Abstract
Background:
Climate change remains a significant challenge to global health. The health care system is a major contributor of greenhouse gas (GHG) emissions. While pharmacists are aware of climate change as an important societal issue, there is little known about the level of implementation of climate-conscious practices in community pharmacies throughout Ontario.
Methods:
An interview-based system was developed to gather insights from pharmacists regarding their perspectives on climate change and identify strategies to involve them in sustainable practices. Convenience and snowball sampling techniques were used to recruit pharmacists. Interviews were conducted by phone or Zoom, and transcripts were developed and analyzed for common themes using a qualitative method.
Results and discussion:
Twenty-four community pharmacists were interviewed. Three overarching themes emerged: 1) there is a knowledge and awareness gap in the pharmacy profession; 2) before pharmacists can prioritize sustainable practices, they must first address more immediate concerns in the pharmacy; 3) sustainable practice integration requires employment and regulatory changes as relying solely or extensively on the good intentions of frontline pharmacists is insufficient.
Conclusion:
While pharmacists show concern about the environmental impacts of their work, sustainable practice integration is very limited in community pharmacies across Ontario. There are many challenges and barriers to address. This includes closing the knowledge and awareness gap by incorporating climate-related topics into pharmacy curricula and providing educational seminars and resources for practicing pharmacists. In addition, improving workflow, changing standard operating procedures at a corporate level and providing incentives for implementing eco-friendly practices are crucial steps to address time and financial limitations. To manage patient safety concerns, providing resources that consider climate considerations as a secondary objective, when clinically appropriate for the patient, is the right approach to engage pharmacists. Lastly, advocating for employment and regulatory changes will be necessary for large-scale, durable changes to pharmacy practice.
Knowledge into Practice
Human-triggered climate change is a pressing global concern of epochal importance.
The contribution of health care work to greenhouse gas emissions is significant and often overlooked and underestimated.
Community pharmacy practice has significant opportunities and responsibilities to reduce climate impacts and mitigate human-caused climate change.
Pharmacists are interested in an open-to-climate-conscious pharmacy practice but perceive they are powerless to make meaningful impacts on greenhouse gas emissions through their individual practice.
Pharmacists perceive a profession-wide effort, enabled by regulatory bodies and corporations, will be needed to drive climate-conscious pharmacy practice forward.
Background
The climate crisis remains an urgent global health issue, with dire implications according to the World Health Organization (WHO). 1 Air pollution kills an estimated 7 million people per year, while carbon emissions are responsible for over a quarter of deaths from heart attacks, stroke, lung cancer and chronic lung diseases. 2 Extreme weather conditions as a consequence of climate change can increase the risk of death, as well as the spread of communicable disease, and trigger health emergencies.1-3
The carbon footprint of the health care system itself contributes significantly to the problem of pollution, greenhouse gas emission and waste disposal, both directly through facility operations and vehicle usage and indirectly through the procurement, storage, distribution and disposal of various goods.3,4 The Canadian health care system contributes close to 5% of Canada’s national carbon emissions, with pharmaceuticals making up 25% of greenhouse gas emissions.3,4
Interest in “climate-conscious pharmacy practice” has been growing, and there have been calls for pharmacists to become more directly engaged in activities to improve planetary health. 5 For example, the use of dry powder inhalers (DPIs) or soft-mist inhalers instead of multidose inhalers (when clinically indicated) reduces waste and risks of climate harm. 4 Appropriate disposal of medications to prevent pollution of groundwater represents another important opportunity for pharmacists to support carbon footprint reduction goals. 6
Despite general awareness of and interest in climate change issues, recent literature suggests there is a lack of knowledge, awareness and empowerment among health care professionals regarding their potential role in reducing planetary harms associated with health care work itself.7-10 A recent study of pharmacy students in Australia indicated that only 10% of respondents were aware of climate-conscious pharmacy practice techniques. 7 This finding was consistent with studies in medicine and dentistry.8,9 Another survey of pharmacists revealed that while the majority believed climate change was real and actually happening, less than 50% of respondents felt the topic was relevant to their work as pharmacists. 10
Mise En Pratique Des Connaissances
Le changement climatique provoqué par l’homme est une préoccupation mondiale urgente d’une importance capitale.
La contribution du secteur de la santé aux émissions de gaz à effet de serre est importante, mais souvent négligée et sous-estimée.
La pratique de la pharmacie communautaire offre des occasions et confère des responsabilités importantes visant à réduire les répercussions sur le climat et d’atténuer le changement climatique d’origine humaine.
Si les pharmaciens montrent de l’intérêt à une pratique de la pharmacie soucieuse du climat, ils se sentent toutefois démunis face aux importantes répercussions engendrées par leur pratique individuelle sur les gaz à effet de serre.
Les pharmaciens estiment qu’un effort de l’ensemble de la profession, soutenu par les organismes de réglementation et les entreprises, sera nécessaire pour faire progresser la pratique pharmaceutique soucieuse du climat.
The central objective of any health care system is to keep citizens and populations healthy—yet, paradoxically, the work of health care itself is contributing meaningfully and negatively to health care damage due to lack of awareness of climate-conscious health care practice techniques. Understanding the perspectives of frontline health care providers (like community pharmacists) to better identify opportunities and priorities related to climate-conscious practice is an essential component of supporting global carbon reduction goals as a tool for optimizing population health.
Research objective
The objective of this exploratory study was to characterize awareness of climate-conscious professional practice in community pharmacies across Ontario and to identify potential barriers and facilitators to adoption of environmentally sustainable practices within community pharmacy.
Methods
There have been little published data exploring community pharmacists’ understanding and awareness of climate-conscious practice; as a result, a qualitative, exploratory study was undertaken to begin to characterize this issue.
Inclusion criteria for this study included English-speaking part A (Ontario)-licensed pharmacist working a minimum of 20 hours/week in a community pharmacy setting. For logistical reasons, a combination of convenience and snowball sampling techniques was used to recruit participants; as a result, the participant pool could not be considered representative of community pharmacists across Ontario or Canada. The research team undertook efforts, however, to recruit participants from diverse geographic regions of Ontario (including urban, suburban and rural communities), from diverse practice settings (including independent, chain and grocery store/big box retailers) and diverse demographic backgrounds with respect to age and ethnocultural background.
One-on-one interviews were scheduled with research participants by phone, Microsoft Teams or Zoom (based on the participant’s expressed preferences). The interviewer used a semistructured interview protocol (Table 1) to explore facets of climate-conscious pharmacy practice. This protocol was based on current expert/consensus guidance in Canada focused on climate-conscious pharmacy practice, curated by Climate Action + Healthcare: Creating a Sustainable Canadian Health System in a Climate Crisis (CASCADES), a national, government- and university-funded organization. 11
Semistructured interview protocol
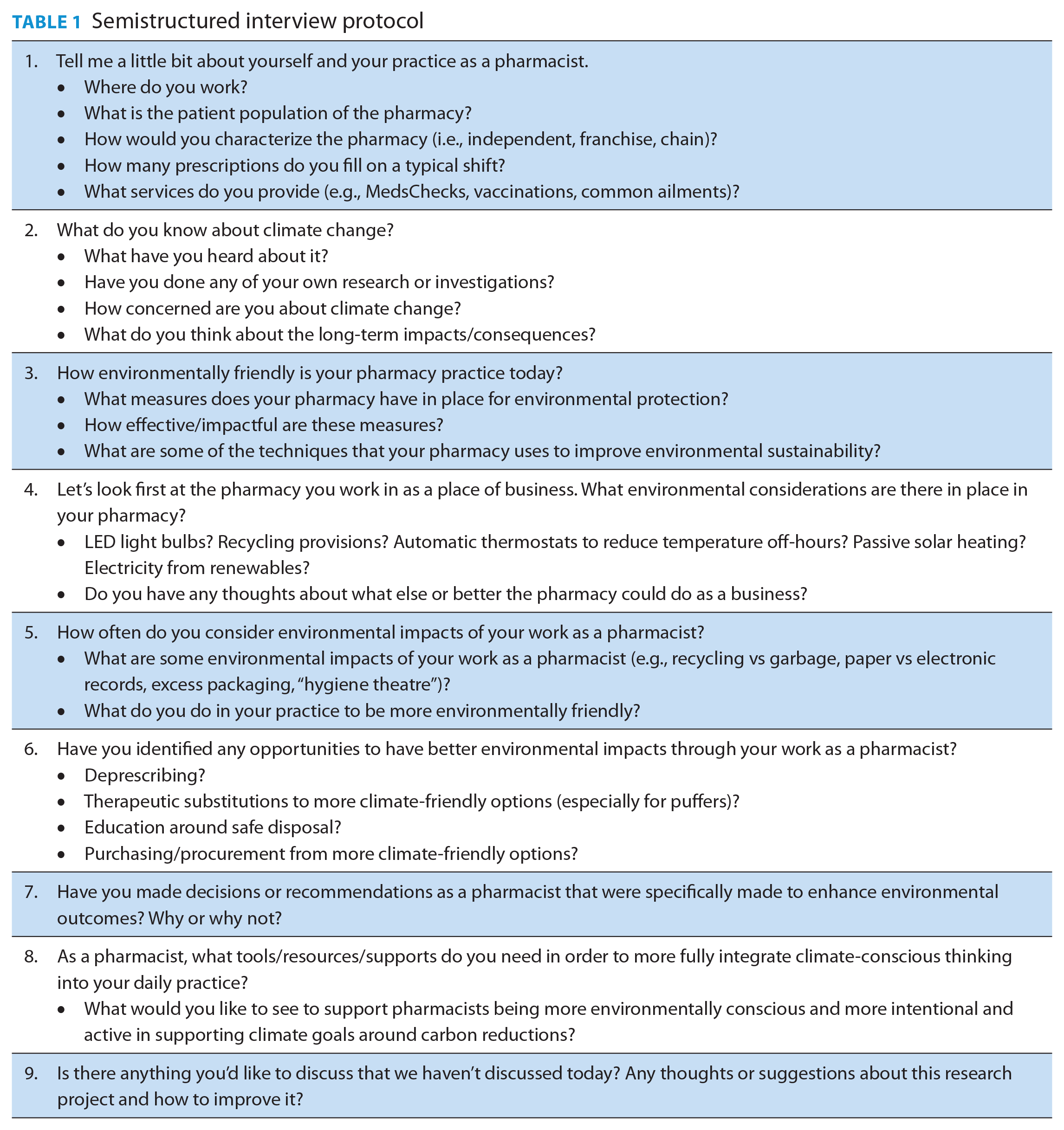
All interviews were recorded and verbatim transcripts generated with permission of the participant, pursuant to an approved research ethics protocol. Transcripts were initially generated using applications embedded in the Teams and Zoom platforms, then were “cleaned” manually by the interviewer to ensure accuracy. No remuneration or honorarium was available or provided for participation in this study. Analysis and coding were undertaken using a constant-comparative method 12 with transcripts reviewed by a minimum of 2 research team members who came to consensus on themes after independent analysis. Interviews were conducted until saturation of common themes emerged. To ensure quality of data analysis, spot-checking of analysis and coding by a third research team member was also undertaken.
This research was approved by the University of Toronto Research Ethics Board.
Results
Interviews were undertaken in 2 separate rounds to support analysis, coding and confirmation of themes. In round 1 of the study, a total of 15 pharmacists were recruited, and thematic saturation emerged after the 12th interview, with the remaining 3 interviews used for thematic confirmation. In round 2 of interviews, undertaken by a second interviewer, 9 additional interviews were undertaken to further explore details of themes identified in round 1 and to confirm understanding and interpretation of these themes. In total, 24 pharmacists were interviewed for this study. Table 2 provides a summary of demographic characteristics of all research participants, while Table 3 outlines primary themes and subthemes, with corresponding transcript excerpts to support the analysis.
Participant demographics (n = 24)
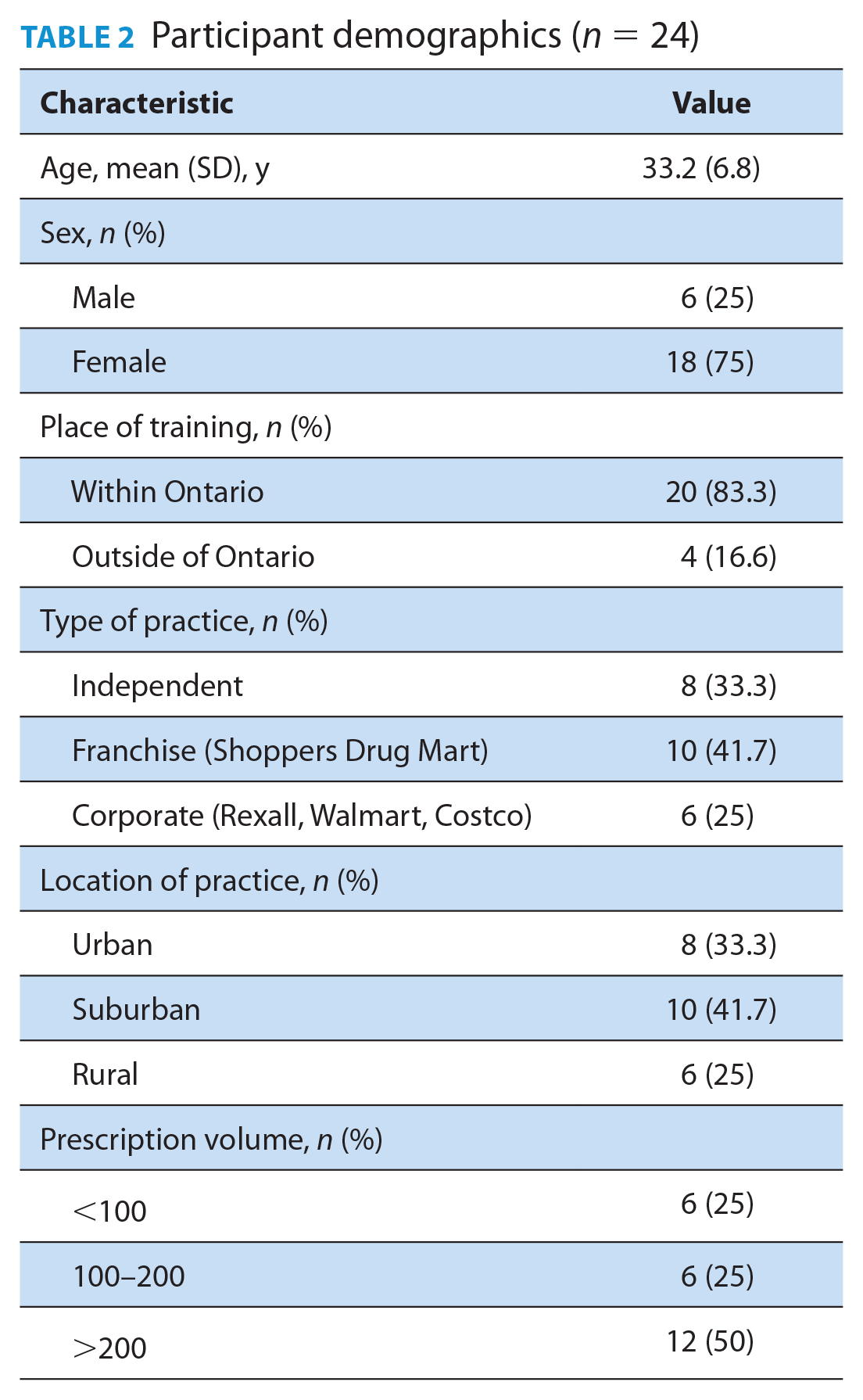
Data themes and transcript excerpts
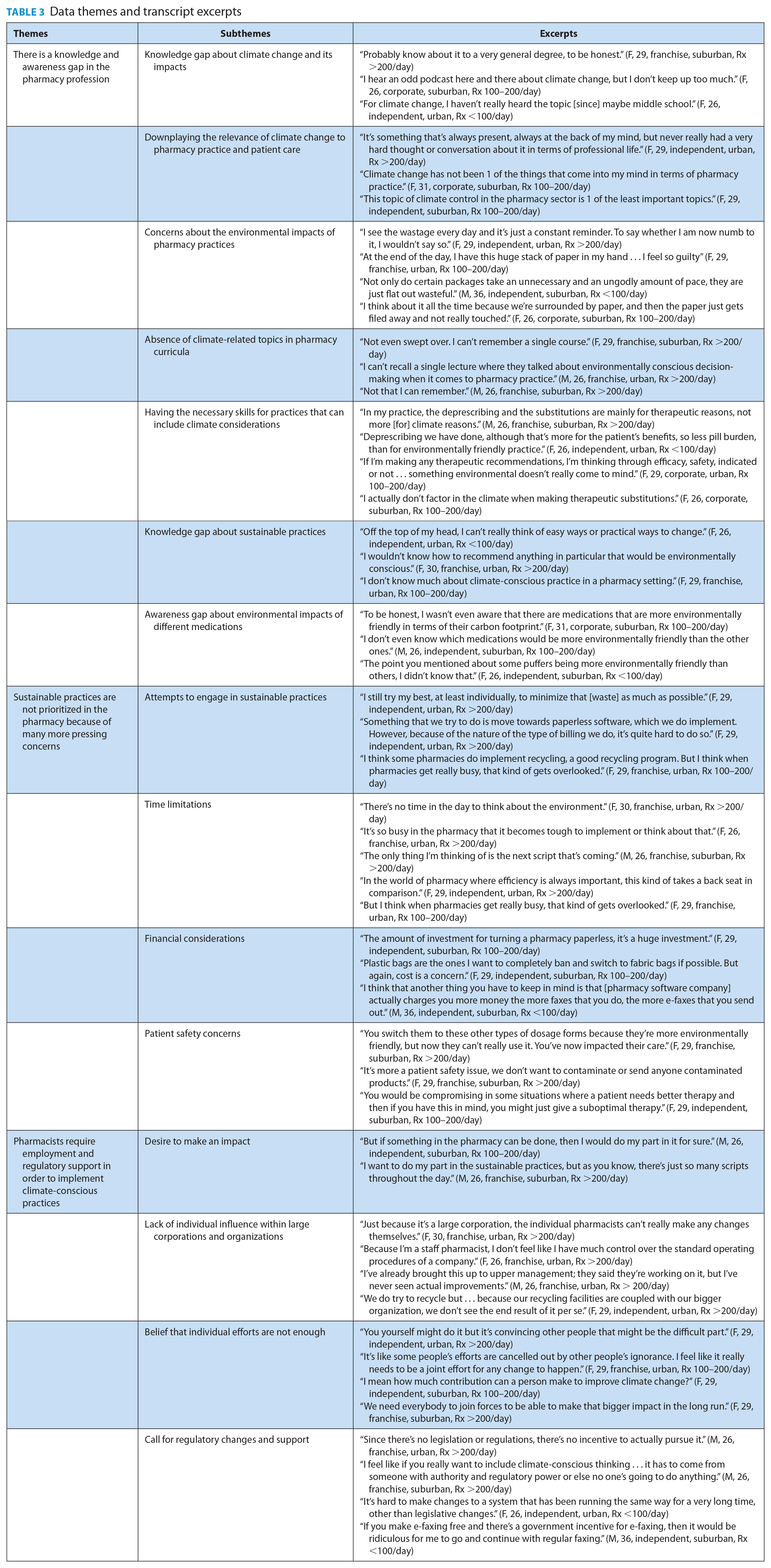
Based on this analysis, 3 key themes emerged from this research:
There is a knowledge and awareness gap related to climate-conscious pharmacy practice
Pharmacists in this study demonstrated only a basic or foundational awareness and understanding of climate change and its implications for planetary health, citing limited encounters with this topic in their personal or professional lives. While all participants in this research demonstrated belief in the reality of human-caused climate change and general concern regarding long-term consequences, there was limited knowledge regarding the specific causes or consequences of this process at the individual, community or global levels. While there was broad general agreement that climate change is an important societal issue, participants noted other pressing societal issues often distracted attention and interest from climate change; most participants understated its urgency, believing the time frames for actual impact of climate change were longer than experts project and that lived impacts themselves would be less severe than currently projected. This lack of urgency, underestimation of severity and deprioritizing of climate change as an issue demanding attention corresponded to a general belief that climate change itself was simply too big an issue for any single individual—let alone a pharmacist—to do anything meaningful. Many participants also expressed belief that other, larger, more powerful groups or individuals bore primary responsibility for managing and mitigating climate change-related issues, both in society generally and in the pharmacy profession specifically. Participants also noted the relative absence of formal or continuing education related to climate-conscious pharmacy practice; few could ever recall even hearing of this concept either during school or subsequently as a pharmacist attending continuing education sessions. Unlike (for example) diversity/equity/inclusion or other important societal issues, the absence of discussion within educational contexts further contributed to the perception that climate-conscious practice was neither a priority nor a practical possibility.
During the course of the interview process, a specific interview prompt scripted into the research protocol provided opportunities to discuss the potential climate impacts associated with high carbon footprint inhalers used routinely for asthma or chronic obstructive pulmonary disease. Within climate-conscious practice, the opportunity to therapeutically substitute less-polluting alternatives is frequently described as a priority strategy and a relatively easy option for pharmacists to consider. None of the participants in this study were aware of this option, nor were they aware of the climate impacts of inhalers in general, despite the prominence of this particular issue within the climate-conscious pharmacy practice literature.
Overall, participants in this research indicated both lack of awareness as well as openness to addressing this lack of awareness through education programs. None of the participants expressed skepticism or climate change denialism, and most expressed some interest in learning more about the issue. This presents useful opportunities for educators, employers, regulators and other stakeholders to consider focused, practical educational programming that builds on general interest, to heighten awareness of climate-conscious pharmacy practice. In the absence of this awareness, even the most commonly cited and relatively straightforward interventions designed to reduce climate impacts of pharmacy work are unlikely to occur spontaneously or at sufficient scale across the profession to have meaningful impact.
Before pharmacists can consider prioritizing environmentally sustainable practices, other more immediate practice-specific concerns must be addressed
While baseline knowledge and awareness of climate-conscious pharmacy practice was noticeably absent among study participants, they also highlighted a variety of structural, workplace, financial and other practice-focused barriers and challenges that they believed would further deprioritize sustainable practices. While most participants indicated that (as individuals) they try to minimize the waste they generate in practice as much as is practically feasible, they also noted that even this relatively straightforward activity was contingent upon time, workload and workplace stress. A prevailing theme throughout this research was the notion that in high-volume, transactionally focused community pharmacy settings, efficiency and cost-effectiveness were priorities that would always trump environmental considerations. Regardless of size or nature of practice (e.g., corporate, independent, grocery, etc.), all participants in this research highlighted the notion that ultimately pharmacies are businesses and business imperatives prioritize short-term financial gain at the expense of environmental sustainability.
One frequent example described by pharmacists working in smaller independent pharmacy contexts included the persistence of paper-based record-keeping/dispensing/inventory management systems, which generate significant waste. Pharmacists in such settings, regardless of their sympathy towards climate-conscious pharmacy practice, highlighted the economic realities associated with shifting towards paperless models of practice and how unrealistic this actually was. Even if pharmacy owners have a strong desire to participate in climate conservation activities, they must weigh this desire against the significant investment in technology, staff training and other opportunity costs. The local physical infrastructure needed to support climate-conscious pharmacy practice has significant costs and implications that could adversely effect business competitiveness.
Of interest, all participants in this study noted that their central professional concern as pharmacists was (and would always be) patient safety. As a result, environmental considerations that were unproven, potentially risky or lacked evidence of proven safety would be regarded with skepticism and likely not be enacted due to fear of potential patient harm. Again, the example of therapeutic substitutions for less polluting inhalers was described: while it may make sense to consider this from an environmental footprint perspective, pharmacists expressed concern that switching a patient who was stabilized on a high-polluting inhaler to a less-polluting alternative, simply for the purpose of carbon footprint reduction, would not be something they would embrace. If this therapeutic substitution had clinical benefits or occurred due to drug shortages, that might be a different matter; however, prioritizing climate impacts of medication choices would be difficult for most of these research participants to actually imagine, given their central concern for patient safety and optimizing therapeutic effectiveness.
This finding raises intriguing questions regarding the way in which climate-conscious pharmacy practice has traditionally been presented to pharmacists. Rather than advocating for climate considerations as the primary reason to select 1 medication over another, it will be necessary instead to provide evidence and resources that highlight therapeutic benefits for individual patients, with secondary climate benefits de-emphasized. Further, the risk-averse nature of pharmacists may resist leveraging of certain expanded scope of practice activities (e.g., therapeutic substitutions or deprescribing) where climate impacts are the primary driver for changing a current stable medication regimen. Further, in the absence of requirements, external grants/funding or other drivers to support “greening” of pharmacy workplaces, it is unlikely that individual pharmacies and pharmacists would consider investing time, money or other resources specifically for the purpose of reducing climate impacts. The abundance of other clinical and business priorities within the environment will relegate climate-conscious pharmacy practice to a “nice to have” role.
Sustainable climate-conscious pharmacy practice will likely require regulatory and employer changes at the profession-wide level, rather than relying solely or extensively on good intentions of frontline pharmacists
A strong and consistent theme throughout this research was the genuine desire of all participants to contribute to the cause of climate-conscious pharmacy practice, despite identified barriers related to economic feasibility or balancing risks and potential patient harms. However, a prevailing sentiment among all participants was also the notion that, as individuals, they could and would only have a very limited potential impact or influence, even if what they were doing required some personal sacrifice. Several participants expressed a sense of powerlessness, particularly within larger corporate structures, where individual pharmacists’ best intentions and goodwill would not result in operational change. Further, some participants noted that even if they as individuals working within larger team or organizational settings worked diligently to adopt climate-conscious practices, these would likely be easily undone by coworkers and colleagues who may not be as conscientious.
Participants in this study independently came to similar general conclusions: the scale of the climate change problem was so large and significant that individual action and good intentions not only were of minimal impact but also verged on meaningless in terms of actual net benefits for the environment. Instead, the issue of climate-conscious pharmacy practice perhaps should be best understood as a collective, profession-wide problem, requiring collective, profession-wide interventions. Several participants noted that the competitive nature of the community pharmacy business meant that large financial investments in “greening” business operations were unlikely, unless they were actually mandated by the regulatory body or another external organization. Several participants spoke about the need for legislated requirements to motivate change and the need for everyone to change simultaneously as the most likely pathway forward for the profession.
Discussion
Findings from this study highlight important concepts for the profession and its leaders to consider. A voluntary approach to climate-conscious pharmacy practice built upon good intentions and personal commitments is unlikely to have meaningful climate impacts, be sustainable in the long term or gain traction because of corporate and competitive realities in the pharmacy world. Mandated requirements (e.g., towards “greening” businesses) that force all pharmacies to undertake the same changes and absorb similar expenses are more likely to be successful, and this will most likely require regulatory leadership. Similarly, mandatory practice guidelines (e.g., with respect to switching to less-polluting inhaler alternatives) would relieve pharmacists of the clinical burden of evaluating on a patient-by-patient basis whether potential clinical harm would outweigh potential environmental benefits. Again, participants noted the role of regulatory mandates and leadership in this area rather than allowing for opt-in decisions based on the individual pharmacist’s clinical judgment. The scope of this kind of regulatory “over-reach” was not considered in this research, nor were the processes by which this could actually be realized. Nonetheless, the notion that other, larger, more powerful forces within the profession would need to mobilize and direct or mandate climate-conscious practice is an important finding of this research: leaving it to the good intentions of individuals would be insufficient for meaningful change.
Findings from this study highlight a central dilemma in climate change work in general,13,14 one that has been described frequently in most contexts beyond pharmacy or health care. The self-perceived powerlessness of individuals to actually undertake meaningful changes to positively influence carbon reduction goals results in perpetuation (and, in some cases, even amplification) of self-destructive polluting behaviours that are paradoxically accelerating climate breakdown. 14 The pervasive belief that 1 individual’s actions and sacrifices will simply be undone by everyone else’s unwillingness to change makes it challenging for individuals to muster the energy or endure the inconvenience or sacrifice that will likely be part of reducing carbon impacts. The belief that external, more powerful societal forces (such as regulatory bodies) or governments need to mandate behavioural change also raises challenging questions. Recent history (e.g., with the carbon tax in Canada) suggests that even these largest of the most powerful of forces cannot resist political pressure or blowback and will often rescind or water down initial proposals, rendering them less impactful.
In many ways, the pharmacists in this study were representative of most Canadians: aware and accepting of the realities of climate change, as well as recognizing the need for something to be done but uncertain that they as individuals could have meaningful impact and, as a result, hesitant to actually sacrifice or adapt personal behaviours in a significant manner. This leads to a belief that a larger, more powerful outside force that compels everyone to change behaviour simultaneously will be required, even though recent history and experience suggest no such force exists. One interpretation of these findings leads to the pessimistic view that climate-conscious pharmacy practice may simply never materialize and that the array of realities (financial, clinical, logistical, etc.) aligned against environmental sustainability is simply too well-entrenched and powerful, and as a result, climate breakdown will worsen over time in catastrophic ways because of human inaction. However, a more optimistic reading of these data highlights some potential levers for educators, policy makers, regulators and others. Pharmacists in this study demonstrated sincere interest in doing something to address climate change but lacked awareness, infrastructure, support and tools to do so. This, in turn, diminished their self-confidence to actually see small, incremental, individual actions as meaningfully contributing to carbon reduction goals. However, this sincere interest is an important starting point for potential change, and further research will be required to identify how to build on this finding in ways that can actually be impactful.
Strengths and limitations
This article is one of the first in Canada to examine climate-conscious pharmacy practice from the perspective of frontline community pharmacists and has identified opportunities for further research in this area. The convenience and snowball sampling method used, coupled with the focus on pharmacists in southern Ontario, limits generalizability. The participants in this study were not representative of the pharmacy workforce as a whole, and in particular, there was an underrepresentation of international pharmacy graduates. While safeguards to ensure the trustworthiness of analysis of data from interviews were employed (including independent double coding of data and interviewing to thematic saturation), other techniques (such as member checking) were not possible due to logistical constraints. These limitations highlight the need for cautious interpretation of these findings and illuminate possibilities for further research across a wider scope of pharmacy and health care settings.
Conclusions
This study has highlighted the complexity associated with adopting climate-conscious pharmacy practice. The perspectives of frontline community pharmacists will be essential to consider: this study has highlighted opportunities for further research and work to build on general interest and goodwill, in ways that are aligned with the practical constraints and realities community pharmacists face. Reduction of carbon footprints will be the most important and challenging work of our lifetimes; creating an environment where each individual feels empowered and motivated to support necessary behavioural changes will require concerted effort. Our planetary health demands it. ■
Footnotes
Author Contributions:
A.Z.: data collection, analysis, first draft of manuscript; P.G.: study conceptualization, data analysis, revision of manuscript; Z.A.: study conceptualization, study design, research ethics approval, oversight of data collection, analysis, manuscript preparation, principal investigator/senior author.
Declaration of Conflicting Interests:
The authors have no conflicts of interest to disclose.
Funding:
This project was funded by the Network for Improving Health Systems (NIHS). The views expressed in this article are those of the authors and do not necessarily reflect those of the funder.
