Abstract
Background:
Potential organ donors are often identified in intensive care following brainstem or circulatory death. Clinical optimisation is fundamental for maintaining organ viability and physiotherapists are well positioned to support this through targeted interventions. Despite this, the physiotherapy role in deceased organ donation remains underexplored. This study aimed to describe current practice and explore the perceptions of physiotherapists in the United Kingdom involved in managing deceased organ donors.
Methodology:
An explanatory sequential mixed methods design was utilised. An online survey was used to describe the national picture of current physiotherapy practice. Online semi-structured interviews were undertaken to explore perceptions and attitudes of physiotherapists towards the physiotherapy management of deceased organ donors.
Results:
Fifty-six physiotherapists completed the survey, with 52% (n = 29) reporting involvement in donor management “always,” or “most of the time.” Treatment aims included secretion clearance (49%, n = 26) and lung optimisation (45%, n = 24). Suctioning was the most frequently performed intervention (95%, n = 53), followed by positioning (71%, n = 40) and manual techniques (71%, n = 40). Only 5% (n = 3) reported having local guidelines. Seven physiotherapists participated in interviews, identifying six key themes: experiences, barriers, role perceptions, physiotherapist learning needs, multidisciplinary team learning needs, and future needs.
Discussion:
The role of physiotherapy in organ donor management is under-recognised and lacks national consensus. Findings highlight disparities in practice, limited guidance and the need for further training to strengthen clinical reasoning. Guidance development that addresses the practical, ethical and emotional complexities of this work is urgently needed to support physiotherapists in this evolving area.
Introduction
Organ failure occurs when vital organs are unable to perform their essential functions. Common causes include congenital heart defects, diabetic nephropathy and chronic pulmonary disease. 1 For patients with irreversible organ failure, organ transplantation remains the most effective treatment. 2 Organ transplantation involves retrieving organs from a living or deceased donor for implantation into recipients. 2 One deceased donor can save up to nine lives and help many more by donating multiple organs. Common transplantable organs include kidneys, heart, liver and lungs. 3 Deceased donors are typically identified in intensive care units (ICUs) following brainstem or circulatory death. 4 Brainstem death can result from trauma, hypoxia, or intracranial haemorrhage. 5 Circulatory death is often secondary to myocardial infarction or cardiac failure. 6 Both forms involve the irreversible loss of function, diagnosed through rigorous clinical criteria. 7
Despite ongoing efforts to increase donation rates, demand in the United Kingdom (UK) continues to exceed supply 8 with over 8000 individuals currently on the transplant waiting list. 3 Multiple barriers hinder organ procurement including family refusal, lack of public awareness, and poor organ viability.9,10 Delays between donor identification and organ retrieval are known to compromise organ quality with physiological deterioration including haemodynamic instability, pulmonary infections, and aspiration. 11 Clinical optimisation of potential donors is therefore critical for maintaining organ viability. 12 Evidence suggests that standardised donor management protocols improve organ viability and reduce complications, particularly for lungs. 13 Use of lung management protocols has been associated with a threefold increase in successful lung procurement. 14 These protocols often include chest physiotherapy, as outlined in the National Health Service (NHS) donor optimisation care bundle. 15
Physiotherapists play an important role in optimising respiratory function in ICU patients, using techniques such as suction, hyperinflation, and mechanical insufflation-exsufflation (MI-E) to enhance lung mechanics and secretion clearance.16–19 Optimised and well-ventilated lungs also enable improved oxygenation to other vital organs. Despite the value of physiotherapy in ICU patients, evidence for the role of physiotherapy in potential deceased organ donors is limited. Existing studies20–22 have small sample sizes, are non-UK based and report inconsistent findings. The term “chest physiotherapy” is frequently referenced in donor care protocols without standardised definitions or guidance regarding frequency and specific techniques. 14
The lack of national guidance and limited evidence-base make this a topic of debate amongst clinicians in terms of when and how physiotherapy should be delivered for potential deceased organ donors. This study aimed to explore current respiratory physiotherapy practice and the confidence, perceptions and attitudes of physiotherapists within deceased organ donor management in the UK.
Methods
Reporting guidelines CHERRIES, 23 COREQ, 24 and GRAAMS 25 were used to structure reporting of the methods and results. Completed checklists are provided in the Supplemental Appendix.
Study design
An explanatory, sequential mixed methods design was employed to capture both breadth and depth of information. A National, cross-sectional online survey first explored current physiotherapy practices and perceived confidence in treating deceased organ donors. Online semi-structured interviews then provided detailed exploration of physiotherapists’ perceptions and attitudes. Interviews were selected over focus groups due to the sensitivity of the topic. They were guided by qualitative description, 26 providing a naturalistic account of participants’ views.
Approvals and risk management
Ethics approval was obtained from UCL (ID: 26647/001). Survey respondents could withdraw at any time prior to submission. Interview participants could pause, decline to answer questions, or terminate the interview if they felt uncomfortable.
Survey development
The web-based survey was developed using “Qualtrics,” informed by existing literature and the research team’s ICU experience. The survey comprised of 15 questions, predominantly multiple choice for ease of completion, with additional free-text options for further explanation (Supplemental Appendix I). All questions were compulsory to complete before the participant could progress to the next section. Questions were not randomised, but adaptive questioning was used to only reveal relevant questions based on previous answers. Participants could review and amend answers before final submission, after which responses were no longer editable. The survey was open access via a shared link. Duplicate entries were avoided by using cookies and IP checks, preventing resubmission within 3 months.
Usability and technical functionality of the survey were tested by colleagues of the research team prior to pre-testing. The survey was then piloted with three respiratory physiotherapists who were independent of the authorship team and final participant sample. For pre-testing, individuals were similar to the target population but did not meet the inclusion criteria as they had less than 6 months’ ICU experience.
Interview topic guide
The semi-structured topic guide was developed based on the research team’s clinical expertise, known practice variations and learning needs. Survey findings also informed the topic guide, focussing on key areas of interest raised by the participants (Supplemental Appendix II). Topics explored the physiotherapist’s role, experiences and learning needs. The topic guide was piloted with one clinician. The pilot interview was recorded, reviewed by the research team and feedback was provided on interview technique. As no substantial changes to the guide were required, the pilot data were included in the final dataset. 27
Recruitment
Recruitment was conducted over 6 weeks (April–May 2024) through social media and the Association for Chartered Physiotherapists in Respiratory Care (ACPRC) newsletter. The ACPRC newsletter, which has 1854 subscribers, featured the study advertisement (Supplemental Appendix III) once in April 2024. The advertisement was also posted three times on X (formerly Twitter) by the primary researcher (SS). Recruitment formed a convenience sample based on voluntary responses; no incentives were offered. A formal sample size calculation was not performed because the number of eligible clinicians who viewed the advertisement was unknown.
Participants self-identified as being eligible against inclusion and exclusion criteria. Eligible participants were Health and Care Professions Council (HCPC)-registered ICU physiotherapists in specialist posts in the UK, fluent in English. Exclusions included non-physiotherapists, non-UK residents, physiotherapists working in a non-specialist role, and non-English speakers. A specialist post was defined as a participant with at least 6 months’ experience in their current ICU post who were practising in ICU at the time of recruitment. Only specialist ICU physiotherapists were included to capture insights from clinicians with consistent ICU exposure, established understanding of physiotherapy’s role in ICU, and awareness of local organ donation policies. Interviews were conducted by purposive sampling, aiming to include a wide geographical spread and mixed levels of experience.
Process
A participant information sheet was displayed on the first page of the survey outlining the study purpose, primary researcher’s contact details and the estimated completion time. Participants were also informed of the data being collected and its storage. Consent was obtained via an online checkbox before the survey could begin. The survey was anonymous unless participants voluntarily provided an email address for contact regarding the interviews. Email addresses were stored separately from survey responses and removed prior to analysis to maintain anonymity.
Interview participants provided written, electronic consent after reviewing the information sheet and gave verbal consent at the interview start. Interviews were conducted by the primary researcher (SS) via Microsoft Teams with audio-visual recording. Only SS and the participant were present. SS transcribed all interviews verbatim with the recording of field notes and non-verbal cues. Participants were informed of the researcher’s interest in the topic, the development of the research question and their background. No repeat interviews were conducted and transcripts were not checked by the participants.
Research team reflexivity
The research team consisted of five female physiotherapists working clinically or in academia. Two currently work in intensive care units. All have had prior research experience, none on the topic of organ donation. The primary researcher was working as a qualified physiotherapist in acute respiratory care at the time of the study. The study was undertaken in partial fulfilment of an MSc in Advanced Physiotherapy: Cardiorespiratory at UCL.
The primary researcher had worked across two hospitals with differing exposure to deceased organ donation and, having observed variations in practice, entered the study with no strong stance. With no previous qualitative research experience, she completed 2 postgraduate research modules at UCL (approximately 400 learning hours) covering qualitative methodology and principles of trustworthiness. 28
Given the small cohort of specialist ICU physiotherapists nationally, prior professional acquaintance between the researchers and participants was possible. This was addressed in the participant information sheet by emphasising voluntary participation, confidentiality, and the right to withdraw. Prior to the interview SS reiterated that the interviewer was present in the context of a researcher rather than a clinician.
Data analysis
Data from the survey was transferred into IBM Statistical Package for Social Sciences (SPSS) and summarised descriptively using counts and frequencies. A Kruskal-Wallis test was used to identify the relationship between confidence and years of experience. A chi-squared test was used to identify the relationship between confidence and frequency of involvement with organ donors. Free-text data were collated into tables and quantified using content analysis to identify recurring patterns in the data and summarise current practice of physiotherapists in the UK. Surveys were screened for completeness prior to data analysis. Only surveys with all multiple-choice items fully completed were included in data analysis.
Interview data were analysed using deductive framework analysis. SS completed initial coding independently. A second researcher (HS) performed independent coding of the full dataset. The two coding frameworks were then compared; discrepancies were identified and resolved through discussion. Participant quotations were extracted to illustrate themes. A formal coding tree was not produced.
Mixed methods integration
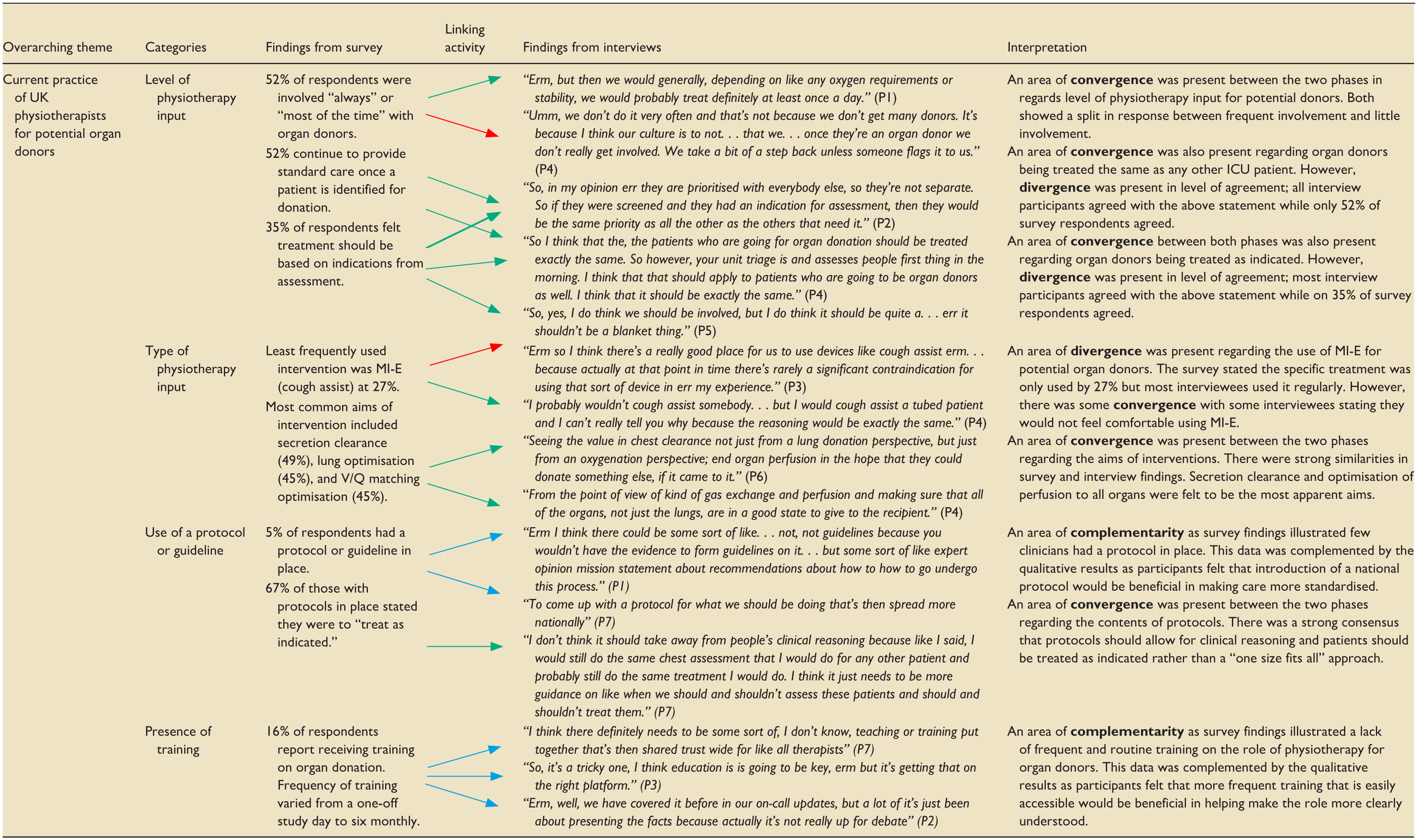
Integration occurred at the design, methods, and reporting levels. 29 Survey data were collected and analysed first and informed the interview topic guide to further explore the quantitative findings. At the methods level, participants were linked across the two phases. Survey respondents formed the sampling frame for the interviews, ensuring that qualitative insights were grounded in the same population. At the reporting level, data were integrated using a joint display table, 30 which summarised survey findings with corresponding qualitative explanations and highlighted the relationships between them.
Data management
Data were stored in password-protected cloud storage. Only authorised individuals could access the data, and access was limited to the primary researcher for all identifiable information, including email addresses and video recordings. Multi-factor authentication and encrypted storage were used to prevent unauthorised access. The rest of the research team received only anonymised data. Video recordings were deleted within 2 weeks post-interview. Transcripts and emails will be retained for 5 years per UCL data protection guidelines (ref: Z6364106/2024/01/108).
Results
Survey results
In total, 56 completed surveys were returned, representing a wide geographical distribution across the UK (Figure 1). Of these, two surveys had missing free-text responses relating to aims of interventions and level of input, although their multiple-choice data were still included. Respondents worked predominantly in a teaching hospital or district general hospital (46%, n = 26 and 39%, n = 22 respectively), with most working in general intensive care units (52%, n = 29), although specialist ICUs were also represented. The number of ICU beds ranged from 6 to 84, with a median (interquartile range) of 20.5 (13–28.25). Respondents reported ICU experience ranging from 1 to 42 years, with a median of 10 years (6–17).
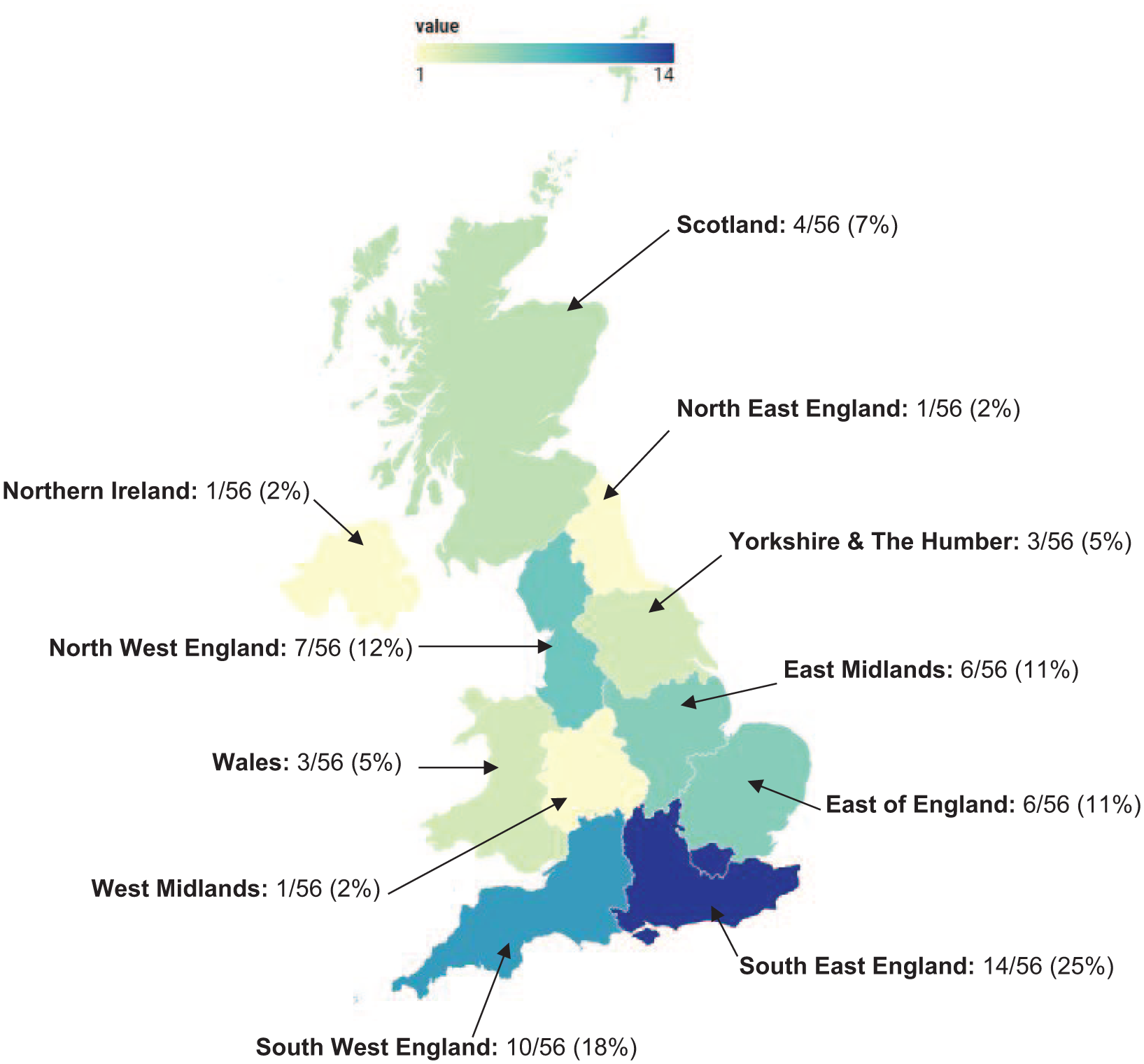
Geographical region of where survey participants worked. Based on n = 56 participants.
Physiotherapy involvement in the management of deceased organ donors varied. Just over half (52%, n = 29) indicated they were involved “always” or “most of the time,” while some reported infrequent or no involvement (Table 1). Once a patient was identified as a potential donor, 52% (n = 29) of physiotherapists reported maintaining their usual level of care (Table 1).
Demographic table of survey responses.
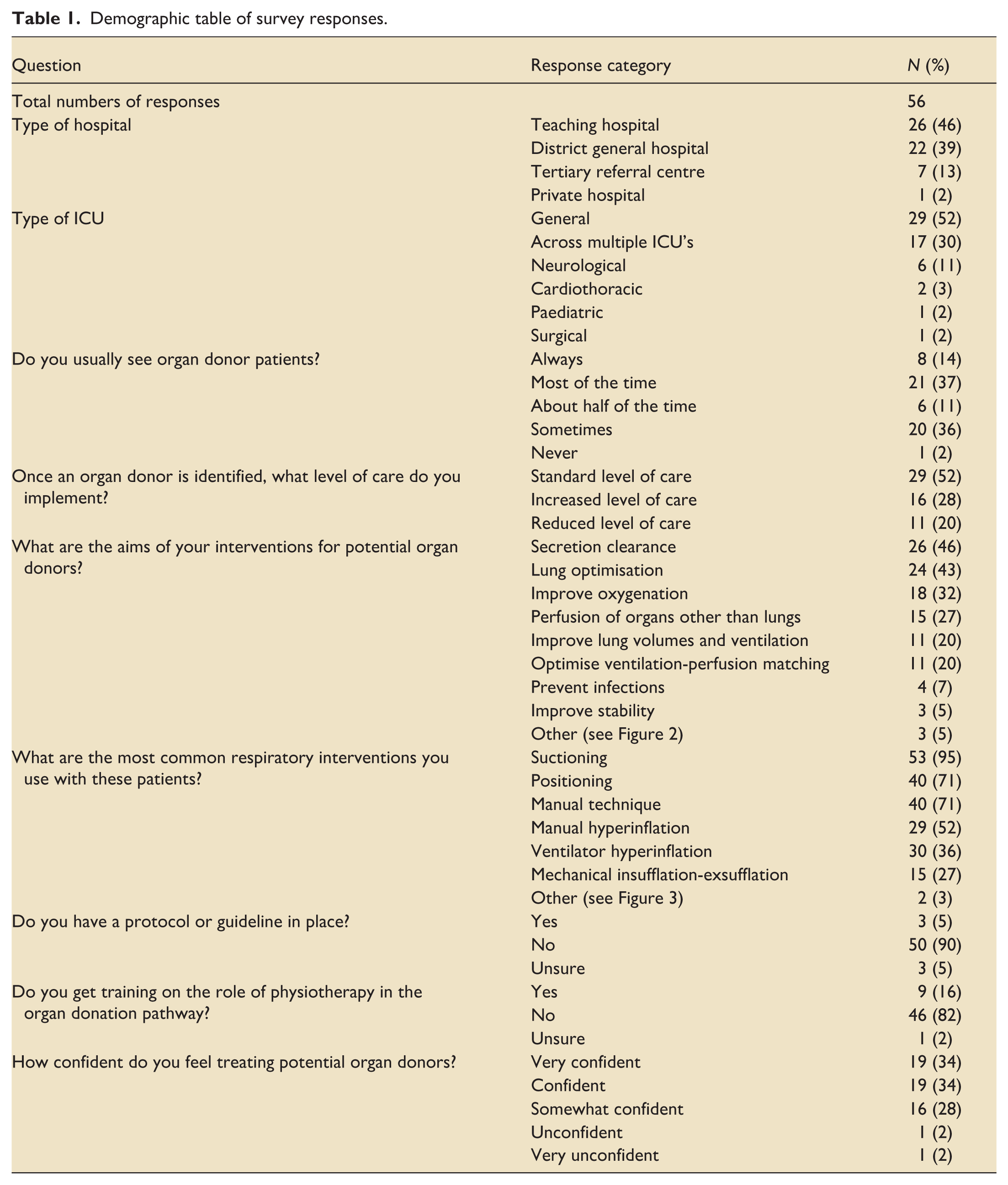
Treatment aims were described by 95% (n = 53) of respondents via a free text box and were subsequently categorised (Figure 2). The most frequently cited aims included aiding secretion clearance (49%, n = 26) and optimising pulmonary function (45%, n = 24). A broad range of interventions were utilised, with suctioning being the most common intervention (95%, n = 53), followed by patient positioning (71%, n = 40) and manual techniques (71%, n = 40). Less frequently employed modalities included manual or ventilator hyperinflation and mechanical insufflation-exsufflation (Figure 3).
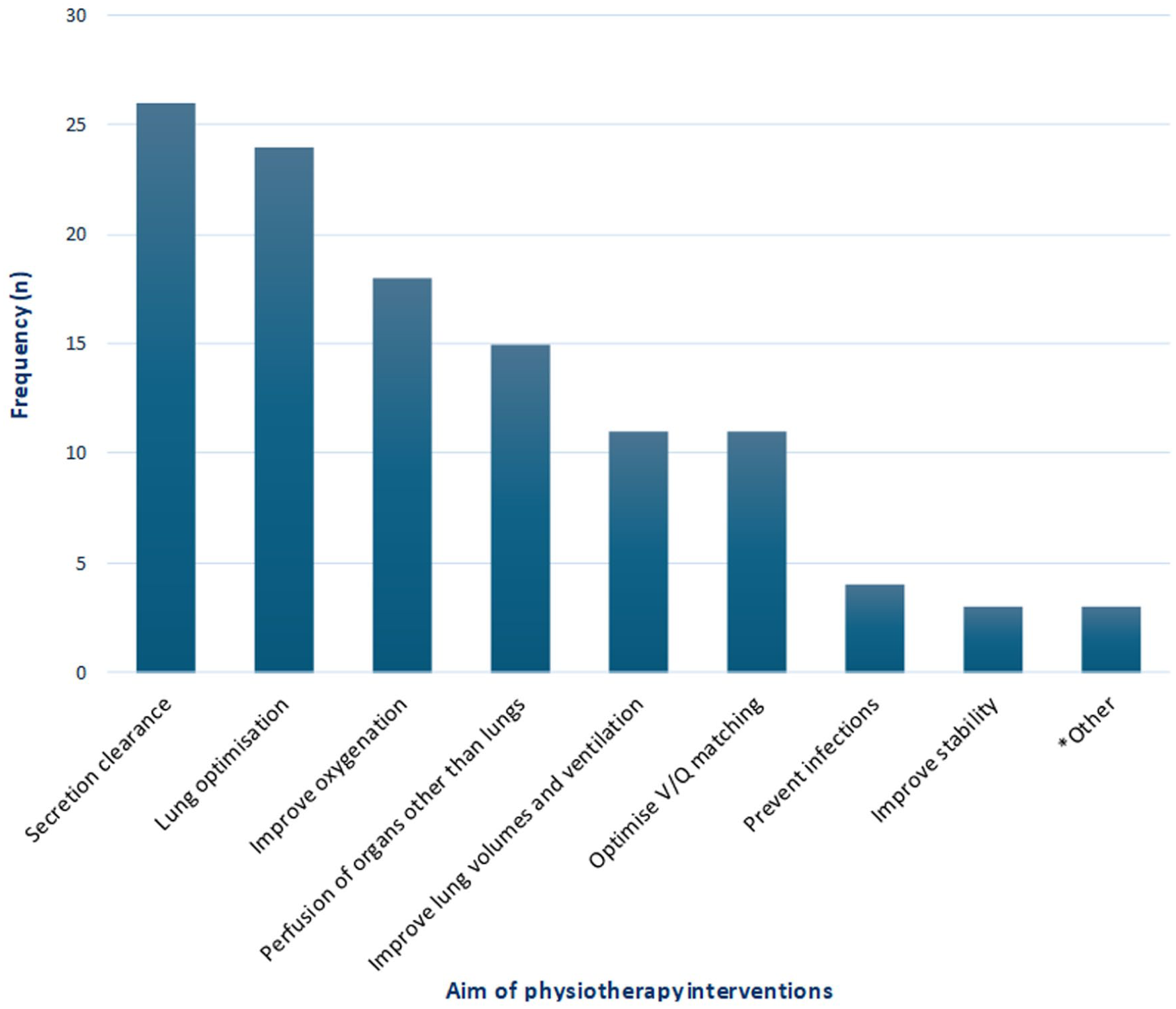
Clinician reported aims of physiotherapy interventions for deceased organ donors. V/Q matching: ventilation perfusion matching. Multiple aims of intervention per respondent were allowed.
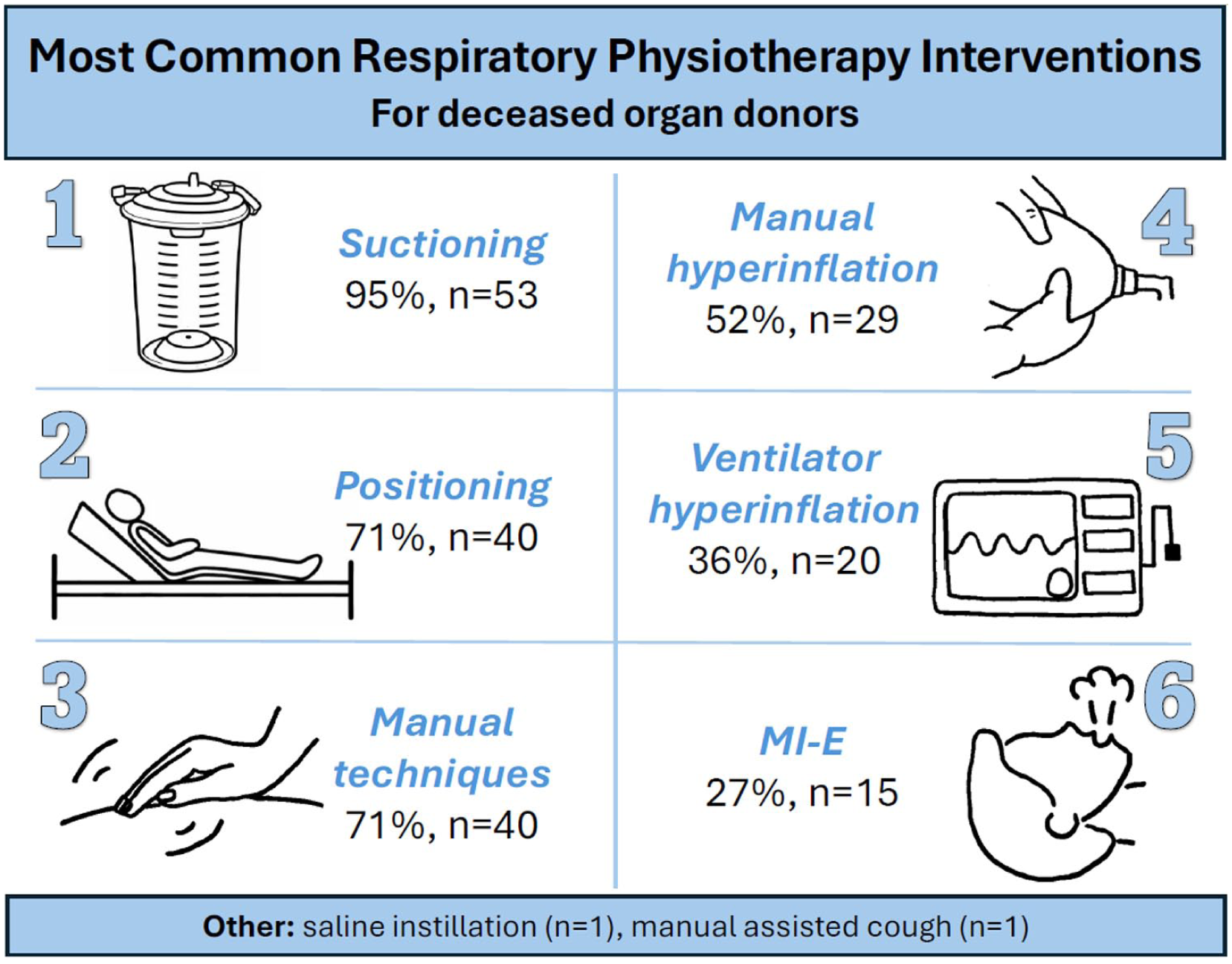
Most common physiotherapy interventions used for deceased organ donors. Respondents were allowed to select more than one respiratory intervention from the tick-box options provided.
Only 5% (n = 3) of respondents reported having access to a local protocol or guidance for the management of organ donor patients. Of these, one referenced the NHS Blood and Transplant Donor Optimisation Care Bundle. Others described general strategies focussed on maintaining oxygenation and preventing hypoxia. Few respondents (16%, n = 9) had received formal training on donor management, with training frequency ranging from a single session to biannual updates. Overall, 68% (n = 38) of respondents reported feeling confident or very confident when managing potential organ donors. Confidence levels were not significantly associated with either frequency of involvement (p = 0.34) or years of ICU experience (p = 0.31).
The survey findings highlighted variability in physiotherapy practice for deceased organ donors in the UK. While common interventions were employed, use of protocols and training availability varied.
Interview results
Of the 56 survey respondents, 39% (n = 22) expressed interest in participating in interviews. Seven interviews were conducted, selecting participants based on availability, geography, and experience. Interviewees were all from different trusts across the UK and had ICU experience ranging from 6 months to 25 years (Table 2). Seniority was classified using the UK National Health Service Agenda for Change bands, reflecting the level of responsibility and experience associated with each role. Participants ranged from Band 6 (senior practitioner or specialist) to Band 8 (managerial or consultant). Most participants working in teaching hospitals (57%, n = 4) and general ICUs (57%, n = 4). Interviews averaged 30 min and 37 s, with durations ranging from 25 to 37 min.
Interview participants’ demographics.
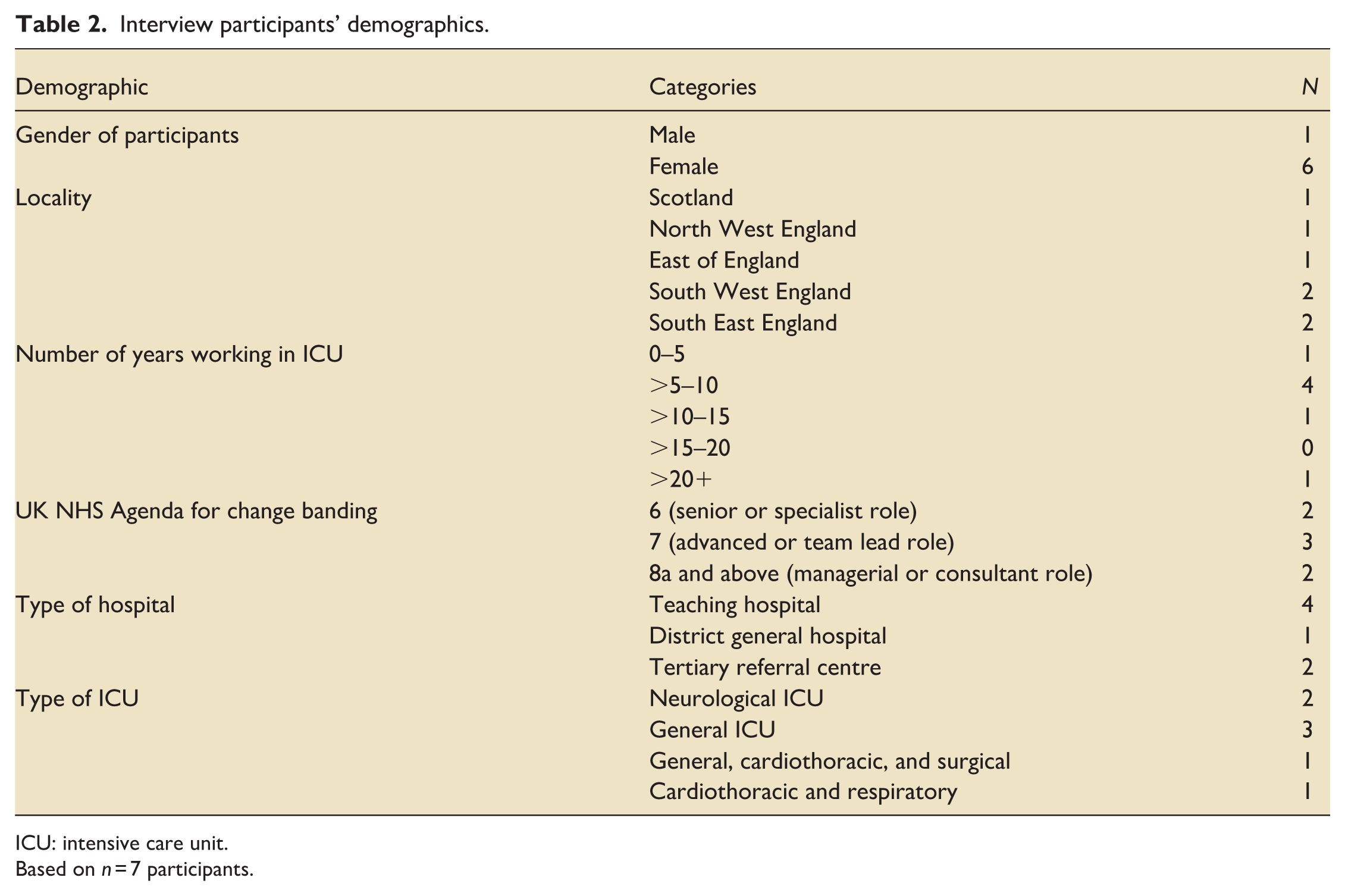
ICU: intensive care unit.
Based on n = 7 participants.
Six themes were developed; 4 identified a priori and 2 deductively. These yielded 22 refined subthemes (Table 3). The a priori themes were drafted from the topic guide, supporting literature and discussions with national and international experts. Their use provided an initial analytical structure aligned with the study aims and reflected a well-recognised approach within framework analysis for understanding current views and practice.
Development of the final themes and subthemes from the dataset.
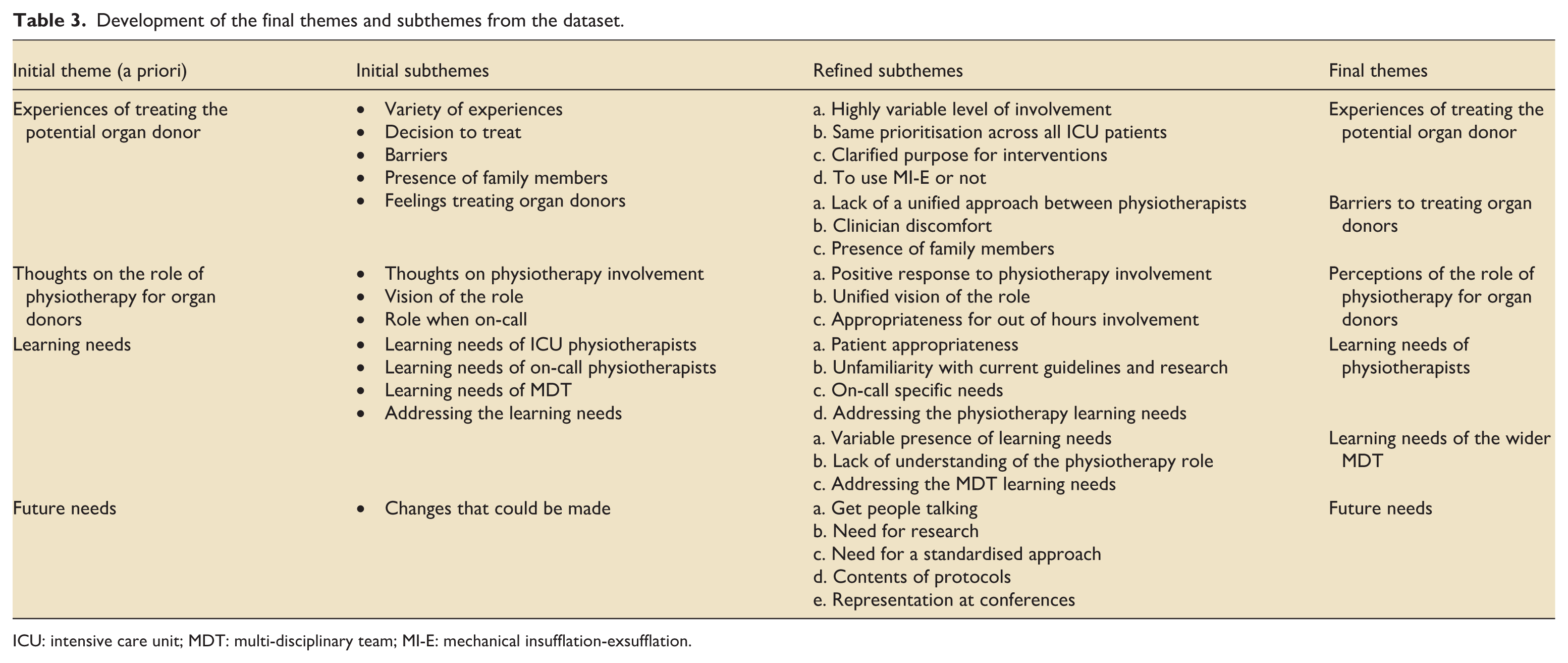
ICU: intensive care unit; MDT: multi-disciplinary team; MI-E: mechanical insufflation-exsufflation.
Theme 1. Experiences of treating potential organ donors
This theme included the level of involvement offered to donor patients, as well as the aims and types of interventions delivered. Physiotherapists’ involvement in organ donor care varied widely. While some reported routine engagement, others only participated upon MDT request: “Once they’re an organ donor we don’t really get involved. We take a bit of a step back unless someone flags it to us.” (P4)
Most participants prioritised donors equivalently to other ICU patients requiring respiratory care, using standard physiotherapy techniques. No formal protocols were referenced: “If they were screened and they had an indication for assessment, then they would be the same priority as all the other as the others that need it.” (P2)
Interventions focussed on secretion clearance, lung optimisation, and end-organ perfusion. Techniques included suctioning, positioning, and manual therapy. Views on MI-E use varied: “I think there’s a really good place for us to use devices like [MI-E] erm. . . because actually at that point in time there’s rarely a significant contraindication.” (P3) “I probably wouldn’t use [MI-E]. . . and I don’t know why that is.” (P4)
Theme 2: Barriers to treatment
Three key barriers were identified. The first was the lack of a unified approach between physiotherapists within the same team.
“Err I think a big barrier is other physios’ perceptions, erm especially the more senior members of the team who have been on the unit a long time and have a set way of doing things” (P7)
The second barrier highlighted was that clinicians expressed ethical unease treating deceased patients.
“You’re treating a dead person. . . I can really see why people feel uncomfortable.” (P1)
The final barrier was family presence at the bedspace. Participants avoided treating donors in front of relatives due to potential misunderstandings.
“To have a physio turn up at the bed of your dying loved one, probably they’re going to think oh god they are going to start trying to get them out of bed.” (P5)
Theme 3: Perceptions of physiotherapy’s role
There was a positive response to physiotherapy involvement in the organ donation pathway, with participants describing how physiotherapy interventions can help maintain lung function and optimise donor organ viability.
“. . .they lose their cough and therefore if you can’t cough, you can’t clear secretions and if you can’t clear secretions, you generally collapse your lungs and if you collapse your lungs, you lose you oxygenation and therefore you’re hypoxic and therefore hypoxemic to those organs. . .” (P3)
A unified vision was identified that patients should be assessed in-line with other ICU patients and treated as indicated in collaboration with the wider team, avoiding a generic “one size fits all” approach. However, opinions diverged on out-of-hours care. Most participants felt that it was appropriate for on-call physiotherapists to be called as indicated if the patient was deteriorating. However, some participants were concerned about on-call staff confidence and emotional vulnerability.
“Yeah, definitely appropriate. . .If you need treating during the day frequently, you’ll probably need treating at night.” (P3) “I don’t necessarily think people should be coming in on-call to treat these patients. . .putting someone that may not be experienced in that area wouldn’t be appropriate.” (P1)
Theme 4: Physiotherapist learning needs
Participants reported limited awareness of current guidelines and evidence regarding donor physiotherapy. Most participants felt physiotherapists lacked understanding around donor physiology and when to prioritise stability over optimisation.
“It would be something that we would need to be mindful on refreshing our competence with. Particularly the instability and how that can occur and how it can happen quite suddenly and what to look for.” (P4)
Most participants felt learning needs were similar across static physiotherapists and on-call physiotherapists. Some participants suggested that while on-call physiotherapists possessed the necessary skills to treat potential organ donors, they might feel less confident working in the ICU environment.
“. . .It’s familiarity and a certain level of confidence, it’s not competence. They’re all competent to be on the rota, but it’s the confidence to actually action with a certain group of patients.” (P2)
Suggested educational strategies included incorporating donor care into annual training and shadowing specialist nurses.
Theme 5: MDT learning needs
Views on MDT knowledge of the physiotherapy role in potential organ donors were mixed. Some reported positive collaboration while others encountered misconceptions.
“..I’ve even had an experience where I’ve gone to treat a patient who’s for organ donation and a doctor has said to me, what are you doing there, like they’re going to be end of life, they’re for donation. I’ve actually had to say to the doctor like, you know, explain to them why we’re doing it.” (P7)
It was felt that education through teaching was the best way of addressing the learning needs of the MDT, but some were sceptical as to whether this would change practice.
“It needs us to communicate sort of teaching through doing as it were. Yeah, I don’t know what else. . . you can do as much teaching and teaching and teaching can’t you? But at the end of the day, it’s maybe what comes out in practise that’s the difficulty.” (P5)
Theme 6: Future needs
Participants recommended several initiatives to formalise and promote the role of physiotherapy in donor care. Most participants described the need to encourage people to talk about the topic and share practice. Suggestions included more representation at national conferences as well as further research.
“. . .knowing if there was research behind whether it, whether we do help or don’t help would, erm would provide more education, wouldn’t it I suppose?” (P5)
All participants advocated for a more standardised approach through the creation of a national clinical statement or guideline. Participants advocated preserving clinical reasoning within this.
“Erm I think there could be some sort of like. . . not, not guidelines because you wouldn’t have the evidence to form guidelines on it. . . but some sort of like expert opinion mission statement about recommendations about how to how to go undergo this process.” (P1)
Data integration
A joint display table was developed to integrate the survey and interview findings (Table 4).
Integration of data from survey and interviews regarding role of physiotherapy for potential organ donors.
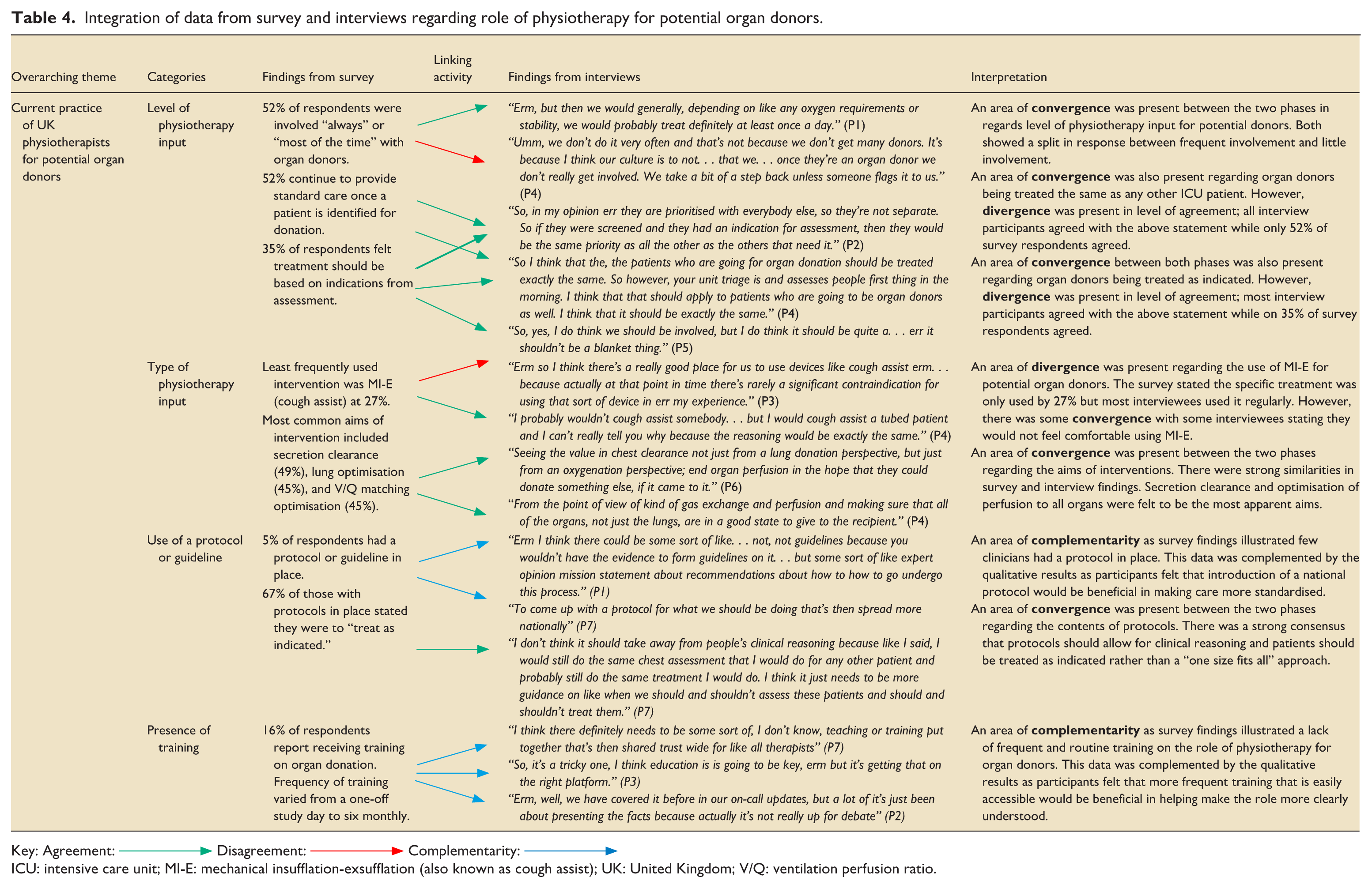
Key: Agreement:  Disagreement:
Disagreement:  Complementarity:
Complementarity: 
ICU: intensive care unit; MI-E: mechanical insufflation-exsufflation (also known as cough assist); UK: United Kingdom; V/Q: ventilation perfusion ratio.
Integration demonstrated areas of convergence, including similar patterns of variability in physiotherapy involvement and shared agreement that organ donors should be treated according to clinical indication. Divergence was noted in the degree of agreement regarding treating donors the same as other ICU patients. Complementarity emerged where survey findings highlighted limited training and lack of protocols, while interview data provided deeper insight into the perceived need for national guidance. Overall, these findings demonstrated that although physiotherapy involvement is generally valued, practice remains inconsistent and influenced by local culture, confidence, and ethical considerations.
Summary of findings
The key findings are summarised below:
Physiotherapy involvement with organ donors is variable and often lacks formal structure.
Standard respiratory interventions are commonly used, but use of advanced techniques including MI-E is inconsistent.
Main barriers include variation in team practices, ethical discomfort, and family presence.
The physiotherapy role is generally viewed positively, with support for routine screening and intervention.
There is limited training available, highlighting a need for structured education.
A national guidance or expert consensus could reduce variability and enhance role clarity.
Further research and increased professional engagement are needed to promote practice development.
Discussion
This study contributes valuable insights into current practice of UK physiotherapists and raises the national profile on the topic. There was significant variability in how UK physiotherapists approached the care of potential organ donors. Variations in decision to treat, frequency of involvement, and prioritisation of organ donation patients were apparent. This aligns with findings from Australia, where O’Connor 22 and Raios et al. 21 identified inconsistencies across geographical regions and within individual hospitals. This variation likely stems from the absence of a national protocol and the rarity of organ donation cases, which limits clinician exposure and expertise. 31 As a result, physiotherapists often model their approach on more experienced colleagues, increasing inconsistency. A more standardised approach would reduce unwarranted variations in practice and improve the quality of care provided to potential organ donors.
Common treatment aims were secretion clearance, lung optimisation, and perfusion to organs, consistent with findings by Raios et al. 21 These aims are fundamental across all mechanically ventilated patients, irrespective of their diagnosis.32,33 Suctioning, positioning, and manual techniques were the most frequently implemented interventions to addressed these aims. There is no pre-defined definition of “standard” physiotherapy care for respiratory patients in ICU, however these are all interventions mentioned in a Delphi study on the minimum standards for physiotherapists working in ICU. 34 This suggests that integrating potential organ donors into standard care does not require clinicians to learn new skills, the necessary interventions are transferable.
Views on the appropriateness of MI-E use were mixed. Some participants found frequent use of MI-E beneficial in aiding secretion clearance whilst others felt uncomfortable using the technique. Although MI-E improves cough efficacy in ventilated patients,35,36 limited evidence in organ donor populations and a lack of confidence in using MI-E 18 likely contributed to varied uptake.
In this study, physiotherapy involvement in organ donor care was viewed positively with a unified vision that physiotherapists should routinely screen and treat as indicated. This contrasts with findings from Raios et al., 21 where opinions were more divided. Although the absolute number of deceased organ donors is higher in the UK 3 than in Australia, 37 rates per capita are broadly comparable. The divergence in findings may therefore reflect contextual differences between healthcare systems such as training pathways or institutional policies rather than donor prevalence. These differences highlight the importance of recognising how national frameworks and local practice models can shape perceptions of physiotherapy’s role within organ donor management.
Physiotherapists demonstrated limited awareness of existing guidelines or evidence specific to the management of organ donors. This mirrors Raios et al., 21 who found a reliance on non-donor evidence to inform treatment aims and interventions. Barriers such as time constraints or access issues 38 may be hindering the development of guidelines and research. This is important in the organ donor population as, although interventions are likely transferable, as described above, non-donor research does not account for the complexities of the physiological changes that deceased organ donors undergo, or the differing aims of intervention compared to other ICU patients.
Views on whether the wider MDT understood the role of physiotherapy varied. Some felt doctors and nurses were knowledgeable, while others worried about the MDT missing appropriate referrals for physiotherapy involvement. Currently there is limited evidence exploring the MDT’s understanding of the physiotherapy role in an ICU setting. Divergence in perspectives may be influenced by the extent of physiotherapy presence in individual ICUs and the availability, or lack of, a 24-h physiotherapy service. As there is limited understanding of the learning needs of the MDT regarding the physiotherapy role, this needs to be explored more in depth by asking MDT members directly.
There was strong support for a national protocol to provide guidance while encouraging clinical reasoning. O’Connor 22 had mixed responses when asking physiotherapists about the use of protocols for organ donation, noting concerns that protocols could stifle clinician judgement. Although no protocols exist on the role of physiotherapy in organ donation, protocols have been beneficial in the management of organ donors, as highlighted by Raios et al. 14 Flexible guidance advising physiotherapists to assess and treat donors as clinically indicated would likely be well received.
Strengths and limitations
The mixed methods design enhanced data breadth and depth; surveys provided broad trends, while interviews offered detailed personal experiences. Rigour was enhanced through piloting, secondary analysis and researcher reflexivity. A wide demographic and geographic sample also strengthens generalisability.
Although the ACPRC newsletter reaches respiratory physiotherapists across the UK, the number of subscribers who work specifically in critical care is unknown. With a monthly open rate of only 51.6%, the number of eligible clinicians who viewed the advertisement is unknown. This meant a survey response rate could not be calculated, limiting certainty regarding the representativeness of the findings. Self-selection may have introduced volunteer bias, with participants more interested in organ donation than the wider population. Social desirability bias was also a risk, though mitigated through anonymity where possible.
The mixed methods approach also introduced inter-method constraints. As interview questions were informed by survey findings, the qualitative results may have been narrower in scope than if developed independently. Integration required aligning qualitative themes with quantitative categories, resulting in some loss of nuance.
Implications for practice and future research
Our findings suggest that physiotherapists across the UK are currently involved in the care of organ donation patients and view their role positively. These insights may encourage clinicians to reflect on the potential benefits of physiotherapy input for potential organ donors and to consider more consistent involvement in their management. Future research should further explore the role of physiotherapy in deceased organ donation with consideration to its impact on patient outcomes and organ procurement rates. Use of the theoretical domains framework 39 and theoretical framework of acceptability 40 may allow for better understanding of the barriers and facilitators to practice. This study did not explore whether the limited use of certain interventions reflected issues of capability, opportunity or other behavioural determinants. Understanding these behavioural drivers would be valuable in informing future implementation efforts. Further consideration of institutional factors, such as organisational culture, leadership support and resource availability would also be valuable for informing future implementation efforts. In the absence of evidence-based protocols, there is a need to work towards a national consensus by drawing on clinical experience and respiratory expertise.
Conclusion
This study explored current UK physiotherapy practice and perceptions in managing deceased organ donors. Despite positive attitudes towards the role, practice remains inconsistent due to a lack of guidelines, clinician uncertainty, and ethical complexities. Participants emphasised the need to raise awareness, educate the MDT, and define the role through a national guidance. Given the difficulties in conducting high-level evidence studies in organ donation, future efforts should aim to create consensus-based guidance through expert collaboration.
Supplemental Material
sj-docx-1-inc-10.1177_17511437261423807 – Supplemental material for Physiotherapy in deceased organ donation: A mixed methods study of current practice and perceptions amongst UK-based intensive care physiotherapists
Supplemental material, sj-docx-1-inc-10.1177_17511437261423807 for Physiotherapy in deceased organ donation: A mixed methods study of current practice and perceptions amongst UK-based intensive care physiotherapists by Shannon Saunders, Ema Swingwood, Zoe van Willigen, Sarah Rand and Harriet Shannon in Journal of the Intensive Care Society
Footnotes
Abbreviations
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.