Abstract
Background:
Balloon pulmonary angioplasty (BPA) is typically performed in a sequential manner.
Objectives:
This study aimed to determine the lowest frequency of BPA for patients who could not reach treatment goals in a short period.
Design:
Retrospective cohort.
Methods:
We retrospectively enrolled 186 BPA-treated patients diagnosed with chronic thromboembolic pulmonary hypertension. According to the accumulative number of performed BPA sessions or treated pulmonary vessels or the ratio of the number of treated pulmonary vessels/the number of baseline lesions (T/P) prior to the initial occurrence of clinical outcome or censored date, we divided patients into different groups. The principal outcome was clinical worsening.
Results:
After stratifying patients by the number of performed BPA sessions, most baseline parameters were comparable among groups. During follow-up, 31 (16.7%) of 186 patients experienced clinical worsening. The 6-month cumulative clinical worsening-free survival rates of ⩾2 performed sessions group were significantly higher than that of 1 performed session group. The 12-month cumulative rates of clinical worsening-free survival exhibited a declining pattern in the subsequent sequence: ⩾3, 2, and 1 performed BPA sessions, and this trend persisted when follow-up time exceeded 12 months. The 6-, 12-, and 24-month cumulative clinical worsening-free survival rates were comparable between patients with 3 and ⩾4 performed BPA sessions. Similar results were also observed when stratifying patients by the accumulative number of treated pulmonary vessels (⩽8, 9–16, ⩾17) and T/P (⩽0.789, 0.790–1.263, ⩾1.264).
Conclusion:
To achieve optimal short-term outcomes, patients might need to undergo ⩾2 BPA sessions or have ⩾9 pulmonary vessels treated or have T/P ⩾0.790 within 6 months, and undergo ⩾3 BPA sessions or have ⩾17 pulmonary vessels treated or have T/P ⩾1.264 within 12 months.
Plain language summary
Why was the study done? Balloon pulmonary angioplasty (BPA) has been recommended for patients with chronic thromboembolic pulmonary hypertension, which can significantly improve patients’ hemodynamics. However, BPA is typically performed in a stepwise manner, and the duration from the initial session to the final session could extend over a year. If patients could not quickly undergo adequate number of BPA sessions and reach hemodynamic target due to various reasons, what is the best frequency of BPA for them? What did the researchers do? We retrospectively enrolled 186 BPA-treated patients diagnosed with chronic thromboembolic pulmonary hypertension. According to the accumulative number of BPA sessions, we divided patients into different groups to identify the best frequency of BPA to improve prognosis. What did the researchers find? Patients who received at least two BPA sessions within six months had significantly better prognosis than those with one BPA session. Patients who received at least three BPA sessions within a year had significantly better prognosis than those with two BPA sessions. What do the findings mean? To achieve optimal short-term outcome, patients might need to undergo at least two BPA sessions within six months, and undergo at least three BPA sessions within a year.
Keywords
Introduction
Chronic thromboembolic pulmonary hypertension (CTEPH) is the only potentially curable cause of pulmonary hypertension, which is featured by chronic thromboembolic obstruction of the pulmonary arteries and concomitant microscopic vasculopathy in non-occluded areas. Pulmonary endarterectomy (PEA) is the preferred therapeutic strategy for patients with surgically accessible lesions. For inoperable patients or those with residual pulmonary hypertension after PEA, balloon pulmonary angioplasty (BPA) has been recommended by current guidelines, which could significantly improve and even normalize patients’ hemodynamics. 1
To mitigate the potential for complications, BPA is typically executed in a stepwise manner, wherein a restricted number of pulmonary vessels is addressed during each session. An estimated range of 3–10 sessions is necessitated to attain hemodynamic outcomes that meet the desired criteria.2,3 There is no consensus on how often BPA should be performed. The temporal gap between two successive BPA sessions has been documented to vary between 1 and 8 weeks,4–7 and it is conceivable that the duration from the initial session to the concluding session could extend beyond 12 months. 8 It should be stressed that most published BPA-related articles came from developed countries before the outbreak of COVID-19.2,9 The annual hospital and medication costs for BPA-treated patients could exceed 30,000 euros. 10 Therefore, the lengthy BPA process could be further prolonged due to strained medical resources during the COVID-19 pandemic (for both developed and developing countries) and limited healthcare budgets (for developing countries). This leads to a crucial question: If patients cannot quickly undergo an adequate number of BPA sessions and reach hemodynamic targets due to various reasons, what is the best frequency of BPA for them? The primary purpose of the study is to determine whether a greater number of BPA sessions or treated vessels is associated with a lower risk of clinical worsening. We also aim to perform sensitivity analysis to corroborate the principal findings through patient stratification based on baseline severity, the implementation of more stringent outcome criteria, or restriction to patients with extended follow-up periods. Moreover, we try to determine the association between the frequency of BPA and the clinical outcome in the exploratory analysis.
Materials and methods
Study design and participants
We conducted a retrospective examination of the medical records of all patients diagnosed with CTEPH who underwent BPA treatment between May 2018 and December 2021 at Fuwai Hospital. The diagnosis of CTEPH was in line with the 2015 version of European guidelines. 11 The evaluation of suitability for BPA was collaboratively conducted by a multidisciplinary team of experts specializing in CTEPH, encompassing surgeons experienced in PEA, radiologists specialized in pulmonary hypertension, and pulmonary hypertension specialists. The subsequent patients were omitted from the present investigation: (1) procedure-related in-hospital death during the first BPA session; (2) no follow-up; and (3) receiving PEA during the follow-up period. The reporting of this study conforms to the Strengthening the Reporting of Observational Studies in Epidemiology statement 12 (Supplemental Material).
Balloon pulmonary angioplasty
BPA was executed in accordance with the methodology detailed in our prior description 13 and the details are in Supplemental Methods. Prior to the initiation of each BPA session, an initial right heart catheterization was conducted to assess the baseline hemodynamic parameters. Subsequently, a pulmonary angiography procedure was undertaken to obtain a comprehensive visualization of the filling defects. Utilizing selective pulmonary angiography as a guide, a 0.014-inch guidewire was advanced through the chosen lesion. Following this, an adequately sized balloon was cautiously inflated, with careful consideration of vessel dimensions as well as balloon performance. Hemodynamic assessments were reiterated upon the conclusion of each BPA session. The patient’s clinical status, including World Health Organization function class, 1 6-minute walk distance, and NT-proBNP, was assessed within 7 days prior to and after each BPA session.
Follow-up and clinical outcome
After discharge, follow-up was routinely performed via telephonic communication or outpatient or inpatient clinical evaluations. The principal outcome event was clinical worsening, including mortality, unforeseen hospitalization associated with PH, unsatisfactory long-term clinical response (NT-proBNP increased by 100% or to ⩾1800 ng/L from baseline to follow-up),14,15 and appearance or worsening of signs/symptoms of right heart failure. 16 The temporal interval to the onset of clinical deterioration events was calculated as the duration elapsed from the initiation of the BPA to the earliest manifestation of clinical worsening or censored date (31 June 2022). Two experienced PH experts independently (QL and QZ) assessed and verified the cases to ensure objectivity and reliability in the evaluation of this composite endpoint. Two supervisors adjudicated the results (ZZ and ZL). Disagreements were resolved by team consensus.
Patient stratification
To provide a comprehensive analysis, we used three ways to classify patients, including BPA sessions, number of treated vessels, and proportion of treated vessels. (1) According to the accumulative number of performed BPA sessions prior to the initial manifestation of clinical worsening or censored date, we divided patients into three groups, namely 1, 2, and ⩾3. (2) According to the accumulative number of treated pulmonary vessels, we divided patients into three groups, namely ⩽8, 9–16, and ⩾17. (3) We also divided patients based on the ratio of the number of treated pulmonary vessels/the number of baseline lesions (T/P), namely ⩽0.789 (⩽25th percentile), 0.790–1.263 (26th–50th percentiles), and ⩾1.264 (⩾51st percentile). BPA is a quite complex procedure and some lesions might be treated more than once. In terms of patients’ response, it might be different between dilating two pulmonary vessels and dilating one pulmonary vessel twice. Given its simplicity, we suggested using T/P to roughly reflect the accumulative effect of BPA procedure on patients and to facilitate clinical utility.
The cutoff values for the number of treated pulmonary vessels and T/P were based on our preliminary study (Supplemental Figures S1 and S2). It should be stressed that the occurrence of clinical outcomes only means ending the observation of patients in the present study instead of permanent termination of the BPA procedure.
Statistical analysis
Continuous parameters are presented as either the mean ± standard deviation or the median with the interquartile range. Categorical parameters are represented in terms of counts and their respective percentages. Group comparisons were conducted using one-way analysis of variance, Kruskal–Wallis tests, or the chi-square test, depending on the nature of the data. Kaplan–Meier survival curve analysis, in conjunction with the log-rank test, was employed to assess disparities in survival outcomes among patient subgroups. The associations between clinical worsening and the number of BPA sessions or the number of treated vessels or T/P were determined using Cox regression models. Covariates demonstrating a significance level of p < 0.05 in univariable analysis or those of notable clinical relevance were chosen for inclusion in the multivariable Cox regression analysis. Not a single missing value was replaced. The main analysis was performed by including all the patients to identify whether a greater number of BPA sessions or treated vessels is associated with a lower risk of clinical worsening. We also performed three sensitive analyses to validate the principal findings: (1) stratifying patients by 6-minute walk distance or mean PAP in the total cohort; (2) excluding the criteria of NT-proBNP from clinical worsening; and (3) including patients with at least 12-month follow-up. We also performed two exploratory analyses to determine the association between the frequency of BPA and the clinical outcome: (1) clinical worsening events occurred in 6 months and (2) clinical worsening events occurred in 12 months. Statistical significance was considered to be present when the two-sided p value was less than 0.05. Data were analyzed using R (version 4.3.1, R Foundation for Statistical Computing, Vienna, Austria).
Results
Patient enrollment
A total of 194 patients with CTEPH received BPA between May 2018 and December 2021. Among them, eight patients were excluded: in-hospital mortality owing to severe reperfusion pulmonary edema during the initial BPA treatment (n = 1); no follow-up data (n = 5), and receiving PEA during the follow-up period (n = 2). Ultimately, 186 patients were included, with a cumulative sum of 548 BPA sessions [median (interquartile range): 4 (3, 5)/per patient] and 4149 pulmonary arteries dilated [median (interquartile range): 29 (18, 38)/per patient]. In the present study, we only counted the number of BPA sessions completed/pulmonary vessels treated before the incidence of clinical worsening or the censored date (31 June 2022). The distribution of indication for BPA was declined to undergo pulmonary endarterectomy (n = 9); persistent PH after pulmonary endarterectomy (n = 2); high risk-to-benefit ratio of PEA (n = 13); and distal lesions (n = 162).
Baseline characteristics
The mean age of all included patients was 59.8 ± 10.8 years and 53.8% were female (Table 1). The median disease duration (from the onset of symptoms to the first BPA session) was 3 (1,7) years. After stratifying patients by the number of BPA sessions (Table 1), the number of treated pulmonary vessels (Supplemental Table S1) and T/P (Supplemental Table S2), most baseline parameters were comparable among groups. Spearman correlation analysis showed that the number of performed BPA sessions was highly correlated with the number of treated pulmonary vessels (r = 0.916, p < 0.001) and T/P (r = 0.786, p < 0.001).
Baseline characteristics of all included patients, stratified by the number of performed BPA sessions.

BPA, balloon pulmonary angioplasty; CI, cardiac index; EF, ejection fraction; LVED, left ventricular end-diastolic diameter; mPAP, mean pulmonary artery pressure; 6MWD, 6-minute walk distance; mRAP, mean right atrial pressure; NT-proBNP, N-terminal pro-brain natriuretic peptide; PAWP, pulmonary artery wedge pressure; PVR, pulmonary vascular resistance; RVED, right ventricular end-diastolic diameter; SvO2, mixed venous oxygen saturation; TRV, tricuspid regurgitation velocity; WHO FC, World Health Organization function class.
Clinical outcome
The median follow-up period was 21.5 (11.8, 35.0) months. Over the course of the follow-up period, 31 (16.7%) of 186 patients manifested clinical worsening: mortality (n = 5), unforeseen hospitalization associated with PH (n = 8), unsatisfactory long-term clinical response (n = 6), and new onset or exacerbation of signs indicative of right ventricular failure (n = 12). According to the last available hemodynamics before the onset of the clinical worsening or censored date (31 June 2022), seven patients reached mPAP <25 mmHg and five of them had oxygen saturation >95%. All these seven patients did not experience clinical worsening.
The cumulative clinical worsening-free survival rates at 1, 2, and 3 years for each stratum have been delineated in Supplemental Table S3, and Figures 1 to 3. The accumulated survival rates free from clinical worsening increased as the number of performed BPA sessions [Figure 1(a)] or the number of treated pulmonary vessels [Figure 2(a)] or T/P [Figure 3(a)] escalated.

Kaplan–Meier survival curves based on the number of performed BPA sessions. (a) The main analysis included all patients. (b) Sensitivity analysis included patients with at least 12-month follow-up data. (c) Explanatory analysis of 6-month clinical worsening-free rates. (d) Explanatory analysis of 12-month clinical worsening-free rates. Please refer to Supplemental Materials for a high-resolution version using the zoom-in function.

Kaplan–Meier survival curves based on the number of treated pulmonary vessels. (a) The main analysis included all patients. (b) Sensitivity analysis included patients with at least 12-month follow-up data. (c) Explanatory analysis of 6-month clinical worsening-free rates. (d) Explanatory analysis of 12-month clinical worsening-free rates. Please refer to Supplemental Materials for a high-resolution version using the zoom-in function.

Kaplan–Meier survival curves based on the ratio of the number of treated pulmonary vessels/number of baseline lesions. (a) The main analysis included all patients. (b) Sensitivity analysis included patients with at least 12-month follow-up data. (c) Explanatory analysis of 6-month clinical worsening-free rates. (d) Explanatory analysis of 12-month clinical worsening-free rates. Please refer to Supplemental Materials for a high-resolution version using the zoom-in function.
Univariable and multivariable Cox analyses showed that the number of performed BPA sessions, the number of treated pulmonary vessels, and T/P were all associated with clinical worsening (Table 2), with the Harrell’s C-index of 0.812, 0.822, and 0.780, respectively (Table 3). These associations remained significant after adjusting for key confounders, including hemodynamics, the anatomic burden, and the distribution of lesions at baseline (Supplemental Tables S4 and S5).
Associations between the number of performed BPA sessions/treated pulmonary vessels and clinical worsening.

Details of adjusted HR are displayed in Supplemental Table S4–S11.
We only count the number of BPA sessions completed/pulmonary vessels treated that happened before the clinical worsening events or the end of follow-up.
Only including patients with at least 12 months of follow-up data.
Only including patients with at least 6 months of follow-up data.
No clinical worsening event happened and HR could not be calculated.
Only including patients with at least 12 months of follow-up data.
BPA, balloon pulmonary angioplasty.
The Harrell’s C-index of the number of performed BPA sessions/treated pulmonary vessels in predicting clinical worsening.
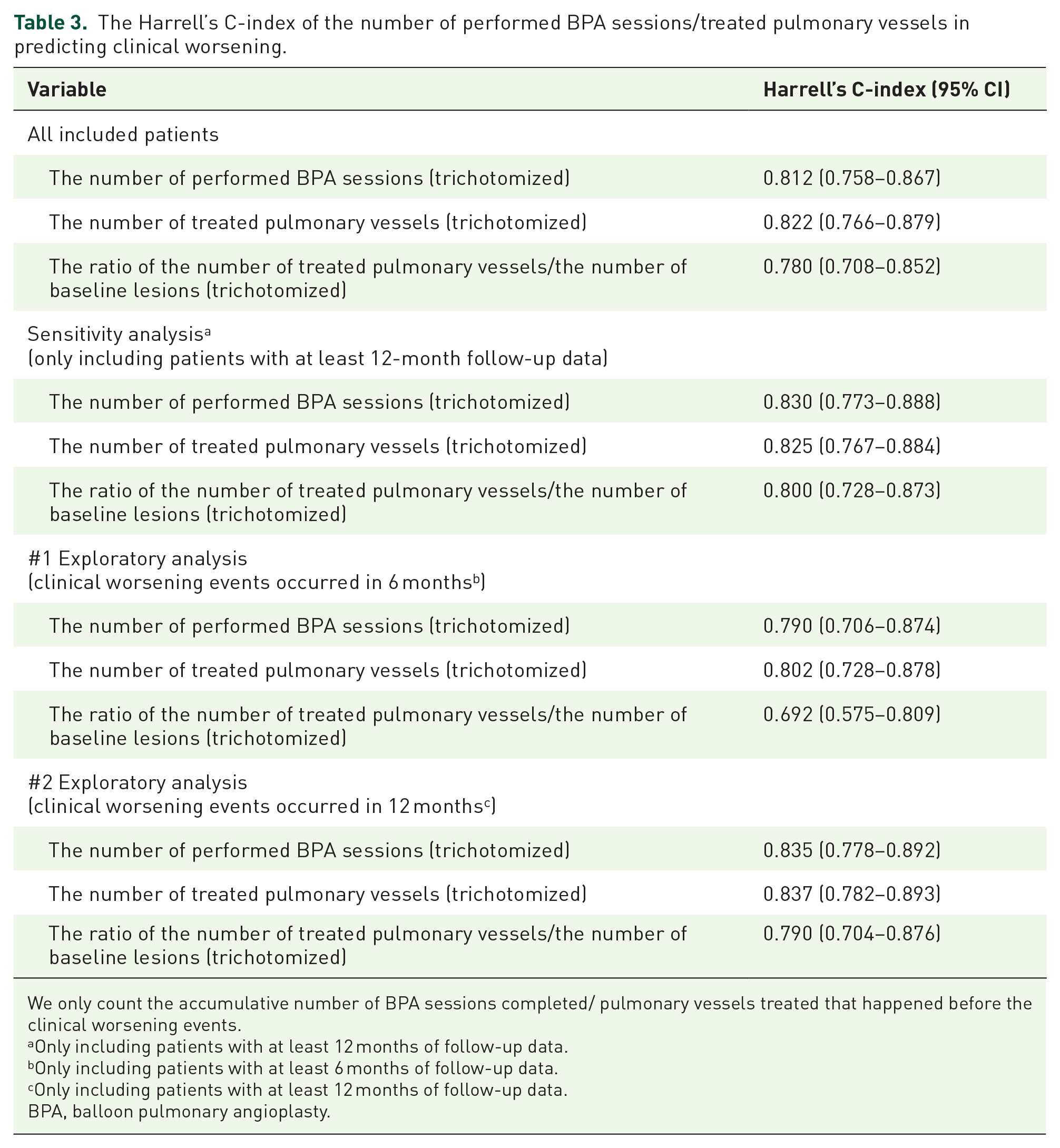
We only count the accumulative number of BPA sessions completed/ pulmonary vessels treated that happened before the clinical worsening events.
Only including patients with at least 12 months of follow-up data.
Only including patients with at least 6 months of follow-up data.
Only including patients with at least 12 months of follow-up data.
BPA, balloon pulmonary angioplasty.
Sensitivity analysis
To validate the robustness of the finding, we also performed three sensitivity analyses. First, we stratified patients by 6-minute walk distance or mean PAP and the subgroup analysis results were consistent with the main analysis (Supplemental Table S6). Second, we excluded the criteria of NT-proBNP from clinical worsening. More BPA sessions treated pulmonary vessels and a higher proportion of T/P were still associated with a lower risk of clinical worsening (Table S7). In the third sensitivity analysis, we only included patients with at least 12-month follow-up data and the findings remained concordant with the primary analysis [Tables 2 and 3, Supplemental Tables S8 and S9 and Figures 1(b)–3(b)].
Exploratory analysis
Clinical worsening occurred within 6 months
In patients with at least 6-month follow-up data, Kaplan–Meier curves showed that the 6-month cumulative clinical worsening-free survival rates of 2 BPA sessions and ⩾3 sessions group were comparable but were significantly higher than that of one session group ([1 versus 2 versus ⩾3 = 80.4% versus 96.3% versus 100%; Figure 1(c)]. It yielded similar results when stratifying patients by the number of treated pulmonary vessels or T/P [Figures 2(c) and 3(c)].
Univariable Cox analysis showed that the number of performed BPA sessions, the number of treated pulmonary vessels, and T/P were all associated with 6-month clinical worsening (Table 2), with the Harrell’s C-index of 0.790, 0.802, and 0.692, respectively (Table 3). These associations remained significant after adjusting for confounders (Supplemental Tables S10 and S11).
Clinical worsening occurred within 12 months
In patients with at least 12-month follow-up data, Kaplan–Meier curves showed that the 12-month accumulated survival rates free from clinical deterioration increased as the number of BPA sessions escalated [1 versus 2 versus ⩾3 = 65.7% versus 87% versus 100%; Figure 1(d)]. It yielded similar results when stratifying patients by the number of treated pulmonary vessels or T/P [Figures 2(d) and 3(d)].
Univariable Cox analysis showed that the number of performed BPA sessions, the number of treated pulmonary vessels, and T/P were correlated with 12-month clinical worsening (Table 2 and Supplemental Table S12), with the Harrell’s Concordance index of 0.835, 0.837, and 0.790, respectively (Table 3). These associations remained significant after adjusting for confounders (Table 2, Supplemental Tables S12 and S13).
Subgroup analysis in ⩾3 BPA sessions, ⩾17 pulmonary vessels, and T/P ⩾1.264 groups
Kaplan–Meier curves showed that 6-, 12-, and 24-month cumulative clinical worsening-free survival rates were comparable between patients undergoing 3 and ⩾4 BPA sessions [Figure 4(a)–(d)], which was also observed between patients with 17–24 and ⩾25 treated vessels (Supplemental Figure S3E–S3H) or patients with T/P 1.264–1.912 and ⩾1.913 (Supplemental Figure S3I–S3L).

Subgroup analysis of Kaplan–Meier survival curves between patients with 3 and ⩾4 performed BPA sessions. It yielded similar results between patients with 17 and 24 and ⩾25 treated pulmonary vessels, or patients with T/P = 1.264–1.912 and ⩾1.913 (Supplemental Figure S3). (a) The main analysis included all patients. (b) Sensitivity analysis included patients with at least 12-month follow-up data. (c) Explanatory analysis of 6-month clinical worsening-free rates in patients with at least 6-month follow-up. (d) Explanatory analysis of 12-month clinical worsening-free rates in patients with at least 12-month follow-up. Please refer to Supplemental Materials for a high-resolution version using the zoom-in function.
BPA complications
According to the number of performed BPA sessions or the number of treated pulmonary vessels or T/P completed within 6 months or 12 months, we divided all included patients into three groups. At the procedure level, the rates of BPA complications were comparable among different groups (Table 4 and Supplemental Table S14–S15). At the patient level, the risk of BPA complications slightly escalated with the increase in the number of performed BPA sessions or the number of treated pulmonary vessels or T/P (Supplemental Table S16–S18, Figure 5 and Supplemental Figure S4). However, most BPA complications were mild (hemoptysis or hemosputum), and no procedure-related death was observed in patients with higher BPA frequency.
Procedure-level analysis of complications, stratified by the number of BPA sessions completed and time interval.

Total number of BPA sessions performed during the study period.
BPA, balloon pulmonary angioplasty.

Patient-level analysis of complications, stratified by the number of performed BPA sessions. It yielded similar results when stratifying patients by the number of treated pulmonary vessels or the ratio of the number of treated pulmonary vessels/the number of baseline lesions (Supplemental Figure S4). Please refer to Supplemental Materials for a high-resolution version using the zoom-in function.
Discussion
BPA is typically performed in a sequential manner, but how often should BPA procedure be performed has not been systematically discussed yet. The main findings of the present study were as follows: (1) ⩾2 performed BPA sessions, ⩾9 treated pulmonary vessels, or T/P ⩾ 0.790 was needed to achieve optimal 6-month clinical worsening-free survival rates; (2) ⩾3 performed BPA sessions, ⩾17 treated pulmonary vessels, or T/P ⩾ 1.264 was needed to achieve optimal 12-month clinical worsening-free survival rates and this trend persisted even when follow-up time exceeded 12 months; (3) short-term clinical worsening-free survival rates were comparable between patients with 3 and ⩾4 performed BPA sessions or patients with 17–24 and ⩾25 treated pulmonary vessels or patient with T/P 1.264–1.912 and ⩾1.913; and (4) although patients with higher frequency of BPA procedure had slightly increased BPA-related complication rates, most complications were mild and no procedure-related death was observed.
The initiation of the BPA procedure does not guarantee event-free survival. The patient’s clinical status is still consistently changing during this lengthy process. Matsubara et al. 17 reported that deteriorated hemodynamics or symptoms were identified in approximately 50% of patients who failed to reach mean pulmonary arterial pressure <25 mmHg and oxygen saturation >95%, which is consistent with our results. Theoretically, the entire BPA procedure should be completed in a limited time to optimize patients’ prognosis. Unfortunately, the definition of “a limited time” is a key unsolved issue. More importantly, several factors could prolong the BPA procedure. In addition to the COVID-19 pandemic and medical costs, the duration of the entire BPA procedure may vary from center to center due to the operator’s expertise and treatment goal. On average, novice BPA operators could treat 2–4 lesions per procedure, while it is 14–16 lesions for experienced ones. 18 Hemodynamic targets like mPAP <30 mmHg or <25 mmHg have been proposed in published articles.19–25 Hug et al. 26 revealed that the hemodynamic improvement would be blunted since the third BPA session. Pursuing complete hemodynamic normalization might require more BPA sessions and a longer treatment duration.
The present study showed that to achieve optimal short-term outcomes, patients should undergo ⩾2 BPA sessions or have ⩾9 pulmonary vessels treated or reach T/P ⩾0.790 within 6 months; undergo ⩾3 BPA sessions or have ⩾17 pulmonary vessels treated or reach T/P ⩾1.264 within 12 months. These results remained statistically significant even after adjusting for key confounding factors such as hemodynamics, the anatomic burden, and the distribution of lesions at baseline. As stated above, the BPA strategy could vary from center to center. However, we offered three different methods of stratifying patients, and the results of these methods showed good consistency. This should reinforce the extrapolation of our conclusions. Although patients undergoing BPA at higher frequency had an increased risk of BPA-related complications, most of the complications were benign and none of them led to in-hospital death. Our results could be used to plan BPA procedures for patients who could not reach treatment goals in a short period, especially in developing countries and start-up BPA centers.
We did not observe significant differences in clinical worsening-free rates between patients with 3 and ⩾4 performed BPA sessions or patients with 17–24 and ⩾25 treated pulmonary vessels or patients with T/P ⩾1.264 and ⩽1.912 and ⩾1.913. However, we do not suggest long-term suspension of the BPA procedure after the third session unless the treatment goal is achieved. Because the comparability between these two groups might be attributed to the short duration of follow-up [median 21.5 (11.8, 35.0) months] and relatively small sample size.
Several strengths of our study are worth noting. First, for the first time, we identified the minimal required BPA frequency to reduce the risk of clinical worsening, which is especially crucial for patients who may not persist with BPA treatment. Second, we performed a series of sensitivity analyses, including stratifying patients based on mPAP and 6MWD, the implementation of more stringent outcome criteria, or restriction to patients with over 12-month follow-up to validate the findings of studies.
Limitations
Our study carries certain limitations. First, this is a single-centered retrospective study. Prospective multi-center studies are warranted. Second, our follow-up time and sample size were relatively small. It remains elusive whether patients with ⩾4 performed BPA sessions or ⩾25 treated pulmonary vessels or T/P ⩾ 1.913 had better clinical outcomes in the long term, compared to those with 3 performed BPA sessions or 17–24 treated pulmonary vessels or T/P ⩾1.264 and ⩽1.912. Third, the quantity of BPA sessions was limited in the current investigation and few patients reached mean pulmonary arterial pressure <25 mmHg and oxygen saturation >95%. The relatively small number of BPA sessions in some patients can be attributed to several factors: (1) limited availability of BPA facilities: in China, BPA procedures are conducted in only a few specialized PH centers, often requiring patients to travel long distances to receive treatment. This inconvenience can deter some patients from continuing BPA after 1–2 sessions, particularly when their symptoms have already been improved; (2) financial constraints: some individuals discontinue BPA treatment owing to financial constraints, particularly as a significant proportion of patients face difficulties in maintaining employment due to the impact of CTEPH; (3) impact of the COVID-19 pandemic: The ongoing COVID-19 pandemic has disrupted healthcare systems worldwide, affecting the continuity of medical treatment. Some patients may have faced challenges in adhering to their BPA treatment schedule due to restrictions and concerns related to the pandemic. These factors collectively contribute to the observed small number of BPA sessions in our patient population. Despite the relatively low BPA sessions, our study provides insights into the least required BPA treatment to reduce clinical worsening, which is especially essential for those who were less likely to adhere to the treatment.
Conclusion
To achieve optimal short-term outcomes, patients might need to undergo ⩾2 BPA sessions or have ⩾9 pulmonary vessels treated or have T/P ⩾0.790 within 6 months, and undergo ⩾3 BPA sessions or have ⩾17 pulmonary vessels treated or have T/P ⩾1.264 within 12 months.
Supplemental Material
sj-docx-1-tar-10.1177_17534666241232521 – Supplemental material for Optimal short-term outcomes in balloon pulmonary angioplasty: the minimum frequency of three sessions annually
Supplemental material, sj-docx-1-tar-10.1177_17534666241232521 for Optimal short-term outcomes in balloon pulmonary angioplasty: the minimum frequency of three sessions annually by Xin Li, Tao Yang, Yi Zhang, Qing Zhao, Qixian Zeng, Qi Jin, Anqi Duan, Zhihua Huang, Meixi Hu, Sicheng Zhang, Luyang Gao, Changming Xiong, Qin Luo, Zhihui Zhao and Zhihong Liu in Therapeutic Advances in Respiratory Disease
Supplemental Material
sj-docx-2-tar-10.1177_17534666241232521 – Supplemental material for Optimal short-term outcomes in balloon pulmonary angioplasty: the minimum frequency of three sessions annually
Supplemental material, sj-docx-2-tar-10.1177_17534666241232521 for Optimal short-term outcomes in balloon pulmonary angioplasty: the minimum frequency of three sessions annually by Xin Li, Tao Yang, Yi Zhang, Qing Zhao, Qixian Zeng, Qi Jin, Anqi Duan, Zhihua Huang, Meixi Hu, Sicheng Zhang, Luyang Gao, Changming Xiong, Qin Luo, Zhihui Zhao and Zhihong Liu in Therapeutic Advances in Respiratory Disease
Supplemental Material
sj-docx-3-tar-10.1177_17534666241232521 – Supplemental material for Optimal short-term outcomes in balloon pulmonary angioplasty: the minimum frequency of three sessions annually
Supplemental material, sj-docx-3-tar-10.1177_17534666241232521 for Optimal short-term outcomes in balloon pulmonary angioplasty: the minimum frequency of three sessions annually by Xin Li, Tao Yang, Yi Zhang, Qing Zhao, Qixian Zeng, Qi Jin, Anqi Duan, Zhihua Huang, Meixi Hu, Sicheng Zhang, Luyang Gao, Changming Xiong, Qin Luo, Zhihui Zhao and Zhihong Liu in Therapeutic Advances in Respiratory Disease
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
