Abstract
Background:
Social connection is fundamental to healthy ageing reducing the serious health impacts of loneliness and social isolation. General practice nurses (GPNs) have skills in assessing and responding to older people’s complex needs, applicable to nurse-led interventions strengthening older people’s social connections.
Aim:
To explore factors influencing the implementation of a GPN-led social prescribing intervention to improve social connectedness among older people.
Methods:
A qualitative descriptive study was conducted through semi-structured interviews (n = 13) and two focus groups with eight Australian GPNs exploring intervention implementation. The intervention comprised assessment, goal setting, co-production of personalised plans, referral, and follow-up. Data were inductively analysed using reflexive thematic analysis.
Results:
Themes revealed individual, organisational, and system-level factors that influenced implementation. Barriers included the attitudes and priorities of older people, the disruptive environmental context arising from natural disasters, and system factors including primary care funding and community infrastructure. Family support, positive general practice workplace cultures, and intervention adaptability were enabling factors.
Conclusions:
GPNs were able to integrate the intervention into their usual workflow and appropriately respond to lonely and socially isolated older people. However, GPN-led interventions are currently limited by funding models. Building nursing workforce capacity can support integrated health and social care for older people.
Introduction
The global population is ageing, and by 2050, people aged over 60 years will comprise 22% of the population (World Health Organization, 2024). This acceleration in population ageing will change the prevalence and patterns of loneliness (Newmyer et al., 2022). Demographic modelling projects that by 2050, there will be a threefold increase in the number of lonely older adults (Newmyer et al., 2022). Such projections challenge health and social care systems worldwide (Newmyer et al., 2022).
The United Nations declared 2021–2030 their Decade of Healthy Ageing, seeking global collaborative action to reduce health inequities and improve the lives of older people, their families and communities (United Nations Department of Economic and Social Affairs, 2020). Integral to achieving these improvements are primary care services responsive to older people (World Health Organization, 2024). A person’s social connectedness influences healthy ageing (Smith et al., 2023). Social connectedness is an umbrella term incorporating structural, functional, and quality factors (Holt-Lunstad, 2022). It may be conceived as a continuum, with strong and supportive social connections at one end and weak social connections at the other, resulting in loneliness and/or social isolation (Holt-Lunstad, 2022; Holt-Lunstad, 2024). Although people may experience both loneliness and social isolation, they do not necessarily co-occur as they are conceptually different. Loneliness is subjective, occurring when a person is dissatisfied with the extent and quality of their social relationships (National Academies of Sciences Engineering and Medicine, 2020). In contrast, social isolation is objective, referring to the presence of social relationships and the quantity of a person’s social contacts (Holt-Lunstad, 2022).
Loneliness and social isolation have been described as ‘the new geriatric giants’ because of their critical impact on physical and mental health (Freedman and Nicolle, 2020: 181). The World Health Organization (2025) has declared social connection a global health priority and has urged member states to integrate social connection strategies into national health and intersectoral policies. There is a strong association between loneliness, social isolation and increased morbidity, mortality, health service use and reduced well-being among older people (Freedman and Nicolle, 2020; Holt-Lunstad, 2022; Suragarn et al., 2021). Supporting older people to develop and maintain social connections reduces the health risks associated with loneliness and social isolation and contributes to healthy ageing (Holt-Lunstad, 2022; Holt-Lunstad, 2024).
There has been significant growth in interventions to reduce loneliness and social isolation in older people (Galvez-Hernandez et al., 2022; Thompson et al., 2023), such as social prescribing, which seeks to address people’s non-medical needs (Morse et al., 2022). Global developments in social prescribing are progressing rapidly, with policy development and practice changes observed in diverse contexts (Khan and Giurca, 2024). In social prescribing, health professionals often refer patients to link workers, who are usually community-based and connect the person to community supports (Morse et al., 2022). However, social prescribing programmes vary substantially in their target population and implementation. Nurses have been identified as optimally placed to contribute to such interventions, given their trusted relationships with older people and skills in preventative and chronic care (Thompson et al., 2023). In particular, primary care nurses are well placed to support social prescribing interventions because of their expertise in holistic and team-based care (Abelsen et al., 2023; Thompson et al., 2023).
The rising prevalence of chronic conditions and population ageing has prompted a shift towards a multidisciplinary team-based model of primary care. In Australia, primary care is largely delivered via general practices. General practice nurses (GPNs) are a growing workforce, with some 90% of Australian general practices now employing nurses (The Royal Australian College of General Practitioners, 2023). Despite high levels of consumer satisfaction with their role (Halcomb et al., 2015), GPNs remain underutilised and frequently do not work to the full extent of their practice scope (Halcomb and Ashley, 2019). This untapped potential provides scope for new models of nurse-led care to support older adults, including those at risk of loneliness and social isolation. Despite the potential, few programmes have been evaluated that engage GPNs in interventions to improve social connection. There is even less emphasis on exploring factors influencing the implementation of such interventions (Abelsen et al., 2023; Thompson et al., 2023).
As loneliness and social isolation are often stigmatising, lonely and socially isolated older people are often difficult to find (Newall and Menec, 2019; Thompson et al., 2023). General practice may be one of the few settings that this group frequents, and GPs and GPNs are often a trusted confidant (Freedman and Nicolle, 2020; Galvez-Hernandez et al., 2022). Thus, general practice provides a promising setting for nurse-led interventions to improve older people’s social connections (Thompson et al., 2024). To optimise such interventions, it is important to understand factors influencing implementation so that modifiable factors can be identified and addressed. Additionally, there is limited qualitative research about the experience of GPNs implementing interventions to support social connections. Therefore, the aim of this study was to explore factors influencing the implementation of a GPN-led social prescribing intervention to improve social connectedness among older people. In this study, participating GPNs are referred to as GPN health connectors to differentiate the role undertaken in the intervention from usual care. The study findings will inform improvements in design, implementation and evaluation of this GPN-led intervention. Findings will also guide the development of more integrated nurse-led interventions that support older people’s health and social needs as they age.
Methodology
Study design
This paper reports a qualitative descriptive study within a concurrent mixed methods project. While the quantitative phase assessed the intervention’s feasibility, acceptability, and preliminary impact, this phase sought to qualitatively explore factors influencing implementation. A qualitative descriptive design allowed a context-rich description of the perspectives of the GPN health connector participants that stayed close to the data (Sandelowski, 2000). Study reporting accords with the Consolidated Criteria for Reporting Qualitative Research (Tong et al., 2007) (Supplemental File 1).
Intervention and setting
Seven general practices responded to an expression of interest to participate. Older people at risk of loneliness and social isolation were identified by participating practices, community (aged and social care organisations) or self-referral. The target population was people living in the Hawkesbury region of New South Wales, Australia, who were aged ⩾75 years and Aboriginal and Torres Strait Islander peoples aged ⩾65 years. The younger age of First Nations peoples reflects their lower life expectancy (Australian Bureau of Statistics, 2023).
Baccalaureate-prepared, or equivalent, registered nurses (RNs) employed in participating practices were trained to work as GPN health connectors. Training included motivational interviewing, personalised planning and goal setting, and strengths-based conversations to improve social connection. It also incorporated use of social network mapping, visual communication aids, and an online community database of activities and services.
The intervention consisted of an individualised assessment, goal setting, and co-production of a personalised activity plan, referral, and follow-up. Initially, the GPN health connector conducted a conversational assessment with the older person to assess their social needs. A personalised plan to improve social connections was jointly developed, focusing on activities meeting the older persons’ preferences and interests. The GPN health connector provided referrals to community-based groups/activities and other providers as necessary. If required, the GPN health connector contacted service providers, arranged transport, and provided printed information. The GPN health connector followed up older people via telephone or during practice visits to encourage and review progress. Approximately 12 weeks after the initial assessment, the GPN health connector conducted a face-to-face follow-up to review goals and collect post-intervention data. Implementation was suspended for 6 months during the COVID-19 pandemic to comply with social distancing requirements.
Participants
Six general practices implemented the intervention with one GPN health connector, and the seventh practice shared the health connector role between two GPNs. All eight GPN health connectors were sent study invitations and agreed to participate, constituting a complete purposively recruited sample. As these GPN health connectors had experience delivering the intervention, they were the most appropriate to provide insights to address the study aim.
Data collection
Thirteen semi-structured interviews and two focus groups were conducted (Figure 1). Interviews allowed participants to discuss the older people they had assisted and their practice environment, whereas focus groups generated interactive conversations about experiences of intervention delivery and reflections on study participation. All sessions were audio-recorded and transcribed verbatim. Field notes captured the researchers’ observations and reflections.
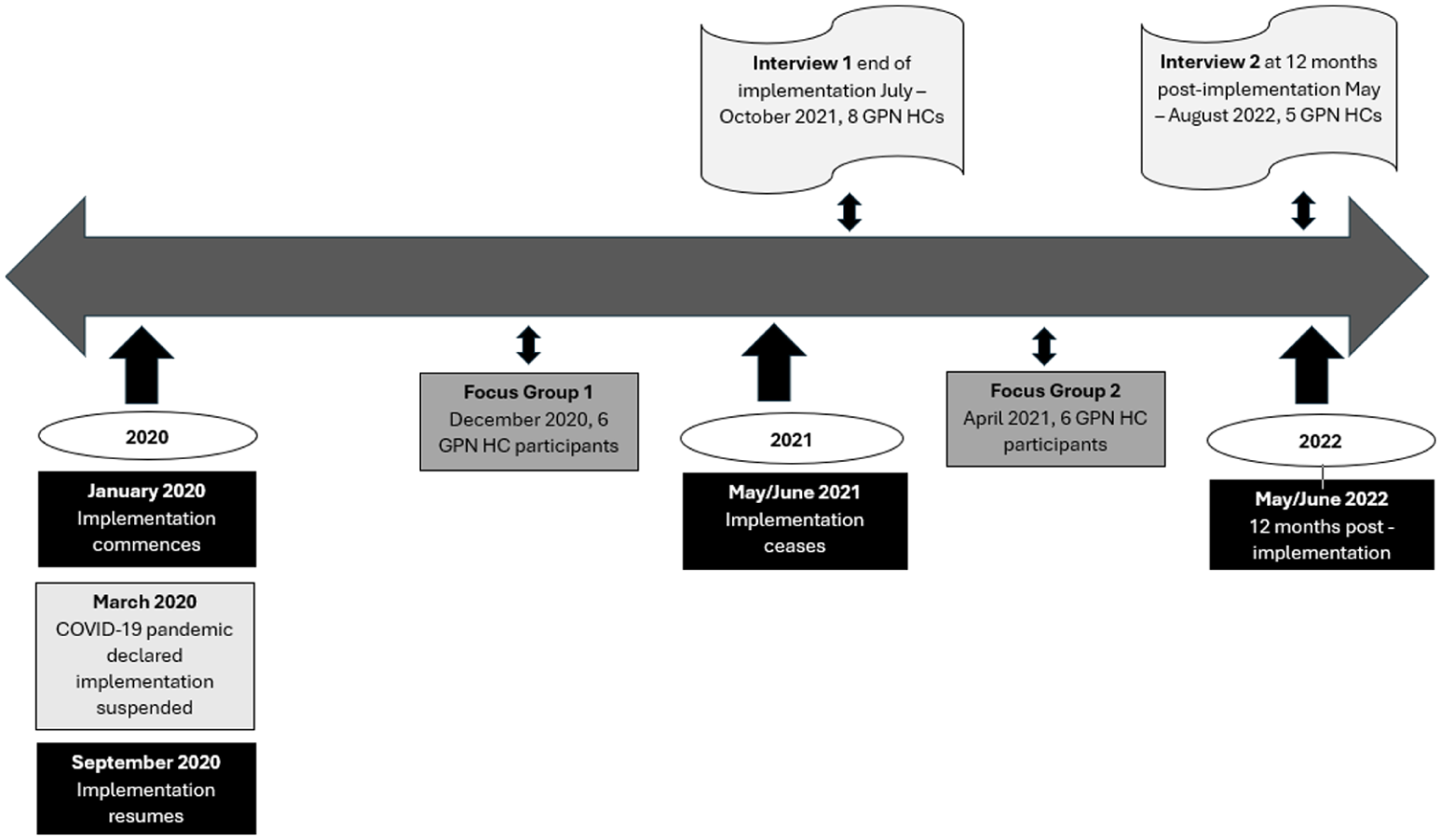
Data collection timeline.
Eight interviews were undertaken at implementation end (July–October 2021) and five were held approximately 12 months later (May–August 2022). The number of interviews undertaken was based on participant availability. Interviews were informed by an interview guide developed by researchers and primary care experts with knowledge of the intervention. Questions addressed the experience of the GPN health connector, motivation, knowledge and skills needed, barriers and facilitators, and lessons learned. Clarifying probes and prompts were used to elicit deeper data. Interviews were conducted by two experienced qualitative researchers who had not previously met participants. An initial pilot interview was conducted to test the interview guide. The average interview duration was 42 minutes.
Two focus groups were held during the intervention, with six GPN health connectors attending each focus group. Questions were framed to elicit the GPN health connectors’ implementation experience, what worked well, and what could be improved. The groups lasted 61 and 68 minutes, and were facilitated by an expert in community development and two researchers. After each interview and focus group was completed, two members of the research team recorded notes critically reflecting on the research process. Researcher reflexivity occurred within the broader team through open discussions about assumptions, possible biases and positionality, and how these views may affect the study findings.
Data analysis
Data were analysed using reflexive thematic analysis (Braun and Clarke, 2022). Data familiarisation occurred by the first author checking transcripts for accuracy against recordings. Transcripts were then imported into NVivo Version 12 Plus® (Lumivero, 2018) into a single dataset. Two researchers (CT and KP) independently generated initial codes for three transcripts. All researchers reviewed these initial codes, comparing and refining them. After all transcripts were coded and patterns of meaning were identified, themes were developed (Braun and Clarke, 2022). The researchers iteratively reviewed coded data and themes within whole transcripts until agreement was reached on the final thematic structure. In writing up, participant quotations were selected to illustrate the factors influencing implementation.
Rigour
Rigour was ensured through attention to confirmability, credibility, dependability and transferability (Lincoln and Guba, 1985). An audit trail was maintained throughout the research process to demonstrate confirmability. The researchers engaged in peer debriefing and used reflexive discussions to support credibility and trustworthiness. Semi-structured interview guides using open-ended questions, probes and prompts supported dependability. Thick description provides detailed information about the context and study participants to assist with judgements about transferability (Lincoln and Guba, 1985).
Ethical considerations
This study received approval from the University of Wollongong Health and Medical Human Research Ethics Committee (Approval No. 2019/248). All participants were provided with information about the study including the purpose, how study data would be stored and used, strategies to ensure participant anonymity and confidentiality, and processes for withdrawing. All participants provided informed consent prior to participation which was documented. Pseudonyms are used in reporting to protect participants’ identities.
Results
Participants
All eight GPN health connectors (participants) identified as female and had over 6 years RN experience. However, most (n = 5) participants had less than 5-years work experience in general practice (Table 1).
Participant characteristics.
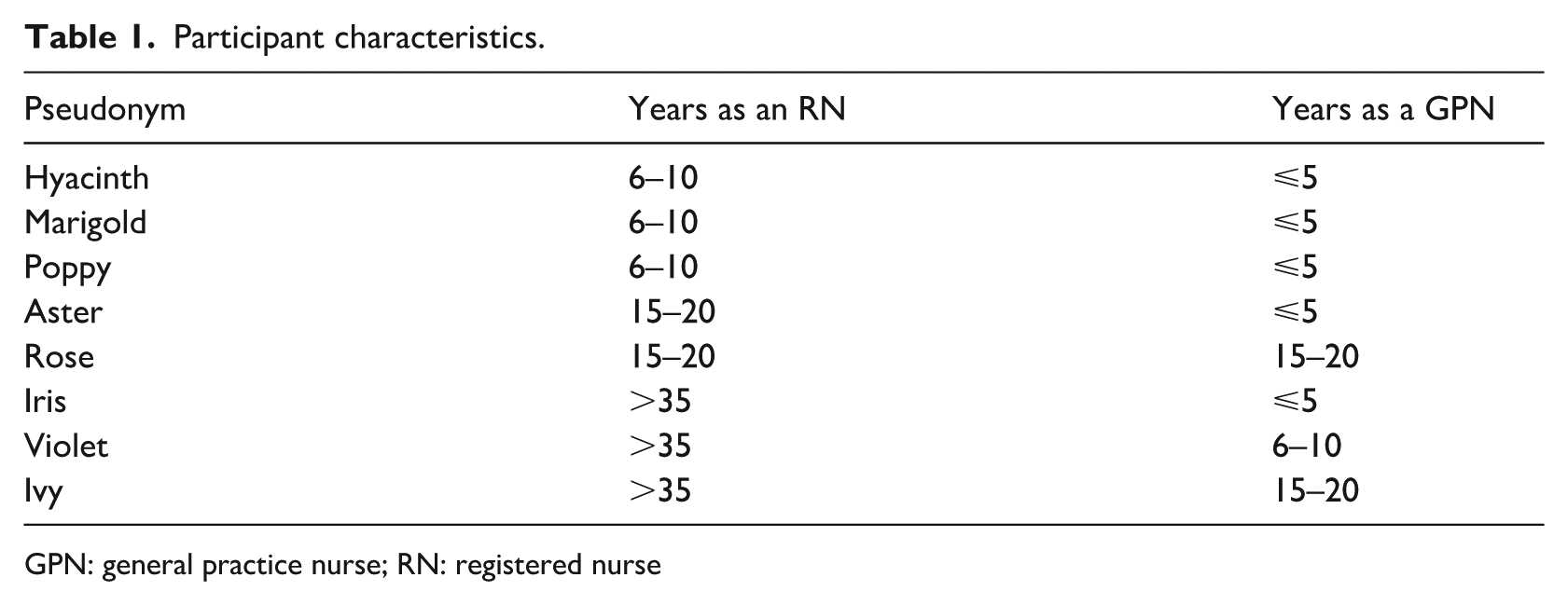
GPN: general practice nurse; RN: registered nurse
Themes
Figure 2 shows the themes identified by the participants as influencing implementation, namely: individual factors relating to older people, organisational factors linked to the general practice, and system factors.
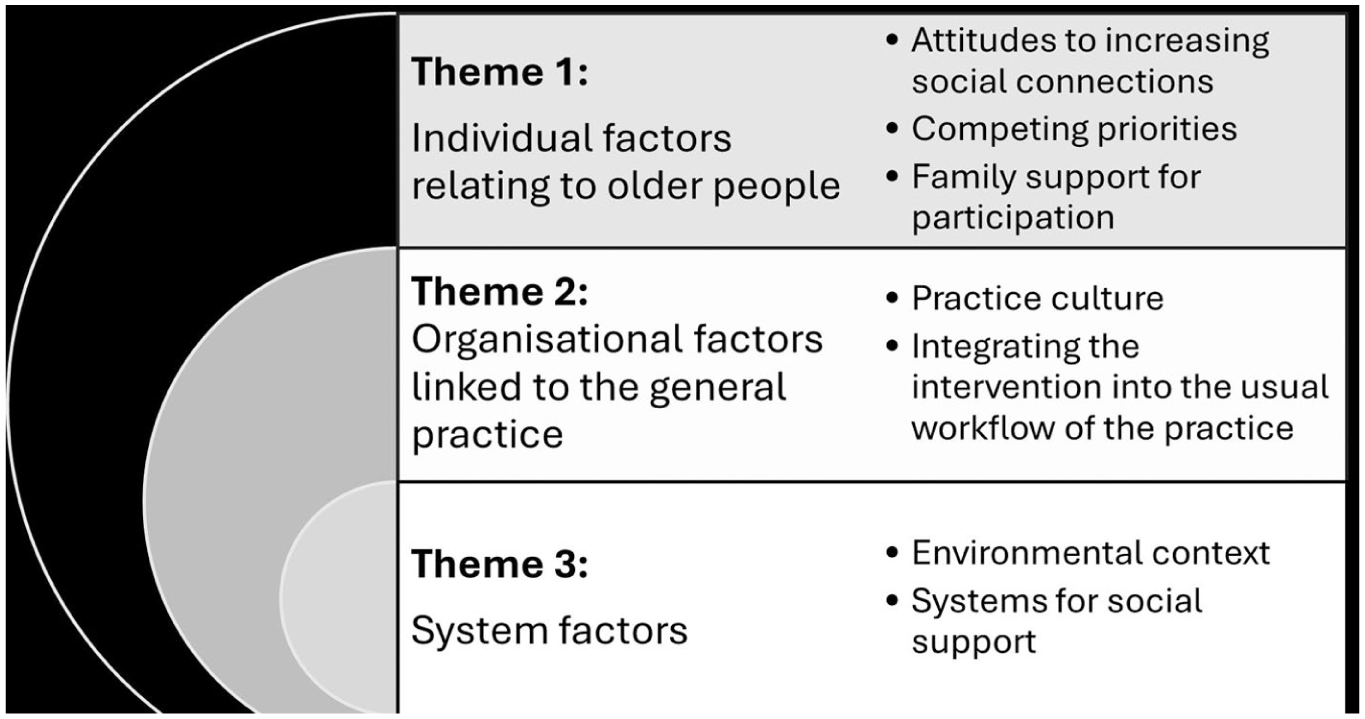
Factors influencing implementation.
Individual factors relating to older people
Participants described individual factors influencing older people’s participation in the intervention through three sub-themes: attitudes to increasing social connections, competing priorities, and family support for participation.
Attitudes to increasing social connections
Three predominant attitudes to increasing social connections were evident and included views about age, concerns about ageism, and the importance of respecting the older person’s autonomy. Participants perceived the intervention’s focus on the older old cohort as a limiting factor. They felt it was occurring too late, and people in the target group faced multiple barriers to engaging in new social connections. Participants expressed that the intervention was better suited to ‘focus on retirement age rather than 75 years’, (Aster) when disruption occurred to workplace social networks. By intervening earlier, participants felt they ‘could capture so many people and prevent loneliness occurring’. (Aster) . . .where people have retired at that age of 65 and they’re not sure what they’re going to do with themselves, and I think that would be a better age to be getting them into a programme like that, because they’re going from. . . being full-time workers to sitting at home, so . . . if you can start to encourage them and show them what’s out there and not let them get to a stage where they’re isolated . . . would be another beneficial thing. (Iris)
Some participants felt that older age negatively influenced participation. Violet stated, ‘A lot of them feel that they’re too old to be bothering with going out and meeting new people’. This view was reinforced by Ivy, who explained: ‘By the time they get to 75, a lot of them are way too set in their ways and starting to get more disabilities and inability to go out’. Older age was also associated with life changes such as the loss of a partner, which potentially made people less receptive.
. . .the lady that I spoke to recently, her husband. . .passed away about six months ago. And she said, ‘I don't want to go, I’m with [Community Transport] and I've had trips booked’. She said, ‘But I just feel that I don't want to go on those anymore. . .’ (Violet) And the other one was an old man who had his wife at the nursing home, and the only thing that he does every day is to visit her. She has dementia, and he just wants to spend all the time with her. (Marigold)
Participants recognised the autonomy of older people and the importance of respecting their wishes, accepting that many may be happy with limited social interaction. However, some participants questioned whether this acceptance stemmed from their preferences or from the older person’s having become ‘so comfortable being in their, what we call, loneliness’. (Rose)
Several participants recognised that discussing loneliness, social isolation and forming new social connections was a sensitive topic for some older people. Rose referred to ‘touching raw nerves’, whereas Violet raised privacy concerns and older people’s perceptions about others ‘intruding into their lives’. Additionally, Marigold described how older people had several reasons for not wanting to have these discussions: These older people are much more secretive about their health. . .That's the way it was before. And they think that a mental health issue is like the end of everything . . . That’s why they don’t seek any help for that. And they don’t want to give problems to their family as well. (Marigold)
Competing priorities
Participants described common reasons older people gave for not engaging with the intervention were existing health issues, caring responsibilities and being too busy. Hyacinth spoke of an older person who was keen to participate but declined because ‘she’s found out she’s got peripheral neuropathy, and she’s going through tests and stuff, so she wants to do all that’. Violet supported this view, describing how ‘. . .a lot of them were bogged down with medical appointments’. However, Rose perceived that ‘. . .some people did use their health as an excuse’.
Chronic conditions created challenges in participation related to symptom burden. As Iris stated, ‘mobility often was an issue for those with chronic illness’. Ivy also noted that ‘. . .if you’ve got people with oxygen. . .it’s just too hard for them’. Similarly, people on diuretics ‘don’t want to go too far from home. Or if they do, they want to know that wherever they’re going to, there’s a toilet close by so that they can get to it quickly. . ..’. (Violet)
Caring responsibilities were another barrier to participation identified by several participants. Iris observed that ‘dementia was a really isolating condition, whether it was those who were suffering from dementia or those who were caring for those with dementia’. Aster spoke of a woman whose husband had dementia and how her life revolved around ‘showering him or getting him dressed’, with these caring needs negatively impacting her ability to maintain social connections.
Finally, some participants described many older people who were already engaged in activities or home responsibilities. Poppy explained that older people she approached did not have space for the intervention as ‘. . .they love to stick with their daily routine’. Similarly, Hyacinth noted, ‘there’s a few that are quite connected with the community. . . I’ve had a few . . .they rang me up and said, “Look, it’s a really good idea, but I'm busy enough”’.
Family support for participation
Family support for older people’s participation in the intervention was described as crucial, encompassing both safety concerns and practical assistance. Participants felt that older people reflected their families’ and broader societal concerns about the safety of older people. However, family concerns became more pronounced with the COVID-19 pandemic and its heightened risk associated with older people interacting in the community. Violet ‘found it quite hard because a lot of patients were too frightened to come out of their homes’. Similarly, Ivy explained, ‘They didn’t even want to come down here and see me. They didn’t want to go anywhere. And their families were saying, “Don’t go out”’.
Following the lockdown period, when community activities gradually resumed, older people remained reticent and fearful, as their families disapproved of them moving about in the community.
. . .due to COVID, their own kids are not allowing them to go anywhere. So they are just sticking in the home. (Poppy)
Beyond the safety concerns, some older people who needed practical assistance to participate in social activities were reluctant to seek family support, as they did not want to bother them. Iris justified this explaining, ‘They [older people] found people were not very patient with their issues, including family members’. Hyacinth agreed stating: They feel like they’re burdening their family members if they have to go somewhere, because of mobility or they don’t have transport, they can’t drive.
Organisational factors linked to the general practice
The two key organisational factors participants described affecting implementation were practice culture and integrating the intervention into usual practice workflows.
Practice culture
For most participants, the general practice culture influenced intervention implementation. A supportive practice culture was typified by teamwork, positive professional interactions, and an authentic ethos of caring for older people. ‘. . .We have a very family-oriented business’ (Violet). Implementation was supported by General Practitioners (GPs) identifying appropriate patients. Rose explained, ‘the doctors instantly go, “Oh, I know, this person, and this person, so this one would be good and that one would be good.” . . . that helps as well and that's a positive’. Participants felt that a supportive practice culture assisted implementation by sharing ideas and challenges. Iris noted, ‘I am lucky to work with a great team and we work really well together. . .’
However, implementation was more challenging when broader practice support was lacking. Hyacinth described how ‘ I don’t have anyone to rely on. So, if I don’t have time to do it, it doesn’t get done. . . if it were done as a team, it would be a lot easier. . .’
The decision to participate in the study was often made by the practice leadership (GP principal and practice manager). Poppy explained, ‘. . .I got this position [GPN health connector] from my GP, but I found it’s my personal interest as well’. In practices with team-based cultures, participation was a shared decision. Several practices had previous positive experience with Primary Health Network-funded projects and were willing to participate again.
. . .we’ve been involved in a number of projects. . . .We can see the benefits, it’s not just from a patient perspective, but also from the medical side of things, of being able to add to our own knowledge and our data systems with some of the other projects.... (Rose)
Integrating the intervention into the usual practice workflows
Participants’ willingness to adjust their workload to support the intervention evidenced their perception of its value.
Once I realised what the project was about, and how it could make a difference for patients. . . we had a [practice] meeting that day . . . and I said, ‘Look, this is what's involved. I think if we rearrange some of our workload or do the health connector on a particular day, I think it can be achievable’. (Aster)
Participants raised the need for flexibility in implementing the intervention, depending on the practice size and the GPN workforce. Ivy felt that larger practices may be able to allocate ‘one specific nurse’ to the intervention. Others described the advantages of a whole-of-practice approach, where the intervention was integrated into all team members’ workflow.
So, it would be good to involve the whole team. I think it would be a much better approach to be actual, like part of the practice, everyone in the practice. (Hyacinth)
Participants relied on the protected time allocated for the intervention. Some felt that this was important to reduce the risk that acute care demands would overtake implementation. However, this occurred regardless. As Poppy explained ‘some emergencies come in; you have to do emergency calls and electrocardiogram (ECG) things and other stuff. It’s been busy, especially now in COVID’.
Several participants raised the option of identifying lonely and socially isolated older people through opportunistic interactions, such as during wound dressings or chronic disease consultations.
. . .I don’t know if you need a dedicated time like that, or if you just opportunistically take it up. It just depends on the workload at the time, how busy things are. Whether you can just do it straight away and be done with it or not. (Ivy)
The 75+ health assessment is a free annual Australian government-funded check-up. These assessments were unanimously described as an important opportunity, as the extended consultation provided funded time to identify older people’s health and social care concerns.
. . .[75+ health assessments] are a good way that we were already doing it [referring to assessing older people’s social engagement]. So that [the intervention] entered into it easily because that was not really an addition. It fitted okay because I was able to set aside the time that we needed to do it and everybody else was on board. (Rose)
System factors
The implementation ecosystem generated barriers and facilitators across the sub-themes of environmental context and social support systems.
Environmental context
Five disaster events, comprising bushfires, floods and COVID-19, occurred during the implementation period. This caused major disruptions, including one practice being partially flooded, another evacuated, and a third cut off by floodwaters. One practice had to treat patients who could not access their usual practice. These events were major stressors for participants as usual practice operations were significantly disrupted on multiple occasions.
We’ve had significant challenges. . . not just. . . COVID but we’ve had two floods in the last 12 months so and the practice has on both occasions been evacuated. (Rose) .. . .in the last two years we’ve had bushfires, and I think we're up to number four flood, which puts a lot of stress on us. Because we were virtually one of the only practices on our side of the river. . . people that can’t get to specialists that can’t get to their own general practice and emergency patients. So it’s about a three-hour trip to the closest Medical Centre when we’re cut off. . .. (Iris)
Participants described the differing implementation contexts before and after COVID-19. When implementation began, there was a sense of optimism, and participants found that older people were interested and enthusiastic. Confidence was high, and recruitment difficulties were not anticipated. When the intervention resumed after the 6-month pause, the implementation experience was overwhelmingly negative, and participants described struggling to regain momentum. Ivy’s comments echoed the collective views: ‘COVID hit and that just threw a huge spanner in the works’. Rose described the change saying: I think that the climate with COVID just changed things so much that 100% when we signed up for this in February, we were all guns a blazing and just. . . yeah. I must say I just have a different feel about it now than before. . .
The irony of delivering a social connectedness intervention during social distancing was not lost on participants. They reported feeling conflicted, wanting to support social connections but also needing to manage COVID-19 risk.
I think the program could have been much more of a success than what it was. And I was also hesitant to send people when I knew that there was a risk involved in additional COVID issues. . . I felt it was morally wrong to send people off into the community when there was COVID. (Aster)
The additional work hours required to provide COVID-19 vaccinations led to exhaustion and little capacity for the intervention. Chronic condition management and health assessments were also curtailed, negatively affecting recruitment and challenging intervention delivery.
And that is, we are vaccinating. Well, I used to only work part-time, and I’ve done 40 hours a week for the last, however many weeks or months now. So unfortunately, it’s really taken a step back [participant referring to the intervention]. . . just because the priorities have changed. (Rose)
The compounding impact of the multiple disaster events significantly affected the mental health of the community and participants, and community infrastructure was damaged.
Because of the flooding. . . and the COVID, anxiety is at an all-time high and affecting everyone’s mental health. I’ve seen a lot of patients who were flooded a couple of times and they’re quite devastated. (Marigold)
Systems for social support
Funding of general practices was identified as a key implementation barrier. Participants reported that, as few billable items existed to support the GPN health connectors, intervention delivery was not funded sustainably. Remuneration provided to participating practices was an essential facilitator of engagement. However, this was limited to the implementation period.
. . .general practice is a business just as much as it’s a healthcare facility. So having the MBS [Medicare Benefits Schedule] item numbers there, it gives you that captured time to be able to look at these things. . . (Rose)
The ability of the participants to assist older people depended not only on their local service knowledge and the service capacity but also on community infrastructure. Participants recognised that they relied on the often poorly resourced community sector to provide services and activities. The study’s online database of community services was perceived as a vital resource, providing current, accessible community information.
Like honestly, the directory if we didn’t have that, I think we would be actually lost. Because I didn’t know what was in the area, available for people. (Aster)
Limited public transport, the inability to drive and high transport costs were frequently cited as barriers to older people participating in activities. Although a community transport organisation existed, access to this service required additional government service approval. The semi-rural nature of some participating practices also limited transport access.
Transport's a big thing. . . They have to have certain things to be able to access that, otherwise they have to have funds to be able to access taxis or things like that. Transport, if they don't drive or don’t have a car, is a big barrier. (Ivy) Most important thing is that distance, travelling thing. . . people if they aren’t able to drive or walk, that's a big challenging thing for them. . . (Poppy)
Discussion
This study has explored individual factors relating to older people, organisational factors linked to the practice and system factors that influenced the implementation of the social prescribing intervention. All of these factors have implications for nurses and the GPN role. This study has identified modifiable factors that, if addressed, can lead to improvements in the design and implementation of nurse-led interventions for older people. For example, as age is a strong predictor of loneliness (Newmyer et al., 2022), this can be a key indicator to prompt nurses to undertake assessment. Although age is not a modifiable factor, decisions about the target population for interventions can be amended. Participants in this study believed that greater flexibility was needed with the study inclusion criteria. The importance of delivering preventive interventions earlier to reduce loneliness and social isolation has been identified in previous research (Pettigrew et al., 2014; Suragarn et al., 2021). Retirement has been shown to result in reduced contact with people and is a time to help older people shift from work to more localised networks (Newmyer et al., 2022). As Barke (2017: 121) notes, ‘numerically, socially, and culturally there is as much difference between 55 and 85 as there is between 25 and 55’. Disruption to older people’s social connections occurs through age-related changes, particularly from diminished energy (Morgan et al., 2021), decreased mobility (Corry et al., 2021), competing demands from chronic conditions, and reluctance to engage in activities (Thompson et al., 2024). Nurses need to consider that older people may be more receptive to increasing social connections while mobile and healthier.
In terms of individual factors, social prescribing interventions that fail to recognise the heterogeneity of older people are unlikely to be successful (National Academies of Sciences Engineering and Medicine, 2020). In their review, Suragarn et al. (2021) found that many interventions were designed for healthy, community-dwelling older adults, with few for older adults living with chronic conditions. Our study identified competing priorities older people face as a factor influencing their participation in the intervention, particularly the demands of managing chronic conditions. The heterogeneity of older people, variety of factors contributing to loneliness and social isolation, and wide-ranging challenges arising for healthy ageing demand interventions tailored to individual contexts (Klusmann et al., 2021). This personalised approach requires flexibility in how social connectedness interventions are implemented. For nurse-led social prescribing interventions, this includes the ability for nurses to adapt how lonely or socially isolated older people are identified, assessed, and assisted. As this study found, GPs and GPNs may opportunistically identify at-risk older people during routine visits. This finding also highlights the importance of GPNs opportunistically identifying at-risk people during usual care.
At an organisational level, for practice-based interventions to be feasible, they must be readily integrated into usual workflows. Previous studies of GPN interventions have identified this as a key component of successful interventions (Raat et al., 2025). In this study, a supportive practice culture, typified by a team-based approach, facilitated workflow integration. Similarly, Corry et al. (2021) found that GP involvement in the intervention improved adoption, as older patients trusted their GP. Practices need the flexibility to adapt interventions to their local context. Indeed, adaptability is a cornerstone of the most effective social connectedness interventions (National Academies of Sciences Engineering and Medicine, 2020).
In this study, system factors were the most complex to modify, particularly primary care funding models, transport systems, and other aspects of community infrastructure integral to meeting social needs. Funding GPN interventions has long been reported as a key barrier to the GPN role (McInnes et al., 2017; Stephen et al., 2024). Despite the policy focus on developing team-based care, funding models still fail to adequately support multidisciplinary preventative care (Australian Government Department of Health and Aged Care, 2021). Current funding models restrict nursing practice by providing limited remuneration for GPNs’ work. This means that nurses are often not working to the full scope of their practice or providing the types of preventive care that they could (Halcomb and Ashley, 2019). Secondly, unreliable and costly public transport have been described as barriers to social connection (Morgan et al., 2021; Smith et al., 2023). Improving these systems requires intersectoral collaboration to effect policy change, and engagement between health, social, and transport services to optimise service delivery. Historically, in Australia, there has been a disconnect between GPNs and policymakers (Halcomb et al., 2006). GPNs may influence system change by advocating for care that better meets older people’s needs through nurse-led interventions integrating health and social care. This input is likely to be more effective through collective efforts, such as those of professional nursing associations. Finally, like this study, Morgan et al. (2021) found that community resource availability is essential to supporting social connections. Similarly, Turcotte et al. (2015) found that social and environmental barriers restricted community participation, and collaborative action by healthcare and social systems was needed to address these barriers and improve older people’s engagement. Community development approaches that enhance access to community resources have been effective (Gardiner et al., 2018). Since multiple health, aged, and social care organisations contribute to older people’s well-being, collaborative action to provide integrated and coordinated ‘touch points’ could provide a mechanism to improve their social connections (Smith et al., 2023).
Strengths and limitations
There were several limitations to this study. It was conducted in a single region affected by multiple natural disasters, which may limit generalisability. Inevitably, different countries and jurisdictions will vary in their primary care systems, which has implications for nursing roles and funding models. The pause in implementation due to COVID-19 may also impact transferability. Additionally, the participants’ relative inexperience in general practice may have introduced a degree of response bias. However, key study strengths included the inclusion of all GPN health connectors and data collection at multiple timepoints to ensure that issues were captured over time.
Implications for practice and further research
GPN-led interventions build workforce capacity and support integrated health and social care. However, further research is needed to establish their effectiveness in improving older people’s social connections. There is stigma associated with loneliness and social isolation (Thompson et al., 2023), and identifying at-risk older adults is challenging (Newall and Menec, 2019). Interventions framed to address well-being, where older people do not have to identify as lonely or socially isolated, are likely to be more appealing (Pettigrew et al., 2014). Equipping GPNs and GPs to address loneliness and social isolation may promote collaborative assessment and support for social connections within usual care (Suragarn et al., 2021). Further studies of opportunistic rather than planned approaches to identify and address older people’s social connectedness are needed to assess acceptability and effectiveness.
Although system factors were less amenable to change, future interventions should address these barriers. Considering how funding models and policy shifts can be leveraged to support the integration of interventions within usual workflows is vital. Additionally, engaging intersectoral stakeholders through collective action can enhance community capacity and promote access to community resources.
Conclusion
Individual, organisational and system factors influenced the implementation of this nurse-led social prescribing intervention. At an individual level, considering the target population and accommodating the competing demands upon older people with chronic conditions can promote engagement. GPNs integrated the intervention into their usual practice workflow and appropriately responded to lonely and socially isolated older people. Promoting a multidisciplinary team-based approach may strengthen intervention delivery. However, system-level barriers, such as funding and transport, presented a more complex challenge and require collaborative action from diverse stakeholder groups. Building nursing workforce capacity can support integrated health and social care for older people.
Key points for policy, practice and/or research
Globally, social prescribing models tend to emphasise the use of community link workers, with the role of GPNs less explored.
There is limited qualitative research about nurse-led interventions to support social connections of lonely and socially isolated older people.
This study provides insights about intervention implementation in the practice environment to improve the design and delivery of nurse-led social prescribing interventions.
GPNs perceived that the trusted relationships they developed with older people facilitated delivery of interventions to this population.
Nursing practice will be enhanced by research exploring interventions and models of care that more effectively integrate the health and social care needs of older people.
Supplemental Material
sj-docx-1-jrn-10.1177_17449871251410561 – Supplemental material for Factors influencing the implementation of a general practice nurse-led intervention to improve social connectedness among older people in Australia: a qualitative descriptive study
Supplemental material, sj-docx-1-jrn-10.1177_17449871251410561 for Factors influencing the implementation of a general practice nurse-led intervention to improve social connectedness among older people in Australia: a qualitative descriptive study by Cristina Thompson, Elizabeth Halcomb, Amy Montgomery and Kath Peters in Journal of Research in Nursing
Footnotes
Acknowledgements
We wish to thank the GPN health connectors who consented to participate in this study. We also express our appreciation to the project team from the Nepean Blue Mountains Primary Health Network: Kate Tye, Janice Peterson, Monique Pryce and Liz Murphy, for their leadership of the pilot and support for the study. We are grateful for the assistance provided by Mr. Darcy Morris in data collection.
Author contributions
Data availability
The data are not publicly available due to privacy and ethical restrictions.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by the Australian Government Department of Health, Disability and Ageing through the Evaluation of the Improving Social Connectedness of Older Australians Project Pilot (Health/18-19/04684). Author Cristina Thompson is supported by an Australian Government Research Training Program Scholarship (doi.org/10.82133/C42F-K220).
Ethical approval
Ethical approval for the study was obtained from the University of Wollongong Health and Medical Human Research Ethics Committee (Approval No. 2019/248). The approval period is from 25 June 2019 to 30 June 2026. All participants provided informed consent which was documented.
Consent to participate
All participants were provided written information about the study and a consent form. They could choose to provide written consent by signing or returning this form prior to participation. An option of verbal consent was provided for participants using a verbal consent script that received ethical approval. When verbal consent was preferred, the interviewer followed the verbal consent script and participant responses were audio-recorded, transcribed and securely stored.
Consent for publication
Informed consent for publication was provided by the participants at the time of consent to participate in the study. Pseudonyms have been used to protect individual’s identity.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
