Abstract
Background:
The role of intravenous (IV) tirofiban administered following endovascular therapy (EVT) for acute ischemic stroke (AIS) due to large vessel occlusion (LVO) remains uncertain.
Aims:
To investigate the associations of IV tirofiban following EVT with clinical outcomes in patients with acute LVO stroke and to determine whether the associations differ between anterior-circulation stroke (ACS) and posterior-circulation stroke (PCS).
Methods:
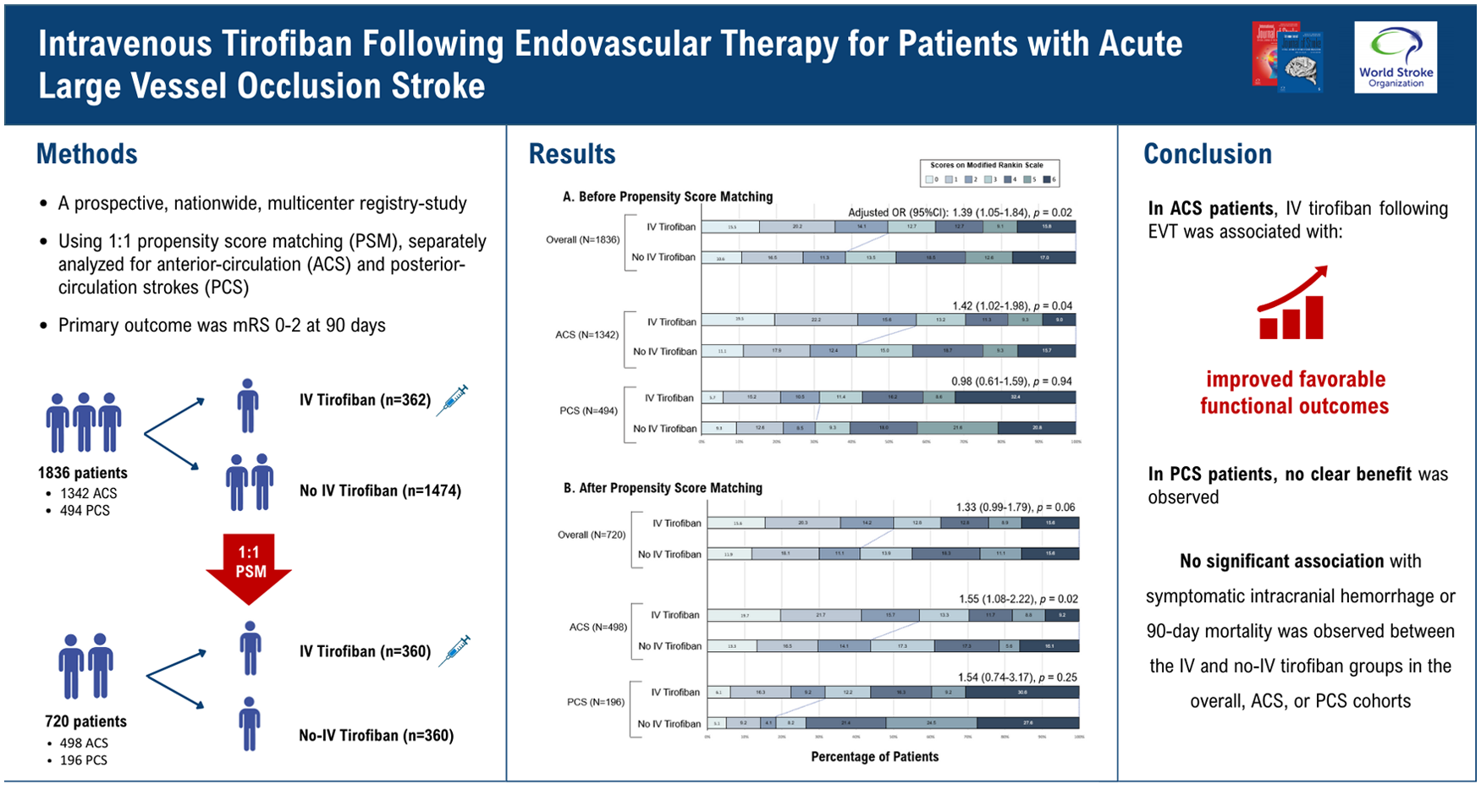
In this prospective, national, multicenter registry, patients with AIS due to intracranial LVO who underwent EVT within 24 h of onset were enrolled and categorized into IV tirofiban and no-IV tirofiban groups. The primary outcome was functional independence at 90 days, defined as a modified Rankin Scale of 0–2. Secondary outcomes included the distribution of 90-day mRS, independent ambulation, symptomatic intracranial hemorrhage (sICH), early neurological deterioration (END), and 90-day mortality. Analyses included univariate and multivariable logistic regression and propensity score matching (PSM, 1:1 ratio).
Results:
Among 1836 eligible patients (1342 ACS; 494 PCS), 362 (19.7%) received IV tirofiban following EVT. After PSM, 720, 498, and 196 patients were included in the entire, ACS, and PCS cohorts, respectively. In the ACS cohort, IV tirofiban was associated with higher odds of functional independence (57.0% vs. 43.8%; adjusted odds ratio (aOR) 1.55, 95% confidence interval (CI) = 1.08–2.22; P = 0.02) and a favorable shift in 90-day mRS. In the entire cohort, the association was attenuated after adjustment (aOR = 1.33, 95% CI = 0.99–1.79; P = 0.06). In the PCS cohorts, IV tirofiban was associated with numerically higher functional independence (31.6% vs. 18.4%), but without statistical significance (aOR = 1.54, 95% CI = 0.74–3.17; P = 0.25). No significant differences were found in sICH, END, or 90-day mortality between groups across all cohorts.
Conclusion:
IV tirofiban administration following EVT was associated with improved favorable functional outcomes in AIS patients with anterior-circulation LVO, without increasing the risk of sICH or END, but no significant association was observed in PCS patients. Further randomized controlled trials are warranted to verify these findings.
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
