Abstract
In the years following the abolition of the English National Board for Nursing, Midwifery and Health Visiting in 2002, concerns were raised within the Critical Care nursing community about a lack of consistency in post-registration education programmes. In response to this, the Critical Care Network National Nurse Leads (CC3N) formed a sub-group, the Critical Care Nurse Education Review Forum (CCNERF) to address these concerns. A review of UK course provision confirmed marked inconsistency in the length, content and associated academic award. The CCNERF commenced a two-phase project, first developing national standards for critical care nurse education such as length of course and academic credit level, followed by the development of a national competency framework. Following significant review and revision, version two of the National Competency Framework for Registered Nurses in Adult Critical Care was published by CC3N in 2015. This paper introduces the National Competency Framework and provides an overview of its background, development and implementation. It then considers the future direction of UK post-registration Critical Care nurse education.
Introduction
The importance of an appropriately skilled and educated workforce is well recognised by commissioners, providers and users of healthcare.1–5 It is also recognised that adult Critical Care nursing is a demanding and highly skilled role. Advances in Intensive Care Medicine have led to critically ill patients becoming increasingly complex to care for, demanding a variety of specialised skills from the critical care nurse (CCN), 6 which requires an in-depth knowledge of the subject and the ability to safely apply that knowledge to clinical practice. 7 To achieve this, education provision accessed by adult CCNs needs to be developed through effective partnerships between clinical practice and educational providers and allow development and assessment of both theoretical knowledge and clinical competence. 6 In this way, we can ensure a quality Critical Care nursing workforce is created, that is fit for purpose and that delivers safe effective practice to vulnerable patients at the bedside.
Background
After the demise of the English National Board for Nursing Midwifery and Health Visiting, responsibility and accountability for post-registration education passed directly to the Higher Education Institutions (HEIs), as a result, concerns were voiced within the Critical Care nursing community regarding the lack of consistency across post-registration education.
1
These included concerns around the variability in:
The academic content of the curriculum The final level of clinical competence attained after completing a course The academic award attached to each course Cost and value for money
These inconsistencies led to a lack of transferability of attained critical care knowledge and clinical skills across geographical boundaries, resulting in workforce recruitment difficulties between conurbations. Concerns were identified in practice and communicated via the Critical Care networks to CC3N, where they were raised for consideration and discussion.
It was recognised that these issues were likely to have a direct impact on the quality of care delivered within Critical Care units and indirectly on the recruitment and retention of an appropriate Critical Care nursing workforce. Consequently, in 2008, CC3N formed an educational sub-group, the Critical Care Nurse Education Review Forum (CCNERF), including representatives from both practice and HEIs (detailed below in ‘writing the competencies’), to address these concerns. The forum’s first task was to undertake a review of critical care nurse education programmes across England to scope the scale of the issue. Two surveys were carried out; these were developed by CCNERF and then sent out by CC3N via the networks to Critical Care units and Critical Care course lead contacts at HEIs. The survey to critical care units asked questions about staff profiling and critical care education needs; the HEI survey asked about the academic level that critical care courses were accredited, how many credits were awarded, and whether practice competencies were included as part of the course assessment. Responses were received from 91 critical care units and 20 HEIs which were collated and presented at CCNERF; these confirmed the forums concerns about inconsistency in the areas identified above. 1
In response to these findings a two-phase project was developed by CCNERF; phase one was the development of National Standards for Critical Care Nurse Education, phase two the development of a National Competency Framework for Adult Critical Care Nurses. The National Standards were published in 2012, providing a framework to guide HEIs so that a consistent and transferable approach is adopted in the development of Critical Care nursing programmes. The standards include specific statements as to the level and number of academic credits a course should achieve; the need to include a combination of theoretical and practice assessment and the need use the national competencies to assess practice competence once these became available. 1 Whilst it is acknowledged that HEIs would normally set course credit bearings in accordance with their own institutional standards, it was apparent that this had led to inconsistency and that the National Standards were needed as part of CCNERF’s work in order to achieve the goal of consistent and transferable courses. It is internationally recognised that to ensure the critical care nursing workforce is fit for purpose, in the context of increasing patient acuity, education needs to include a combination of theoretical knowledge and practice.6,7 Thus, supporting the standard that the assessment of practice competence must be included in critical care courses. The CCNERF then moved on to develop the National Competency Framework that would identify the specific areas of clinical practice that would make up the practice competency assessment.
Writing the National Competency Framework
Phase 2 of the CCNERF project was to develop a suite of core competencies. The original plan had been to utilise existing Skills for Health (SfH) resources, in particular to adopt any National Occupational Standards (NOS) that could be transferred into the Critical Care arena. However, when reviewed in some detail, it became clear that existing NOS were too universal and generalised to be suitable for implementation in critical care. As a result, the group embarked on identifying and describing the essential skills needed by registered CCNs.
A working group was established in collaboration with wider stakeholders, which included critical care nursing colleagues, practice-based educators, managers, critical care networks and academic programme leads and lecturers. Email invitations to join the working group were sent via the networks to clinical and HEI representatives, the working group being formed from those who responded to this invitation. Representatives were included from England, Wales and Northern Ireland; professional nursing bodies were represented and included the Royal College of Nursing (RCN), British Association for Critical Care Nurses (BACCN), Intensive Care Society (ICS) and the Independent Sector. Additional members were then invited when their input was seen as valuable in the development. Unfortunately, despite attempts to engage, the group were unable to secure any representation from Scottish colleagues.
A framework of competencies was developed, organised into three discrete steps to reflect the progression of the nurse from a novice, with no previous experience as a registered nurse in critical care, through to a competent bedside practitioner; identifying in clear measurable terms the level of performance required for specific skills and the evaluation of skill acquisition against a measurable criteria (illustrated in Figure 1). The standards describe competence as: “The combination of skills, knowledge and attitudes, values and technical abilities that underpin safe and effective Critical Care nursing care and interventions”
1
(p. 14).
The three steps of the National Competency Framework. (Reproduced with permission from Critical Care Network National Nurse Leads, CC3N 2016).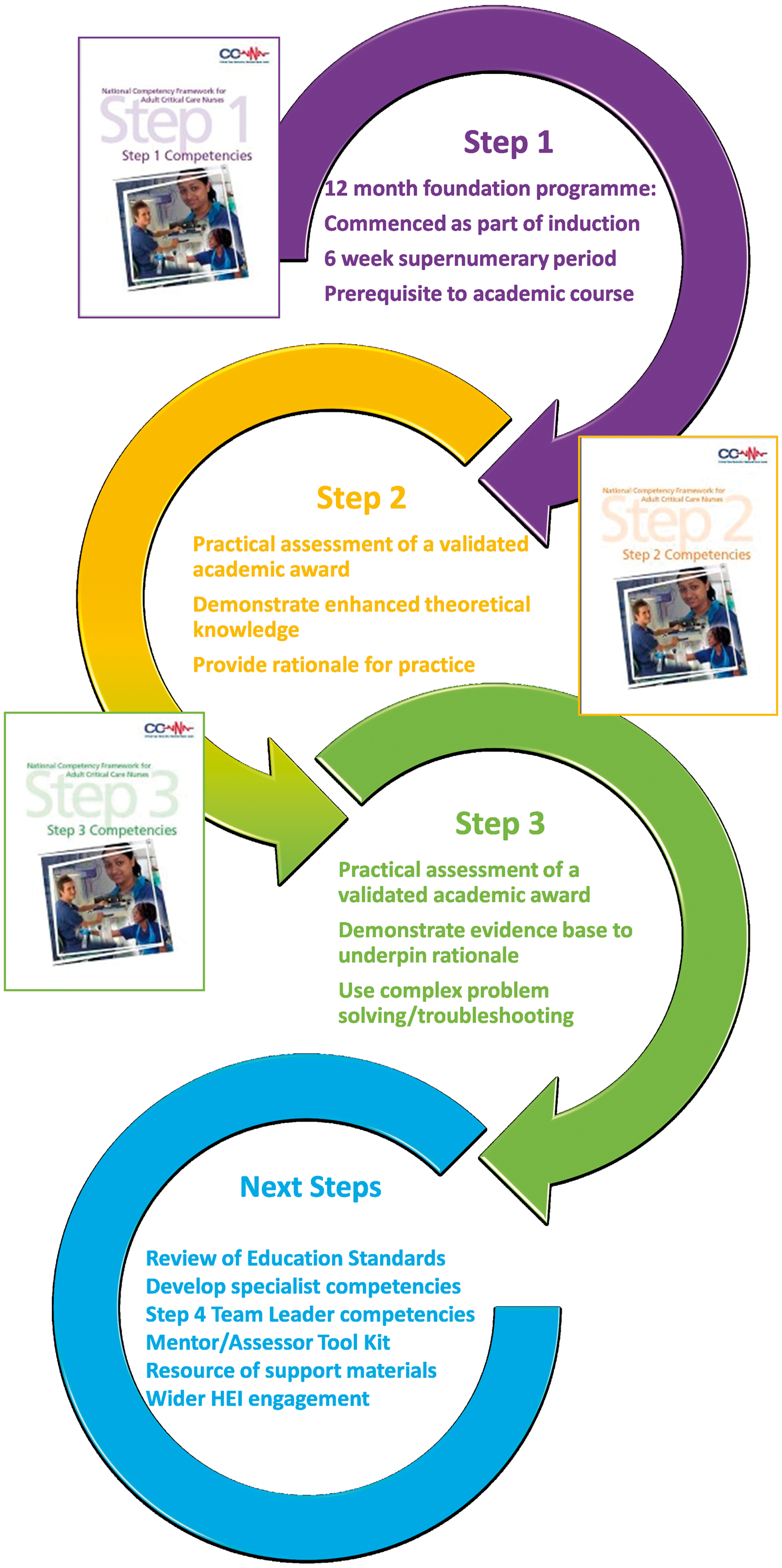
Step 1 competencies are commenced when a nurse starts in Critical Care where s/he has no previous experience of the speciality and can be incorporated into a preceptorship programme. Preceptorship is defined by the Department of Health as: “A period of structured transition for the newly registered practitioner during which he or she will be supported by a preceptor, to develop their confidence as an autonomous professional, refine skills, values and behaviours and to continue on their journey of life-long learning
8
(p. 11).
To support successful implementation of the framework, the following recommendations need to be in place locally (Note: Detailed descriptions relating to these aspects of local support are provided in UK Critical Care Nursing Alliance (UKCCNA), Quality Assurance Standards.
13
):
Learning contract Designated practice educator Supernumerary study time Learner and mentor clinical time A creative environment for learning Mentor and assessor quality assurance
Validation process
Professional consensus within the group was reached on each competency statement and the supporting recommendations. Following national consultation with critical care nursing practitioners, comments were considered and changes made where necessary. Once the consultation process was complete, the endorsing organisations were approached and the documents were processed through their relevant boards for consideration. The group was successful in gaining endorsement from all the organisations approached. Version one of the national competency framework for registered nurses in adult Critical Care was published by CC3N in 2012.
Review, feedback and development of version two of the competency framework
After the publication of the competencies in 2012, the CCNERF reconvened at the end of 2013 to review how the implementation of the competencies was progressing. This obtained feedback from members from different areas as to the experiences and views of both early implementers and those who had not yet adopted the competencies.
Discussion and debate arose when key stakeholders questioned which elements of Critical Care practice were essential and possibly non-essential to a general Critical Care unit. The key focus of the competency framework was also reviewed and discussed; whether the framework was purely focused on the competency requirement of an adult Critical Care nursing course, or if wider Critical Care workforce development issues should be considered. There was further debate around whether Steps 2 and 3 should be amalgamated into one document for simplicity and efficiency in a Critical Care academic course and to prevent duplication. It was decided not to, so that the potential for benchmarking natural developmental of skill acquisition for a learner in Critical Care was not compromised, especially when not all UK nurses have the opportunity to access a course. This is reflected in current guidelines that a minimum of 50% of nurses in UK critical care units should have completed a post-registration Critical Care course. 14
One specific challenge was that not all units had exposure to renal replacement therapies (RRT) or cared for patients with neurological injury, which meant a nurse could not be assessed or signed off as competent. This raised a fundamental question as to what should be deemed as core elements of Critical Care practice, which were not only essential but also achievable in a general Critical Care unit. Some units, albeit a minority, did not have the facility for RRT and therefore their staff would not have or indeed require the skill. The discussions around care of patients with neurological injury focused on the lack of exposure to this group of specialist patients who in many instances are transferred to tertiary centres so they never become patients in general Critical Care units.
Feedback was requested in May 2014 from Critical Care units via CC3N, asking whether the competency requirements pertaining to RRT and neurologically injured patients were achievable and for further feedback comments on this. A total of 26 responses were received; of the 19 units that answered in relation to RRT, the majority (16) indicated that the attainment of the competencies was achievable. Following discussion, it was agreed that the framework would be compromised by removing the RRT competencies to suit a handful of units and the decision was made that the RRT competencies would remain as core in the framework, as the under-pinning knowledge was relevant to all units. However, the practical skills assessment would remain in the document but only be assessed in units that undertook renal replace therapy.
Summary of changes to framework in version 2.

NMC: Nursing and Midwifery Council.
An example of one of the competency statements from step two of the framework is shown in Figure 2. The three-step documents of the competency framework can be accessed in full on the CC3N website http://www.cc3n.org.uk/competency-framework/4577977310.
Example of a competency statement.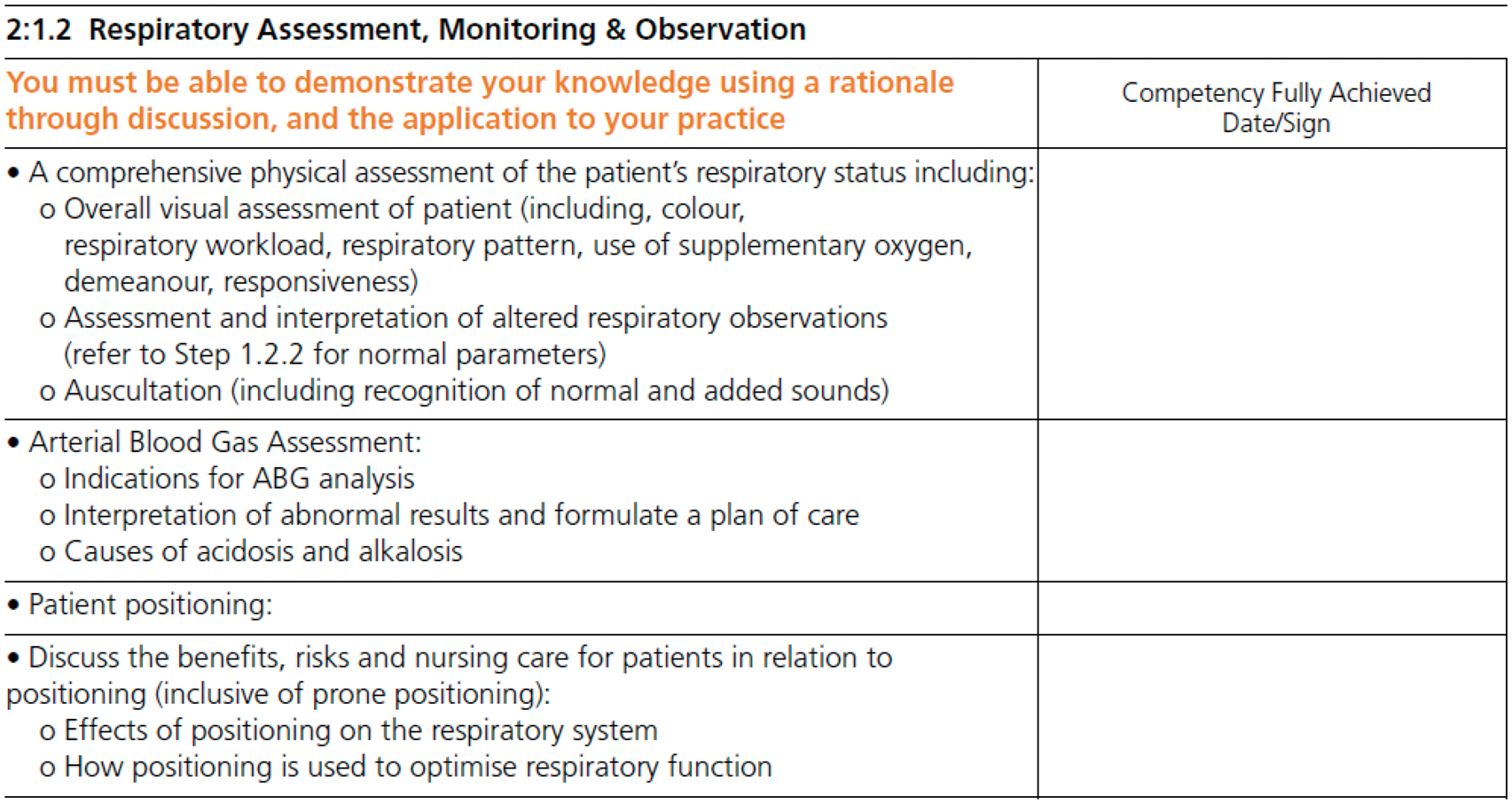
Implementation of the National Competency Framework
The National Competency Framework provides a clear progression plan for nurses entering adult Critical Care, from the newly qualified registrant through to the experienced nurse who has completed step 3 as part of a programme within an HEI. Completion of a post-registration award in Critical Care nursing using the National Competency Framework, alongside the National Standards for Critical Care Nurse Education, is a core standard for nursing staff in the Guidelines for the Provision of Intensive Care Services (GPICS), published by the Faculty of Intensive Care Medicine (FICM) and the Intensive Care Society (ICS) in 2015 and should have been achieved by a minimum of 50% of registered nursing staff within a unit. GPICS 14 is endorsed by 19 organisations representing medicine, nursing and allied health professionals; for nursing this includes CC3N, the BACCN and the UKCCNA. The standards also state that all nursing staff starting in Critical Care should be commenced on step 1 of the National Competency Framework, with an initial supernumerary period which should be a minimum of six weeks for newly qualified staff. 14
In addition to satisfying the core standards discussed, the National Competency Framework document can be used to support nursing staff in the revalidation process required of all registered nurses by the Nursing and Midwifery Council from April 2016 onwards. 12 The framework also allows senior nurses to benchmark the competency level of nursing staff within their unit, aiding workforce development. Processes also need to be in place to ensure that workplace learning adheres to the quality standards that underpin student placements in Critical Care units, during post-registration educational programmes. 13 These standards set out the responsibility of the workplace area for the learners enrolled on a post-registration programme.
Many HEIs have adopted the National Competency Framework into their post-registration critical care awards, those who have not will need to consider how best to adapt their programmes to incorporate them. As nursing is now a degree level (level 6) entry profession, post-registration education will be increasingly required at masters level (level 7); feedback to the CCNERF in 2014 on course provision would suggest a number of HEIs already offer courses at both levels 6 and 7.
HEIs will therefore need to provide post-registration Critical Care courses that satisfy the professional standard by utilising steps 2 and 3 of the National Competency Framework for the practice element whilst adhering to the Quality Assurance Agency for Higher Education (QAA) standards in ‘The Quality Code’. 15 In particular, part A of the Quality Code which includes the frameworks for higher education qualifications, identifying the characteristics of study at differing academic levels, such as analysis, critical evaluation and original application of knowledge. 15
The step competencies are signed off in practice when they are achieved; there is no grading of pass for the step competencies. Therefore, within academic courses, the step competencies will need to be a pass/fail element of assessment, sitting alongside other assessment methods that allow for the demonstration of levels 6 and 7 academic characteristics.
Experience in practice
Competency subject areas by framework step.
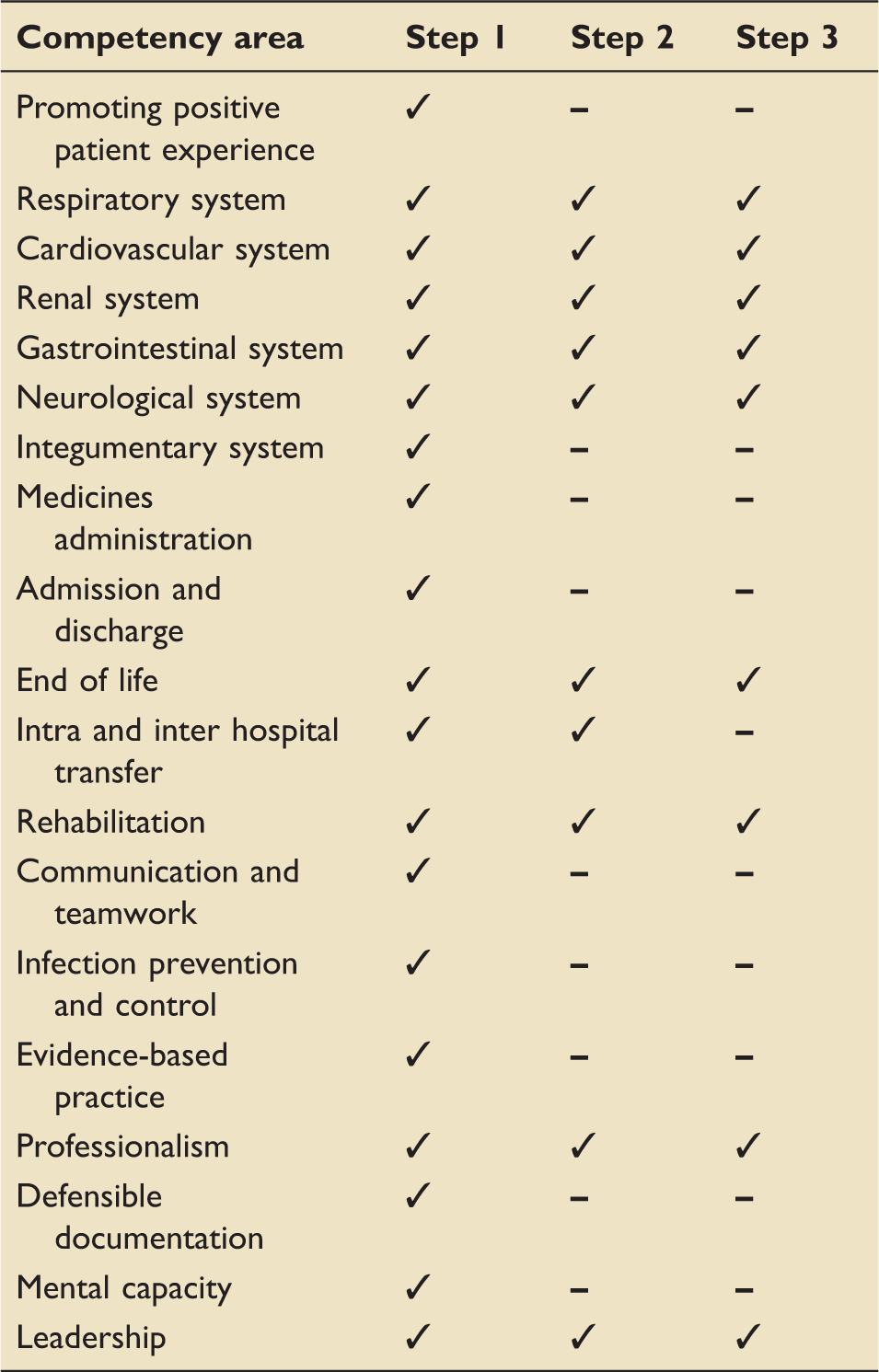
Each unit practice development team will need to decide what support is required for those staff acting as assessors for staff completing the competency framework.
Future direction
The National Competency Framework for Registered Nurses in Adult Critical Care is an evolving document that will continue to be reviewed in the future to ensure it remains relevant to clinical practice and fit for the future workforce. A review of the framework will also be required which focuses on the challenges encountered and implementation strategies, along with a scoping exercise to map the current adoption of the competency framework. The provision of appropriate educational development opportunities for staff that are relevant to the needs of the clinical service and have been developed in partnership between professional bodies and education providers are priorities in the DH16 mandate to Health Education England. This, along with the previously discussed standards in GPICS, 14 will hopefully act as drivers to support continued adoption of the national standards and competency framework.
There are specialist units throughout the UK who require competencies that are more specific to their specialist area and are more in-depth than are covered within the competency framework. To accommodate these units, there are plans to develop specialist ‘bolt-ons’; these would be specific sets of competencies to cover areas such as neurology, cardiothoracic, burns and trauma. This will allow the competency framework to remain generic and achievable by all general Critical Care areas while allowing the inclusion of the extended skills and knowledge required by the specialised units. There are also plans to develop a step 4 of the competency framework, which would focus on the skills and competencies required for a band 6/7 nurse concentrating more on the management and leadership areas of the role. The development of this proposed step will give a clear development structure enabling effective succession planning, growing our own future leaders in Critical Care.
The competency framework has been well received by a number of organisations within the UK and has international interest from Canada, Finland, the Middle East, Nepal, India and Gibraltar, suggesting a wider interest in achieving consistency around education in Critical Care that is comprehensive and transferable. This is supported by Endacott et al. 17 whose survey of CCN education in 24 European countries showed that 54.5% identified a lack of national standards in CCN education as a problem. From their findings, they identified the need for CCN to be recognised as a speciality across Europe (currently only recognised in 54.2% of countries), and for the development of a Europe wide specialist education programme in order to address the barriers that exist to the advancement of CCN across Europe. 17 A similar pattern of inconsistency was previously found in intensive care medicine training which led to the introduction of the CoBaTrICE framework in 2003, which has since been adopted by 15 countries in Europe with a further 12 planning to adopt the framework. 18 The National Standards for Critical Care Nurse Education 1 and the National Competency Framework for Registered Nurses in Adult Critical Care, 3 sit well in the current professional climate which seeks to promote quality Critical Care through consistency of approach to education and would have much to offer any future Europe-wide approach.
Conclusion
In 2015, the CCNERF, on behalf of CC3N published version two of the National Competency Framework for Adult Critical Care Nurses. 3 We believe that alongside the National Standards for Critical Care Nurse Education, 1 the framework provides a basis for post-registration education that is consistent, transferable and fit for purpose. The step competencies provide a standardised framework for practice development from the novice starting out in Critical Care to the experienced and competent nurse who has completed a post-registration award. Future proposed developments will extend this into areas of specialist critical care provision and to senior nurses focusing on leadership and management. We feel the increasing adoption of the national competency framework and positive reaction from stakeholders is indicative of a shared commitment within the Critical Care nursing community to strive for quality and consistency within of our workforce.
Footnotes
Acknowledgements
Thanks to all the members of CCNERF. Thanks are also extended to the original 2012 working party.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
