between comparison groups (Table 1 and Supplemental Table 1).
Demographics and clinical characteristics by number of preventive treatment failures (before IPTW).

BMI, body mass index; FT, full-time; IPTW, inverse probability of treatment weighting; PT, part-time; SE, self-employed; SMD, standardized mean differences.
Comparison of outcomes in weighted group
HRQoL and functional impairment
On average, patients with ≥2 treatment failures (7.8 ± 7.5 days, p < 0.001) and patients with 1 failure (6.7 ± 6.2 days, p = 0.041) had significantly more MMDs than prevention-naïve patients (5.9 ± 6.0 days). Patients with ≥2 treatment failures had significantly more MHDs (11.7 ± 7.9 days) than did prevention-naïve patients (9.6 ± 7.2 days, p < 0.001). However, the number of MHDs for patients with one treatment failure (10.4 ± 7.2 days) did not significantly differ from that for prevention-naïve patients. The average MIDAS score for patients with ≥2 treatment failures (35.4 ± 42.4, p < 0.001) was significantly higher than that for prevention-naïve patients (25.5 ± 35.5). The average PHQ-9 score for patients with ≥2 treatment failures (10.7 ± 7.0, p < 0.001) and patients with 1 treatment failure (9.7 ± 6.8, p = 0.025) was significantly higher than that for prevention-naïve patients (8.7 ± 7.2). The average GAD-7 score for patients with ≥2 treatment failures (8.6 ± 6.0) was significantly higher than that for prevention-naïve patients (7.4 ± 6.2, p = 0.001). The average RAND-36 GHC, PHC, and MHC scores for patients with ≥2 treatment failures (34.4 ± 11.6, 38.3 ± 11.0, and 34.6 ± 11.7, respectively) were significantly lower than those for prevention-naïve patients (37.2 ± 12.2, 41.4 ± 11.3, and 36.6 ± 12.5, respectively; all p ⩽ 0.005). Similarly, the average EQ-5D score for patients with ≥2 treatment failures (0.69 ± 0.20) was significantly lower than that for prevention-naïve patients (0.73 ± 0.17). No significant differences between patients with one failure and prevention-naïve patients were observed for GAD-7, RAND-36 GHC, PHC, and MHC, and EQ-5D scores (Table 2).
Patient self-reported migraine burden by number of preventive treatment failures.

Compared with treatment naïve. Results are based on the study sample after inverse probability of treatment weighting. p Values are derived from t test (continuous) and Chi-square test (categorical).
Female patients only.
EQ-5D, 5-level EuroQoL instrument; GAD-7, the 7-Item Generalized Anxiety Disorder scale; GHC, global health composite score; MHC, mental health composite score; MIDAS, the Migraine Disability Assessment; PHC, physical health composite score; PHQ-9, the 9-Item Patient Health Questionnaire; RAND-36, 36-Item Short Form Survey Instrument; SD, standard deviation.
Impact on work productivity and nonwork activities for patients with ≥2 treatment failures was significantly higher than the impact on prevention-naïve patients (absenteeism: 18.6% vs 10.9%; presenteeism: 39.1% vs 31.5%; overall work productivity loss: 45.9% vs 34.9%; and activity impairment: 46.8% vs 36.7%, respectively; p < 0.001 for all). Impact on patients with 1 treatment failure was less than it was for patients with ≥2 failures (absenteeism, 15.1%, p = 0.034; presenteeism, 36.2%, p = 0.042; overall work productivity loss, 41.0%, p = 0.019; activity impairment, 42.6%, p = 0.002), but still significantly higher than for prevention-naïve patients (Table 2).
Migraine-related treatment use
The prescribed medications for acute treatment most commonly used by prevention-naïve patients were triptans (31.2%), combination analgesics (27.3%), and NSAIDs (20.9%); for those with 1 treatment failure, triptans (21.9%), combination analgesics (14.4%), and NSAIDs (11.6%); and for those with ≥2 treatment failures, triptans (20.4%), combination analgesics (15.5%), and opioids (15.0%). The OTC for acute treatment most commonly used across all three groups were analgesics (23.3%–25.5%) and NSAIDS (20.0%–23.6%) as sole ingredients, followed by analgesics with other combinations (14.8%–18.5%). Migraine-specific medication overuse and overall medication overuse by patients with any treatment failures (34.4%–39.7% and 59.2%–61.6%, respectively) and prevention-naïve patients (39.3% and 62.3%, respectively) were similar (Figures 2 and 3 and Supplemental Table 2).

Bar chart of prescribed medications for acute treatment use by preventive-treatment failure.

Bar chart of over-the-counter acute treatment use by preventive-treatment failure.
Health care resource use
Patients with ≥2 preventive treatment failures had substantially greater HCRU than prevention-naïve patients. The percentage of patients with ≥2 treatment failures who had ≥1 ER visit, hospitalization, and neurologist visit (37.0%, 23.5%, and 17.6%, respectively) in the past 6 months were significantly greater than those of prevention-naïve patients (25.2%, p < 0.001; 12.3%, p < 0.001; and 10.9%, p = 0.001, respectively). Among the patients with at least 1 ER visit, the mean number of ER visits was significantly higher in the ≥2 treatment failure group than in the prevention treatment-naïve group (2.6 vs 2.0, p = 0.01). However, the differences in average number of hospitalization and neurologist visits were not statistically significant between the two groups. The percentage of patients in the one treatment failure group who visited the ER in the past 6 months (32.3%, p = 0.017) and the percentage who had been hospitalized in the past 6 months (19.1%, p = 0.004) were also significantly greater than those for prevention-naïve patients (Table 3).
Patient self-reported health care resource utilization by number of prevention failures.

Compared with treatment naïve, results are based on the study sample after inverse probability of treatment weighting. p Values are derived from t test (continuous) and Chi-square test (categorical).
For participants who had any ER visits only.
For participants who had any hospitalizations only.
For participants who had any neurologist visits only.
ER, emergency room; SD, standard deviation.
Discussion
This retrospective analysis evaluated the burden associated with preventive treatment failures among US adults with frequent migraines (at least four MMDs or MHDs), as prior research suggests these individuals may have substantial unmet needs. 17 In the current study, patients who had failed preventive treatments had greater disease burden than did the prevention-naïve patients by several key measures. Furthermore, the magnitudes of effect sizes suggest that patients who had failed multiple preventive treatments had greater burden than did patients who had failed only one, although the significance of the differences between these groups was not tested. Hence, these results revealed an incremental negative impact of increasing preventive treatment failures on patient-reported outcomes, highlighting the important need for better access to medications that prevent migraines and reduce the likelihood of treatment failures, consistent with the recently updated consensus statement by the American Headache Society. 29
Although patient characteristics in the compared groups were similar after weighting (i.e., average age, time since migraine diagnoses, and sex ratios), patients who had failed ≥2 preventive treatments reported poorer HRQoL (higher MIDAS scores, more MHDs, more MMDs) and greater work productivity loss, nonwork activity impairment, and HCRU than prevention-naïve patients. Patients who failed one treatment did not differ from prevention-naïve patients in some respects (i.e., number of MHDs, number of neurologist visits). Patients who failed 1 treatment had better outcomes than those who had failed ≥2 treatments, suggesting that the number of preventive-treatment failures generally scaled with disease burden, although the significance of differences was not tested between the two groups.
These results are consistent with earlier studies on the relationship between migraine-specific disease burden and number of treatment failures among European patients. For example, a prior real-world study conducted with NHWS data from five European countries found that patients who had failed at least two preventive medications reported greater functional impairment, worse physical and mental health, poorer work performance (i.e., higher absenteeism), and greater HCRU (i.e., more ER visits and hospitalizations) than prevention-naïve patients. 18 A second study of patients at specialized headache centers in 17 European countries (from the burden of migraine in specialist headache centers treating patients with prophylactic treatment failure (BECOME) study) assessed how disease burden varied by both MMDs and number of treatment failures. 16 In that study, both MMDs and the number of treatment failures were associated with psychiatric comorbidities, impaired ability to partake in daily activities, and having at least moderate pain or discomfort. Within certain subgroups of patients, increases in the number of treatment failures were associated with greater burden (i.e., effects on daily activities, social activities, work-related activities, and emotional function) and HCRU (i.e., proportion of patients who visited neurologists or emergency departments, proportions of patients with comorbidities, and the number of comorbidities). Thus, the collective evidence suggests that experiencing treatment failures is associated with greater disease burden and HCRU among patients with high frequencies of migraines. One limitation of these results was that migraine criteria and workplace habits in Europe often differ from those in the United States.1,9
Of US participants with at least four MMDs in the global My Migraine Voice Study, those with at least two earlier treatment failures had the greatest disease burden, having the most disrupted daily routines, work life, and finances. 9 Patients with at least two earlier treatment failures had an especially high emotional burden: being most afraid of their next migraine episode, needing the greatest help with daily activities, and having the most trouble sleeping because of migraines. In other studies, US NHWS respondents who reported at least four MHDs and had failed at least two preventive medicines had the greatest HCRU. 30 These studies therefore also indicate that US patients with migraine prevention treatment failure experienced greater health and economic burdens.
The results of this analysis showed that in general, patients who failed preventive treatments had similar risks of medication overuse compared with prevention-naïve patients. In contrast, some earlier studies found that patients who failed multiple preventive treatments (or who continued to fail such treatments) used acute medications significantly more often than those who did not, possibly because these patients depended on acute medicines for relief, which may suggest greater risk of medication overuse.15,31 –33 These discrepant results may be due to the inclusion criteria applied in this study, which required patients to have been previously or currently treated with a prescription migraine medication. As a result, prevention-naïve patients had to have received in the past or be currently receiving acute treatment to be eligible for the study. Future studies comparing medication overuse among patients who failed preventive treatments versus prevention-naïve patients, without this inclusion criterion, are needed to provide further insights into the relationship between medication overuse and preventive-treatment failure.
The differing characteristics of participants across the comparison groups before weighting suggest that preventive treatment failure may be associated with demographics, socioeconomic status, and health behaviors. Middle-aged patients (30–49 years), males, Black individuals, those with private insurance, and those with a household income above the median were more likely to experience preventive treatment failure. Additionally, current smokers were more likely to experience treatment failure compared to nonsmokers. These findings should be confirmed by future studies using statistical models to assess which patient characteristics may contribute to treatment preventive failure.
This study adds to the literature by providing more granular details about disease burden for US patients with migraine who failed prevention treatments. We measured how number of treatment failures relate to HRQoL, HCRU, comorbidities, and acute and medication use. Few studies have addressed all these variables specifically for US patients.15,17 And compared with earlier US-based studies, we examined a larger, more-representative cohort and described in more detail both medication use (numbers and types of OTC, prescription, acute, and preventive medicines) and HCRU (numbers and types of doctor and hospital visits).9,14,31,34
These added details highlight the negative effects of ineffective preventive treatments on migraine patients’ HRQoL, work productivity and non-work activities, and HCRU. Some evidence suggests that patients with migraine adhere to and benefit more from certain preventive medicines (i.e., CGRP, neurotoxins, calcium channel blockers, and angiotension receptor blockers).15,35 These drugs may even help patients who failed a substantial number of other preventive treatments (over four), as has been demonstrated for some CGRPs. For example, US patients with migraine who had failed many other medicines did not fail fremanezumab, and fremanezumab treatment was associated with better work and daily functioning. 35 Additionally, the oral CGRP rimegepant improves HRQoL for patients who failed other preventive treatments. 36 Atogepant also reduced mean MMDs in patients with episodic migraine who had previously been failed by two to four classes of conventional oral preventive treatments. 37
The current study had several limitations. All data were self-reported; thus, some patients may have incorrectly recalled information or changed their answers to match what they considered more socially acceptable (social desirability bias). Second, these data were gathered through an online survey; thus, the dataset may underrepresent segments of the US population with less access to the internet (sampling bias). Third, this study was a cross-sectional analysis; thus, it does not offer insight into causation, only association. Future work may address these points. Lastly, missing data was removed from the study, which may introduce selection bias if those with missing values differ from those who remained in the analysis. However, the number of participants with missing data was relatively small, and it was unlikely to significantly affect the results.
Conclusion
In summary, results show similar risks of medication overuse, poorer HRQoL, and greater work productivity loss, activity impairment, and HCRU among US adults with migraine who failed preventive medications compared with those who did not have prior preventive failure. These observations are especially pronounced for adults who failed more than two mediciations, highlighting these patients’ critical unmet needs for earlier intervention and optimal migraine preventive treatment.
Supplemental Material
sj-docx-1-tan-10.1177_17562864251337431 – Supplemental material for Measuring incremental burdens associated with increasing preventive-treatment failures among adults with migraine: a retrospective, cross-sectional study
Supplemental material, sj-docx-1-tan-10.1177_17562864251337431 for Measuring incremental burdens associated with increasing preventive-treatment failures among adults with migraine: a retrospective, cross-sectional study by Jessica Ailani, Nemin Chen, Avani Patel, Nathan Spence, Nikoletta Sternbach, Katie B. Tellor, Motomori Lewis and Joshua Brown in Therapeutic Advances in Neurological Disorders
Supplemental Material
sj-docx-2-tan-10.1177_17562864251337431 – Supplemental material for Measuring incremental burdens associated with increasing preventive-treatment failures among adults with migraine: a retrospective, cross-sectional study
Supplemental material, sj-docx-2-tan-10.1177_17562864251337431 for Measuring incremental burdens associated with increasing preventive-treatment failures among adults with migraine: a retrospective, cross-sectional study by Jessica Ailani, Nemin Chen, Avani Patel, Nathan Spence, Nikoletta Sternbach, Katie B. Tellor, Motomori Lewis and Joshua Brown in Therapeutic Advances in Neurological Disorders
Footnotes
Appendix
Acknowledgements
The authors would like to thank Martine Maculaitis, PhD, Oracle Life Sciences, Austin, TX, USA, and Sheila Drakeley, MPH, Oracle Life Sciences, Austin, TX, USA. Medical writing support was provided by Sumit Borah, PhD, at Oxford Square Scientific and Medical Writing Services and was funded by Pfizer.
Declarations
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
