Abstract
Background
The emergency department (ED) may present “teachable moments” for lifestyle medicine (LM) patient education about LM pillars, such as smoking, while they wait. Clinicians may assume that these patients are not motivated to change. This study evaluates readiness to change of ED patients concerning smoking.
Methodology
We utilized nested data from the prospective pilot Lifewise prevention study, randomizing lower acuity patients to an evidence-based lifestyle behavior educational video. Patients completed a validated readiness to change (RTC) survey. This analysis used data from before randomization, including patients who did not receive video education. Ordinal logistic regression was used to compare smokers to non-smokers, irrespective of video exposure.
Results
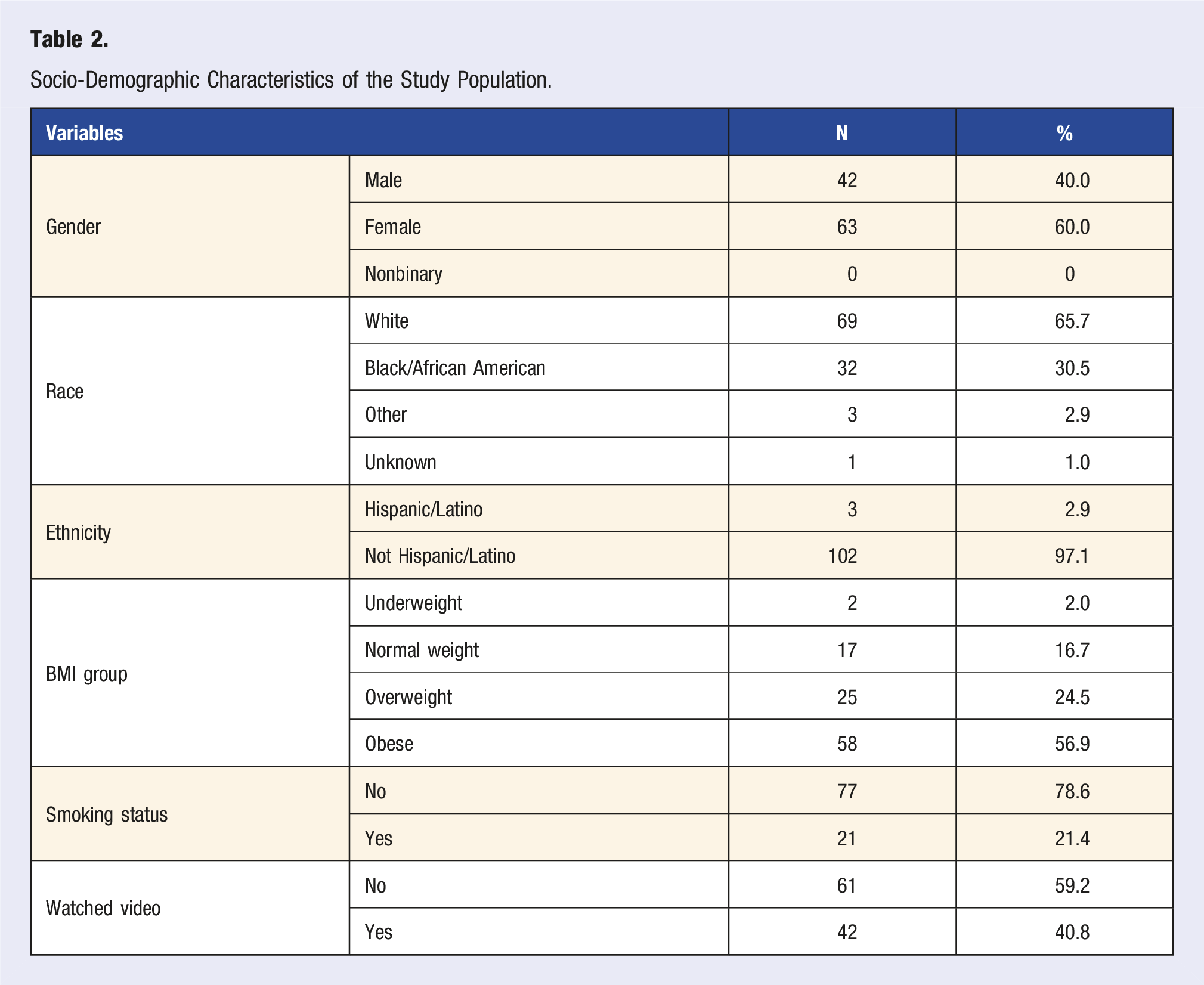
The 105 participants included 63 females and 42 males, with 31% being African American, 66% White, and 21% smokers. Individuals who reported smoking had higher odds of being ready to change their lifestyle behavior (OR 3.75, P = .013), however, participants who smoke exhibited significantly lower confidence levels compared to non-smokers (OR: 0.37, P = .043).
Conclusion
The ED may provide a “teachable moment” and a ripe opportunity for preventive LM education, including tobacco use. The data contradict some practitioners’ assumptions about these patients’ motivation to change.
Keywords
“Our study found that although smokers were motivated to discontinue smoking, they had low confidence in their ability to succeed.”
Introduction
There is an immense need to implement preventive medicine education into clinical practice. As much as four-fifths of health outcomes can be attributed to behavioral factors, with only a small percentage being defined by clinical care.1,2 With changes to lifestyle behaviors such as proper diet, sleep hygiene, regular exercise, and smoking cessation, many chronic diseases and conditions can be prevented. The emergency department (ED) may present “teachable moments” to encourage preventive care. However, the time practitioners spend with patients is increasingly limited, making this education challenging to provide.
Smokers are not being properly educated on smoking cessation despite 11.5% of American adults still smoking cigarettes. 3 According to a cross-sectional survey, although many or most patients are asked about their use of tobacco, far fewer receive counseling on strategies to stop smoking. 4 Physicians cited their lack of time and smoking being a “sensitive subject” as reasons for not educating them on smoking cessation. 4 In addition, practitioners assumed a lack of motivation (readiness) to quit among these patients. This nested study aimed to assess the stage of change for smoking cessation among patients, as defined by the Transtheoretical Model of Change (TMC). This investigation sought to determine patient’s actual readiness and confidence to change with respect to this high-risk behavior.
It has been previously reported that current smokers typically fall into a spread of 40% precontemplation, 40% contemplation, and 20% preparation with regards to quitting smoking. 5 These researchers suggest that when faced with the potential for serious adverse health outcomes, individuals can accelerate through some early stages, such as moving from precontemplation to contemplation or onto the preparation stage.
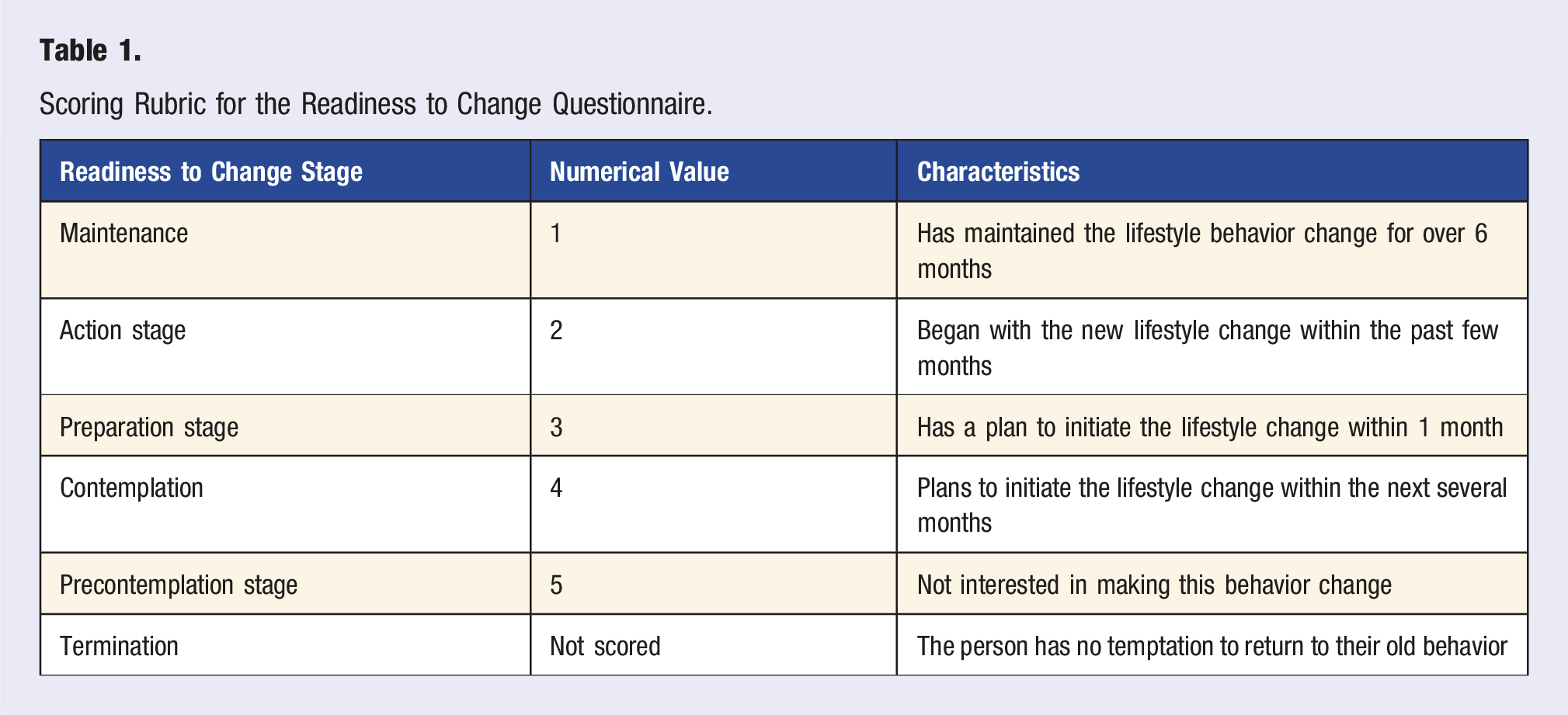
Scoring Rubric for the Readiness to Change Questionnaire.
Methods
Ethical Considerations
This study was approved by the hospital’s Institutional Review Board (Approval E-23-1055), and all participants were required to provide written informed consent for admission. The IRB approved the study as exempt under the implementation of the Final Revised Common Rule of 2017.
Study Design and Recruitment
The study was conducted in a suburban emergency department (ED) with an annual volume of approximately 50,000 patients. The research team deduced that the ED was an opportune setting to implement preventive education, making use of the long waiting times. Patients who presented to the ED with a chief complaint of chest pain had a lower severity of illness (acuity) based on the commonly used Emergency Severity Index (ESI). 7 This was defined as an ESI of 3-5 or 2 with normal vital signs. A total of 105 subjects were enrolled, including 63 females (60%) and none identifying as nonbinary. All participants received informed consent after the preliminary encounter with the practitioner, while patients were waiting for results and visit closure. The video lasted approximately 10 minutes and included 4 pillars of lifestyle medicine, including smoking cessation, exercise, diet, and sleep hygiene. 8 The responses to the survey component took an additional 10-12 minutes. The current study utilizes data on all patients, regardless of whether they received the video, and does not address other lifestyle domains. Further details of the Lifewise Preventive Education Pilot Trial are described previously. 9
After performing informed consent, the REDCap (Research Electronic Data Capture) randomization module assigned patients to the video or control group. REDCap is a secure, web-based software platform that supports data capture for research.10,11 All patients then completed the composite questionnaire in REDCap.
Outcome Measures
The composite questionnaire used the validated Readiness-to-Change and Confidence-to-Change questionnaires. 6 The Readiness-to-Change tool assesses patient readiness to implement ten lifestyle behaviors from the Gillespie and Lenz questionnaire on a 5-point scale. 6 Readiness is defined as a participant’s stage of willingness to adopt a specific lifestyle behavior, based on the TMC. 6 The scores and their descriptions are listed in Table 1.
The Confidence-to-Change questionnaire evaluated patient confidence in implementing the same ten lifestyle behaviors as the Readiness-to-Change questionnaire. The Confidence-to-Change questionnaire is based on a 3-point rating scale. Ratings are as follows: 3 very confident, 2 somewhat confident, and 1 not very confident. 6 Hence, it is very important to note that a higher number on the readiness to change scale corresponds with lower readiness, using a 5-point scale, while a higher number on the confidence to change scale corresponds to higher confidence, using a 3-point scale. The Confidence-to-Change questionnaire aimed to address any barriers or hesitancy that may impact patient confidence in implementing better lifestyle behaviors. The Readiness-to-Change questionnaire aimed to determine which stage of the TMC the patient was in and which behaviors clinicians should focus on first based on patient-reported readiness. Together, these 2 questionnaires allow patients and clinicians to develop realistic goals, discuss solutions to barriers, and strategize methods of maintaining better lifestyle behaviors.
Results
Socio-Demographic Characteristics of the Study Population.
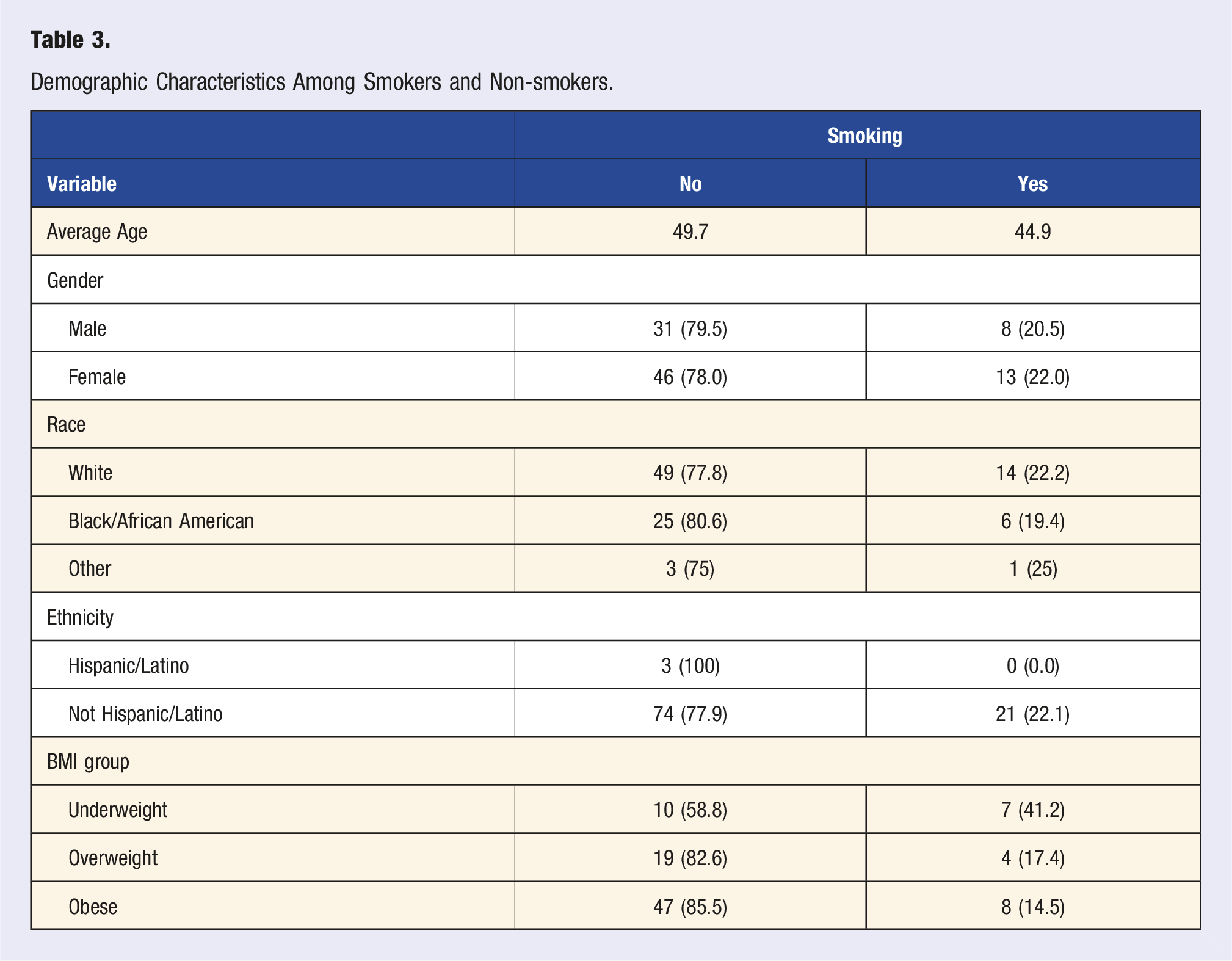
Demographic Characteristics Among Smokers and Non-smokers.
Factor Associated With Readiness to Change Using an Ordinal Logistic Regression Model.

Factors Associated With Confidence in Changing the Ordinal Logistic Regression Model.

Table 4 shows participants who reported smoking had significantly higher odds of being ready to change their smoking, with an OR of 3.75 (95% CI: 1.32, 10.64, P = .013).
Table 5 presents the results of an ordinal logistic regression model investigating factors associated with individuals’ confidence to change lifestyle behaviors. The OR and 95% confidence intervals (CI) reveal the relationship between smoking status and confidence levels. In terms of smoking status, participants who reported smoking exhibited significantly lower confidence levels compared to non-smokers (OR: 0.37, 95% CI: 0.14, 0.97, P = .043).
For smokers, the mean readiness to change value was 3.19, while the confidence to change was low at 2.26. It was interesting to find that smokers exhibited lower confidence to change than non-smokers across all domains of prevention (2.26 vs 2.51, P = .001).
Discussion
Although the sample size in this nested study was limited, measurement of RTC showed that smokers were highly motivated to discontinue smoking. Anecdotally, it may be commonly assumed by many practitioners that patients who exhibit high-risk characteristics may be resigned to their condition and not motivated to engage in meaningful change. A study of awareness of this heightened readiness to improve lifestyle behaviors can serve as a compelling reason for clinicians to serve as agents of health-change education.
Our study found that although smokers were motivated to discontinue smoking, they had low confidence in their ability to succeed. Prior investigations report that smokers typically make multiple unsuccessful attempts to quit, and most of these attempts are made by the individual without assistance. 12 The number of attempts before quitting successfully is estimated to range from 6.1 to as high as 142. 13 This mismatch between readiness and confidence indicates that the focus of the practitioner should be to inform the patient about the most successful strategies. For example, there is evidence that the combination of cognitive behavioral therapy with pharmacotherapy leads to greater success in tobacco cessation. 14 This finding emphasizes that this approach should be the primary message provided to smokers.
Interestingly, smokers exhibit lower confidence to change across all domains, not just smoking. This suggests that low self-efficacy in smoking cessation may extend to other preventive behaviors. Further research could determine whether quitting smoking improves engagement in other areas of preventive health.
This study was conducted in a distinctive setting for preventive education: the emergency department (ED). The relatively high readiness to change (RTC) among patients with these characteristics may be directly linked to the environment where the study took place—the ED. While primary care clinic visits are typically considered the most suitable setting for preventive education, the current study suggests that the ED may also offer a valuable opportunity to educate patients about positive lifestyle behaviors. Comparing the impact of lifestyle counseling across different clinical environments could provide further insights.
According to the Centers for Medicare & Medicaid Services, the median time patients spent in the ED nationwide was 2 hours and 40 minutes. 15 Patients often seek distractions by watching television or using smartphones during this time. Given the profound benefits of healthy lifestyles, prioritizing lifestyle education in the ED is a crucial use of this waiting period.
The limitations of this study include the small sample size of the pilot study from which the nested data was drawn. While the observed significance for RTC with these risk factors suggests strong motivation among these patients, it is important to note that the population was primarily suburban and relatively well-insured. Future studies should prioritize including a larger proportion of patients from lower socioeconomic backgrounds, as this group may benefit most from reduced healthcare needs.
Conclusion
This study using nested data shows promising signs that patients who smoke are ready to adopt healthier behaviors. Translating this readiness into health improvement requires further investigation. The gap between readiness and confidence highlights the need for practitioners to inform patients of the most effective smoking cessation strategies. Future studies should explore the potential for enhanced readiness to receive preventive messages in clinical environments where these strategies are not commonly used.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
Dylan Arroyo is funded by the Clinical Research, Innovation, and Scholarship Program (CRISP), University of Michigan-Dearborn. No pharmaceutical or industrial financing was used in this research.
Trial Registration
This nested data was taken from a small pilot study. Future, larger studies will be registered as clinical trial.
Ethical Statement
Data Availability Statement
The data set is available on request.
