Abstract
Purpose
Previous comparative mechanical thrombectomy device trials reported a substantial crossover rate from first-line aspiration to stent-retriever thrombectomy. A specialized delivery catheter may help track large-bore aspiration catheters to target occlusions. We report our multicenter experience of aspiration thrombectomy of intracranial large vessel occlusions using the FreeClimbTM 70 and Tenzing® 7 delivery catheter (Route 92, San Mateo, CA).
Methods
After local Institutional Review Board approval, we retrospectively reviewed the clinical, procedural, and imaging data of patients who underwent mechanical thrombectomy with the FreeClimb 70 and Tenzing 7.
Results
FreeClimb 70 was successfully delivered using Tenzing 7 to target occlusion in 30/30 (100%) patients (18 M1, 6 M2, 4 ICA-terminus, and 2 basilar artery occlusions), without the use of a stent-retriever for anchoring. In 21/30 (70%) cases, a leading microwire was not needed to advance the Tenzing 7 to the target. Median (interquartile range) time from groin puncture to first pass was 12 (interquartile range 8–15) minutes. Overall first pass effect, or first pass effect (modified thrombolysis in cerebral ischemia 2C-3), was achieved 16/30 (53%). For M1 occlusions, first pass effect was 11/18 (61%). Successful reperfusion (modified thrombolysis in cerebral ischemia ≥ 2B) was achieved in 29/30 (97%) cases after a median of 1 pass (interquartile range 1–3). Median groin puncture to reperfusion time was 16 (interquartile range 12–26) minutes. There were no procedural complications or symptomatic intracranial hemorrhage. Average improvement in National Institutes of Health Stroke Scale at discharge was 6.6 ± 7.1. There were three patient deaths (renal failure, respiratory failure, and comfort care).
Conclusions
Initial data support the use of Tenzing 7 with FreeClimb 70 catheter for reliable access to rapid, effective, and safe aspiration thrombectomy of large vessel occlusions.
Introduction
Aspiration thrombectomy (AT) is an efficient and cost-effective means of rapidly restoring perfusion in large vessel occlusion (LVO) stroke patients.1–3 Proposed advantages of first-line AT over stent-retrievers (SR) include faster time to first pass, less need to pass microwires and microcatheters into more distal artery branches beyond the embolus, decreased damage to the endothelium, 4 decreased vessel traction during device removal, decreased clot disruption, and decreased cost. 5 Two randomized trials comparing first-line SR versus AT techniques achieved similar rates of successful reperfusion and 90-day functional independence,1,2 with cost savings achieved in the AT cohort. In the ASTER trial, 1 however, first-line AT was associated with 32.8% crossover rates to SR thrombectomy or combined SR with local aspiration, either due to inability to deliver the aspiration catheters to the target occlusion, or due to unsuccessful thrombectomy after the initial pass(es).
Aspiration catheter design improvements have permitted larger inner diameter (ID) at the tip (for increased suction force), and improved catheter trackability (or deliverability) through tortuous anatomy. The use of large bore catheters for AT (0.070–0.074 inch distal ID) is associated with increased aspiration flow rates, first pass effect (FPE), faster recanalization, reduced procedure time, and better reperfusion rates.6,7 The FreeClimb 70 (Route 92 Medical, San Mateo, California, USA) catheter with ID of 0.070 inches was recently Food and Drug Administration-cleared for access use in neurovascular procedures, and can be delivered through a 0.088-inch guide catheter. Concurrently, a specialized delivery catheter, Tenzing 7 (Route 92), was developed to assist the tracking of larger aspiration catheters to the target occlusion site. Compared to traditional aspiration catheter delivery using a microwire and microcatheter, Tenzing 7 significantly reduces the ledge or space between itself and the tip of a 0.070–0.074 ID aspiration catheter, which is especially important with the increasing caliber of aspiration catheters, which have a greater tendency to catch on the ophthalmic artery or anterior cerebral artery origins and encounter increased friction in tortuous anatomy. In an in vitro study, Tenzing 7 delivered aspiration catheters to the proximal M1 in half the time compared to leading with a microwire and microcatheter. 8 Tenzing 7 may provide a more robust rail in the center of the vessel lumen and avoid the use of an SR. Tenzing may also be less disruptive to the clot and less likely to induce thrombus fragmentation and distal embolization.
Herein, we report our initial in-human multicenter experience with the FreeClimb 70 catheter delivered using Tenzing 7 for AT, for the purpose of assessing the efficacy and safety of these devices. We hypothesize that the Tenzing 7 and FreeClimb 70 combination is associated with more consistent and rapid access to the clot, FPE, and diminished use of a SR. 9
Methods
Consecutive patients with LVO acute ischemic stroke who underwent first-line aspiration approach thrombectomy using the Tenzing 7 delivery catheter and FreeClimb 70 access catheter at five different stroke centers from October 2022 to March 2023 were retrospectively reviewed.
Eligible patients received intravenous thrombolytic therapy, in the absence of contraindications to thrombolytic therapy, according American Heart Association (AHA) Guidelines. 10 All patients who received mechanical thrombectomy (MT) had evidence of LVO on CT angiogram. Patient selection for thrombectomy was based on the most recent AHA Guidelines, 10 using advanced imaging with head non-contrast computed tomography (CT), CT angiography and/or CT perfusion. Patients included in this series were found to have a large cerebral vessel occlusion with viable ischemic penumbra (6–24 h) in the vascular territory supplied by the occluded target artery. We confirm that this study is an observational, minimal-risk study and no patient informed consent is required as the research does not include any patient-identifying information. This study was approved by the Institutional Review Board of each participating institution.
The Tenzing 7 (Route 92 Medical) is a novel delivery catheter specifically designed to deliver large-bore catheters. The Tenzing 7 has a smooth, flexible, conical tapered 2 cm tip that reduces the ledge between it and catheters with an ID between 0.068 and 0.072 inch (Figure 1). Tenzing 7 can be used with microwires up to 0.016 inch in diameter. It has a 151 cm working length made from a stainless steel reinforced polymer design.
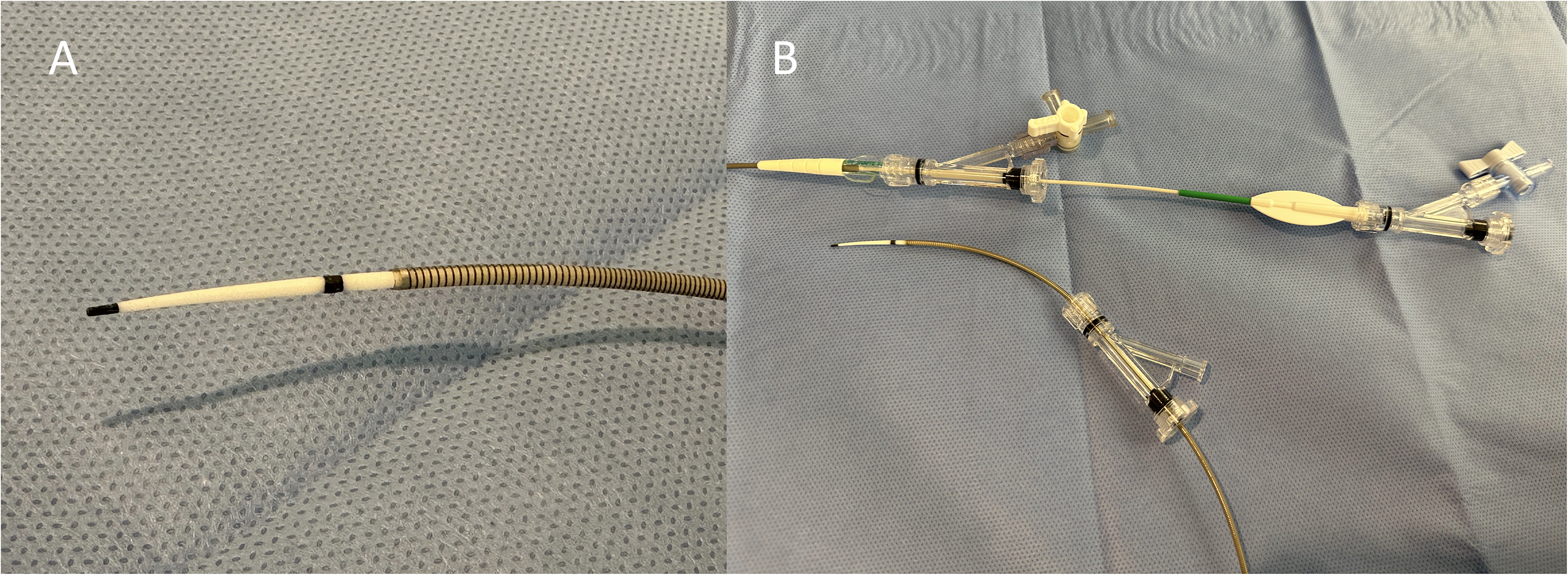
(a) photograph of the 0.070 inch distal inner diameter FreeClimb 70 catheter (gray-black striped) and tapering Tenzing 7 delivery catheter (white with two radiopaque black distal markers). (b) Photograph of typical catheter setup for Tenzing 7 and FreeClimb 70. The Tenzing 7 delivery catheter is positioned within the FreeClimb70 catheter so that the distal tip of the FreeClimb catheter is immediately proximal to the proximal marker of the Tenzing 7 (i.e., just proximal to the tapering tip of the Tenzing 7). The Tenzing 7 is locked in this position with the rotating hemostatic valve of the FreeClimb catheter. Loading a 0.014–0.016 inch microwire inside the Tenzing is optional. (Note: heparinized saline drip connection tubing typically connected but not included in image).
The Route 92 Medical FreeClimb 70 is a catheter with a continuous 0.070 ID and 0.082 inch outer diameter (Figure 1). It has a working length of 132 cm and is of braided nitinol construction. The catheter was designed specifically for use with Tenzing 7, with a tailored stiffness-to-flexibility profile for optimized performance with Tenzing. During the study period, FreeClimb 70 was approved as a catheter facilitating the insertion and guidance of microcatheters into a selected blood vessel in the neurovascular system, according to the FDA indication for use. During the study period, FreeClimb 70 was not FDA-approved as an intracranial aspiration catheter for MT, and the cases included in this study are of off-label use.
Study variables
Collected data for each patient included age, sex, race, stroke risk factors (hypertension, diabetes, hyperlipidemia, atrial fibrillation, and smoking), time of symptom onset, stroke severity on arrival measured by the National Institutes of Health Stroke Scale (NIHSS), baseline functional status as measured by modified Ranking Scale (mRS) before symptom onset, IV thrombolytic use, and time of groin puncture. Patient imaging, including admission CT, admission CT angiography were reviewed to document the admission Alberta Stroke Program Early CT score (ASPECTS), and the location of the vascular occlusion. Angiography, clinical, and procedural reports, and follow-up CT or magnetic resonance imaging were reviewed to document outcome variables: number of passes, reperfusion time, procedural complications, rate of symptomatic intracerebral hemorrhage (sICH), discharge NIHSS, and procedural complications. Reperfusion score using the modified Thrombolysis in Cerebral Ischemia (mTICI) grading scale was used to document pre-thrombectomy occlusion and post-thrombectomy revascularization. sICH was defined using the European Australian Cooperative Acute Stroke Study II definition: any intracerebral hemorrhage on any posttreatment imaging after the start of tissue plasminogen activator and increase of ≥4 points on the NIHSS points. 11
Technique
Thrombectomy procedures were performed by one of 8 experienced neurointerventionalists. In brief, transfemoral vascular access was obtained using a 9-French or 10-French femoral sheath. A large guide catheter [NeuronMAX 088 (Penumbra, Alameda, CA); Infinity Long Sheath (Stryker Corp., Fremont, CA, USA); Ballast (BALT, Montmorency, France); Walrus (Q’Apel, Fremont, CA); TracStar LDP Large Distal Platform (Imperative Care, Campbell, CA); Base Camp® and HiPoint® 088 (Route 92 Medical) was advanced into the proximal cervical segment of the internal carotid artery (ICA) or distal common carotid artery. Radial access was used in one case.
Typical catheter preparation is shown in Figure 1. The Tenzing 7 delivery catheter is positioned within the FreeClimb70 catheter so that the distal tip of the FreeClimb catheter is immediately proximal to the proximal marker of the Tenzing 7 (i.e., just proximal to the tapering tip of the Tenzing 7). The Tenzing 7 is locked in this position with the rotating hemostatic valve of the FreeClimb catheter). Loading a 0.014–0.016 inch microwire inside the Tenzing is optional. These catheters are then advanced as a single unit until the distal tip marker of the Tenzing 7 reaches the angiographic limit of contrast at the site of the LVO. The Tenzing 7 is then pinned, and the Freeclimb 70 catheter is advanced over the Tenzing 7 to the angiographic limit of contrast (Figure 2, Supplemental videos 1 and 2). During this maneuver, we concurrently observe the Tenzing 7 tip movement to ensure that the angiographic limit of contrast is not crossed by the proximal marker of the Tenzing 7 tip. In some cases, subtle back-and-forth movements of the Tenzing 7 during FreeClimb advancement can assist in reducing the static friction between catheters and vessel wall, and assisting in FreeClimb delivery to target. Once the FreeClimb 70 catheter reaches the angiographic limit of contrast, the Tenzing 7 delivery catheter is removed and the Freeclimb 70 catheter is allowed to advance passively into the occlusion, as the vacuum created by Tenzing 7 removal may assist with clot ingestion. 12 Vacuum aspiration was then applied with a pump for 3–5 min. The Freeclimb 70 is then slowly withdrawn until either, (a) free blood return is observed in the aspiration tubing, or, (b) if no free flow is seen in the tubing during withdrawal, the catheter is completely removed from the patient. Infrequently, a microwire (0.014–0.016 inch) is utilized when the tip of the Tenzing 7 device engages a side branch of the parent artery (e.g., ophthalmic, posterior communicating artery, anterior communicating artery) during advancement. If incomplete recanalization was observed, additional AT attempts were made. In some cases, if accessible distal emboli were present, or rescue therapy was necessary, additional devices were used to perform thrombectomy passes, including: Zoom 35, 55, and 71 (Imperative Care), 3MAX and 4MAX (Penumbra), Solitaire X 4 × 20 mm (Medtronic, Minneapolis, MN), and Trevo NXT 4 × 28 (Stryker).
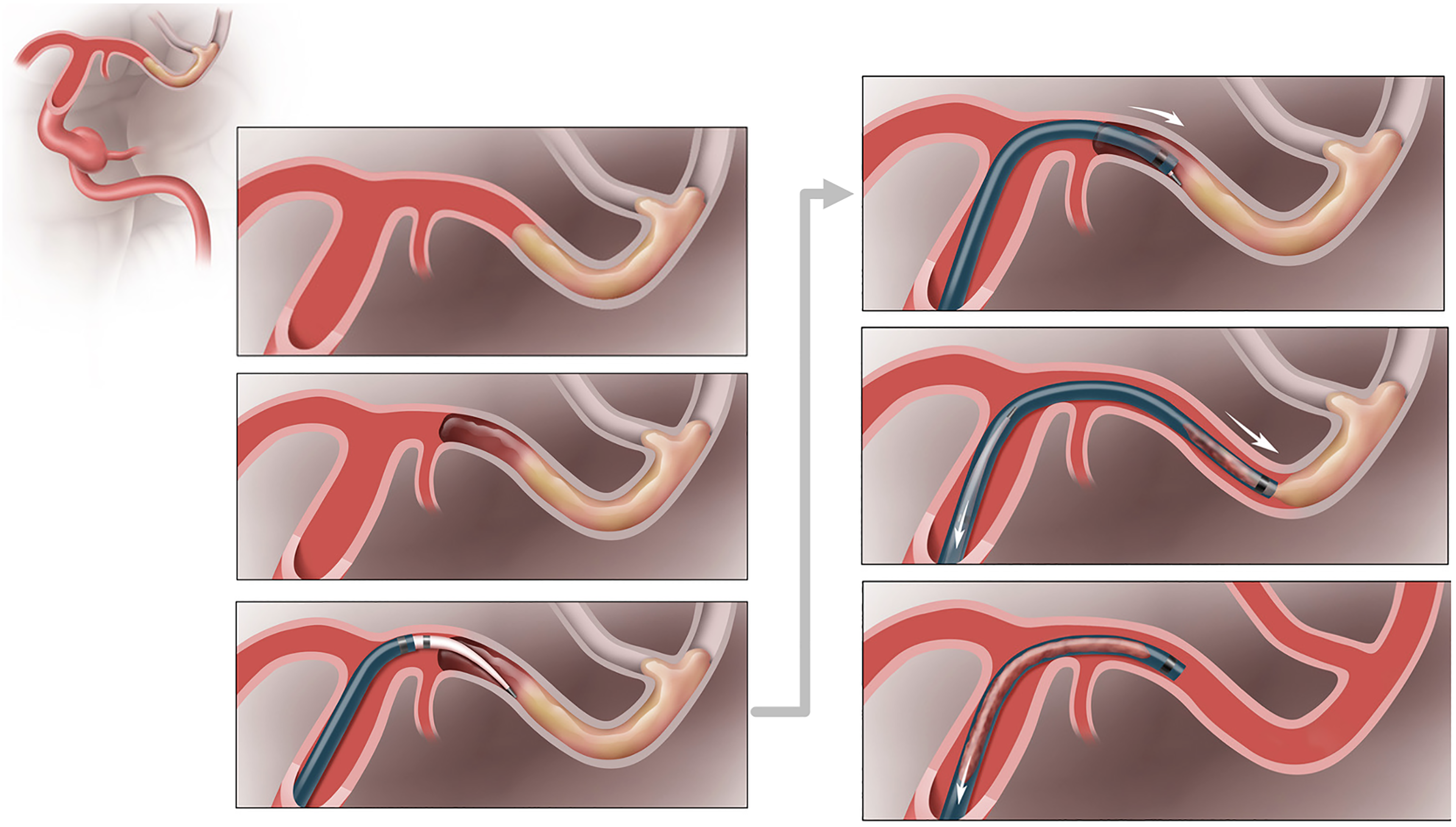
Tenzing technique for aspiration thrombectomy. The Tenzing 7 and FreeClimb 70 catheters are advanced as a single unit (see Figure 1 setup) until the distal tip marker of the Tenzing 7 reaches the angiographic limit of contrast at the site of the large vessel occlusions (LVO). The Tenzing 7 is then pinned, and the Freeclimb 70 catheter advanced over the Tenzing 7 to the angiographic limit of contrast. During this maneuver, we concurrently observe the Tenzing 7 tip movement to ensure that the angiographic limit of contrast is not crossed by the proximal marker of the Tenzing 7 tip. In some cases, subtle back-and-forth movements of the Tenzing 7 during FreeClimb advancement can assist in reducing the static friction between catheters and vessel wall, and assisting in FreeClimb delivery to target. Once the FreeClimb 70 catheter reaches the angiographic limit of contrast, the Tenzing 7 delivery catheter is removed and the Freeclimb 70 catheter is allowed to advance passively into the occlusion, as the vacuum created by Tenzing 7 removal may assist with clot ingestion. 12 Vacuum aspiration was then applied with a pump for 3–5 min. The Freeclimb 70 is then slowly withdrawn until either, (a) free blood return is observed in the aspiration tubing, or, (b) if no free flow is seen in the tubing during withdrawal, the catheter is completely removed from the patient.
Statistical analyses
Descriptive statistics were used to report patient demographic and clinical characteristics in the included patients. The analysis was conducted using SPSS v25 (IBM Corp., Armonk, New York, USA).
Results
Thirty consecutive patients underwent first-line AT using the Tenzing 7 delivery catheter and FreeClimb 70 catheter at five different institutions during the study period (Table 1, Figure 3). Mean age was 73.8 ± 12.8 years, and 16 of 30 (53%) were female. Hypertension was noted in 26/30, and hyperlipidemia in 17/30. Tandem occlusions were present in 3/30 (10%). Median baseline mRS was 0 (interquartile range [IQR] 0–1) and initial NIHSS was 17 (IQR 12–21). Median ASPECTS was 9 (IQR 7–10). 11/30 (37%) patients received IV thrombolytic.
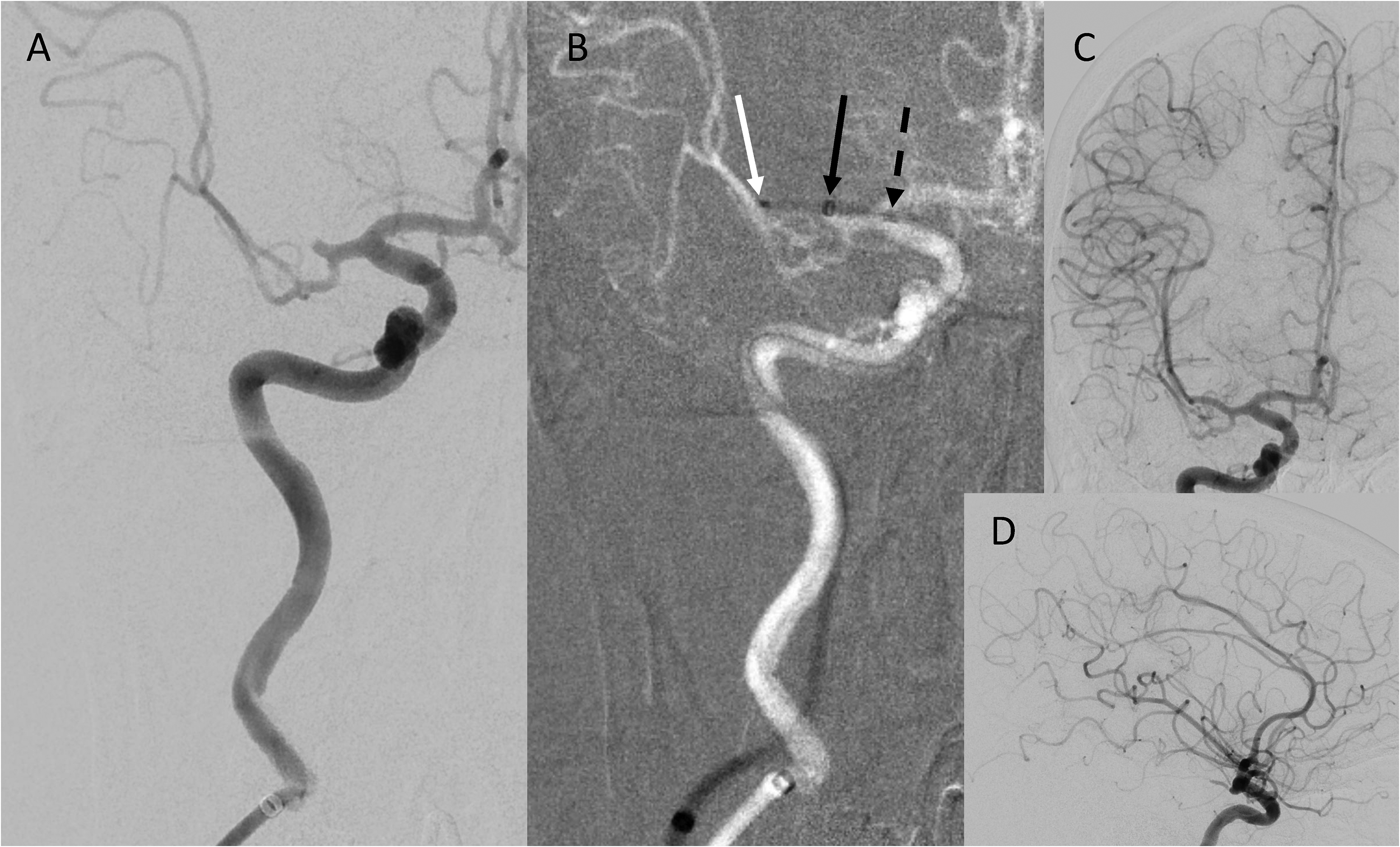
Sexagenarian with an initial NIHSS 20, ASPECTS 7, found to have a right M2 MCA occlusion on CTA and confirmed on (a) initial digital subtraction angiography anteroposterior (AP) view. (b) Navigation of the Tenzing 7 tip (distal marker: White arrow, proximal marker: Dashed black arrow) to the thrombus, used to deliver the FreeClimb 70 catheter to the angiographic limit of contrast (black arrow) (see also online Supplemental videos 1 and 2). After Tenzing 7 removal and 3 min of vacuum pump aspiration, final cerebral angiogram AP (c) and lateral (d) views after one pass showing mTICI 3 reperfusion. At time of hospital discharge, the patient's NIHSS had improved to 3. NIHSS: National Institutes of Health Stroke Scale; mTICI: modified thrombolysis in cerebral ischemia; ASPECTS: Alberta Stroke Program Early Computed Tomographic score; MCA: middle cerebral artery.
Patient demographics, baseline characteristics, thrombectomy results.

ASPECTS: Alberta Stroke Program Early CT Score; ICA: internal carotid artery; MCA: middle cerebral artery; mRS: modified Rankin Scale; mTICI: modified thrombolysis in cerebral infarction; NIHSS: National Institutes of Health Stroke Scale; tPA: tissue plasminogen activator; IQR: interquartile range; FPE: first pass effect.
Angiographic data and outcomes
General anesthesia was used for the thrombectomy procedure in 27/30 cases (90%). Table 1 summarizes the baseline demographics, procedural and outcome characteristics of the study patients. Transfemoral access was used in 29/30 (97%) cases and radial access in one patient. Aortic arch anatomy was Type I in 9/30 (30%), Type II in 17/30 (57%), and Type III in 4/30 (13%). Nearly all target occlusions were in the anterior circulation (M1 segment, n = 18; ICA terminus, n = 4; M2 segment, n = 6; basilar, n = 2). AT was performed with the FreeClimb 70 catheter delivered successfully to the target occlusion over a Tenzing 7 delivery catheter (Figure 2) in all 30/30 cases (100%). None of the patients required a SR to deliver the aspiration catheter to the target occlusion. Median (IQR) time from groin puncture to first pass was 12 (8–15) minutes.
In 7/30 (23%) cases, a leading microwire was required due to the Tenzing 7 preferential selection of an arterial branch (ophthalmic, posterior communicating, posterior inferior cerebellar artery) (supplemental videos 1 and 2). FPE (mTICI 2C or 3 after the first pass) was achieved 16/30 (53%). For M1 occlusions, the FPE (mTICI 2c or 3) was 11/18 (61%). Successful reperfusion (mTICI ≥ 2B) was achieved in 29/30 (97%) cases after a median of 1 pass (IQR 1–3). Final mTICI scores of 2b, 2c, or 3 were achieved in 3 (10%), 11 (37%), and 15 (50%) patients, respectively. Median groin puncture to reperfusion time was 16 (IQR 12–28) minutes. Aspiration alone led to successful reperfusion in 28/30 (93%) patients. In 10/30 (33%) cases, additional devices were used to perform thrombectomy (see Methods). Rescue SR thrombectomy was performed in only 2/30 (7%) patients, with these 2 cases requiring 6 passes each, and procedure times of 68 and 99 min. No vessel perforation, dissection, or other procedural complications were observed during the procedures.
Underlying intracranial atherosclerotic disease (ICAD) was noted in 3/30 (10%), including the cases which required rescue SR thrombectomy. One case with underlying ICAD did not have successful reperfusion (Final mTICI 1) after 6 attempts, including SR: last known well > 2 days prior, with MT achieving transient flow restoration which re-occluded after initial thrombectomy and was not stented due to moderate-sized completed infarct.
Clinical outcomes
None of the patients had symptomatic ICH following the procedure. Post-procedure imaging showed any intracranial hemorrhage in 17/30 patients (57%): 12 with scattered petechial hemorrhage(s) (HI1), 3 with confluent petechial hemorrhage(s) but no mass effect (HI2), and one with small volume subarachnoid hemorrhage, according to Heidelberg bleeding classification. At discharge, the median NIHSS score of the patients who survived was 5 (IQR 2–16). The average improvement in NIHSS from presentation to discharge was 6.6 ± 7.1, excluding three patients that died (3/30, 10%) during hospitalization. One death was from acute decompensation of oliguric chronic renal failure. Another patient suffered acute respiratory failure in the setting of COPD and methamphetamine-related cardiomyopathy and heart failure. The third death was related to transition to comfort care after a large cerebral infarct following unsuccessful reperfusion.
Discussion
This study demonstrated consistent (100%) access to the target LVO when using the Tenzing 7 delivery catheter with FreeClimb 70 access catheter, without the use of a SR for anchoring and without procedural complication. Use of the Tenzing 7 delivery catheter in AT significantly reduces the shelf, or ledge, between an inner delivery catheter and outer aspiration catheter and likely reduces tracking force necessary to advance an aspiration catheter.8,13,14 This is especially important with the increasing caliber of aspiration catheters, which get caught on branch artery origins and/or experience increased friction in tortuous anatomy. The Tenzing delivery catheter provides a robust rail for the aspiration catheter which is relatively centered in the vessel lumen. In an in vitro study, it was previously shown that Tenzing 7 is capable of delivering aspiration catheters to the proximal M1 segment middle cerebral artery in half the time compared to a leading microwire/microcatheter. 8 Another potential advantage of Tenzing is that it may avoid crossing and potentially disrupting the clot. 15 In addition, once the FreeClimb 70 catheter is at the face of the clot, removal of the Tenzing creates a vacuum in the FreeClimb catheter lumen, initiating ingestion of the thrombus by the catheter tip. 12
In our study, the median (IQR) time from groin puncture to first pass was 12 (8–15) minutes. The median (IQR) time from groin puncture to reperfusion was 16 (12–26) minutes which is faster than most previous reports using other large bore 0.070–0.074 inch ID aspiration catheters16–24 (Table 2). Comparison of the results of this study with other aspiration catheter studies is somewhat limited by considerable variation in techniques, with some prior studies using a SR as an anchor and rail over which an aspiration catheter is advanced20,25; other studies using first-line AT technique delivered the aspiration catheter to the target occlusion with a 0.021 inch ID microcatheter over a 0.014–0.016 inch microwire 16 ; and others studies using both techniques, according to operator discretion.17–19,21–24. Nonetheless, Tenzing 7 and FreeClimb 70 AT resulted in similar efficacy [97% successful reperfusion, 53% FPE mTICI 2C-3, after median 1 pass], discharge NIHSS improvement, and an excellent safety profile when compared to previously published reports using other currently commercially available 0.070–0.074 inch ID aspiration catheters (Table 2).16–24
Summary of clinical studies using large bore (0.070–0.074) aspiration catheters.
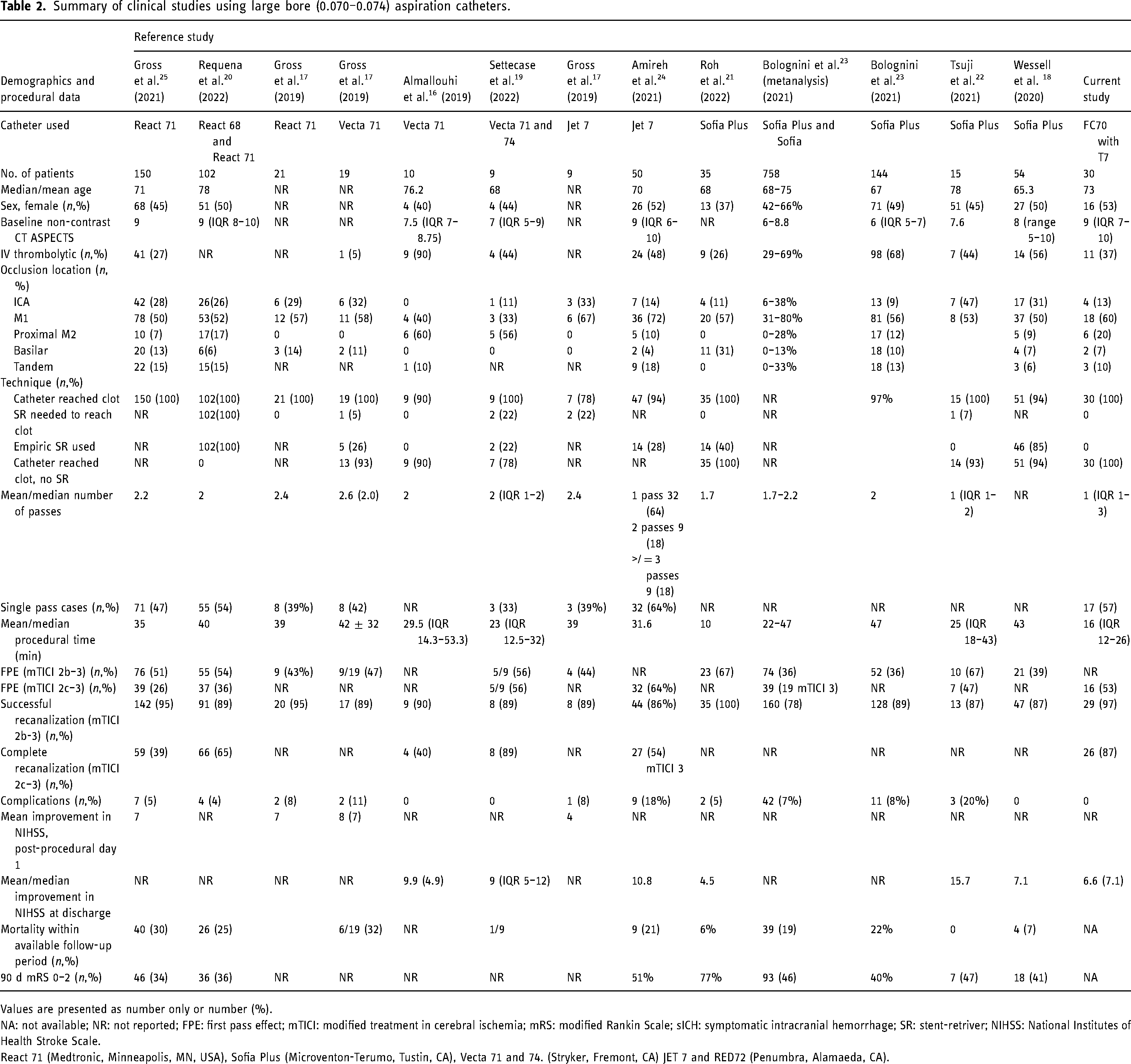
Values are presented as number only or number (%).
NA: not available; NR: not reported; FPE: first pass effect; mTICI: modified treatment in cerebral ischemia; mRS: modified Rankin Scale; sICH: symptomatic intracranial hemorrhage; SR: stent-retriver; NIHSS: National Institutes of Health Stroke Scale.
React 71 (Medtronic, Minneapolis, MN, USA), Sofia Plus (Microventon-Terumo, Tustin, CA), Vecta 71 and 74. (Stryker, Fremont, CA) JET 7 and RED72 (Penumbra, Alamaeda, CA).
Several studies comparing larger aspiration catheters to those with a smaller bore have shown improved outcomes, shorter procedure times, and lower likelihood of using additional devices with larger bore, without impacting complication rates.6,26 This relates not only to increased suction force at clot with larger IDs, but also increased aspiration flow rate with decreasing catheter size to vessel diameter ratio. 7 Consequently, design and engineering improvements have permitted a trend of increasing catheter distal ID, without clinically significant sacrifices in navigability, pushability, and durability in most instances. 27 In the ASTER and COMPASS trials, the first-line AT cohorts used older generation 0.064–0.068 inch ID aspiration catheters. The comparative efficacy of first-line AT with current large bore (0.070 inch ID or greater) aspiration catheters to first-line SR technique, however, has not been studied in comparative clinical trials. Furthermore, comparative studies between SR technique and AT technique using ledge-reducing delivery catheters, such as Tenzing 7, are also lacking.
Previous studies have shown the Tenzing delivery catheter is highly effective for tracking large (0.070–0.074 inch ID) as well as “super large” (0.088 inch ID) bore aspiration catheters12,19,28 to intracranial LVO. In a prospective trial, Caldwell et al. 28 reported Tenzing 7 catheter facilitated delivery of HiPoint 70 aspiration catheter (Route 92 medical), as well as Tenzing 8 (a slightly larger version of the Tenzing developed for 0.088 ID catheters) facilitated the delivery of an HiPoint 88 catheter (Route 92 Medical). 28 In all 45/45 (100%) cases in their study, the catheters were successfully delivered to the target occlusions in the ICA-T (n = 12), M1 (n = 27) and M2 (n = 6) segments. In the same study, the Tenzing delivery catheter navigated to the embolus without needing a leading microwire in 71% (32/45) of cases, a rate similar to that observed in this study (77%). In another multicenter study by Massari et al., 12 a Tenzing 8 was used to successfully deliver HiPoint 88 in 33 (100%) consecutive patients with 34 LVO (17 M1, 17 ICA-T). We previously reported a case series with AXS Vecta 71 and 74 catheters, in which 7/9 cases were first-line AT approach, with Tenzing 7 permitting access to the target occlusion in all 7 cases (4 M2, 2 M1, and 1 ICA-T occlusions). In this study, we were also able to track the FreeClimb 70 catheters to the proximal M2 segment MCA in five patients. It is important, however, that operators using an aspiration catheter of this size for AT recognize that in patients who have significant ICAD or acute angles at the M1 bifurcation, caution should be used to avoid arterial injury. The angle of interaction between the aspiration catheter and the clot has also been found to affect the efficacy of thromboaspiration. 29 Moreover, in some cases utilizing aspiration as a first-line approach, the combination of SR and aspiration catheter may be necessary to retrieve emboli that are resistant to initial direct aspiration passes (including 2/30 cases in this study). The infrequent use of SRs in this study for either delivery of the aspiration catheter or for rescue therapy, suggests that use of a Tenzing delivery catheter and FreeClimb 70 may offer cost-savings compared to other approaches or devices.
This study is limited by the small number of patients treated with the Tenzing 7 and FreeClimb 70 catheters, as well as the lack of a control group. In addition, there was no independent core lab adjudication of angiographic results. Due to the limited initial supply of devices, more patients could not be treated with FreeClimb 70. We sought to reduce the impact of patient selection bias by including consecutive patients with LVO from five high-volume centers with actively maintained thrombectomy databases. Moreover, since these patients were recently treated, a 90-day mRS follow-up is not yet available. Larger scale studies are necessary to confirm the initial findings and detect potential complications of using Tenzing 7 and FreeClimb 70 catheters. Future in-human and in vitro studies comparing aspiration catheters from different vendors should also include Freeclimb 70 catheters and Tenzing delivery catheters.
Conclusions
In this early AT experience with the Tenzing 7 and FreeClimb 70 catheters, access to the target occlusion was 100%, without the use of an SR. This delivery catheter and aspiration catheter combination permitted rapid LVO access and successful reperfusion in 96% of patients without procedural complications. Larger studies are needed to confirm the findings and further assess the efficacy and safety of the Tenzing 7 delivery catheter and FreeClimb 70 catheter.
Footnotes
Author contributions
Concept and designwere handled by FS, JDE. Analysis and interpretation were done by FS. Data collection was done by FS, TS, RK, DR, JDE, JC, and RH. Writing the article was handled by FS. Critical revision of the article was done by FS, JC, RK, RH, DR, TS, WTK, and JDE. Final approval of the article was done by FS, JC, RK, RH, DR, TS, WTK and JDE. Statistical analysis was carried out by FS. Overall responsibilitywas taken by FS.
Ethical approval
All data were deidentified and unlinked to any identifiers. The pseudonymized data of each study were sent to one author for statistical analysis. The Institutional Review Board of each participating center approved the study and waived the need for patient consent.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: FS: Consultant fees, Stryker Neurovascular and Route 92 Medical; Honoraria for lectures, Stryker Neurovascular; Travel, Medtronic; Research Grants: Microvention, Stryker, Sutter West Bay Medical Group. WTK: Consultant fees, Stryker Neurovascular; Consultant fees, Travel reimbursements, and Stock Options, Route 92 Medical. TS: Speaker Fees, Penumbra. RK: None. JC: Consultant fees, Route 92 Medical, SL: Consultant fees and travel/meeting Support, Route 92 Medical. RH: Consultant fees, Imperative Care; Receipt of equipment to institution, Route 92 Medical. DH: No disclosures. JDE: Consultant fees, Stryker Neurovascular; Consultant fees, Travel reimbursements, and Stock Options, Route 92 Medical, Co-founder and Chief Medical Officer, Route 92 Medical.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
