Abstract
Lifestyle physical activity (LPA) interventions emphasize small bouts of movement that can be flexibly integrated into one’s everyday routine. Despite research illustrating benefits for LPA on health outcomes, few LPA interventions and measurement tools have been developed and tested. The purpose of this study was to present a novel LPA self-report scale, including its content, scoring, and internal consistency reliability, and summarize its intervention responsiveness. The LPA scale was administered in a pilot randomized controlled trial that tested a 12-week LPA + Fitbit intervention against a health education (HE) control (matched to LPA + Fitbit on contact time) in a sample of 50 women with depression in alcohol treatment. The LPA scale includes 22 items covering five domains relevant to LPA. Results demonstrated good internal consistency reliability for the total score (ω = 0.84) but poor-to-acceptable internal consistency reliability for the domain scores (ω range: 0.43-0.80). Participants randomized to the LPA + Fitbit intervention had significantly greater improvements in the LPA total score and two domain scores compared to HE participants. Overall, results demonstrate good internal consistency reliability and intervention responsiveness of the LPA scale total score. A larger, more comprehensive psychometric evaluation is needed for validation of this scale.
“Results demonstrated strong internal consistency reliability for the total score and responsiveness to an LPA-based intervention.”
Introduction
Engaging in physical activity is strongly associated with improved mental health and health-related quality of life as well as a reduced risk of mortality.1-3 Sedentary time has also emerged as a potent predictor of health outcomes (e.g., cardiovascular disease incidence, all-cause mortality) independent of the level of physical activity. 4 Dose-response analyses have demonstrated that even small amounts of increased physical activity confer health benefits with the greatest impact occurring for individuals initially engaging in low levels of activity. 5 In a study of over 100,000 people who self-reported no engagement in exercise, bouts of movement lasting as little as one to three minutes were associated with lower risk of major adverse cardiovascular events and mortality. 6 Considering the strong evidence for the value of increasing physical activity in any quantity, expert guidelines and recommendations have increasingly emphasized adding even small amounts of movement and reducing sedentary time (e.g., “move more, sit less”) independent of achieving a pre-specified amount of activity (e.g., 150 minutes/week).5,7-9
Lifestyle physical activity (LPA) is a paradigm of increasing physical activity through a focus on small bouts of movement that can be integrated into an individual’s daily life. 10 LPA encompasses a broad array of household, leisure, transportation, and occupational activities requiring movement (e.g., chores, walking the dog) and underscores the use of strategies to increase movement within one’s day-to-day routine (e.g., climbing the stairs to one’s apartment rather than taking the elevator) as opposed to solely focusing on dedicated physical activity sessions. 11 The LPA model has demonstrated comparable benefits in improving cardiorespiratory fitness to traditional continuous bouts of physical activity 12 and is associated with improved mental health outcomes including depression, anxiety, stress, and well-being. 13 Additionally, LPA’s flexible approach of integrating activity into one’s day-to-day life promotes better physical activity adherence. 14 Despite these promising findings, LPA interventions are largely understudied compared to traditional physical activity programs and there remains a gap in knowledge regarding best practices for measuring the impact of LPA interventions on physical activity. 15 Therefore, research efforts are needed to develop and evaluate both LPA programs and measurement tools to advance the physical activity field.
The purpose of this study was to present a novel LPA scale and report changes in scale scores from a pilot randomized controlled trial (RCT) that tested an LPA + Fitbit intervention against a health education (HE) control in a sample of 50 women with depression who were receiving treatment for alcohol use disorder. The two aims were to: (1) describe the content, scoring, and internal consistency reliability of the LPA scale and (2) examine differences in LPA scale scores between participants randomized to LPA + Fitbit and HE conditions. We hypothesized that those randomized to the LPA + Fitbit intervention would have larger improvements in the LPA scale scores compared to those randomized to the HE control condition.
Methods
Data collection for this two-arm parallel pilot RCT occurred between February 2017 and January 2019. Institutional Review Board approval was granted by the local institution and this study was registered on https://clinicaltrials.gov (NCT02705898).
Participants
The pilot RCT was focused on testing the effect of physical activity on recovery outcomes in women with depression in alcohol treatment. The sample was comprised of female participants between 18 and 65 years old who were enrolled in a partial hospital alcohol and drug treatment program. Additional inclusion criteria were: (a) diagnosis of alcohol use disorder, (b) at least mild depressive symptoms as measured by the Patient Health Questionnaire-9 (total score of at least five and a score greater than zero on one of the first two items), 16 (c) access to the Internet, (d) engaging in less than 150 minutes of moderate-intensity exercise/week over the past six months. Participants were excluded if they had: (a) moderate or severe substance use disorder, (b) current or recent anorexia or bulimia nervosa, (c) history of psychotic disorder, (d) current or recent psychotic or manic symptoms, (e) current suicidality or homicidality, (f) marked organic impairment, (g) physical or medical problems interfering with safe exercise, or (h) current pregnancy or plans to become pregnant during the next 12 weeks.
Out of 119 individuals screened for the study, 52 met inclusion criteria and were randomized. Out of the 52 randomized, two did not receive any intervention sessions, which left a sample of 50 participants.
Interventions
Participants in the LPA + Fitbit intervention condition received information on physical activity guidelines and the benefits of increasing physical activity, strategies for integrating physical activity into daily life (e.g., taking the stairs rather than elevator), and recommendations for using short bouts of physical activity to manage alcohol craving and difficult emotions. Additionally, participants were provided with Fitbit devices to track steps and to assist with setting physical activity goals. Study clinicians provided telephone (30-minute calls at weeks 1, 2, 4, 6, 8, and 10) and text messaging (two text messages/week) support to participants to enhance motivation, reinforce goals, and problem-solve barriers to physical activity.
The HE control condition included general information about health effects of alcohol use and the same contact time (i.e., telephone calls and text messages) as was provided in the LPA + Fitbit intervention group. Telephone calls and text messages focused on health behaviors other than physical activity such as sleep and nutrition. Participants in the HE control condition neither received information on physical activity nor were encouraged to change their physical activity levels during the study.
Procedure
All participants received medical clearance to initiate a physical activity program from the study physician and were randomized 1:1 to the 12-week LPA + Fitbit or HE intervention. Participants completed a paper and pencil version of the LPA scale in person at baseline and at the end of the 12-week intervention period.
Data Analysis
Analyses were conducted using R Version 4.3.2. and P < .05 was the threshold for statistical significance. Descriptive statistics were computed between groups for demographics and LPA outcomes at baseline. In addition to Cronbach’s alpha, McDonald’s hierarchical omega was calculated as a more conservative and robust measure of internal consistency reliability.17,18 The LPA scale total score and domain scores were calculated by summing items. Change scores (12-week minus baseline) for LPA outcomes (total and domain scores) were calculated for participants who completed the measure at both timepoints. A series of independent samples t-tests compared differences in LPA scores from baseline to end of intervention between the two intervention groups.
Results
Participants
Baseline Demographic Characteristics.
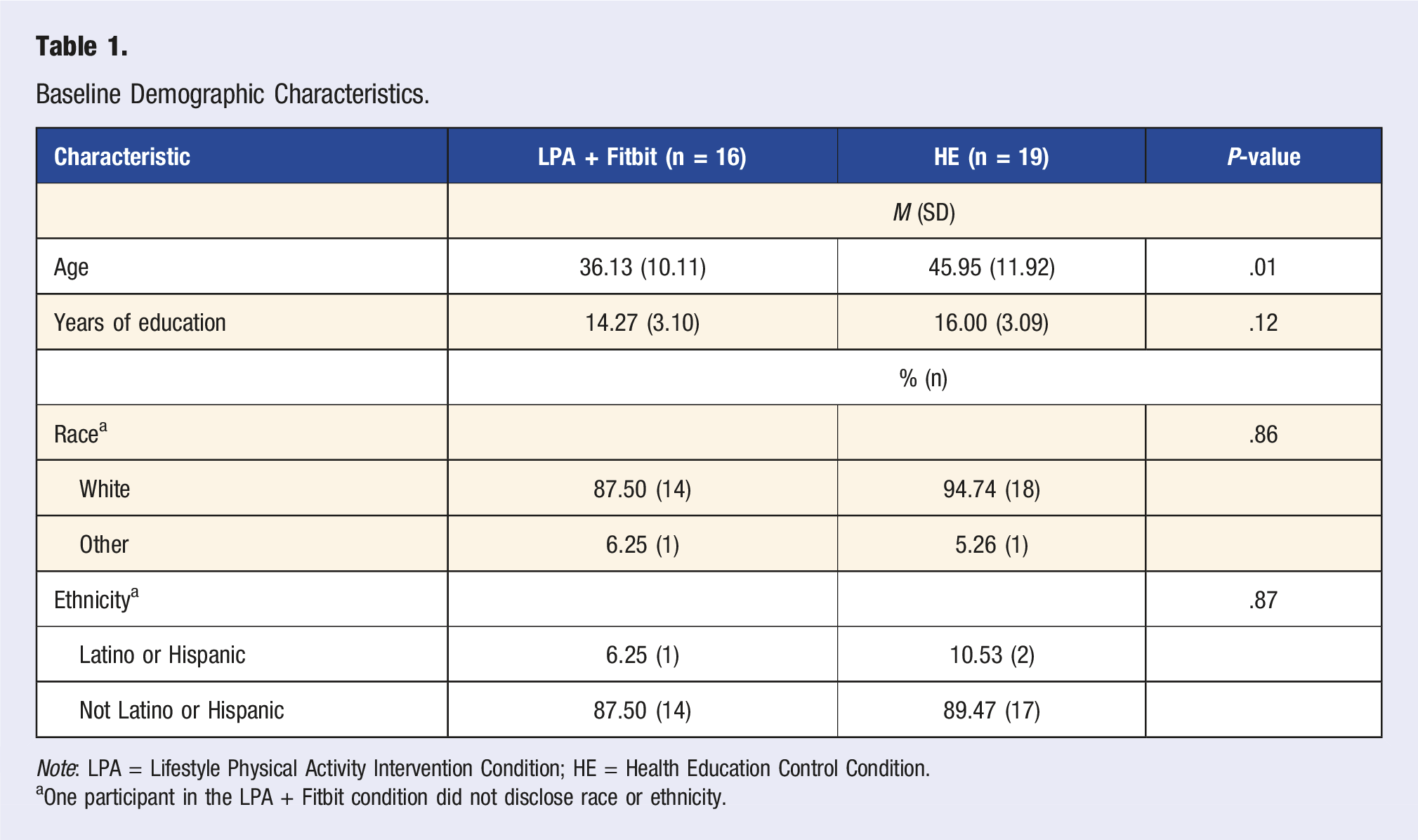
Note: LPA = Lifestyle Physical Activity Intervention Condition; HE = Health Education Control Condition.
aOne participant in the LPA + Fitbit condition did not disclose race or ethnicity.
LPA Scale Content and Scoring
Lifestyle Physical Activity Scale.
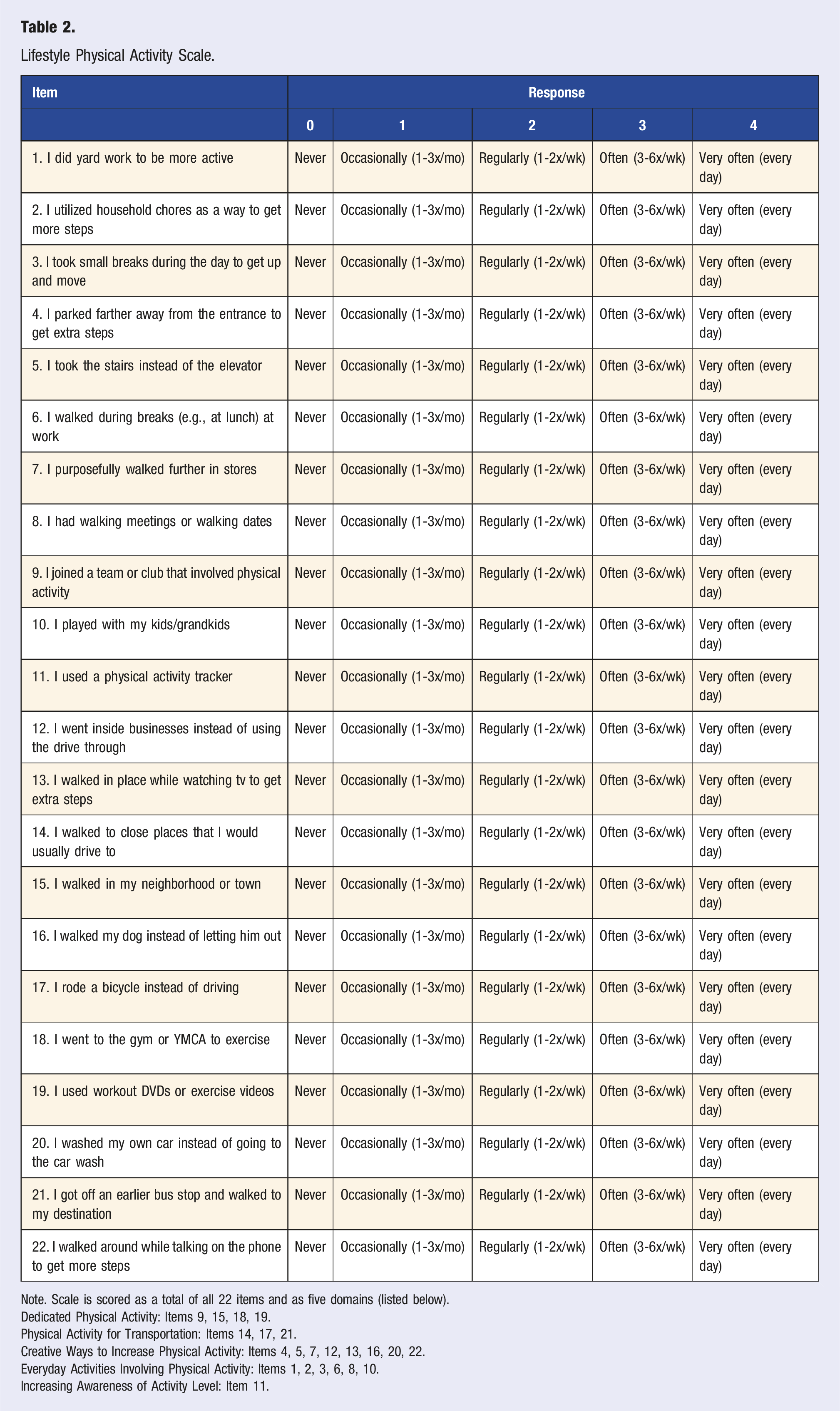
Note. Scale is scored as a total of all 22 items and as five domains (listed below).
Dedicated Physical Activity: Items 9, 15, 18, 19.
Physical Activity for Transportation: Items 14, 17, 21.
Creative Ways to Increase Physical Activity: Items 4, 5, 7, 12, 13, 16, 20, 22.
Everyday Activities Involving Physical Activity: Items 1, 2, 3, 6, 8, 10.
Increasing Awareness of Activity Level: Item 11.
Items on the LPA scale are scored in two ways: (1) a total score using all 22 items and (2) five domain scores comprised of items with conceptual similarities. The first domain, dedicated physical activity, includes four items assessing the frequency of engaging in actions specifically for physical activity (i.e., joining a club or team involving physical activity, walking, going to the gym, watching workout videos at home). The second domain, physical activity for transportation, includes three items (i.e., walking to places would typically drive to, riding a bicycle instead of driving, getting off at an earlier bus stop to walk to destination). The third domain, creative ways to increase physical activity, includes eight items (i.e., parking farther from a building entrance to get more steps, taking the stairs instead of the elevator, purposefully walking further in stores when running errands, going inside businesses instead of using a drive-up window, walking the dog instead of just letting them outside, washing my own car, walking in place while watching TV, walking while talking on the phone). The fourth domain, everyday activities involving physical activity, includes six items (i.e., doing yard work, doing household chores to get more steps, playing with kids/grandkids, taking small breaks to get up and move during the day, walking during breaks at work, having walking meetings or dates). The fifth domain, increasing awareness of activity level, includes one-item assessing how frequently a physical activity tracker is used.
LPA Scale Internal Consistency Reliability
Internal consistency reliability statistics were calculated using baseline data from the entire sample (n = 50). The LPA total score exhibited good internal consistency reliability (α = .79; ω = .84). The internal consistency reliability for conceptually based scores were poor to acceptable (dedicated physical activity: α = .31, ω = .47; physical activity for transportation: α = .38, ω = .43; creative ways to increase physical activity: α = .57, ω = .72; everyday activities involving physical activity: α = .64, ω = .80; Note: internal consistency reliability could not be calculated for the fifth domain as it consists of a single item).
LPA Scale Score Changes by Intervention Condition
LPA Scale Score Changes by Intervention Condition.
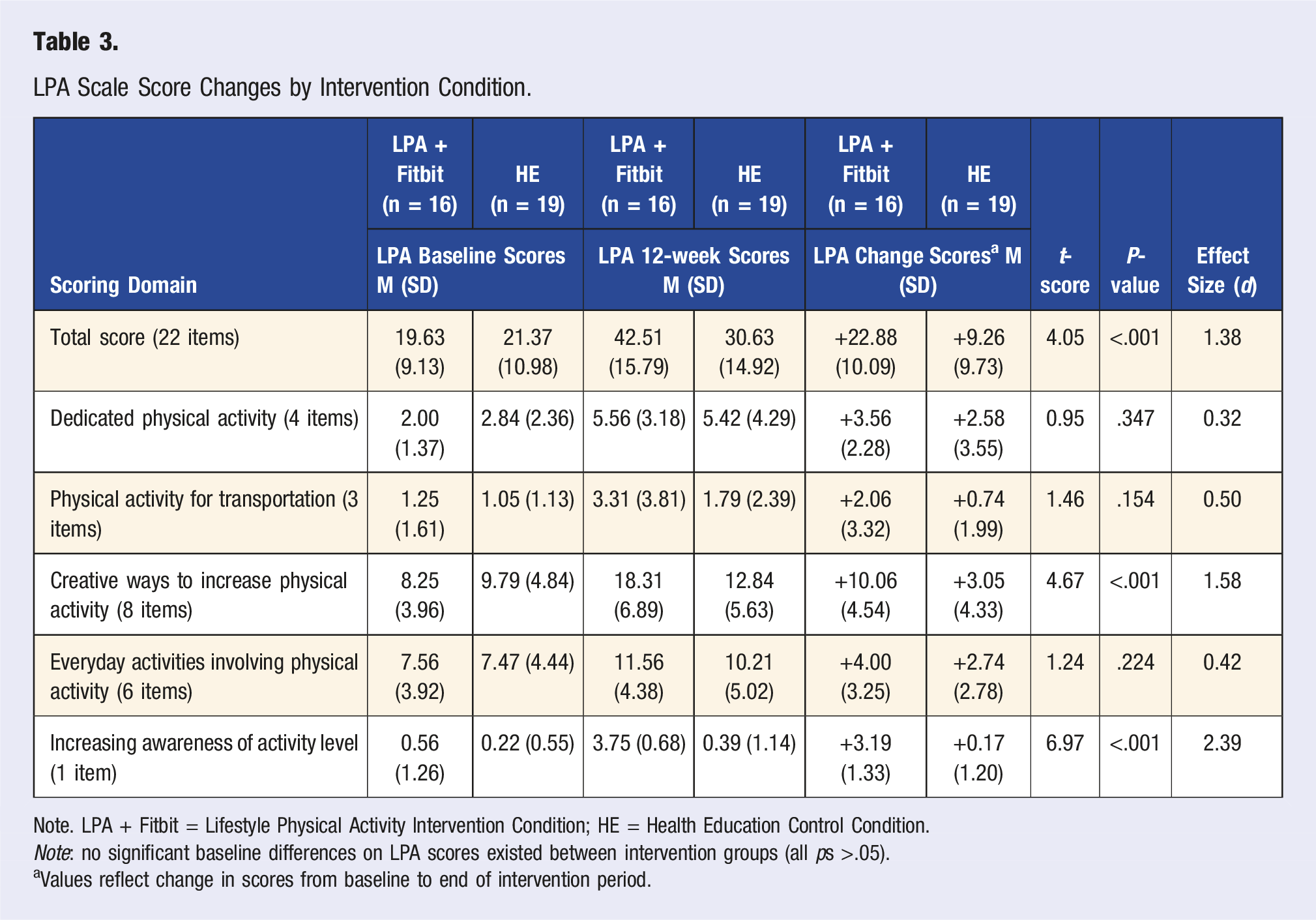
Note. LPA + Fitbit = Lifestyle Physical Activity Intervention Condition; HE = Health Education Control Condition.
Note: no significant baseline differences on LPA scores existed between intervention groups (all ps >.05).
aValues reflect change in scores from baseline to end of intervention period.
Discussion
This study presented a novel LPA scale that was developed for use in a pilot RCT examining an LPA + Fitbit intervention compared to a HE control condition. The LPA scale, which includes 22 items covering five domains relevant to LPA intervention efforts, demonstrated good internal consistency reliability on the total score. Greater improvements were observed for the LPA + Fitbit intervention group relative to the HE control group on the total score and two domain scores (creative ways to increase physical activity and increasing awareness of activity level) of the LPA scale. Overall, these results suggest promising preliminary data supporting the LPA scale’s total score reliability and responsiveness to an LPA-based intervention.
As expected, improvements in the LPA scale favored the LPA + Fitbit intervention group over the HE control condition. The finding that the LPA + Fitbit intervention group had greater increases in the domain of creative ways to increase physical activity compared to HE is especially promising given that this strategy is a central tenet of the LPA paradigm.10,11 Not only does this finding suggest that the LPA + Fitbit intervention performed as intended but it also provides valuable data that can complement additional physical activity metrics. For example, an initial pilot open trial of this study’s LPA + Fitbit intervention demonstrated increases in overall physical activity as measured by steps/day, 20 which suggests a potential intervention effect for increasing activity. Yet, this summary metric of activity does not capture the underlying day-to-day changes in an individual’s routine that led to the increase in activity. As such, the inclusion of the LPA scale has the potential to enhance interpretation of standard physical activity measures that capture amounts of movement 21 by providing context for the changes.
This study had three main limitations that provide important opportunities for future research. First, the sample was comprised of all female participants with depression, the majority of whom were white and Not Latino or Hispanic, who were receiving partial hospitalization treatment for alcohol use disorder, which limits generalizability to other populations. Second, the LPA scale was developed by the research team for use in a pilot RCT and did not undergo comprehensive scale development procedures (e.g., expert consensus, cognitive testing). 22 Third, the sample size was small and precluded our ability to conduct additional psychometric analyses. Relatedly, the domain scores were created based on conceptual similarities among items rather than analytically derived (e.g., through factor analysis), which could explain the low internal consistency reliability scores. As such, future research is needed to comprehensively evaluate the reliability and validity of the LPA measure in a larger, more diverse, sample of individuals. These psychometric analyses could inform important modifications to the domain scores to improve the internal consistency reliability. Additionally, future work could consider administering the LPA scale in combination with objective measures of physical activity (e.g., accelerometry) to explore relationships between these two types of measures.
This study was one of the first to develop and test an LPA scale for use in physical activity intervention research. Results demonstrated strong internal consistency reliability for the total score and responsiveness to an LPA-based intervention. As such, future LPA-based trials should consider including an LPA scale to allow for comparability of physical activity changes across studies.
Footnotes
Author Contributions
Conceptualization: JB, TFH, AMA, Methodology: AMA, MDS, CB; Formal analysis and investigation: TFH; Writing—original draft preparation: JB, TF; Writing—review and editing: JB, TFH, CB, MDS, AB; Funding acquisition: AMA; Resources: AMA; Supervision: AMA, CB, MDS.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: The authors do not have any conflicts of interest or competing interests to disclose. The views expressed in this article are those of the authors and do not necessarily reflect the position or policy of the United States Government or Department of Veterans Affairs (VA).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by the National Institutes on Alcohol Abuse and Alcoholism (NIAAA; R34 AA024038; PI: Ana M. Abrantes, Ph.D.). Drs. Browne and Halverson are supported by VA Rehabilitation Research and Development Career Development Awards (JB: IK2RX005010; TFH: IK2RX004803).
Ethical Statement
Data Availability Statement
Data can be made available upon reasonable request to the corresponding author.
