Abstract
Inhaled therapies allow for the targeted delivery of antimicrobials directly into the lungs and have been widely used in the treatment of cystic fibrosis (CF) acute pulmonary exacerbations. Nebulized levofloxacin solution (MP-376) is a novel therapy that is currently being evaluated in phase I, II, and III clinical trials among patients with stable CF and recent isolation of Pseudomonas aeruginosa from sputum. Phase I studies have investigated the single and multiple-dose pharmacokinetics of MP-376 and shown that it is rapidly absorbed from the lungs and results in low systemic concentrations. A subsequent phase IB study found that MP-376 pharmacokinetics were comparable among adults and children 6–16 years of age. Further phase II studies reported that sputum P. aeruginosa density decreased in a dose-dependent manner among patients who were randomized to MP-376 when compared with patients who received placebo. Improvements in pulmonary function and a decrease in the need for other antipseudomonal antibiotics were also reported for patients who received inhaled levofloxacin. The most common adverse event was dysgeusia (abnormal taste sensation), which was reported by nearly half of the participants who received MP-376. No serious drug-related adverse events were reported. These findings are encouraging; however, data from the two ongoing phase III trials are needed to determine whether MP-376 demonstrates substantial evidence of safety and efficacy as a chronic CF maintenance therapy and therefore may be useful in routine clinical practice.
Keywords
Introduction
Cystic fibrosis (CF) is an inherited disease that affects multiple organ systems [Ramsey, 1996; Zobell et al. 2012]. CF-related morbidity and mortality are primarily attributable to the pulmonary manifestations of this disease, including a progressive loss of lung function and persistent bacterial infections [Gibson et al. 2003; Ramsey, 1996]. Patients with CF are often chronically-infected with Pseudomonas aeruginosa, which can result in recurrent pulmonary exacerbations that necessitate 14–21 days of antibiotic treatment [Flume et al. 2009].
Systemic intravenous antibiotics are limited by their poor ability to penetrate respiratory secretions and bacterial biofilms (Figure 1) [Grenier, 1989]. This has led to the development of inhaled antibiotics, which afford the opportunity to maximize local antibiotic concentrations at target pulmonary tissues [Ratjen, 2008]. Studies conducted using animal models have reported that inhaled therapy enhances the rate of bacterial killing and in vitro studies have shown that inhaled antibiotics effectively penetrate P. aeruginosa biofilms [King et al. 2010; Sabet et al. 2009]. To date, two inhaled antibiotics have been licensed as chronic maintenance therapies for CF in the United States. These include an inhaled tobramycin solution (TOBI, Novartis, East Hanover, NJ) and an inhaled aztreonam lysine solution (Cayston, Gilead Pharmaceuticals, Seattle, WA).

Pseudomonas aeruginosa biofilm formation and growth in the lungs of patients with cystic fibrosis.
The focus of this review is to evaluate the safety and efficacy of inhaled levofloxacin for the treatment of CF acute pulmonary exacerbations. To determine the appropriateness of inhaled levofloxacin for patients with CF several questions must be addressed, including the following. (1) Are the pharmacologic properties of inhaled levofloxacin suggestive of improved antipseudomonal efficacy among patients with CF? (2) Are there sufficient data to evaluate the efficacy of inhaled levofloxacin, and if so, do the data support its routine use? (3) Are there sufficient data to evaluate the safety of inhaled levofloxacin, and if so, what are the conditions for toxicity and adverse effects? (4) What unanswered questions remain that are needed to inform clinical decision making?
Clinical pharmacology of inhaled levofloxacin
Mechanism of action
Levofloxacin is the L-isomer of the racemate ofloxacin (Figure 2) [Croom and Goa, 2003]. It is a third-generation fluoroquinolone that features broad-spectrum Gram-positive and Gram-negative activity, including bactericidal activity against P. aeruginosa [Stockmann et al. 2013]. In comparison with second-generation fluoroquinolones such as ciprofloxacin, levofloxacin possesses improved activity against Gram-positive organisms [Garrison, 2003]. Fluoroquinolones exert their bactericidal effect by disrupting DNA replication [Crumplin et al. 1984]. This occurs principally through interactions of fluoroquinolones and DNA gyrase (topoisomerase II) [Gellert, 1981]. DNA gyrase serves a vital role in maintaining faithful DNA replication in bacterial cells by resealing strand breaks and introducing superhelical twists in DNA that aids in the unwinding of double strands [Wolfson and Hooper, 1985]. In addition, DNA gyrase creates specific sites on DNA that fluoroquinolone agents readily bind, thereby inhibiting the resealing of DNA strand breaks [Wolfson and Hooper, 1989]. This mechanism enables fluoroquinolones to rapidly arrest DNA synthesis and inhibit the initiation and propagation of the DNA replication fork [Filutowicz, 1980].
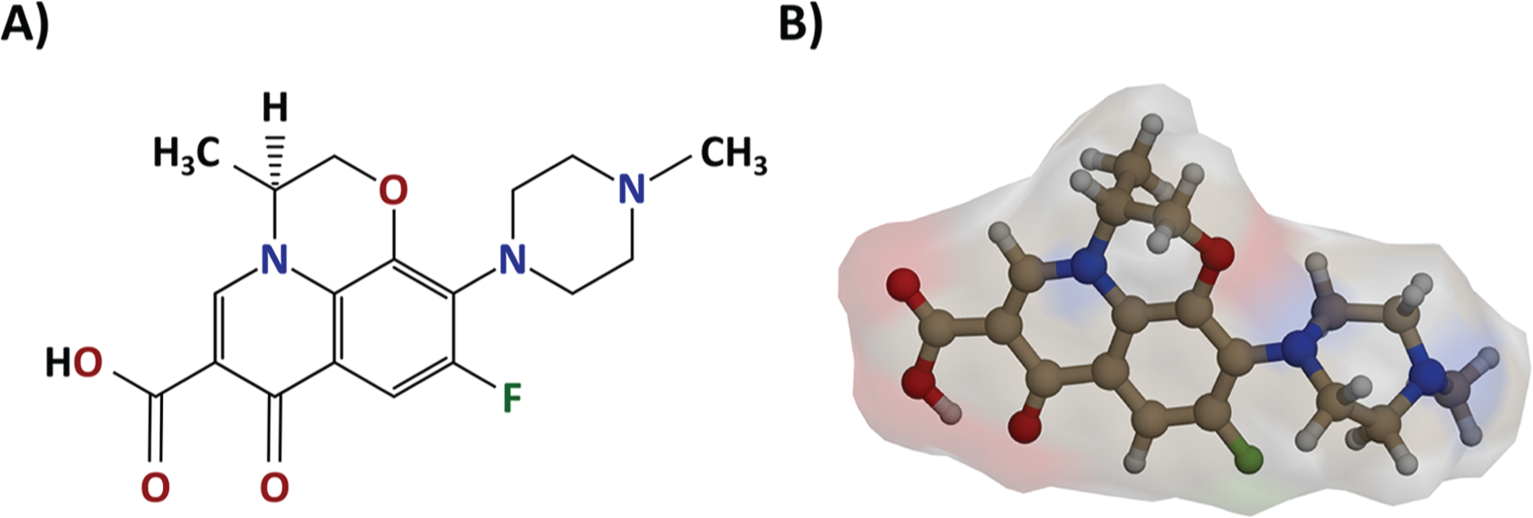
Chemical and molecular structure of levofloxacin.
For patients with CF, local antibiotic concentrations within pulmonary tissues are highly associated with antibacterial efficacy [Dudley et al. 2008]. Inhaled antibiotic administration produces drug concentrations in pulmonary tissues that far exceed those achieved with intravenous or oral dosing methods. MP-376 is a levofloxacin inhalation solution that has been formulated for aerosol administration in a preservative-free 350–500 mOsmol (slightly hyperosmotic) solution that is administered using an investigational Pari eFlow nebulizer and is the subject of several ongoing clinical trials [Geller et al. 2011a]. In addition, a novel dry powder delivery system has been developed to administer levofloxacin across a wide range of inhalation flow rates (iSPERSE, Pulmatrix Inc., Lexington, MA) [Manzanedo, 2012].
Pharmacokinetics
The pharmacokinetics of inhaled levofloxacin (MP-376) have been characterized by Sabet and colleagues in a mouse model of pulmonary infection [Sabet et al. 2009]. The authors reported that aerosolized administration achieved a 9-fold higher area under the curve (AUC) and 30-fold higher maximum concentration (Cmax) in lung tissue when compared with the dose-normalized intraperitoneal administration of levofloxacin. A recently completed trial by Geller and colleagues evaluated the pharmacokinetics of MP-376 dosed at 50 and 100 mg/ml (180 mg dose), followed by 7 days of daily treatment with a 100 mg/ml (240 mg) dose among 10 patients with CF (mean age: 32 years; range: 16–60) [Geller et al. 2011a]. Five minutes before and after administration of the drug, patients rinsed their mouths and swallowed 15 ml of Maalox (400 mg of magnesium hydroxide and 400 mg aluminium hydroxide) to minimize oral absorption of any swallowed levofloxacin. This was done so that serum levofloxacin concentrations would more accurately reflect pulmonary deposition and absorption from the airways. The authors reported rapid but minimal absorption of inhaled levofloxacin from the lungs, with maximum serum concentrations obtained within 20 minutes of dosing (Table 1). Both the 50 and 100 mg/ml (180 mg) doses yielded high sputum concentrations (sputum Cmax of 2563 and 2932 mg/l, respectively) with low systemic concentrations (serum Cmax of 0.95 and 1.28 mg/l, respectively). The 100 mg/ml (240 mg) dose also yielded high sputum concentrations (sputum Cmax of 4691 mg/l) and low systemic concentrations (serum Cmax of 1.72 mg/l). The inhaled levofloxacin 24-hour serum AUC values were 12–19% of the value obtained from a 750 mg oral dose of levofloxacin, which suggests that inhaled administration has the potential to offer improved an improved safety and tolerability profile. However, it must be noted that the between-subject variability was large, with standard deviations that often exceeded the mean value. High variability has been commonly reported among studies of inhaled antibiotic formulations among patients with CF and is likely a consequence of individual differences in disease severity, tidal volume, inspiratory flow, and respiratory rate [Geller, 2008].
Pharmacokinetics and pharmacodynamics of inhaled levofloxacin in patients with cystic fibrosis.

Combined maximum sputum concentration for both the 180 and 240 mg doses. Maximum sputum concentrations for the individual doses were not reported.
Cmax, maximum concentration; Tmax, time to maximum concentration; AUC0-24, area under the concentration time curve from 0-24 hours; t1/2, half-life; MIC50, concentration that inhibits 50% of bacterial growth; MIC90, concentration that inhibits 90% of bacterial growth; MRSA, methicillin-resistant Staphylococcus aureus; MSSA, methicillin-sensitive Staphylococcus aureus.
A single phase IB, multicenter study evaluated the pharmacokinetics of MP-376 in children with CF [Kearns, 2011]. A total of 25 patients between 6–16 years of age were recruited and given 180 mg (body weight 22–29 kg) or 240 mg (body weight ≥ 30 kg) of MP-376 every 24 hours for 14 days. Serum and sputum samples were obtained for noncompartmental pharmacokinetic analyses on days 1 and 14. Serum Cmax and AUC values were comparable with those obtained from adult subjects (Table 1). Maximum sputum concentrations were highly variable with a percentage coefficient of variation of 188. The authors reported no apparent association between current body weight or age with MP-376 serum or sputum AUC values, which led them to conclude that pediatric CF patients of at least 6 years of age who weigh ≥30 kg should receive the same dose as adult patients with CF.
Pharmacodynamics
Levofloxacin is an antibiotic that features concentration-dependent bactericidal activity, such that the rate of bacterial killing increases with higher drug concentrations [Stein, 1996]. Pharmacodynamic measurements that reflect this activity are the Cmax/MIC (minimum inhibitory concentration) ratio and the AUC/MIC ratio (a measure of total drug exposure divided by the MIC of the bacterial isolate) [Flume, 2008]. To optimize the antibacterial activity of levofloxacin it is imperative that we leverage the concentration-dependent killing effects at the target site of action. Inhaled levofloxacin offers several theoretically appealing pharmacokinetic and pharmacodynamic advantages, including a rapid onset of action, a decreased dose requirement to achieve therapeutic effects, and an improved safety and tolerability profile due to lower drug exposure at off-target sites [Geller, 2008].
To the best of the authors’ knowledge, there have not been any published clinical pharmacodynamic studies of inhaled levofloxacin performed among patients with CF. However, King and colleagues performed an in vitro evaluation of the antibacterial activity of several classes of inhaled antibiotics, including levofloxacin, ciprofloxacin, tobramycin, amikacin, and aztreonam [King et al. 2010]. The results of this study revealed that levofloxacin was the most potent antibiotic against P. aeruginosa, Burkholderia cepacia complex, Stenotrophomonas maltophilia, Achromobacter xylosoxidans, and Staphylococcus aureus isolates obtained from patients with CF. Notably, levofloxacin was more potent than the aminoglycosides and aztreonam against P. aeruginosa biofilms. In time-kill experiments levofloxacin displayed the most rapid rate of bacterial killing among both mucoid and nonmucoid strains of P. aeruginosa. Nevertheless, according to susceptibility breakpoints issued by the Clinical and Laboratory Standards Institute (CLSI) a majority of the bacterial isolates obtained from patients with CF in this study were resistant to all of the antibiotics tested [King et al. 2010]. However, it must be noted that these breakpoints pertain to systemic methods of antibiotic administration and may not be appropriate for inhaled antibiotics.
Safety of inhaled levofloxacin
Adverse events and tolerability
Two trials have investigated the safety of the inhaled levofloxacin solution MP-376 (Table 2) [Geller et al. 2008, 2011b]. In the phase I trial, 40 patients with CF and a positive sputum culture for P. aeruginosa within 6 months were randomized to receive MP-376 or placebo every 12 hours for a period of 14 days [Geller, 2008]. This was a dose-escalation study in which patients were increased from 78 mg, to 175 mg, then to 260 mg every 12 hours. Overall, two subjects (5%) withdrew from the study due to adverse effects. One subject was randomized to the MP-376 arm and the other subject was randomized to the placebo arm. None of the study’s participants discontinued treatment due to protocol-defined intolerability. Adverse events were common and ranged from 60% to 100% across all trial arms, including placebo. An increase in adverse events was observed for patients who received 175 mg and 260 mg doses of MP-376 every 12 hours (n = 29 and 25, respectively). This compares with 12 adverse events reported among the 78 mg dose of MP-376 arm and eight adverse events reported among participants who received placebo. The most frequently reported adverse effects attributed to MP-376 included dysgeusia (47%) and cough (8%). Headache (13%), abdominal pain (7%), acute exacerbation of disease progression (7%), hemoptysis (7%), nasal congestion (7%), nasopharyngeal pain (7%), respiratory tract congestion (7%) and wheezing (7%) were also reported among patients who received MP-376; however, these were judged to be unrelated to the study treatment. Two patients experienced acute pulmonary exacerbations that were classified as serious adverse events. Both of these occurred more than 1 week after the last dose of study drug and were deemed to be unrelated to MP-376. Only one patient had a >20% decline in forced expiratory volume in 1 second (FEV1) within 2 hours of dosing; however, they received placebo.
Characteristics of inhaled levofloxacin safety and efficacy trials.

CF, cystic fibrosis; SD, standard deviation; CFU, colony-forming units.
A phase IIB trial conducted by Geller and colleagues evaluated the safety and efficacy of MP-376 among 151 patients with CF and confirmed P. aeruginosa infection within the preceding 6 months [Geller et al. 2011b]. Following 28 days of treatment, the incidence of adverse effects was similar among patients who were randomized to MP-376 and placebo (p = 1.0). Similar to the results of the earlier phase I trial, the most commonly reported adverse effects among patients treated with MP-376 in this trial included dysgeusia (40%), cough (16%), and headache (8%). However, dysgeusia was the only adverse event that was statistically more common among patients who received MP-376 when compared with placebo (p < 0.001). No participants withdrew from the study or discontinued treatment owing to the poor taste of the study drug.
To monitor for drug intolerance, the first dose of MP-376 or placebo was administered at each study site [Geller et al. 2011b]. Drug intolerance was defined as any of the following within 30 minutes after doing: >20% reduction in FEV1 compared with baseline; oxygen saturation <90%; severe coughing, chest tightness, throat discomfort, or moderate to severe dyspnea. Two patients were judged to be drug intolerant, which resulted in their early discontinuation from the study on day 1. A third patient experienced a >20% decline in FEV1 when given a 240 mg dose of MP-376, however they remained asymptomatic and continued to participate in the study.
Four serious adverse events were reported during the 28-day treatment period [Geller et al. 2011b]. Three occurred among placebo-treated patients (two acute pulmonary exacerbations and one occurrence of bronchitis). One patient who was receiving 120 mg doses of MP-376 developed appendicitis; however, this was deemed to be unrelated to the study drug. No musculoskeletal adverse events were reported.
Clinical laboratory values, vital signs, physical examination findings, and electrocardiographic recordings were reported to be stable throughout the trial [Geller et al. 2011b]. Minor shifts from baseline in hematological parameters and electrocardiographic findings were not found to correlate with administration of placebo or MP-376. Overall, 12 (8%) participants were hospitalized during the study period. There was no difference in the incidence of hospitalization between the trial arms.
Efficacy of inhaled levofloxacin
Trial design
The efficacy of a novel inhaled levofloxacin solution (MP-376) has been evaluated in a phase IIB study conducted among patients with stable CF and evidence of chronic P. aeruginosa lung infection (Table 2) [Conrad, 2010; Flume, 2010; Geller et al. 2011b]. Participants were randomized to one of three doses of MP-376 or placebo for 28 days. The primary efficacy endpoint was the change in sputum P. aeruginosa density.
Participants
Across 51 CF centers in the United States and Europe, 151 participants were recruited and randomized. Of these, 143 (95%) completed the trial. Six participants withdrew from the trial due to adverse events that occurred during the 28-day treatment period (two in the placebo arm and four in the MP-376 arms).
The demographic and clinical characteristics of the patients in each treatment arm were comparable. At baseline, the mean FEV1 percentage predicted was 52%. Concomitant medications were commonly reported, including: dornase alfa (78%), azithromycin (74%), and hypertonic saline (46%). Only 38% of P. aeruginosa isolates obtained at baseline were susceptible to levofloxacin based on an MIC breakpoint of 2 µg/ml.
Outcomes
Sputum P. aeruginosa density decreased from baseline following 28 days of treatment with all MP-376 dosing regimens (p < 0.01). This effect was largest for the two 240 mg MP-376 dosing regimens (p < 0.001). Patients treated in the two 240 mg arms also had a 10.9% improvement in their FEV1 when compared with patients who received placebo alone (p < 0.001). In addition, there was a 61–79% risk reduction in the need for other inhaled or systemic antipseudomonal antibiotics among all patients who received MP-376 as compared with placebo (p < 0.001). Respiratory symptoms improved among patients who received MP-376 dosed at 240 mg every 12 hours, however this was not found to be statistically significant (p = 0.09).
Although many patients had P. aeruginosa isolates that were classified as resistant to levofloxacin according to current CLSI MIC breakpoints, there was no correlation between baseline levofloxacin MIC values and the change in sputum P. aeruginosa density of percentage change in FEV1. There was also no evidence suggesting that inhaled levofloxacin resistance developed during the 28-day treatment period or the subsequent 28-day follow-up period.
In this study, more than half of the participants had other nonpseudomonal bacterial species that were isolated from their sputum at baseline. The most commonly identified organisms included S. aureus, S. maltophilia, and A. xylosoxidans. Following a 28-day course of treatment with MP-376, no change was discerned in the microbial composition of these organisms in the airways of the study participants. This suggests that aerosolized MP-376 does not exert a selective pressure against other nonpseudomonal bacterial species. The authors further explored whether microbiologic and clinical outcomes varied among patients with and without S. aureus detected at baseline. Geller and colleagues report that the decrease in sputum P. aeruginosa density and the improvement in FEV1 percentage predicted were comparable among patients with and without S. aureus [Geller et al. 2011b].
Implications for future studies
Inhaled antibiotics have been prescribed for the treatment of acute pulmonary exacerbations of CF for decades, yet comparatively little is known about the safety and efficacy of these formulations when compared with their oral and parenteral counterparts [Anderson, 2010]. Fortunately, several studies investigating inhaled levofloxacin solution are recently completed or ongoing (Table 3).
Recently completed and ongoing clinical trials of inhaled levofloxacin solution (MP-376).

FEV1, forced expiratory volume in 1 second; FEF 25–75, forced expiratory flow at 25-75%; FVC, forced vital capacity.
On the basis of promising phase II data, MP-376 (inhaled levofloxacin solution) has been advanced into phase III clinical trials. The first confirmatory phase III trial involves 112 centers in North America, Australia, New Zealand, and Israel [ClinicalTrials.gov identifier: NCT01180634]. Patients >12 years of age with stable CF and a sputum culture positive for P. aeruginosa within the last year are eligible for recruitment. The trial aims to enroll 330 participants who will be randomized to receive 240 mg of MP-376 or placebo every 12 hours for a 28-day treatment period. The primary outcome is designed to evaluate the efficacy of MP-376 and will measure the time to an acute pulmonary exacerbation. Secondary outcome measures include the time to administration of other antipseudomonal antibiotics; changes in pulmonary function (FEV1, forced expiratory flow at the 25% point to the 75% point [FEF 25–75], and forced vital capacity [FVC]) from baseline to the end of treatment; changes in respiratory symptom reporting; changes in bacterial load and susceptibility patterns; and the reporting of adverse events.
The second confirmatory phase III trial will assess the comparative safety and efficacy of MP-376 and tobramycin inhalation solution [ClinicalTrials.gov identifier: NCT01270347]. Recruitment is currently taking place at 130 centers in the United States, France, Germany, Ireland, Israel, and the United Kingdom. The trial aims to enroll 267 patients >12 years of age with stable CF and a positive sputum culture for P. aeruginosa within the last year. Participants will be randomized to receive either 240 mg of MP-376 or tobramycin inhalation solution every 12 hours for a period of 28 days. The primary safety outcome will be assessed by tabulating the number of adverse events reported from baseline through the final 6-month visit for each of the trial arms. The primary efficacy measure will be the change in FEV1 percentage predicted from baseline at the end of the 28-day treatment period.
Conclusions
Current safety and efficacy data for the inhaled levofloxacin solution MP-376 appear favorable. Decreased sputum P. aeruginosa density, reduced need for other antipseudomonal antibiotics, and improved pulmonary function testing results suggest that inhaled levofloxacin may represent a promising new therapy for patients with CF. The nebulized formulation will likely be dosed every 12 hours and requires 4–6 minutes for administration, which is similar to other currently approved inhaled antibiotics. Mild-to-moderate dysgeusia has been reported by nearly half of the subjects who received MP-376; however, no drug-related serious adverse events have been recorded. A phase III trial is currently ongoing to evaluate the comparative safety and efficacy of inhaled levofloxacin versus inhaled tobramycin solution. Another large confirmatory phase III trial is ongoing and will evaluate the efficacy of inhaled levofloxacin among more than 300 patients with CF. Data obtained from these trials will be pivotal in allowing clinicians and regulators to weigh the evidence for the routine clinical use of inhaled levofloxacin.
Footnotes
Funding
This work was supported by grants from the National Institute of Allergy and Infectious Diseases (grant number U01A1082482; to KA) and the Centers for Disease Control Prevention (grant number U18-IP000303-01; to CS and KA).
Conflict of interest statement
The authors declare that they have no conflicts of interest.
