Abstract
Keywords
“Health issues were the most often endorsed barrier to visiting the Clinic, followed by inadequate supplies of food and inability to store or reheat food.”
Introduction
Food insecurity (FI), defined as limited or uncertain access to affordable and nutritious food, is emerging as an important clinical issue among patients undergoing metabolic bariatric surgery (MBS). 1 Patients with FI are less able to adhere to dietary recommendations that target consumption of nutrient-dense foods and adoption of healthier eating patterns to minimize post-surgical complications and optimize clinical outcomes. 1 Food prescription programs (FPPs), in which produce is prescribed often on the basis of a voucher system, are offered to eligible individuals to increase the availability of fruits and vegetables and to reduce FI in under-resourced populations. To our knowledge, no reports have evaluated FPPs in preoperative and postoperative MBS patients with FI.
Hartford Hospital Food4Health Clinic
In May 2022, Hartford Healthcare, the largest healthcare organization in the state, piloted the Food4Health Clinic (the Clinic) at Hartford Hospital, the system’s 867 bed flagship community-based teaching hospital and tertiary care center located in the capitol city of Hartford, Connecticut. The Clinic was created to address the high rates of food insecurity, lack of access to food and related chronic conditions such as obesity, diabetes and hypertension among Hartford’s under-resourced, urban population. Patients from six hospital divisions: Heart Failure, Dental Services, Metabolic Bariatric Surgery and Obesity Medicine (MBSOM), Adult Primary Care, Specialty Clinics and Diabetes Life Care were provided prescriptions for the Clinic. Eligibility for a prescription to the Clinic was based on the presence of FI documented through affirmative responses to a two-item Hunger Vital Sign screener
2
: 1. In the past 12 months, you worried that your food would run out before you got money to buy more. 2. In the past 12 months, the food that you bought ran out and you didn’t have money to buy more.
Patients were referred to the clinic via a prescription if they answered “sometimes true” or “often true” to either of these questions, were receiving either Medicare or Medicaid or had a diagnosis of chronic diet-related disease state (e.g., diabetes). Patients were prescribed weekly Clinic visits for either 6 or 12 months. The Clinic is open on Monday from 11 am to 3 pm, Tuesday from 3 pm to 7 pm and Thursday from 8 am to noon. It is located in a non-descript building on the Hartford Hospital campus (Figure 1) and is staffed by bilingual (English/Spanish) workers from Hartford Hospital’s community health department who are trained to assess patient needs. Clients are welcome to bring their children, and transportation is provided for those who live within five miles of the Clinic. Upon referral, patients receive a brochure detailing clinic location, schedule and availability of resources, including parking (available in the visitor garage or at a meter for a fee), transportation, assistance with carrying groceries, and the availability of a registered dietitian. Produce grown on roof top gardens at Hartford Hospital (upper left), along with other healthy choices (lower left), is distributed to patients at the food pharmacy, housed at a discreet location on the Hartford Hospital campus (right).
Despite the Clinic’s patient-centered approach, program records indicated that only one-third of the patients prescribed through MBSOM ever visited the Clinic. This underutilization among MBSOM patients was the main reason for the evaluation, which aimed to assess usage, satisfaction, and barriers to participation in the program among patients who had undergone, or were planning to undergo, bariatric surgery.
Evaluation
We explored program usage, satisfaction, and barriers in a convenience sample of 55 consecutive English- and Spanish speaking MBS patients with FI who were written a prescription for the Clinic from May to October 2022.
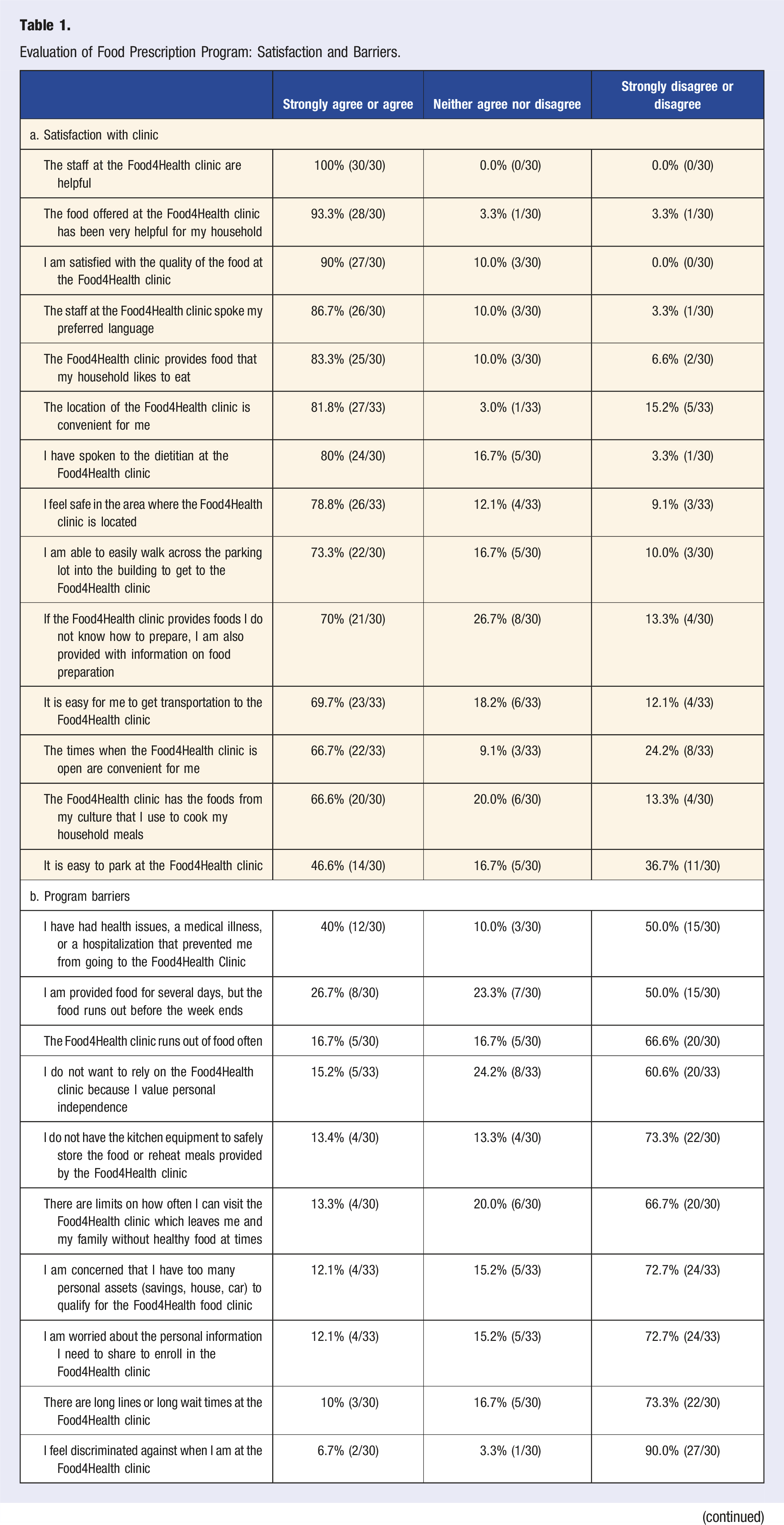
Evaluation of Food Prescription Program: Satisfaction and Barriers.
Referrals, Visits, Facilitators, and Barriers
Referrals
Of the 55 patients referred from MBSOM, 43 provided email addresses and were invited to complete the survey, 33 returned the survey. Among the 55 patients referred, 87.8% were female, 24.2% were African American, 21.2% Caucasian, and 45.4% were Latino. The mean age was 43.4 years and the mean BMI was 41.7 kg/m2 (Class III obesity). A majority of patients (75.8%) had undergone MBS.
Visits
30 patients (90.9%) visited the Clinic at least once; 83% returned. These patients made a median of 5.5 visits out of the 26 visits prescribed. Five out of 30 patients (16.6%) made 12-23 visits (representing 46-88% of the prescribed visits). Twenty-two out of the 30 patients had MBS before their referral. The time from MBS to referral varied widely. Two patients were referred within 6 months of surgery. Two were referred within 10-11 months. Thirteen patients were referred 1 to 4 years after surgery. Three patients were referred 5-8 years after surgery. Finally, 2 patients were referred over 10 years from surgery.
Facilitators and Barriers
Based on survey responses (Table 1), patients perceived the program to be most successful in terms of helpfulness of staff, the quality of food, language spoken and convenience of location (Table 1). Relative to other attributes, fewer respondents strongly agreed or agreed with the statements endorsing ease of transportation, convenience of hours, cultural appropriateness of foods and ease of parking, suggesting possible areas for further evaluation and program improvement. Health issues were the most often endorsed barrier to visiting the Clinic, followed by inadequate supplies of food and inability to store or reheat food (Table 1).
Next Steps
The primary goal of this initial evaluation was to identify barriers preventing patient compliance with the Clinic prescription. The next step will involve working closely with the Clinic’s team, as well as the Community Health and Engagement at Hartford Hospital, to explore ways to address these barriers. HHC has a very active volunteer program and Hartford Hospital serves as a community teaching hospital offering clinical experiences to aspiring physicians and other health care students. Volunteer opportunities and internships could be developed within the Clinic advancing community health experiences for students while allowing the clinic to increase its hours of operation.
A number of strategies could be employed to address issues related to food storage, processing and variety. HHC’s network of contacts at community organizations could be leveraged to obtain donations of kitchen equipment to facilitate the adequate storage of food once patients bring it home. Blenders, steamers and food processors could be particularly useful for patients post-MBS who could use them to process fruits and vegetables for easier consumption in the weeks after surgery. We are currently collecting feedback from Clinic clients on foods that would be more culturally appropriate yet have not been available at the Clinic.
Earlier intervention and use of more MBS-specific evaluation tools are other potential next steps. Evaluating program utilization before the end of the 6 month prescription period could afford us opportunities to determine when withdrawal from participation is most likely to occur. We could then introduce supportive measures to facilitate continued participation. For example, mobile smart devices could be leveraged to distribute reminders. Adding an MBS-specific measurement tool that takes into account the nutritional needs, dietary restrictions, and barriers to food utilization experienced by patients undergoing MBS would help us delineate ways in which these patients may use the Clinic differently from patients referred from other hospital divisions.
Our institution’s administrative and navigational resources could be further leveraged to identify sources of additional funding and to conduct patient education. Further securing state grants could aid in providing transportation services, extending hours of operation, increasing the food supply, and purchasing food storage or food preparation equipment for patients in need. Guiding patients to designate a proxy who can pick up their food at the Clinic if transportation or health issues arise may further support compliance.
Once these strategies are in place, repeating the survey would offer insights into the progress made in reducing barriers and improving adherence. We anticipate that this progress would be reflected in an increase in the number of visits to the Clinic. Finally we are in the process of evaluating utilization and barriers for patients from other hospital divisions and comparing these patients to MBS patients will be a high priority.
Lessons Learned
Almost all patients completing the survey attended the Clinic once, suggesting a high initial interest in the Clinic as an available resource. We learned that issues with transportation, parking, and hours of operation were the most salient barriers to their continued use of the Clinic. These barriers appear to be consistent across clinical and non-clinical populations.4,5
Implications for Practice
Prescribing nutritious foods for patients with food insecurity and comorbidities does not ensure they can or will fully utilize these prescriptions. Practitioners must evaluate obstacles that limit the use of such prescriptions and offer support to promote adherence. When food is used to address medical conditions, compliance should be managed in the same manner as medication prescriptions. Follow-up visits are necessary to document adherence, identify barriers, and assess how dietary interventions influence the resolution of medical issues, just as with any other type of prescription.
Footnotes
Author Contributions
Dawn Garcia: Conceptualization, Methodology, Investigation; Tara Proto: Conceptualization, Methodology, Writing—Original Draft, Writing—Review and Editing, Visualization, Project Administration; Pavlos Papasavas: Conceptualization, Methodology, Writing—Original Draft, Writing—Review and Editing, Supervision, Project Administration; Yin Wu: Methodology, Formal Analysis, Data Curation, Writing—Original Draft, Writing—Review and Editing, Visualization; Darren Tishler: Conceptualization, Writing—Original Draft, Writing—Review and Editing, Visualization, Project Administration, Supervision; Dale Bond: Conceptualization, Methodology, Writing—Original Draft, Writing—Review and Editing.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Darren Tishler serves as a consultant for Boehringer, Medtronic and Olympus. Pavlos Papasavas serves as a consultant for Boehringer and Medtronic.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Consideration
This project was reviewed by the Hartford Healthcare Institutional Review Board and was deemed not research.
Data Availability Statement
Data are available upon request to the corresponding author.
