Abstract
Background
High prevalence of ocular surface disorders includes eye dryness and corneal ulcer among intensive care unit patients remains an issue. This study aimed to compare the effectiveness of Lubratex ointment and vitamin A eye ointment in preventing ocular surface disorders in intensive care unit patients.
Methods
A single-center randomized clinical trial was conducted in critically ill patients of vitamin A eye ointment and Lubratex ointment in preventing ocular surface disorders. Forty-one eligible patients were randomly assigned to administered vitamin A eye ointment in one eye and Lubratex ointment in the other eye. After five days, using fluorescein and Schirmer's tests, an ophthalmologist examined patients and specified those with ocular surface disorders.
Results
The results showed a significant decrease in the incidence of dry eye (
Conclusions
Although Lubratex ointment was more effective than vitamin A ointment in preventing ocular surface disorders, further research is needed to confirm the findings of the present study.
Introduction
Eye care is a significant aspect of the caring process of critically ill patients 1 but often neglected due to continuous focus on the life-threatening situations in this group of patients. 2 In the intensive care unit (ICU), the eyes of patients are exposed to complications such as dry eye, incomplete eyelid closure, conjunctival edema, and defects in the integrity of the cornea.3,4 Ocular surface disorders (OSDs) affect 23–60% of ICU patients. 1
Lagophthalmos is considered as the defective or incomplete closure of the eyelids. 5 Lagophthalmos disables the first protective mechanism of the eyes of these patients, which may predispose them to eye dryness and corneal epithelial breakdown.6,7 In healthy people, the eyelids can protect eyes from trauma and dry eye. Tears keep the eye surface moist and eliminate microorganisms. However, in critically ill patients, these mechanisms can be impaired resulting in a predisposition to dry eye and corneal abrasion, tear, and infection. 8 A recent study reported a 59.4% incidence of corneal injury in patients admitted to the ICUs. 9
Intensive care nurses are often preoccupied by life-threatening issues and this can reduce their attention to other body parts, including the eyes of patients. 10 Several studies have been conducted to assess the effect of various eye care techniques in preventing OSDs in critically ill patients and different results were reported. For example, in Lenart and Garrity 11 study, Lubratex ointment was more effective than glue and passive eyelid closure. Koroloff et al. and So et al. found no significant difference between the use of Lubratex ointment and polyethylene covers in preventing corneal injury.10,12 Babamohamadi et al. 13 reported that vitamin A was more effective in preventing OSDs in ICU patients than the moist chamber. The use of ointment (such as simple eye ointment, Lacrilube (Lubratex) and vitamin A) is recommended in preventing and treatment of OSDs. This needs to be applied correctly into the eye. 1
Despite all reported clinical trials, the high prevalence of ocular complications among ICU patients still remains an issue. Hence, there is a need to develop new protocols to minimize the consequences of eye dryness among these patients. In this regard, this study was conducted to compare the effectiveness of Lubratex ointment and vitamin A eye ointment in preventing dry eye and corneal ulcer in patients admitted to the ICU.
Methods
Design
A single-center, triple-blind, two-armed, randomized clinical trial design was conducted to examine the effectiveness of Lubratex ointment and vitamin A eye ointment in preventing the ocular surface disorders in ICU patients.
Setting and participants
Forty-one participants were recruited using the convenience sampling method during 2017 from an ICU general in a large referral teaching hospital in Shahroud, Iran (Figure 1).
The process of the study according to the CONSORT flow diagram (2010).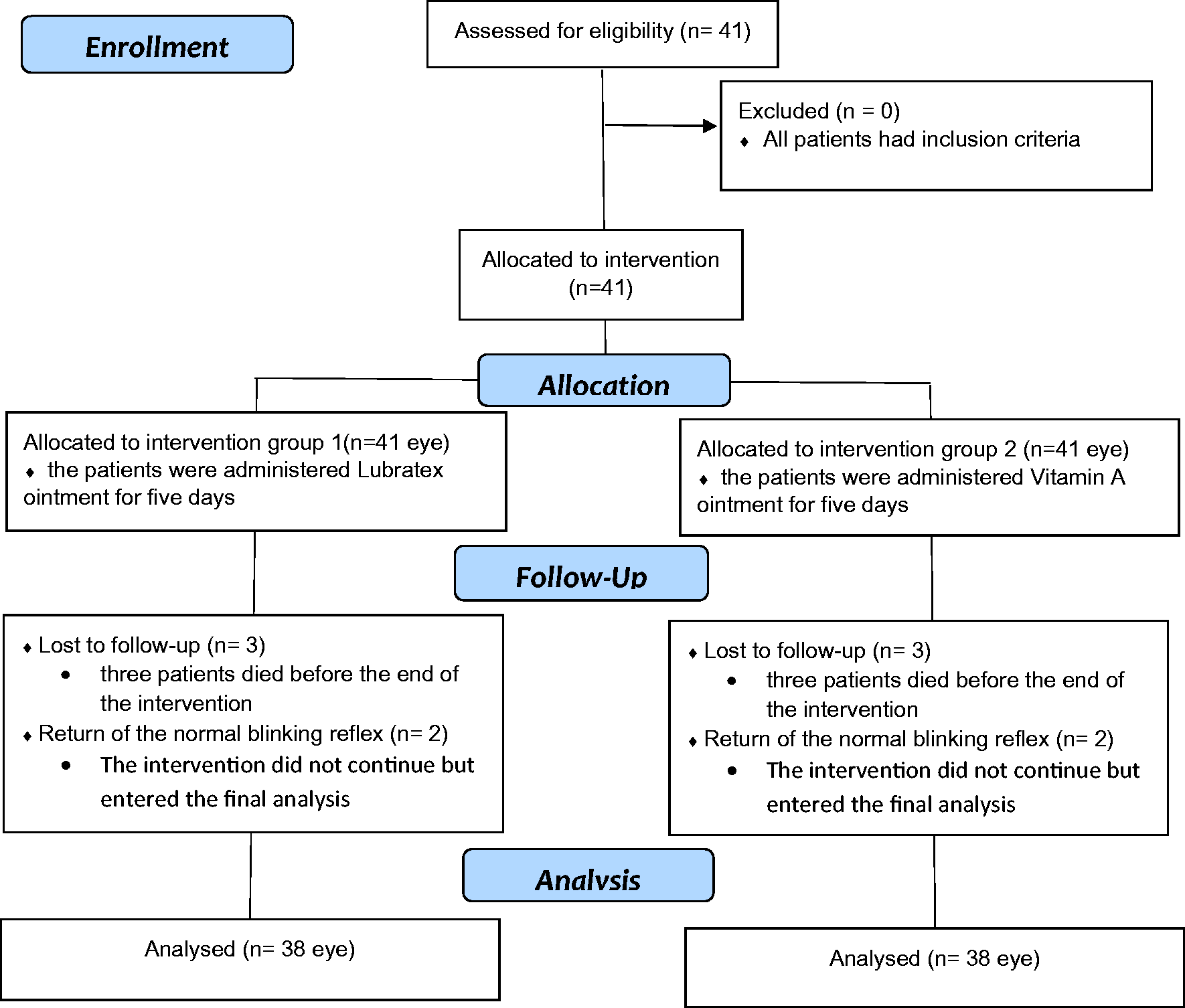
Inclusion criteria and recruitment
The inclusion criteria included admitted to the ICU, the need for mechanical ventilation and endotracheal tube, being older than 18 years, Glasgow Coma Scale (GCS) score of 3–10, healthy cornea (negative fluorescein test), no symptoms of dry eye, absence of facial trauma (preventing provision of eye care), absence of any severe ocular ulcer or injury, no history of eye surgery, absence of eye infection, taking no ophthalmic drug and signing informed written consent form (by patient companion). In addition, in the case of issues including return of the normal blinking reflex (due to sudden alertness), patients who received sedation or paralyzing agents, the demand of a patient's family to leave the study, transfer of a patient to other hospital units, dying before the end of the intervention and the sensitivity to Lubratex and vitamin A eye ointment, the participants were excluded from the study.
Sample size
Based on the results from Ahmadi Nejad et al.'s
6
study, and with a power of 80%, α = 0.05,
Intervention
Severity of ocular surface disease.

Then, the random allocation sequence was obtained by the methodologist with software (quadruple blocks) by using the SPSS syntax. Considering the block size of four, all patients (
Four nurses (one nurse in the morning shift, one nurse in the evening shift, and two nurses in the night shift) provided care to the patients. Groups A and B received the interventions in a different order. Group A received one dose of Lubratex on their right eyes followed by one dose of vitamin A eye ointment on their left eyes. Group B received one dose of vitamin A eye ointment on their right eyes followed by one dose of Lubratex on their left eyes. The nurses were trained equally by the researcher and the ophthalmologist, and their performance (eye care provision) was monitored and tested. They provided one dose of eye care every morning and evening shifts and two doses at each night shift (each dose of eye care contained 2 cm of Lubratex (5 g, made by Sinadarou Labs Company) or vitamin A eye ointment (3.5 g, made by Sinadarou Labs Company) every 6 h). After each ointment's administration, the eyes were closed by the hand. The care lasted for five days. The blinking was observed during the control of GCS and stimulating the patient every hour simultaneously with the control of vital signs, and within five days, patients who blinked were excluded from intervention.
On the fifth day, a nurse washed both the eyes of each patient with sterile water. Then, by using the fluorescein and Schirmer's tests, the ophthalmologist examined the patients and recorded the results. In this study, all patients, the data collector, and the data analyzer were blinded.
Ethical considerations
The research proposal was approved by the Medical Ethics Committee affiliated with Shahroud University of Medical Sciences (decree code: IR.SHMU.REC.1396.18). The research protocol was registered at the IRCT website under the number of IRCT2017040433206N1. The permission to enter the research zone was obtained from the hospitals' authorities. The patients in this study due to the low level of consciousness were unable to provide informed consent, and therefore informed written consent was obtained from the patient companions after providing required information about the study.
Statistical methods
SPSS version 22 was used for the data analysis. Descriptive statistics including mean and standard deviation for quantitative variables and frequency and percentage for qualitative variables were applied to describe these variables. Also, the McNemar test was used to determine the differences in the frequency incidence of OSDs between the two study groups. In addition, Chi-square and Fisher exact tests were conducted to evaluate the relationships between the incidence of OSDs with the variables of age, gender, level of consciousness, cause and duration of hospitalization, and eyelid position. Statistical tests were two tailed and
Results
Out of 41 subjects, three patients died before the end of the intervention, and for two patients the blinking reflex returned to normal during the study period and the intervention did not continue but entered the final analysis. Finally, 38 patients were analyzed. A total of 38 patients (76 eyes) admitted to the ICU participated in this study. The mean and the standard deviation (SD) of patients' age was 57.6 (16.6) years and the mean (SD) hospital stay was 5.6 (0.9) days. Most of the patients (66.7%) were men. Multiple traumas were the most common cause of hospitalization (38.9%). Based on the GCS scale, the most frequent consciousness levels were 5 (19.4%) and 7 (19.4%), respectively. Grade 1 was the most prevalent eyelid position among both the vitamin A eye ointment (41.7%) and Lubratex ointment (38.9%) groups. There was no significant difference between the two groups in terms of the eyelid position (
In total, 4 (11.1%) and 17 (47.2%) cases of dry eye were reported in the Lubratex and vitamin A eye ointment eyes, respectively. In addition, 3 (8.3%) and 15 (41.7%) cases of corneal ulcer were reported in the Lubratex and vitamin A eye ointment groups, respectively.
The comparison between the studied groups in terms of frequency of dry eye and corneal ulcer.
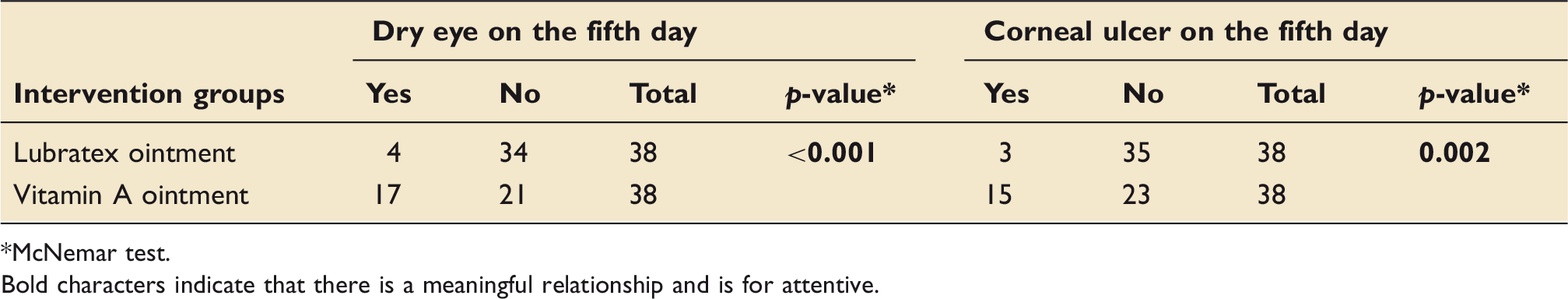

*McNemar test. Bold characters indicate that there is a meaningful relationship and is for attentive.
Distribution of dry eye and corneal ulcer in participants by demographic factors.
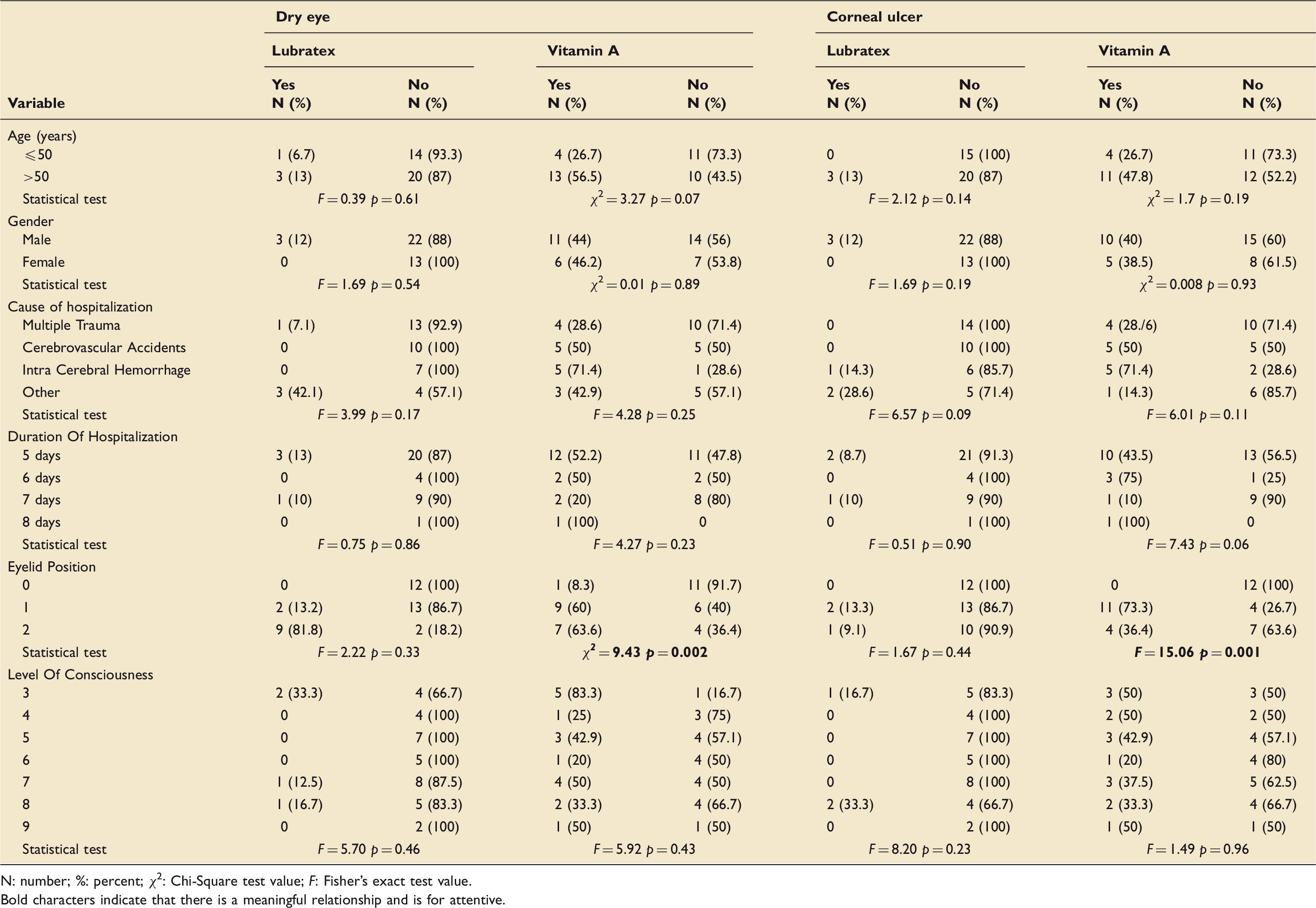
N: number; %: percent;
Grading for eyelid position.

Discussion
The findings of this study showed a significant decrease in the amount of dry eye and corneal ulcer with the use of Lubratex ointment. Also, there was a significant difference between the incidence of dry eye and corneal ulcer with eyelid position in vitamin A ointment group.
Grade 1 was the most prevalent eyelid position among both groups. In the studies of Koroloff et al. 12 and Sivasankar et al., 15 28% and 32% of the patients suffered from Lagophthalmos, respectively, which is consistent with the results of this study.
The incidence of OSDs in the Lubratex group was significantly lower than that of the vitamin A eye ointment group. The result of Lenart and Garrity 11 study showed that the Lubratex ointment was significantly more effective than the glue and passive eyelid closure. But in Koroloff et al.'s 12 study, the incidence of corneal injury in the polyethylene cover group was significantly lower than that of the Lubratex ointment group. Zhou et al. 16 conducted a meta-analysis and concluded that the polyethylene cover can more effectively protect the cornea. The study of Kalhori et al. 17 also suggested the use of polyethylene cover as nonaggressive, non-pharmaceutical nursing, and therapeutic method for the prevention of keratopathy in the patient hospitalized in ICU. The difference may be due to the different hospitalization causes or interventions.
Ahmadi Nejad et al. 6 investigated the effect of two eye care practices in preventing OSDs in patients admitted to the ICU. They found that in the Lubratex ointment group, there was no significant difference between the incidence of OSDs and the variables of age, gender, the cause of hospitalization, eyelid position, and the duration of stay. The studies of So et al., 10 Ezra et al., 14 Lenart and Garrity, 11 and Sharifi Tabar et al. 18 were consistent with the current study. Hernandez and Mannis 19 in their study recorded the highest incidence of keratopathy in traumatic patients. However, the result of this study was not consistent with the present study, presumably attributed to the different hospitalization causes and durations.
Consistent with the present study, Babamohamadi et al. 13 reported that there was no significant difference between the incidence of OSDs and the variables of age, gender, duration of stay, and level of consciousness.
There was no significant relationship between the incidence of OSDs and various eyelid positions. So et al. 10 and Oh et al. 20 obtained similar findings. Sivasankar et al. 15 conducted a study to compare the efficacy of using a combination of ocular lubricants and securing tape over the eyelids (open chamber method) and observed OSDs in 30% of the studied patients. A significant relationship was observed between leaving the eyelids open and the incidence of OSDs. This was not consistent with the results of the present study, presumably attributed to the different sample sizes and research periods. In line with our investigations, Ghanei et al. conducted a study to compare three methods of wet gauze, adhesive tape, and eye ointment to prevent corneal ulceration in patients undergoing general anesthesia and observed that there were no significant differences among the three methods of preventing dry eye and corneal ulcers. 21 Dry eye and corneal ulcers had happened less in the protective method by ointment. Therefore, the use of ointment as a protective way was recommended to prevent dry eyes and corneal ulcers in patients hospitalized in the ICU.
Strengths and limitations
The main strength of this study was using two different eye care interventions to the eyes of one patient, which could lead to the elimination of many confounding variables. However, the current study had several limitations that should be considered. First, this study was a small, single-center study, and therefore further research in multi-center with larger samples is needed to confirm the findings of the present study. Second, the study population of the current study included all the ICU patients; thus, the variety of underlying diseases was limited, and this decreased the generalizability of the results. Third, the assessment of the level of consciousness and also the blink of at least every hour were performed simultaneously with the control of vital signs. If a patient blinks meanwhile and his/her blinking was not observed, an uncontrollable limitation will occur by not excluding such patients from the study. Finally, this research studied only adult patients, and it is recommended to investigate the research variables in newborn care units (NCUs) and neonatal intensive care units (NICUs), too.
Recommendation for practice
This study highlighted that the use of Lubratex ointment is an effective way for the decrease of OSDs incidence in the ICU patients. As a result, the findings of this study if replicated by other studies can be used by healthcare providers, such as clinical pharmacists, physicians, and nurses to reduce the OSDs incidence in ICU patients.
Conclusion
Although the results of this study showed that Lubratex ointment was more effective than the vitamin A eye ointment in preventing ocular surface disorders, further research is needed before it is recommended as an effective intervention in the care of intensive care unit patients.
Supplemental Material
INC912697 Supplemental Material - Supplemental material for Effectiveness of lubratex and vitamin A on ocular surface disorders in ICU patients: A randomized clinical trial
Supplemental material, INC912697 Supplemental Material for Effectiveness of lubratex and vitamin A on ocular surface disorders in ICU patients: A randomized clinical trial by Mitra Badparva, Mohammad Veshagh, Farideh Khosravi, Abbas Mardani and Hossein Ebrahimi in Journal of the Intensive Care Society
Footnotes
Acknowledgements
The present article was extracted from a master thesis in nursing which was conducted at Shahroud University of Medical Sciences. The authors would like to thank the Deputy of Research and Technology of this university and all the staff and nurses of ICU Center of Hospital who helped us in this research.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
