Abstract
Dietary interventions for disease prevention have been well studied, yet standard American diets often fall short. Limited culinary skills and nutritional literacy are key contributors. Shared medical appointments (SMAs) with culinary education offer one solution to enhance culinary and nutrition literacy. In our model, patients were recruited from the University of Texas Southwestern Culinary Medicine Clinic to participate in a culinary medicine-focused SMA program located in local church kitchens in Dallas, TX including 6 classes over 2 months. Classes, led by a physician and culinary dietitian, included goal-setting, culinary skill demonstration, and supervised cooking. Classes were billed as primary care visits through patients’ insurance. Health records and patient reported data were collected to assess feasibility. Sixty patients from four cohorts of SMAs had a 75% average attendance. Patients were predominantly Black (55%) and female (87%). Hypertension, diabetes, and obesity were the most common referral diagnoses. Qualitative telephone interviews (n = 18) reveal that co-learning new skills with peers is an important contributor to patient engagement. In conclusion, culinary medicine-focused SMAs are a feasible approach to deliver culinary nutrition education, demonstrate high levels of engagement and retention, and lay the foundation for a financially sustainable model.
Keywords
“Successful recruitment and retention highlight the potential for sustainable integration of CM into clinical practice, particularly when co-led and co-located within trusted community spaces.”
Introduction
Diet-related chronic diseases including hypertension, hyperlipidemia, diabetes and obesity continue to rise in the United States (US), leading to increased cardiovascular and all-cause mortality.1-6 Evidence shows that dietary interventions like the Mediterranean diet and Dietary Approaches to Stop Hypertension are cost-effective tools for chronic disease prevention.7-12 However, most standard American diets fall short of recommendations. 13
Key barriers to healthy eating include declining culinary skills, 14 limited home cooking,15,16 high availability of convenience foods, 17 and low nutrition and health literacy,18,19 which disproportionately affect urban, low-income populations due to structural, economic, and caregiving demands.19-22 In addition, only 40% of patients report receiving dietary counseling in primary care due to lack of clinician time, compensation, nutrition knowledge, and resources.23-25 Furthermore, diverse cultural norms and community context demand tailored strategies that current clinical models struggle to accommodate.
Shared medical appointments (SMAs)—group visits for patients with similar conditions—offer an efficient, reimbursable solution for delivering nutrition education and peer support 26 and have been shown to improve well-being and clinical outcomes in populations with chronic disease.27-32 Culinary medicine (CM)-focused SMAs (CM-SMAs) expand this model by bridging clinical care with hands-on nutrition education.33,34 Individualized progress with nutrition goals is integrated with traditional medical care in a relaxed environment that builds culinary skills, nutrition knowledge, and peer support.
Although CM-SMAs have shown early efficacy in several pilot studies,35,36 few studies have examined the feasibility of SMAs embedded in community settings with integrated leadership from community partners. This report evaluates the implementation of CM-SMAs at a large academic medical institution by describing clinic-community partnership development, patient engagement and retention, and clinical operations including billing and staffing.
Setting
Following the successful launch of a CM eConsult initiative,37,38 the University of Texas Southwestern (UTSW) CM team established a novel physician-dietitian CM clinic at a community-based, university affiliated clinic in December 2022. 39 Community input from town halls and focus groups identified a strong desire for hands-on, food-focused nutrition education. Utilizing an established CM education framework,40-42 the team partnered with community leaders to develop an SMA-based nutrition curriculum context.
In 2022, CM leaders also engaged two churches in an under-resourced Dallas community to serve as partner sites. These churches were selected based on their proximity to the CM Clinic, availability of commercial kitchen and discussion spaces, location in food insecure ZIP-codes, 43 community service history, and alignment with CM’s mission to support the practical needs of community members while building lasting systems for health promotion.
Planning involved iterative meetings with church leaders and local stakeholders, including community advocates and staff, to define a shared vision. Refurbishment of church kitchen spaces was then conducted, with purchase of all supplies including cookware, kitchen utensils, cutting boards, portable burners, and stainless-steel tables funded by the National Center for Advancing Translational Sciences’ Clinical Translational Science Award Program.
Demonstration classes were then held to gather feedback on logistics, curriculum, class experience, and integration with other community programs. Patient classes began after establishing leasing agreements with the health system that defined the church’s kitchen facilities as a clinical site of service during classes. Leasing a site of service also necessitates paying a fair market value rate determined regionally and required by Centers for Medicare and Medicaid Services (CMS).
44
Each church hosted identical classes on separate days, with didactic components held in fellowship halls and cooking sessions in adjacent church kitchens (Figure 1A-B). (A) Photo of an SMA Teaching Space. This photo shows the community partner’s multipurpose fellowship hall space used for athletic events, meetings, and presentations. Table set-up and cooking demonstration reflect a typical didactic education space for a culinary medicine shared medical appointment. (B) Photo of an SMA Cooking Space. This photo shows the community partner’s kitchen space including the portable stainless-steel table set-up for a culinary medicine shared medical appointment for up to 16 patients.
Participants
Patients were recruited in person or via phone from the UTSW CM Clinic during their initial or follow-up consultation visits in the 6 months leading up to the beginning of classes. A minority of patients were referred by primary care physicians at UTSW. Exclusion criteria included severe food allergies to ensure patient safety, non-English speakers due to lack of bilingual staff available, and physical or cognitive limitations that may preclude safe kitchen participation.
Program Description
Program Course and Curriculum
Each CM-SMA course consisted of six 120-minute classes over 8-10 weeks. Classes were led by a CM-certified physician (JA) and culinary dietitian (MS). 45 Before class, two CM clinic staff members documented attendance and vital signs, including an optional weight measurement, behind a privacy screen. Patients in cohorts 2 and 3 completed a combined Mini-EAT nine-item rapid dietary screener 46 and Cooking and Food Skills questionnaire. 47 During the first class, patients also received a binder to store handouts and recipes from the class.
Class Topics, Key Themes, and Sample Recipes for SMA Series.
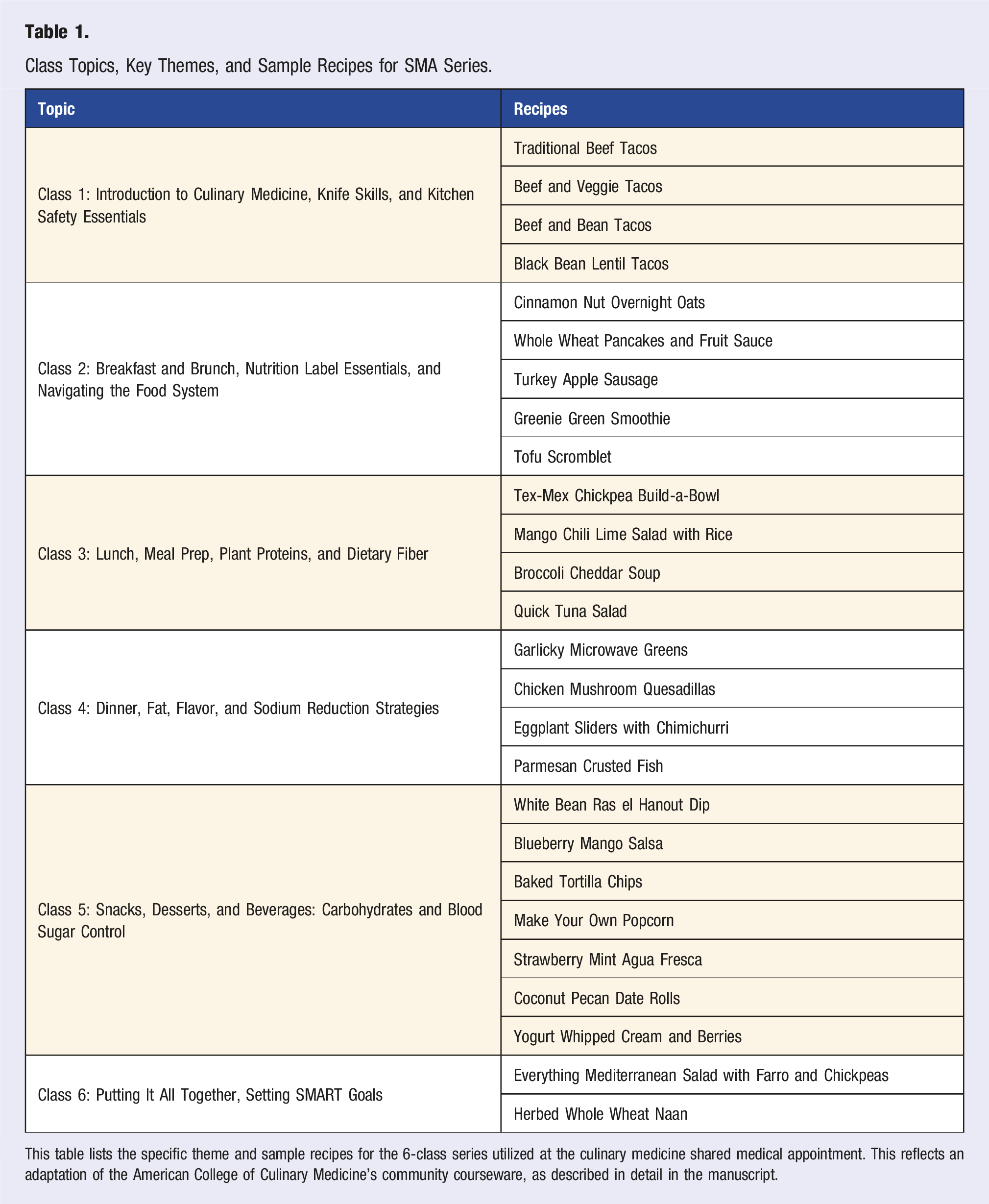
This table lists the specific theme and sample recipes for the 6-class series utilized at the culinary medicine shared medical appointment. This reflects an adaptation of the American College of Culinary Medicine’s community courseware, as described in detail in the manuscript.
Each session began with an icebreaker where patients voluntarily shared information about their health goals and lifestyle change successes and challenges. Patients were given an opportunity to hear peer feedback and encouragement in response. Patients completed individual health goal-setting worksheets and initially discussed these with the physician privately during the cooking portion of the first class, and subsequent classes allowed patients to share updates on their goals publicly in group discussion or privately if preferred. Subsequently, patients participated in hands-on cooking sessions led by the culinary dietitian to prepare a variety of assigned recipes in small groups guided by volunteers and prepared a shared presentation plate for group tasting. Each team then described their dish, sharing reflections on preparation, cultural adaptation, and nutrition takeaways. Sessions concluded with a group discussion and goal reinforcement led by the CM team.
Program Billing
SMA billing, as previously established, 49 applies to established patients in a health system or network. The CM Clinic exists within the primary care service line at UTSW, therefore all patients seen in the CM clinic are considered established patients for the shared appointment billing. The CM physician billed SMA classes as primary care visits to insurance utilizing individual evaluation and management codes (typically billing codes 99213 or 99214 based on complexity of health conditions addressed by the SMA content). Patients may have a copay as required by their individual insurance.
Each patient received individualized care through discussion and documentation of their reasons for joining class and personal goals and challenges, review of their vital signs and class engagement, and review of relevant lab and imaging data. These data informed the treatment plan for each patient which linked their health conditions to both the dietary interventions taught during the SMA as well as their other treatment components including medical therapies.
Program Evaluation
Evaluation Methods
All patients were assigned a patient code to maintain anonymity. Demographics and clinical data were collected from the electronic health record (EHR). Attendance was tracked in Excel. Patient surveys were collected electronically via REDCap. A convenience sample (n = 39) from the first three cohorts were called (up to 3 calls to attempt to reach each patient) by a dietetic intern for a feedback phone interview 3-6 months post-intervention. Responses to five structured questions were analyzed using framework analysis by two independent researchers (WW, AA).
Demographics
Patient Characteristics and Attendance.
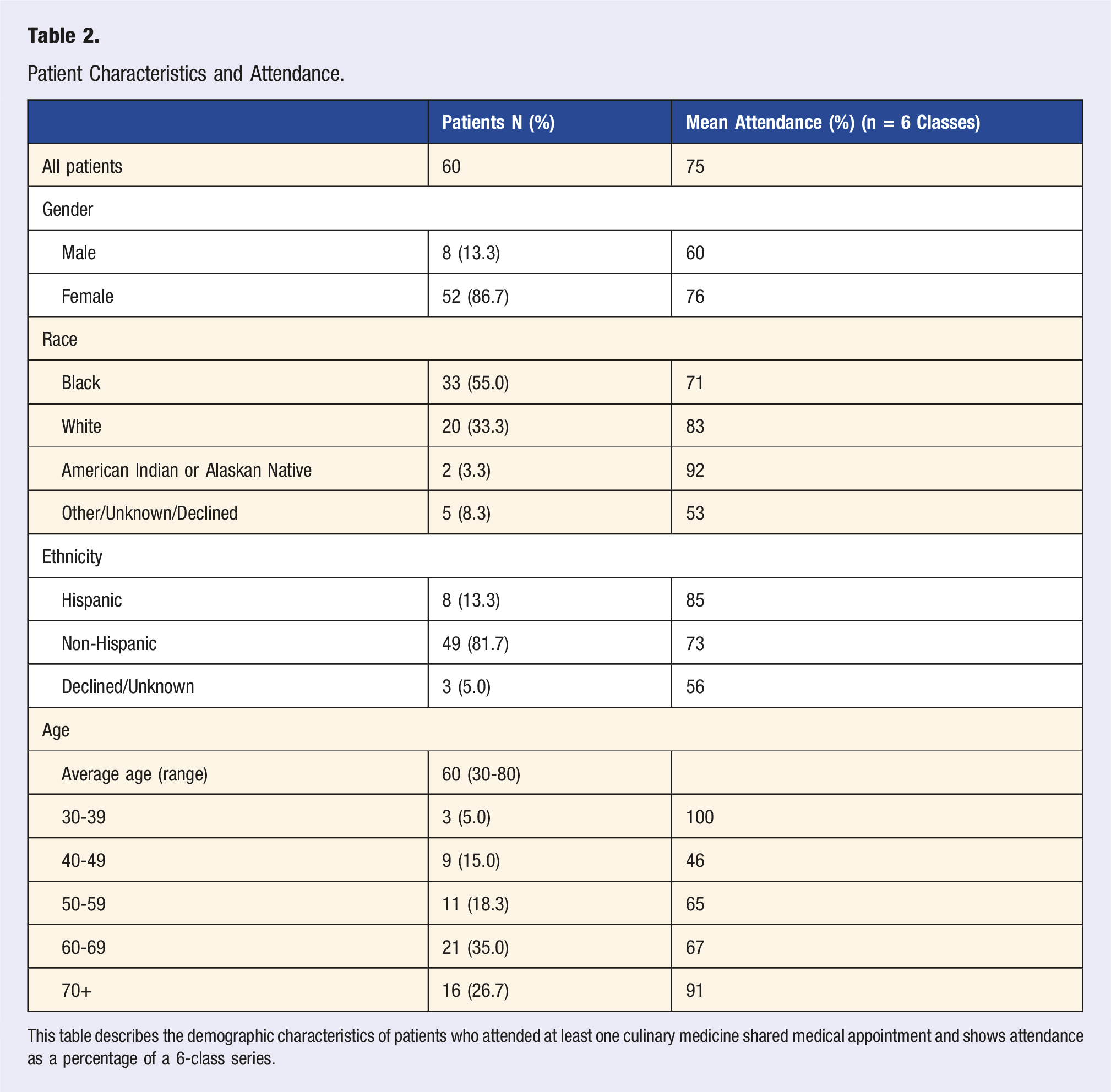
This table describes the demographic characteristics of patients who attended at least one culinary medicine shared medical appointment and shows attendance as a percentage of a 6-class series.
Patient Referral and Billing Diagnosis (N = 60).
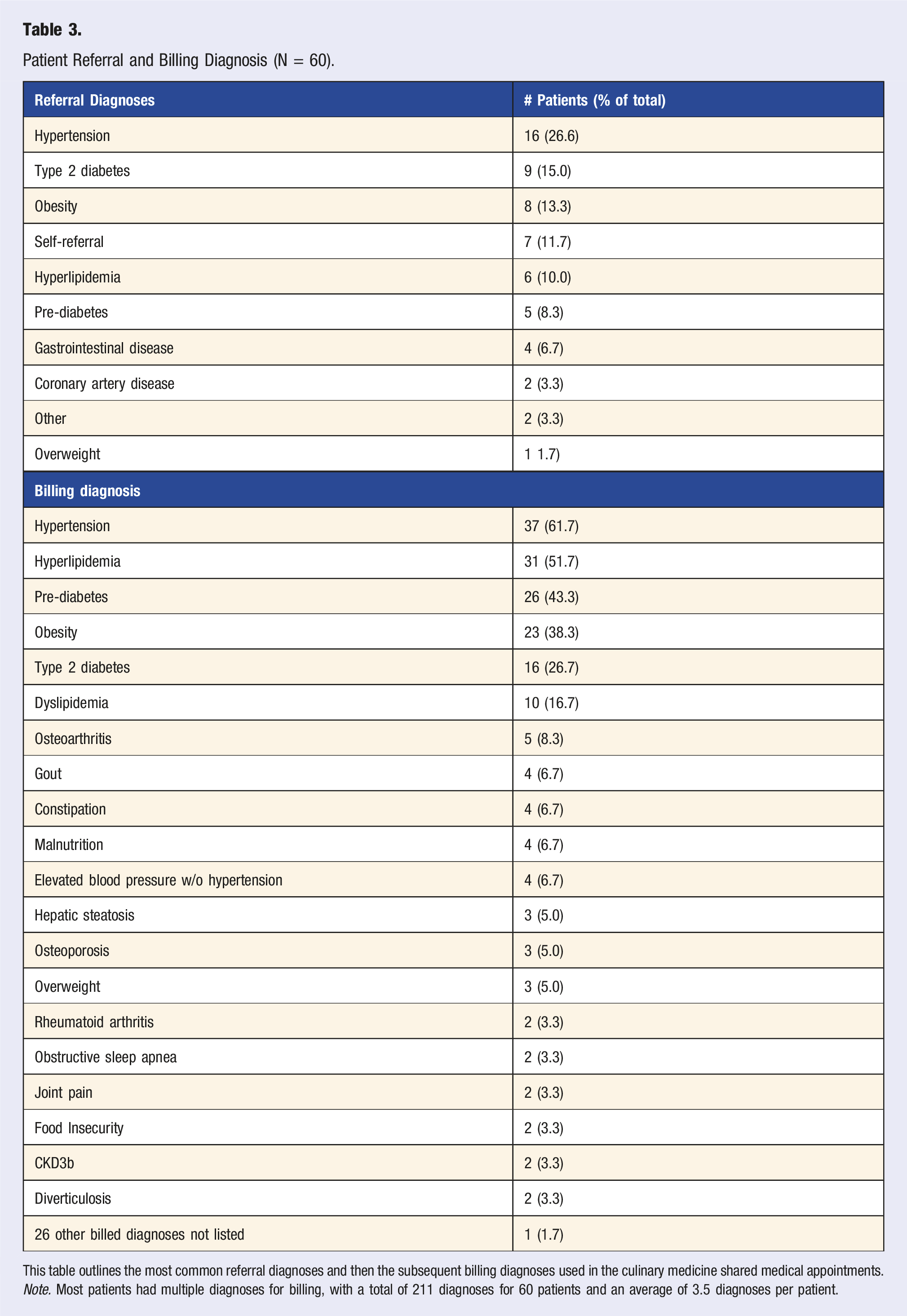
This table outlines the most common referral diagnoses and then the subsequent billing diagnoses used in the culinary medicine shared medical appointments.
Engagement and Retention
Average participation across all cohorts was 75% (4.4 classes out of 6). A majority (n = 46, 77%) of patients attended more than half (four or more) of classes, with one-third of patients (n = 22, 37%) having perfect attendance (Figure 2). Patients by Number of Classes Attended (n = 60). This figure provides a graphic visual of culinary medicine shared medical appointment attendance, showing that the majority of patients attended 4 or more classes in the 6-class series.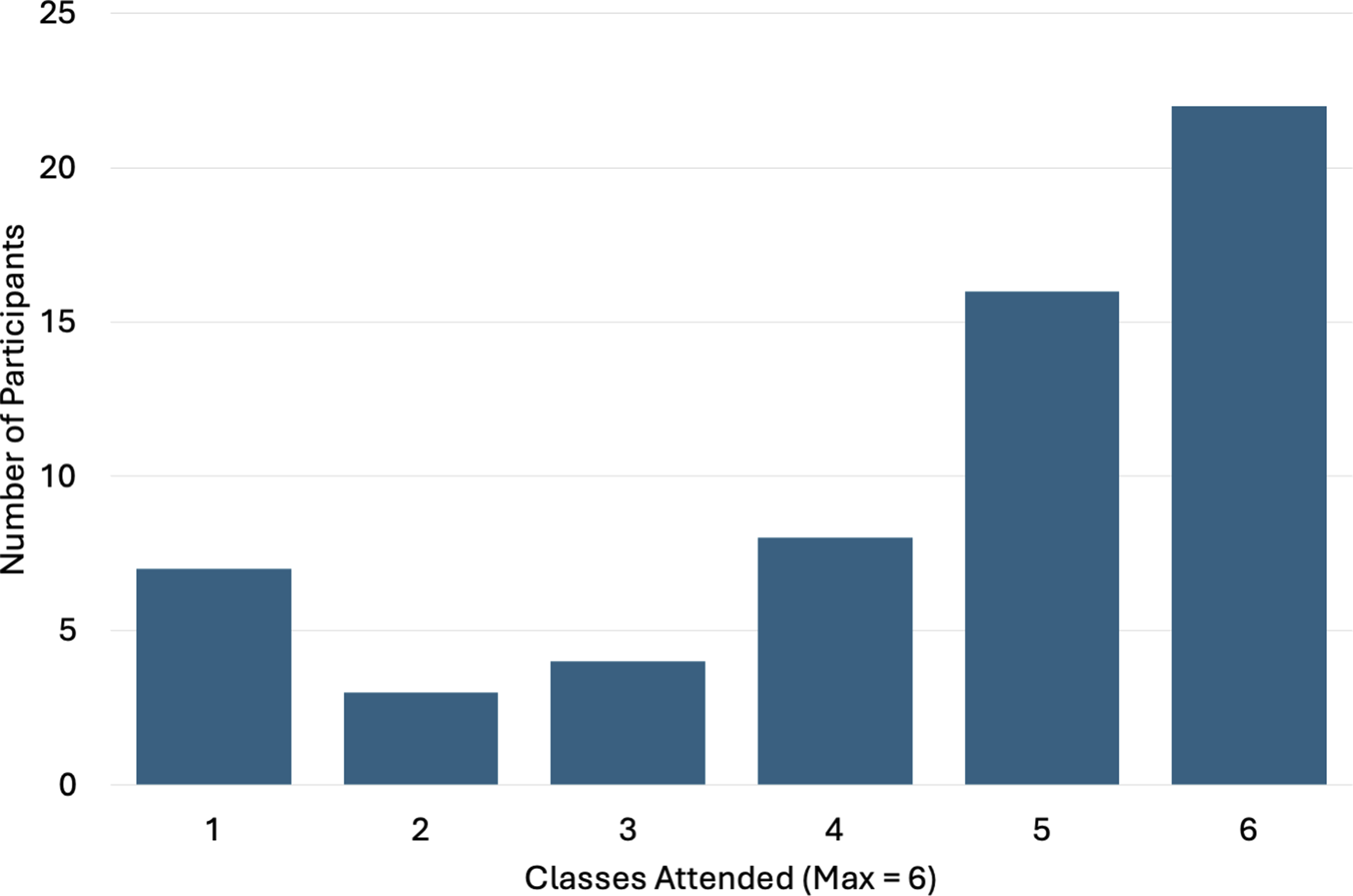
Feedback Interviews
Patient Phone Interview Rapid Analysis Grid.
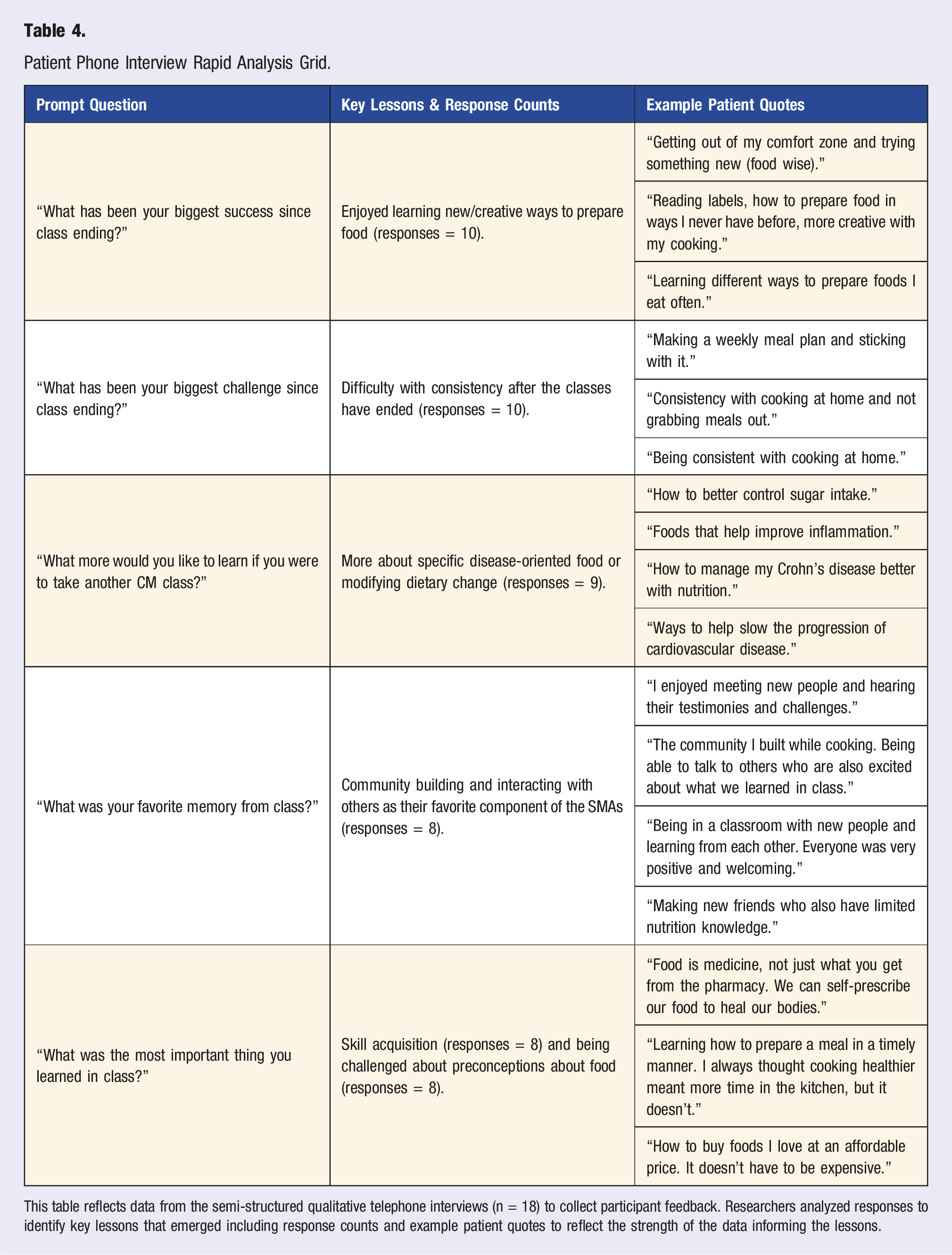
This table reflects data from the semi-structured qualitative telephone interviews (n = 18) to collect participant feedback. Researchers analyzed responses to identify key lessons that emerged including response counts and example patient quotes to reflect the strength of the data informing the lessons.
Discussion
Our study demonstrates the feasibility of and high patient engagement in community-based CM-SMAs, with attendance rates comparable to or exceeding those in similar interventions. 27 Successful recruitment and retention highlight the potential for sustainable integration of CM into clinical practice, particularly when co-led and co-located within trusted community spaces. These partnerships aligned clinical care with community needs which likely contributed to enhanced participation and offer valuable insights for future program development.
Notably, our patients were primarily recruited from the CM Clinic in the southern sector of Dallas County, likely representing a motivated population actively seeking dietary change. While this may limit generalizability, we feel that this group remains representative of a significant and growing portion of the population currently seeking practical tools to improve their health24,51,52 and remains a meaningful starting point for evaluating program feasibility. Additionally, although women predominantly attended our classes—possibly a reflection of societal norms and responsibilities as nutritional gatekeepers53-56—they have the potential to act as catalysts for broader community impact through their culinary education. 57 Future efforts should expand outreach to less motivated populations including engagements of more men in CM.
Qualitative feedback from phone interviews emphasized the value of relationship-building and peer support in the group format, suggesting that consistent patient cohorts may strengthen behavioral change through deeper social connections. Although this may limit the reach for recruitment due to strict cohort start and end dates that may not align with patient’s personal commitments, it may also foster deeper group cohesion and mutual support that can enhance the process of behavior change. 58 Skills learned during the program also appeared to persist for at least 3-6 months. Lastly, patients expressed interest in disease-specific education, which points to future directions for condition-tailored curricula and targeted recruitment.
Several limitations of our study should be noted. First, we were unable to collect and report on relevant clinical measures of diet-related disease (e.g., cholesterol or hemoglobin A1c) as our sample size was limited and our participants experienced a diverse range of metabolic conditions. Additionally, as a pragmatic study in a non-clinical setting, vital signs were not consistently measured with appropriate blood pressure cuff sizes. Weight measurements were also optional based on stakeholder and patient feedback. Further, while we attempted to administer patient surveys via electronic tablets, many found the interface confusing and thus were unable to submit the surveys or submitted incomplete or incorrectly entered responses. This may reflect a gap in technological or health literacy. Future survey administration may necessitate the simplicity of pen-and-paper and incorporation of a higher level of hands-on support for accurate completion.
Launching clinical care in community partner sites adds additional administrative burden, a practical limitation of this work. In addition to initial partnership building, a team member needs to regularly coordinate scheduling and leasing agreement renewals with each partner site. Finally, our small cohort size limits the generalizability of our results to other populations. However, the patients recruited into the SMAs were initially recruited to the CM clinic via primary care clinics, thus are representative of a general primary care population seen in Dallas and supported successful evaluation of program implementation and feasibility in the local context.
Overall, this study demonstrates the feasibility, reimbursement consistency, and high patient engagement of community-based Culinary Medicine Shared Medical Appointments (CM-SMAs) delivered in partnership with local churches in an under-resourced setting. Future iterations should explore strategies to engage broader populations, incorporate robust clinical outcomes to assess long-term impact, and evaluate cost-effectiveness of CM-SMAs at the population level.
Footnotes
Acknowledgments
Contributors: The authors would like to thank the many community partners that helped to shape this model by attending stakeholder classes and providing feedback, particularly including staff and volunteers at Oak Cliff Bible Fellowship, Concord Church, and Crossroads Community Services. Additionally, medical and dietetic students as well as resident physicians provided invaluable support as volunteers who designed educational materials, delivered patient guidance during classes, and endlessly attended to practical needs, from assembling resources to doing many, many dishes! Finally, we wish to thank the UTSW Informatics team including Tin Khine and graduate student Pratikshya Aryal who iteratively built a dashboard to support data collation and analysis for this clinical model.
ORCID iDs
Ethical Considerations
On May 24, 2024, the Institutional Review Board at the University of Texas Southwestern Medical Center determined that the implementation and feedback analyses of the shared medical appointment group classes classified as program evaluation and qualified as non-regulated research.
Consent to Participate
See above ethical considerations section.
Consent for Publication
See above ethical considerations section.
Author Contributions
JA and MS conceptualized the design and implementation of the described model with close collaboration and stakeholder engagement with GS and NDR. AA and AK provided core implementation support. WW led data analysis in collaboration with JA. AA and WW extensively contributed to manuscript drafting and major editing. HK supported acquisition of funding and community engagement expertise. KHH provided community engagement support and data collection support. MEB and CSM provided thoughtful guidance in evaluation approach and formative manuscript edits. All authors reviewed, edited, and approved the final version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Research reported in this publication was supported by the National Center for Advancing Translational Sciences of the National Institutes of Health under award Number UL1 TR003163. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH (National Institutes of Health).
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: MEB declares research support from Boehringer Ingelheim (unrelated to this work). JA serves on the Advisory Board and is a Committee Chair for The American College of Culinary Medicine focused on the development of educational strategy and tools in graduate medical education. JA also serves on the Advisory Board for the Teaching Kitchen Collaborative. All other authors declare no conflicts of interest.
Data Availability Statement
All raw data evaluated in the formation of this manuscript is available upon request to the corresponding author.
