Abstract
Menstrual cycle (MC)-related health issues can significantly impact female athletes’ performance and well-being. However, research on the female para-population remains limited, with existing studies often focusing on specific sports or disability types. This review aims to summarize existing findings on MC-related concerns among female para-athletes and highlight gaps in current research. Literature search was conducted between December 2024 and June 2025 using PubMed (n = 1504) and Scopus (n = 565), retrieving 2069 articles. Keywords were selected collaboratively and combined using Boolean operators to ensure a comprehensive search. After removing 118 duplicates, 1951 articles were screened by two reviewers. Only 5 articles met the inclusion criteria after title and abstract screening. These 5 articles, when reviewed, revealed a high prevalence of MC-related issues among female para-athletes, with 63.4% reporting that MC affected their health and performance. Moreover, there is a low awareness of MC-related health issues, suggesting a lack of education within the broader para-athletic population. Although previous research has explored various aspects of MC experiences, disability-related factors, such as the type and nature of the disability, have largely been overlooked. Existing evidence is constrained not only by small sample sizes but also by the underrepresentation of para-athletes. Importantly, there is a significant gap in the literature concerning the unique perspectives and challenges faced by female para-athletes from Asian countries, as research focusing on this population remains limited. Thus, there is a pressing need for sport, exercise, and impairment-specific research to better understand the specific MC-related issues and experiences of female para-athletes.
Introduction
The menstrual cycle (MC) has a bidirectional relationship with both psychological and physiological aspects of health in female athletes. 1 As international research increasingly addresses MC-related topics, the evidence demonstrates that the MC can significantly influence female athletes’ health, well-being, training, and performance. 2 These effects extend beyond physiology, and are being shaped by cultural beliefs, social expectations 3 and logistical challenges, all of which influence how athletes perceive and manage their menstrual experiences. Although global studies4–6 have identified the prevalence of factors associated with the Female Athlete Triad (FAT) among elite para-athletes, but the perspectives of Asian para-athletes remain conspicuously absent from the literature. This represents a critical gap in understanding the intersection of gender, disability, and cultural context in sport.
The MC, typically lasting 21 to 35 days and classified as eumenorrhea when regular, comprises several phases: early follicular, late follicular, ovulatory, and luteal.7,8 Fluctuations in oestrogen and progesterone across these phases influence key physiological systems—including cardiovascular function, thermoregulation, and energy metabolism—which may, in turn, affect physical performance and exercise capacity.9–11 Additionally, fluctuations in sleep quality, readiness to train, training quality, fitness, and overall performance were perceived throughout the MC phases. 11 While many athletes believe their performance is affected by their MC, objective data from eumenorrheic athletes have yielded inconsistent findings. 7 Nevertheless, understanding these hormonal dynamics is essential for developing individualized training programs that align with athletes’ physiological responses throughout the cycle. These physiological responses can be particularly relevant when considering broader health concerns such as energy availability.
Relative Energy Deficiency in Sport (REDs), as defined by the 2023 IOC Consensus, refers to a medically recognized syndrome resulting from prolonged low energy availability (LEA), affecting multiple physiological functions. 12 In able-bodied athletes, LEA is typically identified through biomarkers such as reduced levels of insulin-like growth factor-1, testosterone, and oestrogen, which are linked to impaired bone health and other clinical symptoms. 13 However, applying these diagnostic markers to para-athletes is complex due to their diverse physiological profiles and underlying impairments. 14 Para-athletes may be at a heightened risk for REDs compared to their able-bodied counterparts because of several interacting factors. 12 These include neurological impairments, altered metabolic function, and movement inefficiencies that can increase energy expenditure during both training and daily activities.4,14,15 For example, ambulatory para-athletes and those with limb loss may require more energy for mobility, thereby increasing the risk of inadvertent LEA.16,17 Furthermore, MC fluctuations—already recognized as a sensitive indicator of LEA in able-bodied athletes—remain underexplored in para-sport populations. This lack of investigation limits our understanding of how MC disturbances may reflect or exacerbate REDs risk in female para-athletes, potentially affecting their recovery, training adaptation, and overall performance.
MC-related issues, such as hypothalamic amenorrhea, are the indicators of LEA or REDs and are well documented in the literature. 12 The hypothalamic-pituitary-gonadal axis (HPGA) may be affected by disabilities and underpinning injuries and, in turn, negatively impact MC in female para-athletes. 4 Additionally, studies on non-athletic females with cerebral palsy (CP), spinal cord injuries (SCI), and traumatic brain injuries (TBI) highlight impairment-specific menstrual dysfunction.4,18,19 The age of menarche tends to be higher in females with CP, 18 with approximately 29.4% of adolescents with CP experiencing menstrual dysfunction. 4 In cases of acute SCI, transient amenorrhea is common, typically lasting an average of five months. 4 Following TBI, nearly half of the affected females report amenorrhea, with prevalence varying according to the severity of the injury. 4 In addition to impairment-related factors, training load, energy balance, and sport-specific demands may adversely affect menstrual health in para-athletic population.14,15,20 However, it is unclear whether this is primarily due to low energy availability (LEA) or other contributing factors, and further research is necessary to explore these issues. 15 Previous studies5,14 have explored health aspects in para-athletes, such as RED-S and FAT, these findings are often disability specific (SCI, wheelchair basketball, and track athletes) and cannot be generalized across all categories of para-sports.
A recent study on Indian endurance athletes reported that most athletes neither monitored their MC nor adjusted their training regimens according to it. Moreover, it was found that these athletes exhibit inadequate communication and lack basic knowledge of MC-related issues. 11 Similarly, McGawley et al. (2023) highlighted that this insufficient knowledge of MC-related health and a significant communication gap between athletes and sports professionals contribute to poor menstrual health literacy. 21 Athletes often avoid conversations focused on MC, due to fear of being misunderstood, which is further influenced by gender dynamics, cultural and social taboos. 3 In India, stigma and taboos surrounding the MC remain prevalent, with studies highlighting negative perceptions of menstruation.22,23
Altogether, there is a significant lack of information regarding menstrual health, attitudes, and challenges faced by female para-athletes from Asian countries, creating a major gap in understanding their specific needs. Therefore, this review aims to summarize the research on menstrual health and perceptions among female para-athletes and discuss the need for future investigations into para-athletes and their unique challenges.
Methodology
A narrative review was conducted with a structured literature review on June 8th using E-databases PubMed (n = 1504) and Scopus (n = 565), which retrieved a total of 2069 articles (see Figure 1). Keywords for Menstrual cycle, Para-athlete, Female athlete, Performance, and Menstrual Health were selected collaboratively by all reviewers. Keywords were connected using the OR, and concepts were linked using the AND Boolean operators (see Table 1). Every keyword was searched in “all fields” to ensure a thorough investigation.
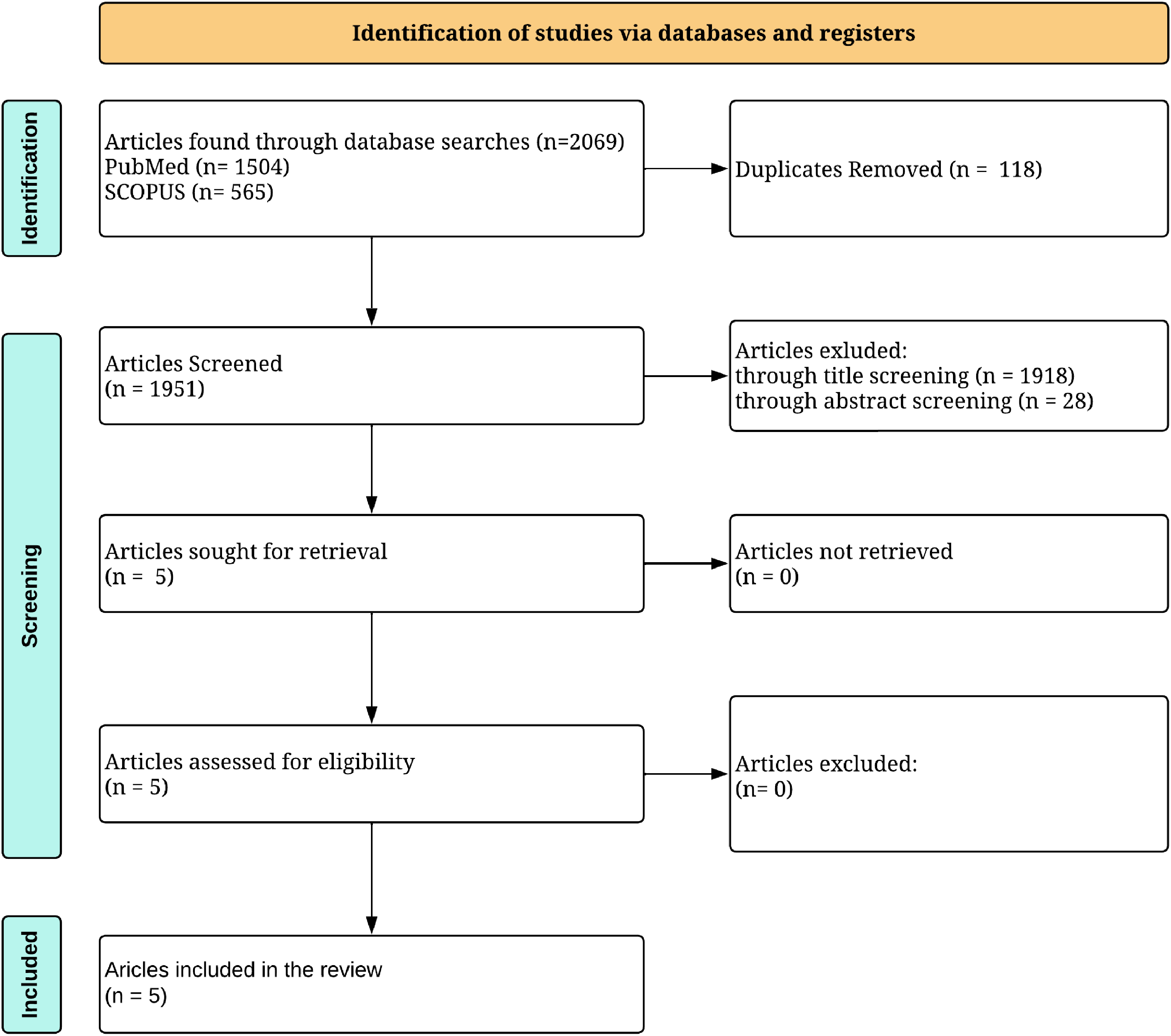
PRISMA flow diagram-produced in lucidchart.com based on the Prisma 2020 statement (24).
Keywords for the literature search.
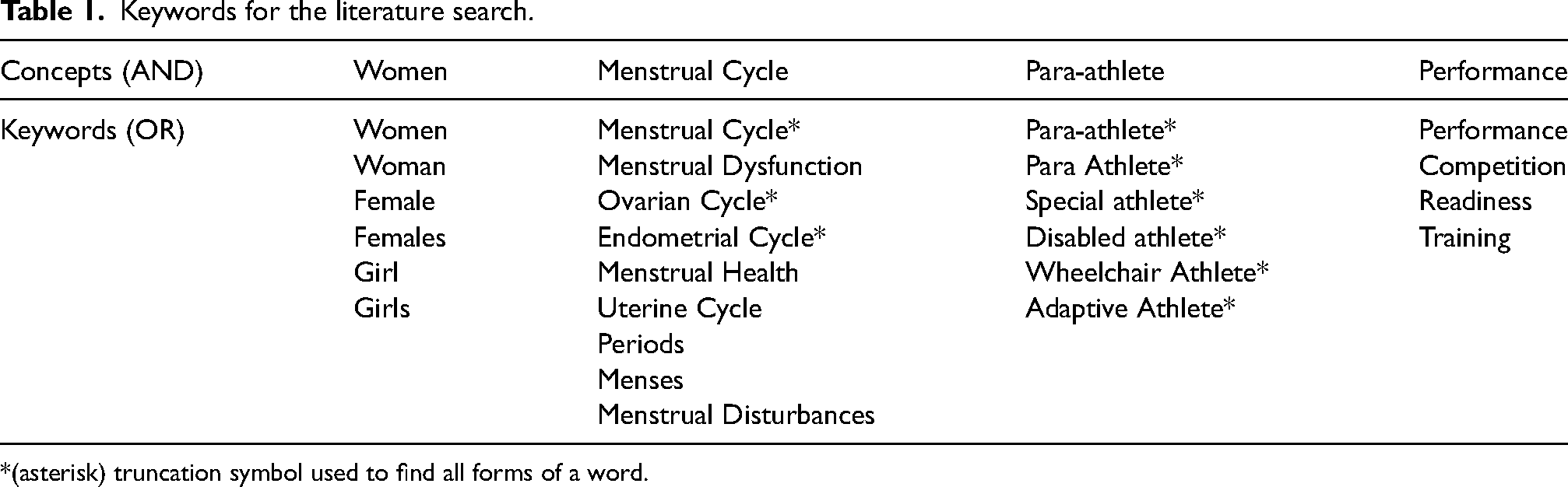
*(asterisk) truncation symbol used to find all forms of a word.
Articles were exported to a website (https://new.rayyan.ai/), using their “Duplicates detection” tool, the duplicates were identified and then removed (n = 118) manually by a reviewer (AI). The remaining 1951 articles were collaboratively screened for inclusion against the inclusion criteria by two researchers (CJ and AI). Inclusion criteria included: The article must be (1) peer-reviewed, (2) focused on the para-athlete population, (3) published in English, (4) published between 2000 and 2024, and (5) available online as full-text articles.
Titles that were not clearly related to the para-athlete population and menstrual cycle were excluded (n = 1918), and then the remaining abstracts unrelated to menstrual health in para-athletes were excluded (n = 28). Any conflict of inclusion was resolved through discussion among the researchers. The included articles (n = 5) were retrieved for full-text review, and three researchers evaluated the data (CJ, AI and TM).
The percentage of athletes reporting MC-related issues affecting performance was found by the summation of the number of athletes included for evaluation and the number of athletes who reported MC-related issues affecting performance. This number can be influenced by various factors, such as the symptoms evaluated by each study, the degree to which MC-related issues affect performance varies for each athlete and is associated with how the researcher frames the questions.
Results
Research on female para-athletes remains limited, but several authors5,6,14,20,24 have emphasized the need for studies to better understand and optimize their health and sports performance.
A survey of 260 elite para-athletes (Female = 110) found that 44% of premenopausal female athletes experienced oligomenorrhea, while 13.4% (n = 5) reported delayed menarche. 25 female athletes were eligible for a menstrual status assessment; of these, 24.0% had oligomenorrhea, and 20.0% had amenorrhea. Notably, awareness of both FAT and REDs was low, with only 8.1% to 9.2% of athletes recognizing these terms, regardless of sex, sport type, or disability classification. 5 A study on elite wheelchair basketball players (n = 13) found that 46.2% experienced menstrual cycle disorders. 23.1% reported excessive menstrual flow, and 69.2% experienced menstrual pain. 6 Similarly, an exploratory investigation (n = 18; F = 9, M = 9) revealed that 67% of female participants used birth control, with three reporting menstrual dysfunction. Additionally, one athlete noted menstrual changes concerning the training load. 14 An Australian study reported that 40 out of 52 para-athletes preparing for the Paralympics 2020 (77%) had their performance impacted by MC. Athletes added symptoms and challenges that were not asked of them. 24 This was a pattern also seen in a study of the physiological challenges of endurance hand cyclists with SCI. The two female participants in the study reported menstrual challenges, with one reporting digestive issues that started after the injury and the other reporting excessive tiredness. 20 Table 2 provides an overview of all the included articles.
Overview of the selected articles.
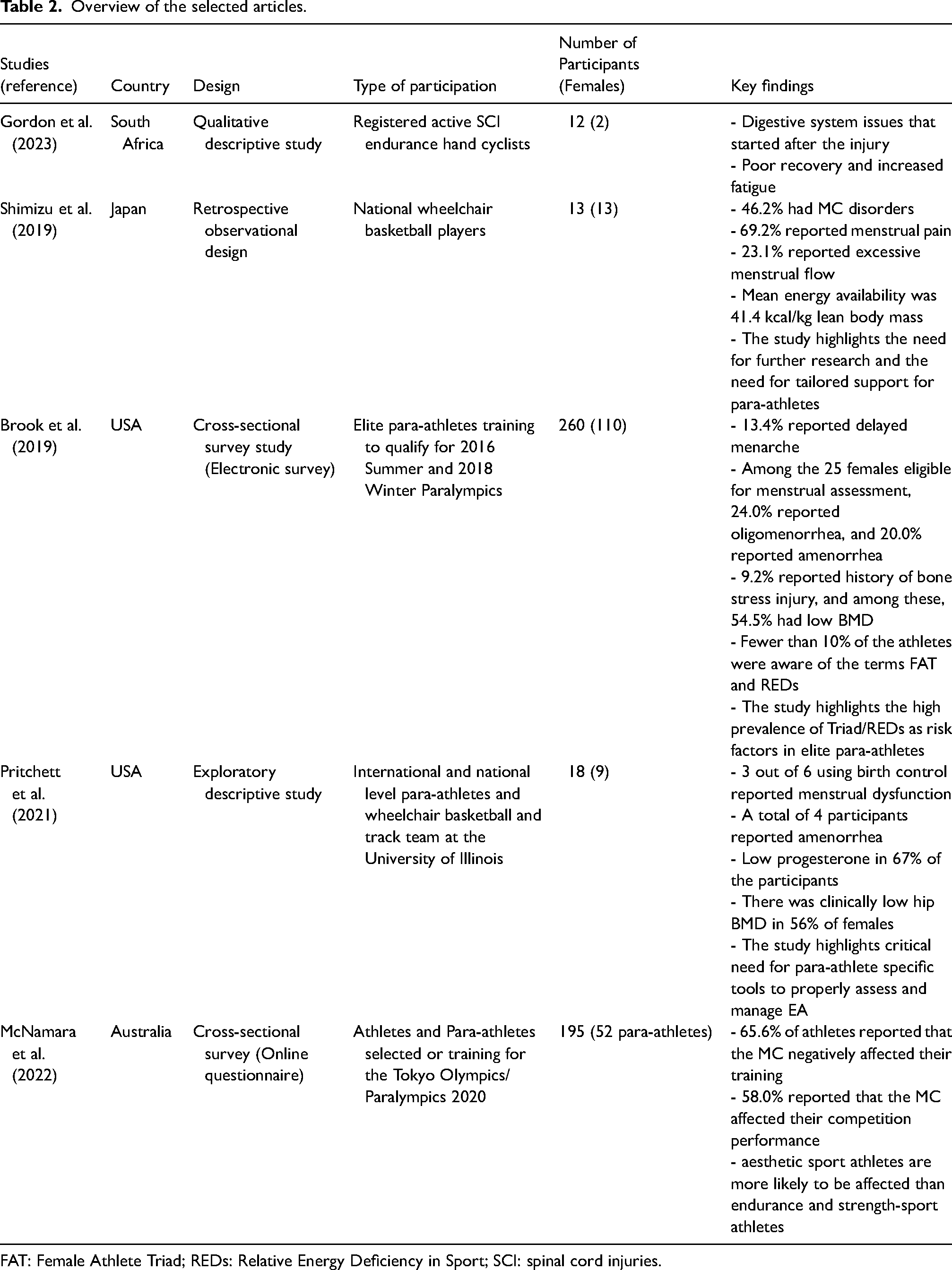
FAT: Female Athlete Triad; REDs: Relative Energy Deficiency in Sport; SCI: spinal cord injuries.
Among the female para-athletes in the reviewed articles, 63.4% reported MC-related issues that impacted their performance. These findings highlight the prevalence of menstrual health issues among female para-athletes and the need for greater awareness, education, and research in this area.
Discussion
In this review, we summarize the research on menstrual health and perceptions among female para-athletes and discuss the need for future investigations into their unique challenges. The main findings were as follows:
Para-athletes have reported experiencing MC-related issues that impact their sports performance. Various psychological, social, and physiological factors influence their overall health and athletic performance. Challenges such as limited accessibility, inadequate education, social stigma, and lack of awareness may further exacerbate difficulties among para-athletes.
The association between MCs and athletic performance has been widely studied in recent years. However, most of this research has been conducted on able-bodied populations. One review analysing 35 papers found that 15 reported at least one performance outcome being affected by menstrual symptoms. 7 In contrast, the current review identified only five studies5,6,14,20,24 focusing on the MC and its effects on performance in the female para-athlete population. This indicates that there is limited evidence on MC and its effects on performance in the para-athlete population, specifically regarding the effects of intense training and energy availability. 5 Additionally, it was found that available evidence5,6,14,20,24 included a few categories of disabilities and a small population, which further hinders the generalizability of findings in this population.
Previous studies on MC-related topics in para-athletes have documented challenges such as menstrual pain, irregular cycles, and excessive bleeding, and the findings of this review align with them.5,6,14,20,24 Lack of motivation to train, increased anxiety, and fear of leakage during menstruation have been reported by para-athletes, which is consistent with perceptions among able-bodied athletes. 25 However, this review also highlights underexplored elements, particularly the influence of training load, energy availability, and sport-specific demands on menstrual health in para-athletes. 5 Additionally, impairment-specific menstrual disorders have been reported in studies on non-athletic females with CP, SCI, and TBI.4,18,19 Energy expenditure may be reduced in individuals with SCI, and studies also raise concerns regarding LEA. While studies on para-athletes suggest similar concerns, additional factors unique to sports participation—such as training stress, nutritional demands, and frequent travel—might further influence menstrual health in this population. The risk of LEA and REDs is not well understood; hence, more research on the para-athlete population and specific assessment tools is required for effective risk evaluation.
Biological, psychological, and social factors may collectively contribute to the MC-related health challenges experienced by female para-athletes. Physiologically, many para-athletes face altered metabolic demands and autonomic nervous system dysfunction due to conditions such as SCI, CP, or limb loss. These impairments may disrupt hormonal regulation and thermoregulation, potentially exacerbating menstrual irregularities. Psychological factors, such as lack of motivation to train, high anxiety, fear of leakage and staining of clothes during menstruation, are reported by para-athletes. 26 Factors pertaining to social stigma and accessibility to menstrual health resources may further influence these difficulties, particularly in countries like India, where discussions around MC remain taboo. 27 Hygiene and privacy concerns also influence sports participation, as young females with disabilities often struggle with menstrual management due to a lack of accessible facilities. 28
The primary asset of this review is its focus on a largely unrecognized population in menstrual health research: female para-athletes. It provides a comprehensive overview of the menstrual health challenges faced by this group. However, several methodological limitations must be acknowledged. Firstly, the generalizability of findings is poor due to the small sample sizes and specific disability types examined in the included studies. Moreover, there can be a recall bias and subjective interpretation of menstrual symptoms, as the studies relied on self-reported data. Furthermore, long-term trends in menstrual health among para-athletes are not well understood because of the cross-sectional nature of most studies. The findings may have been influenced by these limitations, which underestimate or overestimate the true prevalence and impact of MC-related issues in para-athletes.
Research on para-athletes remains limited, with no studies focusing on the Indian population. Multiple categories of para-sports, larger populations, and longitudinal study designs must be adopted to enhance understanding and support for para-athletes’ well-being and performance. Standardized guidelines for menstrual health research in para-athletes are absent; this highlights the need for sport-specific ethical frameworks and training programs to ensure high-quality, inclusive, and responsible research. Customized educational and training programs should be developed using simple language and visual aids to enhance inclusivity and accessibility. These programs should address the unique physiological and psychological needs of para-athletes, promote open discussions, and reduce the stigma around menstrual health.
Although limited in both number and scope, the few existing studies included in this review suggest that a notable proportion of female para-athletes report experiencing MC-related issues that may affect their health and performance. However, the current body of research remains scarce, unevenly distributed across para-sports, and significantly underrepresents regions such as Asia, including India. These findings underscore a potentially important yet underexplored area. Addressing these gaps through targeted, impairment- and sport-specific research—as well as through practical and educational interventions—is essential to better support the health, performance, and sustained participation of female para-athletes in competitive sport.
Conclusion
There are limited available studies on MC in para-sports, with only five studies primarily focusing on female para-athletes’ menstrual health and sports performance. This underscores the current need for targeted research to understand their unique challenges, perspectives, and experiences. Though studies conducted on able-bodied athletes have advanced in verifying MC-related effects on sports performance, it remains unclear whether these findings apply to the para-athletes due to variations in impairment types and disability categories. These findings highlight the critical need for research specialized in para-sports to address their MC-related issues. This review also emphasizes the necessity of customized educational interventions that account for various disability factors to support and enhance both health and sports performance in female para-athletes.
Footnotes
Author contributions
CJ- Data curation, formal analysis, and drafting the original manuscript. AI- Methodology development, critical revision, and editing of the manuscript. TM and ØS- Conceptualization, substantial review, and editing of the manuscript.
Publisher's note
The views expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated institutions, the publisher, or the journal's editorial team.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
ORCID iDs
Chaitali Xrirama Joshi https://orcid.org/0009-0009-2195-9660
Ahmed Ibrahim ![]()
Øyvind Sandbakk https://orcid.org/0000-0002-9014-5152
Tanugatri Majumder ![]()
